Scottish Health Survey 2016 - volume 1: main report
Statistics relating to the health of people living in Scotland.
9 Cardiovascular Conditions And Diabetes
Suzanne Hill
Summary
- Among adults aged 16 and over, 19% had some form of cardiovascular disease (CVD) or diabetes, 15% had any CVD, and 5% had diabetes. These numbers have remained relatively stable in recent years.

- In 2016, 8% of adults reported ischaemic heart disease (IHD) or stroke. This level has remained unchanged since 2008.
- Older people were more likely to have some form of CVD or diabetes than young people (47% of those aged 75 and over compared with 5% of those aged 16-24).
- The prevalence of IHD or stroke was also significantly associated with age, with less than 1% of those aged 16-44 reporting, compared with 29% of those aged 75 and over.
- In 2016, those in the most deprived areas reported a higher prevalence of some form of CVD than those in the least deprived areas (18% and 12% respectively).
- Prevalence of any CVD was highest among ex-drinkers (23%) followed by those that had never drunk alcohol (18%) or drank over 35 units per week (17%). Prevalence was lowest for those who drank between 14 and 35 units per week (13%) or drank within the recommended guidelines of a maximum of 14 units a week (15%) .
- Ex-drinkers were more likely to have had a stroke (5%) than those drinking within or outwith the recommended guidelines (2-3%) and never drinkers (3%), (age standardised).
- The prevalence of CVDs (with the exception of stroke) and diabetes was significantly higher among adults who were obese, compared with those who were underweight, of normal weight, or overweight (but not obese).
9.1 Introduction
Cardiovascular disease (CVD) is a general term describing diseases of the heart and blood vessels whereby blood flow to the heart, brain or body is restricted. It is one of the leading contributors to the global disease burden[1]. Its main components are ischaemic heart disease (IHD, or coronary heart disease) and stroke, both of which have been identified as clinical priorities for the NHS in Scotland[2,3]. Diseases of the circulatory system are the second most common causes of death in Scotland after cancer, accounting for 27% of deaths in 2016 (compared with 29% for cancer). This includes 12% of deaths which are caused by IHD, with a further 7% caused by cerebrovascular disease (e.g. stroke)[4]. Early mortality from heart disease and stroke have both improved in recent years, but concern remains about continuing inequalities in relation to morbidity and mortality linked to these conditions[2,3].
The increasing prevalence (albeit at a reduced rate) of diabetes, the most common metabolic disorder, is a major health issue for Scotland. The prevalence of diabetes continues to increase for a number of reasons including an ageing population, better survival, and better detection rates for Type 2 diabetes and a steady increase in the incidence of Type 1 diabetes in Scottish children over the last 40 years[5]. Scotland has one of the highest levels of Type 1 diabetes in Europe, but it is the increasing prevalence of Type 2 diabetes – linked to obesity, physical inactivity and ageing – which is driving the increased prevalence and causing concern[6]. Diabetes is a risk factor in premature mortality, although more effective treatments of diabetes and hypertension have offset some of the excess risk in recent years and mean some people may be living longer and better with the condition[7].
9.1.1 Policy background
A key Scottish Government National Performance Framework National Outcome is for people in Scotland to ‘live longer, healthier lives’[7]. There is also a National Performance indicator to ‘reduce premature mortality’ (deaths from all causes in those aged under 75)[8]. CVD is described as one of the key ‘big killer’ diseases around which action must be taken if this target is to be met. In addition, a number of the National Indicators[9] are linked to key CVD risk factors, most notably smoking[10], but also physical activity[11] and healthy weight children[12] (the latter two are also major risk factors for Type 2 diabetes). Due to the clinical priority given to heart disease and stroke by the Scottish Government, there has been some success in reducing death rates from these diseases in recent years[15].
In recognition of the challenges posed by CVD and diabetes as long-term conditions for individuals, their families and health and care services – the Scottish Government’s first over-arching strategy for long-term conditions was published in 2009. The Action Plan recognised the need for system-wide action in response to the challenge presented by the increasing prevalence of long-term conditions within the context of an ageing population, the links to health inequalities, and the particular challenges of multi-morbidity (the presence of two or more long-term conditions). Now, responding to the context of the ageing population and the increasing number of people living with long term conditions and multi-morbidity in Scotland, the strategic focus for improving general health and wellbeing and supporting people living with long term conditions is set-out in three over-arching strategies.
The National Clinical Strategy[13], published in 2016, is the high level vision for how health and social care services will develop over the next 10-15 years. The Health and Social Care Delivery Plan[14] sets out the programme to further enhance health and social care services so people can live longer, healthier lives at home or in a homely setting. These establish the overarching aims for public health concerned with prevention, early intervention and supported self-management. In Realising Realistic Medicine[15], published in 2017, the government sets out plans to adopt Realistic Medicine, moving away from a culture where ‘doctor knows best’ to one where people receiving care are at the centre of decision-making and professionals are encouraged to take a personalised approach to their care.
The separate Heart Disease[2], Stroke[3] and Diabetes[16] Improvement Plans, published in August 2014 and November 2014, align with the approaches set out in the three overarching strategies above. They reaffirm the aims and priorities on improved prevention, treatment and care in heart disease, stroke and diabetes, focusing on clinical outcomes and patient experience. They build on the Heart Disease and Stroke Action Plan[17] which was published in 2009, and the Diabetes Action Plan[6] which was published in 2010, both of which set out a comprehensive programme for further reducing deaths and improving the lives of people living with heart disease, stroke and diabetes. Diabetes is known to increase the risk of CVD and the Diabetes Improvement Plan[16] focusses priority action to improve glycaemic control to reduce risk of associated complications and additionally to identify risk of complications early ensuring prompt treatment.
9.1.2 Reporting on CVD conditions and diabetes in the Scottish Health Survey (SHeS)
Valuable information on the prevalence of CVD conditions and diabetes in Scotland is provided by SHeS. It also offers useful information on the patterning of these conditions across different population groups. In this chapter, trends in self-reported CVD conditions and diabetes prevalence for adults are updated for 2016. Self-reported CVD conditions and diabetes are also reported for 2016 by age, sex, deprivation, alcohol consumption, smoking status, overweight and obesity.
The area deprivation data for CVD conditions and diabetes are presented in Scottish Index of Multiple Deprivation (SIMD) quintiles. To ensure that the comparisons presented are not confounded by the different age profiles of the quintiles, the data have been age-standardised. Readers should refer to the Glossary at the end of this Volume for a detailed description of both SIMD and age-standardisation.
Supplementary tables on CVD conditions and diabetes are also published on the Scottish Health Survey website[18].
9.2 Methods And Definitions
9.2.1 Methods
Participants were asked whether they had ever suffered from any of the following conditions: diabetes, angina, heart attack, stroke, heart murmur, irregular heart rhythm, or ‘other heart trouble’. If they responded affirmatively to any of these conditions, participants were asked whether they had ever been told they had the condition by a doctor and whether they had experienced the conditions in the previous 12 months. For the purposes of the analysis presented in this chapter, participants were only classified as having a particular condition if they reported that the diagnosis had been confirmed by a doctor.
It is important to note that no attempt was made to verify these self-reported diagnoses objectively. It is therefore possible that some misclassification may have occurred because some participants may not have remembered (or not remembered correctly, or not known about) diagnoses made by their doctor.
9.2.2 Definitions
Any CVD condition
Participants were classified as having ‘any CVD’ if they reported ever having any of the following conditions confirmed by a doctor: angina, heart attack, stroke, heart murmur, abnormal heart rhythm, or ‘other heart trouble’[19].
Diabetes
Participants were classified as having diabetes if they reported a confirmed doctor diagnosis. Women whose diabetes occurred only during pregnancy were excluded from the classification. No distinction was made between Type 1 and Type 2 diabetes in the interview.
Any CVD condition or diabetes
A summary measure of the above conditions is presented in the tables as ‘any CVD condition or diabetes’.
Ischaemic heart disease (IHD)
Participants were classified as having IHD if they reported ever having angina or a heart attack confirmed by a doctor. All tables refer to ever having had the condition.
Stroke
Participants were classified as having a stroke if they reported ever having had a stroke confirmed by a doctor.
IHD or stroke
A summary measure of the above conditions is presented in the tables as ‘IHD or stroke’.
9.3 Cardiovascular Conditions And Diabetes
9.3.1 Trends in any CVD, diabetes, any CVD or diabetes, IHD, stroke, and IHD or stroke prevalence since 2003
Any CVD
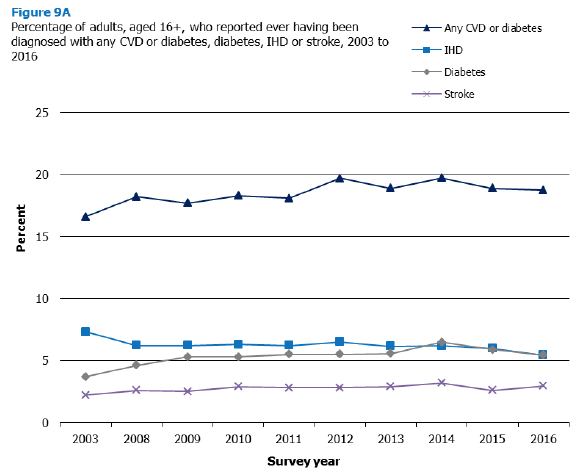
In 2016, 15% of adults reported having ever been diagnosed with any CVD condition. This figure has remained relatively stable across survey years (14-16% between 2003 and 2016), and has not changed significantly during this time period.
The proportion of men reporting any CVD conditions has not changed significantly between 2003 and 2016, with fluctuations from 15% in the period from 2003-2009 to a high of 18% in 2014, dropping to 16% in 2015 and 2016. Similarly for women there has been no significant change in prevalence for any CVD across the period 2003 to 2016, with levels fluctuating between 14% and 16% (15% in 2016).
Doctor-diagnosed diabetes
The prevalence of doctor-diagnosed diabetes was significantly higher in 2016 (5%) than in 2003 (4%). Prevalence in 2016 was not significantly different from 2015 (6%).
The prevalence of doctor-diagnosed diabetes reported by men has decreased significantly from 8% in 2014 to 6% in 2016. Prevalence rates had previously risen from 4% in 2003 to 8% in 2014. For women, the proportion reporting doctor-diagnosed diabetes has been stable at 5% since 2011.
Figure 9A, Table 9.1
Any CVD or diabetes
In 2016, 19% of adults reported experiencing any CVD or diabetes, a significant increase since 2003, when prevalence was 17%. However, prevalence has remained largely unchanged in recent years, staying between 19-20% from 2012 to 2016.
The proportion of men reporting any CVD or diabetes in 2016 was 19%. This rate has fluctuated between 18% and 23% since 2008. There has been a significant increase in any CVD or diabetes in women between 2003 (16%) and 2016 (18%) with levels fluctuating between 16% and 19% over that time period.
IHD
The proportion of adults reporting an IHD diagnosis (angina or heart attack) has significantly decreased from 7% in 2003 to 5% in 2016, with the level having been largely stable in the intervening years (6-7%).
The proportion of men reporting a diagnosis of IHD in 2016 remained stable at 7%. The rate has been 7% or 8% in each of the years between 2003 and 2016. The prevalence of IHD for women was 4% in 2016, continuing the general downward trend from 7% in 2003.
Stroke
In 2016 the proportion of adults reporting stroke was 3%, this level has remained stable since 2008. However, it was significantly higher than 2003 when prevalence was at 2%.
There were no significant differences between men and women in prevalence of stroke. Figure 9A, Table 9.1
IHD or stroke
The proportion of adults reporting an IHD or stroke diagnosis in 2016 has remained stable since 2008 (8%) but was significantly lower than in 2003 (9%).
This is largely accounted for by the proportion of women reporting IHD or stroke falling significantly from 8% in 2003 to 6% in 2015 and 2016. There has been no significant change in the proportion of men reporting IHD or stroke since 2003 with prevalence fluctuating between 9 and 10%.
9.3.2 Any CVD, doctor-diagnosed diabetes, any CVD or diabetes, IHD, stroke, IHD or stroke, 2016, by age and sex
Any CVD
In 2016, 15% of all adults reported being diagnosed with any CVD condition. There was a positive association between the prevalence of any CVD condition and age, with a steady increase across the age categories from 5% for those aged 16-24 to 40% for those aged 75 and over.
For all adults, prevalence of any CVD did not differ significantly between men (16%) and women (15%). A significant increase in any CVD by age was observed for both groups.
Doctor-diagnosed diabetes
The prevalence of doctor-diagnosed diabetes for all adults was 5% overall in 2016, with a significant upward gradient from those aged 16-34 (0-1%) to those aged 65 and over (14%).
There was no significant difference in the prevalence of doctor-diagnosed diabetes between men (6%) and women (5%). A significant increase in doctor-diagnosed diabetes by age was observed for both men and women. Prevalence rose above 0% in an earlier age group for women (age 25-34) than for men (age 35-44) but increased on a steeper gradient for men than for women.
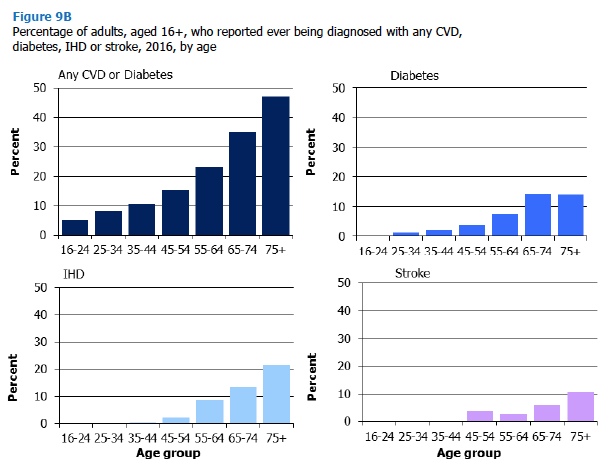
Figure 9B, Table 9.2
Any CVD or diabetes
In 2016 the overall proportion of adults reporting any CVD or diabetes was 19%. There was a significant increase in prevalence of CVD or diabetes with age (from 5% in those aged 16-24 to 47% in those aged 75 and over).
There were no significant differences between men (19%) and women (18%) in the overall prevalence of any CVD or diabetes.
The positive association between any CVD or doctor-diagnosed diabetes and age was observed for both men and women. Prevalence in those aged 16-24 was 5% for both men and women and rose steadily to 48% for men aged 75 and over and 46% for women aged 75 and over.
IHD
The prevalence of IHD diagnosis for all adults was 5% in 2016, with no adults reporting IHD until reaching the 35-44 age group (less than 1%). Prevalence then increased steadily with age, with 21% of adults aged 75 and over reporting an IHD diagnosis. The same age effect was apparent in both men and women, with younger age groups reporting significantly less IHD than older age groups.
There was a significant difference in IHD prevalence between men and women, with 7% of men reporting IHD compared with 4% of women. This difference between men and women can be accounted for the by the significantly lower prevalence levels of IHD amongst women aged 55-64 than amongst men aged 55-64 (5% for women compared with 13% for men) and significantly lower prevalence levels of IHD amongst women aged 65-74 than amongst men aged 65-74 (8% for women compared with 20% for men).
Stroke
In 2016, as in previous years[20], the proportion of all adults reporting ever having had a stroke was low (3%).
No significant difference was observed in prevalence of stroke between men and women (both 3%).
As with other CVD conditions, prevalence of stroke was positively associated with age for all adults (rising from less than 1% amongst 16-44 year olds to 10% amongst those aged 75 and over. A similar pattern was observed for both men and women.
IHD or stroke
Whilst the proportion of all adults reporting IHD or stroke was low (8%) prevalence increased significantly with age (with 29% of those aged 75 and over reporting IHD or stroke compared with less than 1% of those aged 16-44).
There was a significant difference in the prevalence of IHD or stroke between men and women, with men more likely to report than women (9% compared with 6%).
For both men and women the prevalence of IHD or stroke increased significantly with age. Amongst those aged 16-44, prevalence for both sexes ranged from none to 1%. This was followed by an increase amongst those aged 45-54 to 8% for men and 4% for women before increasing steadily to those aged 75 and over (30% for men and 29% for women).
9.3.3 Any CVD, doctor-diagnosed diabetes, any CVD or diabetes, IHD, stroke, IHD or stroke (age-standardised), 2016, by deprivation and sex
In 2016 there was a relationship between area deprivation and age-standardised prevalence of any CVD, with higher prevalence in the most deprived areas (18%) compared with the least deprived areas (12%). This association was true for all cardiovascular conditions and diabetes.
The relationship between area deprivation and all cardiovascular conditions and diabetes was the same for both men and women, with higher prevalence of cardiovascular conditions in more deprived areas for both sexes.
9.3.4 Any CVD, doctor-diagnosed diabetes, any CVD or diabetes, IHD, stroke, IHD or stroke (age-standardised), 2013-2016 combined, by alcohol consumption and sex
Age-standardised prevalence of any CVD was highest amongst ex-drinkers (23%) followed by non-drinkers (18%). Those drinking at hazardous levels were least likely to report any CVD (13%). A similar pattern of highest prevalence amongst ex-drinkers (followed by non-drinkers) and lowest prevalence amongst those drinking at hazardous level was found for all cardiovascular conditions and diabetes apart from stroke. For stroke, prevalence was the same for non-drinkers and those drinking at hazardous and harmful levels (3%).
There were some differences in prevalence between men and women. For men, the pattern of highest prevalence amongst ex-drinkers followed by non-drinkers and lowest prevalence amongst those drinking at hazardous levels was found across all cardiovascular conditions and diabetes. For women some different patterns emerged, for example, for any CVD, among women prevalence was highest for ex-drinkers (22%) followed by those drinking at a harmful level (18%) and for stroke, among women prevalence was highest for ex-drinkers and those drinking at a harmful level (5%).
These data should be interpreted with caution. Prevalence of CVD conditions and diabetes are much higher in older age groups and an individual’s drinking habits can change over time. In particular, the decision to stop drinking or reduce consumption levels could be influenced by the onset of a condition and consequent medical advice.
9.3.5 Any CVD, doctor-diagnosed diabetes, any CVD or diabetes, IHD, stroke, IHD or stroke (age-standardised), 2016, by smoking status and sex
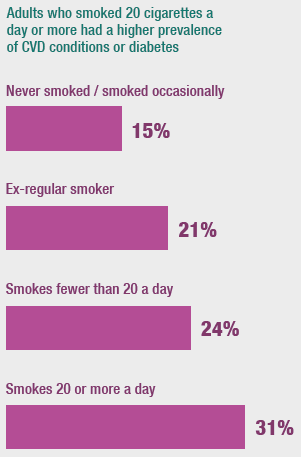
The prevalence of any CVD was lowest amongst those who had never or occasionally smoked (11%) and highest amongst those who smoked 20 or more cigarettes a day (26%).
Similar patterns were observed for any CVD or diabetes (rising from 15% to 31%), stroke (rising from 2% to 12%) and IHD or stroke (rising from 5% to 15%).
Although doctor-diagnosed diabetes prevalence appears to increase with smoking status, this finding was not statistically significant. Also, no statistically significant association was found between IHD and smoking status.
Similar relationships between smoking status and cardiovascular diagnoses were observed in both men and women.
9.3.6 Any CVD, doctor-diagnosed diabetes, any CVD or diabetes, IHD, stroke, IHD or stroke (age-standardised), 2016, by BMI and sex
In 2016 the prevalence of most cardiovascular disease and diabetes was significantly associated with BMI. Prevalence of diabetes, any CVD or diabetes, IHD and IHD or stroke was significantly higher among adults that were obese compared with adults that were underweight or normal weight.
Prevalence of any CVD (excluding diabetes) was significantly higher among adults that were obese compared with adults that were overweight but was not significantly different to adults that were underweight or normal weight.
Prevalence of stroke was not significantly associated with BMI; prevalence was 3% for both the underweight/normal weight group and the obese group.
Similar patterns were observed for men and women.
Contact
Email: Julie Landsberg, Julie Landsberg
Phone: 0300 244 4000 – Central Enquiry Unit
The Scottish Government
St Andrew's House
Regent Road
Edinburgh
EH1 3DG
