Scottish Health Survey 2017 - volume one: main report
Presents results for the Scottish Health Survey 2017, providing information on the health and factors relating to health of people living in Scotland.
3. Dental Health
Caroline Stevens
Summary
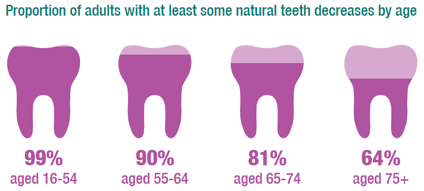
- Men were more likely than women to have at least some natural teeth (94% compared with 90%). This difference was evident only among those aged 65 and over.
- Over 3/4 of adults (78%) did not experience difficulties when visiting the dentist.
- The most common difficulties were finding an appointment that suited (7%), dental treatment being too expensive (6%) and getting time off work (5%).
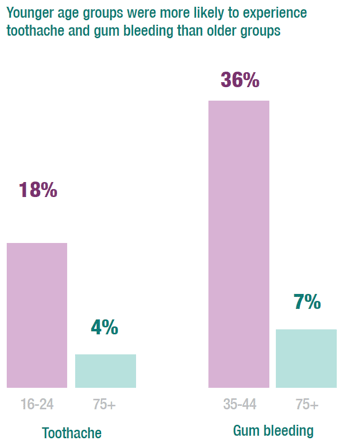
- However, having difficulty chewing either often or occasionally was most common among those aged 55-74 (13% among those aged 55-64 and 14% among those aged 65-74) and least common among the youngest age group (7% among those aged 16-24).
3.1 Introduction
The Oral Health Improvement Plan recently published (in early 2018) states the 'impact of a healthy mouth on general health is significant' with a recognition that improvements in oral health contribute to overall improvements in population health[1]. Oral disease can have a detrimental impact on work, school and other daily activities and as a result it has potentially wider socio-economic consequences. The most common types of oral disease are tooth decay and gum disease. Worldwide, between 60-90% of school children and nearly 100% of adults have tooth decay. As tooth decay[2] is so widespread and is largely preventable, it is considered a public health issue.
The oral condition of greatest concern due to its seriousness and increasing incidence is oral cancer[3]. Head and neck cancer, of which oral cancer and oropharyngeal cancer are types, account for around 3% of total cases of cancer in the UK[4]. There are twice as many cases of oral cancer diagnosed every year in Scotland compared to England and Wales[5]. Major risk factors for oral cancer include tobacco use and excessive alcohol consumption[6] and as a result, incidence is higher in men and older age groups[7],[8].
Child and adult dental registration rates have increased in recent years, 92% of the Scottish population was registered with a dentist in September 2017 with rates higher among children than adults (94% and 92%, respectively)[9]. Over 7 out of 10 (72%) of registered patients had visited an NHS dentist in the previous 2 years with children more likely to have done so than adults (85% and 67% respectively)[10]. There has also been a recent increase in the cost of provision of General Dental Services and Public Dental services since 2015/16[11], highlighting an increase in demand largely due to an ageing population and the increase in people retaining their teeth[12].
Further improvements to oral health is evidenced by the findings of the Detailed Inspection programme of P7 children in 2017 which showed that over three quarters (77%) of P7 children had no obvious signs of tooth decay in their permanent teeth which has increased significantly from 53% in 2005[13]. Despite these improvements, inequalities in oral health persist[14] for example children and adults living in the most deprived areas were less likely to have visited a dentist in the past two years than people living in the least deprived areas (among children 81% in the most deprived and 90% in the least deprived and among adults 64% compared to 75%)[15]. Also while 86.5% of P7 children living in the least deprived areas had no obvious tooth decay only 65.6% of P7 children living in the most deprived areas had no signs[16].
The latest figures indicate that there has been a long term increase in the incidence of oral cancer particularly among young people which is possibly due to changing patterns of alcohol and tobacco consumption[17]. Recent and growing evidence also suggests that there is also a link between human papilloma virus (HPV) and mouth and throat cancer[18] as well as oropharyngeal cancer[19].
3.1.1 Policy background
A Stronger Scotland: The Government's Programme for Scotland 2015-16[20] recognised deficiencies in the current dental system, which had been set up when levels of dental health were poorer and people of all ages required multiple fillings and extractions. It identified a need to transform the system to meet the needs of younger people who require a preventive focus whilst ensuring that the system continues to allow for the treatment needs of the older population.
The Oral Health Improvement Plan was published in January 2018 following extensive consultation with professionals and the public[1]. This plan sets out strategies to improve the oral health of the population and to provide high quality NHS dental services in years to come. The plan proposes a move away from restorative dentistry to a more preventative model. It also recognises poor dental health as a wider public health concern beyond only dentistry as it is closely intertwined with other public health problems such as poor diet as well as smoking and alcohol consumption.
The Oral Health Improvement plan has a number of aims:
- Developing a preventative model for oral healthcare
- Reducing oral health inequalities
- Meeting the needs of an ageing population
- Providing more services on the high street
- Improving information for patients
- Increasing quality assurance and improvement
- Developing and enhancing the dental workforce
Prevention
Childsmile is a preventative programme that encourages toothbrushing and fluoride varnish application in nursery and primary school age children. This programme also distributes toothpaste and brushes for home use and involves dental practices providing preventative care for children. The Oral Health Improvement Plan aims to ensure that good habits learned through Childsmile are maintained throughout childhood and into adulthood. Further, it aims to introduce a preventative care programme for adults. This preventative care programme will be dependent on the degree of risk of developing oral cancer, gum disease and decay due to lifestyle factors such as diet, alcohol consumption and smoking status.
Reducing oral health inequalities
Evidence from the National Dental Inspection Programme[21] (NDIP) shows that although oral health has improved significantly across all communities, children living in the most deprived communities still have more decay experience compared with those in the least deprived. The Oral Health Improvement Plan will ensure that community-level interventions form a significant part of the overall approach to addressing health inequalities as a means to engage 'hard-to-reach' groups. Further, the plan will ensure that practitioners working in deprived areas have appropriate payments and allowances to reflect the needs of their patients. This will encourage dental practices to continue to provide care to patients in areas of greatest oral health need, such as those with a high degree of deprivation.
Meeting the needs of an ageing population
The ageing of the Scottish population means that over the next ten years the number of people over 75 is projected to increase by 27% and by 79% over the next 25 years[22]. The improvements that have been made in oral health in Scotland have also presented new challenges. The increasingly ageing population, combined with more adults retaining some or all of their natural teeth, is likely to mean there will be a significant increase in people requiring domiciliary dental care, either in their own home or in residential care. The Oral Health Improvement Plan aims to provide a greater system of care for those in care homes. Dental practitioners would work with care home staff to ensure adequate preventative care is in place for residents, and would introduce arrangements to enable dental practitioners to visit patients in care homes. This arrangement will also be introduced to people who are cared for in domiciliary settings.
Providing more services on the high street
This aim is to ensure that patients are treated in the appropriate setting i.e. within Hospital Dental Services (HDS) or by General Dental Practitioners (GDPs). This involves obtaining adequate data on primary-secondary care pathways as well as ensuring that GDPs have the skills and expertise to deliver a wide range of treatment and are accredited to do so.
Improving information for patients
In recognition that the public do not consider themselves to have enough information about oral services available from the NHS and the associated costs, action is being taken to ensure that this information is made available and that it is streamlined across all GDPs.
Quality assurance and improvement
The aim is to enhance and improve service delivery, scrutiny and quality assurance in NHS dental care through a number of actions including introducing a Director of Dentistry in each Health Board area and developing a single database for quality improvement information for NHS Boards. Much of this work will build on Building a comprehensive approach to reviewing the quality of care: Supporting the delivery of sustainable high quality services which established the need to develop a new framework in dentistry that will improve care within practices, NHS Boards and nationally[23].
Workforce
The NHS dental practitioner workforce has increased significantly over the past ten years, a 46% increase, from 2,474 dentists in 2007 to 3,603 in 2018[24]. The plan sets out the need for the workforce to continuously develop and adapt with a particular emphasis on working within a healthcare setting which promotes prevention and which needs to adapt to the increased demands as a result of an increase in the older population people.
3.1.2 Reporting on dental health in the Scottish Health Survey (SHeS)
The focus of this chapter is on dental health and actions taken by individuals to improve dental health. The section on dental health presents the findings on the prevalence of natural teeth in the Scottish population in 2017 and allows for further analysis by age and sex. In addition deprivation trends in prevalence of natural teeth are presented from 2008. The remainder of the chapter explores dental treatment in relation to the pattern of visits to the dentist, anxiety about going to the dentist, difficulties experienced when arranging to see a dentist and dental health problems such as toothache, bleeding gums and difficulty chewing.
The area deprivation data are presented in Scottish Index of Multiple Deprivation (SIMD) quintiles. Where appropriate, to ensure that comparisons are not confounded by different age profiles within categories, data have been age-standardised. Readers should refer to the Glossary at the end of this Volume for a detailed description of SIMD and age-standardisation.
The area deprivation trend data have been age-standardised using 2016 mid-year household population estimates applied to each year 2008 to 2017 separately. This enables comparisons across years to be made without estimates being affected by changes to the age composition of the population. However figures may differ slightly from previously published figures using different mid-year population estimates. The closest SIMD rating was used for each year of the data: 2017 data uses the 2016 ranking (as does 2016) whereas the 2012 data uses the 2012 ranking (as does 2010-2015) and the 2008 and 2009 data uses the 2009 ranking.
Supplementary tables are also available on the Scottish Government SHeS website[25].
3.2 Methods and Definitions
Adults aged 16 and over are asked questions on dental health annually and on dental health services and actions taken to improve dental health biennially. Due to several changes made to the questions on dental health prior to 2008 only data from 2008 is presented in this chapter. More information about the changes made in 2008 is provided in the 2008 and subsequent reports[26].
3.3 Dental Health
3.3.1 Number of natural teeth and prevalence of no natural teeth in 2017, by age and sex
In 2017 the vast majority (92%) of adults in Scotland had at least some natural teeth while 8% had none. Around three in four people (76%) had 20 or more natural teeth. Men were more likely than women to have some natural teeth (94% and 90% respectively).
In concurrence with previous SHeS reports, natural teeth prevalence was lower in older age groups for both men and women in 2017. Almost all (97-100%) adults aged 16-54 reported having at least some natural teeth, which decreased to 90% for those aged 55-64, 81% for those aged 65-74, and 64% for those aged 75+.
Overall among those aged 65 and over prevalence of natural teeth is significantly associated with sex. As Figure 3A shows the rate of men reporting to have at least some natural teeth was higher than women in both the 65-74 age group (87% compared with 75%) and the 75 and over age group (70% compared with 60%), although this was outside the 95% level of significance among those aged 75 and over. There were no significant differences in prevalence of some natural teeth between men and women under the age of 65. Figure 3A, Table 3.1

3.3.2 Trends in prevalence of natural teeth since 2008 (age-standardised), by area deprivation and sex
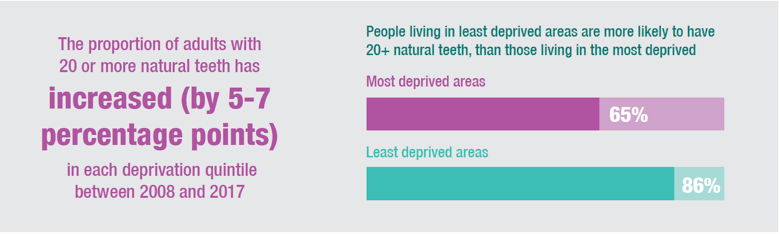
There are some significant trends in natural teeth prevalence from 2008 to 2017 by year and area deprivation. For all adults, results shows that all quintile areas with the exception of the most deprived have seen a significant increase in the rate of having 20 or more natural teeth since 2008. The data shows a 6-7 percentage point increase among those living in all areas, apart from the most deprived, over the time period. Among those living in the most deprived areas, there has been a five percentage point increase although this was not statistically significant.
In every year since 2008, area deprivation has had a significant impact on the prevalence of natural teeth. The rate of those in the most deprived areas reporting to have 20 or more teeth has ranged from 58-65% across the years compared with 79-86% for those in the least deprived area. The gap between the least deprived and most deprived has fluctuated between 19% and 23% between 2008 and 2017 (19% in 2008 and 21% in 2017). Table 3.2
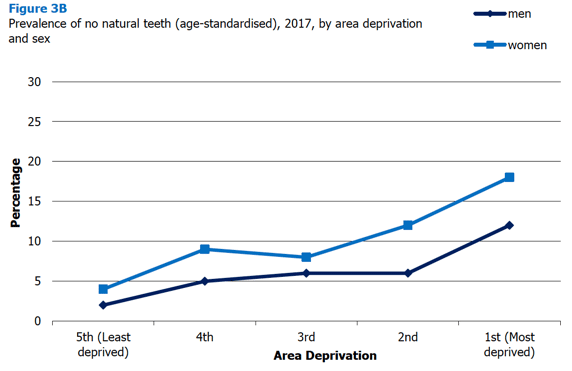
3.3.3 Number of natural teeth and prevalence of no natural teeth in 2017, by area deprivation and sex
There are significant differences in the prevalence of natural teeth by deprivation for both men and women in 2017. While 97% of all adults living in the least deprived areas report having at least some natural teeth, this figure decreases to 93% in the 4th and 3rd deprivation quintiles, 91% in the 2nd quintile, and 85% among those living in the most deprived areas. For men prevalence of having some teeth declined by 10 percentage points from 98% among those living in the least deprived areas to 88% in the most deprived areas. For women it declined by 14 percentage points with the same pattern of decline by deprivation (96% to 82%).
Conversely the proportion with no natural teeth increased fivefold for those living in the most deprived areas to 15% from 3%.
Figure 3B, Table 3.3
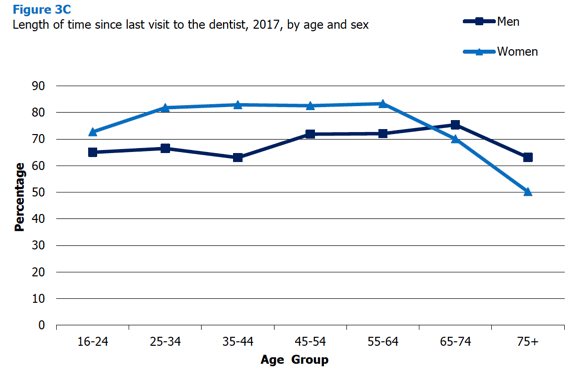
3.3.4 Length of time since last visit to the dentist in 2017, by age and sex
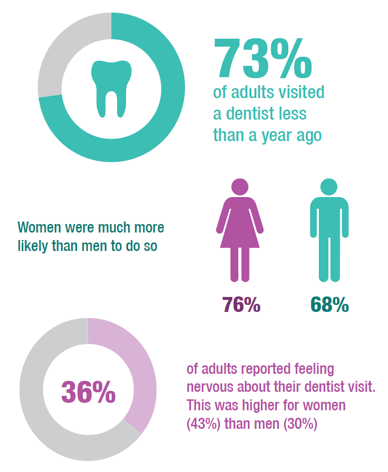
In 2017 around three-quarters (73%) of all adults aged 16 and over reported having visited the dentist less than a year ago. This left 10% having visited the dentist more than one year ago and up to two years ago, for 8% it had been more than two years and up to five years, a further 8% had visited over five years ago and under 0.5% of people had never visited the dentist. Women were significantly more likely to have visited the dentist less than a year ago compared with men (76% and 68%, respectively). Table 3.4
The length of time since last visiting the dentist varied significantly by age and a different pattern was observed for men and women. For women, the rates of visiting the dentist less than a year ago increased from 73% among those aged 16-24 to 82%-83% among those aged 25-64 before declining to 70% among those aged 65-74 and declining further still to 50% among those aged 75 and over. For men the rates were fairly stable among those aged 16-44 (ranging from 63-66%) before increasing to 72% among those aged 45-54 and 55-64 and further increasing to 75% among those aged 65-74 before declining to 63% among those aged 75 and over. Figure 3C, Table 3.4
3.3.5 Dental anxiety about visiting the dentist in 2017, by age and sex
Approximately one-third (36%) of adults in 2017 reported feeling either a bit nervous (21%) or very nervous (15%) about visiting the dentist. Women were more likely than men to report feeling some degree of nervousness (43% and 30%, respectively). The relationship between whether a person experiences nervousness about visiting the dentist and their age was unclear and not statistically significant at the 95% level. Table 3.5
3.3.6 Difficulties experienced when visiting the dentist in 2017, by age and sex
In 2017, almost 8 in 10 adults (78%) did not have difficulties related to visiting the dentist. The most common difficulties people experienced were difficulty in getting an appointment that suited them (7%), dental treatment being too expensive (6%) and difficulty in getting time off work (5%).
There were some differences in the type of difficulties experienced when visiting the dentist by age group. Those aged 25-34 and 35-44 were the most likely age groups to report having difficulty getting an appointment that suited them (13% and 11% respectively). Adults aged 25-54 were the most likely to report difficulty in getting time off work (9% among those aged 25-34 and 8% among those aged 35-54). Younger adults aged 16-24 (9%) and 25-34 (11%) were the most likely to find dental treatment too expensive. Among older people the most common difficulties were dental treatment being too expensive (only for those aged 65-74) and having a long way to go to the dentist (for those aged 65-74 and 75+ both 4%). Table 3.6
3.3.7 Dental health problems in 2015/2017 combined, by age and sex
The 2015/2017 combined data shows that prevalence of toothache was significantly higher among adults in younger age groups than those in older age groups, with 18% of those aged 16-24 reporting this, gradually decreasing to 4% of those aged 75+. This is likely to be partly due to the increasing proportion of adults who report having no teeth in the older age groups.
Gum bleeding is also significantly associated with age although a different pattern is apparent. Of those aged 16-24, 29% reported to have gum bleeding either often or occasionally increasing to 35% of those aged 25-34 and 36% of those aged 35-44 before decreasing steadily to 7% of those aged 75+.
Experiencing difficulty chewing either often or occasionally also varied significantly by age with prevalence highest among those aged 65-74 (14%) and 55-64 (13%) and lowest among those aged 16-24 (7%).