Scottish Health Survey 2014 - volume 1: main report
Presents results for the Scottish Health Survey 2014, providing information on the health and factors relating to health of people living in Scotland.
7 RESPIRATORY HEALTH
Hayley Lepps
SUMMARY
Asthma diagnoses and wheezing symptoms
- In 2014, the reported lifetime prevalence of doctor-diagnosed asthma was 17% for adults aged 16 and over, an increase from 13% in 2003. Prevalence for children aged 0-15 was 11%, a decrease from 16% in 2003.
- Wheezing in the past 12 months was reported by 18% of adults and 12% of children in 2014, with higher prevalence of wheezing at any point in the past (30% of adults and 22% of children).
- Wheezing symptoms in adults were significantly associated with the Scottish Index of Multiple Deprivation (SIMD), with prevalence increasing as area deprivation increased. In the least deprived areas, 12% of adults had wheezed in the last 12 months, and 26% had ever wheezed. In the most deprived areas these figures were 26% and 36% respectively.
- Asthma diagnoses were not associated with deprivation (between 16 and 20% in each deprivation quintile).
- Smoking status was associated with asthma among women and with wheezing symptoms for both sexes. Asthma prevalence was 33% among women who smoked 20 or more cigarettes a day, compared with 16-17% of never or ex-smokers.
- Wheezing in the past twelve months was almost four times higher, and ever wheezing was twice as high, in smokers of 20 or more cigarettes a day compared with never or ex-occasional smokers.
Chronic Obstructive Pulmonary Disease (COPD)
- In 2014, 4% of adults aged 16 and over had doctor-diagnosed COPD. This figure has not changed significantly since 2008.
- COPD increased markedly with age, from 0-1% in the 16-44 age group, to 10% of those aged 75 and over. COPD prevalence was higher among women than men, particularly so in the 65-74 age group.
- COPD prevalence was 2% in the two least deprived SIMD quintiles compared with 8% in the most deprived.
- Just 1% of never or ex-occasional smokers reported COPD. This rose to 8% in men, and 17% in women, who smoked 20 or more cigarettes a day.
- In 2012/2013/2014, 69% of adults with COPD said they had received treatment or advice for their condition (67% of men, 71% of women).
- The most commonly reported treatments / advice were: medication (66%), check-ups (59%), immunisations (34%) and stop-smoking advice (21%).
Phlegm and breathlessness
- In 2012/2014, 10% of adults aged 16 and over reported phlegm production on most days (for at least three months a year), and 23% reported breathlessness either when hurrying or going uphill, or when walking on level ground (a more severe form of symptoms). These figures have not changed significantly since 2003.
- As previously reported, phlegm production was more common in men than women while the reverse was true for breathlessness. Both sets of symptoms increased with age.
- Men's phlegm production has declined since 2003, but with no recent significant changes, while the trend for women has been stable since 2003.
- Phlegm production increased with deprivation, from 6% in the least deprived areas to 16% in the most. The equivalent figures for breathlessness were 14% and 35%, respectively.
- Phlegm production and breathlessness were more common among smokers than non-smokers. Among smokers, higher levels of both symptoms were reported by smokers of 20 or more cigarettes a day than by smokers of fewer than 20 a day.
7.1 INTRODUCTION
Long-term respiratory conditions such as asthma and Chronic Obstructive Pulmonary Disease (COPD) represent a significant challenge for the individuals that live with them, and for health services. Both these conditions are, at present, incurable, and both are thought to be widely underdiagnosed.[1],[2]
The UK has one of the world's highest rates of asthma,[3] an illness characterised by variable and recurring symptoms of breathlessness, wheezing, coughing and chest tightness. It is estimated that 368,000 people in Scotland are currently receiving treatment for asthma, 72,000 of whom are children.[4]
The reasons for the high prevalence of asthma in the UK are not clear, with the existence of the condition being associated with genetic factors, as well as environmental pollutants, including maternal smoking during pregnancy.[5] Factors associated with the onset of asthma attacks are wide ranging and include exposure to house dust mites, pollen, animals, specific foods, viral infections, moulds, fungi, environmental tobacco smoke,[6] and air pollution.[7] Occupational exposures account for a substantial proportion of adult asthma incidence.[8] In many cases, asthma does not significantly affect quality of life when it is properly controlled.[9] The economic burden on the NHS in Scotland is estimated to be around £100 million a year, most of which is accounted for by prescription costs.[10]
COPD is a much rarer chronic and irreversible lung condition caused by restricted airways resulting in breathing difficulties, persistent coughing and abnormal sputum production.[11] The breathing restrictions associated with COPD are a major cause of repeated hospital admissions in Scotland.[12] Estimates suggest that treating COPD also costs the NHS in Scotland around £100 million a year.[12]12
Like asthma, the risk of COPD is increased by exposure to environmental pollutants and smoking. However, the role played by smoking is far greater in the case of COPD than asthma. While asthma often appears in childhood or adolescence, COPD onset occurs in middle to late adulthood (though early life experiences, including childhood asthma, can increase its risk).[13],[14]
7.1.1 Policy background
One of the Scottish Government's National Performance Framework National Outcomes is for people in Scotland to 'live longer, healthier lives'.[15] There is also a National Performance Indicator to 'reduce premature mortality' (deaths from all causes in those aged under 75).[16] COPD is a major cause of death in Scotland, hence COPD prevention and better symptom management contributes to reducing premature mortality.[12]12 In addition, a number of the National Indicators[17] and many of the major public health initiatives that have been introduced in recent years are linked to key respiratory disease risk factors, most notably smoking,[18] but also physical activity[19] and obesity.[20]
Both asthma and COPD are included in the Quality and Outcomes Framework used to measure general practice performance, though only COPD has an associated outcome measure (newly introduced in 2013/14 relating to the measurement of oxygen saturation values).[21]
7.1.2 Reporting on respiratory conditions and symptoms in the Scottish Health Survey (SHeS)
The Scottish Health Survey (SHeS) is an important source of information on the self-reported prevalence of asthma and COPD in Scotland. In addition, it collects information about respiratory symptoms such as phlegm production, wheezing and breathlessness, many of which are experienced by people without a diagnosed respiratory condition. It also provides valuable information on the patterning of these conditions and symptoms across different groups in society. In this chapter trends in adults' self-reported doctor-diagnosed asthma and COPD prevalence, and respiratory symptoms (wheezing, phlegm and breathlessness) are provided. Children's asthma diagnoses and wheezing symptoms are also reported (no other results for children are presented beyond trends). Supplementary tables are also available on the Scottish Government SHeS website.[22]
7.2 METHODS
7.2.1 Asthma and COPD diagnoses
Participants (including parents of children aged 0-12, and children themselves aged 13-15) were asked if a doctor had ever told them they had asthma. This question was asked in the 1998, 2003, 2008 and 2010 surveys, and has been included every year since 2012. Annually since 2008, adult participants have also been asked if they had ever had COPD, chronic bronchitis or emphysema, and if so, whether a doctor had told them they had one of these conditions. Those who reported doctor-diagnosed COPD were also asked what treatment or advice they had received. No objective measures were used to confirm these self-reported diagnoses.
7.2.2 Respiratory symptoms
Questions on respiratory symptoms were included in the 1995-2003 surveys, and in all even years since 2008. The symptoms covered were: phlegm production, breathlessness and wheezing or whistling in the chest. Breathlessness was classified as grade 2 if it occurred when hurrying on level ground or walking up a slight hill, or grade 3 (the more severe form), if it occurred when walking with other people of the same age on level ground. The impact of such symptoms on sleep and people's daily activities was also measured. The MRC Respiratory Symptom Questionnaire was used to collect some of this information.[23]
In this chapter, wheezing symptoms (for adults and children) are reported alongside the data on asthma diagnoses. The results for adult phlegm and breathlessness symptoms are presented in a separate section, and use the combined 2012/2014 data to increase the number of cases available for analysis.
7.3 DOCTOR-DIAGNOSED ASTHMA AND SELF-REPORTED WHEEZING
This section looks at the reported lifetime prevalence of doctor-diagnosed asthma, wheezing or whistling in the chest in the last 12 months (referred to in the text as wheezing in the last 12 months), and lifetime wheezing. Trend data are presented for all adults aged 16 and above from 2003, and for adults aged 16-74 from 1998. Data are also presented for all children, aged 0-15, from 2003, and for children aged 2-15 from 1998. As these questions were only asked of sub-samples in 2008 and 2010, data for those years have been combined.
7.3.1 Trends in asthma and wheezing prevalence since 1998
Adults
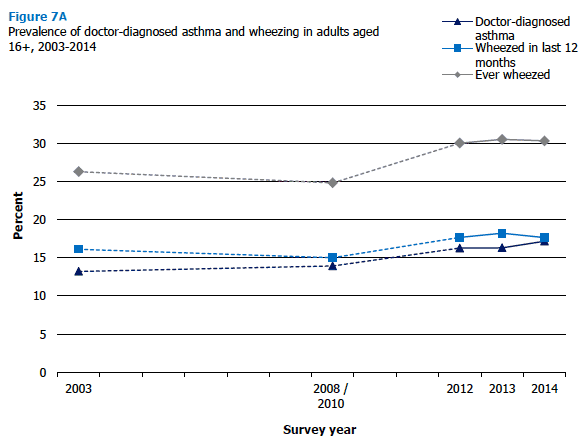
Lifetime asthma prevalence in adults aged 16 and above increased from 13% in 2003 to 17% in 2014, with no significant change since 2012. Figures for those aged 16-74 show that the upward trend started earlier (11% in 1998, 13% in 2003, and 18% in 2014).
The prevalence of wheezing in the last 12 months among all adults has been stable at 18% since 2012, slightly higher than in the years 2008/2010 combined (15%) and not significantly different from the 16% in 2003. Figures for adults aged 16-74 show the same pattern as for all adults, with no change in the earlier survey years.
The prevalence of ever having wheezed followed a similar pattern; it remained at 25-26% from 2003 to 2008/2010 combined, and has been a little higher, at 30-31%, since 2012 (30% in 2014). Again, the trend for adults aged 16-74 was very similar to that for all adults.
The separate figures for men and women followed the same patterns as those for all adults, for all three conditions reported. Figure 7A, Table 7.1
Children
Table 7.1 also shows trends in the prevalence of lifetime asthma diagnoses and wheezing symptoms in children. In 2014, 11% of children aged 0-15 had a diagnosis of asthma, while 12% of children aged 0-15 had wheezed in the past twelve months and 22% had ever wheezed. The small differences between boys and girls were not statistically significant.
The 2014 figure for asthma in all children (11%) is in line with those since 2008/2010, and confirms the pattern of a decline between since 2003, when 16% of children had a diagnosis of asthma. The prevalence of wheezing symptoms in children has been largely stable since 2003. Table 7.1
7.3.2 Asthma and wheezing prevalence in adults in 2014, by age and sex
The lifetime prevalence of doctor-diagnosed asthma in adults aged 16 and over in 2014 was 17% (16% for men, 18% for women). Wheezing in the last 12 months was reported by 18% of men and women, while ever wheezing prevalence was higher at 30% (31% for men, 30% for women).
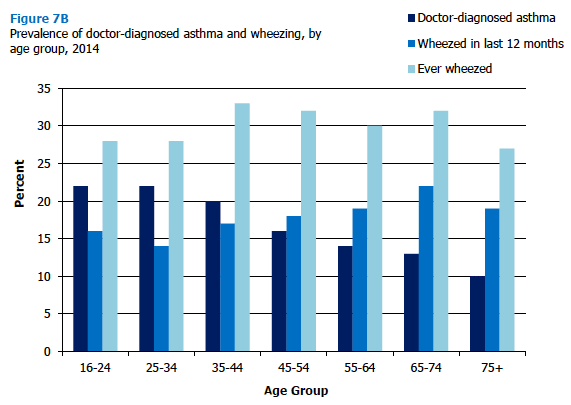
Asthma was more prevalent in the younger age groups; 20-22% for those aged 16-44 compared with 13-16% for those aged 45-74, and 10% for those aged 75 and over. In contrast, differences in wheezing in the last 12 months were much smaller overall, and a little more prevalent in the older age groups (14-17% of those aged 16-44 reported recent wheezing compared with 18-22% for those aged 45 and over). Prevalence of ever wheezing was reasonably stable across all age groups (27-33%) with no clear patterns. The separate overall figures for men and women were generally similar for all three conditions reported. Figure 7B, Table 7.2
7.3.3 Asthma and wheezing prevalence in 2014, by area deprivation
Area deprivation was measured using the Scottish Index of Multiple Deprivation (SIMD), grouped into quintiles. To ensure that the comparisons presented by SIMD are not confounded by the different age profiles of the sub-groups, the figures reported in Table 7.3 (and all other SIMD tables reported below) have been age-standardised (age‑standardisation is described in the Glossary).
Although lifetime doctor-diagnosed asthma prevalence varied somewhat by SIMD quintile (more so for women than men), it was not statistically significant. In contrast, wheezing in the last 12 months was significantly associated with area deprivation with prevalence increasing from 12% in the least deprived quintile to 26% in the most deprived. The pattern was the same for men and women. Prevalence of ever wheezing was associated with deprivation in the same way, with prevalence lowest in the least deprived quintile (26%) and highest in the most deprived (36%). Again, the pattern was the same for men and women. Table 7.3
7.3.4 Asthma and wheezing prevalence in 2014, by smoking status
To ensure that the comparisons presented by smoking status are not confounded by the different age profiles of the sub-groups, the figures reported in Table 7.4 (and all other smoking status tables reported below) have been age-standardised (as noted, age-standardisation is described in the Glossary).
Smoking status was significantly associated with asthma diagnoses and wheezing symptoms, but with different patterns evident for these conditions. The age-standardised lifetime prevalence of doctor-diagnosed asthma was 16% for never or only occasional ex-smokers, 19% for ex-regular smokers, and 18% for current smokers of fewer than 20 cigarettes a day, compared with 26% for smokers of 20 or more a day. However, this difference was largely due to big differences among women, for whom asthma prevalence was as high as 33% in smokers of 20 or more cigarettes a day, but ranged from 16-21% for all other smoking status groups. In contrast, asthma prevalence was 15-22% for men across the smoking status groups.
Both measures of wheezing (ever or in the last 12 months) showed an increase in prevalence across the four smoking status groups, for both men and women. For example, the age-standardised prevalence of wheezing in the last 12 months was 11% in those who have never smoked, 20% in ex-regular smokers, 28% in smokers of fewer than 20 cigarettes a day, and 41% in smokers of 20 or more cigarettes a day. Prevalence of ever wheezing was twice as high in those who smoked 20 or more a day (49%), compared with those who have never smoked (24%). While these patterns were broadly similar for both sexes, wheezing symptoms were higher among women who smoke 20 or more a day than for their male counterparts. Table 7.4
7.4 DOCTOR-DIAGNOSED COPD
This section looks at the reported prevalence of doctor-diagnosed Chronic Obstructive Pulmonary Disease (COPD), in adults aged 16 and over.
7.4.1 Trends in COPD prevalence in adults since 2008
The prevalence of doctor-diagnosed COPD in adults aged 16 and over has been stable since 2008, ranging from 3-5% between 2008 and 2010, and remaining at 4% since 2011. In every year except 2012, women have consistently reported prevalence one percentage point higher than men. Table 7.5
7.4.2 COPD prevalence in 2014, by age and sex
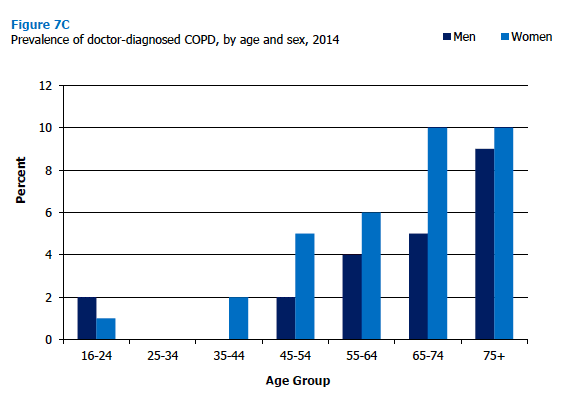
There was a strong gradient by age, with very low rates of COPD among adults aged 16-44 (0-1%), rising to 10% in adults aged 75 and over. Although this overall pattern held for both sexes, as Figure 7C illustrates, women reported higher prevalence of COPD, most notably for the 65-74 age group. Figure 7C, Table 7.6
7.4.3 COPD prevalence in 2014, by area deprivation
Doctor-diagnosed COPD was associated with area deprivation, with the lowest age-standardised prevalence (2%) found among adults in the two least deprived SIMD quintiles, and the highest prevalence (8%) in the most deprived. The pattern was broadly similar for men and women. Table 7.7
7.4.4 COPD prevalence in 2014, by smoking status
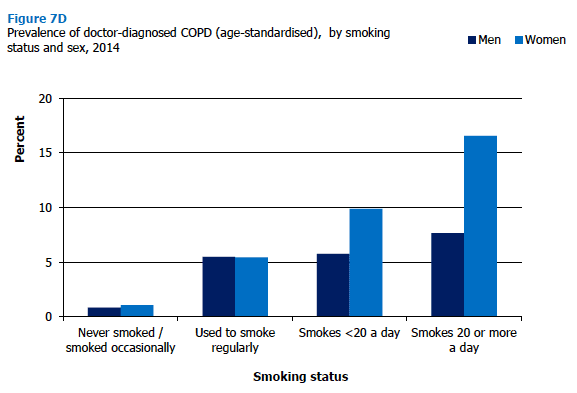
For both men and women the age-standardised prevalence of COPD was strongly associated with smoking status, though the pattern was more pronounced for women. Doctor-diagnosed CPD was reported by 1% of adults who had never smoked (at all or regularly). Prevalence increased to 5% for ex-regular smokers and 8% for current smokers of fewer than 20 cigarettes a day. COPD prevalence then increased to 12% among smokers of more than 20 cigarettes a day. As Figure 7D illustrates, the figures for women who smoked fewer than 20 cigarettes a day were almost twice as high as the figures for men who smoked an equivalent amount (10% compared with 6%). The same pattern applies to those who smoked 20 or more a day (17% for women, compared with 8% for men). Figure 7D, Table 7.8
7.4.5 COPD treatment and advice in 2012/2013/2014
To increase the sample size available, the detailed analysis of COPD treatment and advice uses data from the 2012, 2013 and 2014 surveys combined. Table 7.9 presents the overall levels of treatment and advice reported by adults with COPD, as well as the specific types they mentioned, for those aged 16-64, and 65 and over. Seven out of ten (69%) adults with COPD said they had received treatment / advice for their condition (67% of men and 71% of women). Treatment / advice varied by age, with 63% of those aged 16-64 saying they had received this, compared with 76% of those aged 65 and over. This difference was largely driven by men's experiences, as women with COPD reported similar treatment / advice levels in both age-groups (70% of those aged 16-64; 73% of those aged 65 and over). In contrast, among men with COPD, 53% of those aged 16-64 reported receiving treatment / advice compared with 82% of those aged 65 and over.
The most frequently reported forms of treatment / advice for doctor-diagnosed COPD were: medication (tablets / inhalers) at 66%; regular check-ups with GP / hospital / clinic at 59%; immunisations against flu / pneumococcus at 34%, and advice or treatment to stop smoking at 21%. With the exception of smoking advice, the most common treatments tended to be mentioned more often by those aged 65 and over compared with those aged 16-64. The largest gaps in terms of percentage points between the older and younger age groups were for regular check-ups (69% and 51%, respectively) and medication (73% and 58%, respectively). Reflecting the overall patterns for men and women described above, much larger differences in treatment / advice by age were evident for men than for women. Table 7.9
7.5 PHLEGM PRODUCTION AND BREATHLESSNESS
This section looks at the reported prevalence of the MRC Respiratory Symptom Questionnaire symptoms of phlegm production and breathlessness. Trends from 1995 onwards are reported for adults aged 16-64, while trends from 2003 are based on adults aged 16 and over. Data from the 2008 and 2010 surveys have been combined, as have data from 2012 and 2014, with earlier data representing single years only.
7.5.1 Trends in phlegm production and breathlessness in adults since 1995
Between 2003 and 2012/2014 there was a small decline in the proportion of men who reported producing phlegm from their chest on most days for at least three months of the year (14% in 2003 and 11% in 2012/2014). Prevalence for women and for all adults did not change significantly over the same time period (9% of women and 10% of all adults reported this type of phlegm production in 2012/2014). These patterns for both men and women were also shown in the longer trend going back to 1995 for adults aged 16-64.
The prevalence among all adults of any reported breathlessness (grades 2 and 3 combined) did not change significantly between 2003 and 2012/2014 (24% in 2003 and 23% in 2012/2014), although there was a small decrease in the prevalence of milder forms of breathlessness (grade 2) (13% in 2003 and 11% in 2012/2014). These patterns were also apparent for men, but there were no significant changes for women, who had higher prevalence of breathlessness. The longer trend for adults aged 16-64 showed a fall in levels of grade 2 breathlessness, for both men and women, from 17% of all adults aged 16-64 in 1995 to 9% in 2012/2014, while levels of grade 3 breathlessness remained fairly constant (8-9%). Table 7.10
7.5.2 Phlegm production and breathlessness in 2012/2014, by age and sex
Using combined 2012/2014 data, 10% of adults aged 16 and over reported phlegm production on most days (for at least three months a year), and 23% reported any breathlessness (grades 2 and 3 combined). Men were more likely than women to report producing phlegm from their chest (11% compared with 9%), whereas women were more likely than men to report breathlessness (26% compared with 19%). Prevalence increased with age for both phlegm production (from 5% for those aged 16-24, to 15% for those aged 75 and over) and breathlessness (8% and 45%, respectively). Table 7.11
7.5.3 Phlegm production and breathlessness in 2012/2014, by area deprivation
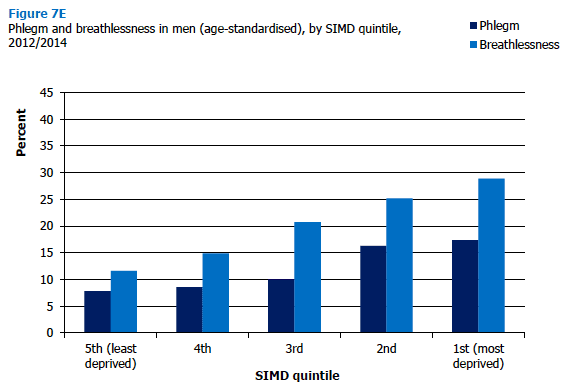
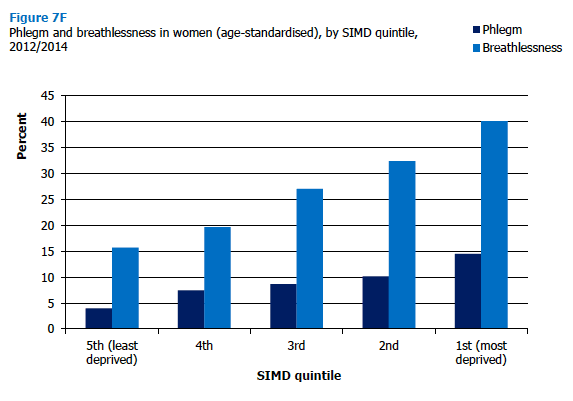
Phlegm production and breathlessness also increased by level of deprivation (using age-standardised and 2012/2014 combined figures). Reported phlegm increased from 6% in the least deprived SIMD quintile to 16% in the most deprived, while the equivalent figures for reported breathlessness showed an even bigger absolute increase, from 14% to 35%, respectively. These patterns were the same for men and women, although as Figures 7E and 7F illustrate, the absolute difference was greater for women reporting breathlessness, with 40% of women in the most deprived quintile reporting this symptom compared with 29% of men in similarly deprived areas. Figure 7E, Figure 7F, Table 7.12
7.5.4 Phlegm production and breathlessness in 2012/2014, by smoking status
Both phlegm production and breathlessness were associated with smoking status (these figures have been age-standardised and use combined 2012/2014 data). The prevalence of phlegm increased from 5-8% for non or ex-smokers, to 34% for those who smoked 20 or more cigarettes a day, while reported breathlessness increased steadily across each group, from 17% for those who have never smoked (regularly or at all) to 41% for those who smoke 20 or more cigarettes a day.
Reported phlegm figures were very similar for men and women across all smoking groups, with the exception of smokers of fewer than 20 cigarettes a day (23% for men, 16% for women). In contrast, prevalence of breathlessness was higher for women than men in each group, with the widest gap found among smokers of 20 or more a day (age-standardised prevalence of 36% for men compared with 48% for women). Table 7.13
Contact
Email: Julie Landsberg