Scotland's Carers 2015: main report
This report brings together statistical analysis and research on caring. The report is intended to provide a useful source of information for carer's organisations, policy makers, local authorities and anyone who is a carer or knows someone who is a carer.
4. Chapter 4: Support for Carers
- 70% of carers said they received no support with caring responsibilities as did 42% of carers who provide 35 or more hours of care a week
- 23% of carers caring for 35-49 hours reported not feeling supported to care as did 11% fo those caring for up to four hours a week
- Short breaks and information, advice and training are effective ways to support carers
- Carers can be supported directly and via provision to the cared for person
- Carers used a range of types of support, the most common being from family and friends
4.1. Introduction
Generally the purpose of support is to reduce the negative psychological, physical and financial effects that caring can have on a carer. The support is often intended to promote carers' wellbeing which can also permit them to continue to provide care and even prevent older people's admission to institutional care (Yeandle & Wigfield, 2011; Seddon, et al., 2010; Pickard, 2004).
There are many forms of carer support including; information, advice and training; practical support; counselling; short breaks and finance. Carers receive support from numerous sources; family, friends and other carers; paid staff; volunteers and via the state. This chapter presents data from two Scottish Government surveys on the proportion of carers in receipt of, and their needs for, support. This is complimented by findings from a research review on the effectiveness of short breaks and information provision for carers and some of the difficulties for carers in accessing support.
4.2. Support received by carers
SHeS shows that around 70% of carers said that they received no support with their caring responsibilities. This was slightly higher for men with 72% saying they received no support compared with 68% of women. The likelihood of support did increase with number of hours of care; 42% of carers providing 35 hours or more of care say that they did not receive any support.
The SHeS shows the range of support received and the source. The single greatest source was family and friends followed by carer's allowance and then advice and information. In all cases, women were more likely to have support than men:
- 18% of women and 16% of men said that they received support from family and friends;
- 9% of women and 6% of men had support in the form of carer's allowance;
- 8% of women and 6% of men received advice and information to help them in their caring role;
- 5% of women and 4% of men had practical support such as help with transport or equipment;
- 5% of women and men had help provided by a personal assistant, community nurse, home help or similar;
- 4% of women and 2% of men had counselling or emotional support;
- 4% of women and 3% of men received help taking a short break or getting respite from caring;
- 2% of women and 1% of men had training and learning to help them in their caring role.
Figure 40: Support received by carers, 2012/2013
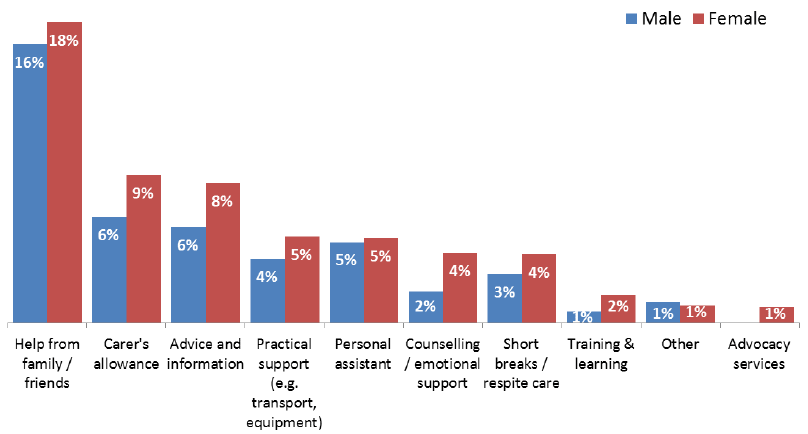
Source: Scottish Health Survey 2012/2013
4.3. Carers' experience of support
- Carers can be unsupported because they are not identified by servces and do not know the support available.
- The assessment process can be useful and be a gateway to further information and services.
- Information, education and training are effective in developing carers knowledge and skills and there are some indication that it can improve their wellbeing.
- Short breaks, mainly in the home, can bring benefits to carers but the nature of the caring context can limit the measureable improvements (Yeandle & Wigfield, 2011).
The Scottish Health and Care Experience Survey (HACE) (Scottish Government, 2014a) shows that many carers are not seeking support. Overall 44% of respondents reported feeling supported to continue caring, whilst 18% did not. Whether respondents feel supported to continue care was related to the number of hours caring. Whereas one in ten respondents caring for up to 4 hours per week reported not feeling supported to continue caring, this rose to over one in five respondents caring for five hours or more and to almost one quarter (23%) of those caring for 35-49 hours (Scottish Government, 2014a).
Figure 41: Proportion of carers who feel supported, 2013/14
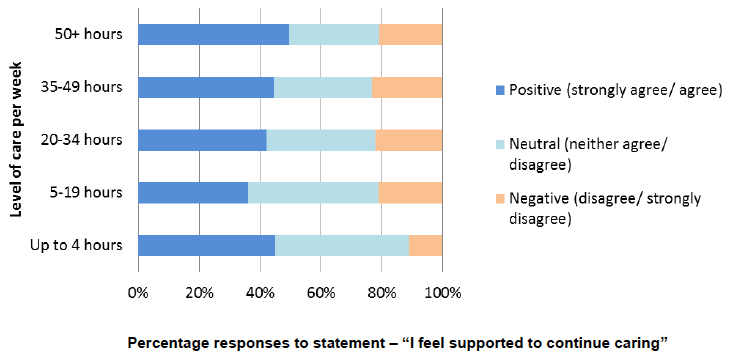
Source: 2013/14 Health and Care Experience Survey
4.4. Ways to support carers
Carers can be supported directly and via provision to the cared for person, as illustrated by the SHeS support received categories. Direct support is provision to the carer, e.g. support groups, training and information. Support via the cared for person is, firstly, provision where the express purpose is to support the carer, e.g. respite care. Secondly it is core services for the cared for person where (incidental) benefits are accrued by the carer (Rand & Malley, 2014; Yeandle & Wigfield, 2011; Parker, et al., 2010; Pickard, 2004). These core services include "personal care services, domestic services…and so on" and there is evidence that these can be the most effective support to carers (Pickard et al., 2004: 9). Indeed a well-established stream of social policy advocates, in line with the independent living agenda, that policy, practice and resources should be directed to support all individuals to live independently (Pickard, 2004). The aspiration is that this will eliminate reliance on family and friends for care (Scourfield, 2005; Pickard, 2004). Scotland's carers policy recognises that provision for the cared for person is integral to carer's outcomes, but is in line with the "dual focus" perspective. This views caring as happening and taking place in a relationship (Scottish Government, 2010a). Consequently the interests of the carer and cared for person can be shared and coincide; or they can differ and even be in conflict (Rand & Malley, 2014; Pickard, 2004). Provision to each party should recognise these permutations and so each should be assessed independently and together and their separate and shared needs addressed (Pickard, 2004). This also means that the effectiveness of support should take into consideration the impact on the carer and cared for person. In this report the focus is on support from public services, aimed at and effective for carers (Pickard, 2004).
4.5. Access to support
The HACE survey findings indicate that at least one in five carers are not sufficiently supported to continue caring (Scottish Government 2014a). The low visibility of carers is one of the numerous reasons that this is the case. Only when professionals and services recognise that individuals are providing care were they likely to signpost them to support (IRISS, Shared Care & Coalition of Carers in Scotland, 2012; Jarvis & Worth, 2004;). However even carers known to local authorities were often unaware of available support (Seddon, et al., 2010). Once they and their needs were identified, carers reported delays in receiving support and practical assistance (such as equipment) (Rand & Malley, 2014). For others the information and support was too late and key decisions taken or a crisis had already occurred (Yeandle & Wigfield, 2011).
Carers themselves can have reasons for being reluctant to involve external services. They may resist external provision due to a strong personal commitment, or obligation, to provide the care; or they can be wary about the upheaval services might bring (Yeandle, et al., 2007a). Young carers reported that they are anxious about being known to public services and the risk of separation from their family (Smyth, et al., 2011). Young and adult carers were found to keep their role hidden to avoid stigma, particularly if they were caring for someone with a drug or mental health problems (Smyth, et al., 2011). Understanding why carers can be reluctant to seek support can inform strategies for improving personal contacts with carers en route to providing them with support. What research identified about what constitutes effective, timely support is the subject of the next section.
4.6. Types of support
4.6.1. Support that benefits carers
This section considers assessment, short breaks and information as three main methods to support carers. The evidence on their impact is not entirely consistent or conclusive but findings point towards positive benefits (Parker, et al., 2010). There are also a range of interventions to support carers and include, inter alia, therapy, counselling, stress management, relaxation and behavioural management skills and specialist support (Parker, et al., 2010). However inadequate evaluations mean it is not possible to draw firm conclusion about the effectiveness of these interventions and so these are not included in this brief review (Parker, et al., 2010).
4.6.2. Carers' assessment
The purpose of a carer's assessment is to identify needs in, and alongside, the caring role. This is the basis for deciding support needs, how these may be addressed and if a service will be provided. The actual assessment process can be beneficial to carers and provide them with emotional support by recognising the contribution they are making and giving them the opportunity to talk through their role (Gray & Birrell, 2013). But research has found that carers are not always aware they have had an assessment nor given an opportunity for an assessment separate, or of equal weight, to that of the cared for person (Newbronner, et al., 2013; Gamiz & Tsegai, 2013). In some instances carers perceived an assessment as a judgement of their ability to provide care (Gamiz & Tsegai, 2013). Staff training and knowledge; time, resources and eligibility criteria can affect whether an assessment takes place (Scourfield, 2005). Whilst an assessment can be a gateway to further information and advice often there is no further support, or it is delayed or it does not meet carer expectations (Victor, 2009). The process for the assessment seems to affect its utility and contribution to an individual's outcomes. A small research project in Scotland found that even with outcomes and carer focused assessments, the method used for assessment was important (Gamiz & Tsegai, 2013). Assessment that involved a conversation with practitioners contributed to more effective outcomes (Gamiz & Tsegai, 2013). Voluntary sector carers' organisations were found to be able to focus more clearly on the carer than statutory organisations where there were different roles and approaches (Gamiz & Tsegai, 2013).
4.6.3. Information and training for carers
Information, education and training have a positive impact on carers' knowledge, skills, mental health and ability to cope (Parker, et al., 2010). These types of support, accompanied by a social component i.e. carers meet with each other, were found to impact positively on psychological well-being (Parker, et al., 2010). Studies found educational interventions reduced depression, certainly in the first few months of caring (Parker, et al., 2010). Studies on carers' of stroke patients found weak evidence but positive impact of education and training on the carers' mental health (Parker, et al., 2010). Information at an early stage was found to improve carers' knowledge. Information reduced depression for those caring for people with dementia but simultaneously increased anxiety for this group and offered no improvement in psychological well-being, carers' burden or quality of life for carers (Parker, et al., 2010). For carers, primarily of older people, information improved their confidence in caring (Yeandle & Wigfield, 2011) and alleviated concerns their actions were inadequate or even harmful (Yeandle, et al., 2007a).
4.6.4. Carers' identified needs and sources of information
Information and advice is sought by carers, particularly at the outset of caring, since many are new to the role and when there are changes in the caring situation. Research with carers found information should to be timely, specific and provided by organisations with specialist knowledge on caring (Newbronner, et al., 2013; Yeandle & Wigfield, 2011; Yeandle, et al., 2007a). Carers identified a wide range of beneficial information-based input including:
- Being told about the caring implications and implications for their role when an individual is diagnosed with dementia (Newbronner, et al., 2013).
- Assistance and advocacy to navigate the complexity of the health and social care systems (McPherson, et al., 2014).
- Financial advice such as on eligibility for benefits.
- Legal advice on employment rights or obtaining "Power of Attorney".
- Information on support groups, short breaks and training on coping skills and managing difficult behaviour.
- Help on dealing with the difficult aspects conditions i.e. challenging behaviour by dementia sufferers (McPherson, et al., 2014; Newbronner, et al., 2013; Parker, et al., 2010; Seddon, et al., 2010; Yeandle, et al., 2007a).
Carers entering into a care giving role feel unprepared for the role and their new tasks. Some feel that their role is imposed on them and that little information is provided about how to care for the person. In an Australian qualitative study (Grimmer et al., 2004) new carers for an elderly person after discharge from acute hospital, reported that they wanted to care but felt their inexperience made day-to-day life more difficult as they adjusted to their role. Carers worried about some of the small practical things and felt that their anxieties were compounded by a lack of information provided to them:
They must think that by some chance or miracle that you can lift the person, and bathe and dress that person. I mean, you've got to work it out for yourself (Wife of person with physical disability.) (Grimmer 2004).
Carers of those with dementia, and couples in same sex relationships, reported information and advice from informal support networks was useful as these also offered mutual support and reduced isolation (Newbronner, et al., 2013). In a similar vein informal networks could be the most effective way to communicate with carers, although it may take a professional to direct a carer to these. Carers did proactively seek information but wanted recommended websites to be confident that the content is accurate and current (Newbronner, et al., 2013).
4.6.5. Short breaks and respite care
Short breaks for carers encompasses diverse provision that can be utilised for a range of purposes. The Scottish Government Carers' Strategy (2010a) statement on short breaks illustrates the range in nature and scope;
"The break might be during the daytime or overnight. The break might be for a couple of hours or for much longer. It might involve the cared-for person having a break away from home, thus benefitting the carer in that they have time for themselves. Or the carer might have a break away, with services being put in place to support the cared-for person. Some people want to have a break together, with additional support to make this happen. Sometimes the service is provided in the home for the cared-for person, with the carer having time to do something themselves for a couple of hours during the day" (Scottish Government 2010a:78).
The Scottish Government publishes annual information on Respite Care Services (Scottish Government 2014b). This shows that:
- There were 203,090 overnight and daytime respite weeks* provided in Scotland in 2013/14. At least a further 12,590 weeks were provided through Direct Payments**.
- The carers of older people (aged 65+) benefitted from 53% of the respite care provided in 2013/14, those of adults aged 18-64 from 36% and those of young people (aged 0-17) from 11%.
* Seven respite nights equal one respite week and 52.5 hours equal one respite week.
** Only 18 out of 32 Local Authorities were able to submit Direct Payment information
4.6.6. Nature of short breaks
Short breaks are for carers "to have a break from their normal routine and the demands in the caring situation" (IRISS, Shared Care & Coalition of Carers in Scotland, 2012). They can reduce the number of hours provided by the carer or provide a brief rest from caring (Phillipson, et al., 2014). The provision can be in the cared for persons home or an external venue. The break can be; for hours or days; frequent or infrequent; on an ongoing, intermittent or one off basis. The carer is the intended beneficiary, although the cared for person is often the recipient of the short break and they may or may not benefit from the break. Short breaks can be taken by the carer and cared for person together to benefit both.
4.6.7. Impact of short breaks
Most research on the effect of short breaks for carers considers the impact on the psychological health of carers (carer burden); the physical health (including reducing mortality); general wellbeing; and ability to continue in employment (Pickard, 2004). Studies have produced differing and even contradictory conclusions on the impact for carers and this is often due to the nature and quality of the evaluation rather than the actual short break (Parker, et al., 2010; Mason, et al., 2007; Pickard, 2004). The demands of caring and the deteriorating condition of the cared for person can be such that community support is inevitably a small influence and measurable positive change for carers difficult to detect (Yeandle & Wigfield, 2011; Pickard, 2004). Short breaks can be disruptive for the cared for person and increased post-break stress and guilt in carers has been identified alongside benefits from the break (Balducci, et al., 2014; Parker, et al., 2010). These bi-directional effects bring added complexity to establishing the effectiveness of short breaks.
These complexities notwithstanding, evidence has indicated that short breaks are beneficial. Carers reported that short breaks provided a rest from caring and the opportunity to maintain a life outside caring (IRISS, Shared Care & Coalition of Carers in Scotland, 2012; Mason, et al., 2007). A major research review concluded that short break provision in the form of institutional respite care and day-care services were beneficial and cost effective for carers of older people (Pickard, 2004). Institutional respite care and day-care services were found to delay admission to residential care for higher care needs older people but not in situations of "bad user-caregiver relationships" and "more reliant care users" (Pickard, 2004). Single studies have found an improvement in a minority of carers over a range of measures including:
- Self-care.
- Coping with stress.
- Quality of caring given.
- Improved social life or taking up a hobby.
- Moving nearer the labour market (e.g. training, considering or contacting an employer).
- Involvement in community and leisure activities (Rand & Malley, 2014; Yeandle & Wigfield, 2011).
Carers in employment benefited from respite care which in turn had a positive effect on them and their ability to continue caring (Yeandle & Wigfield, 2011; Pickard, 2004). In the Yeandle (2011) study half of the respondents experienced no change in wellbeing measures and for one in ten the situation worsened (Yeandle & Wigfield, 2011). Other research concluded that short breaks were neither beneficial nor detrimental to frail older people (Mason, et al., 2007) and negatively impacted on carers' wellbeing and quality of life (Parker, et al., 2010). These differing findings may reflect the complexity of the situation and process and actual provision.
4.6.8. Issues in take up of short breaks
Research found that there are structural and individual issues involved in carers' access to short break. Obtaining provision is one aspect and studies found there to be shortages in rural and urban areas, long waiting times and ineligibility for statutory services (IRISS, Shared Care & Coalition of Carers in Scotland, 2012; Yeandle & Wigfield, 2011; Mason, et al., 2007). Many carers did not know how to obtain a short break and navigating the systems to access these could be difficult (IRISS, Shared Care & Coalition of Carers in Scotland, 2012). Socio-economic factors have an impact and older people and carers on lower incomes were less likely to have had a break (Phillipson, et al., 2014). Some carers expressed concerns around the quality of provision, including lack of trained staff, although there were examples of good, personalised service (Carers UK, 2014; Mason, et al., 2007). Short breaks could be less likely where the cared for person was reluctant to go to residential care even for a short period or eschewed public services generally (Carers UK, 2014; Mason, et al., 2007). Feedback from carers in Scotland indicated satisfaction with the options for, and the support received to organise short breaks. There was less satisfaction with the number and types of services to meet cultural, clinical and practical needs e.g. night services (IRISS, Shared Care & Coalition of Carers in Scotland, 2012). So short breaks are important for carers and can be of benefit but to achieve this can require squaring a number of elements.
4.7. Conclusion
Whilst the majority of carers do not have support, those providing greater numbers of hours care seem more likely to receive support. However at least one in five carers caring for five hours or more did not feel supported to continue caring, although some of these may be receiving an element of support. Carers value and can benefit mentally and physically from tailored, timely information, advice and training. Findings on the impact of short breaks are mixed, although they have been found to be beneficial to the carer. Day care and other provision during the day seem to be effective and more likely to be accepted by the carer and cared for person than residential care. However in many cases caring is demanding and becomes more so with the deterioration of the cared for person. This can limit the wellbeing of carers, even when they are effectively supported.
Contact
Email: Steven Gillespie
