Scottish Health Survey 2015 - volume 1: main report
Findings and trends of the Scottish Health Survey 2015, providing information on the health of people living in Scotland.
8 Obesity
Joe Rose
Summary
- In 2015, two-thirds of adults (65%) were overweight, including 29% who were obese, figures which have changed little since 2008.
- Levels of obesity were similar for both men and women (28% of men and 30% of women).
- Overweight and obesity remain significantly associated with age. In 2015, 38% of men aged 16-24 were overweight or obese, rising to 82% of men aged 65‑74. There was a similar pattern for women, with 46-47% of women aged 16-34 overweight or obese, compared with 75% of those aged 75 and over.
- Waist circumferences were higher on average in 2014/2015 than in 2003 for both men (98.2 cm in 2014/2015 and 95.3cm in 2003) and women (89.5 cm in 2014/2015, 86.3 cm in 2003).
- The proportion of men with a raised waist circumference (greater than 102cm) increased from 28% in 2003 to 37% in 2014/2015. The proportion of women with a raised waist circumference (greater than 88cm) increased from 39% to 52% over the same period.
- Around two-thirds of all women (66%) and three in five men (59%) had an increased risk of disease based on their BMI and waist circumference.
- Overall, 28% of men were categorised as being at very high risk level or above, and 3% at extremely high risk level. Equivalent figures for women were 32% at very high risk level or above, and 4% at extremely high risk level.
- The proportion of boys of healthy weight (73% in 2015) has increased year on year since 2011 (63%) and is comparable to the level seen in 1998 (70%).
- The proportion of girls who were a healthy weight in 2015 was 70%, a level which has remained relatively steady since 1998.
- Just over one in four (28%) children were at risk of overweight in 2015, with no significant difference between boys and girls (26% of boys and 29% of girls).
- In 2015, 15% of boys and 14% of girls were at risk of obesity, figures which were identical to those in 1998.
- Compared with a child with parents of a healthy weight, a child with an obese parent was significantly more likely to be at risk of overweight, including obesity (40% compared with 22%), or at risk of obesity (23% compared with 11%).
3.1 Introduction
Overweight and obesity have been defined as abnormal or excessive fat accumulation that may impair health [1,2] . Obesity is associated with an increased risk of a number of common causes of disease and, at high levels of obesity ( BMI of 35 or above), death. [3] The impact of overweight and obesity upon quality of life and health is felt across the lifecourse. During childhood, those who are overweight or obese have an increased risk of conditions such as hypertension, type 2 diabetes and asthma [4,5] . If their weight continues to be unhealthy into adulthood, children are at an increased risk of numerous conditions associated with adult obesity, such as diabetes, cardiovascular disease, osteoarthritis and some cancers [6,7,8] . There is also evidence suggesting a link between overweight and obesity in midlife and dementia in old age [9,10,11] .
Scotland has one of the worst obesity records among OECD countries[12]. Various studies have attempted to estimate the costs to the NHS in Scotland of overweight and obesity combined, with suggested figures ranging between £363 and £600 million (the majority of these costs are incurred as a result of associated conditions such as cardiovascular disease and type 2 diabetes, rather than direct costs of treating or managing overweight and obesity) [13] . The latest estimate of the total (direct and indirect) cost of overweight and obesity to Scottish society, including labour market related costs such as lost productivity, have been put at £0.9-4.6 billion [13] . The health and economic consequences of obesity mean that tackling it remains a key priority for government and public health professionals.
8.1.1Policy background
A number of government policies and initiatives aimed at addressing the issue of obesity are in place in Scotland. In the Prevention of Obesity Route Map, the Scottish Government and COSLA outlined their long-term commitment to tackle overweight and obesity and achieve a healthier Scotland [12] . The long-term goals of the route map are to have the majority of Scotland's adult population in normal weight throughout life, to have reduced levels of type 2 diabetes, and to have fewer overweight or obese children in Scotland [14] . The commitment to the latter of these goals is reinforced by the inclusion of the National Indicator to 'increase the proportion of healthy weight children' in the National Performance Framework ( NPF) [15] .
The Scottish Health Survey ( SHeS) is used to monitor progress towards the NPF indicator on healthy weight children and several of the Obesity Route Map indicators [16] . Scotland's children and young people's mental health indicators set also includes an indicator on child obesity prevalence [17] .
Eat Better Feel Better is a campaign aimed at promoting healthier eating as a simple, affordable choice for everyone in Scotland. Connecting people with local cooking classes, food co-ops and community groups that can offer support on nutrition and food, the campaign aims to have a long-lasting effect on families and communities. It is supported by supermarkets and the convenience sector throughout Scotland and aims to promote the healthier eating message to as many shoppers as possible.
Regular physical activity helps people maintain a healthy weight. One of the themes of Legacy 2014 programmes is to use the opportunities presented by the 2014 Commonwealth Games to help people be more physically active [18] . The Physical Activity Implementation Plan is one of the many legacy programmes developed under the 'active' theme to meet this desired outcome [19] . The 10 year plan, launched in 2014, links directly to the Scottish Government's legacy ambitions for the Commonwealth Games.
8.1.2Reporting on obesity in the Scottish Health Survey ( SHeS)
The anthropometric measures presented in this chapter focus on measurements relevant to adult and child obesity. Height, weight and waist measurements have been collected during the survey interview every year since its inception in 1995. SHeS is one of a small number of surveys that collects height, weight and waist measures as opposed to using self-reported measures which are known to be less accurate [20,21] . Height and weight are used to calculate Body Mass Index ( BMI), the primary measure of obesity used in the SHeS series. Both adult and child trends in BMI are examined in this chapter as are adult waist circumference and child BMI by parental BMI. Supplementary tables are also available on the Scottish Government SHeS website [22] .
8.1.3Comparability with other UK statistics
Adult obesity is defined consistently in the Scottish Health Survey and the other health surveys within the UK using BMI classifications. Height and weight measurements are self-reported in the Welsh Health Survey and are therefore not directly comparable with equivalent statistics in Scotland, England and Northern Ireland, where direct measurements are taken. Sampling methodologies differ between the surveys. Of the four UK health surveys, the Scottish Health Survey and Health Survey for England are the most closely aligned.
8.2 Methods And Definitions
8.2.1 Methods
Full details of the protocols used for collecting height, weight and waist circumference measurements are included in Volume 2 of this report and are summarised here.
Height
Height was measured using a portable stadiometer with a sliding head plate, base plate and four connecting rods marked with a metric measuring scale. Participants were asked to remove shoes. One measurement was taken, with the participant stretching to the maximum height and the head positioned in the Frankfort plane [23] . If the reading was between two millimetres it was recorded to the nearest even millimetre. No measurement was taken from participants who were pregnant, aged under 2, or unsteady on their feet.
Weight
Weight was measured using either Seca or Tanita electronic scales, both of which use a digital display. Participants were asked to remove shoes and any bulky clothing. A single measurement was recorded to the nearest 100g. A weight measurement was not collected from participants who were pregnant, aged under 2, or unsteady on their feet. Due to the scale limits, when using a Tanita scale those who weighed more than 130 kg were asked for an estimate of their weight, with estimates required for those weighing more than 200 kg if Seca scales were being used. These estimated weights were included in the analysis presented in this chapter.
In the analysis of height and weight, data from those who were considered by the interviewer to have unreliable measurements, for example those who had excessive clothing on, were excluded.
Waist
Since 2012, specially trained interviewers have taken waist measurements from respondents. These interviewers followed a different protocol for taking the measurements than the nurses who previously took the measurements. Results in this chapter are calibrated to allow the comparison of interviewer measurements with those previously taken by nurses.
The protocol for collecting waist measures also changed in 2012. Waist circumference is now defined as around the navel or tummy button. Waist was measured using a tape with an insertion buckle at one end. Interviewers took each measurement twice, using the same tape, and recorded readings. If the reading fell between two millimetres the reading was taken to the nearest even millimetre. Those participants whose two waist measurements differed by more than 3 cm had a third measurement taken. The mean of the two valid measurements (the two out of the three measurements that were the closest to each other, if there were three measurements) was used in the analysis presented in this chapter. Participants were excluded if they reported that they were pregnant, had a colostomy or ileostomy, or were unable to stand. All those with measurements considered unreliable by the interviewer, for example due to excessive clothing or movement, were excluded from the analysis presented in this chapter.
8.2.2Definitions
Body Mass Index ( BMI)
Body Mass Index ( BMI) is a widely accepted measure that allows for differences in weight due to height. It is defined as weight (kg)/square of height (m 2). This has been used as a measure of obesity in SHeS since its inception in 1995. BMI was calculated from valid measures collected by the interviewer.
Adult BMI classification
Based on their BMI, adult participants were classified into the following groups based on the World Health Organisation ( WHO) classification [24] :
| BMI (kg/m 2) | Description |
| Less than 18.5 | Underweight |
| 18.5 to less than 25 | Normal |
| 25 to less than 30 | Overweight, excluding obese |
| 30 to less than 40 | Obese, excluding morbidly obese |
| 40+ | Morbidly obese |
In this chapter, both mean BMI and prevalence for the five categories outlined in the table above are presented for adults. Although obesity has the greatest ill-health and mortality consequences, overweight is also a major public health concern, not least because overweight people are at high risk of becoming obese. Being underweight can also have negative health consequences.
Raised waist circumference ( WC)
BMI has some limitations and does not, for example, distinguish between mass due to body fat and mass due to muscular physique [25,26] . Nor does it take account of the distribution of fat in the body. It has therefore been suggested that waist circumference ( WC) may be a better means of identifying those with a health risk than BMI [2,27,28] .
In accordance with the definition of abdominal obesity used by the National Institutes of Health ( USA) ATP (Adult Treatment Panel) III, a raised WC is defined as more than 102 cm for men and more than 88 cm for women [29] . Following the protocol introduced to SHeS in 2012, described in Section 8.2.1, the equivalent cut-offs on SHeS are 102.75cm for men and 91.35cm for women [30] .
These thresholds help identify people at risk of metabolic syndrome. Abdominal obesity is reported as more highly correlated with metabolic risk factors (high levels of triglycerides, low HDL-cholesterol) than elevated BMI. It has recently been shown that these levels correspond fairly closely to the 95 th percentile of waist circumference for healthy people, indicating that few healthy people have a waist circumference above these thresholds [31] .
Combined assessment of health risk from obesity
The SIGN guideline on obesity cites the WHO's recommendation that an individual's risk of conditions such as type 2 diabetes and CVD is better estimated using a combination of both BMI and waist circumference ( WC) than using either measure on their own [7] .
The classification categories suggested by SIGN [7] are set out in the following table. BMI, derived from height and weight data collected in the main interview, in combination with waist measurements collected in the biological module have been used to estimate the proportion of the adults who fall into each of the risk categories. This combined classification designates those with a raised WC as 'very high' WC, while those towards the upper end of the 'not raised' WC range are designated 'high' WC. As the table indicates, the health risk is similar for adults with very high WC and class I obesity and for adults with high WC and class II obesity. The SIGN guidance notes that increased WC can be a marker for disease even among people of normal weight. The analysis presented in this chapter classifies people with normal weight and a very high WC as at increased risk of disease.
Assessment of health risk from obesity
| BMI Classification | 'High' WC Men WC 94-102cm Women WC 80-88cm |
'Very high' WC Men WC >102cm Women WC >88cm |
| Normal weight ( BMI 18.5 - <25(kg/m 2)) | - | - |
| Overweight ( BMI 25 - <30(kg/m 2)) | Increased | High |
| Obese | ||
| I - Mild ( BMI 30 - <35(kg/m 2)) | High | Very high |
| II - Moderate ( BMI 35 - <40(kg/m 2)) | Very high | Very high |
| III - Extreme ( BMI 40+(kg/m 2)) | Extremely high | Extremely high |
Source: based on Table 3, P11, in SIGN 115 [7] .
Child BMI classification
BMI is defined for children in the same way as it is for adults: weight (kg)/square of height (m 2). The International Obesity Task Force concluded that BMI is a reasonable measure of adiposity in children [32] and it is the key measure of overweight and obesity for children used in the SHeS series. Waist measurements were not collected in the child interview.
Despite the relatively wide acceptance of the use of BMI as an adiposity indicator, the establishment of an agreed specific obesity and overweight classification system for children and young people remains challenging. Constant changes in body composition during growth mean that the relationship between weight-for-height and adiposity during childhood and adolescence is age-dependent, and this relationship is further complicated by both ethnicity and gender [33] .
The classification of children's BMI used in this chapter, set out below, has been derived from BMI percentiles of the UK 1990 reference curves [34,35] (referred to as the national BMI percentiles classification); these have been used in each SHeS to date. The national BMI percentiles classification has been shown to be reasonably sensitive (i.e. not classifying obese children as non-obese) and specific (i.e. not classifying non-obese children as obese) [36,37] . SIGN recommends that these reference curves and thresholds should be used for population surveillance in Scotland [7] . The 85th / 95th percentile cut-off points are commonly accepted thresholds used to analyse overweight and obesity in children. These thresholds have previously been used to describe childhood overweight and obesity prevalence trends in the UK [38,39,40,41] .
| Percentile cut-off | Description |
| At or below 2 nd percentile | At risk of underweight |
| Above 2 nd percentile and below 85 th percentile | Healthy weight |
| At or above 85 th percentile and below 95 th percentile | At risk of overweight |
| At or above 95 th percentile | At risk of obesity |
SHeS uses a method developed by ISD Scotland to plot the exact ages of the children in the sample against the reference population data [42] . While children's exact age was used to calculate the BMI grouping prevalence rates (based on the interview date and the date of birth), results are presented using grouped ages based on age at last birthday.
As noted in the introduction to this chapter, one of the Scottish Government's national indicators relates to healthy weight in children, defined as neither underweight nor overweight or obese [43] . The presented data have been categorised to show the total proportions that are: healthy weight, at risk of overweight, at risk of obesity, and at risk of underweight.
Other changes made to the presentation of child BMI data in 2012 are discussed in detail in Chapter 7 of the 2012 annual report [44] .
8.2.3 Children's BMI categories, by parental BMI
Information in the chapter showing children's BMI by parental BMI is based on children in the main sample where at least one of their parents was also interviewed and had a valid BMI measurement. The data have been re-weighted so this analysis shows the pattern of association between parental and child BMI, and provides population estimates of the prevalence of child unhealthy weight in households with different parental profiles.
For households with BMI measures for two parents, the measure of parental BMI was based on whichever parent's BMI was the highest. If just one parent's BMI was measured this was used for this analysis. For example, if both parents were overweight or obese, or both were of normal weight or underweight, the parental BMI value matched that of both parents. If one parent was overweight and one was normal weight, the parental BMI was taken from the overweight parent. In households where one parent was interviewed, or just one parent provided a valid BMI measurement, the parental value matched that parent's BMI.
8.3 Adult Overweight And Obesity Prevalence
8.3.1 Trends in overweight including obesity prevalence since 1995
Overweight including obesity ( BMI of 25 kg/m 2 or above) prevalence since 1995 is shown in Table 8.1.
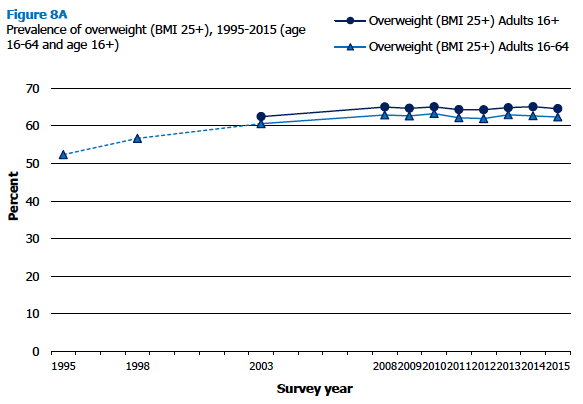
Prevalence of overweight including obesity in adults aged 16 and over has remained largely unchanged, between 64% and 65%, since 2008 (65% in 2015), following a significant increase between 2003 and 2008 (62% in 2003, 65% in 2008). As shown in Figure 8A, the longer trend for adults aged 16-64 follows the same pattern, while also showing a significant increase between 1995 (52%) and 2003 (61%).
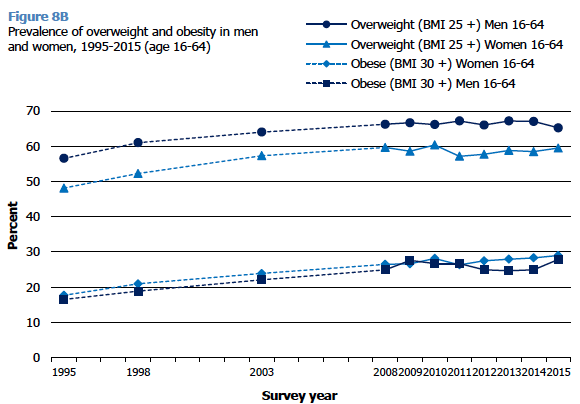
Separate trends for men and women are consistent with the overall trends for all adults, as shown in Figure 8B. Since 2008 levels have remained fairly static, with men continuing to be significantly more likely than women to be overweight including obese (67% for men and 62% for women in 2015). The longer trends for men and women aged 16-64 show significant increases between 1995 and 2008 in the prevalence of overweight (including obesity) for both men and women.
Figure 8A, Figure 8B, Table 8.1
8.3.2Trends in obesity and morbid obesity prevalence since 1995
Levels of obesity, including morbid obesity ( BMI of 30kg/m 2 or above), among adults aged 16 and over have remained fairly constant between 2008 and 2015, at between 27% and 29% (29% in 2015). This followed a significant increase between 2003 (24%) and 2008 (27%). The longer trend for adults aged 16-64 shows a significant increase between 1995 and 2003, from 17% to 23%. Since 2003, the first year with data for all ages, figures for adults aged 16-64 were one or two percentage point lower than those for adults aged 16 and over.
Figures for men and women were similar for most years. This was also the case in 2015, with 28% of men and 30% of women aged 16 and over categorised as obese.
8.3.3Trends in mean adult BMI since 1995
Mean BMI for all adults increased by a small but significant amount between 2003 and 2008 (from 27.1kg/m 2 to 27.4 kg/m 2), with little fluctuation since then (27.6 kg/m 2 in 2015). The mean BMI for men and women was similar in 2015 (a mean of 27.7 kg/m 2 for men and 27.5 kg/m 2 for women). The trend for adults aged 16-64 showed a significant increase between 1995 and 2003 (from 25.9 kg/m 2 to 26.9 kg/ m 2) with little change since then (27.5 kg/ m 2 in 2015).
8.3.4Adult BMI in 2015, by age and sex
In 2015, around two thirds (65%) of those aged 16 and over were overweight, including obese ( BMI of 25 kg/m 2 or above), whilst 29% were obese ( BMI of 30 kg/m 2 or above).The mean BMI among adults aged 16 or over was 27.6 kg/m 2, whereas the maximum recommended BMI considered to be within the healthy range is 25 kg/m 2.
Men remained significantly more likely than women to be overweight including obese (67% compared with 62%) in 2015, with women being more likely to have a BMI within the healthy weight range (36% compared with 32% of men). There was no statistically significant difference between the proportion of women (30%) and men (28%) who were obese (including morbidly obese). Mean BMI was also similar for men and women in 2015 (27.7 kg/m 2 for men and 27.5 kg/m 2 for women).
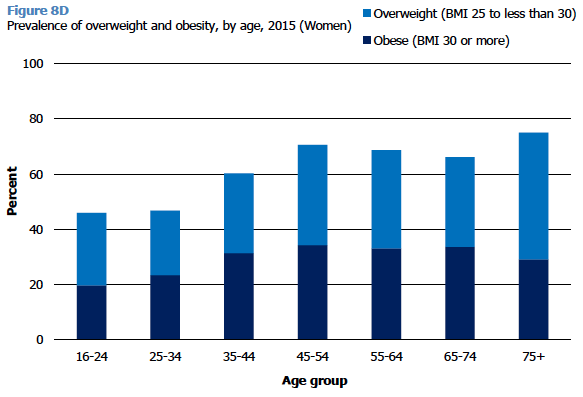
As shown in Figures 8C and 8D, there was a strong association between age and BMI in 2015. Among men, the proportion who were overweight (including obese) steadily increased by age from just under 4 in 10 (38%) of those aged 16-24 years to more than 8 in 10 (82%) of those aged 65-74. Obesity levels among men peaked at age 55-64 (40%). Among women, overweight including obesity levels also increased by age, from 46-47% of those aged 16-34, to 66-75% for those aged 45 and over. Obesity prevalence among women was highest among those aged 45-74 (33-34%).
Figure 8C, Figure 8D, Table 8.2
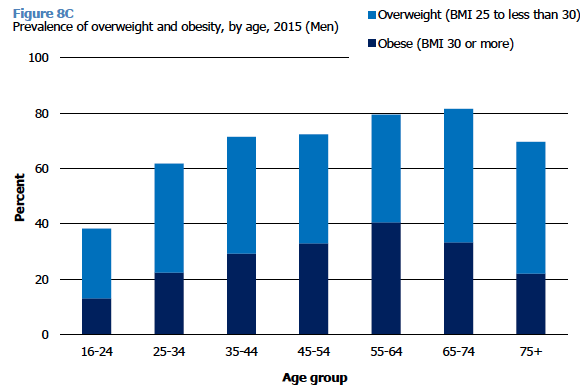
8.4 Waist Circumference And Disease Risk (Based On BMI And Waist Circumference)
8.4.1 Trends in mean and raised waist circumference since 1995
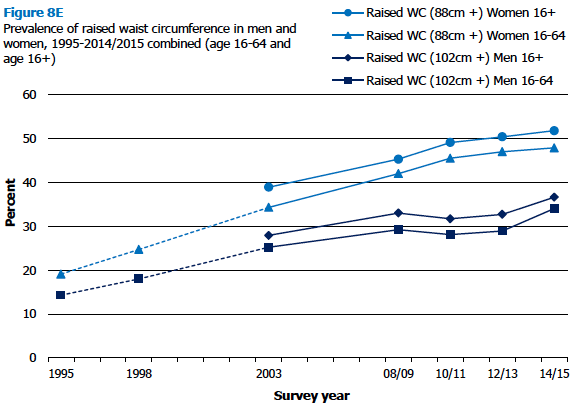
Waist circumferences were higher on average in 2014/2015 than in 2003 for those aged 16 and over (men: 98.2 cm in 2014/2015 and 95.3cm in 2003, women: 89.5 cm in 2014/2015 and 86.3 cm in 2003, using nurse equivalent measures). The longer trend for adults aged 16-64 shows a larger increase going back to 1995 for both groups.
The proportion of men aged 16 and over with a raised waist circumference (greater than 102cm) increased from 28% in 2003 to 37% in 2015. A similar pattern was evident for women in the same age group, albeit with a higher proportion being found to have a raised waist circumference of greater than 88cm (39% in 2003 compared with52% in 2014/2015). For both men and women, the trend for those aged 16‑64 shows further increases between 1995 and 2003.
Figure 8E, Table 8.3
8.4.2Health risk category associated with overweight and obesity based on Body Mass Index ( BMI) and waist circumference, 2014/2015 (combined)
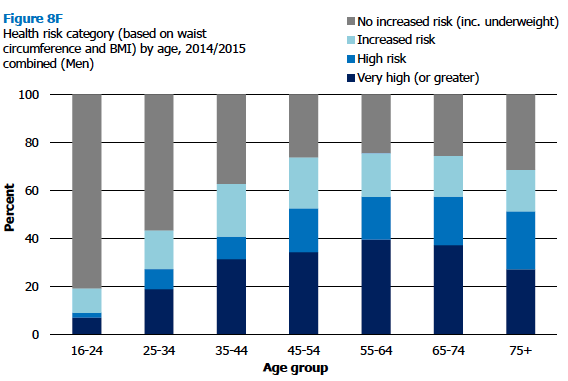
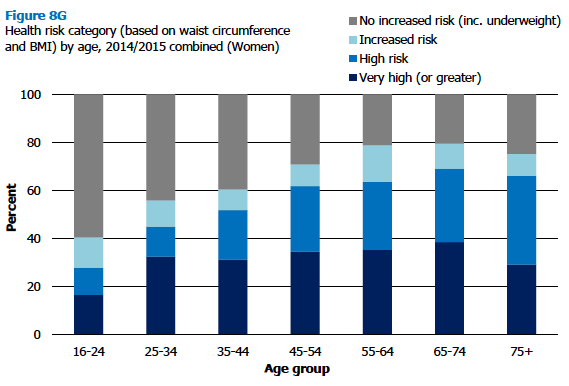
Around two-thirds of women (66%) and three in five men (59%) had at least an increased health risk based on their BMI and waist circumference in 2014/2015. Overall, 42% of men were categorised as being at high risk level or above, with 28% at very high risk level or above, and 3% at extremely high risk level. Equivalent figures for women were 55% at high risk level or above, 32% at very high risk level or above, and 4% at extremely high risk level.
Risk tended to increase with age for both men and women, until older age. Just under a tenth (9%) of men aged 16-24 were classified as being at high risk or above, with this rising to 51- 57% of those aged 45 and over. For women, 28% of those aged 16-24 were at high risk or above, rising 62-69% of those aged 65-74.
Figure 8F, Figure 8G, Table 8.4
8.5 Child Healthy Weight, Overweight And Obesity
8.5.1 Trends in child healthy weight, overweight and obesity prevalence since 1998
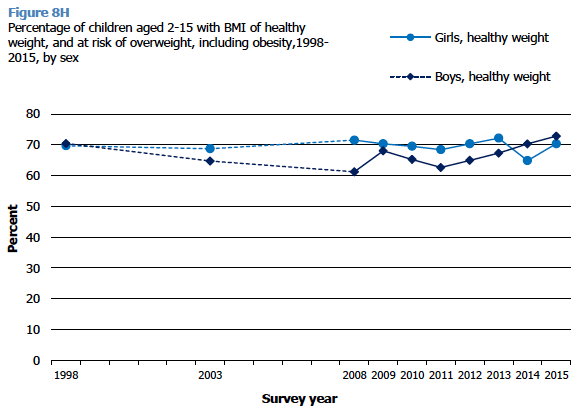
A child is described as being of a healthy weight if their BMI is above the 2 nd percentile and below the 85 th percentile of the UK 1990 reference curves. In 2015, 72% of all children aged 2-15 had a BMI within the healthy weight range, an increase from the low of 65% in 2011 and at a similar level to 1998 (70%).
Between 1998 and 2010 the proportion of boys aged 2-15 with a healthy weight fluctuated from 61-70% but since 2011 (63%) the figure has steadily risen up to the current figure of 73%.This is matched by the decline in the number of boys who are at risk of being overweight in the same period (from 36% in 2011 to 26% in 2015).
No clear pattern across time is evident for girls. The percentage of girls within the healthy weight range in 2015 (70%) is at a similar level to all survey years since 1998 (between 65% and 72%). With the exception of an unusually high figure in 2014 (34%), the proportion of girls at risk of overweight including obesity has not changed significantly over the years (29% in 2015, and between 27% and 30% in all other years from 1998 to 2013).
Figure 8H, Table 8.5
The percentage of boys and girls at risk of obesity ( BMI at or above the 95 th percentile of the UK 1990 references curves) has remained relatively consistent over time. In 2015, 14% of girls and 15% of boys were at risk of obesity, the same as the levels for each group in 1998 and not significant significantly different from any of the intervening years.
8.5.2 Child BMI categories in 2015, by age and sex
In 2015, more than 7 in every 10 children (72%) were of a healthy weight, 13% were at risk of being overweight (not including those at risk of obesity), and 15% were at risk of being obese. In total, 1% of children were underweight. There was no statistically significant difference between the proportion of boys (27%) and girls (30%) who were outwith the healthy range.
In 2015, differences in prevalence of risk of overweight and risk of obesity across the age groups were not statistically significant.
8.5.3 Child BMI categories in 2015, by parental BMI
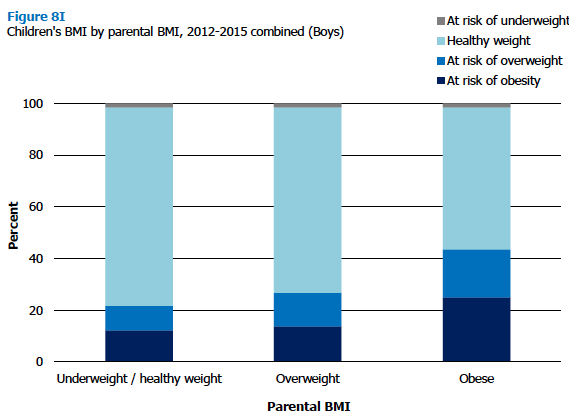
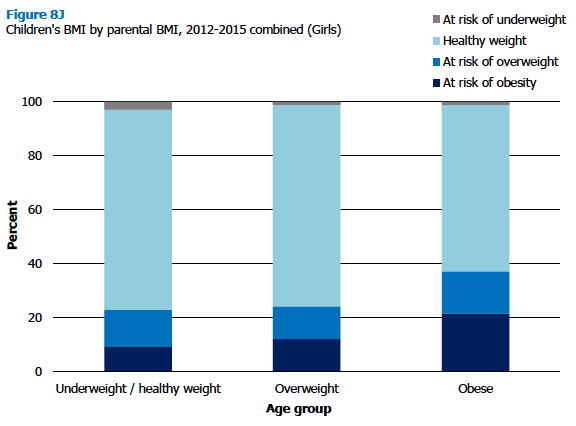
Children with at least one parent who was overweight (but not obese) were found to be statistically no more likely than children with parents of a healthy weight or underweight to be a healthy weight (73% and 76% respectively). However, this was not the case for children with a parent who is obese, with a significantly lower proportion (58%) of those children being a healthy weight.
Children with an obese parent were significantly more likely to be at risk of being overweight including obese (40%) than both those with an overweight parent (25%) and those with no overweight parent (22%). They were also significantly more likely to be at risk of being obese (23%, compared with 13% of those with an overweight parent and 11% of those with no overweight parent). Patterns were similar for both boys and girls.
Figure 8I, Figure 8J, Table 8.7
Contact
Email: Julie Landsberg, julie.landsberg@gov.scot