Scottish Health Survey 2018: main report - revised 2020
An amended version of the Scottish Health Survey 2018 main report.
Chapter 1 Mental Health and Wellbeing
Summary
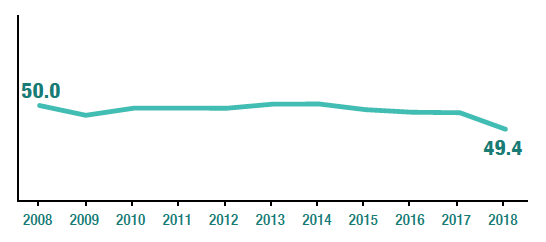
In 2018, the WEMWBS mean score (measuring mental wellbeing) for adults was 49.4, not significantly different to 2017 but the lowest since the time series began in 2008.
- The lowest WEMWBS mean scores among all adults were for men aged 35-44 (47.2) and men aged 45-54 (47.6); the lowest WEMWBS mean score among women was for those aged 16-24 at 48.2.
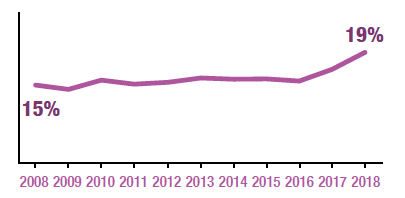
In 2018, 19% of adults exhibited signs of a possible psychiatric disorder (GHQ-12 score of four or more) the highest in the time series.
The percentage of adults with a GHQ-12 score of four or more significantly decreased with age from 24% among those aged 16-24, to 13% among those aged 75 and above.
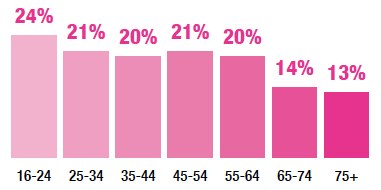
The highest proportions of a GHQ-12 score of four or more were found among women aged 16-24 and 55-64; the highest proportion of men with a GHQ-12 score of four or more was found among those aged 45-54.
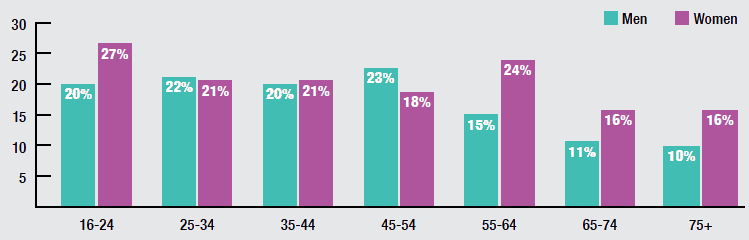
Mental health and wellbeing continued to be clearly linked to deprivation.
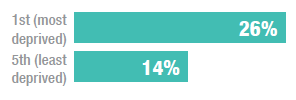
Percentage of adults with a GHQ-12 score of 4 or more (indicative of a possible psychiatric disorder)
Mean WEMWBS scores (measuring mental wellbeing) for adults

1 Mental Health And Wellbeing
Isla Dougall
1.1 Introduction
Mental health is a major determinant of overall health which has increasing international recognition[1],[2]. Mental wellbeing is defined by the World Health Organization as a state of well-being in which every individual realises their own potential, can cope with the stresses of life, can work productively, and is able to make a contribution to their community[3]. Positive mental wellbeing encourages better quality of life overall, healthier lifestyles, better physical health and improved recovery from illness, better social relationships, and higher educational attainment[4]. As such all public services have a role to play in supporting the mental health and wellbeing of Scotland's population from Local Government services to primary care and education providers as well as specialist mental health services[5].
One in three people are estimated to be affected by mental health problems in Scotland in any one year[6]. Globally, both depression and anxiety are more prevalent among women than men[7], however, rates of suicide remain consistently higher for men than for women around the world[8]. Given the evidence that mental ill health in adolescence increases the risk of subsequent mental ill health later in life[9], investing in the mental wellbeing of young people is key to the prevention of mental illness.
Poor mental health, including mental disorder, has a considerable impact on individuals, their families and the wider community[10]. Mental disorders often co-exist with other diseases, including cancers and cardiovascular disease, diabetes, respiratory illnesses and HIV/AIDS[11]. People with severe mental disorders have a life-expectancy 15-20 years shorter than the general population[12] with most of those premature deaths being due to physical health conditions[13]. Many of the risk factors covered in this report, such as obesity, excessive alcohol consumption and low levels of physical activity, are common to both mental disorders and other non-communicable diseases, with outcomes being critically interdependent. Mental health is also strongly associated with both poverty and social exclusion[14] and as a result it is a key indicator of health inequalities in the Scottish population[15].
This chapter examines adult mental health and wellbeing in Scotland.
1.1.1 Policy background
The Scottish Government is now in the third year of delivering the 10 year Mental Health Strategy: 2017-2027[16]. The strategy is one of many measures to help create a Fairer Scotland and a Healthier Scotland[17]. The guiding ambition for the strategy is to prevent and treat mental health problems with the same commitment, passion and drive as is given to physical health problems. Failing to recognise, prioritise and treat mental health problems costs the economy, and harms individuals and communities. As a result, the strategy focusses on prevention, early intervention and physical wellbeing, equal access to safe and effective treatment and accessible services. The strategy works to ensure protection and promotion of rights, better information use and planning. The importance of improving measurement of outcomes in mental health is emphasised, to include not just data on service activity but also on effect and the experience for people.
The strategy contains 40 initial actions to better join up services and to ensure that those who need help, only need to ask once. Underpinning these actions is a commitment to tackle mental health inequalities and embed a human-rights based approach across services with high aspirations for service users. The strategy aims to ensure that people in the most marginalised of situations are prioritised in achieving health.
There is also emphasis on improving support and services for children and young people, including those who come into contact with the criminal justice system. Recently, there has been increased national policy focus on the link between adverse childhood experiences including abuse, neglect and poor parenting and an increased risk of mental health problems in early adulthood[18],[19]. Reducing adverse childhood experiences and promoting resilience in those that experience them are now policy priorities for the Scottish Government[20]. Questions on adverse childhood experiences have been included in the Scottish Health Survey in 2019 and will be reported on in next year's report.
The Government recognises that the support available for young people is not currently enough and that to meet the Government's obligations, including those under the UN Convention on the Rights of Persons with Disabilities and the UN Convention on the Rights of the Child, reform is needed[21]. The 2018-19 programme for Government Delivering for Today, Investing in Tomorrow lists a range of actions to make these changes. In December 2018, the Better Mental Health in Scotland delivery plan was published; it sets out actions to implement the above including:
- reforming children and young people's mental health services
- improving specialist services for children and young people and adults
- taking a 21st century approach to adult mental health
- respecting, protecting and fulfilling rights; and
- making suicide prevention everybody's business.
One of the Scottish Government's National Outcomes is the overall strategic objective for health: We are healthy and active[22]. This is supported by a number of National Indicators including 'mental wellbeing'[23] which is monitored using data from the Scottish Health Survey (SHeS). The 15 year, on average, premature mortality in people with severe and enduring mental illness[24] has a major impact on other National Indicators; on 'premature mortality' and 'healthy life expectancy'. Scotland also has a set of national, sustainable mental health indicators for adults and children, covering both outcomes and contextual factors that confer increased risks of, or protection from, poor mental health outcomes[25]. SHeS is the data source for 28 of the 54 indicators for adults[26] and over 20 of the indicators for children[27].
1.1.2 Reporting on mental wellbeing in the Scottish Health Survey (SHeS)
This chapter updates trends in mental health and wellbeing for adults including data on Warwick-Edinburgh Mental Wellbeing Scale (WEMWBS) and General Health Questionnaire 12 (GHQ-12). Figures are also reported by age, sex and area deprivation.
The area deprivation data are presented in Scottish Index of Multiple Deprivation (SIMD) quintiles. To ensure that the comparisons presented are not confounded by the different age profiles of the quintiles, the data have been age-standardised. Readers should refer to the Glossary at the end of this Volume for a detailed description of both SIMD and age-standardisation.
Supplementary tables on mental wellbeing are also published on the Scottish Health Survey website[28].
1.2 Methods And Definitions
1.2.1 Warwick-Edinburgh Mental Wellbeing Scale (WEMWBS)
Wellbeing is measured using the WEMWBS questionnaire. It has 14 items designed to assess: positive affect (optimism, cheerfulness, relaxation) and satisfying interpersonal relationships and positive functioning (energy, clear thinking, self-acceptance, personal development, mastery and autonomy)[29]. The scale uses positively worded statements with a five-item scale ranging from '1 - none of the time' to '5 - all of the time'. The lowest score possible is therefore 14 and the highest score possible is 70; the tables present mean scores.
The scale was not designed to identify individuals with exceptionally high or low levels of positive mental health so cut off points have not been developed[30].
WEMWBS is used to monitor the National Indicator 'mental wellbeing'[31] and the mean score for parents of children aged 15 years and under on WEMWBS is included in the mental health indicator set for children[32].
1.2.2 General Health Questionnaire 12 (GHQ 12)
GHQ-12[33]is a widely used standard measure of mental distress and mental ill-health consisting of 12 questions on concentration abilities, sleeping patterns, self-esteem, stress, despair, depression, and confidence in the previous few weeks. Responses to each of the GHQ-12 items are scored, with one point allocated each time a particular feeling or type of behaviour is reported to have been experienced 'more than usual' or 'much more than usual' over the previous few weeks.
These scores are combined to create an overall score of between zero and twelve. A score of four or more (referred to as a high GHQ-12 score) has been used here to indicate the presence of a possible psychiatric disorder. A score of zero on the GHQ-12 questionnaire can, in contrast, be considered to be an indicator of psychological wellbeing. GHQ-12 measures deviations from people's usual functioning in the previous few weeks and therefore cannot be used to detect chronic conditions.
1.3 Warwick-Edinburgh Mental Wellbeing Scale (WEMWBS)
1.3.1 Trends in adult WEMWBS mean scores since 2008
In 2018, the WEMWBS mean score for adults was 49.4. This is not significantly lower than the WEMWBS mean score for adults in 2017 (49.8), however it is the lowest since the timeseries began in 2008 (mean scores had previously ranged between 49.7 and 50.0).
There was no significant difference between the WEMWBS mean scores for men and women in 2018 (49.3 and 49.6, respectively). Further, there was no significant change in the scores of men or women compared to last year (in 2017 the WEMWBS mean score was 49.9 for men and 49.7 for women.
Since 2008, WEMWBS mean scores have been stable for women, fluctuating between 49.4 and 49.9. For men, scores fluctuated between 49.8 and 50.4 between 2008 and 2012, followed by what appears to be a downward trend, with a significant decrease from 50.4 in 2012 to 49.3 in 2018.
Table 1.1
1.3.2 Adult WEMWBS mean scores in 2018, by age and sex
In 2018, WEMWBS mean scores varied significantly by age with scores decreasing between the youngest and the middle-age groups, and then increasing again in older age groups. As in previous years, those aged 65-74 had the highest WEMWBS mean score (51.6) and those aged 35-44 had the lowest mean score (48.4).
This pattern by age was primarily driven by men with significant differences between the patterns for men and women. Among men, mean WEMWBS scores dropped from 50.7 among those aged 16-24 to a low of 47.2 among those 35-44. Mean WEMWBS scores then gradually increased to a peak of 51.7 among men aged 65-74.
Among women, there was less variation in WEMWBS mean scores across age groups than for men. WEMWBS mean scores were lowest for those aged 16-24 (48.2). There were only minor fluctuations in the scores of those aged 25-64 (49.1 to 49.6), before scores increased to a peak in those aged 65-74 (51.4).
Figure 1A, Table 1.2
Figure 1A
Adult WEMWBS mean score, 2018, by age and sex
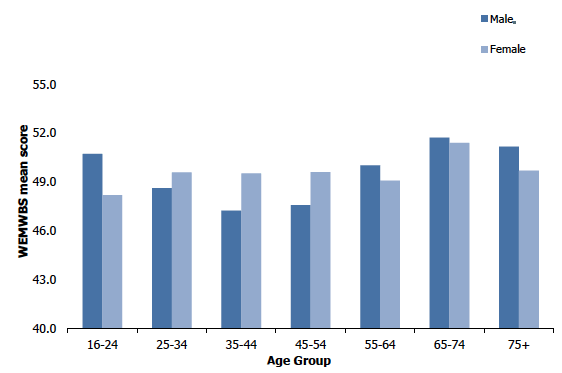
1.3.3 WEMWBS mean scores (age-standardised), in 2018, by area deprivation and sex
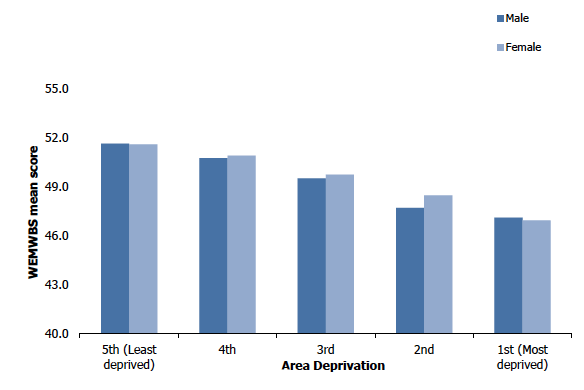
As in previous years, age-standardised WEMWBS mean scores significantly decreased as area deprivation increased. In the most deprived quintile, the mean WEMWBS score was significantly lower (47.0) than in the least deprived quintile (51.6).
This pattern was observed for both men and women. Men in the most deprived quintile had a WEMWBS mean score of 47.1 whilst men in the least deprived quintile had a significantly higher mean score of 51.6. Similarly, women in the most deprived quintile had a WEMWBS mean score of 46.9 whilst women in the least deprived quintile had a significantly higher mean score of 51.6.
Figure 1B, Table 1.3
Figure 1B
WEMWBS mean scores (age-standardised), 2018, by area deprivation and sex
1.4 General Health Questionnaire 12
1.4.1 GHQ-12 scores, 2003-2018
Looking across the time series since 2003, GHQ-12 scores remained relatively static between 2003 and 2017. Between these years the proportion of adults with a GHQ-12 score of four or more (indicating a possible psychiatric disorder) fluctuated between 14-17%. In 2018, 19% of adults had a GHQ-12 score of four or more which is significantly higher than all years since the timeseries began in 2003.
Similarly, in 2018, the proportion of adults with a score of one to three also rose significantly from 23% in 2017 to 28% in 2018 and there was a corresponding decline in the proportion with a score of zero (indicating good psychological wellbeing with no symptoms of mental distress evident) from 60% in 2017 to 53% in 2018.
More men (55%) had GHQ-12 scores of zero, than women (50%) in 2018. This is typical of the pattern since 2003, where a consistently higher proportion of men than women had GHQ-12 scores of zero. Correspondingly, from 2003 to 2018, women were more likely than men to have a GHQ-12 score of 4 or more, however in 2018 this difference was not significant (21% among women and 18% among men).
Table 1.4
1.4.2 GHQ-12 scores in 2018, by age and sex
The percentage of adults with a GHQ-12 score of four or more (indicative of a possible psychiatric disorder) significantly decreased with age. Of those aged 16-24, 24% had a GHQ-12 score of four or more, prevalence ranged between 20% and 21% for those aged 25-64 and then significantly decreased to 13% among those aged 75 and above. Conversely, the percentage of adults with a GHQ-12 score of zero (indicative of good psychological wellbeing and no evident symptoms of mental distress) significantly increased with age. Forty-two percent of those aged 16-24 had a GHQ-12 score of zero, significantly increasing to 62% among those aged 65-74. Consistent with previous years there was then a decline in the percentage of adults with a score of zero among those aged 75+ (56%).
The patterns of GHQ-12 score by age were different for men and women. Among men, the percentage with a GHQ-12 score of four or more was relatively stable between the ages of 16-54 (20-23%). This then decreased to 15% among those aged 55-64 and continued to decrease with age to 10% among those aged 75 and above.
Among women, the percentage with a GHQ-12 score of four or more was highest in young women and peaked again among late middle-aged women before dropping again for older women. Among those aged 16-24, 27% had a GHQ-12 score of four or more, this decreased with age to 18% among those aged 45-54, before peaking again at 24% among those aged 55-64. Of those aged 65 and above, 16% had a GHQ-12 score of four or more.
Figure 1C, Table 1.5
Figure 1C
Percentage of adults with a GHQ12 score of 4 or more, 2018, by age and sex
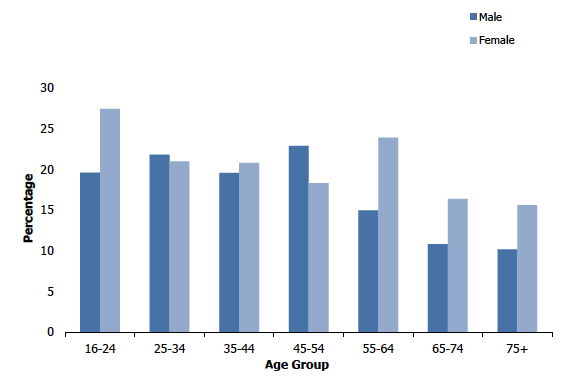
1.4.3 GHQ-12 scores (age-standardised), in 2018, by area deprivation and sex
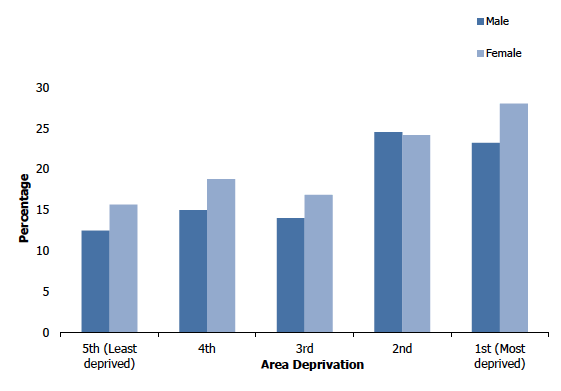
Adults living in the most deprived areas were significantly more likely to have a GHQ-12 score of four or more than those in the least deprived areas. The percentage of adults with a GHQ-12 score of four or more was relatively stable among the 5th (least deprived), 4th and 3rd deprivation quintiles (14-17%) but increased to 24 and 26%, respectively, among the 2nd and 1st (most deprived) quintiles. The percentage of adults with a GHQ-12 score of zero was similar among the 5th (least deprived), 4th and 3rd deprivation quintiles at 55-57%, but decreased in the 2nd and 1st (most deprived) quintiles to 50% and 47%, respectively.
Similar patterns of GHQ-12 scores by area deprivation were found for men and women. Among men, the proportion with a GHQ-12 score of four or more significantly increased from 12% in the least deprived quintile to 23-25% in the two most deprived quintiles. Among women, the proportion significantly increased from 16% in the least deprived quintile to 28% in the most deprived quintile.
Figure 1D, Table 1.6
Figure 1D
Percentage of adults with a GHQ12 score of 4 or more, 2018, by area deprivation
References and notes
1. World Health Organization (2013). Mental Health Action Plan 2013-2020. Available from:
http://apps.who.int/iris/bitstream/10665/89966/1/9789241506021_eng.pdf?ua=1
2. World Health Organization (2017), Mental Health Atlas. Available from: http://apps.who.int/iris/bitstream/handle/10665/272735/9789241514019-eng.pdf?ua=1
3. World Health Organization (2014). Mental Health: a state of well-being. Available from: https://www.who.int/features/factfiles/mental_health/en/
4. World Health Organization (2009). Mental health, resilience and inequalities. Available from: http://www.euro.who.int/__data/assets/pdf_file/0012/100821/E92227.pdf
5. Better Mental Health in Scotland. Edinburgh: Scottish Government, 2018. Available from:
https://www.gov.scot/binaries/content/documents/govscot/publications/strategy-plan/2018/12/programme-government-delivery-plan-mental-health/documents/better-mental-health-scotland/better-mental-health-scotland/govscot%3Adocument
6. See: http://www.gov.scot/Topics/Health/Services/Mental-Health
7. World Health Organization (2018) Depression Fact Sheet. Available from: http://www.who.int/en/news-room/fact-sheets/detail/depression
8. World Health Organization (2017). Depression and Other Common Mental Disorders. Available from: http://apps.who.int/iris/bitstream/handle/10665/254610/WHO-MSD-MER-2017.2-eng.pdf?sequence=1
9. Johnson D, Dupuis G, Piche J, Claybourne Z and Coleman I (2018). Adult Mental Health Outcomes of Adolescent Depression: A Systematic Review. Public Medicine: 35(8): 700-716
10. World Health Organization (2003). Investing in Mental Health. Available from: http://www.who.int/mental_health/media/investing_mnh.pdf
11. World Health Organisation (2018) WHO Guidelines: Management of Physical Health Conditions in Adults with Severe Mental Disorders. Available from: https://apps.who.int/iris/bitstream/handle/10665/275718/9789241550383-eng.pdf?ua=1
12. Mental Health Strategy: 2017-2027 (2017) Edinburgh: Scottish Government Available from: http://www.gov.scot/Publications/2017/03/1750
13. World Health Organisation (2018) WHO Guidelines: Management of Physical Health Conditions in Adults with Severe Mental Disorders. Available from: https://apps.who.int/iris/bitstream/handle/10665/275718/9789241550383-eng.pdf?ua=1
14. Mental Health: Inequality Briefing, Health Scotland, 2017. Available from: http://www.healthscotland.scot/media/1626/inequalities-briefing-10_mental-health_english_nov_2017.pdf
15. Audit Scotland (2012). Health Inequalities in Scotland. Available from: http://www.audit-scotland.gov.uk/docs/health/2012/nr_121213_health_inequalities.pdf
16. Edinburgh: Scottish Government (2017) Mental Health Strategy: 2017-2027. Available from: http://www.gov.scot/Publications/2017/03/1750
17. Fairer Scotland Action Plan. Edinburgh: Scottish Government, 2016. Available from: http://www.gov.scot/Resource/0050/00506841.pdf
18. Mental Health: Inequality Briefing, Health Scotland, 2017. Available from: http://www.healthscotland.scot/media/1626/inequalities-briefing-10_mental-health_english_nov_2017.pdf
19. Couper S, Mackie P. (2016) Polishing the diamonds. Addressing adverse childhood experiences in Scotland. Edinburgh: Scottish Public Health Network (ScotPHN). Available from: https://www.scotphn.net/wp-content/uploads/2016/06/2016_05_26-ACE-Report-Final-AF.pdf
20. A Nation with Ambition: The Government's Programme for Scotland 2017-18. Edinburgh: Scottish Government (2017). Available from: /publications/nation-ambition-governments-programme-scotland-2017-18/
21. Delivering for Today, Investing in Tomorrow: The Government's Programme for Scotland 2018-19. Edinburgh: Scottish Government (2018). Available from: https://www.gov.scot/publications/delivering-today-investing-tomorrow-governments-programme-scotland-2018-19/
22. The National Performance Framework is described here: http://nationalperformance.gov.scot/
23. See: http://nationalperformance.gov.scot/
24. Langan J, Mercer S, W, Smith, D, J. (2013) Multimorbidity and Mental Health: Can Psychiatry Rise to the Challenge? The British Journal of Psychiatry 202: 391-393.
25. See: www.healthscotland.com/scotlands-health/population/mental-health-indicators.aspx
26. Scotland's Mental Health: Adults 2012. Edinburgh: NHS Health Scotland, 2012. Available from: www.healthscotland.com/documents/6123.aspx
27. NHS Health Scotland / ScotPHO (2013). Scotland's Mental Health: children and young people 2013. Available from: https://www.scotpho.org.uk/media/1180/scotpho131219-mhcyp2013-briefing.pdf
28. See: www.gov.scot/scottishhealthsurvey
29. Further information about WEMWBS is available here: www.healthscotland.com/scotlands-health/population/Measuring-positive-mental-health.aspx
30. Stewart-Brown, S and Janmohamed, K (2008). Warwick-Edinburgh Mental Well-being Scale (WEMWBS). User Guide Version 1. Warwick and Edinburgh: University of Warwick and NHS Health Scotland. Available from: http://www.healthscotland.com/documents/2702.aspx
31. See: http://nationalperformance.gov.scot/
32. NHS Health Scotland (2012) Establishing a core set of national, sustainable mental health indicators for children and young people in Scotland: Final Report.
Available from: http://www.healthscotland.com/uploads/documents/18753-C&YP%20Mental%20Health%20Indicators%20FINAL%20Report.pdf
33. Goldberg, D and Williams, PA (1988). A User's Guide to the General Health Questionnaire. Windsor: NFER-Nelson.
Table list
Table 1.1 Adult WEMWBS mean score, 2008 to 2018
Table 1.2 Adult WEMWBS mean score, 2018, by age and sex
Table 1.3 WEMWBS mean score, (age-standardised), 2018, by area deprivation and sex
Table 1.4 GHQ12 score, 2003 to 2018
Table 1.5 GHQ12 score, 2018, by age and sex
Table 1.6 GHQ12 score (age-standardised), 2018, by area deprivation and sex