Developing a community child health service for the 21st century
A report on a review of the community child health service in Scotland.
Section 8: CCH workforce briefing
This examination of the medical workforce issues affecting CCH would not have been possible without the support of the Workforce Officer of the RCPCH and colleagues in NHS Education Scotland and the Scottish Government.
The current "trained doctor" workforce in paediatrics comprises consultants and specialist doctors who were formerly known as staff and associate specialist grade doctors ( SASG). For convenience the latter designation is used.
When enumerating trained doctors in paediatric services the RCPCH census describes them in four categories:
- Specialist - working in tertiary centres with subspecialty interests and accreditation
- General - Working as general paediatricians
- Combined - contributing to both acute and community paediatric services and
- Community - Working most of the time in community settings
Figure 9: Present Configuration of the Paediatric Workforce in Scotland
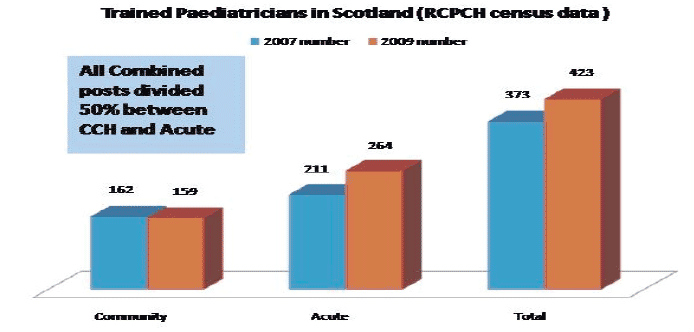
Figure 10: All Career Grade Paediatricians by Gender 2009 ( RCPCH Census)
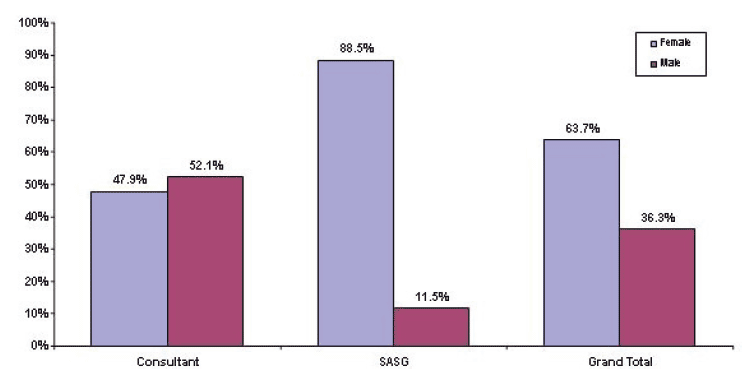
The proportion of trained paediatricians (consultants plus SASG), working in the community has fallen in Scotland from 43% in 2007 to 38% in 2009 and there has been a 16% fall in the number of community consultants in Scotland since 2007 even if "combined" posts are included pro-rata (see Figure 11). Simultaneously there has been a 47% increase in acute paediatric subspecialty consultants including neonatology.
Figure 11: Consultant Paediatricians in Scotland 2007-9 ( RCPCH Census 2009)
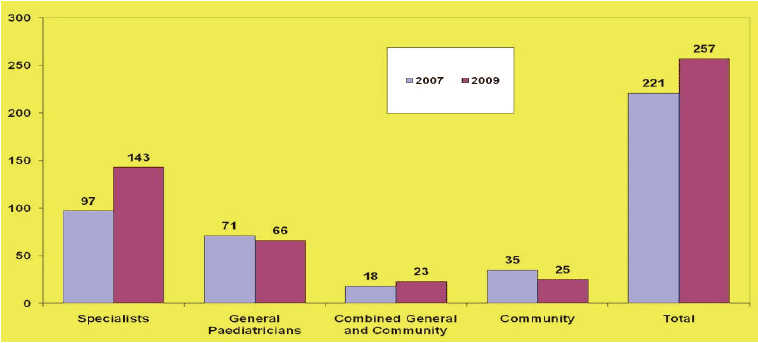
This mirrors the trend over the past 20 years experienced across the UK. In data provided by Dr Cliona Ni Bhrolchain 55 (Figure 12), it is easy to see that the proportion of trained paediatricians in the UK working in CCH has decreased markedly in relation to those working in acute paediatrics over the past 20+ years. Across the UK in 2007 about 38% of all trained paediatricians worked in community having been around 78% in 1988.
Figure 12: Proportion of trained Paediatricians in CCH/Acute (C.Ni Brolchain 2008)
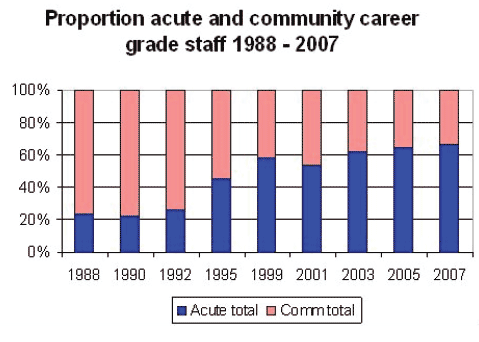
Why Have CCH Numbers Lagged Behind Acute Paediatrics?
Despite clinical pressures on CCH services, there has not been investment in the medical workforce akin to that in the acute sector. Unfortunately, CCH activity has been ill-defined across the UK apart from a few beacon sites such as Derby 56 , and the persistence of paper records (see Health Board survey results) in many services across Scotland has meant that arguing for workforce increases has been difficult to justify with good data.
Where excessive CCH clinic waiting times are recorded, scrutiny would suggest that staffing pressures may be contributing to excessive waits. Often, pressures from the acute sector have taken precedence over CCH when resources are tight and posts may be redesignated as acute posts. Short-sightedly, it has been said that " no child dies if CH services are cut". Unfortunately, there is no cost-benefit analysis available for the CCH service to the author's knowledge.
In recent times in Scotland, consultants have been appointed to combined posts ( ie with both an acute and CCH role) but these numbers appear to be small (18 in 2007, 23 in 2009) although the SACCH questionnaire revealed that quite a few general paediatricians undertake CCH duties without being recognised as such. The RCPCH has been encouraging development of such posts in the Modelling the Future documents 57 , especially in the DGH setting.
The Role of Specialty and Associate Specialist Grade (previously SASG) Doctors
Although it is recommended that there should be consultant-led CCH services, CCH still relies on a substantial cadre of experienced SASG or specialist doctors (the new term for trained paediatricians below consultant grade) who deliver a large proportion of the current clinical CCH service with some SASG doctors also contributing to the acute and specialist care of children.
Figure 13: SASG Doctors in Paediatrics in Scotland 2007-9 ( RCPCH Census 2009)
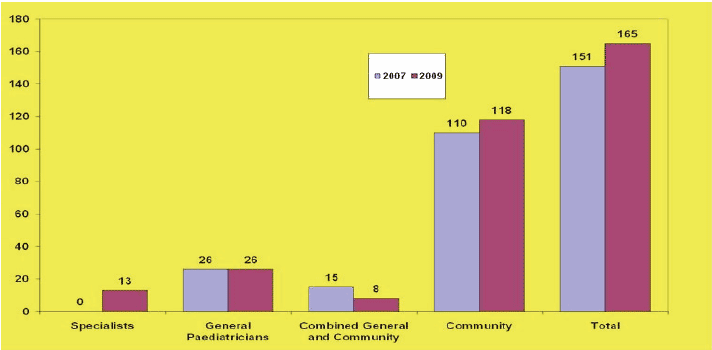
Over the past 10 years or so the proportion of SASG doctors in all paediatric specialities in Scotland has reduced from 50% in 1999 to 39% in 2009. In 2009, SASG doctors made up 39% of the total trained paediatric workforce in Scotland 58 .
However there has been little change in CCH where SASG make up 77% of the total CCH workforce, which means that any future workforce plan needs to factor in their considerable contribution.
Age Demographics
The age profile of paediatricians varies between those practising acute and community paediatrics and between consultants and SASG doctors with CCH and SASG doctors being in general older.
Currently 64% of all consultant paediatricians in Scotland are over 50 years of age versus 72% of SASG 59 doctors. Although retiral at 65 will not be compulsory, present patterns indicate the majority of doctors will be retired by age 65, therefore there will be a need to replace the retirees and/or redesign work presently done by these doctors over the next 10+ years.
Figure 14: Acute and Community Consultants UK - Age Profile % ( RCPCH Census 2009)
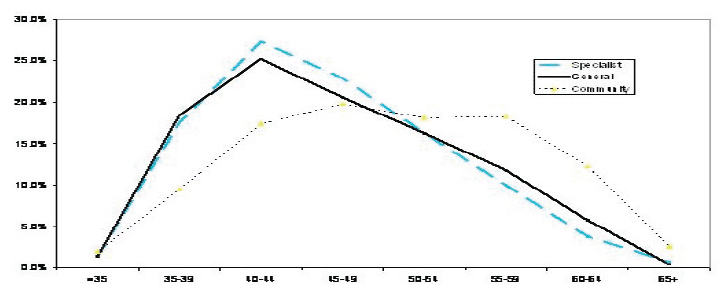
Figure 15: Age of Paediatricians by Grade in Scotland (2010) ( ISD Scotland 2010)
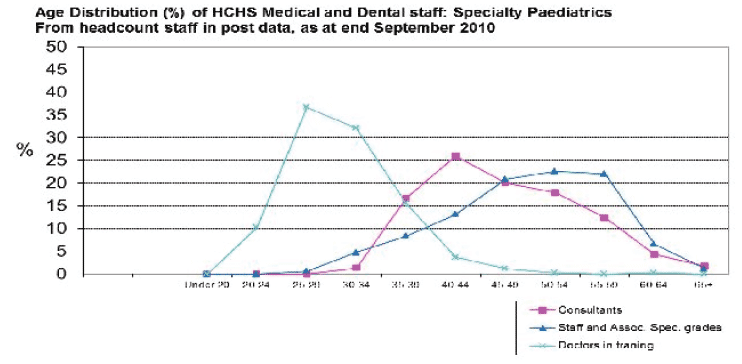
Figure 16: Proportion of UK Paediatric Consultants Under and Over 50 by Specialty ( RCPCH Census 2009)
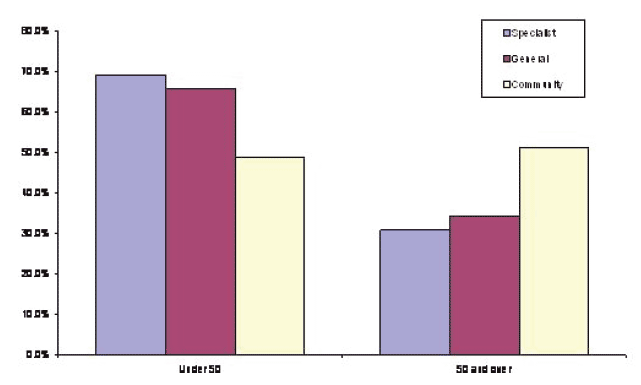
Figure 16 above shows a clear division between the under and over 50s, with more younger consultants in general and specialist paediatrics and more CCH consultants in the older age group. This confirms the trend towards acute specialties over the past 20 years.
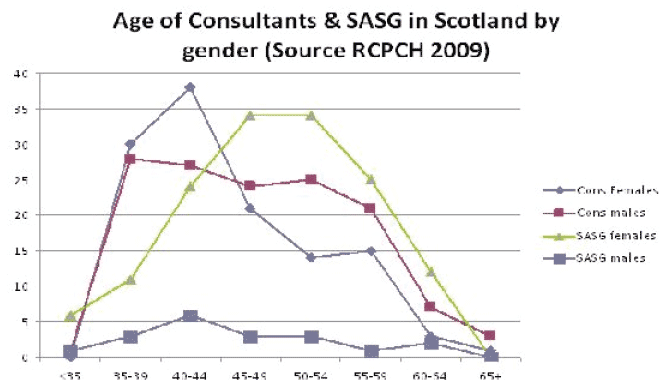
In the Scottish profile below (Figure 17), there is a clear bulge in the number of over 45 SASG female paediatricians (of whom we know about three-quarters work in CCH), but also a peak of female consultant paediatricians of 40 and under.
The implication of these age facts is that currently demand for replacements is exceeding supply, and that younger paediatricians are tending to go into acute and specialist posts.
Figure 17: Consultants and SASG Paediatricians by age in Scotland ( RCPCH Census 2009)
Contact
- Mary Sloan mary.sloan@gov.scot