Scottish Health Survey 2018: main report - revised 2020
An amended version of the Scottish Health Survey 2018 main report.
Chapter 7 Obesity
Summary
In 2018, two thirds (65%) of adults were overweight, including 28% who were obese, with both these trends remaining stable since 2008.
- There has been a small upward trend in mean BMI among adults over time, rising from 27.1 kg/m2 in 2003 to 27.7 kg/m2 in 2018, with no significant difference between the mean BMI of men and women.
33% of adults were a healthy weight (a BMI of 18.5 to less than 25 kg/m2).
BMI increased significantly with age for both men and women.

A greater proportion of men were overweight or obese than women.

A greater proportion of women than men were in the healthy weight category.

Mental wellbeing (measured by WEMWBS mean score) was lowest among those within the morbidly obese BMI range.
- Prevalence of children at risk of obesity has remained relatively stable in 2018 at 16%.
- The proportion of children at risk of obesity significantly increased with age, from 11% of those aged 2-6 to 21% of those aged 12-15. These proportions were the same for both boys and girls.
70% of children (aged 2-15) were of healthy weight.
The proportion of children in the healthy weight range decreased by age; this pattern was more pronounced for girls.
7 Obesity
Isla Dougall
7.1 Introduction
Worldwide obesity has nearly tripled since 1975. In 2016, 39% of adults aged 18 and over across the world were overweight and 13% were obese and the rate of obesity among children and young people aged 5-19 was over four times higher in 2016 (18%) than it was in 1975 (4%)[1]. Obesity levels in Scotland are among the highest of the OECD countries[2].
Being overweight or obese is defined in adults as having a body mass index (BMI) of 25 kg/m² or greater and evidence shows that this may impair health[3]. The impacts can be profound, affecting our health and our ability to lead happy and fulfilling lives. Raised BMI is a major risk factor for non-communicable diseases such as cardiovascular disease, type 2 diabetes, musculoskeletal disorders and some types of cancers[4]. Obesity is the second biggest preventable cause of cancer[5], behind only smoking, and research suggests a reciprocal link between obesity and mental health problems such as depression and anxiety[6],[7],[8]. There is also evidence of a link between overweight and obesity in midlife and dementia in late life[9],[10],[11].
Evidence also shows that younger generations in the UK are becoming obese at earlier ages and staying obese longer[12]. The most recent NHS statistics show that 22.4% of primary one pupils in Scotland are at risk of overweight or obesity, this rate has remained fairly constant since 2001/02[13]. Children at risk of obesity are likely to stay obese into adulthood and become more likely to suffer health problems. In addition to increased future risk, children at risk of obesity can experience an increased risk of fractures, hypertension, type 2 diabetes, asthma as well as negative psychological effects including lower wellbeing and self-esteem during the childhood years[14],[15],[16].
Once considered a problem within high-income countries, overweight and obesity are now also on the rise in low and middle-income countries. Globally, there are more people who are obese than are underweight, and most of the world's population live in countries where overweight and obesity kills more people than underweight. In Scotland there are substantial inequalities in the risk of overweight and obesity between children living in the least and most deprived areas in Scotland – and evidence to suggest that this gap is widening[17]. Latest figures show that the 'proportion of Primary 1 children at risk of overweight or obesity has gone up in the most deprived areas but gone down in the least deprived areas' demonstrating a strong and increasing association between deprivation and obesity[18].
The cost to the health service in Scotland of overweight and obesity combined is estimated to be between £363 and £600 million (most of these costs are incurred because of associated conditions such as cardiovascular disease and type 2 diabetes, rather than direct costs of treating or managing overweight and obesity)[19].The latest estimate, in 2015, of the total (direct and indirect) costs of overweight and obesity in Scotland, including labour market related costs such as lost productivity, have been put at £0.9-4.6 billion[20].
With considerable individual, social, and economic consequences, obesity continues to be a key priority and a major challenge for the Scottish government, the NHS and other public services.
7.1.1 Policy background
In July last year, the Scottish Government published A Healthier Future – Scotland's Diet and Healthy Weight Delivery Plan[21]. The plan sets out a vision for everyone in Scotland to eat well and have a healthy weight. More specifically, it also sets an ambition to halve childhood obesity by 2030, and to significantly reduce diet-related health inequalities. The delivery plan contains a broad range of measures to transform the food environment to make it easier for people to make healthier choices and targeted action to support children and families most at risk of health inequalities.
The Scottish Government is taking a joined up approach to addressing public health challenges and in June 2018, along with the Convention of Scottish Local Authorities' (COSLA), published Scotland's Public Health Priorities which aim to focus efforts to improve the health of the population. Included in these is a priority to create 'a Scotland where we eat well, have a healthy weight and are physically active'. This priority underpins the approach set out in the delivery plan. Sitting alongside the diet and healthy weight delivery plan, the Scottish Government also published a complementary Physical Activity Delivery Plan[22] in July 2018. This recognises the importance of both eating well and being active in promoting and maintaining healthy weight.
The Diet and Healthy Weight Delivery Plan is framed around 5 key outcomes:
- Children have the best start in life – they eat well and have a healthy weight.
- The food environment supports healthier choices.
- People have access to effective weight management services.
- Leaders across all sectors promote healthy weight and diet.
- Diet-related health inequalities are reduced.
Reducing the prevalence of overweight and obesity also contributes to the new National Performance Framework outcome 'we are healthy and active'[23]. There is a related indicator to monitor the proportion of healthy weight adults and children of which SHeS is the official source of data.
The 2018-19 Programme for Government (PfG) Delivering for Today, Investing in Tomorrow[24] reaffirmed the commitment to halve childhood obesity and proposals to reduce the public health harm associated with poor diet by restricting the promotion and marketing of food high in fat, sugar or salt with little or no nutritional value. The consultation ran from 2 October 2018 to 9 January 2019[25].
7.1.2 Reporting on obesity in the Scottish Health Survey (SHeS)
The anthropometric measures presented in this chapter focus on measurements relevant to adult and child obesity. Height, weight and waist measurements have been collected during the survey interview every year since its inception in 1995. SHeS is one of a small number of surveys that collects height, weight and waist measures rather than using self-reported measures, which are known to be less accurate[26],[27]. Height and weight are used to calculate Body Mass Index (BMI), the primary measure of obesity used in the SHeS series. Adults' and children's trends in BMI are examined in this chapter. In addition, adult BMI are explored in relation to mental wellbeing.
Supplementary tables are available on the Scottish Government SHeS website[28].
7.1.3 Comparability with other UK statistics
Adult obesity is defined consistently in the Scottish Health Survey and the other health surveys within the UK using BMI classifications. Height and weight measurements are self-reported in the National Survey for Wales and are therefore not directly comparable with equivalent statistics in Scotland, England and Northern Ireland, where direct measurements are taken. Sampling methodologies differ between the surveys. Of the four UK health surveys, the Scottish Health Survey and Health Survey for England are the most closely aligned.
7.2 Methods and Definitions
7.2.1 Methods
Height
Height was measured using a portable stadiometer with a sliding head plate, base plate and four connecting rods marked with a metric measuring scale. Participants were asked to remove shoes. One measurement was taken, with the participant stretching to the maximum height and the head positioned in the Frankfort plane[29]. If the reading was between two millimetres it was recorded to the nearest even millimetre. No measurement was taken from participants who were pregnant, aged under 2, or unsteady on their feet.
Weight
Weight was measured using either Seca or Tanita electronic scales, both of which use a digital display. Participants were asked to remove shoes and any bulky clothing. A single measurement was recorded to the nearest 100g. A weight measurement was not collected from participants who were pregnant, aged under 2 years, or unsteady on their feet. Due to the scale limits, when using a Tanita scale those who weighed more than 130 kg were asked for an estimate of their weight, with estimates required for those weighing more than 200 kg if Seca scales were being used. These estimated weights were included in the analysis presented in this chapter.
In the analysis of height and weight, data from those who were considered by the interviewer to have unreliable measurements, for example those who had excessive clothing on, were excluded.
7.2.2. Definitions
Body Mass Index (BMI)
Body Mass Index (BMI) is a widely accepted measure that allows for differences in weight due to height. It is defined as weight (kg)/square of height (m2). This has been used as a measure of obesity in SHeS since its inception in 1995. BMI was calculated from valid measures collected by the interviewer.
Adult BMI classification
Based on their BMI, adult participants were classified into the following groups based on the World Health Organisation (WHO) classification[30]:
| BMI (kg/m2) | Description |
|---|---|
| Less than 18.5 | Underweight |
| 18.5 to less than 25 | Normal |
| 25 to less than 30 | Overweight, excluding obese |
| 30 to less than 40 | Obese, excluding morbidly obese |
| 40+ | Morbidly obese |
In this chapter, both mean BMI and prevalence for the five categories outlined in the table above are presented for adults. Although obesity has the greatest ill-health and mortality consequences, overweight is also a major public health concern, not least because overweight people are at high risk of becoming obese. Being underweight can also have negative health consequences.
Child BMI classification
BMI is defined for children in the same way as it is for adults: weight (kg)/square of height (m2). The International Obesity Task Force concluded that BMI is a reasonable measure of adiposity in children[31]and it is the key measure of overweight and obesity for children used in the SHeS series.
Despite the relatively wide acceptance of the use of BMI as an adiposity indicator, the establishment of an agreed specific obesity and overweight classification system for children and young people remains challenging. Constant changes in body composition during growth mean that the relationship between weight-for-height and adiposity during childhood and adolescence is age-dependent, and this relationship is further complicated by both ethnicity and gender[32].
The classification of children's BMI used in this chapter, set out below, has been derived from BMI percentiles of the UK 1990 reference curves[33],[34] (referred to as the national BMI percentiles classification); these have been used in each SHeS to date. The national BMI percentiles classification has been shown to be reasonably sensitive (i.e. not classifying obese children as non-obese) and specific (i.e. not classifying non-obese children as obese)[35],[36]. SIGN recommends that these reference curves and thresholds should be used for population surveillance in Scotland[37].The 85th / 95th percentile cut-off points are commonly accepted thresholds used to analyse overweight and obesity in children. These thresholds have previously been used to describe childhood overweight and obesity prevalence trends in the UK[38],[39],[40],[41].
| Percentile cut-off | Description |
|---|---|
| At or below 2nd percentile | At risk of underweight |
| Above 2nd percentile and below 85th percentile | Healthy weight |
| At or above 85th percentile and below 95th percentile | At risk of overweight |
| At or above 95th percentile | At risk of obesity |
SHeS uses a method developed by ISD Scotland to plot the exact ages of the children in the sample against the reference population data[42].While children's exact age was used to calculate the BMI grouping prevalence rates (based on the interview date and the date of birth), results are presented using grouped ages based on age at last birthday.
As noted in the introduction to this chapter, one of the Scottish Government's national indicators relates to healthy weight in both children and adults, defined as neither underweight nor overweight or obese[43]. The presented data for children have been categorised to show the total proportions that are: healthy weight, at risk of overweight, at risk of obesity, and at risk of underweight.
Warwick-Edinburgh Mental Wellbeing Scale (WEMWBS)
Wellbeing is measured using the WEMWBS questionnaire. It has 14 items designed to assess: positive affect (optimism, cheerfulness, relaxation) and satisfying interpersonal relationships and positive functioning (energy, clear thinking, self-acceptance, personal development, mastery and autonomy)[44]. The scale uses positively worded statements with a five-item scale ranging from '1 - none of the time' to '5 - all of the time'. The lowest score possible is therefore 14 and the highest score possible is 70; the tables present mean scores.
The scale was not designed to identify individuals with exceptionally high or low levels of positive mental health so cut off points have not been developed[45].
WEMWBS is used to monitor the National Indicator 'mental wellbeing'[46] and the mean score for parents of children aged 15 years and under on WEMWBS is included in the mental health indicator set for children[47].
7.3 Adult Overweight And Obesity Prevalence
7.3.1 Trends in overweight including obesity prevalence since 2003
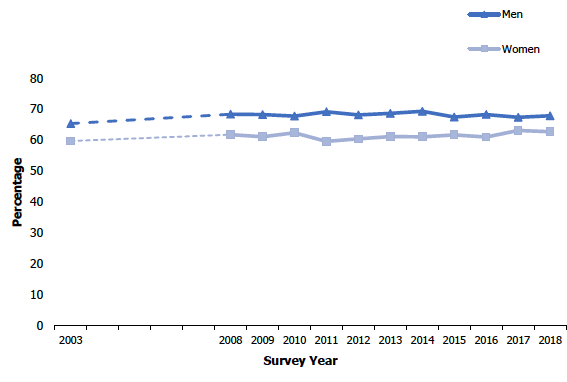
In 2018, 65% of adults were overweight or obese (BMI of 25 kg/m² or greater). Following an increase between 2003 and 2008 (62% to 65%), the prevalence of overweight including obesity has remained stable since, fluctuating between 64% and 65%.
Although prevalence of overweight including obesity has remained stable in both men and women since 2008, men have had consistently higher prevalence compared with women. Since 2008, the proportion of overweight or obese men has fluctuated between 67-69%, compared with 60-63% of women. As in previous years[48], in 2018 prevalence of overweight or obesity was significantly higher among men compared with women (68% and 63%, respectively).
Figure 7A, Table 7.1
Figure 7A
Prevalence of overweight including obesity (BMI 25 kg/m² and over) among adults aged 16 and over, 2003 to 2018
7.3.2 Trends in obesity prevalence since 2003
The prevalence of obesity including morbid obesity (BMI of 30 kg/m² or greater) was 28% among adults in 2018. This pattern remains relatively unchanged since 2008, fluctuating between 27% and 29%.
There was no significant difference between the proportion of men that were obese or morbidly obese compared with the proportion of women. Among men, 27% were obese or morbidly obese in 2018, (fluctuating between 26% and 29% since 2008). Among women, 30% were obese or morbidly obese in 2018 (fluctuating between 27% and 30% since 2008).
Prevalence of morbid obesity has followed a similar pattern – remaining stable among both men and women since 2003 (2-4%). In 2018, significantly more women (5%) were morbidly obese compared with men (2%).
Table 7.1
7.3.3 Trends in mean adult BMI since 2003
There has been a small but significant upward trend in mean BMI among adults over time, rising from 27.1 in 2003 to 27.7 in 2018. There was no significant difference between the mean BMI of men (27.6) compared with women (27.8) in 2018. Further, there has been no change in these figures since 2017.
Table 7.1
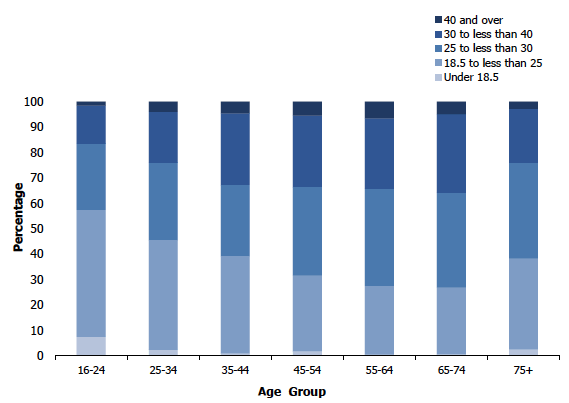
7.3.4 Adult BMI in 2018, by age and sex
In 2018, 33% of adults were in the healthy weight category (BMI of 18.5 to less than 25 kg/m2). Women were significantly more likely than men to be within the healthy weight range (35% compared with 30% respectively).
As in previous years[49], prevalence of overweight including obesity varied significantly with age. The percentage of those overweight including obese (BMI of 25 kg/m² or over), increased with age from 45% of those aged 16-24 to 76% of those aged 65-74, before decreasing to 68% among those aged 75 and over. A similar pattern was observed in both men and women. Prevalence of overweight including obesity was lowest among those aged 16-24 (47% for men, 43% for women) increasing to highest prevalence among those aged 45-54 for men (80%) and among those aged 55-74 for women (72 - 73%).
The prevalence of obesity (BMI of 30 kg/m² or more) also varied significantly by age. Of those aged 16-24, 14% were obese, increasing to 36% of those aged 45-54 before decreasing to 32% of those aged 55-64. Prevalence increased to 36% among those aged 65-74 before decreasing to 24% of those aged 75 and over.
This pattern of results was primarily driven by men, with prevalence increasing from 12% of those aged 16-24 to 39% of those aged 45-54, before decreasing to 30% of those aged 55-64. Prevalence then increased to 36% of those aged 65-74 before dropping to 23% of those aged 75 and over. Among women, prevalence of obesity increased more steadily between those aged 16-74 (from 17% of those aged 16-24 to 36% of those aged 65-74) with prevalence only decreasing in the oldest age group (24% of those aged 75 and over).
Mean BMI varied significantly with age increasing from 25.1 kg/m2 among those aged 16-24 to 28.5 to 28.9 kg/m2 among those aged 45-74, before decreasing to 27.4 kg/m2 among those aged 75 and over. Patterns of mean BMI by age did not differ significantly between men and women.
Figure 7B and 7C, Table 7.2
Figure 7B
BMI scores among men aged 16 and over, 2018, by age
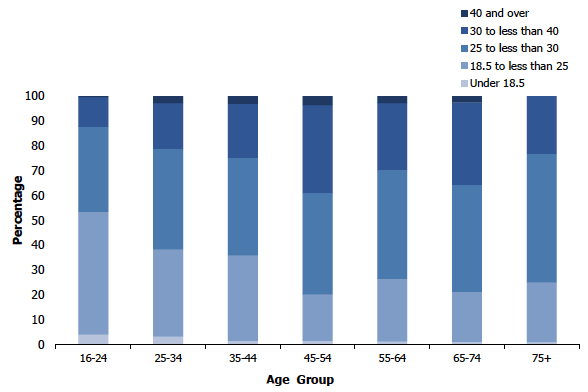
Figure 7C
BMI scores among women aged 16 and over, 2018, by age
7.4 Child Overweight And Obesity Prevalence
7.4.1 Trends in child healthy weight prevalence since 1998
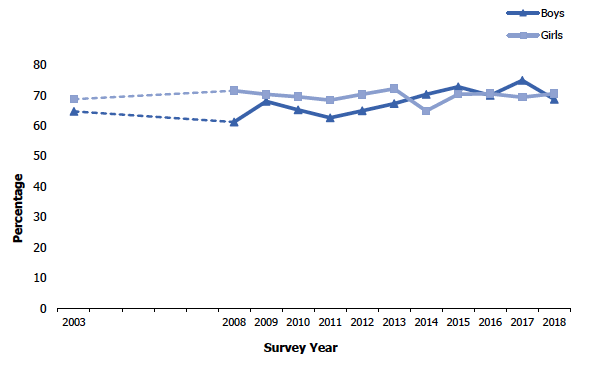
In 2018, 70% of children (aged 2-15) were in the healthy weight range (BMI above the 2nd percentile or below the 85th percentile). This was not significantly different to the proportion reported in 2017 (72%). The proportion of healthy-weight children has fluctuated since the beginning of the timeseries in 1998, with the lowest prevalence occurring in 2011 (65%) and the highest in 2015 and 2017 (both 72%).
Since 1998, the pattern over time has been different for boys and girls. Since the beginning of the timeseries, there have been relatively large fluctuations in the proportion of boys within the healthy weight range (61-75%).
In contrast, the proportion of girls within the healthy weight range has remained relatively stable since the beginning of the time series in 1998 (68-72%; 2014 was an exception at 65%). In 2018, 71% of girls were a healthy weight; this was not significantly different to 2017 (69%).
Figure 7D, Table 7.3
Figure 7D
Proportion of children within the healthy weight range, 2003 to 2018
Prevalence of children at risk of obesity has remained relatively stable in 2018 at 16%. Prevalence in 2017 was the lowest since the time series began, at 13%. However, the steady decline in the proportion of boys at risk of obesity (from 20% in 2012 to 12% in 2017) that had driven overall prevalence has not continued, with a significant rise in 2018 to 17%.
7.4.2 Child BMI categories in 2018, by age and sex
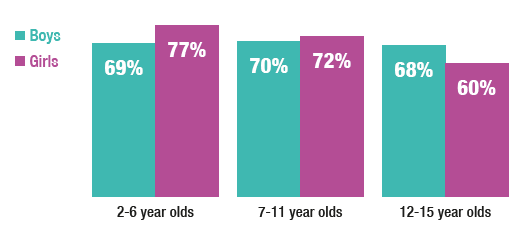
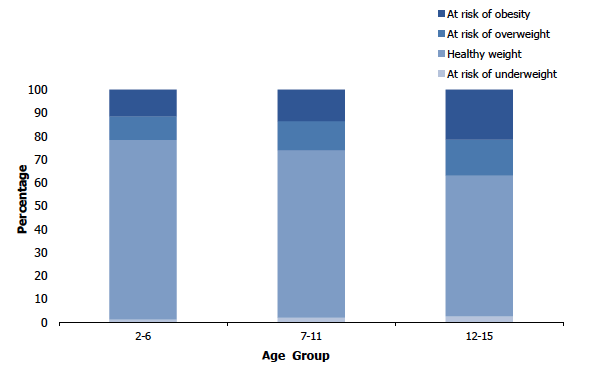
The proportion of children in the healthy weight range decreased significantly by age, from 73% of children aged 2-6 to 64% of children aged 12-15. This pattern was largely driven by girls, for whom prevalence of healthy weight decreased significantly from 77% for those aged 2-6, to 60% for those aged 12-15.
The proportion of children at risk of overweight changed little between those aged 2-6 (15%) and those aged 12-15 (12%). The pattern by age was however significantly different between boys and girls. Among boys, the percentage at risk of overweight significantly decreased from 19% of those aged 2-6 to 9-10% of those aged 7 and over. The opposite pattern was seen among girls, whereby 10% of those aged 2-6 were at risk of overweight, gradually increasing to 15% of girls aged 12-15, however this change was not statistically significant.
The proportion of children at risk of obesity significantly increased with age, from 11% of those ages 2-6 to 21% of those aged 12-15. These proportions were the same among both boys and girls.
Figure 7E and 7F, Table 7.4
Figure 7E
BMI categories among boys aged 2-15, 2018, by age
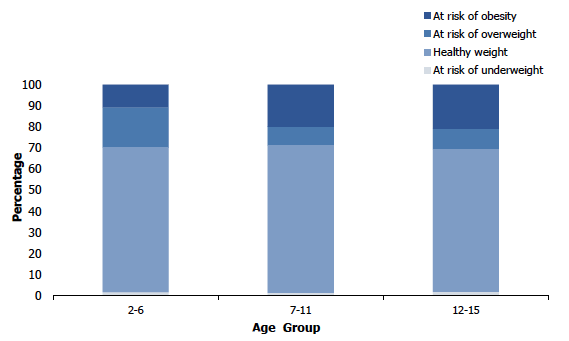
Figure 7F
BMI categories among girls aged 2-15, 2018, by age
7.4 Overweight, Obesity And Wellbeing
7.4.1 Adult WEMWBS mean scores (age-standardised), 2017/2018 combined, by BMI categories and sex
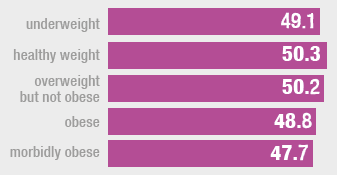
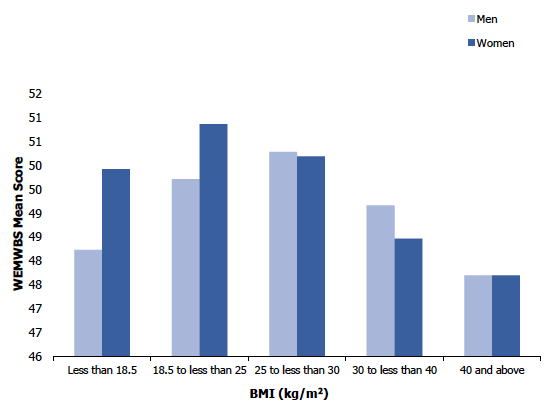
WEMWBS mean scores varied significantly by BMI category. The highest mean WEMWBS score was among adults in the 'healthy weight' or 'overweight but not obese' categories (BMI of 18.5 to less than 25 and BMI of 25 to less than 30 kg/m2) at 50.3 and 50.2 respectively. The lowest mean WEMWBS score (47.7) was found among those in the 'morbidly obese' category (BMI of 40 kg/m2 and above). The second lowest WEMWBS mean score (48.8) was found for those in the obese category (with a BMI of 30 to less than 40kg/m2). There was not a statistical difference in the pattern of WEMWBS mean score by BMI category between men and women.
Figure 7G, Table 7.5
Figure 7G
Adult WEMWBS mean scores, 2017/18 combined, by BMI and sex
References and notes
1. World Health Organisation (2018). Fact Sheet Obesity and Overweight. Available at: www.who.int/mediacentre/factsheets/fs311/en/index.html
3. Moody A (2013). Chapter 10: Adult anthropemetric measures, overweight and obesity. In: Craig R, Mindell J (eds). Health Survey for England 2012. Volume 1: Health, social care and lifestyles. Leeds: Health and Social Care Information Centre. Available from: http://content.digital.nhs.uk/catalogue/PUB13218/HSE2012-Ch10-Adult-BMI.pdf
4. World Health Organisation (2018). Fact Sheet Obesity and Overweight. Available at: www.who.int/mediacentre/factsheets/fs311/en/index.html
5. Katrina F Brown et al (2018). The fraction of cancer attributable to modifiable risk factors in England, Wales, Scotland, Northern Ireland, and the United Kingdom in 2015 http://www.nature.com/articles/s41416-018-0029-6
6. Floriana, S, Luppino, MD, Leonore, M, de Wit, MS, Paul, F, Bouvy, MD et al. (2010). Overweight, obesity and depression: A systematic review and meta-analysis of longitudinal studies. Arch Gen Psychiatry. 2010;67(3):220-229. doi:10.1001/archgenpsychiatry.2010.2
7. Gatineau, M, Dent, M (2011). Obesity and mental health. National Obesity Observatory. SCIE Social Care Online. Available at: https://www.scie-socialcareonline.org.uk/obesity-and-mental-health/r/a11G00000017trJIAQ
8. Rivenes, AC, Harvey, SB, Mykletun, A (2009). The relationship between abnormal fat, obesity and common mental disorders: Results from the HUNT study. Journal of Psychosomatic Research, 66(4): 269-275.
9 Anstey, KJ, Cherbuin, N, Budge, M, and Young, J (2011). Body mass index in midlife and late-life as a risk factor for dementia: a meta-analysis of prospective studies. Obesity Reviews; 12(5):
426-37.
10 Xu, WL, Atti, AR, Gatz, M, Pedersen, NL, Johansson, B, and Fratiglioni, L. Midlife overweight and obesity increase late-life dementia risk: a population-based twin study. Neurology; 76(18): 1568-
74.
11 Loef, M and Walach, H. Midlife obesity and dementia: meta-analysis and dementia: meta-analysis and adjusted forecast of dementia prevalence in the United States and China. Obesity; 21(1): 51-5.
12. Johnson, W, Li, L, Kuh, D, Hardy, R (2015) How Has the Age-Related Process of Overweight or Obesity Development Changed over Time? Coordinated Analyses of Individual Participant Data from Five United Kingdom Birth Cohorts. PLoS Med 12(5)
13. Body Mass Index of Primary 1 Children in Scotland. School Year 2017/18. 11 December 2018. A National Statistics Publication for Scotland. Information Services Division. Available at: https://www.isdscotland.org/Health-Topics/Child-Health/Publications/2018-12-11/2018-12-11-P1-BMI-Statistics-Publication-Summary.pdf
14. Oude Luttikhuis, H, Baur, L, Jansen, H, Shrewsbury, VA, O'Malley, C, Stolk, RP and Summerbell, CD (2009). Interventions for treating obesity in children. Cochrane Database of Systematic Reviews; Issue 1. Art. No.: CD001872
15. Waters, E, de Silva-Sanigorski, A, Hall, BJ, Brown, T, Campbell, KJ, Gao, Y, Armstrong, R, Prosser, L, Summerbell, CD (2011). Interventions for preventing obesity in children. Cochrane Database of Systematic Reviews; Issue 12. Art. No.: CD001871.
16. Sahoo, K, Sahoo, B, Choudhury, AK, Sofi, NY, Kumar, R, Bhadoria, AS (2015). Childhood obesity: causes and consequences. J Family Med Prim Care. 2015 Apr-Jun; 4(2): 187–192. doi: 10.4103/2249-4863.154628
17. Body Mass Index of Primary 1 Children in Scotland. School Year 2017/18. 11 December 2018. A National Statistics Publication for Scotland. Information Services Division. Available at: https://www.isdscotland.org/Health-Topics/Child-Health/Publications/2018-12-11/2018-12-11-P1-BMI-Statistics-Publication-Summary.pdf
18. Body Mass Index of Primary 1 Children in Scotland. School Year 2017/18. 11 December 2018. A National Statistics Publication for Scotland. Information Services Division. Available at: https://www.isdscotland.org/Health-Topics/Child-Health/Publications/2018-12-11/2018-12-11-P1-BMI-Statistics-Publication-Summary.pdf
19. SPICe Briefing – Obesity in Scotland. January 2015. Edinburgh: Scottish Parliament, 2015. Available from: www.scottish.parliament.uk/ResearchBriefingsAndFactSheets/S4/SB_15-01_Obesity_in_Scotland.pdf
20. SPICe Briefing – Obesity in Scotland. January 2015. Edinburgh: Scottish Parliament, 2015. Available from: www.scottish.parliament.uk/ResearchBriefingsAndFactSheets/S4/SB_15-01_Obesity_in_Scotland.pdf
21. A Healthier Future – Scotland's Diet and Healthy Weight Delivery Plan. Edinburgh, Scottish Government. 2018.
Available from: https://www.gov.scot/Resource/0053/00537708.pdf
22. A more active Scotland: Scotland's Physical Activity Delivery Plan. Edinburgh: Scottish Government. 2018. http://www.gov.scot/Resource/0053/00537494.pdf
23. See: http://nationalperformance.gov.scot/
24. Delivering for Today, Investing in Tomorrow: The Government's Programme for Scotland 2018-19. Edinburgh: Scottish Government (2018). Available from: https://www.gov.scot/publications/delivering-today-investing-tomorrow-governments-programme-scotland-2018-19/
25. See: Ref: https://news.gov.scot/news/improving-scotlands-diet
26. Keith, SW, Fontaine, KR, Pajewski, NM, Metha,, T and Allison, D (2011). Use of self-reported height and weight biases the body mass index-mortality association. International Journal of Obesity; 35:401‑8.
27. Merrill, RM and Richardson, JS (2009). Validity of Self-Reported Height, Weight and Body Mass Index: Findings from the National Health and Nutrition Examination Survey, 2001-2006. Preventing Chronic Disease; 6(4): 61-10.
28. See: https://www.gov.scot/publications/scottish-health-survey-2018-volume-1-main-report/
29. The Frankfort Plane is an imaginary line passing through the external ear canal and across the top of the lower bone of the eye socket, immediately under the eye. Participants' heads are positioned with the Frankfort Plane in a horizontal position when height is measured using a stadiometer as a means of ensuring that, as far as possible, the measurements taken are standardised.
30. These cut-offs differ to those used in the previous surveys. In 1995 and 1998 the normal weight range was defined as 20-25 kg/m2, in 2003 it was changed to 18.5-25 kg/m2. From 2008 onwards the ranges are defined as set out below. This brings the definition in line with WHO recommendations. The impact of the change of definition is very marginal as very few people have a BMI measurement that is exactly 18.5, 25, 30 or 40 kg/m2.
| 2003 | 2008 onwards | |
|---|---|---|
| Underweight | 18.5 or under | Less than 18.5 |
| Normal weight | Over 18.5 –25 | 18.5 to less than 25 |
| Overweight | Over 25 – 30 | 25 to less than 30 |
| Obese | Over 30 – 40 | 30 to less than 40 |
| Morbidly obese | Over 40 | 40+ |
31. Bellizzi, MC and Dietz, WH (1999). Workshop on childhood obesity: summary of the discussion. American Journal of Clinical Nutrition; 70: 173-175
32. Daniels, SR, Khoury, PR and Morrison, JA (1997). The utility of body mass index as a measure of body fatness in children and adolescents: Differences by race and gender. Pediatrics: 99: 804-807.
33. Cole, T, Freeman, JV and Preece, MA (1990). Body mass index reference curves for the UK. Archives of Disease in Childhood; 73: 25-29.
34. Cole, T, Freeman, JV and Preece, MA (1998). British 1990 growth reference centiles for weight, height, body mass index and head circumference fitted by maximum penalised likelihood. Statistics in Medicine; 17: 407-429.
35. Reilly, JJ (2002). Assessment of childhood obesity: National reference data or international approach? Obesity Research; 10: 838-840.
36. Reilly, JJ, Wilson, ML, Summerbell, CD, and Wilson, DC (2002). Obesity: diagnosis, prevention, and treatment; evidence based answers to common questions. Archives of Disease in Childhood; 86: 392-395.
37. SIGN (2010). Scottish Intercollegiate Guidelines Network Management of Obesity – A National Clinical Guideline. SIGN guideline no. 115. Available from: http://www.sign.ac.uk/assets/sign115.pdf
38. Jotangia, D, Moody, A, Stamatakis, E and Wardle, H (2005). Obesity Among Children Under 11. London: Department of Health in collaboration with the Health and Social Care Information Centre. Available from: http://dera.ioe.ac.uk/5841/1/dh_065358.pdf
39. Reilly, J, Dorosty, A, and Emmett, P (1999). Prevalence of overweight and obesity in British children: cohort study. British Medical Journal; 319: 1039.
40. Bundred, P, Kitciner, D and Buchan, I (2001). Prevalence of overweight and obese children between 1989 and 1998: population based series of cross sectional studies. British Medical Journal; 322: 1-4.
41. Rudolf, MCJ, Sahota, P, Barth, JH, and Walker, J (2001). Increasing prevalence of obesity in primary school children: cohort study. British Medical Journal; 322: 1094-1095.
42. This method has been developed by ISD Scotland, full details of the procedure are available on request from the Scottish Government Scottish Health Survey Team.
43. See: www.gov.scot/About/Performance/scotPerforms/indicator/healthyweight
44. Further information about WEMWBS is available here: www.healthscotland.com/scotlands-health/population/Measuring-positive-mental-health.aspx
45. Stewart-Brown, S and Janmohamed, K (2008). Warwick-Edinburgh Mental Well-being Scale (WEMWBS). User Guide Version 1. Warwick and Edinburgh: University of Warwick and NHS Health Scotland.Available from: http://www.healthscotland.com/documents/2702.aspx
46. See: http://nationalperformance.gov.scot/
47. NHS Health Scotland (2012) Establishing a core set of national, sustainable mental health indicators for children and young people in Scotland: Final Report. Available from: http://www.healthscotland.com/uploads/documents/18753C&YP%20Mental%20Health%20Indicators%20FINAL%20Report.pdf
48. Bardsley, D. (2018). Chapter 8: Obesity. McLean, J., Christie, S., and Gray, L. (eds). The Scottish Health Survey – 2017 edition: volume 1: main report. Edinburgh: Scottish Government. Available from: https://www.gov.scot/publications/scottish-health-survey-2017-volume-1-main-report/pages/96/
49. Bardsley, D. (2018). Chapter 8: Obesity. McLean, J., Christie, S., and Gray, L. (eds). The Scottish Health Survey – 2017 edition: volume 1: main report. Edinburgh: Scottish Government. Available from: https://www.gov.scot/publications/scottish-health-survey-2017-volume-1-main-report/pages/96/
Table list
Table 7.1 Mean adult BMI, prevalence of overweight and obesity, 2003 to 2018
Table 7.2 Adult BMI, 2018, by age and sex
Table 7.3 Proportion of children with BMI within the healthy range, at risk of overweight and at risk of obesity, 1998 to 2018
Table 7.4 Children's BMI, 2018, by age and sex
Table 7.5 Adult WEMWBS mean scores (age-standardised), 2017/2018 combined, by BMI categories and sex