Scottish Health Survey 2018: main report - revised 2020
An amended version of the Scottish Health Survey 2018 main report.
Chapter 8 Respiratory
Summary
Prevalence of selfreported asthma diagnoses among adults increased from 13% in 2003 to 16% in 2012 and has remained stable since (17% in 2018).
In 2018, 8% of all children aged 0 to 15 were reported to be diagnosed with asthma by a doctor – the lowest level to date.
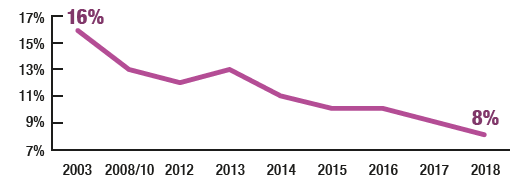
There was not a significant difference in this prevalence between boys (9%) and girls (7%).
- The percentage of adults aged 16 and over who had wheezed in the last 12 months was 16% in 2018. This has not changed significantly since 2003.
- The proportion of children who were reported as having wheezed in the last 12 months was at its lowest in 2018 (10%) compared with between 12% and 14% between 2003 and 2017.
- In 2018, 4% of adults reported having chronic obstructive pulmonary disease (COPD), continuing the stable level since 2008.
- COPD was four times higher among adults living in the most deprived areas (8%) compared with those living in the least deprived areas (2%).
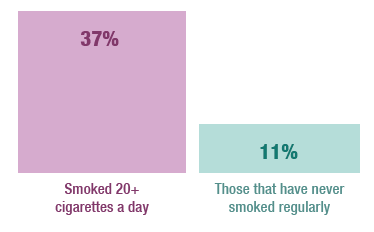
- The prevalence of doctor-diagnosed COPD was thirteen times higher among smokers who smoked 20 or more cigarettes a day (13%) compared with among those who have never smoked regularly (1%).
Difference in asthma diagnosis and wheezing between the most deprived and least deprived areas in 2018
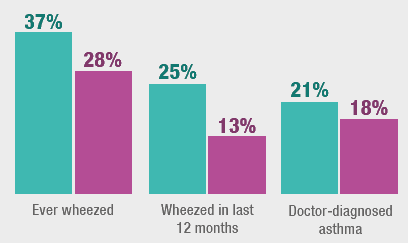
Adults who smoked 20 or more cigarettes a day were more than three times more likely to have wheezed in the last 12 months than those that have never smoked regularly.
72% of adults diagnosed with COPD reported having received treatment for this, with older adults more likely to have done so.
63% of those aged 16-64
80% of those aged 65 and over
8 Respiratory Health
Chi Keng Cheong
8 Introduction
Long-term respiratory conditions, such as asthma and chronic obstructive pulmonary disease (COPD), represent a significant challenge for the individuals that live with them and for health services in Scotland. These conditions affect the flow of air in and out of the lungs and both are currently incurable, with uncertainty and debate around whether asthma is over- or underdiagnosed[1],[2],[3].
The UK has one of the world's highest rates of asthma[4],[5], an illness characterised by variable and recurring symptoms of breathlessness, wheezing, coughing and chest tightness. It is estimated that around 368,000 people in Scotland are currently receiving treatment for asthma, a fifth of whom are children[6]. For the majority of those diagnosed, asthma can be managed in such a way that it has a minimal impact on day-to-day life. However, as a long-term condition, commitment is required from the patient as well as the healthcare sector to manage it effectively and, where possible, limit asthma attacks which may cause lasting damage to the body[7].
The reasons for the high prevalence of asthma in the UK are not clear, however, risk factors identified include environmental (house dust mites, pollen, animals, specific foods, viral infections, moulds, fungi, environmental tobacco smoke and air pollutants) and genetic disposition, obesity and lifestyle/stage (diet, drug use, caesarean sections and breastfeeding)[8]. Occupational exposure also accounts for around one in ten cases of adult onset asthma[9]. Evidence on the financial burden of asthma in Scotland is limited, however, it is estimated to be in the region of £97.5 million per year[10].
The increased prevalence of COPD means that it is estimated that it will be the third most frequent cause of mortality worldwide by 2030. Not only does this strengthen the importance of monitoring and, where possible, tackling the causes and symptoms of this condition, the ageing population and additional complication of older COPD patients being more likely to have other long-term conditions presents a further challenge in managing this condition[11].
The associations of long term conditions like COPD with deprivation, lifestyle risk factors and wider social health determinants are of importance in Scotland given the country's health inequalities[12].While situational factors (such as air quality and working conditions) and genetics can have an impact, smoking is the main cause of COPD with up to 25% of long-term smokers estimated to develop COPD and up to four-fifths of those with the condition having smoked/ continuing to smoke[13]. The risk is increased for women, who tend to develop the condition with lower exposure to smoke than men[14].
Estimates suggest that the number of people with a COPD diagnosis in Scotland will rise from 100,000 (in 2011) to 120,000 by 2030[15]. While smoking rates are expected to decline[16], the impact of this will take some time be reflected in levels of COPD incidence[17]. Coupled with longer life expectancy, the costs of treating COPD in Scotland is expected to increase from £182million (in 2016) to £207 million a year by 2030[18], placing a substantial financial burden on healthcare provision in Scotland for the foreseeable future.
8.1.1 Policy background
A key area of focus in relation to long-term health conditions, including respiratory conditions, is on empowering patients to take control of their care and the management of their long-term condition(s)[19]. Gaun Yersel is a strategy developed on behalf of the Scottish Government which aims to embed self-management across the country, improving the lives of those living with long-term conditions and giving them the support they need to make informed decisions about their own health[20], [21].
Alongside this focus are policies aimed at, or that include, respiratory conditions. One of the Scottish Government's National Performance Framework National Outcomes is for people in Scotland to 'live longer, healthier lives'[22], which includes a National Performance Indicator to 'reduce premature mortality' (deaths from all causes in those aged under 75)[23].
Quality Prescribing for Respiratory: A Guide for Improvement[24] is a healthcare professionals guide to the delivery of high- quality prescribing of medicine but also the recommendation of non-medicinal, in some cases preventative, approaches, such as smoking cessation, a healthy diet and being physically active, wherever possible. The Cross Party Group for Lung Health is a forum in which MSPs from all political parties, along with representatives from a range of relevant organisations, meet to discuss issues relating to respiratory health and strategies to help improve provision for those with such conditions[25].
COPD is a major cause of death in Scotland, hence COPD prevention, early diagnosis and better symptom management should contribute to reducing premature mortality.Within the Scottish Government National Indicators, health risk behaviours linked to respiratory disease, including smoking, harmful drinking, low physical activity and obesity, are monitored against an outcome of reducing the percentage of adults exhibiting two or more of these behaviours[26].
Healthcare Improvement Scotland produced clinical standards for COPD in 2010[27]. A number of clinical guidelines have been produced for respiratory conditions including the Scottish Intercollegiate Guidelines Network guideline on the management of asthma ((SIGN) Guideline 153 - published September 2016[28] alongside booklets explaining these recommendations to patients[29].
In 2016, the Smoking Prohibition (Children in Motor Vehicles) (Scotland) Bill was introduced, making it illegal from the 5th December 2016 to smoke in a car or vehicle whilst carrying those aged under 18 – an offence that could carry a £100 fixed penalty[30].
8.1.2 Reporting on respiratory conditions and symptoms in the Scottish Health Survey (SHeS)
The Scottish Health Survey (SHeS) is a valuable source of information on the self-reported prevalence of asthma and COPD in Scotland. It collects information about respiratory symptoms such as wheezing and breathlessness, symptoms often experienced by people without a diagnosed respiratory condition. It also provides valuable information on the patterning of these conditions and symptoms across different population groups.
This chapter presents data on adults' self-reported doctor-diagnosed asthma, COPD prevalence, and respiratory symptoms (wheezing). Children's asthma diagnoses and wheezing symptoms are also reported. Information on whether people with COPD receive treatment and the treatment type is also reported.
Area deprivation data for respiratory health are presented using Scottish index of Multiple Deprivation (SIMD) quintiles. To ensure that the comparisons presented are not confounded by the different age profiles of the quintiles, the data have been age-standardised. Readers should refer to the Glossary at the end of this Volume for a detailed description of SIMD and age-standardisation.
Supplementary tables providing further breakdowns are available on the Scottish Government SHeS website[31].
8.2 Methods
8.2.1 Asthma and COPD diagnoses
Participants (including parents of children aged 0-12, and children themselves aged 13-15) were asked if a doctor had ever told them they had asthma. This question was asked in the 1998, 2003, 2008 and 2010 surveys, and has been included every year since 2012. Each year since 2008, adult participants have also been asked if they had ever had COPD, chronic bronchitis or emphysema and, if so, whether a doctor had told them they had one of these conditions. Those who reported doctor-diagnosed COPD were also asked what treatment or advice they had received. No objective measures were used to confirm these reported diagnoses.
8.2.2 Respiratory symptoms
Questions on respiratory symptoms were included in the 1995-2003 surveys, and in all even years since 2008. The symptoms covered were: phlegm production, breathlessness and wheezing or whistling in the chest. Breathlessness was classified as grade 2 if it occurred when hurrying on level ground or walking up a slight hill, or grade 3 (the more severe form) if it occurred when walking with other people of the same age on level ground. The impact of wheezing and whistling symptoms on sleep and people's daily activities was also measured. The Medical Research Council Respiratory Symptom Questionnaire was used to collect some of this information[32].
8.2.3 Treatment for COPD
Questions on whether people are currently receiving any treatment or advice for COPD, chronic bronchitis or emphysema and, if so, what type of treatment were introduced in SHeS in 2008 and have been included in the survey every year since.
8.3 Self-Reported Doctor-Diagnosed Asthma and Self-Reported Wheezing
8.3.1 Trends in self-reported doctor-diagnosed asthma and wheezing prevalence in adults since 2003
The prevalence of doctor-diagnosed asthma in adults aged 16 and over in 2018 (17%) has not changed significantly since 2012 (16%), although this has increased significantly since 2003 (13%).
The percentage of adults aged 16 and over who had wheezed in the last 12 months was 16% in 2018 having remained relatively stable since the start of the time series in 2003 (fluctuating between 15% and 18%).
In 2018, 29% of adults aged 16 and over reported ever having wheezed which is consistent with previous survey years, the rate having fluctuated between 28% and 31% since 2012.
Figure 8A, Table 8.1
Figure 8A
Prevalence of self-reported doctor-diagnosed asthma
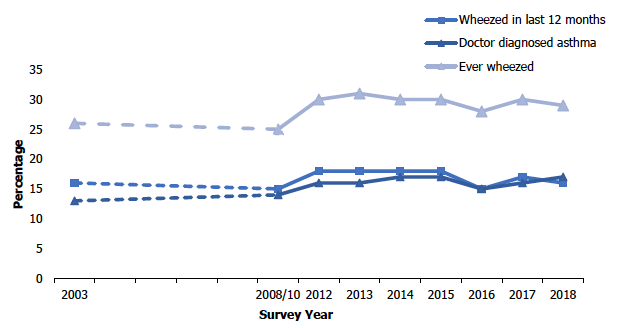
8.3.2 Trends in self-reported doctor-diagnosed asthma and wheezing prevalence in children since 2003
At 8% in 2018, the proportion of children aged 0 to 15 who were reported as having doctor-diagnosed asthma was at its lowest since the beginning of the time series (having declined by eight percentage points from 16% in 2003). The trend of reduced prevalence from 2003 to 2018 was similar among boys (20% to 9%) and girls (12% to 7%) with no significant difference in prevalence of self-reported doctor-diagnosed asthma in 2018 between boys (9%) and girls (7%).
The proportion of children who were reported as having wheezed in the last 12 months was also at its lowest in the time series at 10% in 2018. In previous survey years prevalence has fluctuated between 12% and 14%.
Overall, the proportion of children who were reported as having ever wheezed was at its lowest in 2018 (19%) with no clear pattern of change in previous survey years (prevalence fluctuated between 22% and 25%). Unlike in previous years[33], there was not a significant difference in prevalence of having ever wheezed between boys and girls in 2018 (20% for boys and 17% for girls).
Figure 8A, Table 8.1
8.3.3 Self-reported doctor-diagnosed asthma and wheezing prevalence in adults in 2018, by age and sex
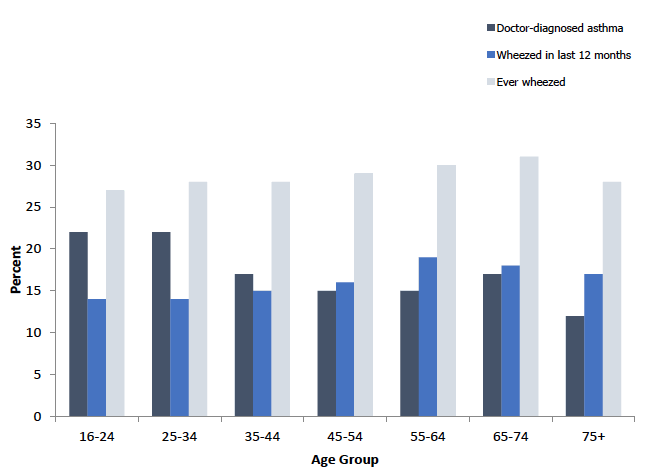
In 2018, the prevalence of self-reported doctor-diagnosed asthma among adults differed significantly by age. The highest prevalence was among those aged 16-34 at 22% and the lowest was among those aged 75 and over at 12%. Similar patterns were found for men and women.
There was no significant difference in the proportion of adults having wheezed in the last 12 months according to age. Prevalence ranged from 14-19% across age groups with no clear pattern by age for men or women.
The proportion of adults in 2018 that reported ever having wheezed fluctuated between 27% and 31% with no clear pattern by age.
Figure 8B, Table 8.2
Figure 8B
Prevalence of self-reported doctor-diagnosed asthma and wheezing, 2018, by age group
8.3.4 Self-reported doctor-diagnosed asthma and wheezing prevalence (age-standardised) in 2018, by area deprivation and sex
In 2018, prevalence of self-reported asthma and wheezing were both significantly linked with deprivation.
Adults living in the most deprived quintile had a higher prevalence (21%) of doctor-diagnosed asthma than those in the other four quintiles (14-18%). A similar pattern was found for both men and women.
The proportion of adults who reported wheezing in the last 12 months increased significantly with deprivation level; from 13% of adults (14% for men, 12% for women) living in the least deprived quintile compared with 25% of those living in the most deprived quintile (23% for men, 26% for women).
Those living in the most deprived quintile were more likely to report having ever wheezed (37%) than those living in the other four deprivation quintiles (25% to 29%). The pattern by deprivation varied between men and women. For women, there was a gradual increase in prevalence of having ever wheezed from 24% among those in the least deprived quintile to 39% in the most deprived quintile. There was no clear pattern in prevalence by deprivation for men.
Table 8.3
8.3.5 Self-reported doctor-diagnosed asthma and wheezing prevalence (age-standardised) in 2018, by smoking status and sex
As in previous years[34] smoking status among adults was significantly associated with prevalence of self-reported doctor-diagnosed asthma and wheezing.
The proportions of adults who had ever wheezed or wheezed in the last 12 months were higher among current smokers than non-smokers or occasional smokers and those who used to smoke. Around a tenth (11%) of non-smokers or occasional smokers had wheezed in the last 12 months, the proportion increased to more than a third (37%) among those who smoked 20 or more cigarettes a day. The pattern was similar for men and women.
Similarly, double the proportion of adults who smoked 20 or more cigarettes per day (44%) reported having ever wheezed in their lifetime compared with around a fifth (22%) of non-smokers or occasional smokers. Similar patterns were found for men and women.
Prevalence of self-reported doctor-diagnosed asthma was significantly higher for those that smoke less than 20 a day than for non-smokers or those that only smoked occasionally.
Table 8.4
8.4 Doctor-Diagnosed COPD
8.4.1 Trends in doctor-diagnosed COPD prevalence in adults since 2008
The prevalence of self-reported doctor-diagnosed COPD in adults was 4% in 2018, continuing the stable trend since 2008 of 4% for every year with the exceptions of 2009 (3%) and 2010 (5%).
There have been no significant differences between the prevalence rates of self-reported doctor-diagnosed COPD for men and women during the timeseries.
Table 8.5
8.4.2 Doctor-diagnosed COPD prevalence in 2018, by age and sex
Similar to previous years[35], the prevalence of self-reported doctor-diagnosed COPD in 2018 was higher within older adults than younger adults. Prevalence increased from 1% among those aged 16-44 to 11% among those aged 65-74. Prevalence did not vary between the sexes and the same pattern by age was observed in both men and women.
Table 8.6
8.4.3 Doctor-diagnosed COPD prevalence (age-standardised) in 2018, by area deprivation and sex
As in previous years[36], self-reported doctor-diagnosed COPD was significantly associated with area deprivation in 2018, with the lowest prevalence (2%) among adults living in the least deprived areas and the highest prevalence (8%) among those living in the most deprived areas. This association was observed among both men and women.
Table 8.7
8.4.4 Doctor-diagnosed COPD prevalence (age-standardised) in 2018, by smoking status and sex
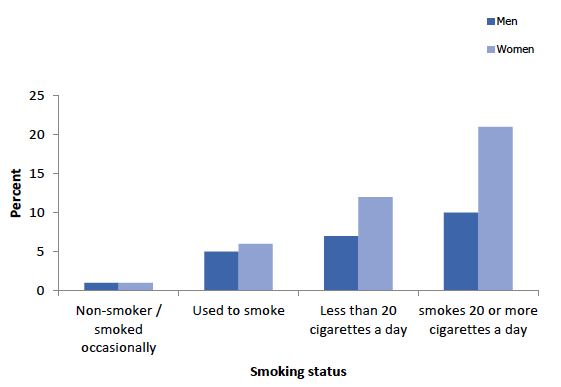
Prevalence of self-reported doctor-diagnosed COPD was lower among non-smokers or occasional smokers (1%) than among those who used to smoke (5%) and increased with the number of cigarettes smoked a day (9% for those who smoked less than 20 cigarettes a day to 13% among those who smoked more than 20 cigarettes a day).
A similar pattern for the prevalence of COPD and smoking status were evident among men and women. However higher proportions of female regular smokers reported doctor-diagnosed COPD than male regular smokers (12% to 21% for female smokers compared to 7% to 10% of male smokers).
Figure 8C, Table 8.8
Figure 8C
Prevalence of self-reported doctor-diagnosed COPD (age-standardised), 2018, by smoking status and sex
8.4.5 COPD treatment and type of treatment in 2015-2018 combined, by age and sex
Among all adults who self-reported doctor-diagnosed COPD in 2018, 72% reported having received treatment for their condition, with similar rates observed among men (71%) and women (73%). This varied with age, with those aged 65 and over more likely to be receiving treatment for their condition than those aged between 16-64 (80% compared with 63% respectively). A similar pattern by age was similar for men and women.
Taking medication (tablets / inhalers)
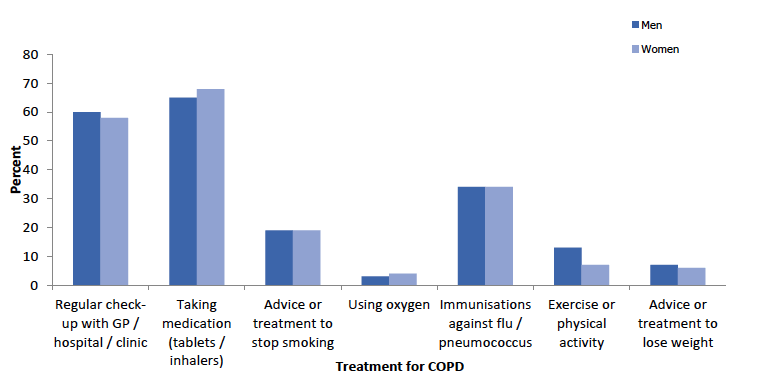
Taking medication including tablets or inhalers was the most common form of treatment for COPD reported (67%) with similar findings for men and women (65% and 68% respectively). Adults aged 65 and over were more likely to report this as a treatment than those aged 16-64 (74% compared with 59% respectively). This pattern by age was similar for men and women.
Regular check-up with GP / hospital / clinic
Regular check-ups with medical professionals was the second most common type of COPD treatment reported (59%) with similar rates for men (60%) and women (58%). Around two thirds (64%) of adults aged 65 and over had received this form of treatment compared with just over a half (53%) of those aged 16-64. This pattern by age was found for men and women.
Immunisations against flu / pneumococcus
Immunisations against flu and/or pneumococcus was the third most common treatment for COPD reported (34%). The rate did not differ significantly across the two age groups for men or women.
Advice or treatment to stop smoking
Just under a fifth (19%) of those who reported a COPD diagnosis had received advice or treatment to stop smoking as a COPD treatment. This varied significantly by age (23% of adults aged 16-64 compared with 15% of those aged 65 and above). A similar pattern by age was found for men and women. This contrasts with most of the other forms of treatment whereby receipt of the treatment was higher among the older age group than the younger age group.
Exercise or physical activity
A tenth of adults who reported doctor-diagnosed COPD reported engaging in exercise or physical activity as a treatment with similar figures for both age groups (10% among those aged 16-64 and 9% among those aged 65 and over). Men who had reported a COPD diagnosis were more likely to engage in exercise or physical activity as a form of treatment for COPD than women (13% compared with 7% respectively).
Advice / treatment to lose weight
Advice or treatment to lose weight for COPD was reported by 6% of those with a COPD diagnosis. No significant differences were found across the two age groups (16-64 and those aged 65 and over) or between men and women.
Using oxygen
Using oxygen was the least common treatment for COPD reported. Prevalence of this treatment among adults with COPD was 3% with no significant differences across the two age groups or between men and women.
Figure 8D, Table 8.9
Figure 8D
COPD treatment and type of treatment, 2015-2018 combined, by sex
References and notes
1. See: www.scotpho.org.uk/health-wellbeing-and-disease/asthma/key-points
3. See: https://www.nhs.uk/news/medical-practice/is-asthma-being-overdiagnosed/
4. To, T, Stanojevic, S, Moores, G, Gershon A S , Bateman, E, Cruz, A A, Boulet L-P (2012). Global asthma prevalence in adults: findings from the cross-sectional world health survey https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3353191/
5. Beasley, R (1998). Worldwide variation in prevalence of symptoms of asthma, allergic rhinoconjunctivitis and atopic eczema: ISAAC. The Lancet; 351(9111): 1225-32
6. See: https://www.asthma.org.uk/scotland
7. See: https://www.asthma.org.uk/advice/manage-your-asthma/
8. See: https://www.scotpho.org.uk/health-wellbeing-and-disease/asthma/risk-factors/
9. See: https://www.asthma.org.uk/advice/understanding-asthma/types/occupational-asthma/
10. Mukherjee, M, Stoddart, A, Gupta, RP, Nwaru, BI, Farr, A, Heaven, M, Fitzsimmons, D, Bandyopadhyay, A, Aftab, C, Simpson, CR, Lyons, RA, Fischbacher, C, Dibben, C, Shields, MD,Phillips, CJ, Strachan, DP, Davies, GA, McKinstry, B and Sheikh, A (2016). The epidemiology, healthcare and societal burden and costs of asthma in the UK and its member nations: analyses of standalone and linked national databases. BMC Med; 14(1):113.
11. Chronic Obstructive Pulmonary Disease (COPD): best practice guide. Edinburgh, Scottish Government, 2017. Available from: https://www.gov.scot/publications/copd-best-practice-guide/
13. See: https://www.chss.org.uk/chest-information-and-support/common-chest-conditions/copd/
15. See: https://www.ed.ac.uk/usher/news-events/news-2016/copd-care-costs-to-exceed-ps2-5bn
16. See: https://www.ed.ac.uk/usher/news-events/news-2016/copd-care-costs-to-exceed-ps2-5bn
18. See: https://www.ed.ac.uk/usher/news-events/news-2016/copd-care-costs-to-exceed-ps2-5bn
19. See: http://www.gov.scot/Topics/Health/Support-Social-Care/Self-Management
20. Gaun Yersel: The Self Management Strategy for Scotland. Edinburgh, Scottish Government, 2008. Available from: https://www2.gov.scot/Resource/0042/00422988.pdf
21. Realising Realistic Medicine, Edinburgh: Scottish Government (2017). Available from: https://www.gov.scot/binaries/content/documents/govscot/publications/progress-report/2017/02/chief-medical-officer-scotland-annual-report-2015-16-realising-realistic-9781786526731/documents/00514513-pdf/00514513-pdf/govscot%3Adocument/00514513.pdf
22. See: https://nationalperformance.gov.scot/
23. See: https://nationalperformance.gov.scot/measuring-progress/national-indicator-performance
24. Quality Prescribing for Respiratory: A Guide for Improvement 2018-2021. Edinburgh: NHS Scotland and the Scottish Government, 2018. Available from: https://www.therapeutics.scot.nhs.uk/wp-content/uploads/2018/03/Strategy-Respiratory-Quality-Prescribing-for-Respiratory-2018.pdf
25. See https://www.parliament.scot/msps/lung-health.aspx
26. See: https://nationalperformance.gov.scot/measuring-progress/national-indicator-performance
27. Clinical Standards for Chronic Obstructive Pulmonary Disease Services. Edinburgh: NHS Quality Improvement Scotland, 2010. Available from: www.healthcareimprovementscotland.org/our_work/long_term_conditions/copd_implementation/copd_clinical_standards.aspx
28. See: http://www.sign.ac.uk/sign-153-british-guideline-on-the-management-of-asthma.html
29. McLean, S., Hoogendoorn, M., Hoogenveen, R T., Feenstra, T L., Wild S., Simpson C R., Rutten-van Mölken M & Sheikh, A (2016) Projecting the COPD population and costs in England and Scotland: 2011 to 2030. Scientific Reports. Vol 6, No 31893.
30. See: https://news.gov.scot/news/smoking-in-cars-with-children
31. See: https://www2.gov.scot/scottishhealthsurvey
32. Prior to 2012 a fuller version of the MRC Respiratory Symptoms Questionnaire was included in the 1995-2003 and 2008 and 2010 surveys, alongside questions about wheezing and whistling in the chest that were added to the survey in 1998 as part of the asthma module. To reduce duplication and participant burden, from 2012 onwards the MRC Questionnaire items on wheezing were cut (the questions on phlegm and breathlessness were retained).
33. Rooney, K.. (2018). Chapter 10: Respiratory Health. McLean, J. and Christie, S (eds). The Scottish Health Survey – 2016 edition: volume 1: main report. Edinburgh: Scottish Government. Available from: https://www.gov.scot/publications/scottish-health-survey-2016-volume-1-main-report/pages/6/
34. Rooney, K.. (2018). Chapter 10: Respiratory Health. McLean, J. and Christie, S (eds). The Scottish Health Survey – 2016 edition: volume 1: main report. Edinburgh: Scottish Government. Available from: https://www.gov.scot/publications/scottish-health-survey-2016-volume-1-main-report/pages/6/
35. Rooney, K.. (2018). Chapter 10: Respiratory Health. McLean, J. and Christie, S (eds). The Scottish Health Survey – 2016 edition: volume 1: main report. Edinburgh: Scottish Government. Available from: https://www.gov.scot/publications/scottish-health-survey-2016-volume-1-main-report/pages/6/
36. Rooney, K.. (2018). Chapter 10: Respiratory Health. McLean, J. and Christie, S (eds). The Scottish Health Survey – 2016 edition: volume 1: main report. Edinburgh: Scottish Government. Available from: https://www.gov.scot/publications/scottish-health-survey-2016-volume-1-main-report/pages/6/
Table list
Table 8.1 Doctor-diagnosed asthma, wheezed in last 12 months, and ever wheezed, 2003 to 2018, by age and sex
Table 8.2 Doctor-diagnosed asthma, wheezed in last 12 months, and ever wheezed, 2018, by age and sex
Table 8.3 Doctor-diagnosed asthma, wheezed in last 12 months, and ever wheezed, (age standardised), 2018, by area deprivation and sex
Table 8.4 Doctor-diagnosed asthma, wheezed in last 12 months, and ever wheezed, (age standardised), 2018, by smoking status and sex
Table 8.5 Doctor-diagnosed COPD, 2008 to 2018
Table 8.6 Doctor-diagnosed COPD, 2018, by age and sex
Table 8.7 Doctor-diagnosed COPD, (age-standardised), 2018, by area deprivation and sex
Table 8.8 Doctor-diagnosed COPD, (age-standardised), 2018, by smoking status and sex
Table 8.9 COPD treatment and type of treatment, 2015 to 2018 combined, by age and sex