Scottish Health Survey 2014 - volume 1: main report
Presents results for the Scottish Health Survey 2014, providing information on the health and factors relating to health of people living in Scotland.
4 DIET
Stephen Hinchliffe
SUMMARY
Fruit and vegetable consumption in adults
- Adults consumed an average of 3.1 portions of fruit and vegetables a day in 2014, the same amount as in 2003.
- Only one in five adults (20%) met the 5-a-day recommendations, while one in ten (10%) did not consume any fruit or vegetables.
- Similar amounts of fruit (1.5 portions) and vegetables (1.4 portions) were consumed per day, plus 0.3 portions a day of fruit juice.
- Women consumed slightly more fruit and vegetables (including fruit juice) than men (3.2 portions a day on average, compared with 3.0 portions for men).
- Younger adults tended to eat less fruit than older people, but similar amounts of vegetables.
Fruit and vegetable consumption in children
- Consumption of fruit and vegetables by children has changed little since 2003.
- In 2014, 14% of children aged 2-15 met the 5-a-day recommendations.
- Children aged 2-15 ate an average of 2.8 portions of fruit and vegetables a day, comprising 1.5 portions of fruit, 0.9 of vegetables, and 0.4 of fruit juice.
- The total number of portions of fruit and vegetables (including fruit juice) consumed did not vary by either age or sex, although younger children did eat more fruit and fewer vegetables than older children. Those aged 2-7 ate an average of 1.7 portions of fruit and 0.8 portions of vegetables, while those aged 11-15 ate 1.2 portions of fruit and 1.0-1.1 portions of vegetables.
Consumption of other foods in adults
- Adults' consumption of other foods, including meat and fish, milk, foods rich in starch and fibre, and foods high in sugar and / or fat, showed very little change between 2008 and 2014, with most measures remaining static.
- Red meat was the only food showing change from 2008 to 2014, where there was a small decrease in the proportion of adults consuming this more than once a week (61% in 2008, 56% in 2014).
- In 2014, a higher proportion of women than men ate oily fish (27% women, 23% men) and tuna fish (30% women, 25% men) at least once a week.
- More men than women ate red meat (61% men, 51% women) or processed meat (37% men, 20% women) twice or more per week.
- Men tended to eat more foods high in fat and / or sugar than women did, particularly chips (37% of men and 25% of women ate chips at least twice a week).
4.1 INTRODUCTION
4.1.1 Diet and health
An individual's diet is one of the contributory factors to health over which they have a degree of control. The risk of many non-communicable diseases, including cardiovascular disease, type 2 diabetes and certain types of cancer is affected by the foods people consume. Estimates from international comparisons have suggested that around 30% of cases of cancer[1] and cardiovascular disease[2] worldwide could be prevented by changes in diet, both through improvements in nutritional content and reductions in body mass.[3]
Early research on diet and chronic diseases focussed on the possible role of fat, particularly saturated fat, and fruit and vegetable intake. Some recent studies have questioned the consideration of fruit and vegetables together, and shown, for example, that vegetable consumption is more important than fruit consumption in explaining reduced risks of certain types of breast cancer,[4] stroke,[5] and diabetes,[6] while reduced risk of coronary heart disease in women,[5]5 and oesophagal and stomach cancers[7] are better explained by levels of fruit consumption.
Other aspects of diet, including the potentially positive effects of fibre and wholegrains[8], oily fish intake[9],[10] and antioxidant vitamin[11] have been studied in relation to cardiovascular disease and cognitive decline in later life. Folates have been shown to have a role in the prevention of neural tube defects;[12] vitamin D and calcium are determinants of bone health;[13] sugar intake is associated wtih dental decay;[14] and salt intake is linked to the development of hypertension.[15] A link between consumption of red and processed meats in bowel disease has been proposed,[16],[17] while it has been suggested that added sugars, particularly those consumed in drinks, may have a particular role in the development of obesity and type 2 diabetes.[18]
Given the broad range of health conditions which may be influenced by diet it is difficult to estimate the economic and social costs of poor eating habits, but some examples can highlight the potential benefits of improving the diet of the population. Treatment of cardiovascular disease, including hypertension, and type 2 diabetes, represent significant costs to the NHS, as do treatment of dental decay in children and bone disease in adults. One study looking at the economic costs of risk factors for chronic disease puts poor diet as the largest burden on the NHS, ahead of overweight and obesity, smoking, alcohol consumption, and physical inactivity.[19]
Surveys of household food intake and of children's diet in Scotland have highlighted socio-economic inequalities in consumption of a wide range of food groups such as fruit and vegetables and soft drinks though differences in fat and sugar content of the diet between those in more versus less deprived areas are not marked.[20],[21],[22]
4.1.2 Policy background
The most widely promoted diet and health message has been the World Health Organisation (WHO) '5-a-day' advice for adults to consume at least five varied 80g portions of fruit and vegetables per day. In Scotland the poor record on diet was first highlighted in 1993 with the publication of the Scottish Diet report and associated Action Plan.[23],[24] The Action Plan included specific Scottish Dietary Targets for eight nutrients and food groups which would constitute a balanced diet. These were replaced in 2013 by the Scottish Dietary Goals.[25] Goals include the 5-a-day recommendation and a target to reduce salt intake from around 9g to 6g per day for adults. There is a goal in place to reduce average calorie intake by 120 kcal per day and average intake of red meat to 70g per day as well as advice to limit fat and sugar intake and increase consumption of fibre and oil-rich fish. More recently the WHO and Public Health England have proposed that added sugars should be reduced by more than half, to provide 5% of energy in the diet.[26],[27]
To tackle the poor diet in children in Scotland, the main target has been food in schools with Healthy Eating in Schools guidance on implementing the Schools Food and Nutrition legislation which prohibits the sale of foods and drinks high in fat, sugar and / or salt in schools.[28] The foods available to children who leave school at lunchtimes have also been considered in the 'Beyond the School Gate' advice to caterers in the vicinity of schools.[29]
The Scottish Government has also developed the Better Eating Better Learning guidance. This has provided refreshed guidance to a range of stakeholders (schools, local authorities, caterers, procurement departments, parents, children and young people) to support them to work in partnership to make further improvements in school food and food education.[30]
The Scottish Government has also outlined specific measures which could be taken by retailers, manufacturers and caterers which would affect the wider population in its 'Supporting Healthy Choices' framework.[31] This is a voluntary framework based on four core principles. These are to:
- Put the health of children first in food-related decisions
- Rebalance promotional activities
- Support consumers and communities
- Formulate healthier products
The Scottish Government is also funding a number of programmes aimed at encouraging people make healthier choices in the way they shop, cook and eat, through its 'Eat Better Feel Better' campaign.[32]
A key part of the Health Promoting Health Service is a focus towards the provision of healthier food choices in hospitals. All NHS-run restaurants for staff, visitors and patients now have the Healthyliving Award Plus as a mandatory requirement with all voluntary sector establishments holding the award. While maintaining this standard along with its expansion into the private sector, attention is shifting to the adoption of a comparable Healthcare Retail Standard in 2015/2016.
4.1.3 Reporting on diet in the Scottish Health Survey (SHeS)
This chapter provides information on fruit and vegetable consumption in adults and children from 2003-2014, along with data on consumption of selected foods and drinks by adults over the same period. Further tables on the trend in fruit and vegetable consumption, and in high-sugar processed foods, by area deprivation (SIMD) over time are included in Chapter 9, along with results for other eating habits for 2014, by SIMD. Supplementary tables on diet, including analysis by socio-economic classification, household income and area deprivation are also published on the Scottish Health Survey website.[33]
4.2 METHODS AND DEFINITIONS
4.2.1 Measuring fruit and vegetable consumption
The module of questions on fruit and vegetable consumption was designed with the aim of providing sufficient detail to monitor adherence to the 5-a-day recommendation. These questions have been asked of all adults (aged 16 and over) participating in the survey since 2003 and of children aged 2 to 15 since 2008.
To establish the total number of portions consumed in the 24 hours preceding the interview, the module includes questions on consumption of the following food types: vegetables (fresh, frozen or canned); salads; pulses; vegetables in composites (e.g. vegetable chilli); fruit (fresh, frozen or canned); dried fruit; fruit in composites (e.g. apple pie); and fresh fruit juice. A portion is defined as the conventional 80g of a fruit or vegetable. Since 80g is difficult to visualise, a 'portion' was described using more everyday terms, such as tablespoons, cereal bowls and slices. Examples are given in the questionnaire to aid the recall process, for instance, tablespoons of vegetables, cereal bowls full of salad, pieces of medium sized fruit (e.g. apples) or handfuls of small fruits (e.g. raspberries). In spite of this, there may be some variation between participants' interpretation of a portion. These everyday measures were converted back to 80g portions prior to analysis. The following table shows the definitions of the portion sizes used for each food item included in the survey:
| Food item | Portion size |
|---|---|
| Vegetables (fresh, frozen or canned) | 3 tablespoons |
| Pulses (dried) | 3 tablespoons |
| Salad | 1 cereal bowlful |
| Vegetables in composites, such as vegetable chilli | 3 tablespoons |
| Very large fruit, such as melon | 1 average slice |
| Large fruit, such as grapefruit | Half a fruit |
| Medium fruit, such as apples | 1 fruit |
| Small fruit, such as plums | 2 fruits |
| Very small fruit, such as blackberries | 2 average handfuls |
| Dried fruit | 1 tablespoon |
| Fruit in composites, such as stewed fruit in apple pie | 3 tablespoons |
| Frozen fruit / canned fruit | 3 tablespoons |
| Fruit juice | 1 small glass (150 ml) |
Since the 5-a-day policy stresses both volume and variety, the number of portions of fruit juice, pulses and dried fruit is capped so that no more than one portion can contribute to the total number of portions consumed. Interviewers record full or half portions, but nothing smaller.
4.2.2 Measuring consumption of other foods and drinks
The eating habits module of the interview was developed from the Dietary Instrument of Nutrition Education (DINE) questionnaire and is similar to that used in the Health Survey for England (HSE). The DINE questionnaire was developed by the Imperial Cancer Research Fund's General Practice Research Group to assess usual intake of a wide range of nutrients, including protein, starch, fat and fibre.[34] The module asks about frequency of consumption for categories of food, but does not ask about either the amount consumed or specific types of food. It cannot be used to estimate daily nutrient intake but can reflect differences in consumption of the specified foods between population and sub-groups or within a population over time. These questions are asked of all children aged 2-15 annually, and a sub-sample of adults biennially.
4.3 FRUIT AND VEGETABLE CONSUMPTION
4.3.1 Trends in adult fruit and vegetable consumption since 2003
Fruit and vegetable consumption by adults has changed very little since 2003. The mean and median number of portions eaten per day were the same in 2014 (mean 3.1, median 2.7) as they were in 2003.[35] In the years in between, these figures varied only by small amounts.
The proportion of adults meeting the 5-a-day recommendations has also remained fairly constant. In 2014, 20% of adults met or exceeded the recommended five portions, down slightly from a high of 23% in 2009, but at a similar level to the 21% in 2003.
The proportion of adults eating no fruit and vegetables has remained at between 9% and 10% each year since 2003 (10% in 2014).
Men and women's separate consumption patterns also remained fairly constant over time. In every survey year, since 2003, women's mean fruit and vegetable consumption was slightly higher than men's (a difference of between 0.1 and 0.3 portions). In 2014, women consumed a mean of 3.2 portions, while men consumed 3.0.
Similar small differences between men and women could be observed in the proportion eating no fruit and vegetables (9% of women and 12% of men in 2014). The proportion of men eating five or more portions was identical in 2008 and 2014 (20%), whereas the proportion fell among women from 24% in 2008 to 20% in 2014. Table 4.1
4.3.2 Adult fruit and vegetable consumption, by age and sex
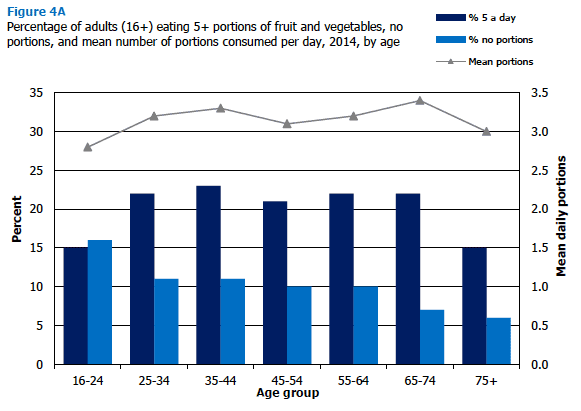
Figure 4A shows that the relationship between consumption of fruit and vegetables and age was not linear. As in previous years, in 2014 it was lowest among those aged 16-24, who consumed a mean of 2.8 portions a day, and highest among those aged 65-74 (a mean of 3.4 portions).
Variations by age in 2014, with the exception of the oldest age group, appear largely to be a result of differences in the amount of fruit consumed. Overall, adults ate similar amounts of fruit (1.5 mean portions) and vegetables (1.4 mean portions), plus 0.3 portions of fruit juice. Vegetable consumption was at a similar level for all age groups under 75 (between 1.3 and 1.5 mean portions, compared with 1.1 for those aged 75 and over); and fruit juice did not contribute greatly to overall consumption for any age group (between 0.2 and 0.4 portions). However, fruit consumption varied to a much greater extent, from a mean of 1.1 portions for those aged 16-24 to 1.8 portions for those aged 65-74.
Patterns of consumption by age for fruit and vegetables, and for fruit, vegetables and fruit juice separately, were similar for both men and women.
The youngest age group (16-24) was the most likely to have eaten no fruit or vegetables (16%, compared with 10-11% of those aged 25-64 and 6-7% of those aged 65 and over).
The youngest and the oldest age groups were also the least likely to have eaten the recommended five portions or more (15% of those aged 16‑24 and of those aged 75 and over, compared with 21-23% of those aged 25-74). Figure 4A, Table 4.2
4.3.3 Trends in child fruit and vegetable consumption since 2003
Levels of consumption of fruit and vegetables by children, like those for adults, have changed little in recent years. Trends are presented for children aged 2-15, since 2008, and 5-15 since 2003. In every year since 2008, mean consumption in the 2-15 age group was no more than 0.1 portions higher than the 5-15 age group, so to avoid unnecessary repetition and allow a longer time series, only figures for those aged 5-15 are discussed in the following paragraphs.
Mean consumption has remained almost constant since 2003, at 2.6 or 2.7 portions in every year (2.7 in 2014). The proportion eating no fruit or vegetables has also remained fairly constant, between 10% and 12% each year (11% in 2014). The proportion eating the recommended five or more portions has remained between 11% and 14% each year (14% in 2014).
Patterns for boys and girls separately were similarly both fairly constant over time, with no significant differences in consumption between boys and girls. Mean consumption varied between 2.4 and 2.7 portions for boys, and between 2.6 and 2.8 portions for girls. In 2014 it was at the upper end of these ranges for both boys (2.7) and girls (2.8). Table 4.3
4.3.4 Child fruit and vegetable consumption, by age and sex
In 2014, children aged 2-15 consumed an average of 2.8 portions of fruit and vegetables, comprising 1.5 portions of fruit, 0.9 of vegetables, and 0.4 of fruit juice.
There were no significant differences by either age or sex in the mean consumption of fruit and vegetables, but there were differences by age in the consumption of the separate components in 2014. Younger children ate more fruit: a mean of 1.7 portions a day was consumed by those aged 2-7, compared with a mean of 1.2 portions consumed by those aged 11-15. Older children tended to eat more vegetables: 1.0-1.1 portions a day for those aged 11-15, compared with 0.8 portions consumed by those aged 2-7.
Older children were more likely to consume no fruit or vegetables at all than younger children. Only 6-7% of children aged 2-7 had eaten no portions, compared with 15% of those aged 13-15.
In 2014, 14% of children aged 2-15 ate the recommended five or more portions, with no significant difference between boys and girls. However, as in Table 4.4, there were slightly different patterns by age, most notably in the higher proportion of girls aged 2-7 meeting the 5-a-day guidelines than those aged 8-15. Table 4.4
4.4 CONSUMPTION OF OTHER FOODS IN ADULTS
4.4.1 Meat and fish
The proportion of adults consuming red meat more than once a week has fallen since 2008, from 61% in 2008, to 56% in 2014. This fall in red meat consumption has been more pronounced among women (from 59% in 2008 to 51% in 2014) than among men (64% in 2008 and 61% in 2014).
Consumption of processed meat products, such as pies or sausages has not changed: 28% of adults ate these more than once a week in 2014, the same proportion as in 2008. A much higher proportion of men than women consumed meat products more than once a week (37% of men in 2014, compared with 20% of women).
The consumption of fish has not changed significantly since 2008. In 2014, around half of adults (48%) ate white fish at least once a week, a quarter (25%) ate oily fish, such as mackerel, at least once a week, and just over a quarter (28%) ate tuna fish at least once a week, with figures in 2008 almost identical (51%, 25% and 30% respectively). A higher proportion of women than men ate oily fish (27% women, 23% men) or tuna fish (30% women, 25% men) at least once a week. Table 4.5
Consumption of meat and fish also varied with age in 2012/2014. As shown in Figure 4B and 4C, older people were more likely than those in younger age groups to eat oily fish at least once a week, white fish at least once a week, and red meat more than once a week. Oily fish was eaten at least once a week by 14% of those aged 16-24, rising steadily to 33% of those aged 55-64 and 35% of those aged 65 and over. Similarly, 34-37% of those aged 16-34 ate white fish at least once a week, rising steadily to 71% of those aged 75 and over. The reverse was true for weekly (or more) tuna fish consumption and eating meat products twice weekly (or more), both of which were more common in younger people. Tuna fish consumption declined fairly steadily from 39% of those aged 16-24, to 15% of those aged 75 and over. Twice weekly (or more) consumption of meat products halved from 39% of those aged 16-24 to 19‑20% of those aged 65 and over. The pattern for consumption of red meat more than once a week was not so consistent, but there was an increase from 48% of those aged 16-24 to 61% of those aged 65 and over. Figure 4B, Figure 4C, Table 4.6
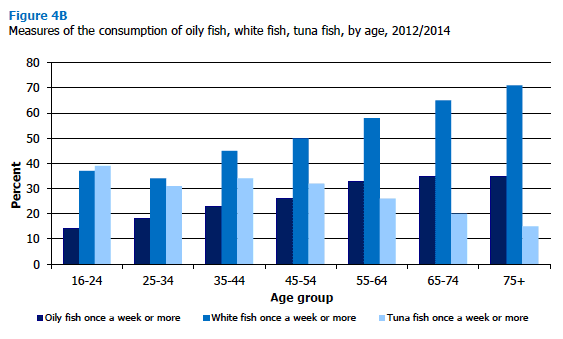
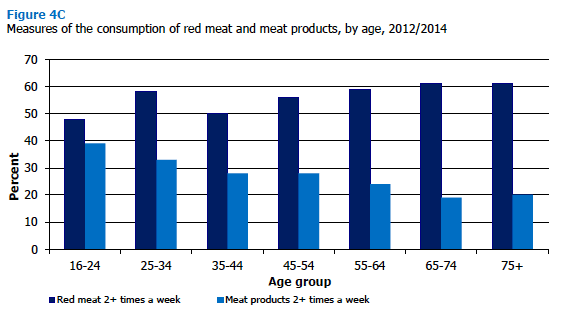
4.4.2 Milk
Three quarters of adults (74%) in 2014 consumed skimmed or semi-skimmed milk in drinks or on breakfast cereal, as opposed to whole milk, other types of milk or no milk. This proportion did not change between 2008 and 2014. Again, as in previous years, a higher proportion of women (77%) than men (71%) in 2014 consumed either skimmed or semi-skimmed milk. Table 4.5
In 2012 and 2014 (combined), 19% of adults chose whole milk most regularly, 64% chose semi-skimmed, 10% skimmed and 2% other types of milk, such as goat's or soya. Just 4% did not drink milk. Consumption of different types of milk did vary by age, but there was no clear pattern. Those aged 25-34 and those aged 75 and over were the most regular consumers of whole milk (27% and 28% respectively, compared with 16-18% in other age groups). Those aged 16-24 were the most regular consumers of semi-skimmed (71%), compared with 59-66% in other age groups. Skimmed milk was most regularly consumed by those aged between 35 and 74 (11-14%, compared with 7-8% of those aged 16-34 and 6% of those aged 75 and over). Table 4.7
4.4.3 Foods rich in starch and fibre
The consumption of foods rich in starch and fibre has not changed significantly since 2008. Half of all adults (51%) ate potatoes, pasta or rice at least five times a week in 2014. Four in ten adults (40%) ate at least 2-3 slices of high fibre bread a day. Three in ten (30%) ate high fibre and low sugar cereal at least five times a week. A greater proportion of men than women ate high fibre bread every day (43%, compared with 37%). Table 4.5
Consumption of high fibre, low sugar cereal increased steadily with age in 2012/2014, from being eaten at least five times a week by 21% of those aged 16-24 to 45% of those aged 75 and over. Consumption of high fibre bread increased from 31% for those aged 16-24 to 46% for those aged 55-64 but then plateaued at 46% and 45% for the older two age groups. Age-based consumption patterns for potatoes, rice and pasta were not so clear, although eating at least five portions a week was lowest for both men and women around the ages of 35-54 and highest for those aged 75 and over. Table 4.8
4.4.4 Foods and drinks high in fat and / or sugar
Consumption of foods and drinks that are high in fat or sugar, or both, has not changed significantly since 2008. In 2014, 34% ate cakes at least twice a week; 31% consumed biscuits at least once a day; 31% consumed chips at least twice a week; 29% ate ice cream at least once a week; 27% of adults consumed sweets or chocolates at least once a day; 27% drank non-diet soft drinks at least once a day; and 21% consumed crisps or other savoury snacks at least once a day. For all of these measures, the figures were similar in 2008.
Figure 4D shows that, with the exception of daily sweets and chocolates consumption (which was similar for men and women), the measures of consuming high sugar / fat foods mentioned above were all higher among men than women. Differences in consumption between men and women were also particularly notable for chips (37% of men ate chips at least twice a week, compared with 25% of women). Figure 4D, Table 4.5
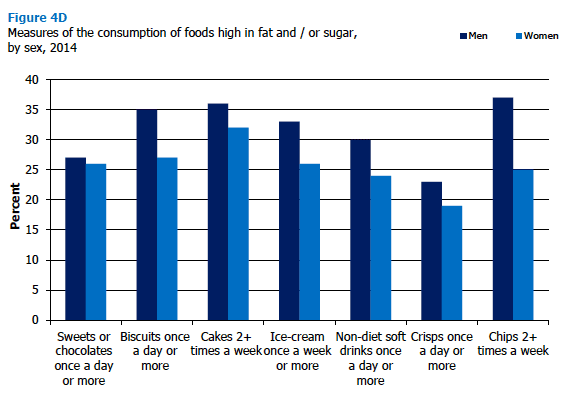
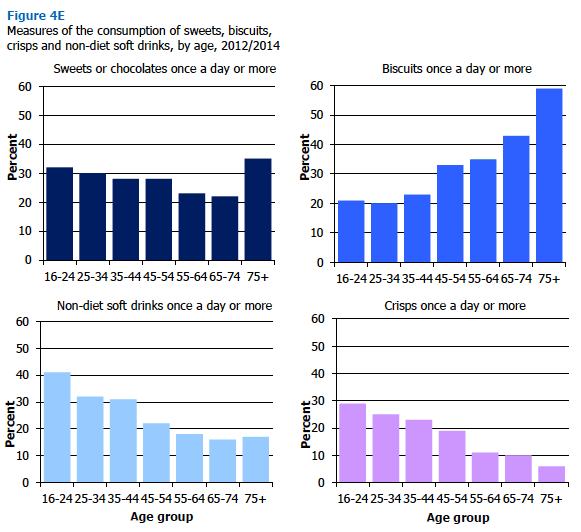
Figure 4E illustrates how consumption of sweet foods tended to be highest among the oldest age group, whereas consumption of non-diet soft drinks and savoury fatty foods decreased with age. For example, 20% of adults aged 25-34 ate biscuits every day, increasing to 59% of those aged 75 and over, and 26% of those aged 25-34 ate cakes at least twice a week, increasing to 52% of those aged 75 and over. At least weekly ice cream consumption increased from 21% of those aged 25-44 to 38% of those aged 75 and over. The pattern for daily consumption of sweets or chocolates was a little different, with a steady decrease from 32% of those aged 16-24 to 22% of those aged 65-74, and then a large jump to 35% of those aged 75 and over.
The proportion consuming non-diet soft drinks daily decreased from 41% of those aged 16-24 to 16-18% of those aged 55 and over. The proportion eating crisps daily also decreased markedly with age from 29% of those in the youngest age group to only 6% of those in the oldest group. The proportion eating chips at least twice a week showed a general downward pattern with increasing age, from 45% of those aged 16-24 to 22-28% of those aged 55 and over. Figure 4E, Table 4.9
Contact
Email: Julie Landsberg