Coronavirus (COVID-19): mental health tracker study - wave 2 report
Wave 2 findings (data collected from 17 July and 17 August 2020) indicate increased rates of suicidal thoughts, no significant changes in rates of depression or anxiety, and an improvement in most other indicators of mental health and wellbeing, compared to Wave 1 (data from 28 May to 21 June 2020)
3. Mental Health Outcomes
This section reports on the main mental health and wellbeing outcomes for Wave 2 of the SCOVID Mental Health Tracker Study. The main aim of this section is to report changes in these outcomes from Wave 1 (28th May to 17th June 2020) to Wave 2 (17th July and 17th August 2020). Wave 1 findings suggested that several key groups reported poorer mental health outcomes, and subgroups[16] who reported poorer outcomes in Wave 2 are also reported in this section. Only statistically significant changes and subgroup differences are reported here.
The main mental health outcomes focused on were: depressive symptoms, anxiety symptoms, suicidal thoughts, severity of potential mental health problems as measured by the general health questionnaire (GHQ), and mental wellbeing. The study also included other correlates of mental wellbeing, such as loneliness, defeat, entrapment, social support, resilience, distress, life satisfaction; with these findings reported more briefly.
In addition, respondents were asked 'Currently, how is your mental health?' (Very good, Good, Fair, Poor, Very poor) at Wave 1 and again at Wave 2. Fewer people reported poor or very poor mental health at Wave 2 (15.4%) than Wave 1 (17.9%), and more people reported very good, good or fair mental health at Wave 2 (84.5%) than Wave 1 (82.1%).
3.1 Suicidal thoughts
To measure suicidal thoughts, respondents were asked: 'how often have you thought about taking your life in the last week?', and were provided with options that ranged from "Never", "One day", "Several days", "More than half the days", "Nearly every day", and "I would rather not answer". For the purposes of this report, respondents who experienced any suicidal thoughts in the week prior to the Wave 2 questionnaire (i.e., one day or more) were included in the suicidal thoughts findings.
Changes between Waves 1 and 2
For the overall sample, there was a significant increase in the proportion of respondents reporting suicidal thoughts from 9.6% of respondents in Wave 1 to 13.3% of respondents in Wave 2.
From Wave 1 to Wave 2, the proportion of several subgroups reporting suicidal thoughts increased, including:
- A higher proportion of men reported suicidal thoughts at Wave 2 than Wave 1
- In particular, a higher proportion of young men (18-29 years) reported experiencing suicidal thoughts, though this finding should be treated with caution due to small sample size at Wave 2.
- A higher rate of respondents with a pre-existing mental health condition reported suicidal thoughts at Wave 2 than Wave 1
The proportion of men experiencing suicidal thoughts increased significantly from Wave 1 (10.2%) to Wave 2 (16.3%). This is particularly evident for the young men (18-29 years) subgroup, there was a significant increase in the proportion reporting having suicidal thoughts from 21.5% at Wave 1 to 34.4% at Wave 2 (Table 3.3). It should however be noted that the young men subgroup experienced a notable dip in response rate in Wave 2 and as such, this finding should be interpreted with caution due to the small sample size. There were no other significant changes in rates of suicidal ideation from Wave 1 to Wave 2 for age groups.
Looking more closely at the subgroups based on background and health, the rate of those with a pre-existing mental health condition reporting suicidal thoughts in the week prior increased from 25.2% in Wave 1 to 36.7% in Wave 2. There were no further significant increases or decreases in rates of suicidal thoughts from Wave 1 to Wave 2 for any of the subgroups.
| Wave 1 | Wave 2 | |||||
|---|---|---|---|---|---|---|
| Men % | Women % | All adults % | Men % | Women % | All adults % | |
| 18- 29 years | 21.5 | 16.1 | 18.8 | 34.4 | 17.2 | 26.3 |
| 30- 59 years | 9.6 | 11.4 | 10.6 | 14.6 | 13.3 | 13.9 |
| 60+ years | 3.0 | 1.0 | 2.0 | 5.3 | 2.1 | 3.6 |
| Total % | 10.2 | 9.1 | 9.6 | 16.3 | 10.5 | 13.3 |
Wave 2 Findings
The Wave 2 data found that 13.3% of respondents experienced suicidal thoughts within the week prior to completing the survey.
Similar to the Wave 1 report, several subgroups reported higher rates of respondents experiencing suicidal thoughts than their subgroup counterpart including:
- young adults (aged 18-29 years),
- those with pre-existing mental health or physical health condition,
- and people from a lower SEG.
There were some differences in rates of suicidal ideation by age and sex, as illustrated in Table 3.3. A higher proportion of men reported suicidal thoughts in the previous week (16.3%) than women (10.5%), which contrasted to Wave 1, where no sex differences were found. A higher proportion of young adults (18-29 years) reported suicidal thoughts (26.3%) than those aged 30-59 years (13.9%) and the older age group (60+ years) (13.3%).
Apart from age and sex, there was additional evidence of differences in rates of respondents reporting suicidal thoughts by health and background factors at Wave 2. Specifically, people with a pre-existing mental health condition were more likely to report suicidal thoughts (36.7%) than those without a pre-existing mental health (10.2%). Additionally, people who had a pre-existing physical health condition (16.7%) reported higher rates of suicidal ideation than those without a pre-existing physical health condition (12.5%). Further, respondents from a lower SEG reported higher rates of suicidal thoughts at Wave 2 (17.1%) than those from a higher SEG (11.1%). These subgroups did not report any significant changes in rate of suicidal ideation from Wave 1 to Wave 2.
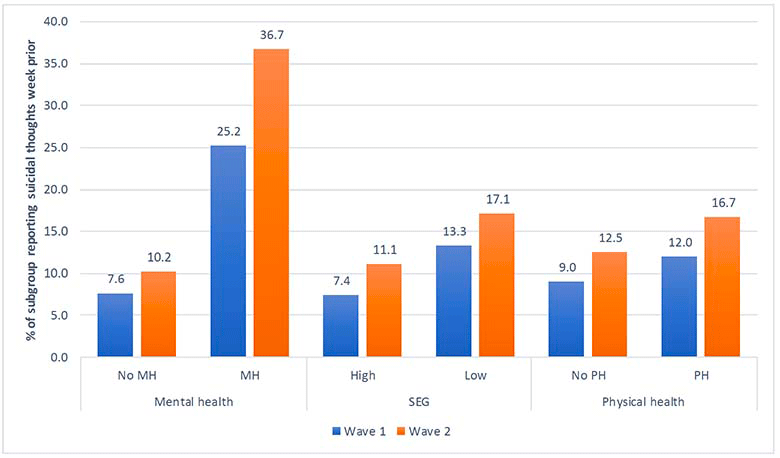
Image description
This figures shows rates of suicidal thoughts in the week prior to Wave 1 and Wave 2 by pre-existing mental health (MH) condition, socio-economic group (SEG), and pre-existing physical health condition.
The figure shows that for respondents without a pre-existing mental health condition 7.6% reported suicidal thoughts at Wave 1 compared to 10.2% at Wave 2. For respondents with a pre-existing mental health condition, 25.2% reported suicidal thoughts at Wave 1 compared to 36.7% at Wave 2.
The figure shows that for respondents from the high socio-economic group, 7.4% reported suicidal thoughts at Wave 1 compared to 11.1% at Wave 2. For respondents from the low socio-economic group, 13.3% reported suicidal thoughts at Wave 1 compared to 17.1% at Wave 2.
The figure shows that for respondents without a pre-existing physical health condition 9% reported suicidal thoughts at Wave 1 compared to 12.5% at Wave 2. For respondents with a pre-existing physical health condition, 12% reported suicidal thoughts at Wave 1 compared to 16.7% at Wave 2.
Findings suggest that employment factors were associated with people's experience of suicidal thoughts in the week prior to the Wave 2 survey. Specifically, more respondents in a key worker role (17.1%) reported suicidal thoughts compared to non-key workers (12.5%). Further, respondents who experienced a change to their working status reported higher rates of suicidal thoughts (16.5%) compared to those with no change to their working status (10.6%). There were no further subgroup differences in suicidal thoughts, or any changes in suicidal thoughts across the subgroups from Wave 1 to Wave 2.
3.2 Depressive symptoms
This study's findings on moderate to severe depressive symptoms are based on participants' responses to questions on the mental health measure called the Patient Health Questionnaire (PHQ-9; Kroenke et al., 2001), which assesses frequency of depressive symptoms over the previous two weeks.[17]
Significant changes between Waves 1 and 2
Looking at the SCOVID Mental Health Tracker Study sample as a whole, rates of moderate to severe depressive symptoms (indicating a need for treatment) did not change significantly from Wave 1 (23.6%) to Wave 2 (24.1%).
A number of subgroups saw changes to rates of moderate to severe depressive symptoms from Wave 1 to Wave 2, including:
- Men's rate of depressive symptoms increased from Wave 1 to Wave 2
- Women's rate of depressive symptoms decreased from Wave 1 to Wave 2
A closer inspection of the Wave 2 findings indicate that some differences by sex from Wave 1 to Wave 2 were evident, as illustrated in Table 3.1. In Wave 1, women reported higher rates of moderate to severe depressive symptoms (27.0%) than men (20.0%) (Table 3.1). In contrast to Wave 1, no significant difference between men (23.7%) and women (24.5%) was found at Wave 2 in terms of proportion of subgroup reporting moderate to severe depressive symptoms. The distribution of reported depressive symptoms between sexes in both waves seems to be accounted for by an increase in rates of moderate to severe depressive symptoms over time for men, from 20.0% at Wave 1 to 23.7% at Wave 2, and a decrease in the rates of moderate to severe depressive symptoms for women from Wave 1 (27.0%) to Wave 2 (24.5%).
No other significant changes between the waves were reported for any other subgroups.
| Wave 1 | Wave 2 | |||||
|---|---|---|---|---|---|---|
| Men % | Women % | All adults % | Men % | Women % | All adults % | |
| 18- 29 years | 34.1 | 47.0 | 40.5 | 47.5 | 37.4 | 42.5 |
| 30- 59 years | 19.0 | 29.0 | 24.3 | 21.2 | 25.6 | 23.5 |
| 60+ years | 10.8 | 10.1 | 10.5 | 12.2 | 11.4 | 11.8 |
| Total % | 20.0 | 27.0 | 23.6 | 23.7 | 24.5 | 24.1 |
Wave 2 Findings
Wave 2 findings suggest that just under a quarter (24.1%) of the overall sample met the cut-off for moderate to severe depressive symptoms. Wave 2 findings suggest that some subgroups had higher rates of moderate to severe depressive symptoms than their subgroup counterpart. These included:
- young adults (18-29 years),
- people with a pre-existing mental health or physical health condition,
- and respondents from a lower SEG.
Consistent with Wave 1 findings, young adults (18-29 years) had higher rates of depressive symptoms (42.5%) compared to 30-59 year olds (23.5%) and 60+ year olds (11.8%).
Respondents' health and socio-economic background also had a bearing on the likelihood of reported rates of moderate to severe depression at Wave 2, as illustrated in Figure 3.1. Specifically, respondents with a pre-existing mental health condition were more likely to report higher rates of depressive symptoms (60.3%) than those with no pre-existing mental health condition (18.9%). Additionally, those who had a pre-existing physical health condition were more likely to report higher depressive symptoms (37.4%) than those who had no pre-existing health condition (20.7%). Further, people who were from a lower SEG reported higher rates of moderate to severe depressive symptoms (29.4%) than those from a higher SEG (20.9%). These findings are consistent with Wave 1.
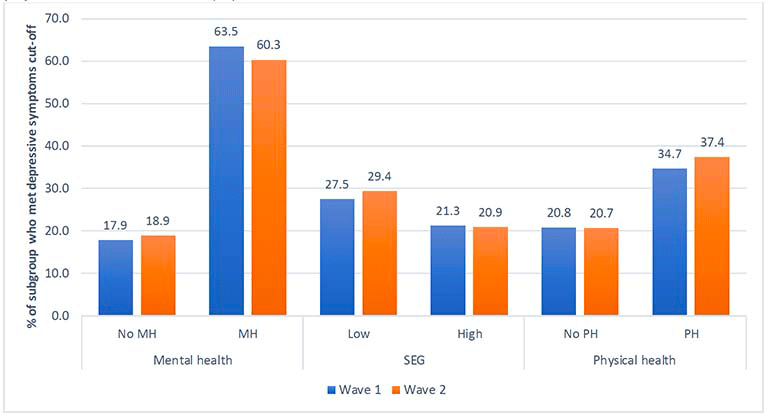
Image description
This figure shows rates of moderate to severe depressive symptoms at Wave 1 and Wave 2 by pre-existing mental health (MH) condition, socio-economic group (SEG), and pre-existing physical health condition (%)
The figure shows that for respondents without a pre-existing mental health condition 17.9% reported moderate to severe depressive symptoms at Wave 1 compared to 18.9% at Wave 2. For respondents with a pre-existing mental health condition, 63.5% reported moderate to severe depressive symptoms at Wave 1 compared to 60.3% at Wave 2.
The figure shows that for respondents from a low socio-economic background 27.5% reported moderate to severe depressive symptoms at Wave 1 compared to 29.4% at Wave 2. For respondents from a high socioeconomic background, 21.3% reported moderate to severe depressive symptoms at Wave 1 compared to 20.9% at Wave 2.
The figure shows that for respondents without a pre-existing physical health condition 20.8% reported moderate to severe depressive symptoms at Wave 1 compared to 20.7% at Wave 2. For respondents with a pre-existing physical health, 34.7% reported moderate to severe depressive symptoms at Wave 1 compared to 37.4% at Wave 2.
Consistent with findings from the Wave 1 report, there was evidence that respondents' circumstances may influence how likely they were to experience depressive symptoms at Wave 2. Specifically, respondents who had unpaid caring responsibilities were more likely to report moderate to severe depressive symptoms (26.9%) compared to those who did not have caring responsibilities (17.7%). Further, respondents who reported a change to their working status (i.e., furloughed, lost job) were more likely to report moderate to severe depressive symptoms (27.1%) compared to those with no change to their work status (21.3%). Unlike at Wave 1, no significant differences were found in Wave 2 for those with dependents at home, key workers, and those who lived alone compared to their subgroup counterparts.
3.3 Anxiety Symptoms
Anxiety symptoms were assessed using the mental health measure called the Generalised Anxiety Disorder (GAD-7; Spitzer et al., 2006) scale, which asks about frequency of anxiety symptoms in the last 2 weeks. For the purposes of this report, the clinical cut-off for moderate to severe anxiety was reported, indicating anxiety symptoms that may require further treatment.
Changes between Waves 1 and 2
Looking at the sample as a whole, there were no statistically significant changes in rates of moderate to severe anxiety symptoms from Wave 1 (16.3%) to Wave 2 (16.9%).
Between Waves 1 and 2 there was an increase in the proportion of the following subgroups reporting moderate to severe anxiety symptoms:
- The rate of young adults (18-29 years) reporting anxiety symptoms increased from Wave 1 to Wave 2
- A higher proportion of young men reported anxiety symptoms at Wave 2 than Wave 1, though this finding should be treated with caution due to loss to follow-up and the small sample size at Wave 2,
- A lower proportion of respondents with a pre-existing mental health condition reported anxiety symptoms at Wave 2 than Wave 1
There were changes between waves in rates of reported moderate to severe anxiety symptoms by age and gender, illustrated in Table 3.2. The rate of moderate to severe anxiety symptoms increased significantly among young adults (18-29 years) from 26% in Wave 1 to 32.4% in Wave 2, but did not for 30-59 year olds or 60+ year olds. In addition, a higher rate of young men reported moderate to severe anxiety symptoms, from 22.8% in Wave 1 to 34.1% in Wave 2. It should however be noted that the young men subgroup experienced a notable dip in response rate in Wave 2 and as such, this finding should be interpreted with caution due to the small sample size.
Whereas at Wave 1 women had higher rates of anxiety symptoms than men, at Wave 2 there were no statistically significant differences between men and women reporting moderate to severe anxiety symptoms (Table 3.2). Despite this, there were no significant changes in moderate to severe anxiety rates from Wave 1 to Wave 2 for men or women.
| Wave 1 | Wave 2 | |||||
|---|---|---|---|---|---|---|
| Men % | Women % | All adults % | Men % | Women % | All adults % | |
| 18- 29 years | 22.8 | 29.3 | 26.0 | 34.1 | 30.7 | 32.4 |
| 30- 59 years | 12.1 | 22.6 | 17.6 | 11.6 | 20.0 | 16.0 |
| 60+ years | 10.1 | 5.1 | 7.5 | 8.4 | 6.1 | 7.2 |
| Total % | 13.9 | 18.6 | 16.3 | 15.8 | 18.0 | 16.9 |
There were no further significant increases or decreases in rates of moderate to severe anxiety symptoms from Wave 1 to Wave 2 for any of the subgroups.
Wave 2 Findings
Wave 2 findings indicate that 16.9% of respondents met the cut-off for moderate to severe anxiety symptoms. Several groups reported higher rates of moderate to severe anxiety than their subgroup counterparts.
These included:
- young adults (18-29 years old),
- those with a pre-existing mental health condition,
- respondents from a lower SEG
- people with a pre-existing physical health condition.
Consistent with Wave 1, at Wave 2 young adults (18-29 years) reported the highest rates of moderate to severe anxiety symptoms (32.4%) compared to 30-59 year olds (16.0%) and 60+ year olds (7.2%).
Wave 2 data suggest a number of the same subgroups were at higher risk of moderate to severe anxiety symptoms, consistent with rates seen in Wave 1. For example, respondents' background and health factors appear to influence how likely they were to experience moderate to severe anxiety symptoms, as illustrated in Figure 3.2. For example, people with a pre-existing mental health condition reported higher rates of moderate to severe anxiety symptoms (41.7%) compared to those with no mental health condition (13.4%). Respondents with a physical health condition reported higher rates of moderate to severe anxiety symptoms (22.8%) than those with no pre-existing physical health condition (15.4%). Those from the lower SEG also reported higher rates of moderate to severe anxiety symptoms (22.4%) than respondents from the higher SEG (13.8%).
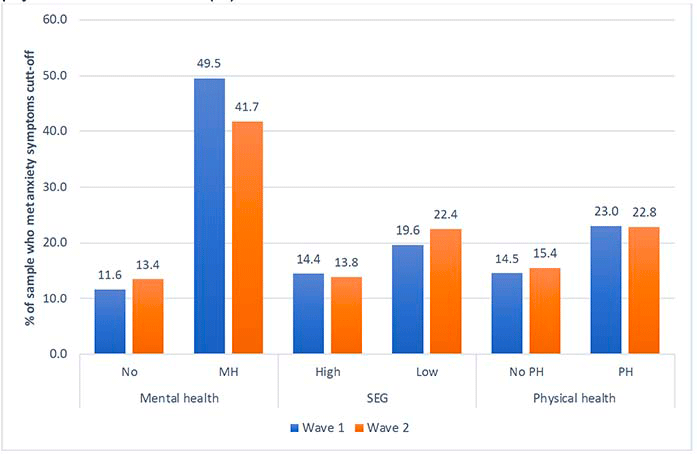
Image description
This figure shows rates of moderate to severe anxiety symptoms at Wave 1 and Wave 2 by pre-existing mental health (MH) condition, socio-economic group (SEG), and pre-existing physical health condition (%).
The figure shows that for respondents without a pre-existing mental health condition 11.6% reported moderate to severe anxiety symptoms at Wave 1 compared to 13.4% at Wave 2. For respondents with a pre-existing mental health condition, 49.5% reported moderate to severe anxiety symptoms at Wave 1 compared to 41.7% at Wave 2.
The figure shows that for respondents from a high socio-economic background 14.4% reported moderate to severe anxiety symptoms at Wave 1 compared to 13.8% at Wave 2. For respondents from a low socio-economic background, 19.6% reported moderate to severe anxiety symptoms at Wave 1 compared to 22.4% at Wave 2.
The figure shows that for respondents without a pre-existing physical health condition 14.5% reported moderate to severe anxiety symptoms at Wave 1 compared to 15.4% at Wave 2. For respondents with a pre-existing physical health condition, 23% reported moderate to severe anxiety symptoms at Wave 1 compared to 22.8% at Wave 2.
Further analysis found that employment factors may influence people's likelihood of experiencing moderate to severe anxiety symptoms at Wave 2. Specifically, people whose working status had changed due to the COVID-19 lockdown (e.g., lost job, furloughed) reported higher rates of moderate to severe anxiety (27.1%) than those with no change to their working status (20.9%). There were no further subgroup differences in moderate to severe anxiety symptoms at Wave 2.
3.4 General Health Questionnaire
The General Health Questionnaire (GHQ-12) is a psychological measure that assesses mental distress and mental ill-health in the previous two weeks, including sleep, self-esteem, stress, despair, depression, and confidence. In this report, as consistent with other mental health research studies (McLean et al., 2018), GHQ-12 scores of four or more are reported because this cut-off is deemed a high GHQ-12 score and indicates the presence of a possible psychiatric disorder.
Changes between Waves 1 and 2
Analysis suggests that the proportion of respondents who met the GHQ-12 cut-off for high mental distress and mental ill-health decreased from Wave 1 (32.6%) to Wave 2 (28.8%), suggesting that poorer mental health and possible psychiatric disorders reduced during the COVID-19 lockdown.
A decrease in rates of high GHQ-12 from Wave 1 to Wave 2 were found for a number of subgroups, specifically:
- A decrease in rates of high GHQ-12 was found for women of all ages, however despite this, they were still higher than for men,
- A decrease in rates of high GHQ-12 was found for respondents with a pre-existing mental health condition.
Differences in rates of high GHQ-12 by sex and age at Wave 2 are presented in Table 3.4. Rates of high GHQ-12 decreased significantly for women from Wave 1 (38.6%) to Wave 2 (31.9%), and this decrease for women was found across all age groups (see Table 3.4). Despite this decrease, women still had higher rates of high GHQ-12 (44.4%) than men (39.1%) at Wave 2. There were no significant changes in high GHQ-12 from Wave 1 to Wave 2 for men across the age groups.
| Wave 1 | Wave 2 | |||||
|---|---|---|---|---|---|---|
| Men % | Women % | All adults % | Men % | Women % | All adults % | |
| 18- 29 years | 38.5 | 52.1 | 45.3 | 39.1 | 44.4 | 41.8 |
| 30- 59 years | 26.3 | 41.2 | 26.3 | 25.6 | 35.1 | 30.6 |
| 60+ years | 17.1 | 25.3 | 21.3 | 14.7 | 18.4 | 16.6 |
| Total % | 26.2 | 38.6 | 32.6 | 25.3 | 31.9 | 28.8 |
Additionally, for those with a pre-existing mental health condition, rates of high GHQ-12 decreased significantly from Wave 1 (62.5%) to Wave 2 (51.3%; see Figure 3.4). No further significant changes from Wave 1 to Wave 2 in high GHQ-12 in the subgroups were found.
Wave 2 findings
In the Wave 2 Scottish COVID-19 Mental Health Tracker Study, over one quarter (28.8%) of the sample met the high GHQ-12 cut-off score. As with the Wave 1 report, the Wave 2 findings suggest that several of the same subgroups reported elevated rates of high GHQ-12 scores at Wave 2 compared to their subgroup counterparts. This included:
- young adults (age 18-29 years),
- women, those with a pre-existing mental health condition,
- and respondents from a lower socio-economic group.
Looking at age and sex, young adults were more likely to report high GHQ-12 scores (41.8%) compared to 30-59 year olds (30.6%) and 60+ year olds (16.6%). Additionally, women reported higher rates of high GHQ-12 scores (44.4%) than men (39.1%) at Wave 2 (despite women reporting an overall decrease in high GHQ-12, Table 3.4).
There were differences in rates of high GHQ-12 scores by health and background factors, as illustrated in figure 3.4. Respondents with a pre-existing mental health condition reported higher rates of GHQ-12 scores (51.3%) than those with no pre-existing mental health condition (25.6%). Those with a pre-existing physical health condition also reported higher rates of high GHQ-12 scores (36.7%) compared to those with no physical health condition (26.8%). Additionally, people from the lower SEG reported higher rates of high GHQ-12 scores (32.3%) compared to those from the higher SEG (26.8%).
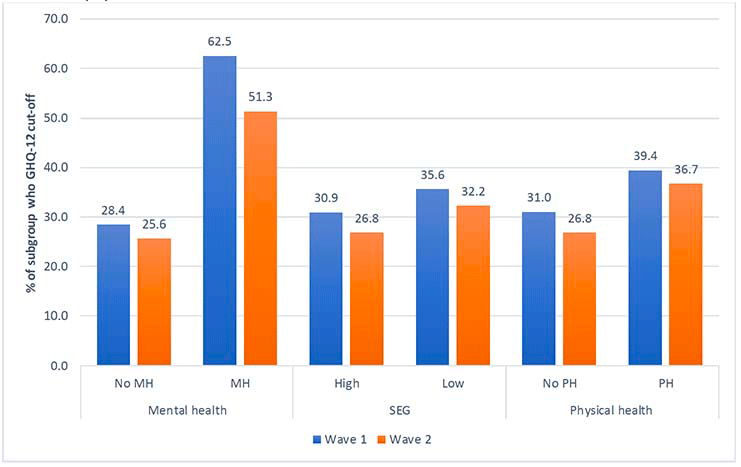
Image description
This figure shows rates of high GHQ-12 scores at Wave 1 and Wave 2 by pre-existing mental health (MH) condition, socio-economic group (SEG), and pre-existing physical health condition (%)
The figure shows that for respondents without a pre-existing mental health condition, 28.4% reported high GHQ-12 scores at Wave 1 compared to 25.6% at Wave 2. For respondents with a pre-existing mental health condition, 62.5% reported high GHQ-12 scores at Wave 1 compared to 51.3% at Wave 2.
The figure shows that for respondents from a high socio-economic, 30.9% reported high GHQ-12 scores at Wave 1 compared to 26.8% at Wave 2. For respondents with a pre-existing mental health condition, 35.6% reported high GHQ-12 scores at Wave 1 compared to 32.2% at Wave 2.
The figure shows that for respondents from a high socio-economic background, 30.9% reported high GHQ-12 scores at Wave 1 compared to 26.8% at Wave 2. For respondents from a low socio-economic background, 35.6% reported high GHQ-12 scores at Wave 1 compared to 32.2% at Wave 2.
The figure shows that for respondents without a pre-existing physical health condition, 31% reported high GHQ-12 scores at Wave 1 compared to 26.8% at Wave 2. For respondents with a pre-existing physical health condition, 39.4% reported h GHQ-12 scores at Wave 1 compared to 36.7% at Wave 2.
Further subgroup differences were found in GHQ-12 scores at Wave 2, depending upon unpaid caring responsibilities and employment status. Specifically, respondents with unpaid caring responsibilities were more likely to report high GHQ-12 scores (38.6%) than those with no caring responsibilities (27.1%). People whose working status had changed were more likely to report high GHQ-12 scores at Wave 2 (33.4%) compared to those who working status had not changed (24.6%). Additionally, people who lived alone also were less likely to report high GHQ-12 scores (19.4%) than those who did not live alone (31.4%), suggesting that living alone was a protective factor for high GHQ-12 scores.
3.5 Mental Wellbeing
Mental wellbeing is an important indicator of mental health. The SCOVID Mental Health Tracker Study measured a respondent's mental wellbeing using the Short Warwick-Edinburgh Mental Well-being Scale (SWEMWBS)[20]. This scale measures the frequency of thoughts and feelings of mental wellbeing over the past two weeks; includes items such as feelings of optimism, feelings of being useful, and feeling that one is thinking clearly.
For the SWEMWBS, a score is created for each individual by adding together their responses to each question. As suggested by the scale authors, scores were adjusted using Rasch transformation. The scores range from 7 (indicating very low wellbeing) to 35 (indicating very high wellbeing), therefore a higher score suggests better mental wellbeing. The scale was not designed to identify individuals with exceptionally high or low levels of mental wellbeing so cut off points have not been developed. Therefore, throughout this section average mean scores are reported for each of the subgroups to compare levels of mental wellbeing between groups.
Changes between Waves 1 and 2
Overall, respondents' mental wellbeing as measured by the SWEMWBS significantly increased from Wave 1 (Mean score=21.52) to Wave 2 (Mean score=21.81).
Additionally, a number of subgroups also reported a change in their mental wellbeing from Wave 1 to Wave 2. Specifically, mental wellbeing increased from Wave 1 to Wave 2 for the following groups:
- The lower SEG,
- Those with a pre-existing mental health condition,
- Respondents who lived alone reported an increase in their mental wellbeing.
There were no significant changes on levels of mental wellbeing from Wave 1 to Wave 2 for sex or age groups (Table 3.5). There were some subgroup changes in mental wellbeing by health and background factors. Those with a pre-existing mental health condition reported an increase in their mental wellbeing from Wave 1 (16.20) to Wave 2 (17.29), although they still reported significantly lower mental wellbeing than those with no mental health condition at Wave 2 (Figure 3.5). Similarly, those in lower SEG reported an increase in mental wellbeing from Wave 1 (20.49) to Wave 2 (21.00), although the lower SEG still reported lower mental wellbeing than the higher SEG subgroup. Those who lived alone reported higher mental wellbeing at Wave 2 (22.05) compared to Wave 1 (21.29), whereas those who didn't live alone reported no change in mental wellbeing.
| Wave 1 | Wave 2 | |||||
|---|---|---|---|---|---|---|
| Men % | Women % | All adults % | Men % | Women % | All adults % | |
| 18- 29 years | 19.59 | 18.87 | 19.24 | 19.99 | 19.54 | 19.77 |
| 30- 59 years | 21.46 | 20.43 | 20.93 | 21.59 | 20.65 | 21.11 |
| 60+ years | 23.57 | 23.77 | 23.66 | 23.88 | 23.96 | 23.91 |
| Total % | 21.85 | 21.18 | 21.52 | 22.11 | 21.49 | 21.81 |
Wave 2 findings
As with the Wave 1 report, the Wave 2 report highlighted a number of the same subgroups that reported higher levels of mental wellbeing during the COVID-19 lockdown than their subgroup counterparts. These groups included:
- older adults,
- people with no pre-existing mental health conditions
- those from the higher SEG
In looking more closely at the data, some differences on mental wellbeing at Wave 2 by age and sex emerge (see Table 3.5). At Wave 1 there were no significant sex differences in mental wellbeing found between men and women, whereas at Wave 2, women reported lower mental wellbeing scores (21.49) than men (22.11). Similar to Wave 1, the oldest age group (60+ year olds) reported the highest mental wellbeing scores (23.91), compared to 30-59 year olds (21.11) and 18-29 year olds (19.77), who reported the lowest.
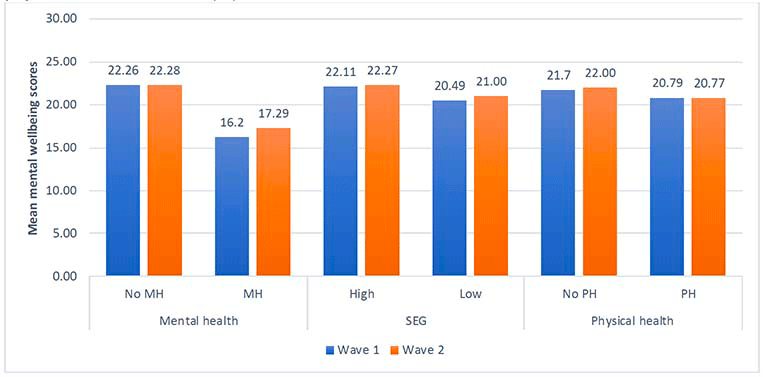
Image description
This figure shows mean mental wellbeing scores at Wave 1 and Wave 2 by pre-existing mental health (MH) condition, socio-economic group (SEG), and pre-existing physical health condition (%).
The figure shows that for respondents without a pre-existing mental health condition, the average score was 22.26 at Wave 1 compared to 22.28 at Wave 2. For respondents with a pre-existing mental health condition, the average score was 16.2 at Wave 1 compared to 17.29 at Wave 2.
The figure shows that for respondents from a high socio-economic background, the average score was 22.11 at Wave 1 compared to 22.27 at Wave 2. For respondents with a pre-existing mental health condition, the average score was 20.49 at Wave 1 compared to 21 at Wave 2.
The figure shows that for respondents without a pre-existing physical health condition, the average score was 21.7 at Wave 1 compared to 22 at Wave 2. For respondents with a pre-existing physical health condition, the average score was 20.79 at Wave 1 compared to 20.77 at Wave 2.
Looking beyond age and gender, there were some subgroup differences found by health and background factors at Wave 2, as illustrated in Figure 3.5. Respondents who did not have a pre-existing mental health condition reported higher mental wellbeing scores (22.28) than those with a pre-existing mental health condition (17.29). Respondents from a higher SEG continued to report higher mental wellbeing scores (22.27) than those from the lower SEG (21.00), People with no pre-existing physical health condition reported higher mental wellbeing (22.00) compared to respondents with a physical health condition (20.77).
Employment status may also have an impact upon mental wellbeing at Wave 2. Those whose working status had changed during the COVID-19 lockdown reported lower mental wellbeing scores (21.27) compared to those whose work status had not changed (22.01).
3.6 Other mental health outcomes
Wave 2 of the SCOVID Mental Health Tracker Study assessed a range of other indicators and correlates of mental health and wellbeing. These included feelings of loneliness, defeat, entrapment, resilience, social support, life satisfaction, and distress. This section provides a brief overview of these measures. The Wave 2 findings suggest that similar subgroups from the Wave 1 report may be more at risk for poor mental health and wellbeing indicators, including:
- Women
- Young adults (18-29 years)
- People from the lower SEG
- Respondents with a pre-existing mental or physical health condition
3.6.1 Loneliness
Loneliness has been associated with poorer physical and mental health, and was a particular concern during the COVID-19 lockdown as people became physically isolated from friends and family. This study measures loneliness using the UCLA Loneliness Scale (Hughes et al., 2014), which assesses 3 aspects of loneliness; namely lacking companionship, feeling left out, and feeling isolated from others.
A total loneliness score was created by adding the responses to each question together, creating a score between 3 (indicating no loneliness) and 9 (indicating high levels of loneliness). As there is no cut-off score demarcating high and low loneliness, mean scores were reported when comparing the different subgroups in terms of perceived levels of loneliness prior to the COVID-19 pandemic and reported levels of loneliness in the week preceding respondents' participation in the study.
Changes between Waves 1 and 2
For the whole sample, feelings of loneliness decreased from Wave 1 (Mean score = 5.06) to Wave 2 (Mean score = 4.67).
Some subgroups also reported a decrease in loneliness from Wave 1 to Wave 2, including:
- People with no pre-existing physical health condition,
- Respondents living in urban areas,
- People whose working status had changed.
Those who did not have a pre-existing physical health condition reported that their loneliness decreased from Wave 1 (5.03) to Wave 2 (4.53). Additionally, people whose working status had changed during the COVID-19 pandemic reported that their loneliness had reduced from Wave 1 (5.29) to Wave 2 (4.80), although this was still significantly higher at Wave 2 than those whose working status had not changed (4.61). Finally, respondents living in urban areas reported that their loneliness decreased from Wave 1 (5.08) to Wave 2 (4.66), and those in rural areas reported no change in loneliness. There were no significant changes from Wave 1 to Wave 2 on loneliness by sex or age.
Wave 2 findings
As at Wave 1, several subgroups were found to report higher levels of loneliness at Wave 2, and these included:
- young adults (18-29 years),
- women,
- people with a pre-existing mental health condition,
- people from a lower SEG.
There were differences in loneliness scores by age and gender at Wave 2. Women reported higher loneliness (4.83) than men (4.56). Young adults (18-29 years) reported the higher loneliness (5.10) than 30-59 year olds (4.84) and 60+ year olds (4.19).
There were some differences in loneliness at Wave 2 by health and socio-economic background factors. People with a pre-existing mental health condition reported higher loneliness at Wave 2 (6.00) than those with no pre-existing mental health condition (4.51). People from a lower SEG also reported higher loneliness (4.93) than those from the higher SEG (4.56). People with a pre-existing physical health condition reported feeling more lonely (5.17) than those who did not have a physical health condition (4.58).
Further subgroup differences on loneliness at Wave 2 were found for living and employment status groups. Those who lived alone reported higher loneliness (5.14) than those who did not live alone (4.57). Those whose working status changed reported higher loneliness at Wave 2 (4.80) than those whose working status had not changed (4.61),
3.6.2 Defeat and Entrapment
Feelings of defeat and entrapment are important indicators of mental health, and have been associated with depression, anxiety, and suicidal thoughts (Taylor et al., 2011). Defeat is a feeling of powerlessness in life and entrapment is a feeling of being trapped by circumstances or your own thoughts. Defeat was assessed using the short form of the Defeat Scale (Gilbert & Allan, 1998; Griffiths et al., 2015) and entrapment using the short form of the Entrapment Scale (Gilbert & Allan, 1998; De Beurs et al., 2020). All respondents are given a score for each measure by adding together each question response, with 0 indicating no feelings of defeat or entrapment and 16 indicating feeling a very high level of defeat and entrapment.
There are no cut-off scores for defeat and entrapment measures to demarcate high or low levels of defeat and entrapment, therefore an average mean score is used to compare differences between the subgroups.
Changes between Waves 1 and 2
For the whole sample, average defeat and entrapment scores significantly decreased from Wave 1 (3.82) to Wave 2 (3.64), and from Wave 1 (3.49) to Wave 2 (3.33), respectively. Several groups reported that their average defeat and entrapment scores had decreased or increased from Wave 1 to Wave 2:
- Defeat and entrapment scores reduced for those with a pre-existing mental health condition
- Entrapment scores decreased for those aged 30-59 years
- Entrapment scores decreased for women
- Entrapment scores increased for those with a physical health condition, and decreased for those with no physical health condition
Looking more closely at subgroup changes in defeat and entrapment, women's entrapment scores significantly decreased from Wave 1 (3.88) to Wave 2 (3.48). For those aged 30-59 years, entrapment scores decreased from Wave 1 (4.06) to Wave 2 (3.77).
People with a pre-existing mental health condition reported that their feelings of defeat had decreased from Wave 1 (8.57) to Wave 2 (7.99), and their entrapment scores also decreased from Wave 1 (8.43) to Wave 2 (7.67). Despite this change, they still reported higher defeat and entrapment scores at Wave 2 than those with no pre-existing mental health condition.
Additionally, respondents with a pre-existing physical health condition reported that their levels of entrapment, but not defeat, significantly increased from Wave 1 (4.57) to Wave 2 (4.79), while entrapment scores decreased for those with no physical health condition from Wave 1 (3.32) to Wave 2 (3.07).
Wave 2 findings
There were some differences in relation to age and sex on feelings of defeat and entrapment at Wave 2. Women reported higher levels of defeat (3.99) than men (3.43), but not significantly higher levels of entrapment. At Wave 2, young adults reported higher defeat (4.91) and entrapment (4.64) than 30-59 year olds (defeat = 4.11, entrapment = 3.77) and 60+ year olds (defeat = 2.27, entrapment = 1.98).
Further differences were found on defeat and entrapment scores based upon respondents' health status. Despite reporting a reduction in levels of defeat and entrapment from Wave 1 to Wave 2, those with mental health conditions still reported much higher defeat and entrapment compared to those with no mental health condition at Wave 2 (defeat = 3.11, entrapment = 2.81). Respondents from the lower SEG reported higher defeat (4.14) and entrapment (3.93) at Wave 2 compared to those from the higher SEG (defeat = 3.48), entrapment = 3.11).
3.6.4 Resilience
Resilience can be protective for mental health problems, including depression, anxiety, and suicidal thoughts. Resilience was assessed using 4 questions from the Brief Resilience Scale (BRS; Smith et al., 2008). Respondents received a total score by summing the responses to each question, and this ranges from 4, indicating very low resilience to 20, indicating very high resilience. As there are no cut-off scores to demarcate high and low resilience, mean scores were used to compare the different subgroups on resilience average.
Changes between Waves 1 and 2
Across the whole sample, levels of resilience increased significantly from Wave 1 (10.52) to Wave 2 (10.72). Looking at subgroup changes, people with a mental health condition reported that their resilience increased from Wave 1 (5.81) to Wave 2 (6.77), although this was still lower than those with no mental health condition (11.17).
Wave 2 findings
Looking closer at the Wave 2 findings, some subgroup differences were found for levels of resilience between age and sex groups. For example, men reported higher resilience (10.83) compared to women (10.43). Older adults (60+ years) had higher resilience at Wave 2 (12.37) than 30-59 year olds (10.05) and 18-29 year olds (9.43).
Beyond age and sex, other health factors influenced peoples experience of resilience at Wave 2. For example, people with a pre-existing mental health condition reported lower levels of resilience (6.77) than those with no mental health condition (11.17). Additionally, respondents with a physical health condition reported lower levels of resilience (9.93) than those with no physical health condition (10.80).
3.6.6 Social support
Questions about sources of emotional and physical support and feelings of connection to those around you were also included in the Wave 2 questionnaire. Social support was measured using four questions from the ENRICHD Social Support Instrument (ESSI; Mitchel et al., 2003) that assess how often an individual feels they currently have emotional and physical support. Responses are summed into a total score, with a potential range from 4, indicating low social support to 20, indicating very high social support. Therefore, higher scores represent higher levels of social support.
Changes between Waves 1 and 2
For the whole sample, social support average scores did not change significantly from Wave 1 (14.54) to Wave 2 (14.51). However, there were some subgroup changes in levels of social support from Wave 1 to Wave 2.
Although men and women did not report significant differences in social support scores at Wave 2, analysis suggests that women's levels of social support decreased from Wave 1 (14.66) to Wave 2 (14.40), and men's increased from Wave 1 (14.33) to Wave 2 (14.49).
Additionally, young adults (18-29 years old) reported that their social support had increased from Wave 1 (14.25) to Wave 2 (14.52), while those aged 30-59 years found that their social support had decreased from Wave 1 (14.17) to Wave 2 (13.85), and therefore reported the lowest social support at Wave 2 for all age groups. The older adults (60+ years) did not report any significant changes in social support from Wave 1 (15.18) to Wave 2 (15.30). Respondents with a pre-existing mental health condition reported that their social support decreased from Wave 1 (12.79) to Wave 2 (12.31), and remained higher at Wave 2 than those who had no mental health conditions (14.74).
3.6.7 Distress
Distress is a feeling of acute anxiety and pain, and it is a correlate of current and future mental wellbeing. To measure levels of distress, we asked respondents to indicate on a 10-point scale how distressed they had felt in the past week, on a range of 0, indicating feeling no distress, to 10, indicating feeling extreme distress. As there is no cut-off for high and low distress, average mean scores were used to compared levels of distress between subgroups.
Changes between Waves 1 and 2
For the whole sample, the average level of distress reduced from Wave 1 (2.61) to Wave 2 (2.41).
Looking closer at changes in distress by age and sex, a number of subgroup changes emerge. For example, women's levels of distress decreased from Wave 1 (3.07) to Wave 2 (2.74), whereas men's remained similar from Wave 1 (2.29) to Wave 2 (2.17). Young adults' (18-29 years) distress reduced from Wave 1 (3.76) to Wave 2 (3.38), as did 30-59 year olds (Wave 1 = 3.00, Wave 2 = 2.67). However, the older adults (60+ years) did not report a significant change from Wave 1 (1.45) to Wave 2 (1.50), and remained the lowest level of distress at Wave 2 across the age groups.
3.6.8. Life satisfaction
At Wave 1 and Wave 2 of the Scottish COVID-19 Mental Health Tracker Study, respondents were asked about their current life satisfaction with the question 'All things considered, how satisfied are you with your life as a whole nowadays?'. They were asked to rate their life satisfaction on a scale from 0 (indicating extremely dissatisfied) to 10 (indicating extremely satisfied).
Changes between Waves 1 and 2
The overall sample did not report changes in life satisfaction from Wave 1 (6.39) to Wave 2 (6.40).
Looking at changes in life satisfaction by subgroups, older adults (60+ years) reported a decrease in life satisfaction from Wave 1 (7.19) to Wave 2 (7.04), though 60+ year olds still reported higher life satisfaction than both 18-29 year olds (6.04) and 30-59 year olds (6.07).
Respondents with a pre-existing mental health condition reported that their life satisfaction had increased from Wave 1 (4.13) to Wave 2 (4.37), although this remained significantly lower than those with no mental health condition (6.64).
Contact
Email: socialresearch@gov.scot