Scottish Health Survey 2015 - volume 1: main report
Findings and trends of the Scottish Health Survey 2015, providing information on the health of people living in Scotland.
9 Cardiovascular Conditions And Diabetes
Laura Brown
Summary
- Fifteen percent of adults aged 16 and over reported ever having been diagnosed with any CVD condition by a doctor in 2015 (similar to the levels of 14-16% since 2003).
- Among adults aged 16 and over, 19% had any CVD condition or diabetes, 6% had doctor-diagnosed diabetes and 8% had ischaemic heart disease ( IHD) or stroke.
- Doctor-diagnosed diabetes increased significantly between 2003 and 2011 (4% to 6%) and has remained at this level since.
- From 2003 to 2015, figures for any CVD condition (14-16%) and IHD (6-7%) were relatively static.
- Prevalence levels of IHD or stroke were significantly higher for men (9%) than for women (6%).
- In 2014/2015, 29% of adults aged 16 and over had survey-defined hypertension, significantly higher than doctor-diagnosed levels (25%).
- The level of survey-defined hypertension has not changed from 2012/2013.
- Prevalence was higher for men (31%) than women (27%) and rose from 3% of those aged 16-24 to 71% of those aged 75 and over.
- More than half (58%) of adults with survey-defined hypertension reported it had been diagnosed by a doctor.
9.1 Introduction
Cardiovascular disease ( CVD) is a general term describing diseases of the heart and blood vessels whereby blood flow to the heart, brain or body is restricted. It is one of the leading contributors to the global disease burden [1] . Its main components are ischaemic heart disease ( IHD) (or coronary heart disease) and stroke, both of which have been identified as clinical priorities for the NHS in Scotland [2,3] . Diseases of the circulatory system are the second most common causes of death in Scotland after cancer, accounting for 27% of deaths in 2015 (compared with 28% for cancer). This includes 12% of deaths which are caused by IHD, with a further 7% caused by cerebrovascular disease (e.g. stroke) [4] . Early mortality from heart disease and stroke have both improved in recent years, but concern remains about continuing inequalities in relation to morbidity and mortality linked to these conditions [2,3] .
The increasing prevalence (albeit at a reduced rate) of diabetes, the most common metabolic disorder, is a major health issue for Scotland. Scotland has one of the highest levels of type 1 diabetes in Europe, but it is the increasing prevalence of type 2 diabetes - linked to obesity, physical inactivity and ageing - which is driving the increased prevalence and causing concern [5] . Diabetes is a risk factor in premature mortality, although more effective treatments of diabetes and hypertension have offset some of the excess risk in recent years and mean some people may be living longer and better with the condition [5] .
9.1.1 Policy background
One of the Scottish Government's National Performance Framework National Outcomes is for people in Scotland to 'live longer, healthier lives' [6] . There is also a National Performance indicator to 'reduce premature mortality' (deaths from all causes in those aged under 75) [7] . CVD is described as one of the key 'big killer' diseases around which action must be taken if this target is to be met. In addition, a number of the National Indicators [8] are linked to key CVD risk factors, most notably smoking, but also physical activity [10] and healthy weight children [11] (the latter two are also major risk factors for diabetes).
In recognition of the challenges posed by long-term conditions such as CVD, diabetes and respiratory conditions - both for the individual and their families, as well as for health and care services - the Scottish Government's over-arching strategy for long-term conditions was published in 2009. The Action Plan recognised the need for system-wide action in response to the challenge presented by the increasing prevalence of long-term conditions within the context of an ageing population, the links to health inequalities, and the particular challenges of multi-morbidity - the presence of two or more long-term conditions. The Keep Well Programme [12] focussed on delivering health improvements in deprived communities by offering health checks to individuals aged 40-64, including screening for CVD and its main risk factors.
The Heart Disease and Stroke Action Plan [2] which was published in 2009, and the Diabetes Action Plan [5] which was published in 2010, both set out a comprehensive programme for further reducing deaths and improving the lives of people living with heart disease, stroke and diabetes. These have been refreshed and separate Heart Disease [13] , Stroke [14] and Diabetes [15] Improvement Plans were published in August 2014 and November 2014. These set out key priorities for the delivery of improvements of treatment and care in heart disease, stroke and diabetes.
9.1.2 Reporting on CVD conditions and diabetes in the Scottish Health Survey ( SHeS)
SHeS is an important source of information on the prevalence of CVD conditions and diabetes in Scotland. It also offers valuable information on the patterning of these conditions across different groups in society. In this chapter, trends in self-reported CVD conditions and diabetes prevalence for adults are updated for 2015. Updated trends in adult hypertension are presented and the extent of diagnosis, treatment and control of hypertension are also explored.
Supplementary tables providing additional data on these conditions are also available on the Scottish Government SHeS website [16] .
9.2 Methods And Definitions
9.2.1 Methods
Participants were asked whether they had ever suffered from any of the following conditions: diabetes, angina, heart attack, stroke, heart murmur, irregular heart rhythm, or 'other heart trouble'. If they responded affirmatively to any of these conditions, participants were asked whether they had ever been told they had the condition by a doctor and whether they had experienced the conditions in the previous 12 months. For the purposes of the analysis presented in this chapter, participants were only classified as having a particular condition if they reported that the diagnosis had been confirmed by a doctor.
It is important to note that no attempt was made to verify these self-reported diagnoses objectively. It is therefore possible that some misclassification may have occurred because some participants may not have remembered (or not remembered correctly, or not known about) diagnoses made by their doctor.
Blood pressure
Blood pressure was measured as part of the biological module [17] , using the Omron HEM device. This equipment has been used on SHeS since 2003. Prior to 2012, blood pressure was collected in a follow-up interview conducted by survey nurses. The nurse interview was discontinued in 2012, and since then specially trained interviewers have been collecting some of the less complex measures and samples previously collected by nurses, as part of the biological module. The equipment and protocol for taking blood pressure readings did not change. A validation study was carried out to assess the impact of the switch from nurse to interviewer administration [18] .
As a result, unadjusted measurements collected by interviewers are used within the report for more recent periods (2012/2013 and 2014/2015), with calibrated estimates (nurse equivalent) being used to show longer-term trends.
Three blood pressure readings were taken from consenting participants at one minute intervals using an appropriately sized cuff and on the right arm where possible. Participants were in a seated position and readings were taken after a five minute rest. Systolic and diastolic pressures and pulse measurements were displayed on the Omron for each measure. As in previous years, pregnant participants were excluded.
Since the size of the cuff used when taking blood pressure readings is an important factor in ensuring that accurate measurements are obtained three different sizes of cuff were available for use. Full details of the protocol used to take blood pressure reading in the survey are available in Volume 2 of this report.
The blood pressure measures used in this chapter are the means of the second and third measurements obtained for those for whom three readings were successful obtained. Analyses exclude results from participants who had eaten, drunk alcohol, smoked or exercised in the 30 minutes before the measurement was taken.
Use of medication
During the biological module, participants were asked about all the prescribed medications they were currently taking (i.e. taken in the last seven days). During the data processing phase, medications were coded according to the classification in the British National Formulary ( BNF), and from this classification it is possible to identify lipid-lowering and anti-platelet medication. Some analyses in this chapter examine the effect of the use of these drugs.
9.2.2 Definitions
Any CVD condition
Participants were classified as having 'any CVD' if they reported ever having any of the following conditions confirmed by a doctor: angina, heart attack, stroke, heart murmur, abnormal heart rhythm, or 'other heart trouble' [19] .
Diabetes
Participants were classified as having diabetes if they reported a confirmed doctor diagnosis. Women whose diabetes occurred only during pregnancy were excluded from the classification. No distinction was made between type 1 and type 2 diabetes in the interview.
Any CVD condition or diabetes
A summary measure of the above conditions is presented in the tables as 'any CVD condition or diabetes'.
Ischaemic heart disease ( IHD)
Participants were classified as having IHD if they reported ever having angina or a heart attack confirmed by a doctor. All tables refer to ever having had the condition.
Stroke
Participants were classified as having a stroke if they reported ever having had a stroke confirmed by a doctor.
IHD or stroke
A summary measure of the above conditions is presented in the tables as ' IHD or stroke'.
Blood pressure levels classification
In accordance with guidelines on hypertension management [20] the threshold of 140/90mmHg is used to define hypertension in SHeS.
Adult participants were classified into one of four groups listed below on the basis of their systolic ( SBP) and diastolic ( DBP) readings and their current use of anti-hypertensive medications. For the purpose of this report, the term 'hypertensive' is applied to those in the last three categories.
| Normotensive untreated | SBP below 140mmHg and DBP below 90mmHg, not currently taking medication specifically prescribed to treat high blood pressure |
| Hypertensive controlled | SBP below 140mmHg and DBP below 90mmHg, currently taking medication specifically prescribed to treat high their blood pressure |
| Hypertensive uncontrolled | SBP at least 140mmHg or DBP at least 90mmHg, currently taking medication specifically prescribed to treat their high blood pressure |
| Hypertensive untreated | SBP at least 140mmHg or DBP at least 90mmHg, not currently taking a drug specifically prescribed to treat their high blood pressure |
Detection, treatment and control of hypertension
In addition to the objective definition of hypertension described above, participants were defined as having self-reported doctor-diagnosed hypertension if they stated during the interview that they had been told by a doctor or nurse that they had high blood pressure.
Hypertension detection was estimated by examining the proportion of those with survey defined hypertension ( SBP at least 140mmHg or DBP at least 90 mmHg or on treatment for hypertension) reporting doctor-diagnosed hypertension. Treatment rates were estimated by examining the proportion of all those defined as having survey-defined hypertension who were on treatment at the time of the survey. The control of hypertension among those on treatment for hypertension at the time of the survey was estimated by calculating the proportion with blood pressure below 140/90mmHg.
When interpreting results it should be borne in mind that although three blood pressure readings were taken, these were all on a single occasion. Clinical diagnoses of hypertension are based on sustained levels of high blood pressure rather than a single measurement.
9.3 Cardiovascular Conditions And Diabetes
9.3.1 Trends in any CVD, diabetes, any CVD or diabetes, IHD, stroke, and IHD or stroke prevalence since 1995
Any CVD
In 2015, roughly one in seven (15%) adults aged 16 and over reported that they had been diagnosed by a doctor with any CVD condition. This figure does not differ significantly from those in 2014 (16%) or previous years (14-16% from 2003 to 2013). The longer-term trend for those aged 16-64 showed little change in the earliest survey years (9% in 1995, 8% in 1998 and 9% in 2003) suggesting that prevalence has remained largely static across the entire survey period. Prevalence for those aged 16-64 was 10% in 2015.
As noted in previous reports [21] , the proportion of men aged 16 and over with any CVD conditions increased gradually from 15% in the 2003-2009 period to 18% in 2014. In 2015, levels stayed at a statistically similar level (16%) to those in both the aforementioned periods. Prevalence for women aged 16 and over remained relatively stable, fluctuating between 14% and 16% since 2003 (15% in 2015).
Doctor-diagnosed diabetes
From 2003 to 2015 there have been significant increases in the prevalence of doctor-diagnosed diabetes among all adults aged 16 and over (4% to 6%), men aged 16 and over (4% to 7%) and women aged 16 and over (4% to 5%). Data for all adults aged 16-64 from 1995 to 2003 (2% in all survey years) suggest that this trend did not begin earlier.
Any CVD or diabetes
Prevalence of the combined measure of any CVD or diabetes for adults aged 16 and over increased significantly from 2003 (17%) to 2015 (19%), although figures were largely unchanged in recent years (19-20% between 2012 and 2015). A similar pattern can be observed among adults aged 16-64 (a significant increase from 11% in 2003 to 13% in 2015), with figures from 1995 (10%), 1998 (10%) and 2003 (11%) suggesting the upward trend did not start before 2003.
There was a similar increase over time from 2003 to 2015 for men (17% to 20%) albeit with the 2014 figure being significantly higher (23%) and possibly the result of sampling fluctuation. There were no significant differences between women from 2003 (16%) to 2015 (18%).
IHD
The proportion of adults aged 16 and over reporting an IHD diagnosis ranged between 6% and 7% between 2003 and 2015 (6% in 2015).
While there has been a significant downward trend in IHD among women aged 16 and over (from 7% in 2003 to 5% in 2015), there has been little change in IHD prevalence among men over this same period, with figures varying from 7-8% (7% in 2015).
Stroke
There is no significant difference in stroke prevalence for adults aged 16 and over between 2003 (2%) and 2015 (3%). For both men and women prevalence has been 2-3% since data were first collected in 2003.
IHD or stroke
The combined prevalence of IHD or stroke has not changed significantly from 2003 (9%) to 2015 (8%). While there has been no significant change in the proportion of men aged 16 and over reporting either condition (10% in 2003 and 9% in 2015), there has been a significant drop in prevalence among women (8% in 2003 to 6% in 2015).
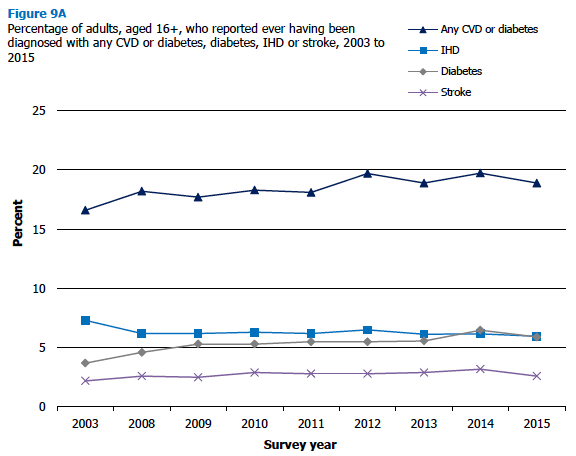
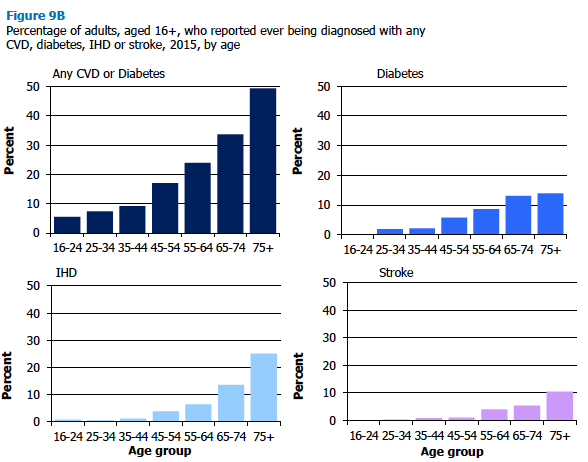
9.3.2 Any CVD, doctor-diagnosed diabetes, any CVD or diabetes, IHD, stroke, IHD or stroke, 2015, by age and sex
Any CVD
In 2015, 15% of adults aged 16 and over reported being diagnosed with any CVD condition. Levels did not vary significantly between men (16%) and women (15%), with levels of prevalence increasing significantly with age (from 6% for those aged 16-24 to 44% for those aged 75 and over). Levels increased with age for both men and women but with a sharper gradient of increase for men (from 3% of those aged 16-24 to 49% for those aged 75 and over) than for women (from 9% to 40% respectively).
Doctor-diagnosed diabetes
In 2015, 6% of adults aged 16 and over reported that a doctor had diagnosed them with diabetes, with no statistical difference in prevalence by sex (7% of men and 5% of women). There was a clear age-related pattern to prevalence with none of those aged 16-24 reporting a diagnosis, compared with 13-14% of adults aged 65 and over. Similar patterns of increase were seen for both men and women.
Any CVD or diabetes
Around a fifth (19%) of adults in Scotland in 2015 reported any CVD or diabetes diagnosed by a doctor, with comparable proportions for men (20%) and women (18%). Similar to the pattern discussed above for any CVD, prevalence was lower among younger age groups (6% of adults aged 16-24) and increased with age up to 49% of adults aged 75 and over. A sharper rate of increase with age was again apparent for men (from 3% for those aged 16-24 to 55% for those aged 75 and over) than for women (9% to 46% respectively).
IHD
In 2015, 6% of adults in Scotland reported ever having being diagnosed with IHD with a significant difference in prevalence between men (7%) and women (5%). Prevalence was very low among adults aged 16-44 (0-1%), and rose to 4-6% for those aged 45-64 and 14-25% for those aged 65 and over. Prevalence increased with age for men from 0.5% or less for those aged 16-34 to 32% for those aged 75 and over, with a slower rate of increase for women (0-1% to 20% respectively).
Stroke
In line with previous years [21] , the proportion of adults in Scotland reporting ever having had a stroke in 2015 remained low (3%), with similar levels for men and women (both 3%). The proportion of those aged 16-54 with a diagnosis was 0-1%, increasing to 4-5% of adults aged 55-74 and 10% of those aged 75 and over. Men and women had similar patterns of prevalence by age.
IHD or stroke
In 2015, 8% of adults reported having had a stroke or IHD that had been diagnosed by a doctor, with statistically higher figures for men (9%) than women (6%). Prevalence increased with age, from 1% in the two youngest age groups (16-24 and 25-34), to 32% of adults aged 75 and over. As with the measure for IHD, rates rose with age more steeply for men (from 0.5% or less for those aged 16-34 to 38% for those aged 75 and over) than for women (1% to 28%).
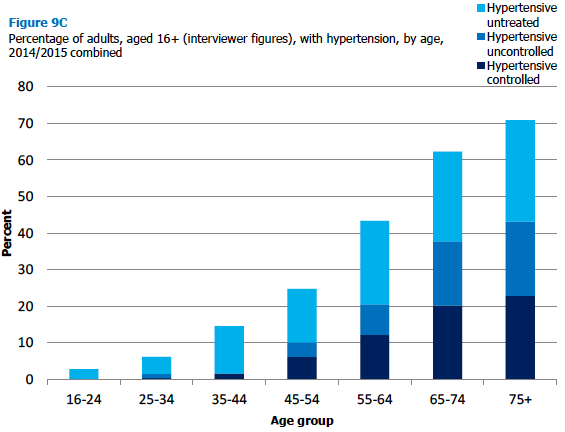
9.3.3 Blood pressure level, 2014/2015 (combined), by age and sex
To increase the sample size available, data from the 2014 and 2015 surveys combined were used in the blood pressure analysis. In 2014/2015 (using unadjusted interviewer figures, see section 9.2.1), 29% of adults aged 16 and over in Scotland had survey-defined hypertension [22] , consisting of 15% with untreated hypertension, 8% with controlled hypertension and 6% with hypertension that was uncontrolled despite being treated.
There was a significant association between presence of hypertension and age in 2014/2015, with 3% of the youngest age group (aged 16-24) having survey-defined hypertension rising to 71% among those aged 75 and over. While prevalence was significantly higher among men than women (31% compared with 27% respectively), different patterns by age were seen for each sex, with a sharper rate of increase for women (from 1% for those aged 16-24 to 76% for those aged 75 and over) than for men (from 5% to 65% respectively).
Figure 9C, Table 9.3
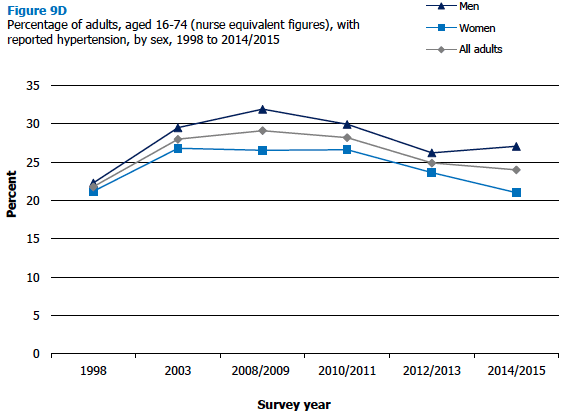
9.3.4 Blood pressure level, 1998 to 2014/2015 (combined)
2014/2015 data for blood pressure using interviewer figures (see section 9.2.1) showed 29% of adults aged 16 and over having survey-defined hypertension, the same proportion as in 2012/2013. The longer-term trend using nurse-equivalent calibrated estimates for all adults from 2003, showed a significant decrease between 2010/2011 (33%) and 2012/2013 (28%) and remained at this level in 2014/2015. Nurse-equivalent figures for those aged 16-74 suggest that there may have been an earlier increase in prevalence, with a significant change from 22% in 1998 to 28% in 2003 (as shown in Figure 9D).
Figure 9D, Table 9.4
9.3.5 Comparison of doctor-diagnosed with survey-defined hypertension, 2014/2015 (combined), by age and sex
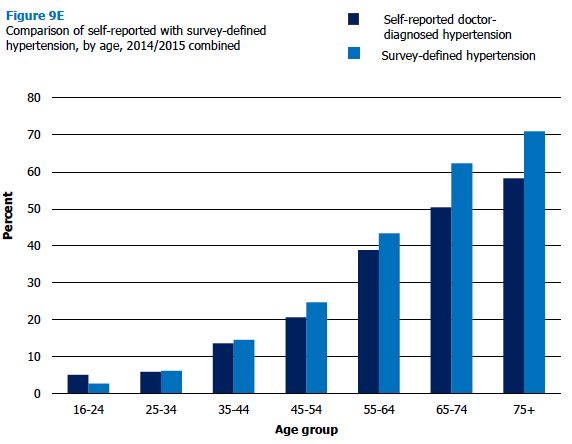
To increase the sample size available, the comparison of doctor-diagnosed hypertension with survey-defined hypertension, by age and sex, used data from the 2014 and 2015 surveys combined. In 2014/2015, 25% of adults aged 16 and over reported that they had received a diagnosis of hypertension from a doctor compared with 29% of adults having survey-defined hypertension. For both men and women, survey-defined hypertension was four percentage points higher than doctor-diagnosed hypertension (31% and 27% for men, 27% and 23% for women).
Across the age groups, prevalence of survey-defined hypertension was generally higher than reported doctor-diagnosed hypertension in 2014/2015 combined, with the gap between the two growing with age. Whereas for those aged 16-24, survey-defined hypertension was two percentage points lower than doctor-diagnosed hypertension (3% and 5%), there was no difference at age 25-34 (both 6%). For those aged 75 and over survey-defined hypertension was 13 percentage points higher (71% compared with 58% for doctor diagnosed hypertension). Among those aged 75 and over, the percentage point gap between prevalence of survey-defined and reported doctor-diagnosed hypertension was 17 for women (76% and 59% respectively) compared with 8 for men (65% and 57% respectively).
Figure 9E, Table 9.5
9.3.6 Detection and treatment of hypertension, 2014/2015 (combined), by age and sex
The detection rate in Table 9.6 shows the proportion of participants with survey-defined hypertension who reported doctor-diagnosed hypertension. In 2014/2015 the hypertension detection rate among adults with survey-defined hypertension was 58%. Detection rates were patterned by age, increasing from 44% among adults aged 35-54, to 57% for those aged 55-64 and 69% for adults aged 65 and over. Age-related patterns of detection differed by sex, with there being a significant increase with age for men from 51-54% for those aged 35-64 to 69-70% for those aged 65 and over. For women, there was a significant and steeper increase from 29% for those aged 35-54 to 64-69% for those aged 55 and over.
In 2014/2015, around one in five adults (21%) with survey-defined hypertension were on medication for high blood pressure but also had high blood pressure readings (hypertension treated but not controlled). As with detection rates, there was an age-related pattern to treated but not controlled hypertension, increasing from one in ten adults (10%) aged 35-54 to nearly three in ten adults (28-29%) aged 65 and over. In 2014/2015, over a quarter of adults with survey-defined hypertension (27%) were taking medication and did not have a high blood pressure reading (hypertension treated and controlled). There continued to be an age-related pattern, with levels increasing from 20% of adults aged 35-54, to 28% of those aged 55-64 and 32% of adults aged 65 and over.
Contact
Email: Julie Landsberg, julie.landsberg@gov.scot