Health and homelessness in Scotland: research
Study exploring the relationship between homelessness and health.
Chapter 4: Acute Hospital Admissions
There were 2.3 million acute hospital admissions ( SMR01) for the 1.3 million people in the study over the time period 1 April 2002 to 31 March 2015. For more information on the acute admissions data see Section 2.3.4.
In this chapter we discuss the study cohorts and their acute admission activity and how this relates to homelessness. How this relates to deprivation and health needs is discussed in Chapter 11.
4.1 Comparative activity between the EHC and their controls
Accounting for one third of all people in the study, people in the EHC (Ever Homeless Cohort) accounted for 52% of all acute admissions (27% male, 26% female). Acute admissions amongst the MDC (20% Most Deprived Cohort) accounted for 31% of acute admissions during the period (15% male, 16% female), acute admissions from the LDC (20% Least Deprived Cohort) accounted for 17% (9% male, 8% female).
Table 4.1: Number of people, number of admissions and the ratio of the number of acute hospital admissions between EHC and MDC, and between EHC and LDC, by age and sex.
| Age (at 31 March 2015) | Male | Female | ||||||
|---|---|---|---|---|---|---|---|---|
| Number of people | Admissions | EHC : MDC | EHC : LDC | Number of people | Admissions | EHC : MDC | EHC : LDC | |
| 0 to 15 | 135,444 | 170,531 | 1.2 | 1.6 | 127,461 | 127,225 | 1.2 | 1.6 |
| 16 to 20 | 49,263 | 51,570 | 1.2 | 1.8 | 51,276 | 52,115 | 1.3 | 2.4 |
| 21 to 25 | 64,209 | 66,299 | 1.8 | 2.7 | 78,690 | 98,483 | 2.0 | 3.9 |
| 26 to 30 | 75,363 | 83,063 | 2.2 | 3.9 | 93,003 | 135,473 | 2.2 | 5.0 |
| 31 to 35 | 70,407 | 86,344 | 2.6 | 4.8 | 74,493 | 119,083 | 2.2 | 4.9 |
| 36 to 40 | 58,347 | 84,160 | 2.6 | 5.3 | 53,259 | 95,300 | 1.9 | 4.2 |
| 41 to 45 | 55,737 | 101,775 | 2.3 | 5.0 | 48,873 | 103,163 | 1.7 | 3.6 |
| 46 to 50 | 49,818 | 107,472 | 2.1 | 4.3 | 43,563 | 110,521 | 1.6 | 3.3 |
| 51 to 55 | 37,746 | 103,429 | 2.0 | 4.1 | 31,578 | 93,160 | 1.5 | 3.0 |
| 56 to 60 | 25,017 | 84,758 | 1.8 | 3.4 | 19,017 | 63,565 | 1.4 | 2.8 |
| 61 to 65 | 15,765 | 66,244 | 1.6 | 3.1 | 11,436 | 44,695 | 1.4 | 2.3 |
| 66 or over | 21,591 | 131,506 | 1.4 | 2.1 | 16,203 | 86,210 | 1.2 | 1.9 |
| All ages | 658,707 | 1,137,151 | 1.8 | 3.1 | 648,852 | 1,128,993 | 1.7 | 3.1 |
In order to see how acute admissions compare in the different cohorts, ratios of acute admissions were constructed for each age band and sex ( Table 4.1) and the admission rate is also calculated ( Figure 4.1).
The EHC have more acute admissions
In total, the EHC has nearly double the number of acute admissions compared with MDC (1.8 times for males, 1.7 for females) and 3.1 times the number of acute admissions compared with LDC (both for males and for females).
The acute admission rate is highest among older people for each cohort
In each cohort the number of acute admissions per 1,000 people increases with age from 31–35 to 66+.
For each age and sex breakdown, the EHC have more acute admissions
Compared to the controls in the MDC or LDC, the ratio of acute admissions is always greater than one (minimum ratio is: 1.2, EHC : MDC for males at 0–20 years, and for females at 0–15 and 66+).
EHC males aged 36–40 years have the most acute admissions compared with their controls
For males EHC : LDC peaks at 5.3 at 36–40 years, and EHC : MDC peaks at 2.6 at 31–40 years. For the controls the acute admission rate decreases with age, reaching a minimum around 30-35 years and then increases again , while for the EHC the admission rate increases from 16 years and onward. This difference in shape is what drives the variation in the ratio with age ( Figure 4.1). The peak ratio occurs around when the admission rate among the controls reaches a minimum, and the EHC admission rate is continuing to increase.
EHC females aged 26–30 years have the most acute admissions compared with their controls
For females EHC : LDC peaks at 5.0 at 26–30 years, and EHC : MDC peaks at 2.2 at 26–35 years. This is a similar effect to that seen among males. However among females the admission rate minima among the controls occurs at younger ages, and there is a bulge in the EHC admission rate between 16–20 and 41–45. Both of these differences push the peak ratio between the cohorts to a younger age group.
Figure 4.1: Number of acute admissions per 1,000 people (admission rate) by age, sex and cohort.
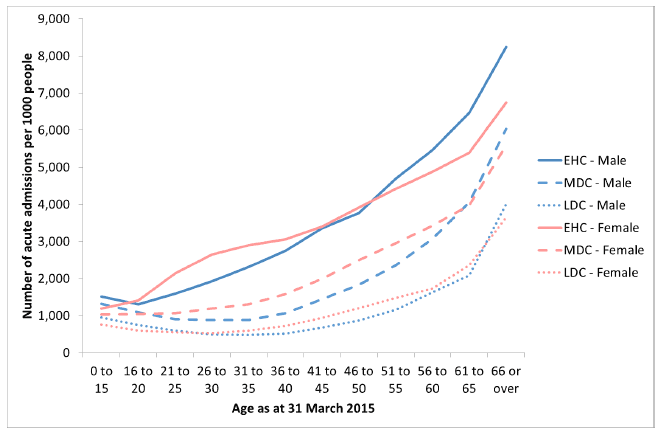
Note: this is not a rate per year so is not comparable with admission rates published elsewhere.
4.2 Distribution of the number of acute hospital admissions
The previous section found that, on average, people in the EHC had more acute admissions than their controls. This section explores whether this is due to a higher proportion of the EHC having acute admissions, or a higher proportion of the EHC who had attendances having many acute admissions, or both ( Figure 4.2). The following points apply for both sexes:
More of the EHC had at least one acute admission
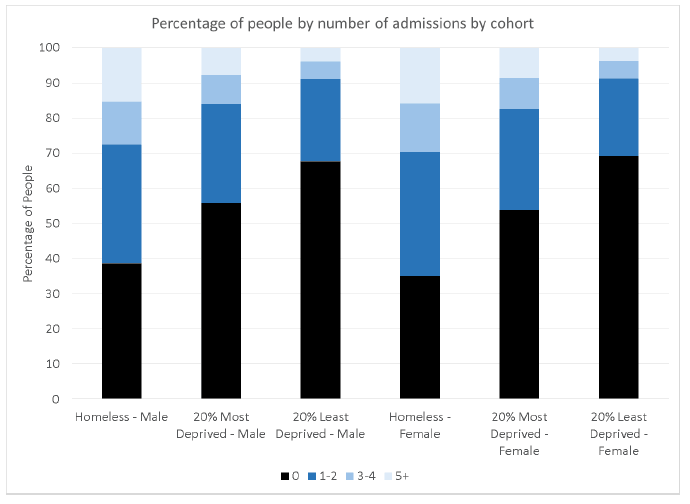
A higher proportion of the EHC (61% males, 65% females) had at least one acute admission than the MDC (44% males, 46% females) and LDC (32% males, 31% females) over the study period.
More of the EHC had many acute admissions
A higher proportion of the EHC (15% males, 16% females) had five or more acute admissions than the MDC (8% males, 9% females) and LDC (4% males, 4% females) over the study period. Even among people who had at least one acute admission, a notably higher proportion of the EHC had many admissions than the MDC and LDC.
Figure 4.2: Percentage of people by number of acute admissions by cohort and sex.
4.3 Length of stays by age and cohort
Having seen that the EHC have more acute admissions than the control cohorts, this section explores the length of these admissions ( Table 4.2 and Figure 4.3). Each admission record contains information on the length of stay in days. This is the difference between the date of admission and the date of discharge [37] . Note that the data used in this study does not distinguish between inpatient admissions with a zero length of stay and day case admissions. For the purposes of the average inpatient length of stay, inpatients include only those admissions with a length of stay of at least one day. This will therefore not be directly comparable with the ISD (Information Services Division, National Services Scotland of the NHS) average length of stay publication, as that includes zero length of stay inpatient admissions [38] .
Figure 4.3: Percentage of admissions by length of stay, by cohort and sex.
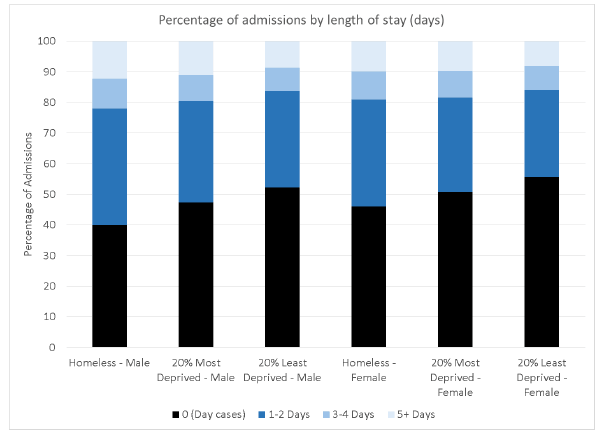
More of the EHC acute admissions include an overnight stay
A higher proportion of the EHC acute admissions (60% male, 54% female) include an overnight stay than among those in the MDC (53% male, 49% female), and LDC (48% male, 44% female).
The distribution of length of stay among acute inpatient admissions is similar between cohorts
The distribution of length of stay among admissions that include an overnight stay is about the same between the different cohorts for males, and also about the same between cohorts for the females ( Table 4.2).
Perhaps people in the EHC have more health issues requiring an inpatient admission. However as these inpatient admissions are then discharged within a similar time (and do not require longer stays) to those in the controls, perhaps these health issues have similar severity to those of the controls.
Table 4.2: Percentage of admissions by the number of days the admission was over, for each cohort and sex. Also shown is the average (mean) length of stay of each inpatient admission (admission with a length of stay of 1+ days), calculated from the total length of all admissions and the number of inpatient admissions.
| Male | Female | |||||
|---|---|---|---|---|---|---|
| EHC | MDC | LDC | EHC | MDC | LDC | |
| Percentage of admissions that have length of stay (days) of: | ||||||
| 0 | 40 | 47 | 52 | 46 | 51 | 56 |
| 1 | 27 | 23 | 22 | 24 | 21 | 20 |
| 2 | 11 | 10 | 9 | 11 | 10 | 9 |
| 3 | 6 | 5 | 5 | 6 | 5 | 5 |
| 4 | 4 | 3 | 3 | 4 | 3 | 3 |
| 5+ | 12 | 11 | 9 | 10 | 10 | 8 |
| Total | 100 | 100 | 100 | 100 | 100 | 100 |
| Number of inpatient admissions (where admission had a length of stay of 1+ days) | 362,312 | 177,930 | 93,749 | 316,235 | 174,276 | 83,661 |
| Total length of stays in days | 1,507,223 | 727,978 | 343,885 | 1,128,889 | 650,280 | 301,365 |
| Average inpatient length of stay | 4.2 | 4.1 | 3.7 | 3.6 | 3.7 | 3.6 |
4.4 Temporal analysis: admissions relative to the date of first homelessness assessment
In Section 4.1 it was found that the EHC have more acute admissions than both control cohorts. In order to explore the relationship between homelessness and acute activity, this section compares the timing of acute admissions with the date of first homelessness assessment ( Figure 4.4). Detail on this method is described in full in Section 2.10.
The shape of the graph for the EHC is markedly different from the MDC. The following points apply for both sexes:
The MDC had consistently more acute admissions than the LDC
The MDC had approximately double the number of acute admissions than the LDC. This ratio is roughly constant over time. This makes sense as there would be no particular reason for the activity of people in these cohorts to change with reference to the date of first homelessness assessment.
Even several years before the date of first assessment, the EHC ratio is higher
People who go on to become homeless appear to have more acute admissions, years prior to their first homeless assessment.
EHC acute admissions increase towards assessment date
From around four years prior to, to a few months before, the date of first homelessness assessment, EHC acute admissions increase relative to LDC acute admissions (from a ratio of around 2.5 to 3.25).
There is a clear peak in EHC acute admissions around assessment date, especially for males
In the weeks and months immediately prior to the date of first homelessness assessment, EHC acute admissions increase sharply (peak value of around 5 for males and 4 for females). Notably, the observed peak is not after the date of first homelessness assessment. This suggests that becoming homeless is, for some people, part of a crisis, which has health components.
EHC acute admissions stabilise after the peak, but at a higher level
EHC acute admissions stabilise one to two years following the date of first homelessness assessment for several years at a level (roughly 3.25), similar to that immediately prior to the sharp increase.
If differences in acute admissions between the cohorts were driven by deprivation alone, then the shape of the EHC line would be similar to that of the MDC. Therefore, it appears that homelessness has a relationship with acute admissions.
Figure 4.4: Ratio of acute admissions per month (relative to assessment date) for each cohort to the admissions among the LDC, by sex.
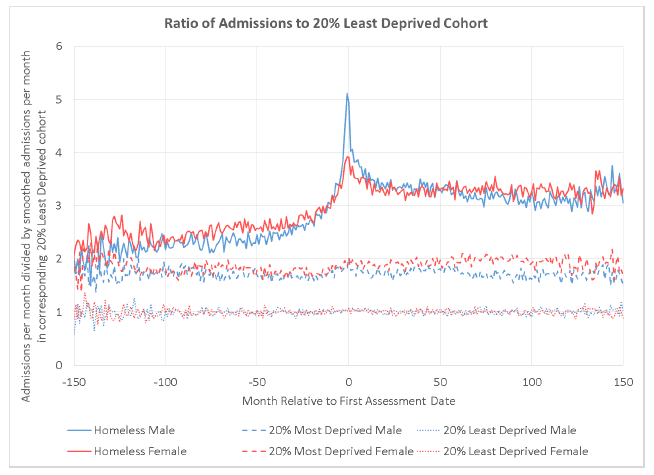
4.5 Acute admissions for Once-Only and Repeat Homelessness
In the previous section, EHC acute admissions were shown to be higher after the date of first homelessness assessment than before. This could be due to more periods of homelessness, but at different times for different people, or it could be a long term effect of the original homelessness assessment. To better understand this, this section explores differences in acute admission ratios between those people in that have only been assessed as homeless once ( Figure 4.5) (Once-only EHC), and those who have been assessed as homeless on multiple occasions, referred to as repeat homelessness (repeat EHC) ( Figure 4.6). More information on repeat homelessness is available in section 2.1.3.
Acute admission ratios for Repeat EHC are higher than for Once-only EHC. The following points generally apply for both sexes:
Acute admission ratios prior to assessment date are higher for Repeat EHC
For the Repeat EHC the ratio prior to the assessment date is around 3 (for both males and females). This is higher than that for the once-only EHC, which is around 2.5 (for both males and females).
The acute admission peak ratio is sharper for Repeat EHC
The peak around the date of first homelessness assessment increased more sharply for the repeat EHC than for the once-only EHC.
The ratio falls back to pre-homelessness levels only for once-only EHC
For the once-only EHC, by around five years for males (around 10 years for females) following the assessment date the ratio has reduced to around the level it was at two years prior to the assessment date.
This contrasts with the repeat EHC ratio, which remains above the ratio value immediately prior to the peak, for the remainder of the period.
Figure 4.5: Ratio of admissions per month (relative to assessment date) for people with one homelessness assessment for each cohort to the admissions among the LDC by sex.
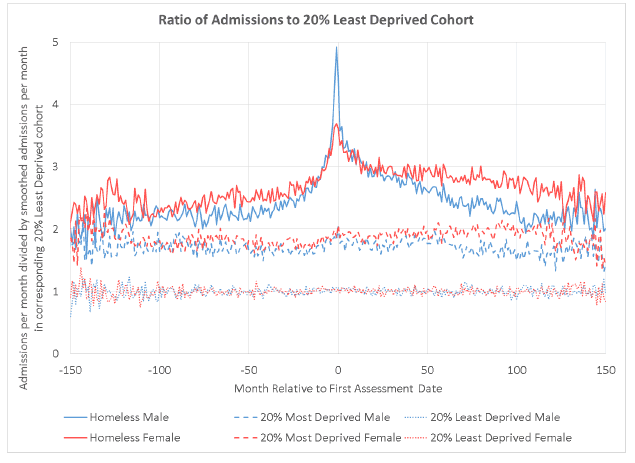
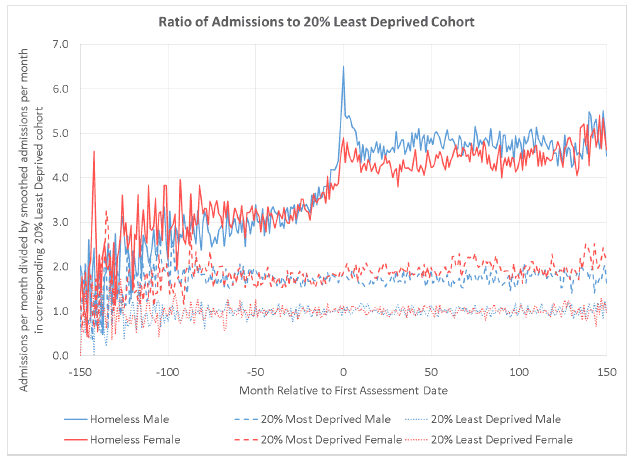
Figure 4.6: Ratio of admissions per month (relative to assessment date) for people with repeat homelessness assessments for each cohort to the admissions among the LDC by sex.
4.6 Reason for admission
For each acute admission record in this study there is an indication of whether it is related to: drugs, alcohol, mental health, injuries or poisonings, or respiratory diseases (as defined in Section 2.3.1). Acute admissions can have one or more of these indicators flagged and so the total of all admission reasons will exceed the total number of admissions. However, if an admission is not related to any of the above conditions, then the admission is labelled as an 'other condition' admission [39] .
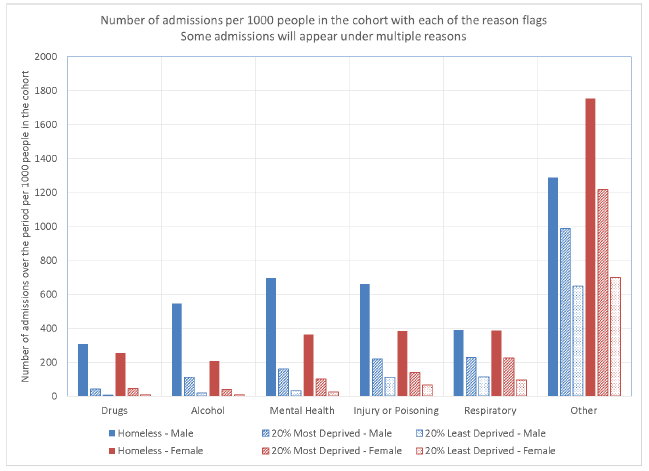
Figure 4.7 indicates the number of admissions that have each of these flags by sex and cohort per 1,000 people. For each indicator there is a higher admission rate among the EHCs than among the other cohorts. This is particularly pronounced for drugs, alcohol and mental-health related admissions. For all indicators apart from respiratory illness and other there is generally a higher admission rate among males than females.
Figure 4.7: Number of admissions per 1,000 people in the cohort with each of the reason flags by sex.
In order to analyse the ratios between the cohorts, and to look at the temporal analysis broken down by these reasons, we need to identify a set of admissions to include for each reason. This could be done in various ways ( Table 4.3).
The problems against options 1 and 2 listed in Table 4.3 are taken as reasons not to use these methods.
Therefore option 3 is used. This requires an ordering of the reason flags to be decided. To decide on an order of the hierarchy the two Option 3 alternatives are explored.
Table 4.3: Options for assigning admissions to reasons for the purpose of analysing ratios and temporal effects driven by these reasons, and problems associated with these.
| Option | Set of admissions | Problem |
|---|---|---|
| 1 | All admissions that include that flag | Effects observed (ratios and temporal effects) could be due to the other flags in cases where many admissions include other flags and the other reasons result in larger effects. This could particularly be the case for mental health, where only 17.7 per cent of the admissions with that flag do not include any other flags. |
| 2 | Only admissions that include the flag and no others | Can result in very few admissions in the set. For example there are over 145,000 admissions with the drugs flag, but only 75 of them have no other flags. In any case, these admissions could be associated with another condition not included in the five reasons provided for the study. It simply shows that any other reason is not included in the set of reasons captured for the study. So the purpose of this method (to isolate the effect of the specific reason for the admission) cannot be achieved using the study's data. |
| 3 | Categorization by hierarchy of reasons | A decision would be required whether to choose an order based on:
|
Firstly, the scale of the difference of the activity with that flag between the cohorts is considered. It would be preferable for the set of admissions considered for a particular reason to exclude admissions that also have a reason that exerts a large difference in activity between the cohorts. This is because they could have an impact on the results. The four ratios ( EHC : MDC and EHC : LDC for males and females) for admissions with each reason flag are shown in Table 4.4, ordered in general decreasing order of the size of the ratios.
Table 4.4: Number of admissions with each admission flag and the ratios of these numbers between the EHC and both the MDC and LDC, by sex.
| Admission flag | Male | Female | ||||
|---|---|---|---|---|---|---|
| Admissions | EHC : MDC | EHC : LDC | Admissions | EHC : MDC | EHC : LDC | |
| Drugs | 236,526 | 7.2 | 44.1 | 200,691 | 5.5 | 26.8 |
| Alcohol | 444,768 | 4.9 | 29.2 | 166,854 | 5.0 | 25.4 |
| Mental Health | 586,131 | 4.3 | 21.3 | 316,710 | 3.6 | 15.6 |
| Injury or Poisoning | 654,231 | 3.0 | 5.9 | 385,380 | 2.7 | 5.7 |
| Respiratory | 483,462 | 1.7 | 3.4 | 460,188 | 1.7 | 4.1 |
| Other | 1,927,794 | 1.3 | 2.0 | 2,381,913 | 1.4 | 2.5 |
Secondly, the number of admissions with only the particular flag is considered. This is to ensure that there are a reasonable number of admissions included. For example if drugs was last in the hierarchy then only 75 admissions would be included against this reason. This is because all the other admissions with the drugs flag also have another flag, and so these would then be counted against one of those reasons. Table 4.5 shows the number of admissions that have that flag and no other (the ones that would be counted against that reason if it was last in the hierarchy).
Table 4.5: Number of admissions with only one reason flag by reason.
| Reason | Admissions with only this flag | Percentage of all admissions |
|---|---|---|
| Drugs | 75 | 0.00 |
| Alcohol | 20,538 | 0.91 |
| Mental Health | 53,221 | 2.35 |
| Injury or Poisoning | 189,481 | 8.36 |
| Respiratory | 241,589 | 10.66 |
| Other | 1,436,569 | 63.39 |
| Total admissions with 1 flag | 1,941,473 | 85.67 |
Conveniently, these two alternatives result in the same ordering of the reasons. Therefore this hierarchy is adopted in the following analysis. This is summarized as below:
- Drugs: all admissions with the drugs flag
- Alcohol: all admissions with the alcohol flag, apart from those included above
- Mental Health: all admissions with the mental health flag, apart from those included above
- Injury or poisoning: all admissions with the injury or poisoning flag, apart from those included above
- Respiratory: all admissions with the respiratory flag, apart from those included above
Table 4.6: Percentage of admissions by combination of indicators present. Superscripted letters indicate the groupings of these combinations used in the remainder of this chapter: d for drugs, a alcohol, mh for mental health, ip for injury or poisoning, r for respiratory and no superscripted letter(s) for other.
| Mental Health | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| No | Yes | ||||||||
| Injury or Poisoning | Injury or Poisoning | ||||||||
| No | Yes | No | Yes | ||||||
| Respiratory | Respiratory | Respiratory | Respiratory | ||||||
| Drugs | Alcohol | No | Yes | No | Yes | No | Yes | No | Yes |
| No | No | 63.39 | 10.66 r | 8.36 ip | 0.49 ip | 2.35 mh | 1.07 mh | 0.24 mh | 0.04 mh |
| Yes | 0.91 a | 0.18 a | 0.16 a | 0.01 a | 3.61 a | 0.62 a | 1.37 a | 0.09 a | |
| Yes | No | 0.00 d | 0.00 d | 1.79 d | 0.10 d | 1.14 d | 0.37 d | 0.89 d | 0.09 d |
| Yes | 0.00 d | 0.00 d | 0.62 d | 0.03 d | 0.34 d | 0.06 d | 0.93 d | 0.05 d | |
Table 4.7: Percentage of all admissions by the category to which they have been assigned.
| Categorization | Percentage of admissions |
|---|---|
| Drugs | 6.4 |
| Alcohol | 7.0 |
| Mental Health | 3.7 |
| Injury or Poisoning | 8.9 |
| Respiratory | 10.7 |
| Other | 63.4 |
| Total | 100.0 |
As discussed above some admissions might be related to more than one factor. Table 4.6 shows the breakdown of admissions by combinations of these indicators, shaded by the categorization indicated in the previous section. Table 4.7 shows the total percentage of admissions in each category.
Having categorized all the admissions to particular reasons, the following analyses explore the differences between the cohorts within each category ( Figure 4.8 and Table 4.8).
Figure 4.8 is similar to Figure 4.7 but breaks down the admissions by the category to which they have been assigned, rather than indicating all the admissions with the corresponding indicator. It can be seen that there are now fewer mental-health admissions. This is because many mental-health admissions also include the drug or alcohol flags, and these will be categorized as drug or alcohol admissions. This is particularly the case among males, who tend to have more alcohol admissions, resulting in there now being more female mental health admissions than male ones. Injury or poisoning, and respiratory have also been affected, but to a lesser extent. The following points apply for both sexes:
The EHC have more acute admissions for each of the admission categories
Compared to the controls in the MDC or LDC, the ratio of admission is always greater than one (minimum ratio is: 1.3, EHC : MDC for males for other admissions, see Table 4.8).
Drugs and alcohol have the highest ratios
The EHC have more drugs and alcohol related admissions than their controls (the minimum EHC : MDC ratio is 4.5 and the minimum EHC : LDC ratio is 23). These differences are larger than the differences for any of the other admission reason categories.
The mental-health EHC : LDC ratios are notably larger than for all categories combined
For males the mental-health EHC : LDC ratio is 6.1 (compared with 3.1 across all admissions). For females the mental-health EHC : LDC ratio is 7.8 (compared with 3.1 across all admissions).
All other ratios are roughly similar to those of all categories combined
The EHC : MDC ratios for remaining categories for males - injury or poisoning, respiratory and other - range from 1.3 to 2.1 (compared with 1.8 across all admissions, for females the range is 1.4 to 2.0 compared with 1.7). The EHC : LDC ratios for remaining categories for males range from 2.0 to 3.5 (compared with 3.1 across all admissions, for females the range is 2.5 to 3.2 compared with 3.1).
Figure 4.8: Number of admissions per 1,000 people in the cohort by admission category by sex.
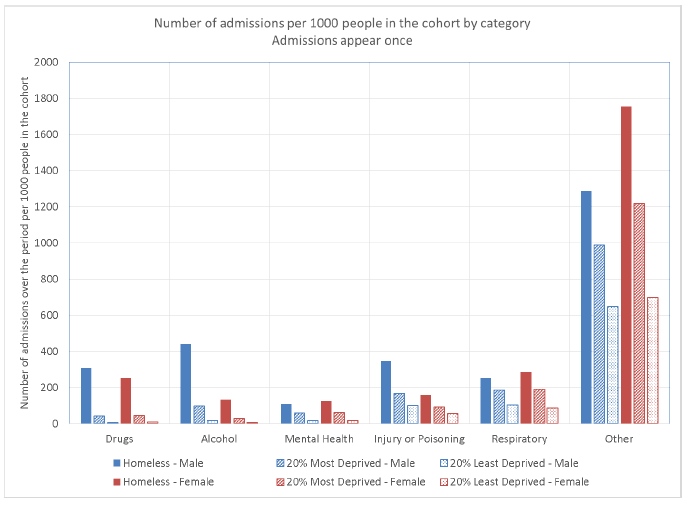
Table 4.8: Number of admissions by category and sex. Also shown are the ratios EHC : MDC and EHC : LDC by category and sex.
| Admission category | Male | Female | ||||
|---|---|---|---|---|---|---|
| Admissions | EHC : MDC | EHC : LDC | Admissions | EHC : MDC | EHC : LDC | |
| Drugs | 78,842 | 7.2 | 44.1 | 66,897 | 5.5 | 26.8 |
| Alcohol | 121,728 | 4.5 | 26.6 | 35,997 | 4.5 | 23.1 |
| Mental Health | 40,433 | 1.9 | 6.1 | 43,509 | 2.0 | 7.8 |
| Injury or Poisoning | 134,182 | 2.1 | 3.5 | 66,398 | 1.7 | 2.9 |
| Respiratory | 119,368 | 1.4 | 2.4 | 122,221 | 1.5 | 3.2 |
| Other | 642,598 | 1.3 | 2.0 | 793,971 | 1.4 | 2.5 |
| All | 1,137,151 | 1.8 | 3.1 | 1,128,993 | 1.7 | 3.1 |
4.7 Admissions relative to the date of first homelessness assessment by reason
In section 4.4 it was found using temporal analysis that admissions in the EHC relative to their controls peak around the time of first homelessness assessment. In section 4.6 it was found that the ratios vary across categories of admissions (based on the reason flags attached to each admission record). This section explores temporal analysis for each of the admission categories to explore how admissions in the different categories vary over time relative to the date of first homelessness assessment.
Figure 4.9: Ratio of admissions to that of the 20% least deprived cohort ( LDC), by sex, against the time difference(months) between the first assessment and the attendance date. There is one panel for each admission category.
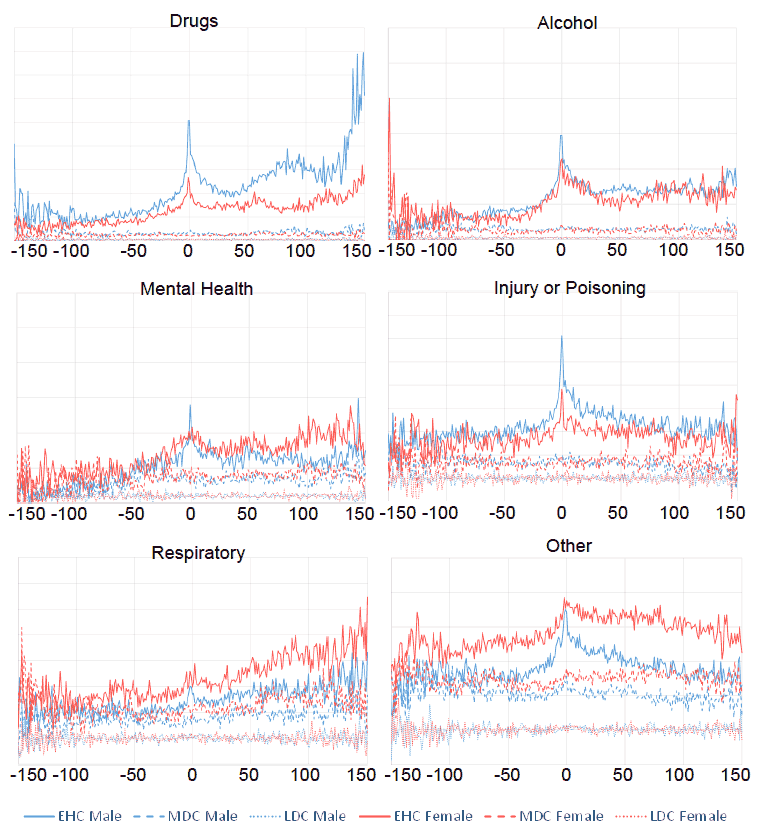
The shape of the graph for the EHC is markedly different from the MDC ( Figure 4.9). The following points apply for both sexes:
- The ratios increase in the years prior to first assessment for drugs, alcohol, mental health and to a lesser extent for other
- Peaks at time of first assessment are observed for drugs, alcohol and injury or poisoning, and also for the remaining categories for males
- Injury and poisoning, and male other ratios eventually return to the prior levels
- Respiratory ratios notably increase following the peak
In addition:
- There is an increased peak for drugs ten years after the first assessment, especially for males.
- Alcohol admissions stay constant but high for both males and females after the first homelessness assessment.
- Mental health admissions stay higher for females, more so than for males.
- Other admissions return to pre-first assessment levels, but this takes longer for females.
4.8 Summary
The EHC have more acute admissions than the control cohorts. This is true for each age and sex breakdown. The rate of admissions per 1,000 people increases steadily with age also, and this is true for each cohort. More of the EHC having at least one acute admission, and among those who do have acute admissions, the EHC have more multiple admissions. A higher proportion of acute admissions amongst the EHC included an overnight stay. Of those that stay one or more days, the length of stay for inpatients is similar between cohorts.
Among the EHC there is a relationship between the timing of acute admissions and that of the first homelessness episode, suggesting some relationship between these. There is a clear peak in acute admissions around the time of first homelessness assessment (particularly for males but with a less marked peak for females), with a rise leading to this, yet stabilising at a higher activity level afterwards. This is especially the case for those who have multiple homelessness episodes, with a high ratio and longer lasting peak ratio. For people who have only one homelessness assessment, the acute admissions ratio eventually returns to the level it was prior to the homelessness episode.
This chapter derives a flag to analyse acute admissions by reason for admission. Many of the admission types do not occur in isolation and a hierarchy of types is created. For each admission flag (drugs, alcohol, mental-health, injury or poisoning, respiratory, and other) the EHC has more, with drugs and alcohol having the highest ratios.
It is clear that there is evidence to support each of the four research questions:
- A gradually worsening health condition prior to the date of first assessment (as observed with increasing acute admissions prior) that results in excess acute admissions, occurs prior to homelessness, particularly for drugs, alcohol, mental health and to a lesser extent for other admission types.
- Also for some people the (first) homelessness episode is associated with some crisis with a health activity component, as observed by an acute admission peak around that time. Peaks are observed for drugs, alcohol and injury or poisoning, and also for the remaining categories for males.
- Ratios after the first assessment notably increase following the peak for respiratory admissions, and for people with repeat homeless assessments. Injury and poisoning, and male other ratios eventually return to the prior levels.
- Even several years prior to their first homeless assessment, the EHC ratios are higher. This could be a result of the EHC having an even higher proportion of individuals than the MDC who are affected by factors associated with deprivation.