Health and homelessness in Scotland: research
Study exploring the relationship between homelessness and health.
Chapter 11: Discussion
Having analysed all the health and homelessness study data, this chapter aims to bring the findings together and consider these in relation to the four study research questions. Any other findings of interest relating to homelessness and/or health are also presented.
11.1 Homelessness
11.1.1 Homelessness affects many people in Scotland
Annual homelessness publications report that there were 28,247 HL1 applications assessed as homeless or threatened with homelessness during 2016/17. It is not known whether assessments made in different years are by the same people or different people. If these were all the same people then that would suggest that homelessness affects a relatively small proportion of the Scottish population (5.3 million in 2011, as reported by Scotland's Census). However if these are all different people then a more substantial proportion of the population would be affected.
This study covers 435,853 people who were included in at least one HL1 application that was assessed as homeless or threatened with homelessness between June 2001 and November 2016. Even though not all HL1 applications were included in the study (76% of applications over this time are included), and not all people were included in all the applications provided, this still represents 8% of the Scottish population as at 30 June 2015. Therefore a significant minority of people in Scotland have experienced homelessness at some point.
This indicates that the assessments do not represent a small group of people making many homelessness applications. Specifically we see that 29% of males and 26% of females among the Ever Homeless Cohort ( EHC) were classed as repeat homelessness; they were included in more than one HL1 application that was assessed as homeless or threatened with homelessness over the study period.
11.1.2 Time spent as homeless
People included in the EHC spent 9.7% of their time (for males, 9.2% for females) in open homelessness cases. Open cases are those where the Local Authority has not yet discharged its duties under the homelessness legislation – for example, waiting for suitable accommodation to become available. The above time was calculated from the date of their first homelessness assessment until the end of the study period (or the date of their death, whichever is earlier). Further work would be required to determine how sensitive this is to the study period used. (For example were the study period very short then the majority of EHC people would still be in open homelessness cases by the end of the study period and this figure would be much higher.)
11.1.3 Homeless people are younger than the general population
The homeless people included in the study tend to be younger than the population generally. This finding is consistent with published data [51] . It was also observed that health activity related to drugs was higher among younger people. If drug use is a cause of homelessness then this could also explain why some homeless people tend to be younger. The proportion of people in the EHC at around 20–30 years was higher for females than for males.
While this younger distribution is consistent with published data, it also indicates that comparisons cannot be made directly between the EHC and the general population. Any observed differences could be due to the difference in the age distribution. Therefore for the study comparisons are made with two control cohorts: drawn from people residing the 20% most deprived areas ( MDC) and in the 20% least deprived areas ( LDC). Each of these cohorts has the same age and sex distribution as the EHC so differences observed will not be due to age or sex.
11.2 Research questions
During the analysis, the following research questions arose to describe the relationship between health and homelessness:
1. How does health prior to the first homelessness assessment influence homelessness?
2. Does the point at which someone becomes homeless have an impact on one's health? Is a crisis with a health component involved?
3. How does homelessness influence health?
4. Is there a relationship between health, homelessness and area-based deprivation?
The EHC is selected from a population identified by an individual measure, while the controls are selected from a population identified by an area-based measure. It is likely that more people in the EHC are affected by factors associated with deprivation than in the LDC or even the MDC. For example, most people in the 20% most deprived areas are neither income or employment deprived. It is therefore possible that differences between the EHC and both the LDC and MDC are due to different levels of these factors associated with deprivation, rather than homelessness itself.
The MDC and LDC may also contain people from the 24% of homelessness assessments that were not submitted for the study. The inclusion of these people in the MDC and LDC cohorts would lead to smaller differences between the cohorts than would otherwise be the case. This issue is likely to affect the MDC cohort more than the LDC cohort.
To better explore the link between health activity and homelessness itself (as distinct from factors associated deprivation), analysis is done that compares the time of the health activity with the date of first homelessness assessment. The following figures in this chapter bring together these analyses from across the analysis chapters ( Chapters 3 to 9). The findings from these are discussed in the following sub-sections.
Health activity ratios between the EHC and LDC in relation to the date of first homelessness assessment are shown in Figures 11.1a, 11.1b, 11.2a and 11.2b, as was done in previous chapters. Figures 11.1b and 11.2b are zoomed in versions of 11.1a and 11.2a respectively. The MDC : LDC ratios are not shown for clarity. Also for clarity, the trends have been further smoothed to reduce the noise and make the overall structure clearer. This also has the effect of making the peaks around the time of first homelessness assessment less pronounced. In most cases these are separated out by Repeat and Once-only EHC. The exception to this is the acute admissions to hospital ( SMR01), which are shown for each of the six reason categories discussed in Chapter 4. Figures 11.1a and 11.1b relate to males, while figures 11.2a and 11.2b relate to females.
Figure 11.1a: An increase in health activity precedes the first homelessness assessment for males. Some activity remains higher after this date, particularly for drug-related and alcohol-related acute admissions, and for repeat homeless people - mental health admissions ( SMR04) and mental health prescriptions.
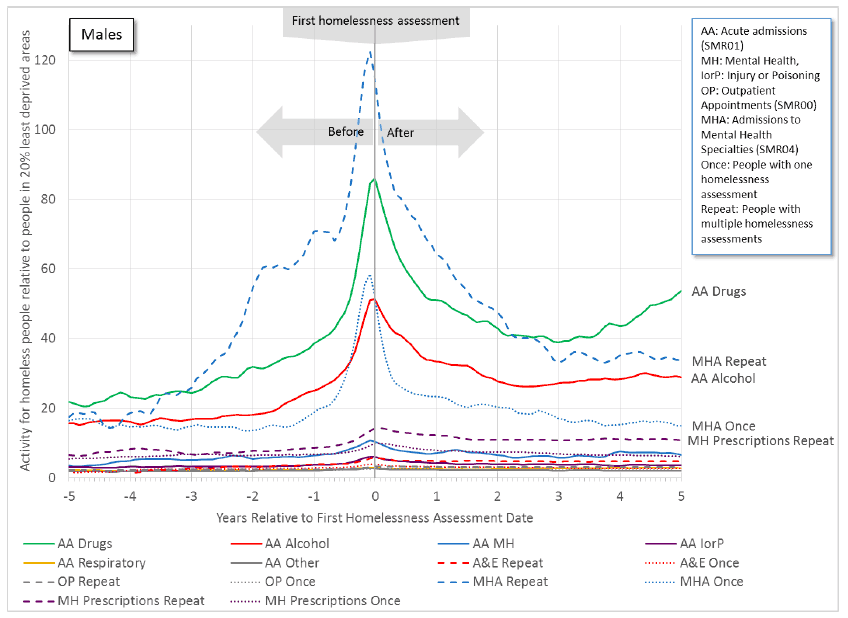
Figure 11.1b: An increase in health activity precedes the first homelessness assessment for males. Some activity remains higher after this date, particularly for mental health acute admissions ( SMR01), mental health prescriptions and A&E attendances by repeat homeless persons.
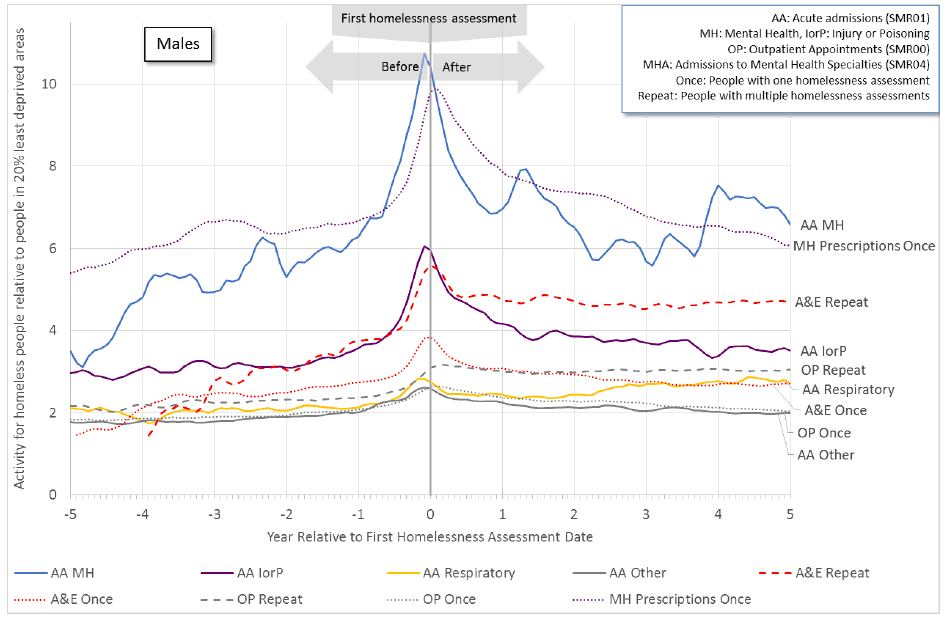
Figure 11.2a: An increase in health activity precedes the first homelessness assessment for females. Some activity remains higher after this date, particularly for drug-related and alcohol-related acute admissions, and for repeat homeless people - mental health admissions ( SMR04) and mental health prescriptions.
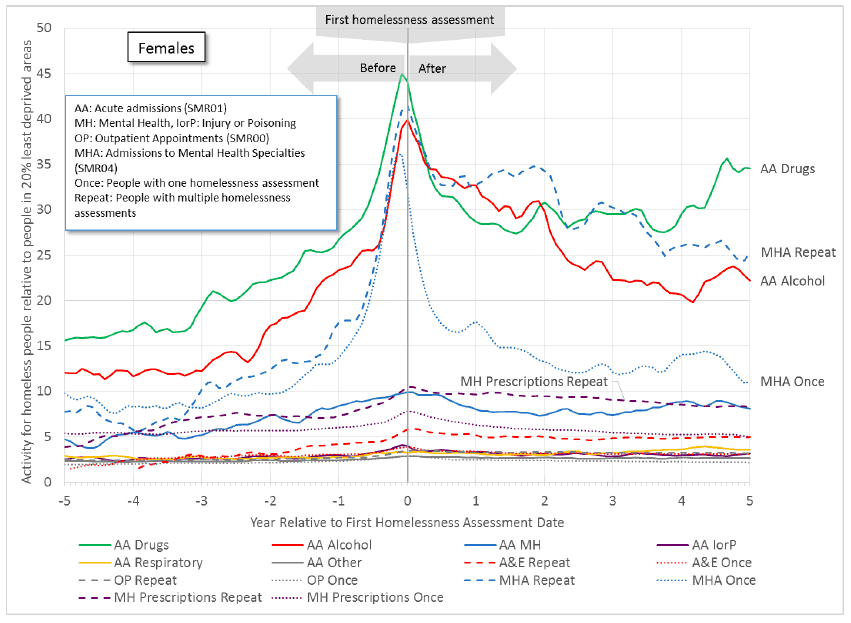
Figure 11.2b: An increase in health activity precedes the first homelessness assessment for females. Some activity remains higher after this date, particularly for mental health acute admissions ( SMR01) and A&E attendances by repeat homeless persons.
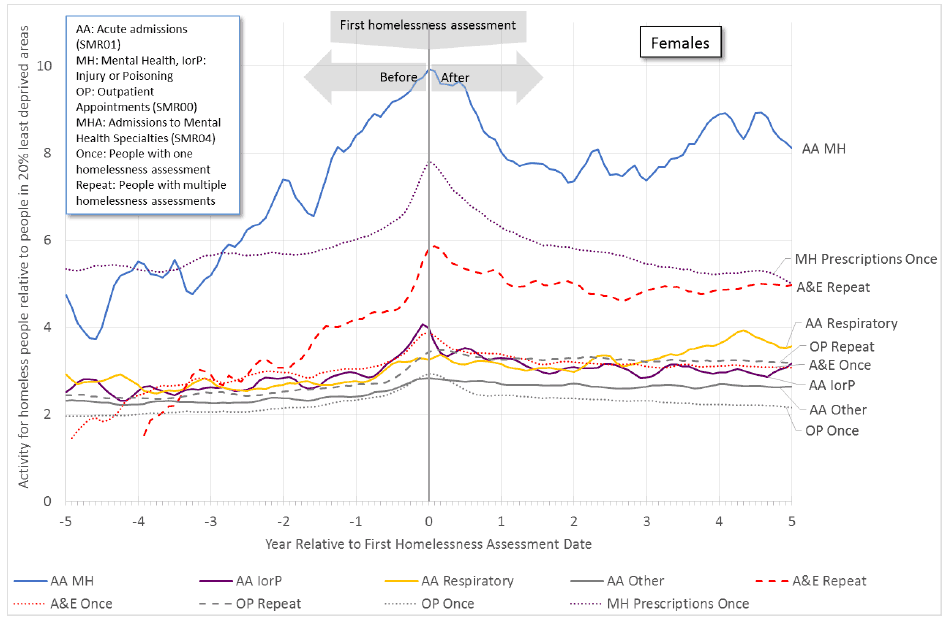
11.2.1 Research question 1: How does health prior to the first homelessness assessment influence homelessness?
Research question 1 concerns whether people with poorer health are more likely than people who are otherwise similar to go on to become homeless. This effect can be explored through examining the temporal plots prior to the date of first homelessness assessment. We are specifically interested here where the temporal ratios increase in the lead up to the date of first homelessness assessment.
An increase in health activity up to the date of the first homelessness assessment is observed for:
- drug, alcohol and mental-health acute admissions, and A&E
- outpatients, and mental-health prescriptions (to a lesser extent)
- acute admissions for injury and poisoning and mental-health admissions ( SMR04) (for males)
- SDMD assessments ( figures 8.4 and 8.5)
- People with experience of repeat homelessness (the repeat EHC) in particular
Such patterns are not observed (or if it is observed the effect size is much lower) for:
- acute admissions for respiratory conditions and other acute admissions
It is interesting that these effects are less apparent for respiratory conditions and other acute admissions. The effects are most clearly seen for health activity that relates to issues such as mental health, drugs and alcohol. These issues are likely to be risk factors for homelessness.
11.2.2 Research question 2: Does the point at which someone becomes homeless have an impact on one's health? Is a crisis with a health component involved?
Research question 2 relates to health activity around the time of first homelessness assessment. This explores whether becoming homeless can be associated with an acute crisis that has a health component. Such activity would show on the temporal plots as a peak around the date of homelessness assessment.
A peak in activity around the first homelessness assessment is observed for:
- drug, alcohol and injury or poisoning acute admissions, mental health admissions ( SMR04), A&E, mental-health prescriptions
- acute admissions for mental health,
- for males acute admissions for respiratory and other conditions
- SDMD assessments (figures 8.4 and 8.5)
Such patterns are not observed (or if it is observed the effect size is much lower) for:
- outpatient appointments among the Repeat EHC
- for females, acute admissions for respiratory and other conditions
Peaks in health activity occur around the date of the first homelessness assessment (with larger peaks for males). This suggests a relationship between becoming homeless and health activity. It may be that for some people becoming homeless is associated with a crisis that has a health aspect. This is particularly (although not exclusively) associated with activity related to drugs, alcohol and mental health. The health activity may be symptomatic of acute problems, which in turn could lead to homelessness.
Given that crises around the time of homelessness appears to have some impact on health activity, it would seem likely that preventing homelessness could reduce health activity, and improve health outcomes.
11.2.3 Research question 3: How does homelessness influence health?
Research question 3 concerns whether homelessness episodes have an effect on health. This effect can be explored through examination of the part of the temporal plots following the date of first homelessness assessment. To ensure that the activity is related to the homelessness episode(s) it is necessary to compare these activity levels with activity levels prior to homelessness.
Under research question 2, a peak of activity can occur around the first homelessness assessment. Therefore, for people who have multiple homelessness assessments there is likely to be heightened health activity around the time of these later assessments. This would show up as a similar pattern to that sought by research question 2. To address this the difference between the patterns for the Once-only EHC and that for the Repeat EHC are discussed. Any such pattern that is observed among the Once-only EHC cannot be due to these further peaks, and so would likely be due to the effect of homelessness. Patterns observed among the Repeat EHC may be due to effects of homelessness itself or due to further crises.
A pattern of higher activity following first assessment is observed for:
- drug, alcohol, mental health and respiratory acute admissions (although this has not been split by once-only and repeat homelessness)
- all repeat trends (mental-health admissions ( SMR04), mental-health prescriptions, outpatient appointments and A&E attendances)
- female once-only A&E
- repeat SDMD assessments ( figures 8.4 and 8.5)
Such patterns are not observed (or if it is observed the effect size is much lower) for:
- all once-only trends (apart from female once-only A&E)
- acute admissions injury or poisoning
- other acute admissions for males
It is not possible to say that health activity following homelessness is the direct consequence of homelessness itself. It could be due to a further crises or health problems such as drug or alcohol related conditions, or a mental health condition.
For those who had been homeless on only one occasion health activity eventually returned to the (albeit higher) pre-homelessness levels. However, for people who were homeless on multiple occasions, levels of health activity remained high.
There is clear evidence of a relationship between repeat homelessness, drugs, alcohol and mental health. Chapter 9 showed that drug-related deaths were much higher amongst those experiencing repeat homelessness. Chapter 10, showed a much higher proportion of repeat homeless people have drug, alcohol and mental health related health issues. These factors may be driving some of the increase in health activity following the first homelessness assessment.
Temporal analysis was not done for deaths. For males in the EHC, mortality was around a third higher during periods of homelessness than during periods when they were not in open homelessness cases. This difference may be driven by the higher number of drug-related deaths amongst males that had been homeless on multiple occasions.
11.2.4 Research question 4: Is there a relationship between health, homelessness, and area-based deprivation?
Homeless people are more likely to come from deprived areas, based on their last settled address. The distribution of homeless people across the area-based deprivation spectrum (as measured by the Scottish Index of Multiple Deprivation) closely follows the distribution of income and employment deprived people.
The health activity of people in the EHC was consistently higher than for the non-homeless controls in the 20% most deprived areas ( MDC). In turn, this was consistently higher than the non-homeless controls in the 20% least deprived areas ( LDC).
This was observed for:
- all types of health activity (especially for activity related to mental health, and drugs and alcohol)
Health inequalities are known to exist across Scotland and they are monitored using area-based measures of deprivation. Using health activity as an imperfect proxy for poor health, the study provides evidence that health inequalities are likely to exist between people that have experienced homelessness and those who have not.
11.3 Other findings
11.3.1 Cause of death
Differences in mortality between the cohorts varied by cause of death, although for each cause mortality among the EHC was at least as high as for the controls. The differences were highest for drugs, alcohol, intentional self-harm, and assault. This results in the main causes of death among the EHC being drugs, heart disease and strokes, and, for males, alcohol and, for females, cancer. Note that the extent of the study period is limited so deaths for only a minority of the EHC are recorded. As the EHC age further the distribution of cases of death will likely vary and so these cases may not ultimately be the main causes of death across the whole EHC.
Differences in mortality due to drug-related conditions between the EHC and the controls were higher for people who have multiple homelessness assessments, than for the differences for those who have exactly one homelessness assessment during the study period.
11.6.2 Proportion of study with no drugs, alcohol or mental health issues
Chapters 3– 9 were concerned with examining the differences in health activity between the cohorts for a number health activity datasets. Chapter 10 focused instead on individuals, and what health activity they had experienced during the study across multiple datasets.
A majority of the EHC did not have any evidence of mental-health, drugs or alcohol health related activity during the study period (51%), which is lower than for both control cohorts ( MDC 74%, LDC 86%).
Just under a third of the EHC (30%) have had a mental health issue which excludes drug- or alcohol-related issues. This was higher than in the control groups.
There was evidence of drug and/or alcohol-related interactions for the remaining fifth of people (19%). Of these, the vast majority (94%) also had evidence of mental health issues.
11.6.3 Overlap of drugs, alcohol and mental health issues
In total, 49% of the EHC had a least one mental-health, drugs or alcohol health related activity during the study period. These did not occur independently – i.e., having one issue meant that an individual was more likely to have another.
More people in the EHC had drug-related issues than alcohol-related issues. However, in the controls these were comparable. Of those that had drugs and/or alcohol related issues, a higher proportion in the EHC had both than in the controls.
5.9% of the EHC had evidence of mental-health, drugs and alcohol related issues during the study period, which is considerably more than for both control cohorts. A higher proportion of males have all three issues than females for the EHC. Furthermore, the proportion of people with all three issues is much higher among those that have had multiple homelessness assessments (11.4% compared with 3.8% for once-only homeless).
11.6.4 Proportion of EHC by background flags (prison, sleeping rough, previously looked after by a local authority)
Chapter 10 examined the overlap between people in the EHC who experienced mental-health, drugs and alcohol issues during the study with a range of other background attributes.
Higher proportions of people who had been looked after, had slept rough, or had been recently discharged from prison had evidence of all three mental-health, drugs and alcohol issues during the study. Higher proportions of drug-related issues amongst these groups are consistent with published work.
11.4 Possible further work
Further work may wish to use the data from this study to:
- Create a predictive model using healthy activity data to identify people at risk of homelessness.
- Consider the health activity of people who were not assessed as homeless. These people applied to local authorities for assistance but were excluded from the study as they were not assessed as homeless or threatened with homelessness.
- Investigate how health activity varies with the time spent when people are in open homeless cases and at other times.
- Investigate the health activity of people who were in homeless applications as children. How many of these children subsequently became the main applicant of a future homelessness assessment?
Additional datasets could be brought into the study to consider the impact of factors such as prison leavers, leaving care and the justice system on health and homelessness. Survey data might also be useful to consider what background factors may impact upon health activity and homelessness.
Further work may wish to consider whether homelessness can be used as an individual indicator of deprivation to help target resources.
11.5 Summary
In summary:
- At least 8% of the Scottish population (as at 30 June 2015) had experienced homelessness at some point in their lives.
- Of those who had experienced homelessness:
- over half (51%) had no evidence of health conditions relating to drugs, alcohol or mental health conditions. This was much lower than in the control groups ( MDC 74%, LDC 86%).
- Around 30% had evidence of a mental health problem at some point during the study period (with no evidence of drug or alcohol-related conditions at any point). This was higher than in the control groups.
- There was evidence of drug and/or alcohol-related interactions for the remaining fifth of people (19%). Of these, the vast majority (94%) also had evidence of mental health issues.
- In particular, around 6% of people experiencing homelessness had evidence of all three of the following conditions – a mental health condition, a drug-related condition and an alcohol-related condition – although not necessarily concurrently. This was much higher than in the control groups. The figure was markedly higher for those experiencing repeat homelessness.
- Increased health activity preceded people becoming homeless
- A peak in health activity was seen around the time of the first homelessness assessment.
- Increased health activity was seen after some people had become homeless, although this may be due to factors other than the person being homeless.
- Based on their use of services, people who go on to become homeless have poorer health than others. This is likely to be due to a wide range of complex factors.