Developing a community child health service for the 21st century
A report on a review of the community child health service in Scotland.
Section 2: Context of child health in Scotland
Wellbeing of Children in Scotland
The poor comparative wellbeing and health of children in Scotland and in the UK as a whole have been highlighted by UNICEF 13 and the OECD 14 . The precursors of these findings are well documented and discussed and the Scottish Government has sought to address the problems in a variety of ways. Beginning with "Better Health, Better Care" in 2007, "Equally Well" in 2009 and the "Early Years Framework" in 2009 15 , early intervention has been prioritised and effective ways of supporting children and families signposted through the "Getting it Right for Every Child" ( GIRFEC) initiative beginning in 2008 16 .
Figure 1. Showing OECD Wellbeing ranking for 23 member countries in 2000
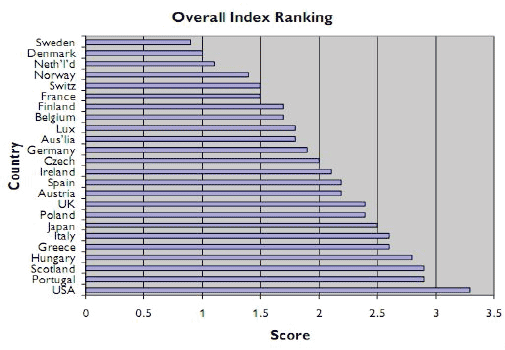
Health Inequalities in Childhood in Scotland
In addition to poor comparisons with other developed nations in terms of child wellbeing, there are substantial inequalities across society in Scotland, with persisting differences in the outcomes of pregnancy, child death rates 17 , accident rates and in the health morbidity experienced between the least deprived and the most deprived SIMD quintiles. Around 25% of Scottish children are living in poverty today.
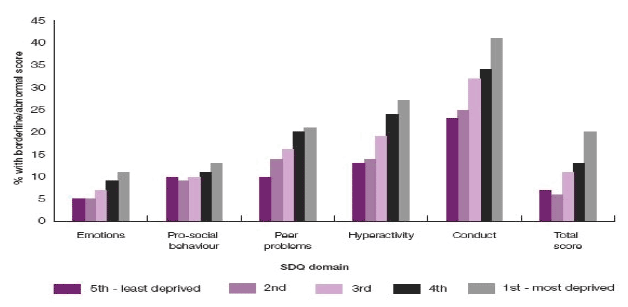
The "Growing up in Scotland Study" ( GUS) is following 13,000 children across Scotland longitudinally and is a useful barometer of the status quo of child wellbeing across a range of domains. The authors have highlighted a number of health outcomes and associated risk factors which are known to impact on the future health of a child both pre-birth and during the early years, and documented the social gradient of morbidity across a number of domains for example, symptoms of behavioural disorder as elicited by the Strengths and Difficulties Questionnaire ( SDQ) administered to parents of 46-month-old children. The graph illustrates the worsening symptoms of disorder from the least to the most deprived youngsters.
Figure 2: SDQ individual domain scores, by SIMD quintile (46 months) ( GUS Study 2009)
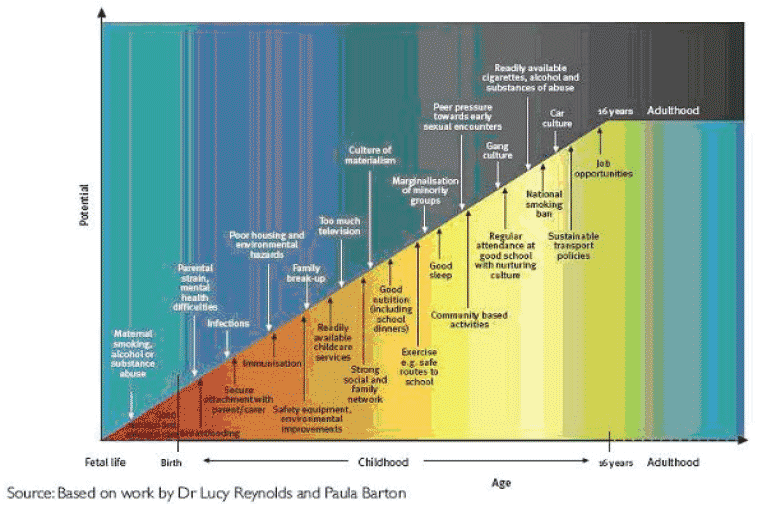
The welcome improvements in acute hospital performance measures such as waiting times seem not to have impacted significantly on the global wellbeing of children and young people. More fundamental societal measures such as parenting capacity which may be influenced by circumstances (including substance misuse), physical or mental health issues for parents, family composition, access to play and education, housing etc. are factors which affect mental health, attachment, educational attainment etc. Increased awareness of the protective influence of resilience factors in children and their families has guided the GIRFEC initiative in its quest to improve children's life outcomes. Figure 3 shows the complex interaction of positive and negative factors which may prevail in a child's life.
Figure 3: Interaction of positive and negative factors in a child's life
Economic Arguments for Early Intervention
In terms of economic gain for the country, it has been estimated by James Heckman 18 that there can be a 12-16% gain per annum for every £1 invested in very young children who are in disadvantaged households and a 5 times benefit for each such child reaching adulthood after appropriate interventions. This emphasises the necessity for long-term planning to produce sustained investment and effort over many years. The high tariff spend for young people who may have been looked after by the state; become involved in the criminal justice system, suffer from mental illness etc. cannot easily be disinvested and diverted to early intervention. This dilemma is highlighted in the diagram below.
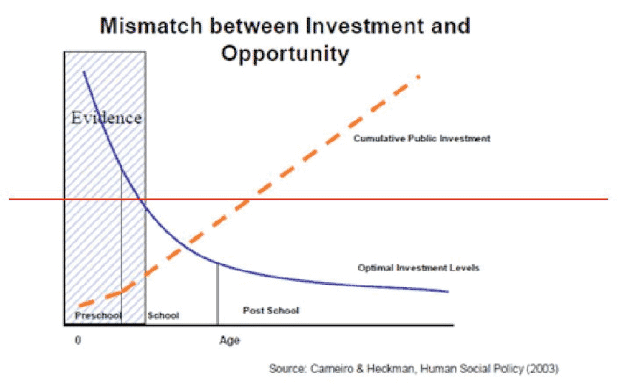
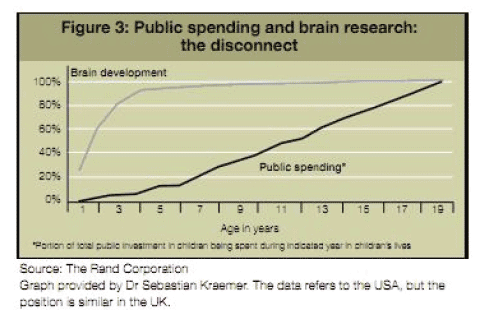
Such efforts require attention to the intervention mechanisms and structures supporting children and families and to the workforce (capacity and numbers). Sir Ian Kennedy also showed this mismatch graphically in data from the USA in terms of investment during the critical period of brain development in his recent report for the DoH 19 .
Figure 5: Public spending and brain development
Getting it Right for Every Child ( GIRFEC)
The Scottish policy Getting it Right for Every Child ( GIRFEC) 20 emphasises the collaborative nature of working with parents and their children, both between agencies at a strategic level and between those working directly with families. It sets out a comprehensive methodology for redesign of services focused on the child and their family and sets out to avoid duplication, to provide clear pathways of care and support and to produce a Child's Plan where additional input is needed. There are numerous examples of good practice in this domain, but significant case reviews of specific harm events to individual children have shown families may not be getting optimum support from one or several agencies because of ineffective use of resources or personnel, or poor communication or all three. Adoption of the GIRFEC principles in the context of the NHSScotland Quality Strategy 21 should enable best care for every child and young person.
Epidemiological Trends: 21 st century Morbidity
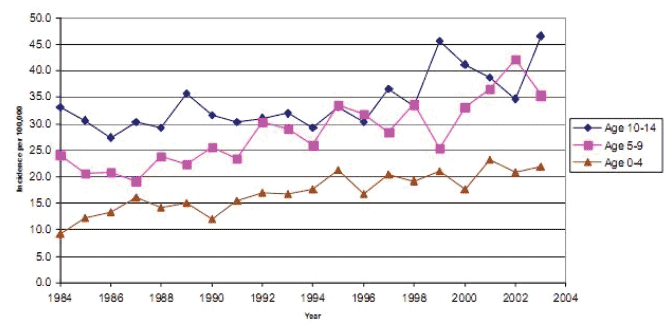
A change in the pattern of morbidity is also placing increased pressure on local and specialist services for children and young people. An increase has been observed in obesity amongst children, with 20% of all primary school entrants in Scotland having an overweight BMI and 8% measured as obese 22 . There has also been an increase in Type 1 diabetes with the fastest relative increase in under 5s and with Scotland having one of the highest incidence rates in the world.
Figure 6: Incidence of Type 1 Diabetes in Children in Scotland by Age at Diagnosis 23
Asthma also has a high prevalence causing 23% of all emergency hospital admissions of 15 years and under children in 2005/6 24 in Scotland. Mental health disorders amongst children and young people are worryingly prevalent at 8.5% of all children 25 . Children with complex needs, often consequent upon very low birth weight, are surviving longer, often into adult life and their care needs may be very intense. The UK Epicure study has shown 45% of children born before 26 weeks gestation exhibit severe functional disability at 11 years of age (Johnson, S et al 2009) 26 .
Children affected by a range of previously untreatable conditions are able to live longer due to advances in medical technologies, but they may require very demanding multi-agency packages of support at home and at school to enable them to be fully included. These packages can be enormously challenging for parents and the agencies who are striving to deliver them and require the highest standard of interagency working to devise and maintain 27 , and awe-inspiring dedication by their parents and carers.
Family supports are less strong than in former times and parents may be juggling with pressures of employment or seeking work, their own health and the needs of the other children in the family. UK public sector spending is now under pressure with both central government and local systems examining services closely in terms of effectiveness and efficiency. NHSiS is not exempt from this.
Responding to a Child and Family's Needs: Clear Pathways and Good Co-ordination
In order to respond to child and family needs in a timely and appropriate fashion, the health services for children need to be responsive and highly attuned to the needs of all and especially vulnerable families. Universal contacts in antenatal and postnatal settings need to be enabling of parents; adopt a strength-based approach such as has been demonstrated in the Family Nurse Partnership methodology (Olds) 28 and be able to respond to their concerns and enable quick referrals through defined pathways of care for children whose social, emotional or physical development causes concern.
All early years practitioners in health, social work and education and the third sector need to know how to access diagnostic, therapeutic and supportive services for children. The local multi-disciplinary team around the child should be cohesive and mutually supportive. The Scottish GIRFEC model of integrated working and the English equivalent "Every Child Matters" signpost evidence-based successful methodologies for the team around the child. However, firm evidence in terms of improved outcomes for individual children and families across the UK is limited 29 but a recent evaluation of the Highland GIRFEC pathfinder site 30 has shown significant improvements for both parents and professionals.
The care-co-ordination model which has recently been reviewed by Riddell et al 31 and GIRFEC principles also can assist in more effective working with the family by provision of a trained key worker, particularly at the various transition stages of a child's life.
The Key Role of Primary Care in Community Child Health
GPs, Paediatricians, nurses and therapists working in the community need to be both well-positioned in terms of their partners in the acute and specialist healthcare sector, but also firmly embedded and orientated in relation to local community services from both a case management and a planning perspective.
For a service encompassing the whole spectrum of care for children and young people to function effectively, all concerned have to share a vision for children and be confident in each other's skills and contributions, so that children who present through the screening process, or opportunistically to a variety of practitioners, can be referred and seen quickly by the appropriate clinician. Conversely, children presenting to acute settings with developmental or social problems can be seen and assessed by the paediatrician who can initiate investigations and refer the child to other colleagues within the multi-disciplinary team in the community such as early years workers, AHPs, social workers, educational or clinical psychologists, specialist peripatetic teachers etc. and keep the child under review to ensure ongoing support is given to the child and their family.
General Practitioners are an essential part of these mechanisms and contribute their knowledge of the whole family as it impinges on any particular child with problems. If mutual confidence does not exist then children may fall through the net and parents are left to negotiate their way through thickets of inter-professional rivalries, suspicions and unnecessary delays may be incurred.
In relation to paediatric expertise in primary care, concern was expressed by Professor Steve Field (outgoing Chair of RCGP) in 2010, about the lack of training of GPs in paediatrics (only 40% currently have had specific training) 32 , and initiatives are afoot to correct this. The recent RCGP "Child Health Strategy" 33 document has emphasised the need for additional training in paediatrics although this is mainly in the sphere of "the sick child". It also points out that currently less than 3% of the UK "Quality Outcome Framework" ( QOF) indicators for primary care relate to children and young people. The RCPCH "Facing the Future" report also draws attention to the need to enhance GP competencies in paediatrics. Wolfe et al (2011) recently reviewed outcomes for children across Europe and expressed concern about the primary to secondary care interface and a range of outcomes in comparison to other European systems of care for children 34 .
In his 2010 report for the Department of Health in England "Getting it right for children and young people", Sir Ian Kennedy recommended that "both initial training and revalidation (of GPs) should include the comprehensive care (author's font) of children and young people, as should the Quality and Outcomes Framework" because of the gaps he found in his enquiry.
Hopefully, GPs can gain more experience in paediatrics through extended training programmes and initiatives such as the NES GP paediatric scholarship scheme 35 and through access to improved CME. They have a vital role as navigators through the health system for parents and children with difficulties and disorders and will often take over the lead role after a young person with additional support needs leaves school.
Contact
- Mary Sloan mary.sloan@gov.scot