Coronavirus (COVID-19): mental health tracker study - wave 2 report
Wave 2 findings (data collected from 17 July and 17 August 2020) indicate increased rates of suicidal thoughts, no significant changes in rates of depression or anxiety, and an improvement in most other indicators of mental health and wellbeing, compared to Wave 1 (data from 28 May to 21 June 2020)
4. COVID-19 Contextual Factors
This section provides a summary of respondents' experiences of, and views on the easing of the COVID-19 restrictions during phase 3 of the COVID-19 Routemap from the 17th July to 17th August 2020 (see annex Sections 2-4 for further details). Some of the items in this section were included at Wave 1 and Wave 2. This section also includes items specific to the phase 3 of the COVID-19 route map which assessed people's experiences during the easing of lockdown restrictions in order to provide an understanding of the context in which respondents were living while they responded to the mental health and wellbeing focussed questions in the Wave 2 SCOVID Mental Health Tracker Study questionnaire. Tracking these contextual factors is useful in understanding whether particular factors are correlated with certain mental health outcomes as findings from subsequent waves of this tracker study are gathered.
4.1 COVID-19 related experiences
Of the Wave 2 sample, 0.8% of respondents reported that they had been diagnosed with COVID-19, and 6.8% reported that they had not been diagnosed but suspected they had contracted COVID-19. Over three quarters of this group (78.5%) reported self-isolating as a result of their symptoms. 12.5% of respondents reported that they knew someone diagnosed with COVID-19 and 2.9% of respondents reported having lost friends or family members to COVID-19.
4.1.1 Summary of views on COVID-19
Respondents were asked a series of questions about their views and experiences of COVID-19 and the related restrictions.
- Respondents reported feeling that COVID-19 affected their lives less severely and that they were less emotionally impacted by the virus compared to the Wave 1 survey. However, there was no change in level of life satisfaction reported by respondents between Waves 1 and 2.
- Respondents felt less concerned about COVID-19 and felt there were higher levels of control over COVID-19, compared to the Wave 1 survey.
- Consistent with Wave 1, roughly half of respondents (55.5%) felt they had an 'average' chance of contracting COVID-19, a fifth of the sample felt they had a lower than average (20.0%) chance, and almost a fifth of respondents felt they had a greater than average chance (19.8%) compared to others of the same sex and age.
- Respondents viewed social distancing and lockdown measures to be just as necessary to help prevent the spread of COVID-19 at Wave 2 as at Wave 1.
- The majority of respondents reported that they had been following the guidelines regarding social distancing and COVID-19 prevention measures in the two weeks prior to their completion of the Wave 2 survey (see table G in annex) at all times or often. There were no significant differences between subgroups regarding adherence to the government guidelines. This is consistent with Wave 1.
Wave 2 specific items
- Respondents with pre-existing mental (52.6%) or physical (42.1%) health conditions reported feeling negatively affected by the fact that others seemed to be living more normally than they were.
- Respondents with pre-existing physical health conditions and the 60+ age group showed the highest levels of concern about the occurrence of a second wave of COVID-19.
- Three quarters of the sample (84.6%) at Wave 2 felt the Scottish Government guidance on Phase 3 COVID-19 restrictions were easy to understand.
Interacting with others
At Wave 2, respondents indicated higher levels of concern (6.9/10) around interacting with people they didn't know, and these individuals' ability to adhere to COVID-19 restrictions than interacting with people they did know (4.8/10). The areas of concerns varied across key groups.
- Women were more concerned than men about being in close proximity to others, interacting with strangers and strangers' ability to adhere to guidelines.
- Women were more concerned about catching COVID-19 at work than men.
- Respondents in the 60+ age group were more likely to be concerned about being in close proximity to others, interacting with both people they know and strangers, and stranger's ability to adhere to guidelines than the younger age groups.
- Respondents in the youngest age group (18-29 year olds) were more likely to express concern over their own willingness/ ability to follow the restrictions than the older age groups.
- Those from the lower SEG were more concerned than those from the higher SEG about interacting with people, and their own willingness/ability to follow the restrictions when interacting with people they know
- Respondents with pre-existing mental health conditions were more concerned than those without about being in close proximity to others, interacting with both people they know and strangers and stranger's ability to adhere to guidelines.
Support seeking
- Compared to Wave 1, respondents at Wave 2 reported feeling more willing to contact their GP about a non-COVID-19 related health concern (Wave 1 average = 6.9, Wave 2 average = 7.2).
- There was no change in respondent's willingness to seek professional help for their mental health between Waves 1 and 2. Most respondents reported being willing to seek help (on a scale of 0-10 with 10 indicating high willingness, the average was 7.5).
4.2 General health and lifestyle factors during COVID-19
This section presents a brief breakdown of physical health, sleep, activity levels, and other lifestyle factors at Wave 2. Comparison to Wave 1 will not be made in this section, however Wave 1 data can be found in section 4.2 of the Wave 1 report. Wave 2 findings suggest that respondents felt that their overall health was reasonably good. Respondents with pre-existing mental or physical health conditions reported worse perceptions of their health compared to those without pre-existing mental or physical health conditions.
4.2.1 Perceptions of overall health
At the time of the Wave 2 survey, most respondents (64.4%) reported that their health was 'very good' (16.5%) or 'good' (47.9%). Around a quarter (25.3%) reported their health as 'fair', and around one in ten felt their health was either 'poor' (8.0%) or 'very poor' (1.9%).
Looking more closely at the data, there were some differences in reports on perceived health according to groups categorised by background factors:
- Respondents in the youngest age group (18-29 years) (2.6%) were least likely to report feeling their health was poor or very poor compared to 30-59 year olds (11.0%) and the 60+ years group (13.4%).
- Women and respondents from lower SEG were more likely to report poorer general health than men and higher SEG.
- Around 40% of respondents with pre-existing mental (43.4%) or physical health conditions (38.7%) reported poor or very poor general health compared to those without a pre-existing mental (5.1%) or physical health (2.6%) conditions.
4.2.2 Sleep
This section presents a brief overview of respondents' sleep in the week prior to Wave 2. Respondents were asked how they felt their sleep quality had been in the week prior to the Wave 2 survey, and this information is illustrated in Figure 4.1. The data indicates that the highest proportion of respondents (37.7%) rated their sleep as 'average', a quarter of respondents rated their sleep as good (24.7%) while a fifth felt their sleep had been poor (19.4%), and close to a tenth rated their sleep as either very good (9.5%) or very poor (8.6%).
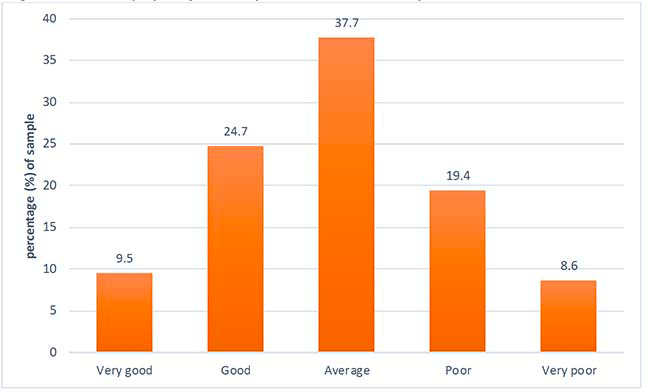
Image description
This figure shows how respondents rated their sleep quality in the past week at Wave 2.
It indicates that the highest proportion of respondents (37.7%) rated their sleep as ‘average’, a quarter of respondents rated their sleep as good (24.7%) while a fifth felt their sleep had been poor (19.4%), and close to a tenth rated their sleep as either very good (9.5%) or very poor (8.6%).
A more detailed analysis of the sleep data shows that there were some subgroup differences by background:
- Interestingly, young adults (18-19 year olds) were most likely to report having good (27.7%) or very good (11.1%) sleep quality compared to those aged 30-59 years (good 21.8%, very good 8.1%) and those in the 60+ years age group (good 27.2%, very good 10.6%).
- The middle age group (30-59 year olds) were more likely to report poor (19.4%) or very poor (11.0%) sleep compared to around a quarter of respondents in the 60+ years age group (poor 18.0%, very poor 6.4%) and third of the youngest age group (poor 21.4%, very poor 6.4%).
- Women were more likely to report poor (21.3%) or very poor (10.6%) sleep compared to men (poor 17.5%, very poor 6.5%). Respondents from the higher SEG were more likely to report experiencing poor sleep (20.9%) than those from the lower SEG (17.0%). Whereas the lower SEG were more likely to report very poor (12.5%) sleep compared to the higher SEG (6.3%).
Sleep quality differed starkly among respondents with or without pre-existing mental health conditions:
- Over half of respondents with pre-existing conditions reported poor (21.2%) over very poor (29.8%) sleep quality in the past week, compared to under a quarter (poor 19.1%, very poor 5.6%) of those with no mental health condition.
- Less than 15% of those with a pre-existing mental health condition reported good sleep quality (very good 4.2%, good 10.3%) compared to over a third (very good 10.3%, good 26.8%) of those with no condition.
4.2.3 Lifestyle factors
Lifestyle factors can be an important factor in an individual's mental and physical wellbeing. This section presents a brief breakdown of respondents' lifestyle factors at Wave 2. At Wave 2, survey respondents were asked to indicate whether, in comparison to their usual behaviours, they felt that they had done various activities 'Less than usual', 'About the same' or 'More than usual' in the week prior to the questionnaire. The lifestyle factors and behaviours included alcohol use, smoking, drug use (other than prescription or over the counter medicines), online gambling, and physical activity. The following section provides a brief overview of these lifestyle factors, noting significant differences by subgroups.
Alcohol
Just over a third of respondents (36.2%) reported not drinking alcohol in the past week. Around 40% (38.7%) reported no changes in their drinking in the past week, 15.1% reported drinking less than usual while 10.1% of respondents felt they had drunk more than usual.
Smoking
The majority of the sample (79.5%) reported not smoking during the previous week. Under 10% of the sample reported changes in smoking behaviour with 1.4% of respondents reporting having smoked less than usual, while 4.9% felt they had smoked less than usual.
Drugs
The majority of the sample (88.5%) reported not using drugs, 2.0% of the sample reported increased drug use in the previous week prior compared to their usual usage, while 0.8% reported decreased use.
Gambling
The majority of the sample reported not engaging in online gambling (80.4%) in the week prior. Of respondents who did gamble online, the majority (63.8%) reported no change in their gambling in the preceding week and around a fifth (22.9%) reported gambling less than usual and 13.1% reported gambling more than usual.
Physical Activity
This section reports on how many days in the last week respondents had engaged in moderate or vigorous physical activity for 15 minutes or more. Over 40% (42.6%) of respondents rated being able to exercise more easily as a positive of the easing of lockdown. Overall, respondents reported engaging in exercise for an average of just under 3 days per week (mean= 2.85). The younger age groups (18-29 and 30-59 year olds) and those from higher SEG's reported engaging in significantly more vigorous physical activity compared to the 60+ group and those from lower SEGs.. Additionally, those without pre-existing mental or physical health conditions reported more vigorous activity than those with pre-existing mental or physical health conditions.
4.3 Support network and emotional support
This section presents an overview of respondents' emotional and social support at Wave 2. Given the possibility that people would be isolated from their usual support networks due to the COVID-19 restrictions, Wave 2 asked respondents how connected they felt to friends, family, colleagues, and their community during the COVID-19 lockdown. For the purposes of this report, those who reported being quite a bit, moderately or extremely connected were grouped in the category of 'Connected', and those who reported feeling not or a little bit connected were grouped as being 'Not connected'.
Those that felt the most connected included:
- Young adults (18-29 years) felt more connected to friends while 30-59 year olds felt more connected to colleagues than the other age groups.
- Women felt more connected to family than men whereas men felt more connected to colleagues.
- Those in the higher SEG felt more connected to family, friends, and colleagues than those in the lower SEG
- Respondents without pre-existing mental or physical health conditions felt more connected to family, friends, colleagues, and community than those with pre-existing mental or physical health conditions
4.3.1 Support Network
Family and Friends
The majority of the sample (71.1%) felt connected to family, while half the sample felt connected to friends (50.0%) only around a quarter (26.6%) felt connected to colleagues and a fifth (19.7%) felt connected to their community.
Differences in feelings of social connectedness to friends or family were found for different groups based on age and sex and background:
- Young adults (18-29 year olds) were more likely to report feeling connected to their friends (60.0%), followed by older people (50.5%), and then the middle age (30-59 years old) group (45.1%).
- Women were more likely to feel connected to family (73.1%) than men (68.9%). Respondents from the lower SEG were less likely to feel connected to family (31.9%) and friends (55.2%) compared to those from a higher SEG (family 27.2%, friends 46.9%).
Living with an illness also correlated with different reports of connectedness:
- Respondents with pre-existing mental (41.7%) or physical health (37.5%) conditions were much less likely to feel connected to family compared to respondents without a pre-existing mental (27.1%) or physical (26.8%) health condition.
- Two thirds of respondents with pre-existing mental (69.6%) or physical (62.9%) health conditions felt connected to friends compared to just under half of those a pre-existing mental (47.2%) or physical (46.8%) health condition.
Colleagues and Community
Around a quarter (26.6%) of the whole sample felt connected to their colleagues, although this included people who may not work or had been furloughed. A fifth (19.7%) of the overall sample reported feeling connected to their community. Difference arose across subgroups such as age, sex, background and health status:
- 38.6% of the youngest age group reported feeling connected to their colleagues compared to a third (29.7%) of 30-59 year olds and 13.2% of the 60+ age group. Around a third (32.5%) of men reported feeling connected to colleagues compared to a fifth of women (21.1%).
- Respondents from the higher SEG were more likely to feel connected to colleagues (30.2%) than those from the lower SEG (20.5%).
- Those with a pre-existing mental health condition were less likely to feel connected to colleagues than those without a pre-existing condition (9.6% vs 29.0%). They were also much less likely to report feeling connected to their community (87.5%) compared to those with no pre-existing mental health condition (79.2%).
- Respondents with a pre-existing physical health condition were less likely to feel connected to colleagues than those without a pre-existing physical health condition (9.0% vs 30.9%). They were also less likely to feel connected to their community (87.4%) compared to without a pre-existing physical health (78.5%).
4.3.2 Emotional support
This section presents a breakdown of sources of emotional support respondents used in the month prior to Wave 2. Sources of emotional support included family, counsellors, GP, and NHS services. The findings for the whole sample are displayed in Table 4.2 below, with the percentage of people who had made contact with a particular source prior to COVID-19, and during or before the Wave 2 period of this study.
Friends and family were the most used source of support and NHS 24 was least used. Young adults (18-29 years old) were most likely to make use of the supports available. Women were more likely to have sought support from friends and family, while men were more likely to access resources online or by telephone.
| Source of support | Respondents accessing in month prior to Wave 2 survey (%) |
|---|---|
| Friends or family | 39.9 |
| Professional counselling or therapy (via telephone, online or face-to-face) | 6.8 |
| GP or community health worker (e.g. health visitor, midwife, pharmacist) | 9.7 |
| NHS 24 111 telephone service | 5.1 |
| NHS Inform/Shielding support telephone line | 6.6 |
Differences in use of support:
- The youngest age group were more likely to report having contacted friends and family for emotional support (63.0%) than the 30-59 year olds (39.7%) and the 60+ group (23.4%). They were also more likely to have used professional counselling or therapy services (15.5%) than the other age groups (30-59 6.4%, 60+ 1.0%). The youngest age group were more likely to report having contact with a GP or community health worker (15.9%) than the 30-59 year olds (8.5%) and the 60+ group (7.2%). The youngest age group were more likely to report using NHS 24 (9.7%) than the 30-59 year olds (4.2%) and the 60+ group (3.1%). The youngest age group were also more likely to report using NHS Inform/Shielding support telephone line (16.1%) than the 30-59 year olds (5.1%) and the 60+ group (2.2%).
- Women were more likely to have contacted friends and family for emotional support (47.2%) than men (32.0%). Men were more likely to have contacted NHS 24 (6.5%) or to have used NHS Inform/Shielding support telephone line (8.6%) than women (NHS 24 3.7%, NHS Inform 4.7%).
- Respondents with a pre-existing mental health condition were more likely (53.5%) to have contacted friends and family for emotional support than those with no pre-existing condition (37.9%). Those with a pre-existing mental health condition were also more likely to have used professional counselling or therapy services (10.3%) compared to those with no pre-existing condition (6.2%). Respondents with a pre-existing mental health condition were more likely to report contact with GP or community health worker (18.2%) than those with no pre-existing mental health condition (8.5%). Respondents with a pre-existing mental health condition were more likely to have contacted NHS Inform/Shielding support telephone line (9.9%) compared to those without (6.2%).
- Respondents with a pre-existing physical health condition were less likely (34.7%) to have contacted friends and family for emotional support than those with no pre-existing condition (41.1%). Those with a pre-existing physical health condition were also less likely (4.6%) to have used professional counselling or therapy services than those with no pre-existing physical health condition (7.2%). Those with a pre-existing physical health condition were also less likely (3.0%) to have used NHS 24 than those with no pre-existing physical health condition (5.6%).
- Respondents from the lower SEG more frequently reported using professional counselling or therapy services (8.4%) than higher SEG (5.7%). Those from lower SEG were more likely (11.9%) to report having contact with a GP or community health worker than higher SEG (8.4%). Respondents from the lower SEG were more likely to report using NHS Inform/Shielding support telephone line (9.3%) than higher SEG (5.0%).
4.4. Finances during easing of lockdown
Respondents were asked questions around work status and financial security during the Wave 2 study period. Overall, just under half of respondents (46.1%) reported that their job had changed in some way during the COVID-19 pandemic. As displayed in Figure 4.2, at Wave 2 the most commonly reported changes were:
- 13.9% of the sample were working from home,
- 11.8% were furloughed,
- 7.1% of respondents a reduction in paid employment hours.
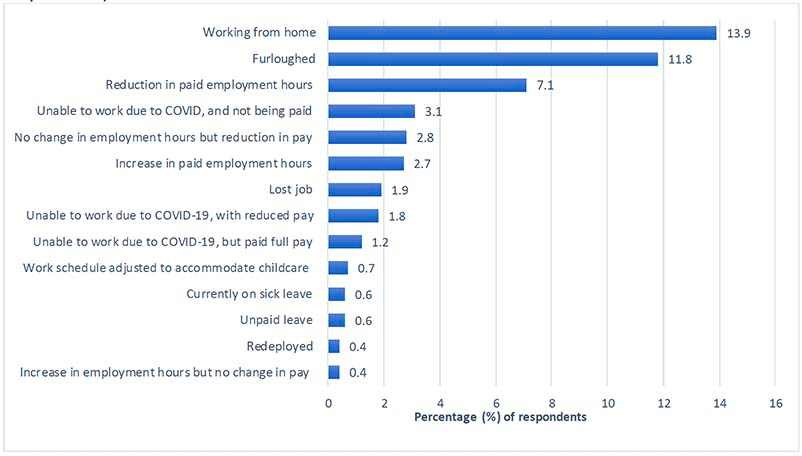
Image description
This figure shows changes to job role experienced during COVID-19 pandemic by percentage of respondents at Wave 2. The most commonly reported changes were: 13.9% of the sample were working from home, 11.8% were furloughed, 7.1% of respondents a reduction in paid employment hours. Less commonly reported changes were: 3.1% were unable to work due to COVID, and not being paid, 2.8% had no change in employment hours but reduction in pay, 2.7% had an increase in paid employment hours, and 1.9% lost their job, 1.8% were unable to work due to COVID-19, with reduced pay and 1.2% were unable to work due to COVID-19, but paid full pay. The following categories made up less than 1% of the sample, each: work adjusted to accommodate childcare, currently on sick leave, unpaid leave, redeployed, increase in employment hours but no change in pay.
To assess perceived financial coping during COVID-19 in Wave 2 of the SCOVID Mental Health Tracker Study, respondents were asked: "How well would you say you are managing financially these days?" Responses ranged from 'living comfortably' to 'doing alright', to 'just about getting by', to 'finding it quite difficult' to 'finding it very difficult'. At the time of the Wave 2 survey:
- Just under a quarter (23.4%) of respondents felt they were living comfortably
- 43.2% of respondents reported doing alright,
- Under a quarter (23.7%) said they were just about getting by,
- 6.1% were finding it quite difficult and 3.6% finding it very difficult financially.
Particular groups within the sample reported finding things more difficult financially, in particular 30-59 year olds, women, and respondents with pre-existing mental health conditions.
- Across all age groups over 40% of respondents felt they were doing alright financially (18-29 41.2%, 30-59 41.5%, 60+ 47.1%).
- Only 17.6% of the 30-59 year olds felt they were living comfortably compared to 23.0% of 18-29 year olds and 32.9% of the 60+ group.
- Financial difficulties were more likely to be reported by 30-59 year olds (quite difficult 8.5%, very difficult 4.6%) feeling compared to the youngest (quite difficult 4.7%, very difficult 4.4%) and oldest age (quite difficult 3.4%, very difficult 1.3%) groups.
- Women were less likely to feel they were coping well financially (living comfortably 19.9%, quite difficult 7.7%) compared to men (living comfortably 27.3%, quite difficult 4.5%).
- The most stark contrast was in those with and without a pre-existing mental health condition. Those with a condition were 3 times more likely (24.3% vs 7.6%) to report feeling financial difficulties (quite difficult 16.0%, very difficult 8.3%) compared to those with no pre-existing condition (quite difficult 4.7%, very difficult 2.9%).
4.5 Trust in others and authorities
Trust is an important indicator of how confident people are in society more widely. In Wave 2 of the SCOVID Mental Health Tracker Study, Trust towards others (people and strangers) and the authorities (police, NHS, UK, and Scottish governments) was assessed.
4.5.1 Trust in others
Two statements were used to assess trust in others: 'In general one can trust people' and 'When dealing with strangers it is better to be careful before you trust them'. Response options were 'strongly disagree', 'disagree', 'agree' and 'strongly agree. Two thirds of the sample (68.5%) agreed or strongly agreed that on the whole, people could be trusted.
Differences in subgroups arose by age and health status:
- Respondents in the 60+ year age group were more likely to reported feeling that people were generally trustworthy (78.1%) compared to two thirds (65.0%) of 30-59 year olds and 62.6% of 18-29 year olds.
- Respondents with no pre-existing mental health conditions were more likely to report feeling that people were generally trustworthy (71.2%) compared to respondents with pre-existing mental health conditions (49.4%).
- Those with no pre-existing physical health conditions were more likely to report feeling that people were generally trustworthy (69.3%) compared to respondents with pre-existing physical health conditions (65.2%)
The majority of respondents (88.9%) agreed or strongly agreed that it was better to be careful when dealing with strangers. Differences arose by age and health status:
- The younger age groups were more likely to disagree with the sentiment that it is better to be careful of strangers before you trust them. Over a tenth of the 30-59 year olds (13.5%) and the 18-29 year olds (11.4%) disagreed compared to 7.0% of the 60+ years age groups. Respondents with no pre-existing physical health conditions were more likely to disagree about the need to be careful with dealing with strangers (11.8%) compared to respondents with pre-existing physical health conditions (8.0%).
4.6 Interpersonal harm
This section gives a brief overview of the findings about respondents' recent experiences of physical harm and bullying or psychological harm in the 2 weeks before the Wave 2 questionnaire.
Overall, 3.3% of respondents reported that they had been physically harmed by another person in the prior 2 weeks. Additionally, 3.7% of respondents reported experiences of being bullied, controlled, intimidated or psychologically hurt by somebody else.
Particular groups within the sample reported higher rates of interpersonal harm than their subgroup counterpoint:
- Young adults (18-29 years) reported more physical and psychological harm
- Women reported higher rates psychological harm than men
- Those in the lower SEG reported higher rates of physical harm
- Those with a pre-existing mental health condition reported higher physical and psychological harm
- Those with a pre-existing physical health condition reported higher psychological harm
Contact
Email: socialresearch@gov.scot