Developing a community child health service for the 21st century
A report on a review of the community child health service in Scotland.
Annexe 4: Health Board Questionnaire Findings
Notes :
- Where graphs are shown, the Health Boards are displayed on the X axis in order of population from the left.
- Comments follow as appropriate for each finding or group of findings
- The RCPCH terminology refers to a combined and integrated child health service , ie with acute and community services co-managed and working closely with partners in local authorities, criminal justice and the police and the third sector.
Structure and Infrastructure Issues for CCH services
- Management Configuration of CCH
8/14 (57%) of HBs report CCH is combined with acute paediatrics which rises to 8/11 (73%) if Island Boards are omitted. One large HB currently has a standalone CCH in various community health partnerships ( CHPs) with an overarching manager. 35.7% of Boards have a combined service with acute paediatrics in a directly managed unit. 21.4% are combined with acute in a CHP. 7 HBs co-manage community paediatrics, community children's nursing, paediatric AHPs and CAMHS services. 11 HBs (79%) report significant management change affecting the CCH services within the past 5 years.
- Co-management of CAMHS
In 45% of HB CAMHS in Scotland are not co-managed with CCH.
Comment: The majority of services are organised as a combined service with acute and community co-managed. Sometimes CCH is co-managed with CAMHS or CAMHS may be separate from other children's services with adult MHS. The shared interests of Paediatric Services and CAMHS require there is close co-ordination of service delivery and strategy.
- Clinical leadership models
64% HBs have a dedicated clinical director for their combined service. Other boards have adopted similar lead clinician models. One HB reported a Head of Service.
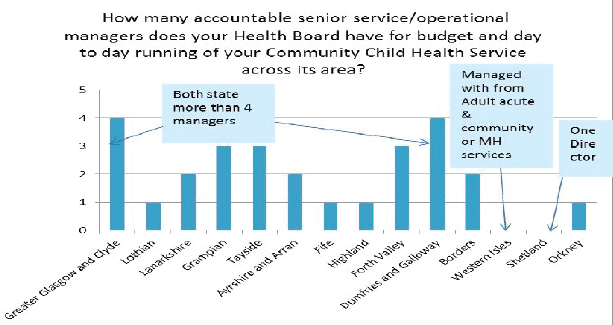
- Accountable senior/operational managers
The number of managers for CCH vary from 1 to more than 4 (mean 2.25 managers reported).
Comment: There was no clear correlation with the size of the health board population. There might also have been a lack of clarity in the question eliciting vague answers.
- Pattern of delivery of CCH and General Paediatric clinics
In 10 (71%) HBs CCH staff provide general paediatric outpatient clinics ( MTF model).
In 93% of HBs general paediatric OP clinics are provided by outreach from Hospital with 10 (71%) HBs using a combination of CCH and outreach from hospital (91% without island boards).
Comment: Perhaps some further discussion is needed about how general paediatric OP should be delivered by a combined service most efficiently.
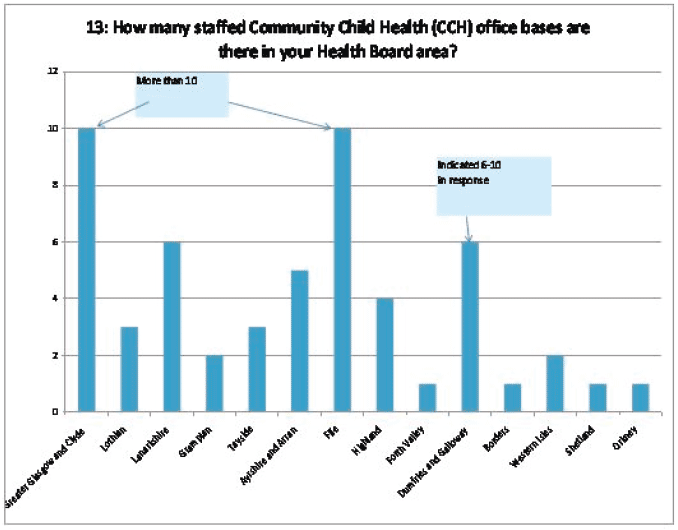
- Staffed CCH office bases
The average number of CCH staffed office bases is reported as 4 with a range of 1-10.
Comment: Numbers of bases are not obviously related to population size of the HB but obviously rurality may be a factor here.
- Patient administration systems ( PAS) used in CCH
57% of HBs are using paper-based PAS systems
29% use a locally devised database such as Excel
36% use a proprietary system shared with acute services such as Medtrack etc -
14% of services do not share their system with acute services but can access acute patient information by agreement.
Comment: Analysis of patient flows and DNAs is more difficult and time-consuming without adequate IT for patient administration and can lead to poorer attendance rates eg because text reminders cannot be sent easily. Some databases eg using excel do not adequate security.
- Use of National Support Needs System ( SNS) to monitor children with additional support needs
11 HBs (64%) reported using the national SNS or similar database to monitor children and young people with additional support needs ( ASN). One HB mentioned its local authority has an LD register. 4 HBs had no means of monitoring youngsters with ASN. The percentage of Children and YP on these databases varied from 0.6%-5%. 5 boards did not answer this question. Across the UK, a figure of 2% of children and YP with ASN is evidenced. 77
Comment: Carefully monitoring the number of children and young people with ASN is the way in which their needs can be best ascertained and planned for.
- Premises used by CCH staff to see children and young people
HBs were asked where CCH consultations took place from a range of venues: local primary care clinic in a health centre; local GP surgery; rural general hospital; community hospital; schools (mainstream); schools (special); respite facility; secure unit; local DGH out-patients; children's hospital out-patients; child and family centre; forensic medical facility; private school facilities, eg Royal Blind School.
Only one 1 HB uses 10 of the possible 12 venues described.
6 (43%) HBs indicate CCH clinicians are using rural general hospitals for consultations.
6 (43%) HBs report that CCH staff are using community hospitals.
8 (57%) are using mainstream schools and special schools.
5(36%) consult in a children's respite facility.
In only one HB do clinicians visit a secure unit 78 .
64% HBs indicated CCH staff use local DGH outpatient facilities
43% HBs state CCH staff use children's hospital outpatient facilities
29% of HBs report CCH staff visit child and family centres.
In 29% of HBs CCH staff use a forensic medical facility ( FMF).
Comment: A wide range of premises are used but a minority of CCH services use child and family centres, forensic medical facilities and respite facilities for consultations.
Process Issues
- Availability of referral guidelines for CCH
50% of HBs have online referral guidelines for CCH.
64% HBs use paper guidelines (2 use only paper guidelines). Paper guidelines may be difficult to access and become outdated rapidly.
29% of HBs have referral guidelines "for a few conditions" only.
Comment: Guidelines should be available online as well as on paper in all HBs. They can assist referrers in making the correct referral and avoid delays (see BACCH OP Clinic standards Annexe 9).
- Shared pathways between CAMHS and CCH for "overlapping conditions" such as ASD, ADHD, somatising disorders etc.
8(57%) HBs do have shared pathways and 5 (36%) HBs do not have shared pathways.
Comment: A lack of shared pathways could lead to duplication or delays in accessing diagnosis and treatment.
- Availability of consultation sessions between CAMHS and CCH
10 (71%) HBs have consultation sessions available but 2 HBs do not
2 HBs don't know if they have consultation sessions.
Comment: Consultation sessions enable communication between CAMHS and CCH clinicians to ensure effective referrals and appropriate patient management in the case of doubt. They are an accepted part of service in most HBs and perhaps should be regarded as essential.
- Access to laboratory, neurophysiological and imaging investigations by Community Paediatricians
- Imaging
9 (64%) of HBs indicated community paediatricians have access to all of CT, MRI, ultrasound and ordinary X-ray facilities.
2 HBs indicated no access at all (one mainland and one island).
5 HBs indicated no access to nuclear scans.
- Labs
In 7 HBs CCH doctors can access all of clinical chemistry, pathology, genetics, and microbiology.
3 mainland boards indicated no access to lab investigations and one did not know.
Comment: As community paediatricians are diagnosing and investigating children access to all these facilities is essential.
- Neurophysiological investigations ( EEG, Sleep EEG and evoked potentials)
7 HBs have all three but 2 had none. These investigations are used with children suspected of epilepsy, language disorders and vision problems.
- Online access to imaging and laboratory results by Community Paediatricians
In 9 HBs (64%) access to both lab and imaging results online is available to CCH doctors.
79% have access to lab results only.2 HBs (one mainland) indicated no access at all.
Comment: Online access to results allows clinicians to act in a timely and evidence-based way and can speed up diagnosis and communication with parents and avoid delays in appropriate treatment.
- CCH clinic facilities
- Local clinic venues
All HBs have local CCH clinics accessible to under 16s.
4 HBs do not operate clinics in schools (2 island and 2 mainland).
10 boards have Child Development Centre ( CDC) clinics accessible to under 16s. Others may restrict CDCs to younger children but this information was not elicited.
- Clinic reception and booking capacity
7 HBs reported >75% of their CCH clinics had these facilities.
5 HBs reported less than 25% of their clinics had reception and booking available on site.
Comment: BACCH clinic standards 79 suggest a named clerk for each clinic. Not having reception or booking facilities may make life difficult for parents and can waste valuable clinic time if the flow of patients is not managed. Parents of vulnerable children who may miss appointments can be contacted in advance of a clinic by reception staff to improve their chances of attending.
- Capacity to accommodate paediatric trainees with consultant supervision (dual-consulting) in CCH clinics
3 (21%) HBs report they have 100% of their clinics available for dual-consulting
4 (29%) HBs have >75% of their clinics available for dual-consulting.
4 (29%) HBs have <50% of their clinics available for dual-consulting.
Comment: RCPCH recommends that CCH trainees be taught access to a consultant or other senior colleague during clinics. There needs to be two adjacent consulting rooms available in any clinic where trainees practise.
- Availability of specialist community paediatricians in HB areas
- Neurodisability
All but 2 island HBs have a lead (Tier 3) neurodisability consultant.
5 of these 12 consultants work in school clinics
8 in child development centres
7 in CCH clinics
7 undertake inreach to hospital
Comment: The Chair of the CSAG for the neurodisability grid 80 indicates that their workforce model recommends one paediatric neurodisability consultant for a total population of 100,000. This would amount to 52 for Scotland and 13 for Greater Glasgow & Clyde. Exact numbers of PND consultants in Scotland are not available to the author.
- Long-term illness
In relation to children with chronic illness and long-term conditions, care is delivered via school clinics in all but 3 HBs. These children and YP also receive care in CCH clinics in 12 HBs (86%) and by inreach to hospital clinics in 9 HBs (64%).
- Special Senses
- Visual Impairment
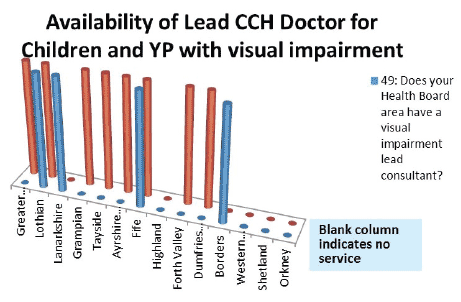
4 HBs report a lead consultant (blue columns in diagram) for visual impairment and 8 an associate specialist (red columns in diagram). One HB has both. One mainland board has neither.
Comment: As part of the Scottish Vision Strategy ( SVS) Implementation Plan (May 2009) NES was to "examine future workforce needs to meet skills and competencies and to consider service redesign". It is not clear if this recommendation applied to CCH services. At present there are no standards for the provision of visual impairment services for children and young people although there are opportunities in the formation of networks as recommended by the SVS.
- Hearing impairment
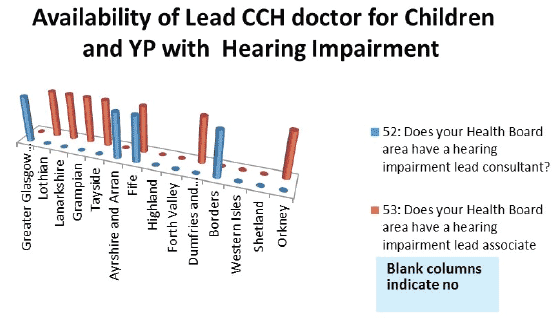
HBs were asked if they have a lead CCH doctor (Consultant or Associate Specialist) for children with a hearing impairment. The graph shows what is in place.
4 HBs have a lead consultant for children with hearing impairment.
6 HBs have an associate specialist lead.
One HB (not a tertiary centre) has both.
2 mainland HBs reported having neither.
Comment: Many children with significant sensorineural hearing loss will be detected by neonatal screening but their ongoing care needs to carry throughout their childhood and adolescent years, with a need for continuing team support, especially in the education setting. Children will develop also significant hearing loss during their later childhood. Doctors in paediatric audiology work as part of multi-disciplinary teams with close links to ENT and audiometricians.
- CCH Services for vulnerable children and young people
All 14 boards indicated that they provide comprehensive services for vulnerable children in respect of adoption and fostering.
13 boards also provide comprehensive medical assessment ( CME) of vulnerable children and also child protection services including assessment of children suspected of being abused (non-accidental injury; child sexual abuse; neglect and emotional abuse).
One HB indicated they did not provide CME or Child Protection services.
The question was asked "Is a one door entry in place for child protection referrals?"
All save 2 island boards replied it was.
CCH staff are involved in interagency referral discussions ( IRDs) except 2 island boards.
The majority of boards undertake peer review sessions for staff involved in child protection.
Comment: The RCPCH recommends that paediatricians participate in peer review sessions. HMIe recommends that IRDs are held when dealing with suspected abuse. HMIe has undertaken an inspection process of child protection processes in all local authority areas and further information can be obtained from their reports.
Planning activity
Health boards were asked about the participation of community child health staff in local regional and national networks.
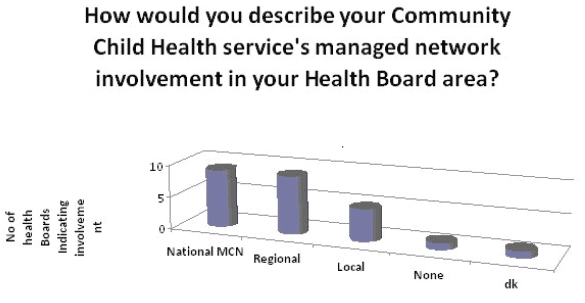
8/14 HBs reported involvement in both national and regional health networks.
One HB reported no network involvement and one did not know.
Only 4 (29%) reported CCH involvement in local networks (eg local authority/ CHP etc.).
Comment: The local network response indicates that CCH is still working in isolation from other agencies and acute services and there has been little inter-Board or inter-regional network activity compared to acute services for children, which have benefited from investment in regional networks.
However, when the question was asked about CCH engagement in children's services planning at locality/ CHP, board and regional planning group level a slightly different picture emerged,
- CCH engagement in children's services planning
11 boards indicated CCH staff engagement at locality level, 11 at board level and 10 at regional level. 2 mainland boards had no engagement in planning at Board level. One mainland Board stated they did not know of engagement at any level.
Comment: It is encouraging the CCH is involved in children's services planning in a majority of HBs at all levels (79%). The answer to this question conflicts with that of the previous one.
CCH service performance and outcome measures
- HBs were asked "Is 18-week Referral to Treatment ( RTT) in place for CCH clinics?"
12 of the 14 (86%) HBs have 18 week RTT in place for CCH and two mainland boards do not. Two HBs covering large urban populations stated they did not intend to introduce 18 week RTT for CCH clinics.
Comment: These 2 boards have the highest proportion of Scotland's most deprived children. There may be further worsening of health inequalities as these children and young people may have to wait the longest for a CCH consultation.
- Did Not Attend ( DNA) rates
The average Did Not Attend ( DNA) rate in CCH clinics varied from 0-5% to 26-30%. Three HBs did not know their CCH clinic DNA rate 81 . Six HBs had a CCH clinic DNA rate of between 21 and 30%.
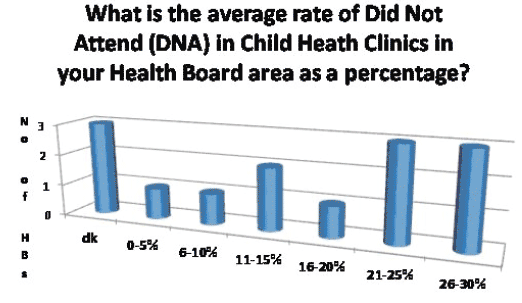
Three HBs had >26% DNA rate but not all these HBs had a high deprivation factor ( SIMD).
One had only 1.4% of the total most deprived wards for health; one had13.7% of the total most deprived wards for health and the third HB had 50% of the total most deprived wards for health.
Comment: There is a documented association between deprivation and DNA rates, but some centres in the UK 82 have managed to reduce these rates below 20% for disadvantaged families by the judicious use of texting prior to appointments and HV follow-up and a determined focus on the most vulnerable families.
Of note, 3 HBs indicated don't know responses. DNAs can lead to a serious delay in diagnosis and intervention for our most needy children. Highly mobile families, children of asylum-seekers and families where there is parental substance misuse or chronic ill-health may be in this high risk group, increasing their health inequalities and measures are required to be applied to increase access for such children.
- New to return (N/R) patient ratios for CCH clinics
Boards were asked to give their "new to return (N/R) patient ratios for CCH clinics". This question seemed problematic as there was a high number of no replies and don't knows (7/14 HBs) 50%. Across the 7 boards which replied, the average N/R ratio was 1:3, similar to acute general paediatrics (anecdotal evidence), but there was a wide range of 1:1.5 to 1:9.
Comment: Further work may be needed in this area as this measure is standard in medical paediatrics out-patient clinics.
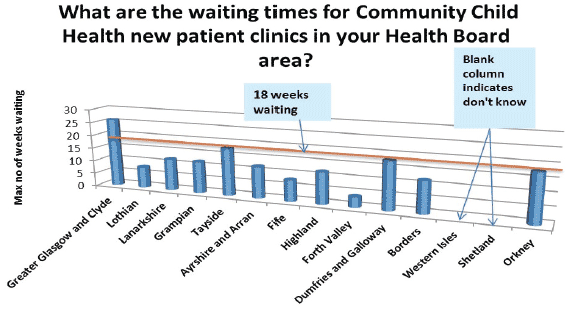
- Waiting times for CCH clinics
In the question about waiting times for new referrals to CCH clinics there was a wide range of waits from a maximum of 4 weeks to a maximum of 6 months.
The largest, most deprived HB declared the longest waiting times (a maximum of 6 months) and 3 HBs have waiting times up to 18 weeks (One larger; one small; one island). 2 island HBs indicated don't know for waiting times.
Comment: It appears that in the largest health board with 50% of the most deprived wards in Scotland, children have to wait the longest to see a paediatrician in community settings.
- Quality assurance processes for CCH activities
12 (86%) HBs monitor attendance rates at CCH clinics. 10 (71%) HBs monitor referrals to CCH clinics. 2 HBs monitor investigations, 4(29%) HBs monitor parent/carer satisfaction and it is not clear if this monitoring is part of generic surveys rather than direct feedback with parents at the time of clinical contact. No HBs monitor actions such as DLA or interagency reports etc.
Comment: Clinic effectiveness can be measured by monitoring attendance, referral patterns, pattern of investigations and patient (parent/carer) satisfaction. There is a low level of measurement of parent/carer satisfaction with CCH services and no monitoring of CCH activities such as report writing which can be very time-consuming.
Contact
- Mary Sloan mary.sloan@gov.scot