Scottish Health Survey 2018: main report - revised 2020
An amended version of the Scottish Health Survey 2018 main report.
Chapter 2 General Health, Cardiovascular Diseases and Caring
Summary
- 71% of adults, in 2018, described their health as ‘good’ or ‘very good’, the lowest recorded since 2008.
- 94% of children described their health as ‘good’ or ‘very good’, with little change from previous years.
Adults who assessed their general health to be ‘good’ or ‘very good’ varied by age:
- In 2018, 16% of adults reported having any CVD (cardiovascular disease), with 7% reporting having doctor-diagnosed diabetes (primarily type 2 – 6%), 20% having any CVD or diabetes, 5% having IHD (ischaemic heart disease), 3% having a stroke and 7% having a stroke or IHD.
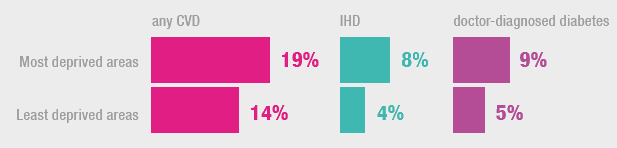
Prevalence of diabetes, any CVD and IHD continued to be higher in the most deprived areas.
- The proportion of adults providing unpaid care for a family member, friend or someone else remained at 15% among those aged 16 and over and 4% for children aged 4-15.
- The largest proportion of carers spent up to 19 hours per week providing unpaid care in 2017/18 (32% up to 4 hours and 34% 5-19 hours per week). Nearly twice as many of those aged 65 and over (22%) reported providing 50 hours or more, compared with 12% of those aged 16-44 and 2% of those aged 4-15.
- 7 in 10 unpaid carers aged 4 and over reported receiving no help or support (69%), with a significant variation between those who provided care for fewer than 35 hours per week (75%) and those who provided 35 hours or more of unpaid care per week (40%).
Provision of unpaid care was higher among adults living in the most deprived areas compared with the least deprived areas.

Unpaid care provision was higher among women than men.
Average age standardised WEMWBS scores amongst care givers showed that mental wellbeing was significantly lower among those who spent a greater number of hours per week providing unpaid care.

2 General Health, Cardiovascular Conditions And Caring
Victoria Wilson
2.1 Introduction
This chapter covers the following topics: self-assessed general health, cardiovascular disease, diabetes and unpaid caring.
Population measures of self-reported health can be general indicators of the burden of disease on society. They can reflect subjective experiences of both diagnosed and undiagnosed illnesses, and their severity, which more objective measures for the whole population can sometimes overlook.
Self-assessed general health is often a reflection of the presence or absence of long-term conditions, both physical and mental. An estimated 2 million people in Scotland live with one or more long term conditions[1], placing substantial operational and financial responsibility on healthcare provision and services[2]. Older people are more likely to have at least one long-term condition and often multiple conditions. In the context of an ageing population, where the proportion aged 75 and over is expected to increase by 60% by 2031[3], this remains a critical health issue for Scotland.
Cardiovascular disease (CVD) is a general term describing diseases of the heart and blood vessels whereby blood flow to the heart, brain or body is restricted. Its main components are ischaemic heart disease (IHD, or coronary heart disease) and stroke, both of which are well-established clinical priorities for the NHS in Scotland[4],[5]. Since 2008, there has been a steady downward trend in deaths from coronary heart disease and stroke in Scotland. Between 2008-2018 the mortality rate for coronary heart disease has decreased by 37.2% and mortality rates for stroke has decreased by 40.9% over the same period.[6],[7] Despite these reductions, coronary heart disease (CHD) remains one of the leading causes of death in Scotland. In 2018, there were 6,615 deaths in Scotland where CHD was the underlying cause[8]. Stroke also remains one of the biggest killers in Scotland and the leading cause of disability[9].
Diabetes, the most common metabolic disorder, is a growing health challenge for Scotland. Prevalence of people registered with Type 1 diabetes has increased from 26,294 in 2006 to 31,447 in 2017 and the number of people registered with Type 2 diabetes increased from 166,926 in 2006 to 263,271 in 2017[10]. For Type 1 diabetes, this reflects better survival and the rising incidence in children[11]. For Type 2, increase in reported prevalence depends on a number of factors, including: demographic change - diabetes is more prevalent in older people, so the increasing number of older people each year increases the prevalence of diabetes - better survival, and possibly better detection[12].
It is estimated that 3 in 5 people are likely to become a carer at some point in their lives[13]. The care they provide is of significant value, however, such a role can have a negative impact on the physical and mental health and wellbeing of carers, especially given the over-representation of carers in midlife and older age groups[14]. Around half of those who provide unpaid care are living with a long term condition themselves[15]. Having caring responsibilities can also impact on finances, employment opportunities, social relationships and more[16]. Understanding the prevalence of caring and the level of support received from the perspective of carers themselves is vital in informing the delivery of support plans and initiatives for these individuals.
2.1.1 Policy background
The Scottish government recognises the importance of working towards sustainable healthcare provision, particularly in the context of the changing Scottish demographic, notably an ageing population and increasing numbers of people living with long term conditions and multi-morbidity. The strategic policy focus on promoting and improving general health and wellbeing and supporting people living with long term is set-out in three over-arching strategies.
The National Clinical Strategy[17], published in 2016, is a high level vision for how health and social care services need to and should change over a 15 year period. The Health and Social Care Delivery Plan[18] presents a programme that is focused on prevention, early intervention and support for self-management. The aim is to enable those living in Scotland to live longer, healthier lives with the highest standard of care, be this at home or in a homely setting.
Practising Realistic Medicine[19], publishedin 2018, outlines ways to support the translation of the principles of the previous report(Realising Realistic Medicine[20]) from theory through to patient-centred, practical application. In addition to encouraging a personalised approach to individual patient care and tackling sustainability of NHS service provision, the report examines the ways in which the principles of realistic medicine can be applied to positively influence the social determinants of health such as childhood experiences, social support, access to health services and more.
Underpinning these strategies, Public Health Priorities for Scotland[21]sets out six public health priorities, aimed at improving the health of Scotland and increasing healthy life expectancy, including, amongst others a range of initiatives geared towards achieving a Scotland where people eat well, have a healthy weight and are physically active.
The Scottish Government's strategy for long-term condition self-management Gaun Yersel[22] recently celebrated its tenth anniversary. Since its launch in 2008, the strategy has been widely referenced as a means of supporting individuals with long-term conditions and their carers to take control of and manage their own health and care. This, along with the Scottish Government's long-term condition strategies (the over-arching Action Plan[23] published in 2009 and the separate heart disease[24], stroke[25] and diabetes[26] improvement plans published in 2014) supports the National Performance Framework National Outcome that 'we are healthy and active[27]. A number of the National Indicators are linked to reducing Cardiovascular Disease (CVD) risk factors, most notably smoking as part of the health risk behaviours indicator, but also physical activity and maintaining healthy weight[28],[29](the latter two are also major risk factors for Type 2 diabetes).
The Scottish Government's commitment to unpaid carers in Scotland is reflected in the Carers (Scotland) Act 2016[30], which took effect in 2018. This extended the rights of carers to ensure that they receive better support whilst also maintaining/ improving their own health and enjoying a life beyond their caring role. Significant rights enshrined in the Act include a personalised plan to identify a carer's needs for support and help them to access appropriate support before situations reach crisis point[31].
Embedding carers' rights to support under the Carers Act is a priority for the Scottish Government and partners, in line with the agreed implementation plan[32]. This is complemented by initiatives such as the Short Breaks Fund[33] and the Carer Positive scheme which recognises employers who provide a supportive working environment for carers[34].
2.1.2 Reporting on general health, long-term conditions, CVD conditions, diabetes and caring in the Scottish Health Survey (SHeS)
The Scottish Health Survey provides valuable information on self-reported general health, prevalence of CVD conditions and diabetes across different population groups in Scotland. In this chapter, trends in self-assessed general health, self-reported CVD conditions and diabetes prevalence for adults are presented between 2003 and 2018 and each is also reported separately for 2018. Prevalence of caring and hours spent caring each week is reported for both adults and children. In addition, mental wellbeing (WEMWBS mean score) and support received by carers are both reported by hours spent caring per week.
The area deprivation data are presented in Scottish Index of Multiple Deprivation (SIMD) quintiles. To ensure that the comparisons presented are not confounded by the different age profiles of the quintiles, the data have been age-standardised. Readers should refer to the Glossary at the end of this Volume for a detailed description of both SIMD and age-standardisation.
Supplementary tables on general health and CVD are also published on the Scottish Health Survey website[35].
2.2 Methods And Definitions
2.2.1 Methods
Self-assessed general health
Each year, participants who are aged 13 and over are asked to rate their health in general with answer options ranging from 'very good' to 'very bad'. For children under the age of 13 the question is answered by the parent or guardian completing the interview on their behalf.
CVD conditions and diabetes
Participants were asked whether they had ever suffered from any of the following conditions: diabetes, angina, heart attack, stroke, heart murmur, irregular heart rhythm, or 'other heart trouble'. If they responded affirmatively to any of these conditions, participants were asked whether they had ever been told they had the condition by a doctor and whether they had experienced the conditions in the previous 12 months. For the purposes of the analysis presented in this chapter, participants were only classified as having a particular condition if they reported that the diagnosis had been confirmed by a doctor.
It is important to note that no attempt was made to verify these self-reported diagnoses objectively. It is therefore possible that some misclassification may have occurred because some participants may not have remembered (or not remembered correctly, or not known about) diagnoses made by their doctor.
Caring
Participants were asked whether they look after, or give any regular help or support to, family members, friends, neighbours or others because of a long-term physical condition, mental ill-health or disability; or problems related to old age. Caring which is done as part of any paid employment is not asked about. From 2014 onwards, this question explicitly instructed respondents to exclude caring as part of paid employment. This question has been asked of adults aged 16 and over since 2008, and of children aged 4 to 15 since 2012. Those who say they provide such care are then asked how many hours per week they typically provide. An additional question explores the impact that caring has on employment.
2.2.2 Definitions
Any CVD condition
Participants were classified as having 'any CVD' if they reported ever having any of the following conditions confirmed by a doctor: angina, heart attack, stroke, heart murmur, abnormal heart rhythm, or 'other heart trouble'[36].
Diabetes
Participants were classified as having diabetes if they reported a confirmed doctor diagnosis. Women whose diabetes occurred only during pregnancy were excluded from the classification. In 2018 a new question was introduced asking participants to report if they had been told they had Type 1 or Type 2 diabetes. Prior to 2018, no distinction was made between Type 1 and Type 2 diabetes in the interview.
Any CVD condition or diabetes
A summary measure of the above conditions is presented in the tables as 'any CVD condition or diabetes'.
Ischaemic heart disease (IHD)
Participants were classified as having IHD if they reported ever having angina or a heart attack confirmed by a doctor. All tables refer to ever having had the condition.
Stroke
Participants were classified as having a stroke if they reported ever having had a stroke confirmed by a doctor.
IHD or stroke
A summary measure of the above conditions is presented in the tables as 'IHD or stroke'.
2.3 Self-Assessed General Health
2.3.1 Trends in self-assessed general health since 2008
The highest level of self-assessed 'good' or 'very good' health for adults was reported in 2009 (77%). Between 2017 and 2018, the level fluctuated between 73% and 74%, with the 2018 level the lowest in the timeseries so far at 71%. At the other end of the scale, the level of self-assessed 'bad' or 'very bad' health has remained relatively stable within the range of 7-9% since 2008 (9% in 2018). The patterns for men and women have been similar since 2008.
The clear majority of children self-assessed their health to be 'good' or 'very good' in 2018 (94%), while 1% indicated that this was 'bad' or 'very bad'. These levels are consistent with those recorded since 2008 (94-96% 'good' / 'very good' and 0-1% 'bad' / 'very bad'). In 2018, there was very little variation between the proportions of boys (93%) and girls (95%) that self-assessed their general health to be 'good' or 'very good'.
Table 2.1 and Table 2.1.2
2.3.2 Self-assessed general health among adults in 2018, by age and sex
In 2018, just over seven in ten adults aged 16 and over (71%) described their general health as 'good' or 'very good', while just under one in ten (9%) described it as 'bad' or 'very bad'. The 2018 figures for men and women did not vary significantly.
As in previous survey years, the association between self-assessed general health levels and age continued to be evident among adults in 2018. The proportion of adults who assessed their general health to be 'good' or 'very good' decreased with age from 85% among those aged 16-24 to 57% among those aged 75 and over. A reversal of this pattern was seen in the proportion that self-assessed their general health to be 'bad' or 'very bad', increasing from 2% among those aged 16-24 to 12% of those aged 75 and over.
Patterns of general health by age were similar for men and women.
Figure 2A, Table 2.2
Figure 2A
Percentage of adults (aged 16 and over) with 'good' or 'very good' self-reported general health, 2018, by age and sex
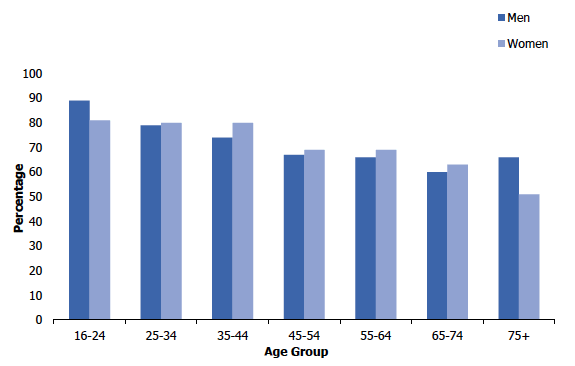
2.4 Cardiovascular Conditions And Diabetes
2.4.1 CVD and diabetes, 2018, by age and sex
Any CVD
The proportion of adults that reported having any CVD in 2018 was 16%, similar to 2017 (15%)[37]. Prevalence was the same for men and women (both 16%).
The significant association between the prevalence of CVD conditions and age reported in 2017[38] was also evident in 2018. In 2018, 4% of those aged 16-24 reported any such condition increasing across the age groups to 41% of those aged 75 and over. The same pattern was found for both men and women.
Doctor-diagnosed diabetes
In 2018, 7% of adults reported having doctor-diagnosed diabetes; this was primarily Type 2 (6% reported Type 2 and 1% reported Type 1). There was no significant difference in prevalence between men and women of doctor-diagnosed diabetes. As in 2017Error! Bookmark not defined., the prevalence of any type of doctor-diagnosed diabetes generally rose with age in 2018 (from 1% among those aged 16-24 to 16% among those aged 65-74 (13% for those aged 75 and over). There was no significant difference in the pattern by age for men and women.
Type 1 diabetes
Prevalence of Type 1 diabetes did not differ by age for men or women.
Type 2 diabetes
Men were more likely than women to have Type 2 diabetes (6% compared to 5% respectively). Prevalence of Type 2 diabetes increased with age, from <1% for those aged 16-24 to 15% among those aged 65-74 (12% for those aged 75 and over). Similar patterns by age were found for men and women.
Any CVD or diabetes
Two in ten adults reported having any CVD or doctor-diagnosed diabetes in 2018 (20%), figures were similar for men (21%) and women (20%). There was again a clear association by age with prevalence ranging from 5% among those aged 16-24 to 48% of those aged 75 and over.
The pattern by age was different for men and women. Prevalence among women was higher than among men in the 25-44 age group (12-14% for women compared to 8-9% for men) however it was lower for women than men among those aged 55 and over (24-44% for women compared to 30-54% for men).
IHD
The proportion of adults reporting an IHD diagnosis in 2018 was 5%, equal to that reported in 2017Error! Bookmark not defined.. Men were more likely than women to report an IHD (7% compared to 4% respectively).
The proportion reporting such a diagnosis also increased with age, from less than 1% among those aged 16-24 to 19% among those aged 75 and over. This pattern was evident for both men and women.
Stroke
Stroke prevalence was 3% for all adults in 2018 with similar rates for men and women (2% among men, 3% among women).
Stroke prevalence increased significantly by age (from less than 1% to 2% for those aged 16-54 to 9% among those aged 75 and over). The pattern by age differed for men and women. For women prevalence rose steadily with age (from less than 1% among those aged 16-24 to 13% among those aged 75 and over. For men there was no clear pattern by age.
IHD or stroke
In 2018, the prevalence of an IHD diagnosis and / or stroke was 7%. Prevalence was higher among men (8%) than women (7%). Prevalence was associated with age, increasing steadily from 1% or less among those aged 16-44 to 26% among those aged 75 and over.
Prevalence increased with age for both men and women, but the patterns were different. Prevalence of less than 1% was evident among men up to age 35, compared with only up to age 25 for women. The first steep increase in prevalence for men was at an earlier age (from 6% among those aged 45-54 to 14% among those aged 55-64) than for women (from 6% among those aged 55-64 to 15% among those aged 65-74).
Table 2.3
2.4.2 Trends In Cvd And Diabetes Prevalence (Age-Standardised) Since 2003, By Area Deprivation And Sex
Any CVD
The extent of inequalities in age-standardised CVD prevalence by area deprivation has varied since 2003 but with no clear pattern. In 2018, there was a higher prevalence of CVD among those living in the most deprived quintile (19%) compared with those living in the four less deprived quintiles (14-16%). The pattern by area deprivation was not significantly different for men or women.
Doctor-diagnosed diabetes
As in previous survey years[39], the age-standardised prevalence of doctor-diagnosed diabetes was higher among those living in the most deprived areas (9%) compared with those living in the least deprived areas (5%). This pattern was evident for both women and men.
IHD
The prevalence of self-reported age-standardised IHD varied significantly by area deprivation. Twice as many adults living in the most deprived areas reported an IHD diagnosis (8%) than those living in the least deprived areas (4%). A similar pattern was found for men (8% compared to 5%) and for women (7% compared to 2%). This pattern has been consistent across previous survey years.
Stroke
Stroke prevalence, for all adults and by sex, has been relatively stable since 2008. Health inequalities by deprivation area have varied in previous survey years. In 2018, there was a significance difference in stroke prevalence in the most deprived (4%) and least deprived areas (2%).
Table 2.4
2.5 Caring
2.5.1 Caring Prevalence in 2018, by age and sex
Adults
In 2018, prevalence of reported unpaid care for a family member, friend or someone else among those aged 16 and over remained at 15%. As in previous years (reported in previous SHeS reports[40]), provision of unpaid care in 2018 was higher among women (18%) than men (12%).
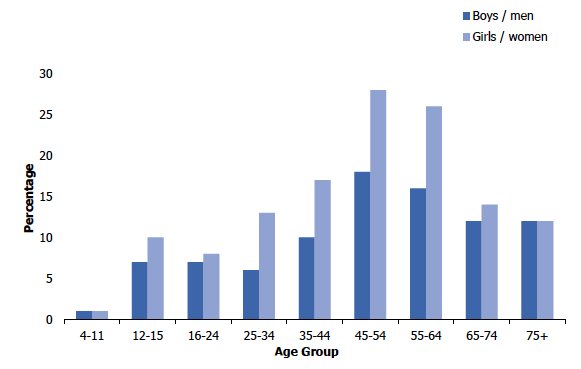
Prevalence of unpaid care varied significantly by age, increasing from 8% among those aged 16-24 to 23% among those aged 45-54 followed by a decrease to 12% of those aged 75 and over. A similar pattern by age was found for men and women.
Children
In 2018, the prevalence of unpaid care provision among children aged 4-15 was 4%, with no significant difference in prevalence between boys (3%) and girls (4%). For both sexes, the prevalence of care provision was highest amongst those aged 12-15 (9% overall, 7% boys, 10% girls).
Figure 2B, Table 2.5
Figure 2B
Prevalence of providing regular unpaid care, 2018, by age and sex
2.5.2 Caring prevalence, 2013/2014 combined – 2017/2018 combined, by age and sex
The combined survey results indicated a consistent level of caring provision prevalence among adults aged 16 and over, with rates ranging between 14-16% for adults and 3-5% for children across the time-series. There were no significant differences in prevalence across the time series between men and women or boys and girls.
Table 2.6
2.5.3 Caring prevalence in adults (age-standardised), 2017/2018 combined, by area deprivation and sex
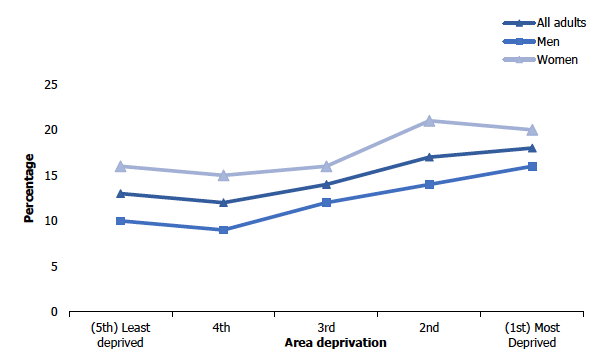
The age standardised results indicate that prevalence in the provision of care by adults varied by deprivation area with adults in the most deprived areas more likely to provide regular unpaid care than those in the least deprived areas (18% compared to 13% respectively).
A similar pattern of prevalence of caring provision by area deprivation was found for men and women.
Figure 2C, Table 2.7
Figure 2C
Caring prevalence in adults (age standardised), 2017/2018 by area deprivation and sex
2.5.4 Prevalence of caring among children 2017/2018 combined, by area deprivation and sex
The results indicated a similar pattern of increased provision of regular unpaid care among children aged 4-15 by deprivation area; with 1% prevalence in the two least deprived quintiles compared with 2-3% in the other three quintiles. A similar pattern was found for boys and girls.
Table 2.8
2.5.5 Hours spent per week by carers providing help or unpaid care among adults and children, 2017/2018 combined, by age and sex
In 2017/2018, the largest proportion of carers reported spending 19 hours or less a week providing unpaid care; around a third reported providing below 5 hours a week (32%) and around another third reported caring for between 5 and 19 hours a week (34%). The proportion providing care for 50 hours or more was 15%.
Age variations in the reported hours spent caring remained evident. A higher proportion of carers aged 65 and over reported providing 50 hours or more of unpaid care each week (22%) than younger age groups (14% of those aged 45-64, 12% of those aged 16-44 and 2% of those aged 4-15). A higher proportion of children than adults reported that they provided less than 5 hours a week of care (54% among those aged 4-15 compared to 29-35% among adults).
A higher proportion of female than male carers aged 65 and over reported providing 50 hours or more of care a week (26% compared to 16% respectively). Girls were more likely than boys to provide care for more than 34 hours per week, (7% compared to less than 1% respectively).
Table 2.9
2.5.6 WEMWBS mean score 2017/2018 combined, (age-standardised), by hours spent each week providing help or unpaid care
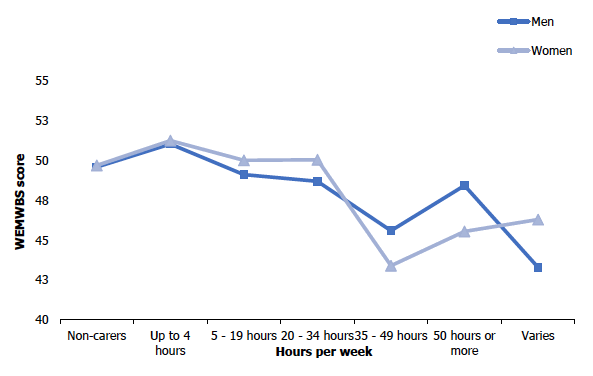
Mean WEMWBS scores varied significantly with the number of hours spent each week providing help or unpaid care, with wellbeing generally lower among those spending higher numbers of hours caring. Higher WEMWBS mean scores were found among those who provided care for 34 hours or less (49.4-51.2) as well as for non-carers (49.7) than for those who those who provided care for 35-49 hours a week (44.4) and those who provided care for 50 hours or more a week (46.6). WEMWBS mean scores indicated higher wellbeing among those that spent 4 hours or less per week providing care compared with non-carers (51.2 and 49.7 respectively). Those who reported that the number of hours per week they spent caring was variable also had relatively low mental wellbeing with a mean WEMWBS score of 45.3.
The patterns of mental wellbeing by hours spent caring did not vary significantly between men and women.
Figure 2D, Table 2.10
Figure 2D
Hours spent each week providing help or unpaid care, 2017/18 combined, among adults, by sex and WEMWBS mean scores
2.5.7 Support received by carers in 2017/2018 combined, by hours spent caring per week
Around seven in ten unpaid carers aged 4 and over reported receiving no help or support (69%), with those who provided unpaid care for less than 35 hours per week more likely to receive no help or support than those who provided 35 or more hours of unpaid care per week (75% compared to 40% respectively).' The most frequently cited form of support was help from family, friends and neighbours (19%), those who provided 35 hours or more per week were almost twice as likely to receive this type of support than those who provided less than 35 hours per week (30% compared to 17%).
The second most common form of support reported was the carer's allowance. Of those eligible to receive carer's allowance (those who provided 35 hours or more of unpaid care per week) 31% reported that they were in receipt of the benefit.
Advice and information, a personal assistant/support worker/community nurse or home help, short breaks or respite, practical support or counselling or emotional support were each received by 6% or less of all carers.
Less than 1% of young carers reported receiving help from teachers at school or social activities and support.
Table 2.11
References And Notes
1. Long-term conditions collaborative: Making the Connections – Food For Thought (2010), Edinburgh: Scottish Government, 2010. Available from: https://www.webarchive.org.uk/wayback/archive/20180518153228/http://www.gov.scot/Publications/2010/08/04125659/15
2. Auditor General (2018). NHS in Scotland. [Online] Available from: http://www.audit-scotland.gov.uk/report/nhs-in-scotland-2018
3. See: www.gov.scot/Topics/Health/Services/Long-Term-Conditions
4. Heart Disease Improvement Plan. Edinburgh: Scottish Government, 2014. Available from: https://www2.gov.scot/Resource/0045/00458289.pdf
5. Stroke Improvement Plan, Edinburgh: Scottish Government, 2014. Available from: https://www.gov.scot/publications/stroke-improvement-plan/
6. Information Services Division (2019). Scottish Heart Disease Statistics. Available from: https://www.isdscotland.org/Health-Topics/Heart-Disease/Publications/2019-01-29/2019-01-29-Heart-Disease-Summary.pdf
8. Information Services Division (2019). Scottish Heart Disease Statistics. Available from: https://www.isdscotland.org/Health-Topics/Heart-Disease/Publications/2019-01-29/2019-01-29-Heart-Disease-Summary.pdf
10. Scottish Diabetes Data Group, NHS Scotland (2017). Scottish Diabetes Survey 2017. [Online] Available from: http://www.diabetesinscotland.org.uk/Publications/SDS%202017.pdf
11. Scottish Diabetes Data Group, NHS Scotland (2017). Scottish Diabetes Survey 2017. [Online] Available from: http://www.diabetesinscotland.org.uk/Publications/SDS%202017.pdf
12. Scottish Diabetes Data Group, NHS Scotland (2017). Scottish Diabetes Survey 2017. [Online] Available from: http://www.diabetesinscotland.org.uk/Publications/SDS%202017.pdf
13. See: https://carers.org/country/carers-trust-scotland
14. Scotland's Carers (2015), Edinburgh, Scottish Government, 2015. Available from: https://www.gov.scot/publications/scotlands-carers/pages/3/
15. Carers (Scotland) Act 2016: national implementation plan 2016-2019, Edinburgh, Scottish Government, 2017. Available from: https://www.gov.scot/publications/carers-scotland-act-2016-national-implementation-plan-2016-2019/
16. Scotland's Carers (2015), Edinburgh, Scottish Government, 2015. Available from: https://www.gov.scot/publications/scotlands-carers/pages/3/
17. A National Clinical Strategy for Scotland, Edinburgh: ScottisGovernment, 2016. Available from: https://www.gov.scot/publications/national-clinical-strategy-scotland/
18. Health and Social Care Delivery Plan, Edinburgh: Scottish Government, 2016. Available from: https://www2.gov.scot/Resource/0051/00511950.pdf
19. Practising Realistic Medicine, Edinburgh, Scottish Government, 2018.Available from:https://www.gov.scot/publications/practising-realistic-medicine/
20. Realising Realistic Medicine, Edinburgh: Scottish Government, 2017. Available from: https://www2.gov.scot/Resource/0051/00514513.pdf
21. Public Health Priorities for Scotland, Edinburgh: Scottish Government/COSLA, 2018. Available from: https://www.gov.scot/publications/scotlands-public-health-priorities/pages/9/
22. Gaun Yersel: The Self-Management Strategy for Long-Term Conditions in Scotland, Edinburgh: Scottish Government, 2008.Available from: https://www2.gov.scot/Resource/0042/00422988.pdf
23. Improving the Health and Wellbeing of People with Long Term Conditions in Scotland: A National Action Plan (2009). Edinburgh: Scottish Government. Available from: https://www.gov.scot/Publications/2009/12/03112054/0
24. Heart Disease Improvement Plan (2014). Edinburgh: Scottish Government, 2014. Available from: https://www.gov.scot/Publications/2014/08/5434/0
25. Stroke Improvement Plan (2014). Edinburgh: Scottish Government, 2014. Available from: https://www.gov.scot/Publications/2014/08/9114/0
26. Diabetes Improvement Plan (2014). Edinburgh: Scottish Government, 2014. Available from: www.gov.scot/Publications/2014/11/6742
27. See: https://nationalperformance.gov.scot/
28. A Healthier Future: Scotland's Diet and Healthy Weight Delivery Plan (2018) Edinburgh: Scottish Government, 2018. Available from: https://www.gov.scot/publications/healthier-future-scotlands-diet-healthy-weight-delivery-plan/
29. A more active Scotland: Scotland's Physical Activity Delivery Plan. Edinburgh: Scottish Government. 2018. Available from: http://www.gov.scot/Resource/0053/00537494.pdf
30. Carers (Scotland) Act 2016, Edinburgh, Scottish Government, 2016. Available from:https://www.gov.scot/publications/carers-scotland-act-2016-statutory-guidance/
31. Carers' charter, Scottish Government, 2018. Available from: www.gov.scot/publications/carers-charter/pages/0
32. Carers (Scotland) Act 2016: Implementation Plan 2018-2020, Edinburgh, Scottish Government, 2017. Available from: https://www.gov.scot/publications/carers-scotland-act-2016-national-implementation-plan-2016-2019/
35. See: https://www2.gov.scot/scottishhealthsurvey
36. Diabetes and high blood pressure are not included in the definition of 'any CVD condition' as they are risk factors for CVD.
37. Feng, Q. (2018). Chapter 1: General Health, Long-Term Conditions And Cardiovascular Conditions. McLean, J., Christie, S., and Gray, L. (eds). The Scottish Health Survey – 2017 edition: volume 1: main report. Edinburgh: Scottish Government. Available from: https://www.gov.scot/publications/scottish-health-survey-2017-volume-1-main-report/pages/6/
38. Feng, Q. (2018). Chapter 1: General Health, Long-Term Conditions And Cardiovascular Conditions. McLean, J., Christie, S., and Gray, L. (eds). The Scottish Health Survey – 2017 edition: volume 1: main report. Edinburgh: Scottish Government. Available from: https://www.gov.scot/publications/scottish-health-survey-2017-volume-1-main-report/pages/6/
39. Bardsley, D. (2017). Chapter 7: General Health And Caring. McLean, J., Christie, S., Hinchcliffe, S. and Gray, L. (eds). The Scottish Health Survey 2016: volume 1: main report. Edinburgh Scottish Government. Available from: https://www.gov.scot/publications/scottish-health-survey-2016-volume-1-main-report/pages/60/
40. Bardsley, D. (2017). Chapter 7: General Health And Caring. McLean, J., Christie, S., Hinchcliffe, S. and Gray, L. (eds). The Scottish Health Survey 2016: volume 1: main report. Edinburgh: Scottish Government. Available from: https://www.gov.scot/publications/scottish-health-survey-2016-volume-1-main-report/pages/60/
Table list
Table 2.1 Self-assessed general health, adults and children, 2008 to 2018
Table 2.2 Adult self-assessed general health, 2018, by age and sex
Table 2.3 Any CVD, doctor-diagnosed diabetes Type 1 or 2, any CVD or diabetes, IHD, stroke, IHD or stroke, 2018, by age and sex
Table 2.4 Any CVD, doctor-diagnosed diabetes, IHD, stroke, IHD or stroke, (age-standardised), 2003 to 2018, by area deprivation and sex
Table 2.5 Caring prevalence, 2018 by age and sex
Table 2.6 Caring prevalence, 2013/2014, 2015/2016 and 2017/2018, by age and sex
Table 2.7 Caring prevalence in adults, (age-standardised), 2017/2018 combined, by area deprivation and sex
Table 2.8 Caring prevalence in children, 2017/2018 combined, by area deprivation and sex
Table 2.9 Hours spent each week by carers providing help or unpaid care, 2017/2018 combined, by age and sex
Table 2.10 WEMWBS mean scores (age-standardised), 2017/2018 combined, by hours spent each week providing help or unpaid care
Table 2.11 Support received by carers, 2017/2018 combined, by hours spent caring per week