Developing a community child health service for the 21st century
A report on a review of the community child health service in Scotland.
Section 5: The modernisation agenda for paediatrics in the UK
Modelling the Future
To provide some guidance for services and to meet the challenges in delivery of paediatric services the RCPCH "Modelling the Future" ( MTF) 45 reports described a variety of models of paediatric care depending on local circumstances and in the context of changing training arrangements and EU working time regulations ( EWTR) which limit working hours.
Figure 7: Modelling the Future: Vision of Care across Acute and Community Settings ( RCPCH 2008)
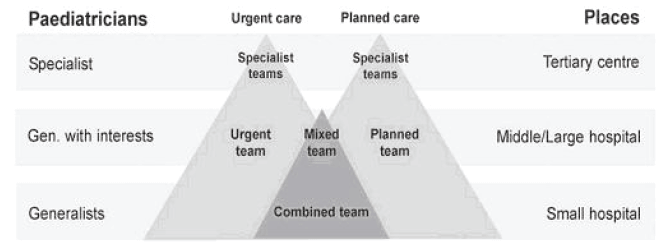
Modelling the Future envisages teams of paediatricians delivering "urgent" and "planned" care with a portfolio of skills within a team of other professionals across hospital and community settings. The career of a consultant paediatrician would include very demanding acute work with a great deal of out-of-hours cover in the early consultant years to a greater emphasis on planned care in their later years. Innovative approaches to job planning for clinicians and good continuing professional development will obviously contribute to implementing such "portfolio" careers
Changes in Training of Junior Doctors
In 2005 the Modernising Medical Careers ( MMC) programme marked a major reform in postgraduate medical education across all specialities. Following graduation all doctors spend 2 years in foundation programmes which lead doctors through a holistic programme of training and education. Subsequently they will enter an 8 year specialty (( ST1- ST8) or GP orientated "run-through" training programme leading to a certificate of completion of training ( CCT) at the end.
In order to match the number of trainees to consultant posts, the number of trainees is strictly controlled. However, once enrolled in a training programme, with a "number", the trainee can take time out or work flexibly and still be guaranteed a place to re-enter training. This issue creates difficulties when combined with EWTR requirements maintaining middle grade ( ST3-6) rotas.
This need for consultant cover for acute rotas has resulted in consultant appointments which are reconfigured with solely acute duties or with a more generic role combining community and acute duties as Professor Craft envisaged in the RCPCH report "Strengthening the care of Children in the Community" (2002).
The Basket of Competencies for CCH
The MMC changes resulted in a positive move to provide every trainee with an assured set of assessed competencies, including a minimum of 6 months in Community Paediatrics 46 as part of their core training. However, the author finds there is a considerable overlap between the competency framework for level 3 General Paediatrics and those for Community Paediatricians so perhaps in the future these programmes could be better integrated.
The essential competency domains for CCH in the Higher Specialist programme for CCH ( ST4- ST8) require skills in the following areas of practice:
- Vulnerable children/social paediatrics
- Neurodisability and chronic disease management
- General Paediatrics component
- Behavioural Paediatrics
- Public Health and Epidemiology
Note: If a model is adopted whereby a generic breed of paediatrician is appointed who undertakes duties both in the acute setting and in the community, then they require training at the ST5-8 stage to assure appropriate competencies in the care of children in the community.
Workforce Challenges
Because of workforce challenges, over the next few years it is anticipated that services will be delivered by trained doctors in consultant-led teams working in multi-disciplinary and skill-mixed teams. Workforce data shows that the current CCH workforce in Scotland is primarily female and a significant proportion of these are near retirement.
Figure 8: Age of Acute and Community Consultants ( RCPCH 2008)
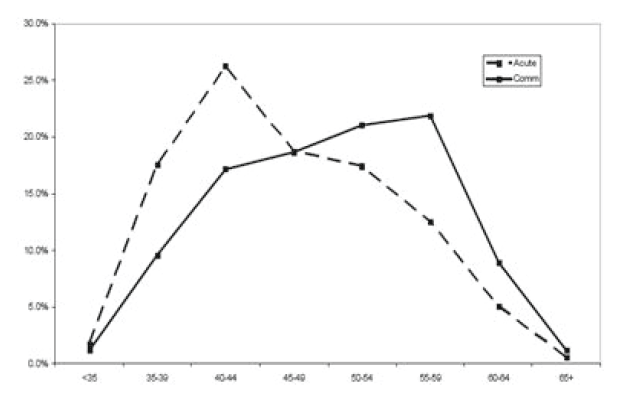
Challenges for the Present Service in Scotland
During the course of visits, by personal communication and from discussion with key stakeholders such as RCPCH and SACCH, it appeared that a variety of models of care are prevailing across Scotland. Informal networks exist but are not formally constituted with the exception of Child Protection and Complex Needs (Managed Clinical Network for children with exceptional healthcare needs ( CEN)).
Children may receive one service or assessment in one area and not in another. Relationships with local authorities are variable, with some very successful partnerships with unitary authorities. However, where there are several authorities corresponding to a health board unit, complexities can arise when, for example, education and social work policies and structures vary across boundaries. Public health challenges such as obesity and improving the wellbeing of children and young people may have slipped in terms of priority because of the pressures on face-to-face clinical services. Strategic planning, which needs to be done in partnership with commissioners, local authority officers and communities, may also have suffered in this respect. The Health Board questionnaire has given an overview of how services are being delivered in 2010.
Contact
- Mary Sloan mary.sloan@gov.scot