Health and homelessness in Scotland: research
Study exploring the relationship between homelessness and health.
Chapter 7: Admissions to Mental Health Specialties
There were around 100,000 admissions to mental health specialties ( SMR04), hereafter referred to as mental health admissions) over the time period 1 April 2002 to 31 March 2015 inclusive for the 1.3 million people in the study [42] . Note that this is almost 100 times smaller than the number of mental-health prescriptions discussed in the previous chapter. These mental health admissions represent the most severe mental health issues. For more information on SMR04 mental health inpatient and day case data see Section 2.3.7.
In this chapter we discuss the study cohorts, their mental health admissions activity and how this relates to homelessness. How this relates to deprivation and health needs is discussed in Chapter 11.
7.1 Comparative activity between the EHC and their controls
Accounting for one third of all people in the study, people in the EHC (Ever Homeless Cohort) accounted for 80% of mental health admissions (47% male, 33% female). Mental health admissions amongst the MDC (Non-homeless 20% Most Deprived Cohort) accounted for 16% of admissions during the period (9% male, 7% female). The LDC (Non-homeless 20% Least Deprived Cohort) accounted for 4% of admissions (2% male, 2% female).
Table 7.1: Number of people, number of Mental health admissions and the ratio of the number of Mental health admissions between EHC and MDC, and between EHC and LDC, by age and sex.
| Age (at 31 March 2015) | Male | Female | ||||||
|---|---|---|---|---|---|---|---|---|
| Number of people | Admissions | EHC : MDC | EHC : LDC | Number of people | Admissions | EHC : MDC | EHC : LDC | |
| 0 to 15 | 135,444 | 131 | 0.1 | 1.3 | 127,461 | 97 | 3.1 | 0.5 |
| 16 to 20 | 49,263 | 554 | 4.5 | 4.7 | 51,276 | 804 | 4.0 | 1.7 |
| 21 to 25 | 64,209 | 2,353 | 6.5 | 14.5 | 78,690 | 2,713 | 3.6 | 10.4 |
| 26 to 30 | 75,363 | 5,560 | 8.6 | 25.2 | 93,003 | 4,505 | 5.5 | 19.0 |
| 31 to 35 | 70,407 | 8,761 | 6.1 | 25.4 | 74,493 | 6,174 | 5.5 | 30.5 |
| 36 to 40 | 58,347 | 8,669 | 6.4 | 31.8 | 53,259 | 5,928 | 4.8 | 21.8 |
| 41 to 45 | 55,737 | 9,628 | 5.4 | 55.9 | 48,873 | 6,287 | 4.0 | 21.2 |
| 46 to 50 | 49,818 | 8,211 | 4.8 | 34.7 | 43,563 | 6,213 | 3.4 | 17.1 |
| 51 to 55 | 37,746 | 6,558 | 4.6 | 23.2 | 31,578 | 4,585 | 4.5 | 19.9 |
| 56 to 60 | 25,017 | 3,416 | 4.7 | 34.9 | 19,017 | 2,277 | 5.3 | 19.1 |
| 61 to 65 | 15,765 | 1,928 | 4.1 | 12.8 | 11,436 | 1,150 | 4.0 | 20.1 |
| 66 or over | 21,591 | 2,237 | 3.8 | 9.2 | 16,203 | 1,316 | 3.3 | 6.7 |
| All ages | 658,707 | 58,006 | 5.4 | 25.5 | 648,852 | 42,049 | 4.4 | 16.0 |
In order to see how mental health admissions compare in the different cohorts, ratios of mental health admissions were constructed for each age band and sex ( Table 3.1).
The EHC have more mental health admissions
In total, the EHC has around five times the number of mental health admissions compared with the MDC (5.4 times for males, 4.4 for females) and around 20 times the number of mental health admissions compared with the LDC (25 times for males, 16 times for females).
For each age and sex breakdown among adults (those aged 16+ years), the EHC have more mental health admissions
Compared to the controls in the MDC or LDC, the ratio of attendances is always greater than one (minimum ratio is: 1.7, EHC : LDC at 16–20 years for females).
For male children, the EHC have fewer mental health admissions than the MDC, but similar to the LDC
The ratio EHC : MDC is 0.1, while EHC : LDC is 1.3. This is the only age-sex breakdown across the entire study where the MDC has the highest activity.
For female children, the EHC have more mental health admissions than the MDC, but fewer than the LDC
The ratio EHC : MDC is 3.1, while EHC : LDC is 0.5. The LDC has significantly higher activity than the EHC or the MDC for females aged 0 to 15 years.
Among adults, the ratios for EHC : LDC vary more with age than those for EHC : MDC
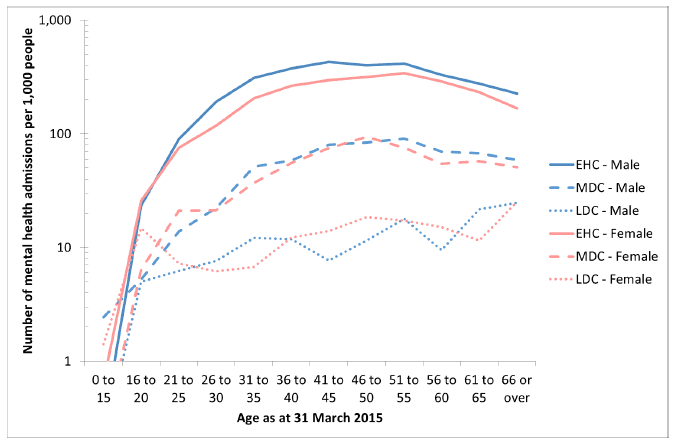
The ratios for EHC : MDC vary with age. For adult males the maximum EHC : MDC ratio is 8.6 (at 26–30 years) and the minimum is 3.8 (at 66+ years). For adult females the highest and lowest are 5.5 (at 26–35 years) and 3.3 (at 66+ years). The age profile of admissions among the EHC is roughly similar to that of the MDC ( Figure 7.1). In contrast the highest and lowest of the adult male EHC : LDC ratio are 56 (at 41–45 years) and 4.7 at 16–21 years. For females the highest and lowest are 30 (at 31–35 years) and 1.7 (at 16–20 years). In particular the mental health admission rate increases much less between 16–20 and 36–40 years among the LDC than among the MDC or EHC. Beyond about 50 years the EHC and MDC admission rates start to decline, while the LDC admission rate increases.
Figure 7.1: Number of mental health admissions per 1,000 people (admission rate) by age, sex and cohort. (Note: the y-axis uses a logarithmic scale.)
7.2 Distribution of the number of mental health admissions
The previous section found that, on average, people in the EHC had more mental health admissions than their controls. This section explores whether this is due to a higher proportion of the EHC having admissions, or a higher proportion of the EHC who had admissions having many admissions, or both ( Figure 7.2). The following points apply for both sexes:
More of the EHC had at least one mental health admission
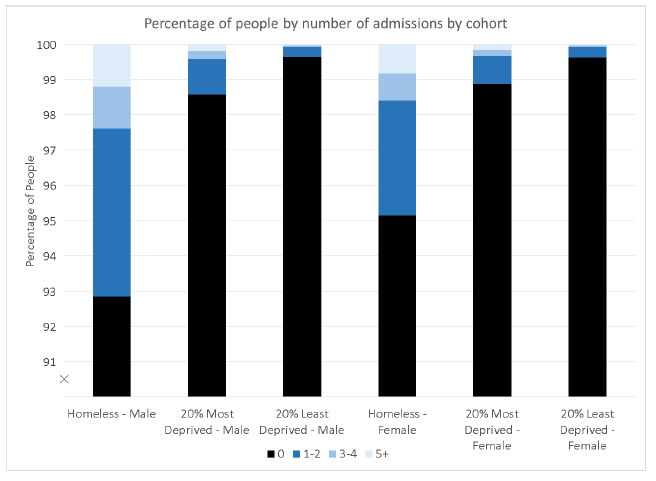
A higher proportion of the EHC (7.2% males, 4.9% females) had at least one mental health admission, compared to the MDC (1.4% males, 1.1% females) and LDC (0.4% males, 0.4% females) over the study period.
More of the EHC had many mental health admissions
A higher proportion of the EHC (1.2% males, 0.8% females) had five or more mental health admissions than the MDC (0.2% males, 0.2% females) and LDC (0.04% males, 0.04% females) over the study period. Even among people who had at least one mental health admission, a higher proportion of the EHC had multiple admissions compared to the MDC and LDC.
Figure 7.2: Percentage of people by number of mental health admissions, by cohort and sex. (Note: there is a break in the y-axis.)
7.3 Mental health admissions relative to the date of first homelessness assessment
In Section 7.1 it was found that the EHC have more mental health admissions than both control cohorts. In order to explore the relationship between homelessness and mental health activity, this section compares the timing of admissions with the date of first homelessness. Detail on this method is described in full in Section 2.10.
As shown in previous chapters, there appears to be differences in activity for Once-only EHC and Repeat EHC. This could be due to more periods of homelessness, but at different times for different people, or it could be a long term effect of the original homelessness assessment.
This section presents ratios between those people in that have only been assessed as homeless once ( Figure 7.3) (Once-only EHC), and those who have been assessed as homeless on multiple occasions, referred to as repeat homelessness (Repeat EHC) ( Figure 7.4). More information on repeat homelessness is available in section 2.1.3.
Mental health admission ratios for Repeat EHC are higher than for Once-only EHC. The following points generally apply for both sexes:
Admission ratios begin increasing four years prior to assessment date for Repeat EHC males
For Repeat EHC males the admission ratio increases from around 10, four years prior to the assessment date, to around 80, immediately prior to the peak. This pattern is not observed among the females to the same extent or for the once-only EHC. This pattern was not observed for prescriptions for mental health, where the mental health issues are likely of lesser severity.
The admission ratio peak is more pronounced for Once-only EHC, especially among males
For Once-only EHC males the peak value is around 80 compared with about 25 surrounding this (around three times larger). For females the peak is around 45, compared with less than 20 either side of the peak (around 2.5 times larger). For the Repeat EHC males the peak value is around 145, compared with around 80 either side (around 80% larger). For female Repeat EHC the ratio increases from about 25 to 45 (around 80% larger), but does not immediately drop substantially.
The ratio falls back to pre-homelessness levels only for Once-only EHC
For the Once-only EHC, by around five years for males (around seven years for females) following the assessment date the ratio has reduced to around the level it was at two years prior to the assessment date. This contrasts with the Repeat EHC ratio. For the males the ratio gradually decreases but remains notably above the value it had before it began to increase about four years before the first assessment. For females the ratio does not substantially decrease at all, but remains almost at the level it had at the time of first homelessness assessment.
Figure 7.3: Ratio of mental health admissions per month in each cohort to that of the LDC, where the homeless person had one homelessness assessment during the period, by sex.
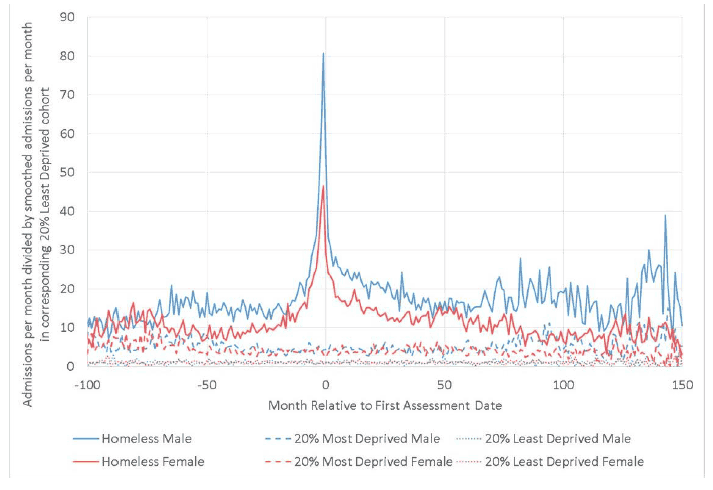
Figure 7.4: Ratio of mental health admissions per month in each cohort to those of the LDC, where the homeless person had multiple homelessness assessments during the period (repeat homelessness), by sex.
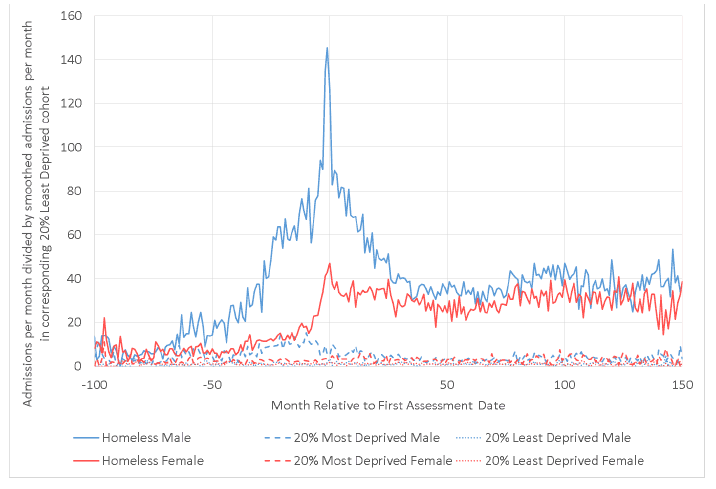
7.4 Summary
The EHC have more of the most acute mental health admissions (as recorded in the SMR04 dataset). The age profile of admissions among the EHC is roughly similar to that of the MDC, with more admissions in the 26-50 year age range. In contrast, admissions for people in the LDC vary less with age. More of the EHC had at least one mental health admission, and more of these had multiple mental health admissions.
It is clear that there is evidence to support each of the four research questions:
- A gradually worsening condition prior to the date of first assessment that results in excess mental health admissions, occurring prior to homelessness. This is particularly pronounced for Repeat EHC males.
- Also for some people the (first) homelessness episode is associated with some crisis with a health activity component, as observed by a mental health admission peak around that time. Both Once-only and Repeat EHC have very large and well defined peaks around that time, with Once-only being more pronounced.
- The larger ratios after the first assessment date for those who have multiple homelessness episodes could be due to: further crises around the time of those later episodes, or long-term effects of the earlier underlying worsening condition, crises or homelessness itself.
- Lastly, people who go on to become homeless appear to have more of the most acute mental health admissions, even several years prior to their first homeless assessment.