Scottish Health Survey 2016 - volume 1: main report
Statistics relating to the health of people living in Scotland.
7 General Health And Caring
Diana Bardsley
Summary
- The proportion of adults reporting to be in ‘very good’ or ‘good’ health was significantly higher amongst the youngest age group (88% of those aged 16-24) and lower amongst the oldest age group (52% of those aged 75 and over).
- Almost all children aged 0-15 continued to report to be in ‘very good’ or ‘good’ health (95%) in 2015/2016. Overall, girls were more likely than boys to report this (97% and 94% respectively).
- Reported levels of ‘good’ or ‘very good’ health were lowest among children aged 14-15 (91%), compared to 95-98% for children aged 0-13.
- The prevalence of limiting long-term health conditions was significantly higher in the older age groups than younger age groups (from 7% of those aged 0-15, to 60% of those aged 75 and over).
- More than one in seven (15%) adults provided regular, unpaid care to a family member, friend or someone else in 2016, with women more likely to do so than men (17% and 13% respectively).
- Of all children aged 4-15, 3% provided care, with older children more likely to provide care than younger (5% of those aged 12-15 compared with 1% of those aged 4-11).
- Women working full time were significantly more likely to provide unpaid care than men working full time (17% and 12% respectively).
- In 2015/2016, adults providing unpaid care were most likely to do so for 5-19 hours per week.
- Those over the age of 65 were most likely to provide more than 50 hours of care per week at 24%, compared with 13-14% of those aged 16-64.
7.1 Introduction
This chapter covers three interrelated topics: self-assessed general health, co-morbidity of multiple long-term conditions and caring.
Population measures of self-reported health can be a general indicator of the burden of disease on society. They can reflect subjective experiences of both diagnosed and undiagnosed illnesses, and their severity, which more objective measures for the whole population can sometimes overlook.
Self-assessed general health is often a reflection of the presence or absence of long-term conditions, both physical and mental. In Scotland today people are living longer but with multiple long-term conditions and increasingly complex needs[1]. Such conditions account for 80% of all GP consultations and for 60% of all deaths in Scotland[2]. People with a long-term condition are twice as likely as those without to be admitted to hospital and stay in hospital disproportionately longer[3]. Older people are more likely to have multiple long-term conditions. Given Scotland’s ageing population (in 2016, 8% of the population were 75 and over; this is predicted to rise to 14% by 2039[4]), this has become an increasingly important public health issue.
The associations of general health and long term conditions with deprivation, lifestyle risk factors and wider health determinants are also of importance in Scotland given its persistent health inequalities. For example, those living in disadvantaged areas are more than twice as likely to have a long-term condition as those in affluent areas and to develop it an earlier age (up to 10 years earlier)[5].
It is also recognised that the majority of care for those living with long-term conditions is provided by family and other unpaid carers although most will ultimately increasingly require support from health and social care services[5].
It is estimated that around 788,000 people are caring for a relative, friend or neighbour in Scotland including 44,000 people under the age of 18[6]. The provision of unpaid care to family members, friends or others is not shared equally across social groups. Also, the mental and physical health and wellbeing of carers can be negatively affected by the caring demands placed upon them; around a third of carers have reported that caring has a negative impact on their health and the more care that a carer provides, the less likely they are to report good health[6].
The prevalence of long-term conditions therefore represents significant personal, social and economic costs both to individuals and their families as well as to health and care services and Scottish society more widely.
7.1.1 Policy background
The Scottish government recognises the need to change the way services are delivered in the context of the changing Scottish demographic, notably the ageing population and the increasing number of people living with long term conditions and multi-morbidity. The strategic focus for improving general health and wellbeing and supporting people living with long term conditions is set-out in three over-arching strategies.
The National Clinical Strategy[7], published in 2016, is the high level vision for how health and social care services will develop over the next 10-15 years. The Health and Social Care Delivery Plan[8] sets out the programme to further enhance health and social care services so people can live longer, healthier lives at home or in a homely setting. These establish the overarching aims for public health concerned with prevention, early intervention and supported self-management. In Realising Realistic Medicine[9], published in 2017, the government sets out plans to adopt Realistic Medicine, moving away from a culture where ‘doctor knows best’ to one where people receiving care are at the centre of decision-making and professionals are encouraged to take a personalised approach to their care. It aims to reduce harm and waste, tackle unwarranted variation in care, manage clinical risk, and support innovation to improve care and sustainability in the NHS.
Prior to this, in 2008, the Scottish Government’s strategy for self-management Gaun Yersel[10] was launched, supported annually by the self-management fund. Self-management is a set of approaches which enable people living with long term conditions and those who care for them to take control and manage their own health and care.
One of the Scottish Government's National Outcomes is the overall strategic objective for health: We live longer, healthier lives[11]. This is supported by a number of National Indicators including 'improve self-assessed general health'. Data from SHeS is used to monitor progress towards this indicator. In addition, the purpose target to improve healthy life expectancy over the 2007 to 2017 period uses
SHeS data for children (aged 0-15) in the calculations used to measure progress.
The Carers (Scotland) Act (2016) will be commenced on April 1, 2018. It extends and enhances the rights of carers to ensure better and more consistent support for carers and young carers so that they can continue to care, if they so wish, in better health and to have a life alongside caring. This builds on a range of national policy drivers. Caring Together: The Carers Strategy for Scotland 2010-15[12] was published in July 2010 and set out actions to support carers and ensure their health and wellbeing, including the commitment to the voluntary sector Short Breaks Fund[13] , and the inclusion of an indicator on carers in the core part of the GP contract[14]. In 2011 Reshaping Care for Older People[15] was published with the vision that 'older people are valued as an asset, their voices are heard and they are supported to enjoy full and positive lives in their own home or in a homely setting' and includes ambitions to improve support for unpaid carers.
Recognising that children and young people provide unpaid care, and have particular needs, the Scottish Government, along with COSLA, published a separate strategy Getting it Right for Young Carers[16] which aims to ensure that young carers are relieved of inappropriate caring roles and supported to be children first and foremost. Questions to ascertain the prevalence of young carers (aged 4-15) were introduced to SHeS in 2012.
The Scottish Government has recently made commitments to increase the Carers Allowance and introduce a package of new measures to support young carers including a Young Carer Grant for young carers aged 16-18.
7.1.2 Reporting on general health, long-term conditions and caring in the Scottish Health Survey
This chapter reports on self-assessed general health and prevalence of long-term conditions for adults and children. The prevalence of those with caring responsibilities is reported by deprivation, employment status and sex. Finally, hours spent each week providing help or unpaid care is reported.
The area deprivation data are presented in Scottish Index of Multiple Deprivation (SIMD) quintiles. To ensure that the comparisons presented are not confounded by the different age profiles of the quintiles, the data have been age-standardised. Readers should refer to the Glossary at the end of this Volume for a detailed description of both SIMD and age-standardisation.
Supplementary tables on general health and caring are also published on the Scottish Health Survey website[17].
7.2 Methods and definitions
7.2.1 Self-assessed general health
Each year, participants who are aged 13 and over are asked to rate their health in general with answer options ranging from ‘very good’ to ‘very bad’. For children under the age of 13 the question is answered by the parent or guardian completing the interview on their behalf. This question is used to monitor the National Indicator ‘improve self-assessed health’, while the data for children (aged 0-15) is used in the calculation of healthy life expectancy used to monitor the related purpose target to improve healthy life expectancy between 2007 and 17.
7.2.2 Long-term conditions
All participants were asked if they had any physical or mental health condition or illness lasting - or likely to last - for twelve months or more. Those who reported having such a condition were asked to provide details of the type(s) of conditions or illnesses reported. Answers were recorded verbatim and then coded by an analyst. These questions did not specify that conditions had to be doctor-diagnosed; responses were thus based on individuals’ perceptions.
At a later stage of the interview, participants were asked about a number of specific health conditions, including diabetes and hypertension. If the participant mentioned that they had doctor-diagnosed diabetes or that they had doctor-diagnosed hypertension in response to these questions, but they had not mentioned them as a long-term condition, they were each counted as such a condition.
7.2.3 Caring
The provision of unpaid care is measured by asking participants if they look after, or give any regular help or support to, family members, friends, neighbours or others because of a long-term physical condition, mental ill-health or disability; or problems related to old age. Caring which is done as part of any paid employment is not asked about. From 2014 onwards this question explicitly instructed respondents to exclude caring as part of paid employment. This question has been asked of adults aged 16 and over since 2008, and of children aged 4 to 15 since 2012. Those who say they provide such care are then asked how many hours per week they typically provide. From 2014 onwards this question has also explicitly instructed respondents to exclude caring as part of paid employment. Additional questions explore the impact that caring has on activities. From these additional questions, the impact on employment is reported this year. The support available to carers is also explored but not reported here.
7.3 Self-Assessed General Health
7.3.1 Self-assessed general health among adults in 2016, by age and sex
As shown in table 7.1, almost three quarters (73%) of adults aged 16 and over described their health as ‘very good’ or ‘good’ in 2016. Approximately one in ten (9%) adults reported their health as being ‘bad’ or ‘very bad’.
As shown in figure 7A, the proportion of adults reporting to be in ‘very good’ or ‘good’ health declined significantly with age, from 88% of those aged 16-24, to 52% of those aged 75 and over - a decrease of 36 percentage points.
In a related finding, the percentage of adults reporting to be in ‘bad’ or ‘very bad’ health increased significantly with age, from 3% of those aged 16-24, to 18% of those aged 75 and over.
Whilst age was significantly associated with self-assessed general health for adults, sex seemed to have little effect on self-reported general health, with men and women reporting broadly similar levels of health across all age groups (see Figure 7A).
Figure 7A, Table 7.1
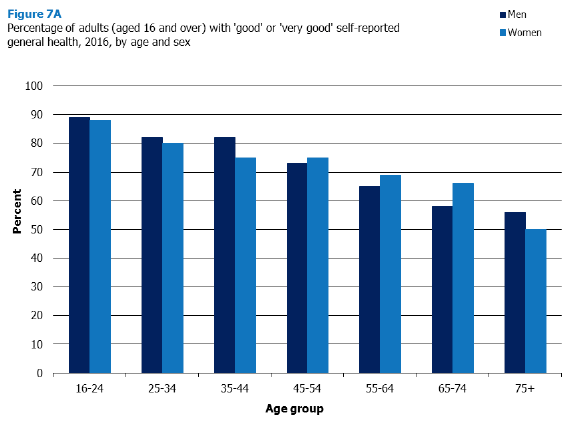
7.3.2 Self-assessed general health among children in 2015/2016 combined, by age and sex
In 2015/2016, almost all children aged 0-15 in Scotland were reported as being in ‘very good’ or ‘good’ health (95%), and 4% as having ‘fair’ general health. Only 1% of children were reported as having ‘bad’ or ‘very bad’ general health.
Overall, girls were more likely than boys to report ‘good’ or ‘very good’ general health (97% of girls, compared with 94% of boys). There was no difference between the percentage of boys and girls reporting ‘bad’ or ‘very bad’ health (both 1%).
Self-assessed health varied significantly by age with reported levels of ‘good’ or ‘very good’ health being lower among older children aged 14-15 (91%), compared with children aged 0-13 (95-98%). This finding could in part be explained by the survey design which involved asking parents of children aged 0-11 about their child’s health status, and asking children aged 12-15 directly.
The pattern by age was different for girls and boys, with more fluctuation in rates for boys than girls. Furthermore, parents of younger girls (0-7) were more likely to report they had ‘good’ or ‘very good’ health than parents of boys in the same age range (97-98% for girls compared with 91-96% for boys).
7.4 long-term conditions
7.4.1 Prevalence of long-term conditions in 2016, by age and sex
Children
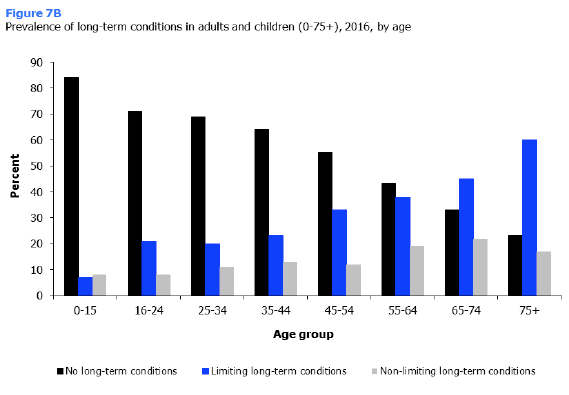
In 2016, almost one in six (16%) children (aged 0-15) had at least one long-term health condition. This proportion was comprised of 8% of children that had non-limiting condition(s) and 7% that had at least one limiting long-term condition. Boys were significantly more likely than girls to have any form of long-term condition (18% and 14% respectively) as well as at least one limiting long-term condition (9% and 6% respectively).
Adults
Around half (47%) of adults aged 16 and over in Scotland were living with at least one long-term condition in 2016. Prevalence of adults with limiting long-term conditions was more than double that of those with non-limiting conditions (33% and 14% respectively).
Prevalence of limiting long-term health conditions increased markedly with age, from 21% of those aged 16-24 to 60% of those aged 75 and over. The sharpest increase in limiting long term health conditions occurred between ages 65-74 (45%) and 75 and over (60%) - an increase of 15 percentage points.
Younger people were significantly more likely to be free of long-term health conditions, with prevalence rising with age. Just 23% of those aged 75 and over were free of any long term health conditions, compared with 71% of those aged 16-24 - a difference of 48 percentage points. This pattern by age was true for both men and women.
Women were more likely than men to have one or more limiting long-term health condition (35% and 30% respectively).
Prevalence of adults with non-limiting conditions also varied significantly by age. Although the pattern was not linear, older age groups tended to report higher prevalence than younger age groups (8-13% for those aged 16-54 compared with 17-22% for those aged 55-75 and over). Prevalence of adults with non-limiting conditions did not differ significantly between men and women.
Figure 7B, Table 7.3
7.5 Provision Of Unpaid Care
7.5.1 Unpaid caring prevalence in 2016, by age and sex
Adults
Over 1 in 7 (15%) adults aged 16 and over were providing regular, unpaid care to a family member, friend or someone else in 2016.
Women were more likely than men to be providing unpaid care for someone (17% and 13% respectively). The gap between men and women was most notable in the 45-54 year age group (27% of women, compared with 18% of men providing care).
As shown in Figure 7C, caring prevalence increased in line with age up to age 45-54 (9% for those aged 16-24 to 23% for those aged 45-54) before declining with age down to 9% for those aged 75 and over. Of all adults, women aged 45-54 were the most likely to be providing unpaid care (at 27%) and men aged 16-24 were the least likely to (at 6%).
Children
In 2016 a small proportion (3%) of children aged 4-15 were providing regular, unpaid care to a family member, friend or someone else. In contrast with adult caring rates, there was little difference by sex (3% of boys, compared with 2% of girls providing care overall).
As shown in Figure 7C, older children were much more likely to provide unpaid care than their younger counterparts (5% of those aged 12-15 compared with 1% of those aged 4-11).
The proportion of boys caring varied significantly by age, with boys aged 12-15 being the mostly likely to provide care (7%). The difference between caring prevalence and age for girls was not significant (2% among girls aged 4-11 and 3% among girls aged 12-15 providing care).
Figure 7C, Table 7.4
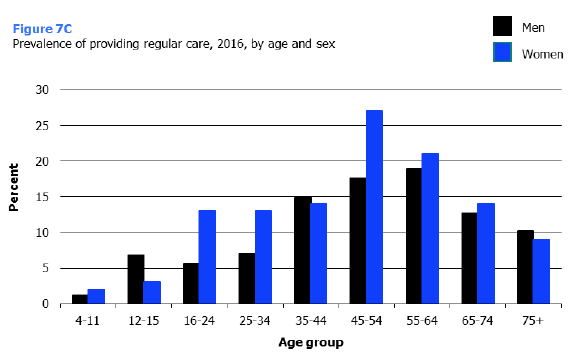
7.5.2 Unpaid caring prevalence in 2016, by area deprivation and sex
There was no significant difference between rates of caring in the most and least deprived areas. Age standardised results showed that 14% of adults in the least deprived quintile were providing care in 2016, compared with 15% of adults in the most deprived quintile. This overall finding was true for both men and women.
7.5.3 Unpaid caring prevalence in 2016, by employment status and sex
Adults working full time were significantly less likely to provide unpaid care (14%) than adults of the same age who were not working (19%) or working part time (18%). Women working full time were significantly more likely than men working full time to provide unpaid, regular care (17% of women, compared with 12% of men).
7.5.4 Hours spent caring in 2015/2016 combined, by age and sex
The majority of carers reported spending less than 19 hours a week on their caring responsibilities. Adult carers were most likely to spend between 5 and 19 hours a week (34%) or below 5 hours a week (31%) providing help or unpaid care. Just 1 in 7 (15%) carers were providing care for 50+ hours per week. Only 4% of adults providing care did so for 35-49 hours per week.
There were some significant differences between age groups in the hours of care that they provided. Carers aged 65+ were the most likely to provide care in excess of 50 hours a week (24% did so, compared with 14% of those aged 16-44 and 13% for those aged 45-64). This pattern was more pronounced for men, with 33% of male carers aged 65 and over providing care for 50 or more hours a week, compared with 17% of female carers in the same age group.
Younger adults were more likely than older adults to provide up to 4 hours of help or unpaid care (36% of carers aged 16-44 compared with 25% of carers aged 65 and over).
The proportion of those providing the most common amount of care (5-19 hours) also varied significantly by age with those aged 45-64 being most likely to do so (39%) compared with 31% of carers aged 16-44, and 27% of those aged 65+.
Contact
Email: Julie Landsberg, Julie Landsberg
Phone: 0300 244 4000 – Central Enquiry Unit
The Scottish Government
St Andrew's House
Regent Road
Edinburgh
EH1 3DG
