Scottish Breast Screening Programme: major review
Major review of the Scottish Breast Screening Programme.
The Current Service
Background
Breast screening policy in NHS Scotland (and across the UK) is that all women aged 50-70 years +364 days are invited for breast screening once every 3 years. Women are invited to participate in breast screening based on calling the eligible women within the GP practice with which they are registered. Women over the age of 71 can self-refer for breast screening once every 3 years.
Configuration and operational delivery
Breast screening in Scotland is delivered via 6 breast screening centres across the country, complimented by the provision of a fleet of 20 mobile breast screening units. Operationally the six breast screening centres are hosted to deliver screening services across their catchments by NHS Boards (six Boards). The mobile fleet is scheduled and staffed by the centres, with medical physics, facilities and procurement support provided centrally via National Services Scotland (NSS), Procurement, Commissioning and Facilities (PCF).
The breast screening service offers 2-view digital mammographic screening on a 3-yearly basis to approximately 750,000 women across Scotland in each 3-year screening round. The service reads and interprets the mammograms directly, and sends out the results. All breast screening mammograms are double-read by 2 readers (radiologists, or advanced practice radiographers), with independent third party arbitration for cases where there is disagreement.
Where an abnormality is identified on the mammogram the service invites the woman for comprehensive clinical assessment. Onward referral to local symptomatic breast services for treatment is made when necessary.
Digital mammography has been in place across the whole of Scotland since 2015.
National service co-ordination and service governance
The service is nationally coordinated via NSS National Services Division (NSD) which supports the service level agreement, annual performance review, and annual reporting. NSD co-ordinates the planning and programme development work for the service at national level, involving NHS Boards and other delivery partners.
Governance of the service nationally is via the Breast Screening Programme Board. The governance structure is outlined in figure 1 below. A Monitoring and Evaluation Group is in place to examine the key data from the service and to support service quality assurance and development. A National Users Group delivers and manages the development plan for the IT system which underpins the service – the Scottish Breast Screening System (SBSS).
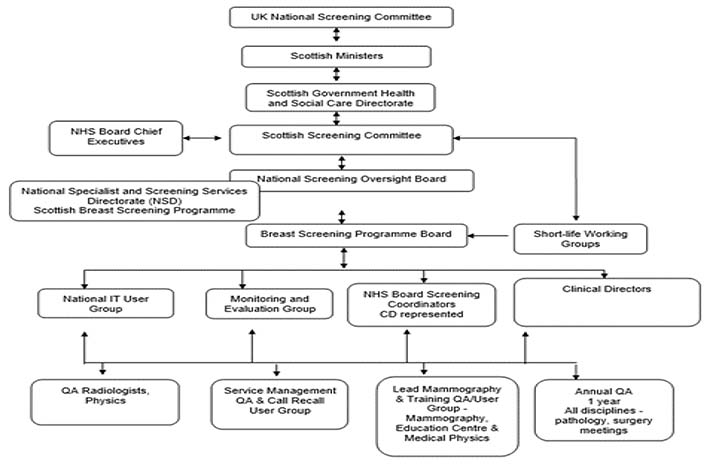
High level overview of current activity, costs, and performance
Published data for breast screening for the 3-year period from 2016/17 to 2018/19 shows that a total of 546,379 women attended a routine breast screening appointment, from 756,341 invited, equating to an attendance rate of 72.2% across Scotland[1]. This is just above the minimum standard of 70%. The invasive cancer detection rate was 6.8 per 1,000 women screened for women aged 50-52 and new to screening, and 7.0 per 1,000 women screened for women 53-70.
In 2018/19, the number of screen-detected breast cancers in women of all ages was 1,738. Of these, 87.7% (1,524) were invasive breast cancers. Just under half (49.2%) of these were less than 15 mm in size. Such small tumours are unlikely to be detected by physical examination, highlighting the importance of screening in the early detection of breast cancer.
The SBSP costs for 2019/20 are just over £ 15.5 million with pays accounting for around 74% of overall costs. These costs equate to a cost of around £76 per woman screened.
Previous reviews of Breast Screening
In 2011 a review of Breast Screening was undertaken by the SBSP chaired by Mr Calum Campbell (CEO NHS Borders at the time). This considered the review of service delivery and future model for the service and involved describing key pressures and costs:
- Assessing performance against the 6 domains of quality
- Reviewing geographical distribution
- Considering commissioning and planning models for the service
- Setting out organisational, financial and staffing implications of implementing digital mammography and
- Developing a sustainable staffing model
Not all of the recommendations could be taken forward at the time, either because of pressures in breast services or because they were not approved by Scottish Government.
Contact
Email: screening@gov.scot