Scottish Health Survey 2014 - volume 1: main report
Presents results for the Scottish Health Survey 2014, providing information on the health and factors relating to health of people living in Scotland.
1 GENERAL HEALTH AND MENTAL WELLBEING
Laura Brown
SUMMARY
Self-assessed general health
- In 2014, 74% of adults identified their health as 'good' or 'very good'; 8% said it was 'bad' or 'very bad'.
- Almost all (95%) children were reported to have 'good' or 'very good' health, and just 1% 'bad' or 'very bad'.
- Levels of self-assessed general health have remained fairly static since 2008, for both adults and children.
- Self-assessed health tended to decline with age, with 85% of those aged 16-24 reporting their health as 'good' or 'very good', and just 2% 'bad' or 'very bad'. By ages 75 and over, the respective figures were 53% and 15%.
- Self-assessed health also declined as levels of deprivation increased. Using age-standardised figures, 84% of adults in the least deprived areas were in good health, and 2% bad, compared with 57% in good health in the most deprived areas, and 18% in bad health.
Long-term conditions
- In 2014, 46% of adults had one or more long-term conditions (31% limiting, 15% non-limiting), with 19% of children having a long-term condition.
- The prevalence of long-term conditions increased with age, from a quarter (25%) of adults aged 16-24 to three-quarters (77%) of those aged 75 and over. Prevalence, and patterns by age, were similar for both men and women.
Wellbeing
- Levels of wellbeing in the population, as measured by the Warwick-Edinburgh Mental Wellbeing Scale (WEMWBS) have remained fairly constant since 2008 (a mean of 50.0 in both 2008 and 2014).
- Wellbeing was lowest for those aged 45-54 (a mean of 49.2), with similar levels for both men and women.
- WEMWBS mean scores were lower in more deprived areas, declining from 51.1 in the least deprived to 47.3 in the most deprived.
Mental health
- In 2014, 16% of adults exhibited signs of a possible psychiatric disorder (GHQ-12 score of four or more).
- Women were slightly more likely than men to have a high GHQ-12 score (17% four or more, compared with 14% of men).
- High GHQ-12 scores were more common among those aged 16-64 (15-19%) than those aged 65 and over (8-12%).
Life satisfaction
- On a scale of 0-10, the average level of life satisfaction for adults in 2014 was 7.8. It was highest for those aged 65 and over (8.0-8.1) and lowest for those aged 45-54 (7.5).
1.1 INTRODUCTION
This chapter covers two interrelated topics: self-assessed general health, including self-reported long-term conditions, and mental health and wellbeing. Population measures of self-reported health can be a general indicator of the burden of disease on society. It reflects subjective experiences of both diagnosed and undiagnosed illnesses, and their severity, which more objective measures for the whole population can sometimes overlook. Mental wellbeing, together with physical and social wellbeing, is one aspect of overall wellbeing. It is important as an indicator of quality of life, and reflects positive affect and mental functioning, rather than just mental ill-health. Both general health and mental wellbeing are critical measures of the population's overall health status and are key markers of health inequalities.[1]
Self-assessed general health is often a reflection on the presence or absence of long-term conditions, both physical and mental. Such conditions account for 80% of all GP consultations and for 60% of all deaths in Scotland.[2] People with a long-term condition are twice as likely as those without to be admitted to hospital and stay in hospital disproportionately longer.[3] Older people are more likely to have multiple long-term conditions. Given Scotland's ageing population (in 2012, 8% of the population were 75 and over; this is predicted to rise to 13.5% by 2037[4]), this becomes more of a public health issue. [2] The link with deprivation, lifestyle factors and wider health determinants is also of importance in Scotland given its persistent health inequalities.[2] Long-term conditions therefore represent personal, social and economic costs both to individuals and their families and to Scottish society more widely.
The World Health Organisation (WHO) considers mental wellbeing to be fundamental to their definition of health.[5] Mental disorders often co-exist with other diseases, including cancers and cardiovascular disease, and many of the risk factors covered in this report, such as obesity, excessive alcohol consumption, and low levels of physical activity, are common to both mental disorders and other non-communicable diseases.
Mental illness represents a significant public health challenge globally. Those with mental disorders have disproportionately higher disability and mortality than the general population, dying on average more than 10 years earlier.[6] Neuropsychiatric disorders are the second largest contributor to the burden of disease in Europe and mental disorders account for around 40% of all years lived with disability.[6]6 Accounting for 4.3% of the global burden of disease, depression is now the largest single cause of disability worldwide (11% of all years lived with disability globally) and is the leading chronic condition in Europe.[5],[6] Inequalities in mental health and wellbeing exist. Globally, depression is more prevalent among women than men,[5] while, throughout Europe, prevalence of most mental disorders is higher among those living in more deprived areas.[6]
1.1.1 Policy background
In recognition of the challenges posed by long-term conditions - both for the individual and their families, as well as for health and care services - the Scottish Government's National Action Plan for long-term conditions2 was published in 2009. This defined long-term conditions as 'health conditions that last a year or longer, impact on a person's life, and may require ongoing care and support'. Conditions include mental health problems and a wide range of physical conditions such as chronic pain, arthritis, inflammatory bowel disease. Delivering on a commitment made in the earlier Better Health, Better Care: Action Plan, the National Action Plan recognised the need for system-wide action in response to the challenge presented by the increasing prevalence of long-term conditions within the context of an ageing population, the links to health inequalities, and the particular challenges of multi-morbidity - the experience of two or more long-term conditions.
The Mental Health Strategy for Scotland: 2012-2015,[6] published in August 2012, sets out the Scottish Government's key commitments in relation to improving the nation's mental health and wellbeing and for ensuring improved services and outcomes for individuals and communities. The strategy includes 36 commitments, 7 key themes and 4 key change areas it will adhere to in achieving these priorities. It promotes safe, effective and person-centred health and care. In addition to focussing on improved service delivery there is also an emphasis on the actions that individuals and communities can take to maintain and improve their own health.
Examples of this approach include the Living Life Guided Self Help Service operated by NHS 24, the Steps for Stress resources managed by NHS Health Scotland, and Ginsberg - a web-based tool launched by the Scottish Government to help people manage their wellbeing in relation to other aspects of their lives. Ginsberg allows people to see patterns that are developing, to draw links between what they are doing with their time and how they are feeling, and to see the changes they can make to improve their wellbeing.
There are a number of other mental health strategies, including the Autism strategy, the Learning Disability strategy "the keys to life", the dementia strategy and the alcohol framework and road to recovery drug strategy.
Supporting the Scottish Government's overall purpose, the current strategy builds upon the work of a number of key policy documents including Delivering for Mental Health[7] (published in 2006), and Towards a Mentally Flourishing Scotland,[8] which covered the 2009-2011 period. The previous strategy was aimed at promoting good mental wellbeing; reducing the prevalence of common mental health problems, suicide and self-harm; and improving the quality of life of those experiencing mental health problems and mental illnesses.
One of the Scottish Government's National Outcomes is the overall strategic objective for health: We live longer, healthier lives.[9] This is supported by a number of National Indicators including 'improve self-assessed general health' and 'improve mental wellbeing'.[9] Data from the Scottish Health Survey (SHeS) is used to monitor progress towards both these indicators. In addition, the purpose target to improve healthy life expectancy over the 2007 to 2017 period uses SHeS data for children (aged 0-15) in the calculations used to measure progress. The fact that those with mental disorders die, on average, earlier than the general population impacts on another National Indicator; to 'reduce premature mortality'. Scotland also has a set of national, sustainable mental health indicators for adults and children, covering both outcomes and contextual factors that confer increased risks of, or protection from, poor mental health outcomes.[10] SHeS is the data source for 28 of the 54 indicators for adults[11] and over 20 of the indicators for children.[12]
There was an NHS Scotland HEAT target to reduce the suicide rate between 2002 and 2013 by 20%.[13] By 2013, the suicide rate declined by 19%, just short of the target.[13] There were additional NHS Scotland HEAT targets for specialist Child and Adolescent Mental Health Services (CAMHS), and for access to Psychological Therapies (across all ages in the population), to achieve 18 week maximum referral to treatment times.[14] In January 2015, the targets become standards in NHS Scotland Local Delivery Plans[15]. Figures for the quarter ending March 2015 show that the target was met for 79% of referrals of children and young people[16]. Figures from data still under development suggest that around 83% of patients (across all ages) starting a psychological therapy met the target during the same period.[14],[17] The Scottish Government has announced additional funding to continue to improve mental health across Scotland and ensure that people get timely access to services.
1.1.2 Reporting on general health and mental wellbeing in the Scottish Health Survey (SHeS)
This chapter updates trends in self-assessed health for both adults and children, and trends in mental wellbeing for adults. Figures are also reported for 2014 by age and sex, and by area deprivation. Prevalence of long-term conditions, mental health (as measured by the GHQ-12 questionnaire) and life satisfaction are reported for different age groups in 2014.
1.2 Methods and definitions
1.2.1 Self-assessed general health
Each year participants aged 13 and over are asked to rate their health in general with possible answer options ranging from 'very good' to 'very bad'. For children under the age of 13 the question is answered by the parent or guardian completing the interview on their behalf. This question is used to monitor the National Indicator 'improve self-assessed health,' while the data on children is used in the calculation of healthy life expectancy used to monitor the purpose target on this. It is also included in both the adult and child mental health indicators sets.10
1.2.2 Self-reported long-term conditions
All participants were asked if they had any physical or mental health condition or illness lasting - or likely to last - for twelve months or more. Those who reported having such a condition were asked to provide details of the type(s) of conditions or illnesses reported. Answers were recorded verbatim and then coded in the office. Those reporting a condition were also asked if it limited their daily activities a lot, a little, or not at all. This enabled conditions to be classified as either 'limiting' or 'non-limiting'. These questions did not specify that conditions had to be doctor-diagnosed; responses were thus based on individuals' perceptions.
1.2.3 Warwick-Edinburgh Mental Wellbeing Scale (WEMWBS)
Wellbeing is measured using the WEMWBS questionnaire. It has 14 items designed to assess: positive affect (optimism, cheerfulness, relaxation) and satisfying interpersonal relationships and positive functioning (energy, clear thinking, self-acceptance, personal development, mastery and autonomy).[18] The scale uses positively worded statements with a five-item scale ranging from '1 - none of the time' to '5 - all of the time'. The lowest score possible is therefore 14 and the highest score possible is 70; the tables present mean scores.
The scale was not designed to identify individuals with exceptionally high or low levels of positive mental health so cut off points have not been developed.[19] The scale was designed for use in English speaking populations, however in a very small number of cases, the questions were translated to enable the participation of people who did not speak English.[20]
WEMWBS is used to monitor the National Indicator 'improve mental wellbeing'.[9] It is also part of the Scottish Government's adult mental health indicator set, and the mean score for parents of children aged 15 years and under on WEMWBS is included in the mental health indicator set for children.[10]
1.2.4 GHQ-12
GHQ-12[21] is a widely used standard measure of mental distress and psychological ill-health consisting of 12 questions on concentration abilities, sleeping patterns, self-esteem, stress, despair, depression, and confidence in the previous few weeks. Responses to each of the GHQ-12 items are scored, with one point allocated each time a particular feeling or type of behaviour is reported to have been experienced 'more than usual' or 'much more than usual' over the previous few weeks. These scores are combined to create an overall score of between zero and twelve. A score of four or more (referred to as a high GHQ-12 score) has been used here to indicate the presence of a possible psychiatric disorder. A score of zero on the GHQ-12 questionnaire can, in contrast, be considered to be an indicator of psychological wellbeing. GHQ-12 measures deviations from people's usual functioning in the previous few weeks and therefore cannot be used to detect chronic conditions.
1.2.5 Life satisfaction
Life satisfaction is measured by asking participants to rate, on a scale of 0 to 10, how satisfied they are with their life in general. On the scale, 0 represented 'extremely dissatisfied' and 10 'extremely satisfied' (the intervening scale points were numbered but not labelled). This measure has been used in numerous international surveys. There are no pre-defined cut-off points within the scale to distinguish between different levels of satisfaction. However, a summary measure was used in this analysis which identified three groups of interest based on the overall distribution of scores in the whole population: people with the highest levels of satisfaction (scores of 9 or 10), people with an average satisfaction level (score 8), and those with below average scores (0-7).
1.3 SELF-ASSESSED GENERAL HEALTH AND MENTAL WELLBEING
1.3.1 Trends in self-assessed general health since 2008
Table 1.1 reports trends in self-assessed general health for adults (aged 16 and over) and children (aged 0-15). Since 2008 the self-assessed general health of adults (aged 16 and over) has remained largely unchanged. Over this period, the proportion of adults reporting their general health as 'good' or 'very good' has fluctuated between 74% and 77% (staying at 74% for the past three years). Likewise, the proportion of adults describing their general health as 'bad' or 'very bad' has changed very little (7-9%, in all years, 8% in 2014).
Levels of self-assessed general health have been relatively stable for both men and women over time. However, there has been a slight decline in the proportion of men describing their health as 'good' or 'very good' (from 77% in 2011 to 74% in 2014).
The proportion of children (aged 0-15) reported to have 'good' or 'very good' health has also remained relatively constant since 2008 (at 94-96%). In 2014, 95% of children had 'good' or 'very good' health (the same as in 2013). The proportion of children with 'very good' health has shown some variation over time (from 65-70%), but this was largely due to a peak in 2011, as the remaining years' figures were more similar (65-68%). Since 2008 the proportion of children reporting 'bad' or 'very bad' general health has remained consistently low, at 1% or less. Table 1.1
1.3.2 Self-assessed general health among adults in 2014, by age and sex
In 2014, 32% of adults (aged 16 and over) assessed their general health as 'very good', 41% as 'good' and 18% as 'fair'. In addition, 6% said it was 'bad' and 2% that it was 'very bad'. Men's and women's self-assessed health were not significantly different.
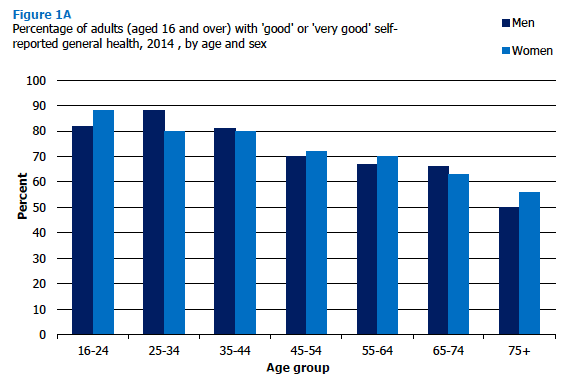
The age-related patterns in self-assessed health in 2014 were similar to those presented in previous SHeS reports.[22] Levels of 'good' or 'very good' self-assessed health decreased as age increased (from 84-85% among adults aged 16-34, to 53% of those aged 75 and over). Conversely, self-reported 'bad' or 'very bad' health increased with age (from 2% for adults aged 16-24, to 15% of adults aged 75 and over).
These age-related patterns were true for both men and women. Figure 1A, Table 1.2
1.3.3 Self-assessed general health among adults in 2014, by area deprivation and sex
Area deprivation was measured using the Scottish Index of Multiple Deprivation (SIMD), grouped into quintiles. To ensure that the comparisons presented by SIMD are not confounded by the different age profiles of the sub-groups, the figures reported in Table 1.3 (and all other SIMD tables reported below) have been age-standardised (age-standardisation is described in the Glossary).
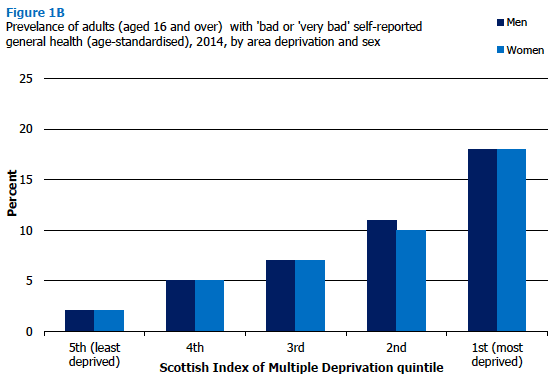
In 2014, self-assessed general health was significantly associated with area deprivation. Adults (aged 16 and over) living in the least deprived areas had the highest levels of 'good' or 'very good' self-assessed health (84%), and this declined successively across the quintiles to 57% among those in the most deprived areas. The opposite was true for 'bad' or 'very bad' health, which increased from 2% among adults living in the least deprived areas, to 18% for adults living in the most deprived areas. These patterns were true for both men and women. Figure 1B, Table 1.3
1.3.4 Prevalence of long-term conditions in 2014, by age and sex
Adults
In 2014, 46% of adults (aged 16 and over) had at least one long-term condition. This figure was comprised of 31% who had one or more limiting conditions, and 15% with only non-limiting conditions. The prevalence of long-term conditions was the same for both men and women.
As noted in previous reports, the prevalence of long-term conditions increased markedly with age in 2014, from a quarter (25%) of adults aged 16-24 to around three-quarters (77%) of those aged 75 and over (with very similar patterns for men and women). Most of this increase with age was due to rising prevalence of limiting conditions (15% and 61%, in the youngest and oldest groups, respectively). In contrast, the proportion with only non-limiting conditions increased from 10-11% in the 16-34 age group, to 22% of those aged 65-74 (and 16% in the oldest group). Table 1.4
Children
Table 1.4 also includes the 2014 figures for children aged 0-15. In total, 19% of children had a long-term condition (11% limiting, 9% only non-limiting). The figure for boys (21%) was higher than for girls (18%), although this difference between sexes was not significant. Boys were, however, significantly more likely than girls to have a limiting condition (12% and 9%, respectively). Table 1.4
1.3.5 Trends in WEMWBS mean scores since 2008
WEMWBS mean scores continue to be relatively static, with only minor, non-significant, fluctuations observed since 2008 (50.0 in 2008 and in both 2013 and 2014). Mean scores have not changed significantly over time for men or women. Table 1.5
1.3.6 WEMWBS mean scores in 2014, by age and sex
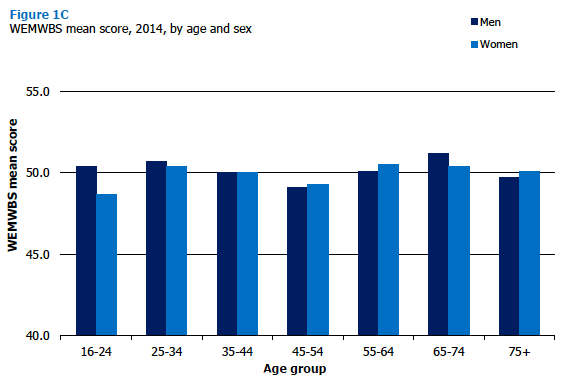
In 2014, the average mean WEMWBS score for adults (aged 16 and over) was 50.0. The scores for men (50.1) and women (49.9) were not significantly different. As seen in previous years,[23] and illustrated in Figure 1C, levels of wellbeing varied across age groups. Men's wellbeing was lowest for those aged 45-54 (49.1), and highest for those aged 65-74 (51.2). Women's wellbeing showed less variation for those aged 25 and over (49.3-50.5), with lower levels seen for those aged 16-24 (48.7). Figure 1C, Table 1.6
1.3.7 WEMWBS mean scores in 2014, by area deprivation and sex
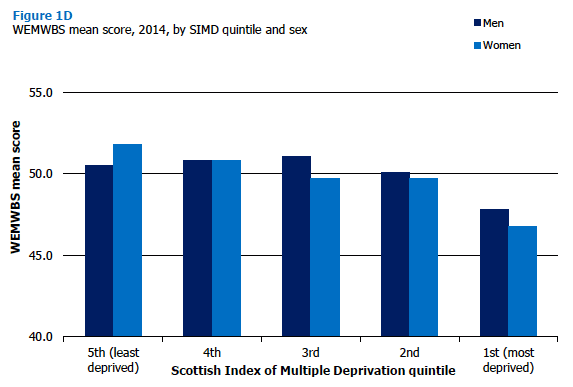
Figure 1D and Table 1.7 show that in 2014, age-standardised WEMWBS mean scores for adults decreased as levels of area deprivation increased. The mean score among adults (aged 16 and over) living in the least deprived areas was 51.1; it then declined across each quintile to 47.3 for adults living in the most deprived areas. Women's mean scores generally followed the same pattern as for adults (51.8 in the least deprived areas, 46.8 in the most). For men, however, there was a slightly different pattern. Mean scores were highest (51.1) for those in the middle (third most deprived) quintile, and lower in other quintiles, particularly for men living in the most deprived areas (47.8). Figure 1D, Table 1.7
1.3.8 GHQ-12 scores in 2014, by age and sex
In 2014, 16% of adults (aged 16 and over) exhibited signs of a possible psychiatric disorder (a GHQ-12 score of 4 or more), with 61% of adults reporting no symptoms (GHQ-12 score of 0).
Women were more likely than men to have a GHQ-12 score of 4 or more in 2014 (17% women and 14% men), whilst men were more likely to have a score of 0 (65% men, 56% women).
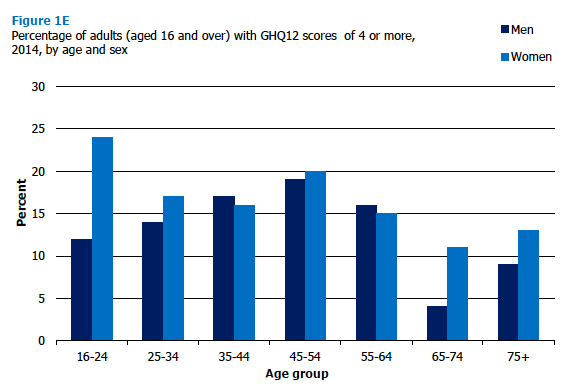
The prevalence of GHQ-12 scores of 4 or more was fairly similar (15-19%) in the 16-64 age group, and was lower (8-12%) for those aged 65 and over. However, as Figure 1E shows, the patterns across the age groups differed for men and women. For men, prevalence of scores of 4 or more increased steadily with age to a peak of 19% in the 45-54 age group, before dropping markedly to 4% for those aged 65-74, and increasing again to 9% for the oldest men. Among women, high GHQ-12 scores were most prevalent in the 16-24 (24%) and 45-54 (20%) age groups, and varied across the other age groups without a clear pattern, but were least common for those aged 65 and over (11‑13%). Figure 1E, Table 1.8
1.3.9 Life satisfaction mean scores in 2014, by age and sex
The average mean life satisfaction score for adults (aged 16 and over) in 2014 was 7.8. The proportion of adults with above average scores (of 9-10) was 34%. The prevalence of average mean scores (8), and below average scores (0-7) were similar (32% and 33% respectively). Scores did not vary significantly by sex.
Life satisfaction varied by age in 2014. In common with the patterns observed above for WEMWBS and GHQ-12, and as reported previously,23 life satisfaction was lowest among those aged 45-54 (reflected in both the mean score of 7.5 and the proportion with scores below average of 39%). Life satisfaction scores were highest for those aged 65 and over (41-42% above average and mean scores of 8.0‑8.1). Table 1.9
Contact
Email: Julie Landsberg