Developing a community child health service for the 21st century
A report on a review of the community child health service in Scotland.
Section 13: Future workforce requirements
In terms of model of care advice from RCPCH 63 , in the small to medium DGH, it is thought that "combined" or "generic" paediatricians with a broad range of competencies could work across planned and acute care, in hospital and community settings, enabling a 24/7 consultant-led service with sufficient doctors in a team (assuming minimal middle grade cover) to comply with EWTR 64 . It is envisaged that with team job planning and the advent of "portfolio careers", consultants may opt to change the balance of planned and acute care during their working lifetime. Opportunities for retraining may be needed for consultants with no previous CCH experience. Any review of the paediatric workforce therefore needs to incorporate mechanisms to enable retraining in order to maintain maximum flexibility in a team of consultants.
The job plans of these "combined" paediatricians should allow a balance of time spent between CCH and hospital settings. In addition, acute on-call organised around "hot weeks" would be required. However, adequate time spent in community to build up networks and undertake interagency work in multi-disciplinary teams will also be needed. The challenge for these acute combined paediatricians is maintaining competencies where neonatal cover is also required. It is doubtful whether this model of consultant could be competent across all three domains of neonatology, general and community paediatrics.
Subspecialisms in Community Child Health
The issue of sub-specialties in CCH (paediatric neurodisability, child protection, looked after children and YP, behavioural paediatrics etc.) may require additional training to meet local needs, particularly in large urban populations. In Scotland, paediatricians with enhanced skills may be part of a regional or national managed network (eg child protection), ensuring delivery of the whole range of expertise across Scotland. Maintenance of these skills using peer review and telemedicine is already established through the existing managed networks. Managed networks could be considered for vision and hearing impairment services. Succession planning for such specialists needs to happen well before retiral to avoid a gap in service as they are very few in number.
Future of the Specialty Doctor in CCH
The future of specialty doctors (previously SASG) in CCH must be considered actively because of their age profile; the high level of contribution to CCH in Scotland; the vacancy rate of 10% amongst SASG doctors, and with many centres reporting difficulty in recruitment of suitably trained individuals.
High attrition rates in the first few years of paediatric training have not resulted in good recruitment to the SD cadre in CCH. The reasons for this are not clear, but may relate to a perceived unattractiveness of SD posts per se or CCH itself, or (more likely) of the increased attractiveness of general practice as a career in terms of satisfaction, family friendliness and remuneration.
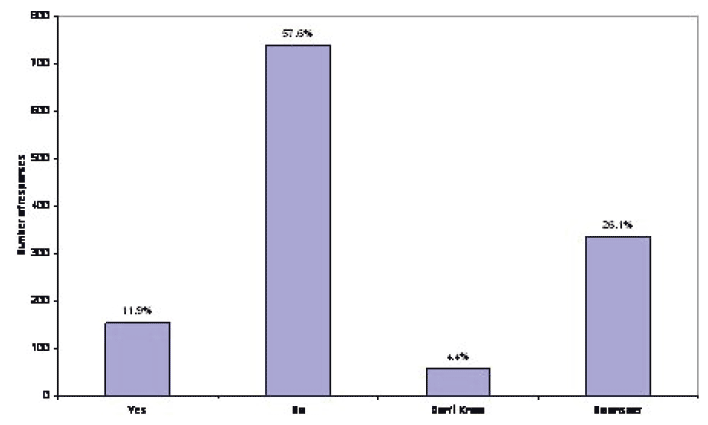
The RCPCH 2009 UK census document included the following question and responses (referring to all SASG doctors in paediatrics): if a SASG post became vacant would it be replaced by a Consultant post? A response was received in respect of 950 of the 1285 SASG doctors (73.9%). Figure 18 shows that for 57.6% of posts, there would not be conversion, for 11.9% there would be, leaving 4.4% who were not sure and 26% non-responders. There is a significant number of non-responding services, but this suggests only a minority of services were contemplating conversion of SASG vacancies to consultants in 2009 . In view of the difficulty of recruitment, further examination of this problem would appear necessary.
Figure 19: If a SASG post became vacant would it be replaced by a Consultant post? ( RCPCH Census 2009)
There are a number of options in terms of the way ahead and these may be applied in various combinations according to local circumstances:
1. Status quo: ie seek to fill SD/ AS vacancies as they arise:
If there are excess CCT holders over the next few years due to the ST "bulge" would some of these accept jobs at a lower grade? To work in the CCH service, additional "on the job" training may be required to enable such appointees to develop enhanced skills as required in CCH. To enable ST's entering the Specialist Doctor grade at the bottom to progress and have a satisfying career, excellent continuing professional development programmes need to be in place to allow competence and skills to be developed to meet local need.
An alternative route to filling SD posts is from existing paediatric trainees wishing a career break from an ST training programme without acute duties. Presently this route does not favour re-entry to a programme at a later date.
Another alternative would be to "decouple" run-through training at ST3/4 stage so that trainees could take up an SD post and possibly be able to re-enter training through competitive appointments if desired.
Note: There has been no "decoupling" of posts after ST3/4 stage in Paediatric ST programmes across the UK unlike some other specialties such as emergency medicine, therefore doctors who might seek an alternative post at this stage will not be available unless they drop out of "run-through", which seems undesirable in terms of rational workforce planning.
2. Skill mix:
Adopt a policy whereby vacant SDAS posts are reviewed and considered for re-allocation to either SD or consultant grade posts (accepting they may change to generic or CCH consultants as described above) as part of a pre- planned workforce plan.
3. Redesign: Review vacant SASG posts and reallocate to advanced AHP or nursing or both specialist/practitioner posts in the particular local clinical area of need according to requirements 65 .
How Do We Know What CCH Workforce We Need?
In 1999 the British Association for Community Child Health ( BACCH) published a workforce guide 66 which remains as the only guide of its type. The methodology of the guide is on the BACCH website 67 . However, because of service changes since the guide was published there has been a reworking of the guide taking into account the following factors:
- The original sessions were designated in 3.5 hour slots. These have been adjusted to 4-hour slots to fit the unit of programmed activity ( PA) of the new SASG and consultant contracts.
- A number of tasks of CCH doctors have changed including:
- Cessation of child health screening activity by CCH doctors
- Contribution by doctors in training has diminished
- Greatly increased survival of young people with complex needs
- Greater recognition of disorders such as ADHD and Autism
- General paediatric duties were excluded
- Child protection work has become more demanding
The consultant contract initiated across the NHS in 2000 provides a balance between Direct Clinical Care activity ( DCC) and Supporting Professional Activity ( SPA) measured in units of 4-hour programmed activities. When the consultant contract was changed in 2000 a ratio of 7.5 PAs to 2.5 PAs was negotiated. More recently the expectation has been a ratio of 8.5 DCCs:1.5 SPAs and the onus has been on consultants themselves to argue for any additional SPAs on the basis of their responsibilities during the job planning process. For SASG doctors, in their new contract in 2008, 1 SPA was agreed, ie a ratio of 9:1.
Deriving the total DCC PAs from the revised workforce guide (Annexe for a total population of 300,000 the table below shows workforce requirements.)
Table 2: Revised Workforce Guide: Estimated DCC PAs
| total DCC Pas |
||||
|---|---|---|---|---|
| Clinical Activity |
consultants |
Assoc spec |
Spec docs |
total |
| ASN/disability/gen paediatrics |
10 |
7 |
8 |
25 |
| Sub-specialties |
6.5 |
16 |
8.8 |
31.3 |
| Vulnerable children/ YP |
14.255 |
2 |
7.38 |
23.635 |
| Public Health |
1.75 |
1.75 |
||
| total DCC PAs required |
32.505 |
25 |
24.18 |
81.685 |
Making a range of assumptions about the number of SPAs in a job plan ranging from one ( SASG and some consultants) to 2.5, the required establishment based on the assumptions in the revised workforce guide would be as follows:
Table 3: Estimated Required CCH Establishment for Population of 300,000
| For 300K total population CCH establishment would be: |
|||
|---|---|---|---|
| Consultant |
AS |
Spec Doc |
Total |
| WTE With 1 SPA |
|||
| 3.57 |
2.8 |
2.7 |
9.07 |
| WTE with 1.5 SPA |
|||
| 3.8 |
2.8 |
2.7 |
9.3 |
| WTE with 2 SPA |
|||
| 4.1 |
2.8 |
2.7 |
9.6 |
| WTE with 2.5 SPA |
|||
| 4.3 |
2.8 |
2.7 |
9.8 |
To see exemplars of this model some defined populations in Scotland see Annexe 10.
The Whole of Scotland Model
Applying the model to the whole of Scotland (Population 5.194 million) 68 , the total establishment of trained CCH paediatricians derived is very similar to the current workforce numbers which implies that the current trained doctor CCH workforce numbers are adequate, although the balance of SASG versus consultants has not been examined at national level and the distribution of those trained CCH doctors across the country needs to be benchmarked against the workforce model for local populations.
In addition, no weightings or corrections for rurality, deprivation or number of part-time staff have been applied to the anticipated numbers of staff, and these would need to be agreed to a consistent formula (perhaps akin to the Arbuthnott formula for funding of health boards 69 ). As already stated, there are currently 2.8 WTE trained CCH doctors in Scotland/100,000 population versus 2.4/100,000 in England and Wales, although the Chair of the RCPCH CCH CSAG suggests the aspiration is 4.5 per 100,00 population.
There is also no allowance for CCH subspecialties at Regional level. In relation to PND for example, the Chair of the CSAC suggests that the recommendation is 1 per 100,000 population, equivalent to a total of 52 for Scotland, although this level has not been reached across the UK. Encouragingly, all Scottish Health Boards bar two reported a lead consultant for paediatric neurodisability in the HB survey.
Table 4: Estimated Whole of Scotland CCH Workforce Requirements
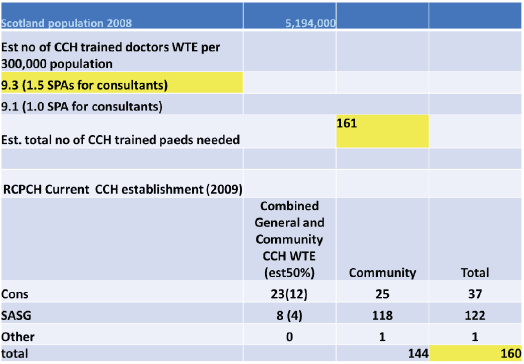
Summary of Workforce Findings
There are insufficient expected CCTs in the pipeline to fill the expected number of CCH posts ( SASG and consultant) likely to become vacant over the next 10 years. There is already a 10% vacancy rate amongst SASGs and a 6% vacancy rate amongst Consultant posts. Most current trainees have only core training in CCH, although this needs to be confirmed. There is a vacuum in terms of plans for filling the CCH SASG posts despite their age profile and large proportion of CCH work which they carry out.
Replacement consultant posts are now more likely to be "combined" paediatricians who have skills across acute and community, but support and further training will be needed for young consultants who are expected to carry out CCH duties with limited training.
Contact
- Mary Sloan mary.sloan@gov.scot