Scotland's Carers 2015: main report
This report brings together statistical analysis and research on caring. The report is intended to provide a useful source of information for carer's organisations, policy makers, local authorities and anyone who is a carer or knows someone who is a carer.
2. Chapter 2: Carers' Health and Wellbeing
- Caring can be a positve and rewarding experience and can have a positive impact on wellbeing
- Caring can be associated with poor psychological wellbeing and physical health
- Those most at risk of psychological distress are carers in more demanding care situations, providing higher levels of caring over extended period
- Poor carer ill-health can have lasting impacts on the carer which can persist
2.1. Introduction
This chapter explores the health and wellbeing of carers and outlines the impact that caring can have on wellbeing, drawing from a range of research and statistical surveys. It also explores how carers respond to their caring situation and role and draws out the implications for policy and practice.
It's important to understand the impact that caring can have on wellbeing to ensure that appropriate supports are put in place to maintain the health and wellbeing of the carer. It is also important to consider the influence on wellbeing arising from other individual characteristics and circumstances as caring may interact with and exacerbate existing inequalities. For example the last section identified that carers are over-represented in middle and older age groups. These carers may have age-related health problems which they have to manage alongside their caring responsibilities. Similarly the differences between men and women in psychological and mental wellbeing seen in the general population are heightened in the carer population (Hirst 2004). As in other similar studies, our analysis also shows that carers with more significant caring responsibilities are drawn disproportionately from more deprived areas. Caring may therefore stem from lack of choice and unfair circumstances and may be exacerbated by these existing inequalities (Hirst, 2004).
Poor carer health and wellbeing is concerning for both the carer and the cared for person. It can result in greater use of health and care services by the cared for person, particularly older people for example through admission to, and delayed discharge from, hospital; referral to a day hospital or geriatric unit; and admission to institutional care (Pearson et al., 2002; Armstrong, 2000; Williams and Fitton, 1991). Carer ill-health has therefore important implications for formal health and care sectors.
Coping with the stresses and demands, and a willingness to continue caring, are both associated with lower levels of stress in carers (McKee et al., 1999). Therefore it is widely recognised that it is important to maintain the health and wellbeing of carers to enable them to support the people they care for and maintain the quality of their relationships (Hirst 2004).
2.2. Caring can be a positive and rewarding experience
While much attention is focused on the negative aspects of caring, it is important to consider the positive aspects to understand the range of factors that can sustain carers in their role (Hirst, 2004). Caring can be a positive and rewarding experience for both carers and cared for person(s). It can also have a positive effect on wellbeing including hobbies, family life and friendships as well as mental health through the development of self-esteem and confidence (IRISS, Shared Care & Coalition of Carers in Scotland, 2012).
A recent Scottish survey of GP practice patients found that 70% (n= 16,107) of carers surveyed felt that they had a good balance between caring and other things in life (Scottish Government, 2014a). There is also evidence to suggest that there are wellbeing gains for some carers who provide a small amount of care. As discussed later in this chapter, recent analysis of SHeS found that those who provide up to 4 hours per week have higher mean mental wellbeing scores than non-carers (Scottish Government, 2015). Caring can therefore be a positive contributing factor towards wellbeing, providing that it is balanced with other activities.
Some argue that caring can't be seen as a one-dimensional experience, with either positive or negative attitudes: caring satisfaction can co-exist with stressful aspects of the care giving role (Lopez et al., 2005). This implies that interventions to support carers should not just focus on reducing the negative aspects of caring but also find ways to enhance the positive aspects (Bulducci et al., 2008).
Understanding how carers cope with their role is important for policy responses. There is no clear, linear explanation as to why some people experience mental distress while others faced with similar circumstances do not. Factors directly related to the caring situation can have an influence on broader aspects of an individual's life, such as employment and wider family relationships (Sörensen et al, 2006). A carer's subjective view of their ability to cope, can also influence mental health including the presence of depressive symptoms (Pinquart and Sörensen, 2003).
However, certain factors can 'moderate or mediate' the impact of stress on carers (Sörensen et al., 2006). In a study looking at carers of people with dementia, these factors included larger social networks, frequent social contact and the ability to arrange for assistance from friends (Sörensen et al., 2006). Carer enrichment can be experienced through closer familial and wider relationships as well as increased inner strength, confidence and self-esteem (Gelkopf and Roe, 2014; Green, 2007; Deeken, 2003).
Although caring be hugely rewarding, there is a large body of research which highlights carer burden and/or stress with negative consequences for carer health and wellbeing. The section which follows considers such research and discusses which groups of carers are most at risk.
2.3. A note about research
It's worth noting that research on carer wellbeing is vast and varied, ranging from subjective carer assessments largely derived from convenience sample surveys to studies comparing the health of carers with non-carers using probability population surveys and in some cases controlling for other potentially influential variables. The latter identify the factors associated with carer ill-health and provide useful insights into those most at risk from poor carer wellbeing. The former tend to comprise those with heavier caring responsibilities, however, they nonetheless provide useful insights into the demands of care giving from the perspective of carers themselves.
2.4. What do carers say about their health?
- Fewer carers report having "very good" or "good" health, compared with non-carers - 75% of carers compared with 83% of non-carers
- The more care someone provides, the less likely that carer is to report "very good" or "good" health
- Only 3% of carers who care for less that 19 hours a week report "bad" or "very bad" health compared with 5% of non-carers
- 32% of carers reported that caring had a negative impact on their health
This section discusses findings from population and carer-specific surveys on carers' self-reported health.
Population surveys, such as Scotland's 2011 Census, provide useful evidence of the self-reported health of carers compared to non-carers. Scotland's 2011 Census shows that around 5% of the household population claim to have "bad" or "very bad" health. Overall, this percentage is higher for carers at 7%. However only 3% of those caring less than 19 hours a week claim to have "bad" or "very bad" health, while 14% of those who care for 50 or more hours a week report "bad" or "very bad" health.
Carers are less likely to report "very good" or "good" health - overall 83% of non-carers reported "very good" or "good" health compared to 75% of carers. This may partly reflect the fact that carers are likely to be older and may have age-related health problems.
Figure 24: Self-reported health of carers, by hours of care, 2011
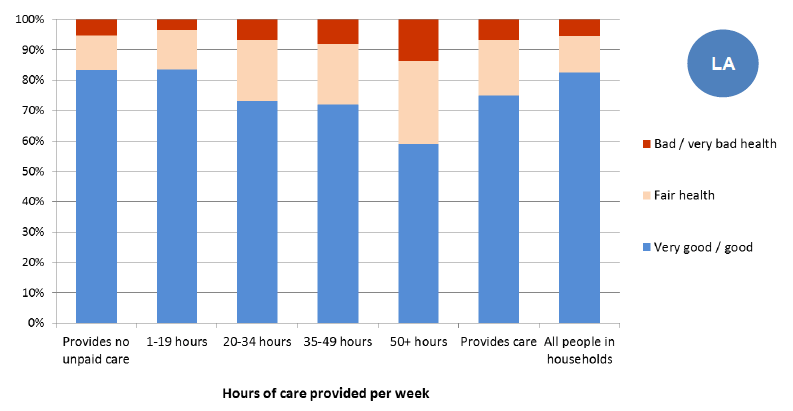
Source: Scotland's Census 2011
Scotland's 2011 Census also shows that the more care someone provides, the less likely they are to report having "very good" or "good" health and this is true for different age groups. For example, 97% of people aged under 25 who provided no care said that their health was "very good" or "good". This compares with 94% of people who provide 1-19 hours of care a week and 86% of people who provide 50 or more hours of care each week. Interestingly, there was very little difference between the group caring for 20-34 hours per week and 35-49 hours per week for this age group.
Figure 25: Percentage of carers who say their health is either "very good" or "good" by age and intensity of care, 2011
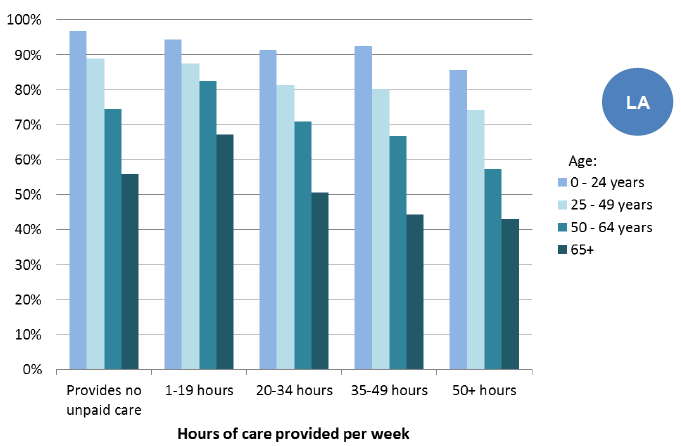
Source: Scotland's Census 2011
The figures presented here represent each person's perception of their health. In some cases the Census may be completed by one person on behalf of the household and in this case it may be that person's perception of the health of each member of the household. In addition it should be noted that people who require care may be more likely to be included in the non-carers category though this is not the case for everyone. Carers' self-reported health deteriorates with age across all levels of caring intensity.
Carers often report poor health as a result of caring in surveys. For example in the recent Health and Care Experience Survey (HACE) of Scottish GP practice patients, 32% (n=4,903) of carers indicated that their health was negatively impacted by their caring role (Scottish Government, 2014a:69) and this rose to 41% in those providing 50+ hours of care.
2.5. Physical wellbeing of carers
- 41% of carers said that they had a long-term condition or illness and this rose in line with care hours provided
- Poorer physical health is associated with old age, challenging care situations, lower socio economic status and less informal support
- Poor carer health can have lasting impacts on the carer which can persist well beyond the end of care giving
- Caring may impact on an individual's ability to look after their own health
- 22% of younger carers (aged under 25) had a long-term condition or disability. This is twice the rate for non-carers (11%)
This section considers the physical wellbeing of carers. Drawing on analysis of population surveys, it highlights the difference in health conditions between carers and non-carers. In addition, it explores the potential effects of caregiving on physical health. While considerable research has been conducted on the effects of care giving on psychological health, there has been less attention focused on the physical impacts of caring (Piquart and Sorensen, 2007). This may be because the evidence around negative impacts of caring on physical health is inconsistent. Studies examining physical associations with caring using objective health measures such as chronic illness, number of hospitalisations etc tend to show smaller associations than those using other physical and subjective indicators which may be because diseases examined are unlikely to be influenced by caregiving (Piquart and Sorensen, 2007).
The 2011 Census analysis shows that carers are more likely to have a long-term condition or illness than non-carers. Overall:
- 41% of carers had a long-term condition or illness; while only
- 29% of non-carers had a long-term condition or illness
As discussed earlier around carers' self-reported health, the reason for the difference could be partly explained by the fact that carers tend to be older and the likelihood of developing a long-term illness or disability increases with age. However this also raises the question of whether caring has an effect on health or whether people who have poor health are more likely to become carers (Parker and Lawton, 1994).
Scotland's 2011 Census shows that 41% (over 203,000 people) of the 492,000 carers said that they had a long term condition or illness.
Figure 26: Percentage of carers who have one or more condition, by level of care, 2011
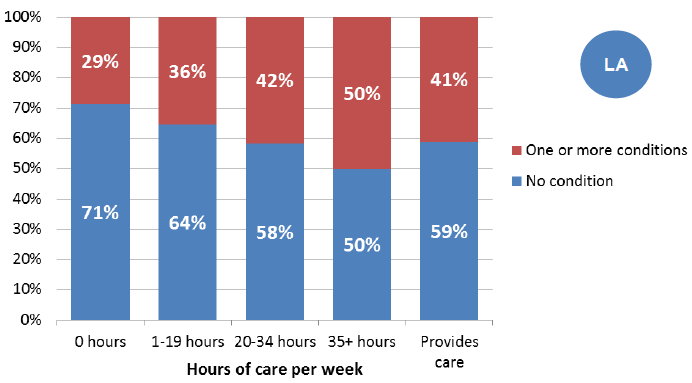
Source: Scotland's Census 2011
Scotland's 2011 Census shows that carers providing more hours of care each week are more likely to have a long-term illness or disability:
- 36% of carers who care for 1-19 hours a week have a long-term condition or disability;
- 42% of carers who care for 20-34 hours a week have a long-term condition or disability;
- Half of carers who care for 35 hours of more each week have a long-term conditions or disability.
It shows that when the proportion of people with long-term conditions is presented for different age groups, younger people are more likely to say they have a long-term condition or disability if they are a carer.
- 22% of young carers (aged under 25) had a long-term condition or disability. This is twice the rate for non-carers (11%).
- 30% of carers aged 25-49 had a long-term condition or disability compared to 21% of non-carers.
- For the 50+ age group there was very little difference between carers and non-carers; just over half had a long-term condition or disability.
Figure 27: Percentage of carers and non-carers who have long-term conditions, by age, 2011
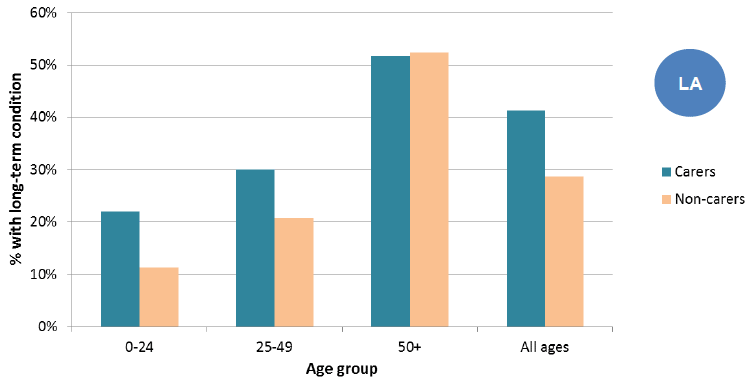
Source: Scotland's Census 2011
Scotland's 2011 Census shows the types of long-term conditions and disabilities experienced by carers and the amount of caring they do. For those carers who said that they had one or more long-term conditions:
- 16% were deaf or had partial hearing loss
- 16% had a physical disability
- 11% had a mental health condition
- 44% had some other condition not listed in the question categories
Figure: 28: Long-term conditions of carers, and level of care per week, 2011
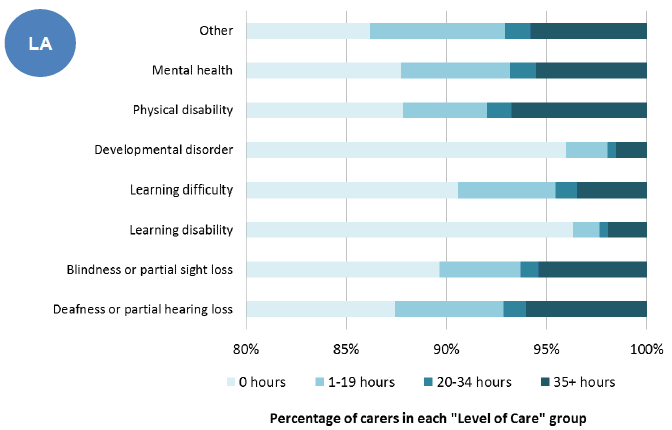
Source: Scotland's Census 2011
2.6. Findings from review of research on physical wellbeing of carers
Carers themselves report poor physical health in carer specific surveys and this rises the more hours spent caring. While these surveys are often based on convenience samples, comprising those with heavier caring responsibilities, they nonetheless provide insight into the demands of care giving from the perspective of carers themselves. For example a recent Scottish carers' survey found that 44 per cent of carers reported that caring had a negative impact on their physical health (IRISS Shared Care & Coalition of Carers, 2012). In the qualitative research which followed the survey, exhaustion and lack of sleep were widely reported among carers.
Studies examining the association between caring and other physiological 'non disease' indicators show differences between carer and non-carer populations. For example Vitaliano et al., (2003) meta-analysis found that carers took more medication for physical illness, had 23% higher levels of stress hormones and 15% lower antibody responses compared with non-carers (Vitaliano et al., 2003). Although this study did not analyse predictors of impaired physical health among carers, it is important given that prolonged stress hormones can increase the risk of hypertension and diabetes, and lower levels of antibodies can reduce resistance to viruses (Vitaliano et al., 2004).
There are many reasons why caring can have an impact on physical health. Some carers encounter particular risks of injury related to their caring activities, and emotional distress associated with care giving may increase susceptibility to physical illness (Brown and Mulley, 1997 and Dyck et al., 1999 cited in Hirst 2004). Increased stress can reduce antibodies and increase the likelihood of infection, and caring situations may lead to health behaviours such as poor diet and lack of exercise (Pinquart and Sorensen, 2007; Glaser and Kiecolt-Glaser, 2005).
Particular groups of carers are more at risk from poor physical health. In a meta-analysis of 176 studies on indicators of physical health, higher levels of care recipient behaviour problems were more consistently related to poor carer health than were care recipient impairment and intensity of care giving (Piquart and Sorensen 2007). Older age, lower socio economic status and lower levels of informal support were related to poorer health. Associations of caregiving stressors with health were stronger among older samples, dementia caregivers and men. The researchers concluded that "the negative effects of caregiving are mostly likely to be found in psychologically distressed caregivers facing dementia related distressors" (Piquart and Sorensen 2007: 132).
In the above meta-analysis, co-resident carers were more likely to experience stronger impacts on physical than on mental health (Pinquart and Sorensen, 2007). Living with the cared for person is likely to mean heavier caring responsibilities and fewer opportunities to take a break from caring (Zarit and Talley, 2013). Having a life alongside caring and being able to take a break is important to carer wellbeing. The absence of such can result in stress and the lack of ability for individuals to look after their own needs (Vitaliano et al, 2003). Co-resident care giving may also be detrimental to health-related habits such as getting sufficient sleep and engaging in healthy eating (Pinquart and Sorensen, 2007).
Studies which have examined the influence of spousal caring on health are mixed. The meta-analysis described above suggested that after controlling for age (since spousal carers are on average older) spousal effects on carer health are generally weaker. This may be because spousal caring is more typical than providing care for other people and because there are less likely to be conflicts between the caring role and other family roles (Pinquart and Sorensen, 2007).
However a number of other studies have shown that caring for a spouse is related to poor physical health. A US longitudinal study of a large sample of adults which modelled the chronicity of caregiving with respect to risk of Cardio Vascular Disease (CVD) onset, found that spousal caring independently predicted risk of CVD. Care giving was associated with a modest, significant elevation in risk of CVD onset among spousal caregivers overall and a near-doubling of risk of CVD onset among spousal caregivers with high intensity caregiving (Capistrant et al., 2012: 3). It's not clear from the study whether this was a direct result of caring or indirectly from health behaviours.
2.7. Carers may find it difficult to look after their own health
Carers may be unable to look after their own health to ensure the wellbeing of the cared for person. Arskey and Hirst (2005) found that women with heavy caring responsibilities were less likely to visit their GP than non-carers. It appears that some carers may treat their own health as secondary to the care recipients. Indeed carers themselves report that it's difficult to look after their own health - 58% of carers responding to the Carers UK survey indicated that they do less exercise since starting caring and 45% find it hard to maintain a balanced diet as a result of caring (Carers UK 2014).
Given that caring may impact on carers' physical health, albeit to a lesser degree than psychological wellbeing, interventions to support carers should also focus on physical health promotion such as providing opportunities for exercise, healthy eating, and preventative care visits (Pinquart and Sorensen, 2007; Patterson and Grant 2003 cited in Pinquart and Sorensen, 2007:132)
2.8. Carers and mental wellbeing
- Nearly 6% of carers say they have a long-term mental health problem; compared with 4% of non carers
- Although there appears to be wellbeing benefits for those caring for up to 4 hours, unpaid caring is a significant predictor of poor mental wellbeing and the presence of possible psychiatric disorder
- Carers who provide more than 35 hours per week are significantly more likely to have lower mental wellbeing scores and exhibit signs of a possible psychiatric disorder than non-carers and those providing fewer hours of care
- Those most at risk of psychological distress and poor mental wellbeing are carers in more demanding care situations, providing higher levels of caring over extended period and co-resident/spousal carers and women are also at risk
This section considers caring and mental wellbeing drawing on objective assessments of mental wellbeing status from population surveys as well as subjective assessment through carer focused studies.
Scotland's 2011 Census allows for analysis of specific long-term conditions or illnesses. Each person is asked whether they have any conditions which have lasted, or are expected to last, at least 12 months. One of the conditions listed is "Mental Health condition". Overall 4% of the population said that they had a mental health condition that had lasted or was expected to last at least 12 months but this was the case for nearly 6% of carers.
Figure 29: Percentage of people with mental health condition, 2011
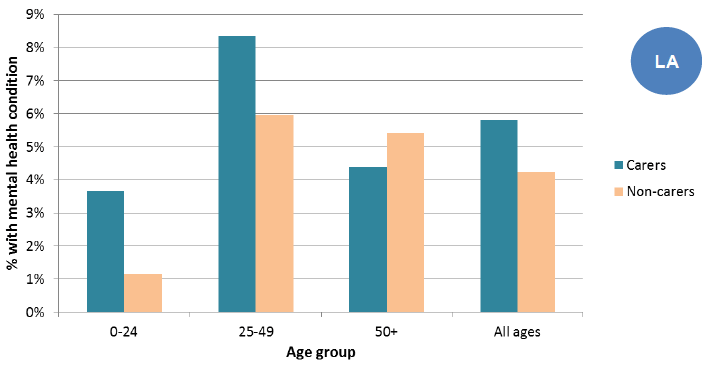
Source: Scotland's Census 2011
Nearly 4% of young carers (aged under 25) said that they had a mental health condition compared with just over 1% of people in this age group who were not carers.
Over 8% of carers aged 25-49 said that they had a long-term mental health condition, compared with 6% of people in this age group who were not carers.
For the age 50 and over age group, the picture is different with 4% of carers saying they had a long term mental health condition (similar to the overall population rate) and over 5% of those not caring having a long-term mental health problem.
2.9. Mental wellbeing and psychiatric disorders
A recent published analysis of SHeS found that mental wellbeing scores were lower among adults who provide unpaid care indicating a lower level of mental wellbeing. SHeS uses the Warwick-Edinburgh Mental Wellbeing Scale (WEMWBS) to measure mental wellbeing and the General Health Questionnaire (GHQ) to identify individuals showing signs of the presence of a possible psychiatric disorder; GHQ12 scores of 4 or higher indicate the signs of the presence of a possible psychiatric disorder. However those who provide a small amount of care (0-4 hours) per week scored more positively on both measures of mental health and wellbeing than non-carers. Those caring 35+ hours per week were significantly more likely to have lower wellbeing scores and exhibit signs of the presence of a possible psychiatric disorder than other groups of carers and non carers (Scottish Government, 2015). More detailed findings from this analysis are outlined below.
The mean score on the WEMWBS scale in 2012/2013 was 50.3 for men and 49.6 for women. Mental Wellbeing is significantly associated with age, with mean scores high in the youngest adults age groups, dropping among adults aged 45-54 (48.9), rising to a peak between aged 65 and 74 (51.1) and then dropping off again among the over 75s (49.5). The analysis comparing carers and non-carers controlled for age to take account of the age profile of carers.
Among carers who provide support for more than 35 hours per week, WEMWBS scores (46.4) were considerably lower than among non-carers (49.9). However, carers who provide a small amount of care, in particular those who provide up to 4 hours per week, showed a higher mean WEMWBS score (51.5) than non-carers, indicating a higher level of mental wellbeing.
Figure 30: WEMWBS mean scores, by sex and hours of unpaid care, 2012/2013
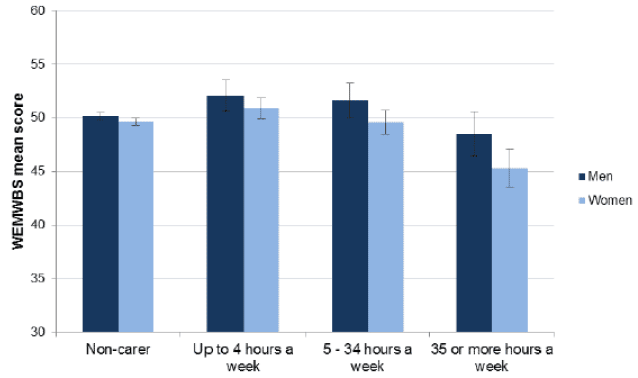
Source: Scottish Health Survey 2012/2013
SHeS also uses the General Health Questionnaire (GHQ) to identify individuals showing signs of the presence of a possible psychiatric disorder. Carers who provide more than 35 hours per week (35%) were significantly more likely to exhibit signs of the presence of a possible psychiatric disorder than non-carers (15%), carers who provide 0-4 hours (10%) or carers who provide 5-34 hours (17%) of care per week. The difference in the proportion exhibiting signs of the presence of a possible psychiatric disorder, comparing carers providing up to 4 hours per week compared to non-carers, was also statistically significant (Scottish Government 2015)
Figure 31: Proportion of adults with GHQ12 scores of four or higher, by hours of unpaid care, 2012/2013
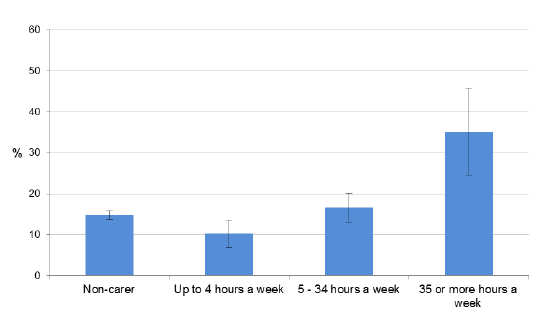
Source: Scottish Health Survey 2012/2013
The above SHeS analysis shows that although there appears to be wellbeing benefits for those caring for a small number of hours each week, unpaid caring is a significant predictor of low mental wellbeing and the presence of possible psychiatric disorders after controlling for other related factors. In addition women who are heavy carers are at risk of poor mental wellbeing. Specifically, women who carry out 35 or more hours of unpaid care were more likely to have a low WEMWBS score compared to those who do not provide any unpaid care. Although the same results were not significant for male carers, in GHQ12, men and women in an unpaid caring role for more than 35 hours per week had greater odds, compared to non-carers, of having a score of four or higher, indicating the presence of a possible psychiatric disorder. GHQ12 results are also marginally significant among women in a caring role for 5-34 hours per week.
Furthermore, women who provide 35 hours or care or more per week were significantly more likely than non-carers to respond negatively for nine of the fourteen WEMWBS component questions. However this was most notably significant for the component 'feeling relaxed' (Scottish Government 2015).
These SHeS findings replicate other similar studies. For example Hirst (2004) found that after taking account of other health determinants, those providing at least 20 hours of care per week were twice as likely to experience psychological distress compared with non-caregivers (Hirst 2004). The study also found that carers' participation in caregiving over time, the number of care episodes, and significant increases in the intensity of caring activities were also associated with a raised risk of emotional and mental health problems in carers.
These findings are reinforced in qualitative studies and surveys of carers involving subjective assessments of impacts. 50% of carers responding to a recent Scottish carers' survey indicated that caring had impacted on their mental wellbeing (IRISS Shared Care & Coalition of Carers in Scotland, 2012).
Co-resident carers are particularly associated with additional health problems (Hirst, 2004). As described earlier, such carers tend to provide more demanding physical and personal care and to be sole carers and least likely to be receiving any support (Parker, 1992 cited in Hirst, 2004). In contrast out-of-household care tends to be less intensive focused more on practical support such as shopping, housework etc (Parker and Lawton, 1994). Indeed non-resident carers who support a friend or neighbour often present better health than non-carers.
Taken together these findings suggests that those most at risk of psychological distress are carers in more demanding care situations, providing higher levels of caring over an extended period.
2.10. Conclusion
Caring can be an extremely rewarding experience. However the evidence suggests that while there appears to be wellbeing gains for some carers, these diminish as caring responsibilities increase. In such circumstances, carers often experience additional health needs which can persist beyond the care giving role. Carers in more complex and demanding caring situations are most at risk of experiencing poor mental and physical health than other carers and the wider population. Although these carers may represent a minority of the carer population, they nonetheless provide the bulk of unpaid care. Taken together the evidence suggests the need to provide adequate support for carers, particularly those most at risk of poorer health to ensure their wellbeing and sustain them in their role. Chapter 4 considers the nature, purpose and effectiveness of support for carers.
Contact
Email: Steven Gillespie
