Gender identity healthcare: evaluation of the impact of Scottish Government funding
This report presents findings of an independent evaluation into the impact of Scottish Government funding, as allocated to NHS Health Boards, to implement local work to improve access to, and delivery of, gender identity services. The evaluation covers period between December 2022 and August 2024.
7. NHS Grampian - Adult Services
7.1 Overview of the clinic
The NHS Grampian Gender Identity Clinic (GIC) is based in Mental Health Services at the Royal Cornhill Hospital in Aberdeen. The GIC provides adult gender identity services to patients living in the Grampian, Orkney and Shetland NHS Board areas.
Current staff mix
As of August 2024, the core staff of the NHS Grampian GIC comprises:
- two consultant psychiatrists (each providing 1 session per week)
- a psychologist (0.2 WTE, band 8a, currently on secondment)
- a psychologist (0.1 WTE, band 8a, currently on secondment)
- a gender identity nurse practitioner (1 WTE, band 7)
- a medical secretary (1 WTE, band 4)
- a service manager (who is also manager for the Mental Health unit)[99]
In total, therefore, the Grampian GIC Adult Services draw on the equivalent of 2.3 WTE staff, as of August 2024.[100] In addition to core staff, the clinic receives support from Psychology at NHS Grampian, and service delivery input from other NHS Grampian teams, including two endocrinologists and a speech and language therapist.
Service History
The GIC has always been based within Mental Health Services at Grampian, and there are reports from interviewees that the service has run very well in the past. However, interviewees also shared that there have been periods when the clinic was temporarily paused to new outpatient appointments to progress governance arrangements. Such periods of reduced service occurred during this period of evaluation work.
Previously, the Grampian GIC was inactive during 2017-18, after key staff members - including the original consultant psychiatrist and consultant psychologist - retired. At that time, “there was an explosion of referrals” to the GIC, according to one staff member in an interview, and a new local consultant psychiatrist, clinical psychologist and administrator were brought into the service, funded by NHS Grampian.[101] This team provided initial assessments and treatment, as well as first and second opinions for hormone treatment, while referring second opinions for surgery to the Sandyford GIC. After key staff departed in 2020, NHS Grampian hired new staff in 2021, including a psychiatrist and a clinical psychologist, who became clinical lead. The team worked on seeing patients, reducing the waiting list, and providing training to staff; they also submitted an application for SG improvement funding.
The Grampian GIC was successful in winning SG funding for its proposal (see below). However, in November 2022, the clinical lead left the service, and a recruitment process was launched to hire three new psychologists. According to one staff member, the Grampian GIC had initial difficulties in recruiting a senior psychologist to the team (a situation common to other gender identity services in Scotland - see other case studies). However, in late 2023, the GIC successfully recruited new staff to the GIC as per its redesigned workforce structure, including a gender identity nurse practitioner and two psychologists on secondments who came into post in early 2024.
During this period of reduced service capacity, the GIC continued to advertise a Band 8C Psychologist role, to provide supervision, leadership and training. Within the gender identity service, the two existing consultant psychiatrists continued to see previously referred patients and a limited number of new patients during this period. The GIC provided first assessments and psychiatry follow-up appointments, though the team were unable to provide psychology second opinion during this period. The newly recruited team worked on updating the governance processes and clinical procedures to enable the GIC’s resumption of full service in August 2024.
However, there was a delay in receiving the SG funding allocation confirmation for 2024-25 and, in addition, the GIC did not have access to all of the previous years’ SG improvement funding underspend. In a progress report to the SG in June 2024, NHS Grampian confirmed that, as of 31 March 2024, it had only spent £89,000 of the £328,000 allocated for gender identity healthcare improvement work, leaving an underspend of £239,000 against the allocated funding (these figures preceded the allocation of the third tranche of funding, £181,000, for the period 2024-25). NHS Grampian further confirmed that the underspend of £239,000 during 2022-24 had not been earmarked by the Health Board for work to improve gender identity healthcare, but was instead used by NHS Grampian against the wider Health Board deficit that was unrelated to gender identity healthcare.
7.2 Scottish Government Funding Proposal
NHS Grampian submitted a proposal for SG improvement funding to expand the gender identity service through a multidisciplinary approach, and to improve resilience within the GIC, with the aims of improving care and addressing waiting times. The total amount of funding applied for by NHS Grampian was £319,713 for 2022-23, with indicative spend for 2023-24 and 2024-25 calculated in the proposal as being £609,400 for both years should the model be established.
The NHS Grampian bid proposed to establish a new service delivery model for the GIC consisting of a psychosocial pathway, an ancillary healthcare needs pathway and a medical pathway, with SG funding to be used to develop a larger MDT team to provide these pathways. Specific posts identified for recruitment were: a clinical lead, consultant psychiatrist, psychologists, clinical nurse specialists, endocrinologist, occupational therapist, speech and language therapist, sexual health doctor, dermatology nurse, counsellors (outsourced) and Four Pillars support posts.
The aim of the improvement funding, as one staff member described it in an interview, was to “use the funding to create a sustainable kind of well-governed service that involved both sufficient clinical staff, including the psychological assessment side of it, but also the medical side of it.” Other aims of the proposal included providing clearer information to patients, reducing waiting times, and providing additional support for people on waiting lists from the third sector. Especially on the latter point, the funding bid included a proposal to work closely with Four Pillars, an LGBT+ organisation based in Grampian, to provide social transition support, peer support and wrap-around support for those on waiting lists.
After submitting the proposal, NHS Grampian received £207,000 from the SG in December 2022 to support work in 2022-23; it received £121,000 to support work in 2023-24; and it received £181,007 in 2024-25. The total funding allocation for NHS Grampian for the three-year period of funding 2022-25 was therefore £509,007. However, as described above, not all of the SG improvement funding allocated to NHS Grampian has been spent on supporting gender identity healthcare services, due to the Board’s decision to use an underspend of £239,000 against the wider Board deficit.
At that time, interviewees informed us that a reduced service was being provided by the GIC as it was awaiting confirmation of the third tranche of SG funding for 2024-25. Consultant psychiatrists continued to see patients and a recruitment process was underway for new psychology posts. Staff explained in interviews that, once the SG funding for 2024-25 was received, they planned to hire an external clinical lead and expand the service to realise the full service plan. Senior staff from Psychology were brought in to support the GIC and put in place new structures and staff hires in advance of fully resuming the service in August 2024. According to one staff member, who was interviewed prior to the resumption of full service, “the service has been at a bit of a standstill and then all the funding issues came in…previously the Board would have absorbed these things.” However, there has been significant financial pressures on Health Boards across Scotland. NHS Grampian’s Interim CEO has spoken of a budget deficit and the need to make £77 million in cuts in 2024-25.[102] As described above, some of the SG funding underspend has been used to address this budget deficit.
The GIC confirmed that, after the new SG funding allocation for 2024-25 was received in June 2024, it was able to hire external clinical psychology supervision (with a view to hiring a senior clinical lead in the long-term). From August 2024, staff at the GIC confirmed that it was able to secure external supervision and resume full service.
7.3 Mapping the System
NHS Grampian’s GIC works with a range of teams to deliver gender identity services. These include NHS secondary teams and external organisations:
NHS Secondary Teams:
- Endocrine Service; Maxillofacial Surgery; Gynaecology; Plastics; Dermatology; Speech and Language Therapy; Public Health, Health Improvement Team.
External Organisations:
- Four Pillars (third sector organisation), Wig Prescription Services
Patient Referrals:
- Referrals from General Practitioners (GPs) and from Child Services (for the transfer of patients transitioning from paediatric care to adult care)
The clinic makes formal referrals to services provided by the NHS Secondary teams and external organisations listed above.
These partnerships are viewed as crucial in enabling the GIC to provide comprehensive and coordinated care for their patients. These relationships are mapped below.
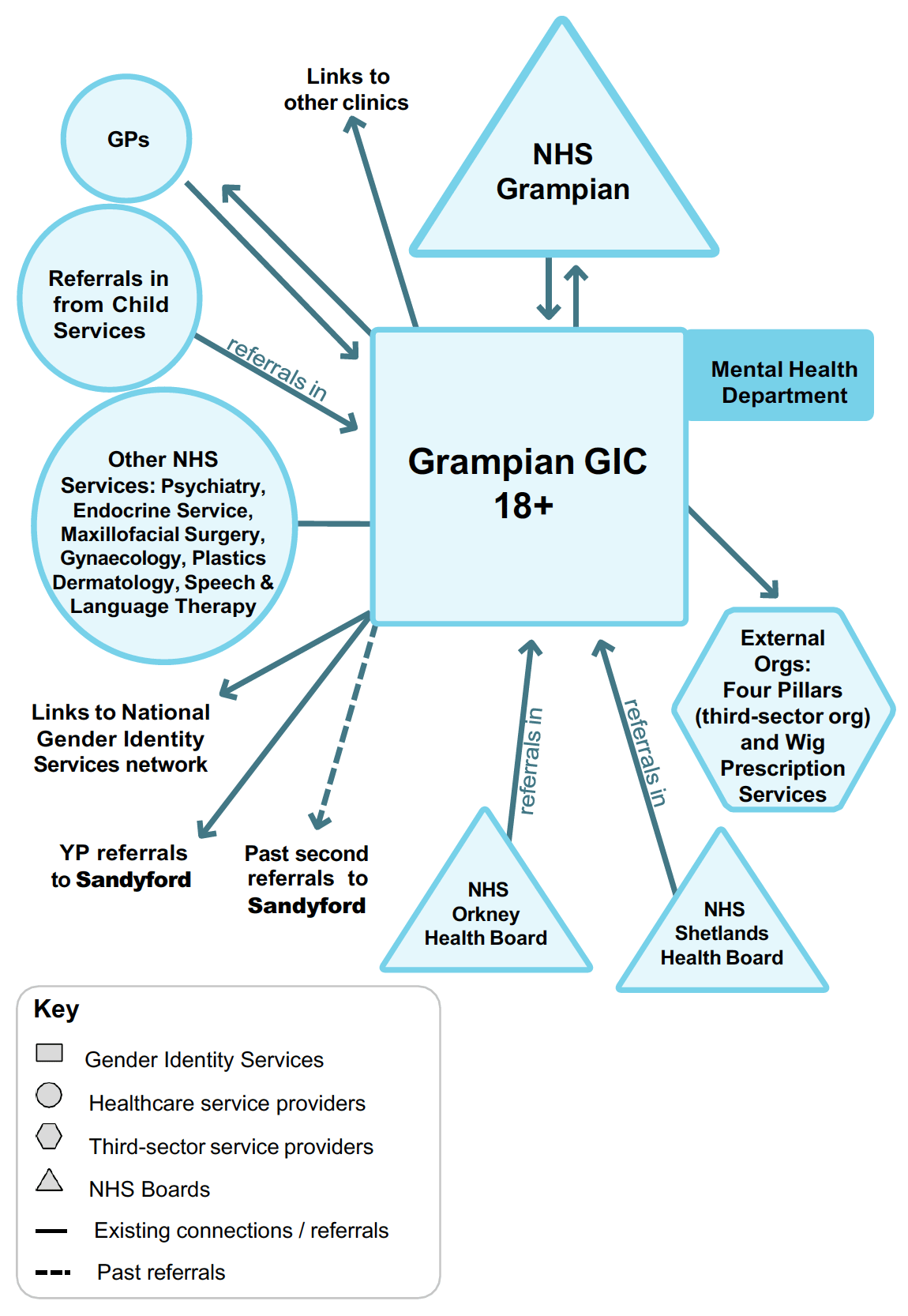
As the map shows, the Grampian GIC has developed numerous links across the Health Board to deliver gender identity services. Notably, the GIC historically has strong links with Endocrinology, Psychiatry and Speech and Language Therapy at NHS Grampian. Members of staff from the GIC confirmed in interviews that they have met with infertility specialists, but do not yet have strong links into Sexual Health. The GIC receives referrals from GPs and Child Services (for patients transitioning from paediatric to adult care), and makes referrals to NHS secondary teams. There are two other Health Boards referring to the Grampian GIC: NHS Orkney and NHS Shetland. Finally, the GIC has developed connections with the LGBTQIA+ organisation Four Pillars.
7.4 Services being delivered
The NHS Grampian GIC offers a range of gender identity healthcare services to patients. These include initial reviews (with the nurse practitioner or psychologists), first and second psychological assessments for those presenting with gender dysphoria, and onward referrals for gender-affirming care where appropriate, such as endocrinology treatment, speech and language therapy, fertility treatments, hair removal, and referrals for surgery (where required). The GIC holds monthly operational team meetings to discuss clinical and operational issues within the service, to implement improvements based on service user input. The team is also planning to initiate monthly MDT meetings. NHS Grampian’s Gender Identity Care pathway is currently under review, however the pathway currently includes the following stages:
- Initial Assessment and Diagnosis: Conducted by a psychologist or psychiatrist to assess and diagnose gender incongruence.
- Discharge or Onward Referral: Following the initial assessment, patients may be discharged or referred to other services as appropriate.
- One-Year Review: A follow-up review is conducted by any clinician one year after the initial assessment, followed by onward referral if necessary.
- Second Opinion: A second opinion is sought from a psychologist or psychiatrist, depending on the case. Patients requiring a second diagnostic opinion are placed on a dedicated waiting list and another clinician, either a psychologist or psychiatrist, will conduct the second assessment.
- Subsequent Reviews: To be scheduled based on the needs of the patient.
To record, manage and report data to deliver services and allocate resources, the GIC collects and manages patient data through the TrakCare PMS system, where all patient information is recorded. Additionally, the clinic utilises Datix and Tableau Illuminate to generate reports that inform their service delivery and resource allocation.
As of August 2024, NHS Grampian was serving 377 returning patients, with 368 patients on the waiting list.[103] The management of waiting lists involves several steps:
- Validation: The clinic regularly validates its waiting lists to ensure that patient information is accurate and current. This includes confirming that all details are correctly recorded and that patients are categorised appropriately based on their specific needs and the services required.
- Reporting: The clinic produces and reviews regular reports on waiting list metrics using their data management systems (see below). These reports include details on patient numbers, waiting times, and demand for services. The information helps staff monitor performance, identify trends, and make informed decisions to improve service delivery.
- Clinical Triaging: Referrals from GPs are triaged by the Consultant. All patients are treated with the same level of urgency.
During the period that the NHS Grampian GIC was operating a reduced service to enable the development of governance, systems and processes whilst new staff were starting in post (prior to August 2024), staff shared in interviews that they were focused on service planning.[104] A key task of the team was to implement service redesign, including building up linkages across teams within NHS Grampian and developing internal processes. These included creating systems for keeping in contact with people on waiting lists, systems for triaging patients, and processes for deciding which staff member is doing what, i.e. “working out what assessments need to be done by psychologists, psychiatrists and what can be done by the nurse.” Staff also focused on patient communications, by updating patient details and developing resources to support people on waiting lists. This included a ‘Waiting Well’ resource pack for service users, which provided information on local support services and charities, and guidance on what to expect and prepare for people’s first appointment.
The GIC also initiated discussions with the Health Point and the Public Health Waiting Well service to explore how they could assist in contacting patients and offering further support services. Furthermore, the GIC plans to measure patient satisfaction through a number of channels, including Care Opinion, a platform where patients can share their experiences and feedback, and the Complaints/Feedback Service, which collects and addresses complaints and feedback from patients and staff.
7.5 Partnership working and cross-clinic links
The GIC team has been active in building links with other clinics across Scotland, to learn about service delivery processes and protocols in other places. Many staff have shared in interviews that these linkages to other clinics have been invaluable in helping them with their own service planning: “I think having that establishment with the other Health Boards [across Scotland] will be a real benefit to us.”
While cross-clinic links have been considered valuable to Grampian GIC staff, especially with a view to implementing the redesigned service plan, it has also engendered a feeling, for one interviewee, that “the setups are all different.” The biggest difference being that other GICs are based in Sexual Health, while at Grampian it is based in Mental Health. Despite these differences, staff have found other clinics to be “very welcoming” and GIC staff have also attended SG meetings, consultation meetings and cross-clinic training opportunities to stay informed about advancements.
In addition to learning from other clinics, GIC staff have been in discussions with Four Pillars, a local LGBTQ+ third sector organisation offering a range of services to the community, about offering wrap-around services for people on waiting lists:
“Right now we're currently sitting with a 3 year waiting list. There will be a lot of our patients who will benefit from the services that Four Pillars can offer them. So we would like to do more of a referral service for those on the waiting list, and then have Four Pillars work with them … ensuring that they've got all the right documentation, and providing advice on name changes and getting a CHI number changed.”
7.6 Training and Education
All of the Grampian GIC staff interviewed highlighted the importance of training and supervision to ensure that the service ran effectively. In the past, the GIC offered training sessions to other organisations and service providers. This ranged from specialist training for GPs around hormone prescribing, to general sessions for NHS staff on ‘what is trans, in a very broad information-giving way.’ The new team is in a different position, in that some staff do not have extensive prior experience in gender identity healthcare, and one staff member said it had been “a sharp learning curve.”
In tandem with training, staff have emphasised the importance of clear supervision. As one interviewee said, “supervision is vital for my role. That’s something I need in this area, because there can be a lot of complex presentations where it’s not quite clear what exactly is going on, and it would be really useful just to have that space to be able to chat and think about what might be going on, and how can I explore things further.” Training is also crucial to career development, with interviewees sharing that this would be important in their journey of taking on supervisory roles in the future. The GIC has since confirmed, as of August 2024, that staff are now receiving specialised training and supervision from an external clinician who is an expert in the area of gender identity healthcare. This training will help to ensure that staff are equipped to provide high-quality care to their service users.
7.7 Impacts of the Funding on Service Delivery
As the GIC was unable to access all of the SG improvement funding it received for 2022-23 and 2023-24 as a result of financial decisions by NHS Grampian Health Board to use earmarked funds (i.e. underspend) on reducing the Board’s overall budget deficit, the service had been reduced for much of the period of this evaluation. The SG confirmation of funding for 2024-25 did not arrive until June 2024, which added further delays to fully resuming all of the GIC services. NHS Grampian staff confirmed that, following receipt of the confirmation of SG funding for 2024-25, as of August 2024 the GIC has expanded its services to realise its full service plan and external supervision has been put in place. Nevertheless, the temporarily reduced services provided by the GIC during the period of this evaluation project had made it difficult to fully assess the impact of SG funding on service delivery over the whole period.
In August 2024, after the new funding allocation from the SG for 2024-25 was received, GIC staff confirmed that service delivery was progressing and staff capacity and development had been strengthened:
“With our funding allocation now secured, we have made significant progress in implementing and developing our pathway. Training and supervision for our new psychologists and nurse specialist has commenced, enabling them to begin seeing patients and advancing them through our pathway. However, we acknowledge that there is still considerable work to be done to fully realise the service’s potential.”[105]
Importantly, the Grampian GIC has been able to secure external clinical supervision for psychology and nursing staff working in the clinic as a result of the SG funding, enabling NHS Grampian to increase clinic capacity and fully implement its new service delivery model. This is part of a longer-term plan to hire a gender specialist clinical lead directly into the team, the recruitment period for which may take 6+ months.
7.8 Impacts of Funding on Patient Outcomes
As the GIC service was reduced for the majority of the period of this evaluation project, it is difficult to evaluate the impact of SG funding on patient outcomes. However, we can draw on some data to understand patient outcomes generally during this period.
Waiting Lists and Patient Numbers
Official statistics in development reported by Public Health Scotland (PHS) found that, as of 31 March 2024, there were 335 people waiting for an initial outpatient consultation at NHS Grampian adult gender identity services[106] The number of people waiting had increased by 30% between 30 June 2023 and 31 March 2024. During this period, NHS Grampian adult gender services had received 120 new referrals for outpatient appointments. As of August 2024, the Grampian GIC was serving 377 returning patients, and the number of people on the waitlist stood at 368.[107]
Service User Impacts
In July-August 2024, a survey was sent to users of gender identity healthcare services across Scotland, to enquire about their experiences. It comprised a mix of open and closed questions. The survey received 74 responses. A total of 10 of 74 respondents to the service user survey indicated that they were either currently accessing, on a waiting list, or had in the past accessed services at NHS Grampian GIC. Half of these respondents (5) were currently on a waiting list, while four respondents were currently accessing services and one had accessed the GIC’s services in the past. Table 5 below provides a summary of these individuals’ responses to the survey.
Table 5: Summary of survey responses amongst those who have accessed, are currently accessing, or are on a waiting list to access services at NHS Grampian GIC[108]
|
Current status |
No. |
% |
|---|---|---|
|
Currently accessing services |
4 |
40 |
|
On a waiting list |
5 |
50 |
|
Have accessed services in the past |
1 |
10 |
|
Total |
10 |
100 |
|
Has your overall experience with your GIC been a positive or a negative one? |
No. |
% |
|
Positive |
1 |
10 |
|
Negative |
5 |
50 |
|
Neither positive or negative |
4 |
40 |
|
Total |
10 |
100 |
|
Since the allocation of additional SG funding (from Dec 2022), have you noticed any changes in how gender identity services are delivered in your area? |
No. |
% |
|
Yes |
2 |
20 |
|
No |
4 |
40 |
|
Don’t know |
4 |
40 |
|
Total |
10 |
100 |
|
If you are being seen by a GIC, do you feel that you have a say over the gender identity care you are receiving? |
No. |
% |
|
Yes |
3 |
30 |
|
No |
1 |
10 |
|
Don’t know |
5 |
50 |
|
Would rather not say |
1 |
10 |
|
Total |
10 |
100 |
Overall, half of the respondents who had accessed, were currently accessing, or on a waiting list to access services at Grampian GIC said that their overall experience with the GIC had been a negative one, while one respondent said it had been positive and four said it had been neither positive or negative. Amongst those currently on the waiting list, negative aspects of the experiences described by respondents included very lengthy waiting times, a perception that the GIC plays a gatekeeping role that makes being trans harder than it needs to be, and poor communication from the GIC:
“The long wait on the waiting list has been very difficult, especially now that I have been waiting long past the length of time on the letter I received (22 months).”
“Communication is terrible ... The waitlist just keeps getting longer and longer.”
Respondents currently accessing services similarly described experiences of slow service delivery, with a lack of communication and infrequent appointments:
“Very negative, the service is too slow, they put people on a waiting list for procedures that don’t even exist.”
Two respondents said they had noticed changes in the delivery of gender identity services in their area since the allocation of SG funding. However, one of these respondents noted the main change they had observed was reduced services at the GIC: “The GIC in Aberdeen was closed for six months. Nobody was informed. Since it reopened, service has been minimal.” Of the respondents who had not noticed any changes, or who did not know, in their experiences there continued to be slow treatment, minimal levels of communication and lengthy waiting lists.
In addition to the survey with service users, a small number of follow-up interviews were conducted. These interviews confirmed many of the views shared in the survey, namely that people waiting to access services were extremely concerned about the long waiting times and absence of communications from the GIC. In response, one interviewee said that they turned to private healthcare and self-medication (through their own research) as the only options available to them due to long waiting times.
“I was aware of how long the waiting lists were to access the GIC [in Grampian], so my first protocol was to make an appointment with a private clinic. I then made an appointment with my GP and asked for a referral to the GIC. Since then, I have continued to see doctors at the [private] clinic and have started on a course of hormone replacement therapy … I have received one letter since [from the GIC], confirming that I was on the waiting list. Since then, I haven't received any communication from them.”
While some patients considered themselves lucky in having the means to access private healthcare, others were unable to do so due to financial constraints. Interviews also revealed that some patients felt that their gender identity was not taken seriously if they were non-binary. These service user experiences reflect broader SPHN and NHSGGC research around non-binary people feeling as though they were not receiving adequate support at GICs. One service user shared that,
“I felt pressured to present a certain way. Like I didn't feel like I could come to any of the appointments in jeans and a t-shirt. I felt like I had to perform a binary gender in order to be taken seriously … There are still people who believe that binary identities are the only ones that are valid. There hasn’t been the training to stop that kind of bigotry.”
In interviews, service users also felt that the reluctance of some GPs to support trans and non-binary patients, and the absence of Shared Care Agreements between GICs and GPs, was a particular obstacle for patients trying to access care.
“GPs should be responsible for more gender care. It doesn’t need specialists. We don't need the gender identity clinic system. It's not specialist care. [A lot of it is] low frequency stuff, and a lot of things GPs deal with is low-frequency stuff. You just have to reference the training materials [for GPs in supporting gender identity care]. Centralising care into a few nexuses [i.e., specialist GICs] is, I think, detrimental.”
Interviewees also shared some positive experiences in accessing services. One service user at Grampian GIC said that they had been waiting for laser hair removal treatment for over a decade and were finally able to have this treatment in 2022, which they believed was due to the additional SG funding provided for improvement work.
“It must have been 2023 or so that I was actually able to access the laser hair removal … the extra funds actually allowed me to access treatment that wasn’t available to me before … it had taken me a decade to get it because of the lack of funding.”
In interviews, service users spoke positively about the move to make appointments at the GIC more accessible through virtual options.
“[before], I had to travel two hours [to get to the GIC], which for some other people is nothing compared to the journeys they have to make. I will say that having the ability to do stuff via the web and Teams has significantly reduced that load and made it easier. That wasn’t really available before or when I first started [accessing services].”
Finally, service users were positive about the care they’d received from secondary services within NHS Grampian, after they had accessed the GIC.
“Some of the services were absolutely brilliant. The voice training I had was absolutely perfect ... the way I was treated going in for laser hair removal, that was brilliant. It took two years for the Aberdeen Hospital to get their own laser systems in and people trained, and that's how I was able to access laser hair removal about two years ago.”
However, interviewees felt that these positive experiences were often overshadowed by the extremely long waiting times to access services. While service users expressed understanding for clinicians and compassion for heavy workloads, there was a sense of disbelief that waiting list numbers had not come down:
“All the waiting lists are just too long. A two to three year waiting list does not seem particularly fair and the worst part of it is you have to feel grateful because I'm aware that it’s longer [in other places] ... It shouldn't be acceptable … I don't necessarily have a lot of confidence that I will be seen in two or three years.”
In addition, in response to the third sector survey carried out as part of this project, one respondent pointed to the issues that “the service has essentially been ‘closed’ for a significant period of the funding period”, with the effect that “waiting lists are now longer than they were at the start of the framework.” In an interview with a third sector representative, there was understanding that the GIC had been facing challenges due to recruitment issues: “I know that Grampian had quite a difficult time, they had qualified clinicians leaving. But when they [paused] the service, they didn’t tell anyone.”
7.9 Structural and systemic issues
There are a number of structural factors that have influenced the delivery of gender identity healthcare services in NHS Grampian.
Fragility of service
Perhaps the most important of these is the fragility of the service, due to recruitment challenges and the lack of long-term funding, which has led to the service being reduced several times in recent years. To fully resume services, it had to bring in new staff who required training in gender identity healthcare. For one interviewee,
“I think one of the problems as to why we’re where we are now is because there aren’t any staff who have been working previously in the clinic. So there isn’t that experience. I think it’s important to retain that experience. But also, there is this ‘stop, start, stop, start’ that we’ve been experiencing over the last three or four years.”
While the service has benefitted from two consultant psychiatrists who have worked continuously through periods of reduced service, the fragility of the service has been compounded by the temporary lack of a permanent clinic lead, who is able to lead the development of the service and shape a cohesive workforce that is resilient to staff shortages, despite NHS Grampian’s multiple attempts to hire for this position.
Team leadership, clarity and cohesion
Interviewees have stressed the importance of having someone to lead the GIC, of having clarity around job roles, and a cohesive team culture where everyone pulls together and communicates effectively. One interviewee said that bringing in a clinical lead was the most important factor for making the GIC successful: “It’s my number one priority, having someone who can actually make these decisions, because we have lots of ideas we want to take forward.” Another interviewee felt that the stress of the long waiting list was blurring lines between roles as everyone tried to tackle it, and having more clarity around their role would be helpful for ensuring a more efficient service.
Team-building was also mentioned as an important key to the success of the gender identity service team, as in any organisation. The part-time nature of roles, and lack of full-time permanent posts (owing to the nature of the funding), was viewed as hindering team development. One interviewee said, “it just feels like a very part-timer kind of service … sometimes, arranging a meeting can be so difficult, because we all work on different days.” Finally, staff members felt that stronger and clearer communications from senior management would help embed a more effective and cohesive service.
Support from the Health Board
Finally, several staff interviewees expressed a desire to receive more support and communication from the NHS Grampian Health Board. This went beyond resources (funding) to a desire to feel valued by Boards, and their work being seen as important. One interviewee said they felt that the GIC was not fully embedded in the NHS Health Board: “it just seems to be a bit disjointed.” Another interviewee felt that having more support from the Board would enable the development of the necessary infrastructure, data and evidence base around the service that could help with continuous improvement and learning, such as performance data and patient feedback data.
7.10 Conclusion
To help evaluate the effects of SG funding on services at Grampian GIC, we have developed a bespoke Theory of Change (ToC) for NHS Grampian, shown below. This is based on the main ToC presented at the start of this report, and then tailored to NHS Grampian based on its aims for the SG improvement funding, the activities they have since undertaken, and the outcomes these changes are leading to.
Situation:
- Wider structural context (high demand for services, long wait lists, overstretched staff, lack of specialists)
- Consideration of local context
- (based in Mental Health Services; referrals from Grampian, Orkney and Shetland NHS board areas; previous periods of inactivity)
- Fostering collaboration / relationships (links to other NHS Grampian teams; GP practices; third sector partners
Inputs:
- Total of £509k SG funding allocated to NHS Grampian over 2022-25 to improve access to, and delivery of, gender identity services
- Use of this funding by NHS Grampian to support activities, by:
- Expanding the gender service in line with MDT approach
- Increasing the hours of existing staff to see more patients/ build relationships
- Staff training / development
Activities:
- NHS Grampian implementing plans to improve services, in line with SG funding:
- Improve provision of information to patients
- Provide more tailored / personalised pathways
- Build partnership with Four Pillars
- Address inequalities through a needs-led approach
- Increase activity to reduce waiting times, support those waiting
Preconditions:
- Robust data & evidence
- General training for mainstream NHS staff, to enable joined-up care
- Specialised training on gender identity for GIC staff
- Safe and fulfilling workplaces
- Local, regional and national leadership
- Empowered and resourced staff, able to confidently make decisions
- Shared care GP agreements
Outcomes:
- Changes to meet the needs of patients (improved wait times, prevention of backlogs, increased psychosocial and peer support)
- Changes to understanding of systems (new demand / capacity model, increased coordination across the pathway)
- Changes to governance of systems (quality improvement work, Choice and Partnership Approach)
Impacts:
- Realistic Medicine vision:
- Empowered patients, Personalised Care, Informed Decisions, Joined Up care
- GIC-specific:
- Accessible, inclusive services (including pre-service support), educated workforce, sustainable and well-funded services, good governance, strong networks, mainstreamed and joined-up care, reduced inequalities
Overall, the NHS Grampian case study provides an example of a GIC that has been hampered by infrastructural fragility and high staff turnover. As the clinic has not been able to access all of the funding that had been made available by the SG, due to financial decisions by the Health Board to use the SG improvement funding underspend to reduce the Board’s overall budget deficit, this has had a significant impact on service delivery. The GIC operated reduced services for a period of time as it did not have the necessary resources to hire a clinical lead to supervise staff and make decisions about service delivery and care pathways. The PHS waiting list data reveal that during the year 2023-24 when the SG improvement funding had been allocated, waiting times increased by 30%.[109] The survey and interview data from service users suggest that patients were experiencing the adverse effects of long waiting lists and did not feel that communication was sufficient.
At the same time, the GIC staff who have been working to implement the new service plan and fully resume services at the clinic have been passionate, dedicated and fully committed to improving patient outcomes. Staff have made great progress in implementing service redesign. They have rebuilt links with other NHS teams in Grampian including endocrinology, speech and language therapy and psychiatry; they have met with other GICs in Scotland to learn best practice and undertake training; they have started rebuilding relations with the LGBTQ+ organisation Four Pillars; and they have been developing resources for patients who are on the waiting list and reviewing communications strategies with patients, prior to the service fully resuming in August 2024. It is therefore likely that the SG funding will continue to have positive impacts on service delivery and patient outcomes going forward, with the clinical supervision and training now in place as a result of the SG funding. It may take time, however, for these service changes to trickle down to service users and result in the outcomes set out in the Grampian funding proposal and the Theory of Change.
Therefore, while the SG funding has enabled the Grampian GIC to fully resume its gender identity services and realise its service plan in August 2024, it still faces some structural challenges in delivering services in line with the Theory of Change. Notably, several preconditions are required - including robust data and evidence, training and support for staff to feel empowered, and shared care with GPs - to enable activities to lead to outcomes. Furthermore, the achievement of outcomes and longer-term impacts in line with the Realistic Medicine vision may be enabled at the local (GIC), regional (Board) and national (SG/NHS Scotland) levels by putting in place a number of best practice learnings. These learnings are elaborated in full towards the end of this report, and include: creating a cohesive team with the right staff mix and appropriate grading; continuous improvement ethos; strong communications with patients; consistent structures and pathways; greater collaboration with the third sector and GPs; stronger Health Board leadership and support; long-term (earmarked) core funding; clinical governance; staff training; shared care with GPs; and involvement in national networks. These best practice learning may help address questions around how to ensure the resilience and sustainability of the GIC going forward.