Health and homelessness in Scotland: research
Study exploring the relationship between homelessness and health.
Executive Summary
Whilst health inequalities across Scotland are well evidenced, this study links homelessness and health datasets for the first time at a national level, to explore the relationship between homelessness and health in Scotland.
Study design
This study considered 435,853 people who had been in households assessed as homeless or threatened with homelessness between June 2001 and November 2016. These households had been assessed by Scottish Local Authorities under section 28 of the Housing (Scotland) Act 1987. These people formed the Ever Homeless Cohort ( EHC).
Each person in the EHC was matched on age and sex to a non-homeless individual from the 20% least deprived areas of Scotland, and a non-homeless individual from the 20% most deprived areas of Scotland. This formed two control cohorts - the Least Deprived Cohort ( LDC) and the Most Deprived Cohort ( MDC). Each cohort had the same number of people and the same age–sex distribution. In total, the study contained over 1.3 million people.
Key findings
- At least 8% of the Scottish population (as at 30 June 2015) had experienced homelessness at some point in their lives.
- Of those who had experienced homelessness at some point:
- over half (51%) had no evidence of health conditions relating to drugs, alcohol or mental health. This was much lower than in the control groups ( MDC 74%, LDC 86%).
- Around 30% had evidence of a mental health problem at some point during the study period (with no evidence of drug or alcohol-related conditions at any point). This was higher than in the control groups ( MDC 21%, LDC 13%).
- There was evidence of drug and/or alcohol-related interactions for the remaining fifth of people (19%), higher than in the control groups ( MDC 5.1%, LDC 1.2%). Of these, the vast majority (94%) also had evidence of mental health issues.
- In particular, around 6% of people experiencing homelessness had evidence of all three of the following conditions – a mental health condition, a drug-related condition and an alcohol-related condition – although not necessarily at the same time. This was much higher than in the control groups ( MDC 1%, LDC 0.2%). The figure was markedly higher for those experiencing repeat homelessness (11.4%).
- Increased interactions with health services preceded people becoming homeless.
- A peak in interactions with health services was seen around the time of the first homelessness assessment.
The study contained six health datasets from NHS National Service Scotland covering Accident and Emergency attendances (A&E2), Inpatient admissions ( SMR01), Outpatient appointments ( SMR00), Prescriptions ( PIS), the Scottish Drugs Misuse Database ( SDMD) and Mental Health admissions ( SMR04), together with information about deaths from National Records of Scotland.
There was a particular focus on mental-health, drug-related health conditions and alcohol-related health conditions. Comparisons of interactions with health services (hereafter referred to as “health activity”) between these cohorts were made by looking at the number of times people appeared in these various datasets.
Findings
Homelessness affects a sizable minority of people in Scotland (at least 8% of the population as at 30 June 2015 had experienced homelessness at some point in their lives). This is an under-estimate as the homeless assessments in the study only covered around three quarters of all Scottish homelessness assessments for the study period.
Of the EHC people, 29% of males and 26% of females had been in households assessed as homeless on multiple occasions during the study period. Following their first homelessness assessment, people included in the EHC cumulatively spent 9.7% of their time for males (9.2% for females) in open homelessness cases, before local authorities had discharged their duties under the homelessness legislation.
The EHC people tended to be younger than the Scottish population. The proportion of people in the EHC at around 20–30 years was higher for females than for males.
Health Service Activity
- The Ever Homeless Cohort ( EHC) accounted for 1.16 million (or 55%) of Accident and Emergency Attendances, out of a study total of 2.12 million. The EHC rate of attendances was almost twice (i.e. 1.9) as high as the Most Deprived Cohort ( MDC) and three and a half ( i.e. 3.5) times higher than the Least Deprived Cohort ( LDC).
- Similarly, the EHC accounted for 1.19 million (or 52%) of Acute Hospital Admissions, out of a study total of 2.27 million. The EHC rate was 1.7 times greater than the MDC and 3.1 greater than the LDC.
- There were 9.01 million Outpatient Appointments over the study period with 4.40 million (or 49%) by people in the EHC. The rate was 1.6 and 2.3 times higher than the MDC and LDC cohorts respectively.
- The EHC accounted for 6.23 million (or 66%) of the 9.49 million Dispensed Prescriptions, with a rate 2.5 times higher than the MDC and 8.2 higher than the LDC. The differences in rates was much more pronounced for Alcohol related (3.9 and 23.5 times higher respectively) and Opioid related (6.4 and 169 times higher respectively) prescriptions.
- There were around 100,000 Admissions to Mental Health Specialities over the study period, with 80,000 (80%) by people in the EHC. The rate was 4.9 times greater than the MDC and 20.5 times greater than the LDC.
- The EHC accounted for 80,761 (90%) of Initial Assessments at Drug Treatment Services over the study period, which was 10 times higher than the MDC and 132 times higher than the LDC.
Interactions with Health Services Over Time
The study showed increased interactions with health services preceded people becoming homeless and that a peak in interactions was seen around the time of the first homelessness assessment. Some health service interactions remained at a higher level following the first homelessness assessment, whereas others returned to previous levels. The four charts in this summary (repeated from the charts in Chapter 11) illustrate these findings where health service activity for the Ever Homeless Cohort ( EHC) is shown relative to the health service activity of the Least Deprived Cohort ( LDC).
- Figure 11.1a for males (with a higher scale) shows some activity remains higher after the first homelessness assessment date, particularly for drug-related and alcohol-related acute admissions, and for repeat homeless people - mental health admissions ( SMR04) and mental health prescriptions.
- Figure 11.1b for males (with a lower scale) shows some activity remains higher after the first homelessness assessment date, particularly for mental health acute admissions ( SMR01), mental health prescriptions and A&E attendances by repeat homeless persons.
- Figure 11.2a for females (with a higher scale) shows some activity remains higher after the first homelessness assessment date, particularly for drug-related and alcohol-related acute admissions, and for repeat homeless people - mental health admissions ( SMR04) and mental health prescriptions.
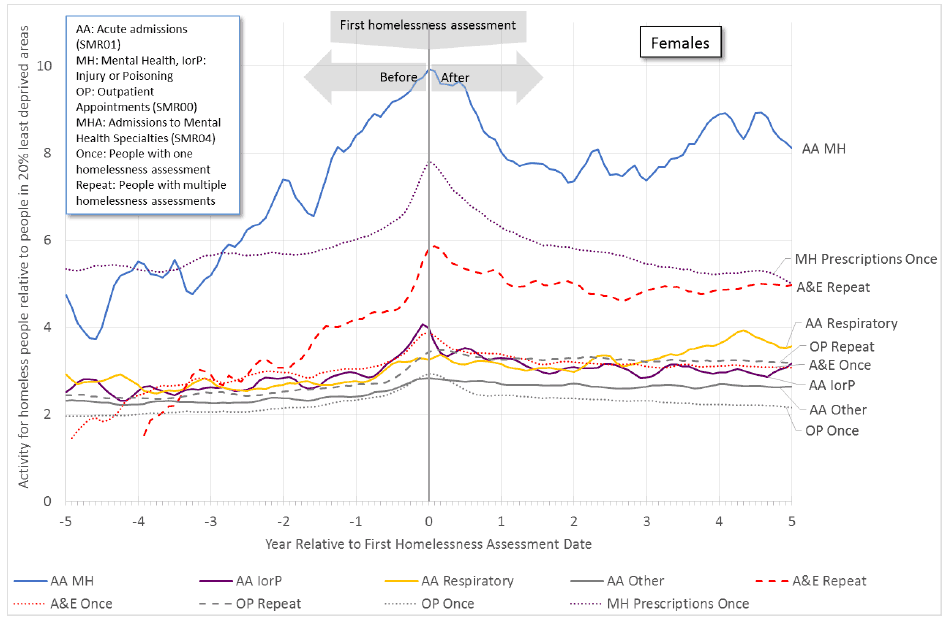
- Figure 11.2b for females (with a lower scale) shows some activity remains higher after this date, particularly for mental health acute admissions ( SMR01), mental health prescriptions and A&E attendances by repeat homeless persons.
From these charts, the following observations can be made:
Increased interactions with health services preceded people becoming homeless
It was found that health activity increases in the years prior to the homelessness assessment date for people in the EHC, indicating a relationship. The relationship is most clearly seen for health activity that relates to mental health, drugs and alcohol. These issues are likely to be risk factors for homelessness.
A peak in interactions with health services was seen around the time of the first homelessness assessment.
This suggests a relationship between becoming homeless and health activity. This is particularly (although not exclusively) associated with activity related to drugs, alcohol and mental health. Preventing homelessness could reduce health activity, and improve health outcomes.
Higher levels of interactions with health services followed the first homelessness assessment for people experiencing repeat homelessness.
For those who had been homeless on only one occasion health activity eventually returned to the (albeit higher) pre-homelessness levels. However, for people who were homeless on multiple occasions, levels of health activity remained high. It is not possible to say that health activity following homelessness is the direct consequence of homelessness itself. It could be due to a further crises or health problems such as drug or alcohol related conditions, or a mental health condition.
For males in the EHC, mortality was around a third higher during periods of homelessness than during periods when they were not in open homelessness cases. This difference may be driven by the higher number of drug-related deaths amongst males that had been homeless on multiple occasions.
Health, homelessness, and area-based deprivation
Homeless people are more likely to come from deprived areas, based on their last settled address. The distribution of homeless people across the area-based deprivation spectrum (as measured by the Scottish Index of Multiple Deprivation) closely follows the distribution of income and employment deprived people.
The health activity of people in the EHC was consistently higher than for the non-homeless controls in the 20% most deprived areas ( MDC). In turn, this was consistently higher than the non-homeless controls in the 20% least deprived areas ( LDC).
Health inequalities are known to exist across Scotland and they are monitored using area-based measures of deprivation. Using health activity as an imperfect proxy for poor health, the study provides evidence that health inequalities are likely to exist between people that have experienced homelessness and those who have not.
Deaths
- Of the 23,718 Deaths recorded over the study period, 14,186 (60%) were in the EHC, with a death rate 2.1 times higher than the MDC and 5.3 times higher than in the LDC.
Differences in mortality between the study cohorts varied by cause of death, although for each cause mortality among the EHC was at least as high as for the controls. The differences were highest for drugs, alcohol, intentional self-harm, and assault. This results in the main causes of death among the EHC being: drugs, heart disease & strokes, and, for males, alcohol and, for females, cancer. Differences in mortality due to drug-related conditions between the EHC and the controls were higher for people who have multiple homelessness assessments during the study period.
Overlap of drugs, alcohol or mental health issues
The majority of the EHC had no evidence of mental-health, drugs or alcohol related issues during the study (51%). This is lower than for both control cohorts ( MDC 74%, LDC 86%).
Just under a third of the EHC (30%) had evidence of a mental health issue which excluded drug- or alcohol-related issues. This was higher than in the control groups ( MDC 21%, LDC 13%).
There was evidence of drug and/or alcohol-related interactions for the remaining fifth of people (19%) in the EHC. Of these, the vast majority (94%) also had evidence of mental health issues. The proportion of people with all three conditions – mental-health, drugs or alcohol related issues - was higher among the EHC (5.9%) than in the MDC (1.0%) or the LDC (0.2%). This proportion was also much higher among people with multiple homelessness assessments (11.4% compared with 3.8% for once-only homeless). This difference cannot be explained by the younger age profile amongst the repeat homeless cohort, suggesting a relationship between repeat homelessness and drug, alcohol and mental health issues.
Figure 11.1a: An increase in health activity precedes the first homelessness assessment for males. Some activity remains higher after this date, particularly for drug-related and alcohol-related acute admissions, and for repeat homeless people - mental health admissions ( SMR04) and mental health prescriptions.
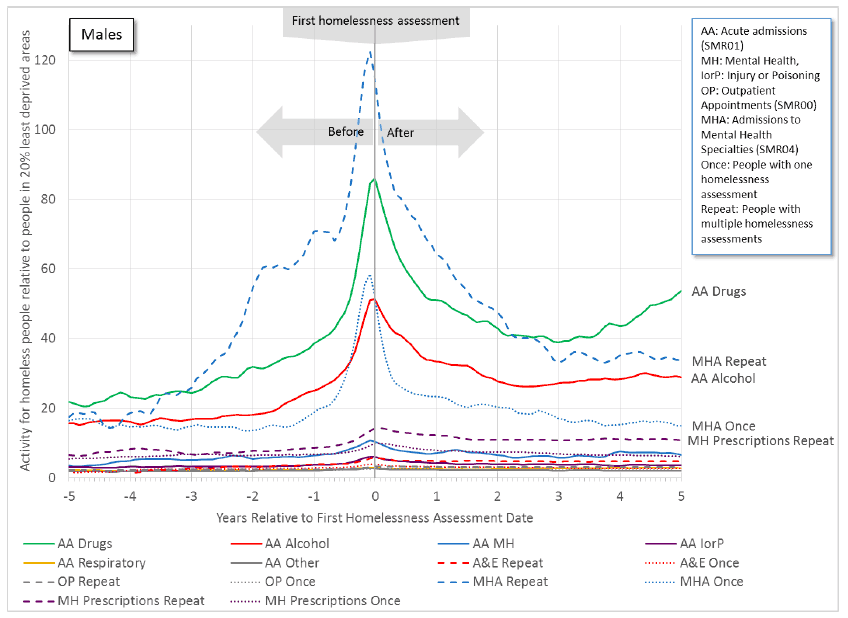
Figure 11.1b: An increase in health activity precedes the first homelessness assessment for males. Some activity remains higher after this date, particularly for mental health acute admissions ( SMR01), mental health prescriptions and A&E attendances by repeat homeless persons.
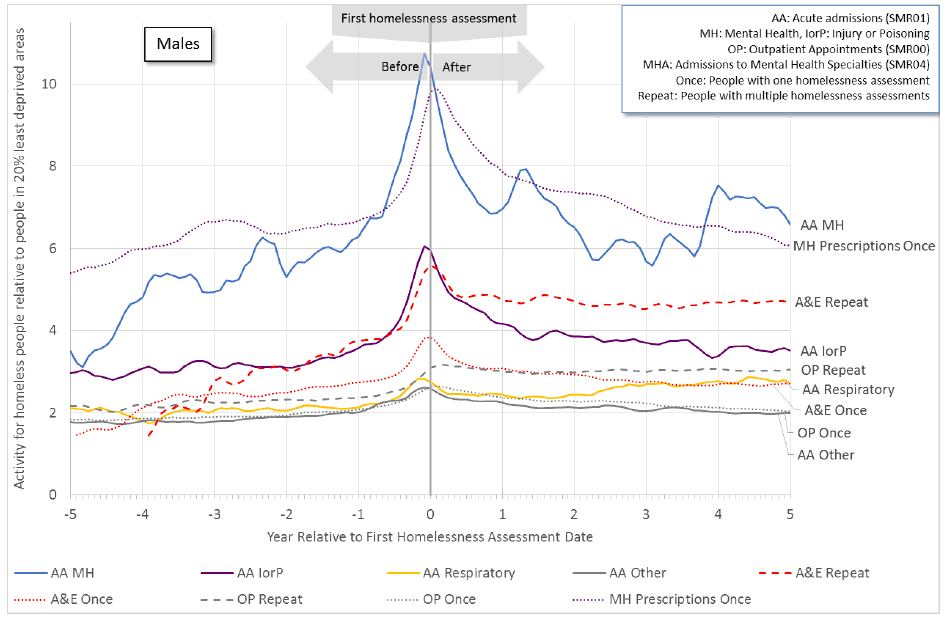
Figure 11.2a: An increase in health activity precedes the first homelessness assessment for females. Some activity remains higher after this date, particularly for drug-related and alcohol-related acute admissions, and for repeat homeless people - mental health admissions ( SMR04) and mental health prescriptions.
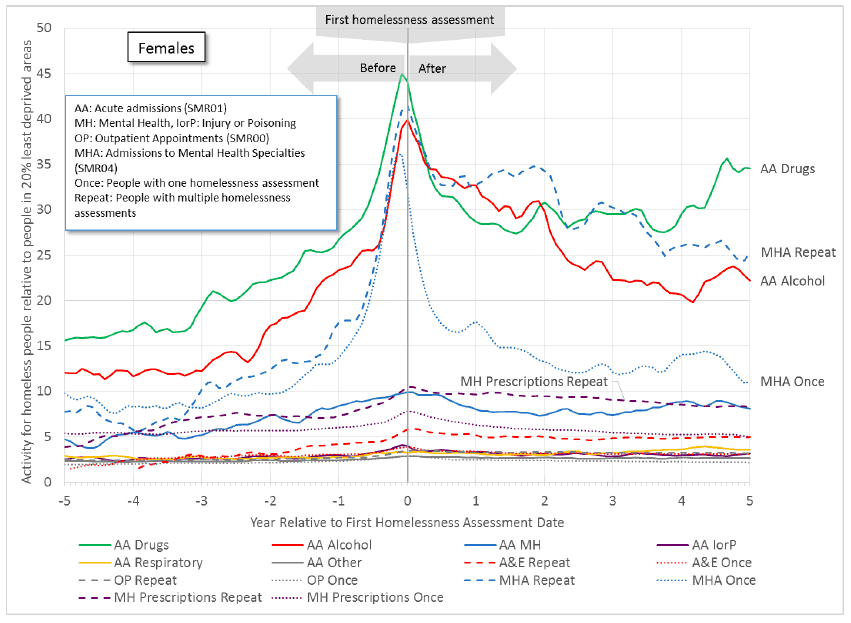
Figure 11.2b: An increase in health activity precedes the first homelessness assessment for females. Some activity remains higher after this date, particularly for mental health acute admissions ( SMR01) and A&E attendances by repeat homeless persons.