Scottish Breast Screening Programme: major review
Major review of the Scottish Breast Screening Programme.
Improving Data and Intelligence
Data and IT constraints
Review data
Obtaining and using data was a significant constraint for the review. This was unexpected, led to delay in the review work programme, and ultimately forced the review to change its planned approach, priorities and workstream objectives.
The review team obtained analytical support from Public Health Scotland, and discussed analytical requirements. In the context of understanding that only aggregate data from the Breast Screening Programme was available to Public Health Scotland, the review sought to obtain patient level data from SBSS, over a full screening round. This was requested to create a dataset to support review and modelling of call-recall options; specific cohorts within the screening population; variations in access and uptake; demand and capacity via mobile and static screening clinic utilisation and delivery locations, examining catchments and screening centre configuration / boundaries; geospatial modelling of developed options for screening location and delivery; as well as to support other sub-projects within review workstreams.
Initial exploration of the DaS 'Connect' rather than 'Collect' approach was considered, to connect to the full data-set and avoid the need to copy the data. However, this approach proved not to be possible at the time to support the review.
Current SBSS BOXI reports available were also explored to determine whether these could be utilised (however these were deemed to be too limited).
A number of factors contributed to the difficulty in obtaining and using data at this level. These included:
- No clear data definitions and limited awareness of the level of data and data available from SBSS – knowledge of this rested with the external supplier
- A complex and multi-step process to scope, specify, and make the request for data – via the development request process
- A lack of patient level data for the Breast Screening Programme in Public Health Scotland
- A reliance on working through NSS Digital and Security to explore what data might be available via the 3rd party system, and as above, limitations in data definitions
- Information governance requirements of the 3rd party supplier, appropriately intended to protect and ensure that approval is in place to support release of data previously not requested, however with a complex and uncertain process for approval.
- Initial uncertainty over data controller status within NSS (with complexity added by the migration of analytical resources to Public Health Scotland). The DaS Data Release process was followed, with the required Caldicott Guardian approval obtained.
Whilst the initial specification for analysis was completed and discussed in December 2019, due to the process to specify, request and approve the data, and time for the 3rd party IT system supplier to undertake the development work to deliver the data, the data was not downloaded into NSS until May 2020. Data was supplied in 'XML' format and because of this, and the size of the dataset, expertise in Digital and Security (DAS) was required to format the data and provide Public Health and Intelligence (now part of PHS) with the file format and storage space they required. Digital and Security (DAS) resources at this time were appropriately prioritised to supporting the Covid-19 response, unfortunately entailing a significant delay in handling the data obtained for the review. Following processing, and PHS data quality assurance, a limited review dataset became available for analysis in December 2020.
Development resource
The review has heard from many SBSS system users a frustration over the lack of data to support operational, performance and strategic planning at Breast Screening Centre level. The availability and format of data seems restricted, with consequent limitations to collaborating across centres on performance and planning. The National User Group is seeking to improve this via the further development of BOXI reporting, however it remains an area for improvement.
The SBSS National User Group (NUG) has also raised concerns regarding the process for the prioritisation of the SBSS development resource, with competing demands for IT development coming from Covid recovery work, planned developments to SBSS to support the operational functioning of the service, and strategic exercises such as requests made via this review. Funding allocated for SBSS development in the 'Committed Development Resource' should be examined with a view to increasing resource to support user development requests prioritised, and SBSS data reporting functionality.
This situation will improve with the creation of the new National Screening Digital Service Management Board (NSDSM Board) which will specifically consider change requests for screening IT systems, meaning that they will no longer have to be prioritised alongside non-screening IT developments. This group will report into NSOB as well as into wider SG and NHS Digital governance structures
Additionally, opportunity exists to make significant improvements in data access and reporting, as outlined below.
Screening Intelligence Platform
The Future Data Depository of All Analytical Purposes in Relation to the National Screening Programmes
The objective of the Screening Intelligence Platform (SIP) is to provide an efficient, single point of access to linkable data from all of the National Screening Programmes regardless of where the data are held. It will do this by creating views of the source data which can be more easily used for all types of analysis and to automate update of dashboards and routine reports reliant on these data. The platform will allow NSS and Public Health Scotland (PHS) and other public sector bodies to make better, more efficient use of data, to make better insights, and ultimately to make better informed data driven decisions.
The Screening Intelligence Platform (SIP) builds on the successful implementation of Phase 1 of the Cancer Intelligence Platform (CIP) in late 2019.
What is the Cancer Intelligence Platform (CIP), and why is it important for the Screening Programmes?
The objective of the CIP is to provide an efficient, single point of access to linkable cancer data regardless of where the data are held by creating views of the source data, covering the whole cancer pathway. The development process will ensure that these data are CHI linkable to describe and understand the whole cancer patient pathway from:
- Prevention
- Early detection including screening
- Diagnosis
- Treatment
- Cure
- Recurrence
- Palliation
- End of life
- Death
Cancer screening data will also sit within the CIP. It will be possible to follow the whole screening population through their entire journey, into secondary care, treatment and outcomes.
Figure 1 illustrates the datasets which will be available within CIP, including the SCR and the three National Cancer Screening Programmes.
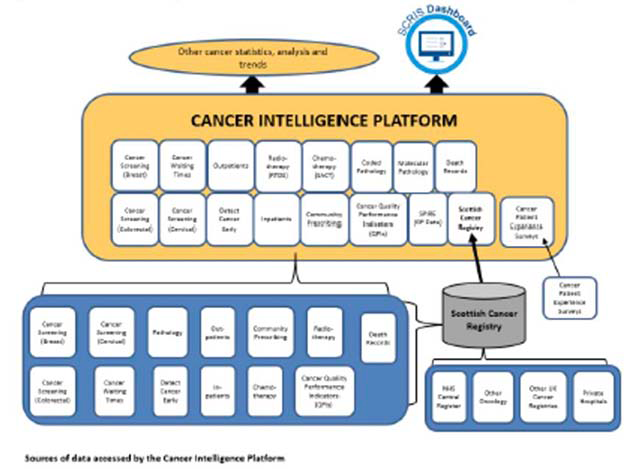
Completion of the CIP is now an action within the Recovery and redesign: An action plan for cancer services published by the Scottish Government on 9th December 2020[26]. This key policy document reinforced the concept of bringing all cancer datasets together, initially for PHS cancer analysts, but in future, for all cancer analysts across NHS Scotland.
What is the Screening Intelligence Platform, and How it will Relate to the CIP?
Data from the breast screening programme (as well as the other 2 national cancer Screening programmes) will be available within both the CIP and the SIP. All of the datasets will draw the data needed directly from the screening IT systems into accessible, linkable views within the platform(s). In addition to cancer screening data, analytical data from the AAA and DES Programmes will be drawn in (into the SIP only), and data from the New-born and Pregnancy Screening Programmes will be added to the SIP as data become more widely accessible.
Data fields from both the live service systems and the reporting tools will be drawn into the SIP to ensure all the analytical reporting is available directly from the SIP. Views of additional datasets, such as acute activity in SMR01, NRS deaths, mapping of SIMD to different geographies for example, will also be drawn into the SIP as views to allow easier linkage and mappings.
Gaining access to all of these CHI linkable datasets is in process, and will be covered by overlapping Information Governance documentation (see below). Initially, access to the SIP will be limited to analysts with PHS and NSS NSD centrally, but once established and fully tested, the intention will be to widen access to other public sector bodies.
What are the benefits of having the SIP?
It will be possible to create and follow the whole screening history of the population through their screening journey, whether the people remain in primary care, or tracking their journey into secondary care, treatment and outcomes. Linkable data may be used:
- to make the reporting of recovery metrics easier and more standardised across the Programmes, with the ultimate aim of having an automated dashboard which can report regularly straight from the SIP;
- to make analyses of inequalities much easier, both within and across Screening Programmes (e.g. identifying small areas where uptake is poor to allow NHS Boards/HSCP/LA/Communities to target interventions more appropriately):
- making examination of full screening histories possible to explore changes in behaviour over time and/or easier assessment of impact of particular intervention;
- in helping to identify and understand patterns of behaviour
- by allowing more efficient and easier access to screening co-ordinators, analysts etc. to understand core health services analyses;
- and allow smoother and more efficient provision of data to researchers (with appropriate ethics and IG).
Information Governance
To fulfil the provision of both the CIP and the SIP, Public Health Scotland (PHS) will be viewed as joint data controllers with NSS and/or the territorial NHS Boards as appropriate. All of the datasets will be shared within the health service under the NHS Data Sharing Accord[27], and each dataset will have its own supporting DPIA within PHS covering this.
In addition, a single MOU will cover all of the cancer datasets, including the CIP, and is under consideration by the National NHS Information Governance Leads for approval. With this approval, this will allow CHI linkable data to be sourced from the three cancer screening IT systems to create views within the CIP for all appropriate analyses.
Contact
Email: screening@gov.scot