Family Nurse Partnership: 10 year analysis
To mark the first ten years of the Family Nurse Partnership in Scotland, we have undertaken a review of data from the programme over this time.
Section 2: Programme Delivery
Summary – Programme Delivery
- To gain most benefit from FNP, clients should be enrolled by 16 weeks and 6 days gestation. While around half (51%) of clients were enrolled by 16 weeks and 6 days overall, this is slightly lower than the benchmark of 60%. However, a higher proportion of clients have enrolled by 16 weeks and 6 days in recent years (56% in 2020-21). There is geographical variation in enrolment by 16 weeks and 6 days. Clients in the East of Scotland region were more likely than clients in other regions to enrol by 16 weeks.
- The majority (97%) of FNP clients enrol onto the programme prior to 28 weeks and 6 days. For those that enrol later this is usually due to late interaction with maternity services.
- Some FNP clients in Scotland are receiving fewer visits in each phase when compared to the set benchmarks. In the pregnancy phase 46% of graduates received their expected number of visits as per the standard schedule. In infancy phase, 60% of clients met the benchmark of 19 or more visits. In toddlerhood 57% of clients received 14 or more of expected visits.
- On average the benchmark of 60 minute visits for each phase was exceeded in every phase for clients who completed FNP, with visits lasting an average of 68 minutes in pregnancy, 62 minutes in infancy and 61 minutes in toddlerhood.
- The majority (80%) of FNP clients completed the programme and graduated. One in five (20%) left prior to graduation (attrition).
- Completion rates are similar across Scotland and have increased over the ten years of programme delivery. Completion rates were slightly higher for clients who lived in the most deprived (SIMD 1) areas (80%) at enrolment, compared to the least deprived (SIMD 5) areas (74%).
- The most common reasons for leaving the programme among the 1262 clients who left prior to completion (20%) were having no contact with the programme for 6 months (client inactivity - 463 clients), followed by moving out of the service area to an area where FNP is not offered (174 clients), and the client's child going into long term care (160 clients).
- There was some evidence of a correlation between the number of visits a client received in a given phase and likelihood of graduating, with those that graduated receving slightly more visits as per the standard visit schedule than those that did not.
- Of all planned scheduled visits, 77% were completed, 9% were attempted, 12% were cancelled by the FNP Client, and 1% were cancelled by the FNP Nurse.
Enrolment and Visit Data
Enrolment
There is a model for the delivery of FNP (Core Model Elements (CME)), some of which have associated national benchmarks that are set by the licence holder, the University of Colorado Denver, in conjunction with the delivering country. These benchmarks are also known as fidelity measures or stretch aims that are used as goals to drive continuous improvement. In Scotland, there is variation in achievement of the benchmarks.
There are benchmarks for the point of gestation at which clients should be enrolled on FNP to get the most benefit from the programme. These benchmarks state that 60% of clients should have enrolled before 16 weeks and 6 days gestation and 100% before 28 weeks and 6 days gestation.
However, following a review of enrolment data in early 2016, it became apparent that some of the most vulnerable potential clients were not presenting to maternity services until very late in the pregnancy journey (concealed pregnancy) and sometimes even at birth. Up to 2016, these potential clients would have been excluded from FNP due to the timing of their first interaction with maternity services, despite there often being a high level of need for this service. Following the review on eligiblity, a change to the enrolment criteria and agreement with the licence holder to alter the related benchmark was put in place for Scotland. This change allowed first time mothers, who would have ordinarily been eligible for the programme, to enrol onto FNP despite not being referred or enrolled prior to the 28 weeks and 6 days. Although small in number, this change will have implications for the data below.
Half (51%) of FNP clients enrolled onto the programme by 16 weeks and 6 days, falling short of the benchmark of 60%. However, almost all FNP graduates (97%) had received their first home visit by 28 weeks and 6 days, almost meeting the benchmark of 100%.
Clients in the East of Scotland were more likely than clients in other regions to enrol by 16 weeks and 6 days and 28 weeks and 6 days, with 57% and 99% enrolling by these time points respectively.
There was a reduction over time in clients enrolling by 16 weeks and 6 days between 2012-13 and 2017-18 (from 58% to 47%), followed by a subsequent increase for clients enrolling between 2018-19 to 2020-21 (from 47% to 56%).
Linked to the changes to the enrolment criteria, FNP clients in the most recent enrolment cohorts have been slightly less likely to enrol by 28 weeks and 6 days, when compared to earlier cohorts. While 99% of clients enrolled by this time point between 2011-2018, this had reduced to 95% between 2018-2021 to allow for later enrolment. Overall, a very small proportion of clients have been enrolled beyond 28 weeks and 6 days (3%).
There was a lower proportion of clients of Caribbean or Black ethnicity and clients of Asian, Asian Scottish, or Asian British ethnicity who had enrolled by 16 weeks and 6 days (42% and 44% respectively) though a similar proportion had enrolled by 28 weeks and 6 days (95% and 96% respectively). Clients who primarily spoke a language other than English and who required an interpreter were also less likely to have enrolled by 16 weeks and 6 days (34%) and 28 weeks and 6 days (86%).
Number of visits
The data on visits relates to those that completed the programme (graduates) as the data is incomplete for those that left the programme prior to completion.
As part of the programme materials and dosage requirements, there is set guidance on the number of visits that FNP clients should receive throughout the duration of the FNP programme, as per a standard visiting schedule. The standard visiting schedule is as follows:
- Weekly visits for the first four weeks upon initial enrolment prenatally, then every other week until delivery
- Weekly visits for six weeks after infant birth, followed by visits every other week until the baby is 21 months of age
- Monthly visits from 21 through 24 months of age.
The benchmarks state that all FNP clients should ideally receive at least 80% of scheduled visits in pregnancy, 65% in infancy and 60% in toddlerhood. For infancy, this equates to a benchmark of 19 visits, in Toddlerhood it equates to 14 visits. In pregnancy, the expected number of visits depends on the length of time the clients was enrolled before giving birth.
In the pregnancy phase, 46% of graduates received their expected number of visits as per the standard schedule, given the length of time they were enrolled before infant birth. In infancy phase, 60% of clients met the benchmark of 19 or more visits. In toddlerhood 57% of clients received 14 or more of expected visits as per the standard schedule of visits.
There was geographical variation in this, with a notably lower proportion of graduates from the West of Scotland reaching the benchmark number of visits in each phase (36% in pregnancy, 49% in infancy, and 51% in toddlerhood).
On average, FNP graduates received 10 visits during pregnancy, 19 during infancy and 14 during toddlerhood. As shown in table 4 below, younger FNP graduates had a marginally higher number of overall visits than the older age groups.
| Phase | Number of visits | |||
|---|---|---|---|---|
| Aged 17 and Under | Aged 18 to 19 | Aged 20 and Over | Benchmark | |
| Pregnancy | 10 | 10 | 9 | Dependant on client gestation at enrolment |
| Infancy | 20 | 19 | 19 | 19 |
| Toddlerhood | 14 | 14 | 14 | 14 |
Note: Data only included for those that completed the programme prior to 31 March 2021
The average number of visits received per phase was broadly similar across SIMD quintiles. FNP graduates in SIMD 1 (most deprived) at enrolment received, on average, 9 visits in pregnancy, 19 visits in infancy and 14 visits in toddlerhood. FNP graduates in SIMD 5 (least deprived) at enrolment received, on average, 10 visits in pregnancy, 19 visits in infancy and 14 visits in toddlerhood.
The average number of visits received by graduates was slightly less for clients in "African, African Scottish, or African British" and "Asian, Asian Scottish, or Asian British" ethnic groups, with these clients typically receiving one fewer visit per phase than graduates of "White" ethnicity. Also, clients who did not speak English as their primary language received, on average, one fewer visit in each phase than clients who did speak English as a first language at enrolment. This was consistent across regions of Scotland.
The number of visits received per phase varied somewhat between graduates. In pregnancy, the majority of graduates received either 6-10 visits (2379 graduates, 48%) or 11-15 visits (1959 graduates, 39%). However, a notable minority received less than 5 visits in pregnancy (579 graduates, 12%). There was a clear correlation between weeks gestation at enrolment and the number of visits clients received during pregnancy, with the majority of clients who enrolled later than 16 weeks and 6 days receiving less than 10 visits in this phase. There was also a higher proportion of graduates based in the West of Scotland who received less than 5 visits in pregnancy (18%).
The majority of graduates received at least 16 visits in the infancy phase (4052 graduates, 81%) and almost all received at least 11 visits (4833 graduates, 96.5%), as shown in table 5.
As show in table 6, in the toddlerhood phase the majority of graduates received either 11-15 visits (2097 graduates, 42%) or 16-20 visits (1469 graduates, 29%). There was a higher proportion of graduates receiving 10 or less visits in toddlerhood in the West of Scotland (28%) than nationally (22%).
| Phase | Average Number of Completed Visits | Benchmark | Proportion of Clients Reaching Benchmark |
|---|---|---|---|
| Pregnancy | 9.57 | Dependant on client gestation at enrolment | 46% |
| Infancy | 19.30 | 19 visits | 60% |
| Toddlerhood | 14.08 | 14 visits | 57% |
| Phase | Less Than 5 | 6-10 | 11-15 | 16-20 | More Than 20 |
|---|---|---|---|---|---|
| Pregnancy | 12% | 48% | 39% | 2% | 0% |
| Infancy | 1% | 3% | 16% | 43% | 38% |
| Toddlerhood | 3% | 19% | 42% | 29% | 7% |
Duration of Visit
The national benchmark for duration of visit at each phase is 60 minutes. On average, this benchmark was exceeded for every phase for clients who completed FNP, with visits lasting an average of 68 minutes in pregnancy, 62 minutes in infancy and 61 minutes in toddlerhood. Visit duration during pregnancy was slightly higher in the West of Scotland, averaging 69 minutes, perhaps reflecting the higher instances of later enrolment. Visit duration during toddlerhood was slightly lower in the North of Scotland, averaging 59 minutes.
When viewing average visit duration for graduates at the client level, however, there was wide variation in the average duration of visits received. In the pregnancy phase, the lowest average visit duration for a client was 30 minutes, while the highest was 150 minutes. In the infancy phase, the lowest average visit duration for a client was 32 minutes, while the highest was 108 minutes. In the toddlerhood phase, the lowest average visit duration for a client was 19 minutes, while the highest was 117 minutes.
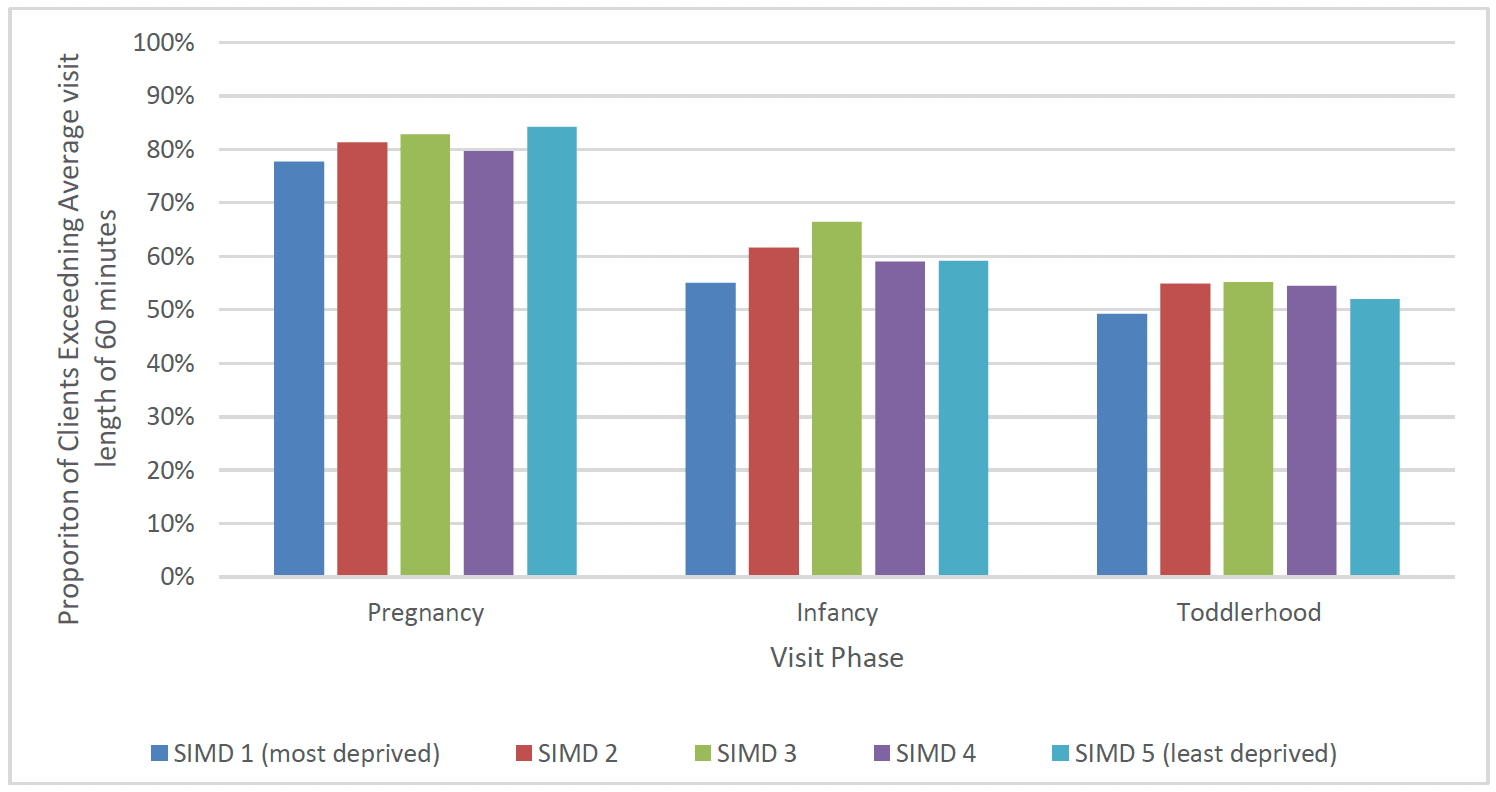
In the pregnancy phase, 80% of graduates had an average visit length at or exceeding the benchmark of 60 minutes. During the infancy phase, 59% of graduates had an average visit length exceeding the benchmark, as did 52% of graduates during the toddlerhood phase. Since the beginning of FNP, the vast majority of clients have had visits lasting at least 60 minutes during pregnancy. There has been a general pattern of increase in the proportion of clients with visits lasting at least 60 minutes during infancy and toddlerhood throughout implementation of FNP in Scotland.
Graduates from the least deprived areas (SIMD 5) were most likely to have an average visit length of at least 60 minutes during pregnancy. Clients from SIMD 3 were more likely to have an average visit length of at least 60 minutes during infancy and toddlerhood (Chart 12). A higher proportion of younger clients had visits exceeding 60 minutes in each phase of the programme – 66% of clients aged 17 and under had an overall average visit length exceeding 60 minutes, compared with 59% of clients aged 20 and over.
Reflecting on the earlier demographic findings where overall younger clients were more likely to have a higher number of complex needs, this is possibly reflected in the fact they received longer and more frequent visits overall. However, this was not necessarily reflected for clients living in more deprived areas overall, who were not more likely to receive longer or more frequent visits than other clients.
Composition of Visits
The composition of individual visits are broken down into 5 domains: Personal Health (My Health), Maternal Role (My Child and Me), Environmental Health (My Home), My Family & Friends (Family & Friends), Life Course Development (My Life). FNP nurses record how much time is spent on each domain per visit, as a proportion of the overall visit.
In the pregnancy phase, the benchmark for proportion of time spent on the My Health domain per visit is 35-40%. In infancy the benchmark for this domain is 14-20% and in toddlerhood it is 10-15%. Across FNP graduates, the average coverage of My Health fell within these benchmark ranges during pregnancy phase (35%) and infancy (20%), and slightly exceeded the benchmark in toddlerhood (17%).
In the pregnancy phase, the benchmark for proportion of time spent on the My Child and Me domain per visit is 23-25%. In infancy the benchmark for this domain is 45-50% and in toddlerhood it is 40-45%. Across FNP graduates, the average coverage of My Child and Me slightly exceeded the benchmark during pregnancy phase (28%), fell just short during infancy (44%), and met the benchmark in toddlerhood (41%).
In the pregnancy phase, the benchmark for proportion of time spent on the My Home domain per visit is 5-7%. In infancy the benchmark for this domain is 7-10% and in toddlerhood it is 7-10%. Across FNP graduates, the average coverage of My Home slightly exceeded the benchmark during pregnancy phase (10%), infancy (11%), and toddlerhood (12%).
In the pregnancy phase, the benchmark for proportion of time spent on the Family & Friends domain per visit is 10-15%. In infancy the benchmark for this domain is 10-15% and in toddlerhood it is 10-15%. Across FNP graduates, the average coverage of Family & Friends met the benchmark during pregnancy phase (15%), infancy (14%), and toddlerhood (14%).
In the pregnancy phase, the benchmark for proportion of time spent on the My Life domain per visit is 10-15%. In infancy the benchmark for this domain is 10-15% and in toddlerhood it is 18-20%. Across FNP graduates, the average coverage of My Life met the benchmark during pregnancy phase (12%) and infancy (12%), and fell just short during toddlerhood (15%), as show in Table 7.
| Domain | Pregnancy Benchmark (%) | Pregnancy actual (%) | Infancy benchmark (%) | Infancy actual (%) | Toddler benchmark (%) | Toddler actual (%) |
|---|---|---|---|---|---|---|
| Personal Health (My Health) | 35-40% | 35% | 14-20% | 20% | 10-15% | 17% |
| Maternal Role (My Child and Me) | 23-25% | 28% | 45-50% | 44% | 40-45% | 41% |
| Environmental Health (My Home) | 5-7% | 10% | 7-10% | 11% | 7-10% | 12% |
| My Family & Friends (Family & Friends) | 10-15% | 15% | 10-15% | 14% | 10-15% | 14% |
| Life Course Development (My Life) | 10-15% | 12% | 10-15% | 12% | 18-20% | 15% |
Completion of Visits
Data is also captured on planned scheduled visits that did not take place. Of all planned scheduled visits, 77% were completed, 9% were attempted, 12% were cancelled by the FNP Client, and 1% were cancelled by the FNP Nurse. A higher proportion of planned scheduled visits during pregnancy and infancy (80%) were completed, when compared to planned scheduled visits during toddlerhood (72%). This was due to a higher proportion of attempted visits that were not completed and a higher proportion of visits cancelled by FNP clients during toddlerhood phase.
Programme Completion and Attrition
The majority (80%) of the 6,268 clients on the FNP programme to 31 March 2021 completed the programme and graduated. One in five (20%) left prior to graduation (attrition).
Graduation
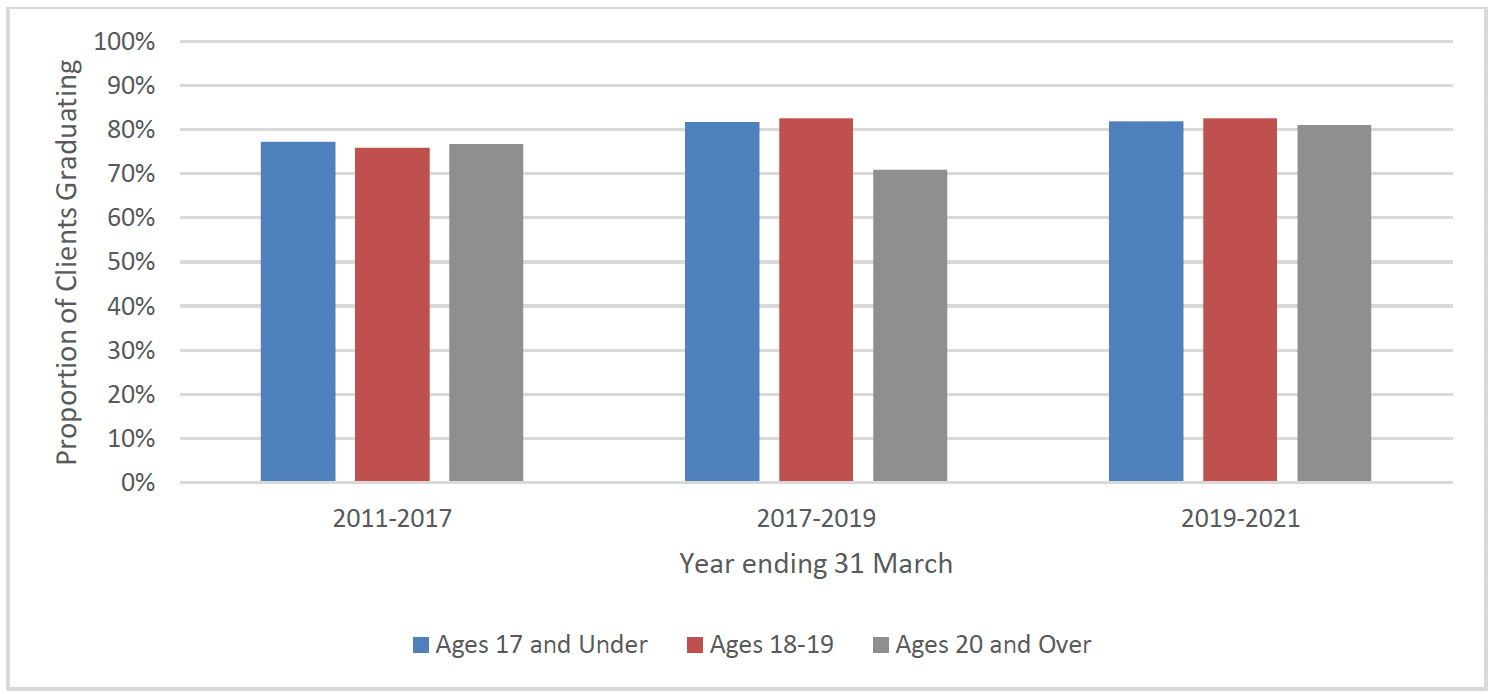
The rate of clients completing the programme was consistent across the regions of Scotland (East 79%, North 80% and West 81%). Completion rates have marginally increased over the years, from 77% completion in 2010-2017 to 81% in 2017-19 to 82% in 2019-21. Completion rates were also largely similar across client age groups (80% aged 17, 80% aged 18-19 and 78% aged 20 and over) as shown in Chart 13.
As shown in Chart 14 below, completion rates were slightly higher for clients who lived in the more deprived areas at enrolment compared to less deprived.
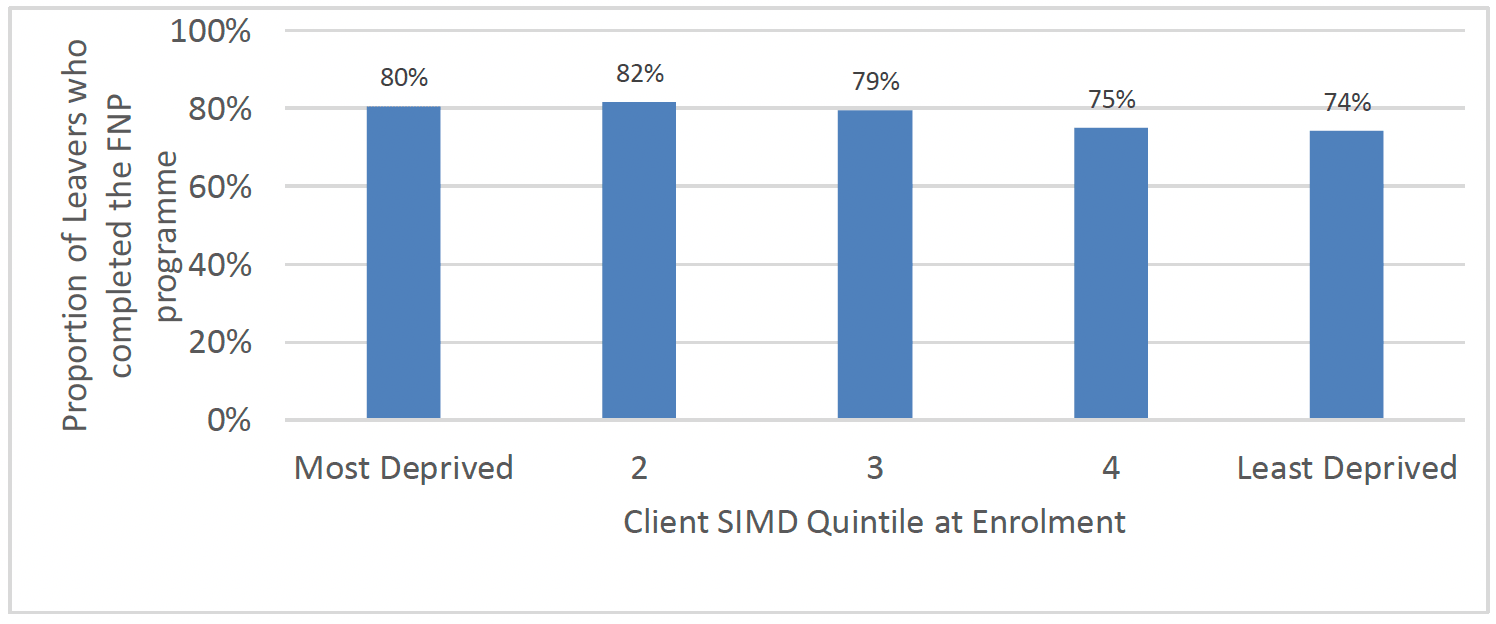
When a client leaves the programme prior to their child turning two years old it is classed as 'attrition', as they did not stay on the programme until graduation. Therefore clients that do not graduate from the programme are included in the attrition rates. Overall around 20% of clients leave by attrition each year, with attrition rates decreasing slightly in more recent years.
In general, clients from more deprived areas were less likely to leave by attrition, and younger clients were slightly less likely to leave by attrition. The client group with the lowest attrition rate was those clients aged 17 and under in SIMD 2, with 17% attrition. Conversely, the client group with the highest attrition rates (33%) were clients in SIMD 5 (least deprived) in the youngest age group (17 and under). (Table 8).
| Deprivation quintile | Age of client at enrolment to FNP | |||||||
|---|---|---|---|---|---|---|---|---|
| Aged 17 and Under attrition | Aged 18 to 19 attrition | Aged 20 and Over attrition | Total attrition | |||||
| SIMD 1 (Most Deprived) | 187 | 20% | 277 | 19% | 78 | 21% | 542 | 20% |
| SIMD 2 | 97 | 17% | 167 | 18% | 49 | 22% | 313 | 18% |
| SIMD 3 | 59 | 22% | 104 | 20% | 26 | 21% | 189 | 21% |
| SIMD 4 | 37 | 24% | 78 | 25% | 23 | 28% | 138 | 25% |
| SIMD 5 (Least Deprived) | 25 | 33% | 42 | 25% | 10 | 20% | 77 | 26% |
| Total | 405 | 20% | 668 | 20% | 186 | 22% | 1262 | 20% |
Of the 1262 clients who left through attrition, 468 left during pregnancy (7% of all clients who have completed or left FNP) , 411 (7%) left during infancy (the client's child was less than 1 year old) and 383 (6%) left during toddlerhood (the client's child was between 1 and 2 years old), and this was broadly consistent across geographical regions of Scotland. For each phase, the national benchmarks for attrition of 40% or less across the programme consisting 10% in pregnancy 20% in infancy and 10% in toddlerhood were met consistently in each part of Scotland. Attrition during pregnancy and infancy has decreased throughout implementation and attrition during toddlerhood has been consistently low.
The phase in which clients left the programme was largely consistent across regions of Scotland. The higher overall rate of attrition in the earlier years of FNP (2010-2017) is largely explained by attrition during pregnancy, with 10% of all clients leaving FNP in these years doing so during pregnancy, compared to 6% in 2017-19 and 6% in 2019-21.
Clients aged 17 and under at enrolment were slightly less likely to leave during pregnancy (6%), compared with other age groups (8% aged 18-19 years and 9% aged 20 and over).
Clients living in the least deprived areas (SIMD 5) had slightly higher overall attrition rates and were more likely than other groups to leave the programme during pregnancy. 10% in SIMD 5 left in pregnancy, compared to 8% in SIMD 1 and 6% in SIMD 2.
Reasons for Leaving the FNP Programme
The most common reasons for leaving the programme among the 1262 clients who left through attrition were: having no contact with the programme for 6 months (client inactivity), with 443 clients having this stated as their leaving reason (35%), followed by moving out of the service area to an area where FNP is not offered (174 clients, 14%) and the client's child going into long term care (160 clients, 13%). A further 214 clients who left the programme before completion had a reason coded as "other" (17%). Table 9 outlines the reasons why clients left the FNP Programme.
| Reason | Number of Clients | Proportion (of clients leaving through attrition) |
|---|---|---|
| Client Left Programme Voluntarily | ||
| Client has had no contact with programme for 6 months (client inactive) | 443 | 35% |
| Too much commitment | 50 | 4% |
| Strong friend/family support | 20 | 2% |
| Did not accept change of family nurse | 7 | 1% |
| Father is the main carer of the child | * | *% |
| Other | 214 | 17% |
| Social Work Involvement | ||
| Child into long term care | 160 | 13% |
| Parental rights terminated | 16 | 1% |
| Miscarriage/Termination/Stillbirth/Death | ||
| Miscarriage | 36 | 3% |
| Still birth (greater than 26 weeks gestation) | 33 | 3% |
| Neonatal death (i.e. death in first four weeks of life) | 20 | 2% |
| Infant death (i.e. death in the first year of life) | 19 | 2% |
| Termination | 17 | 1% |
| Maternal death | * | *% |
| Transfers | ||
| Client has transferred to FNP site outside Scotland | 40 | 3% |
| Client has moved out of service area | 174 | 14% |
Note: * indicates number supressed due to small numbers.
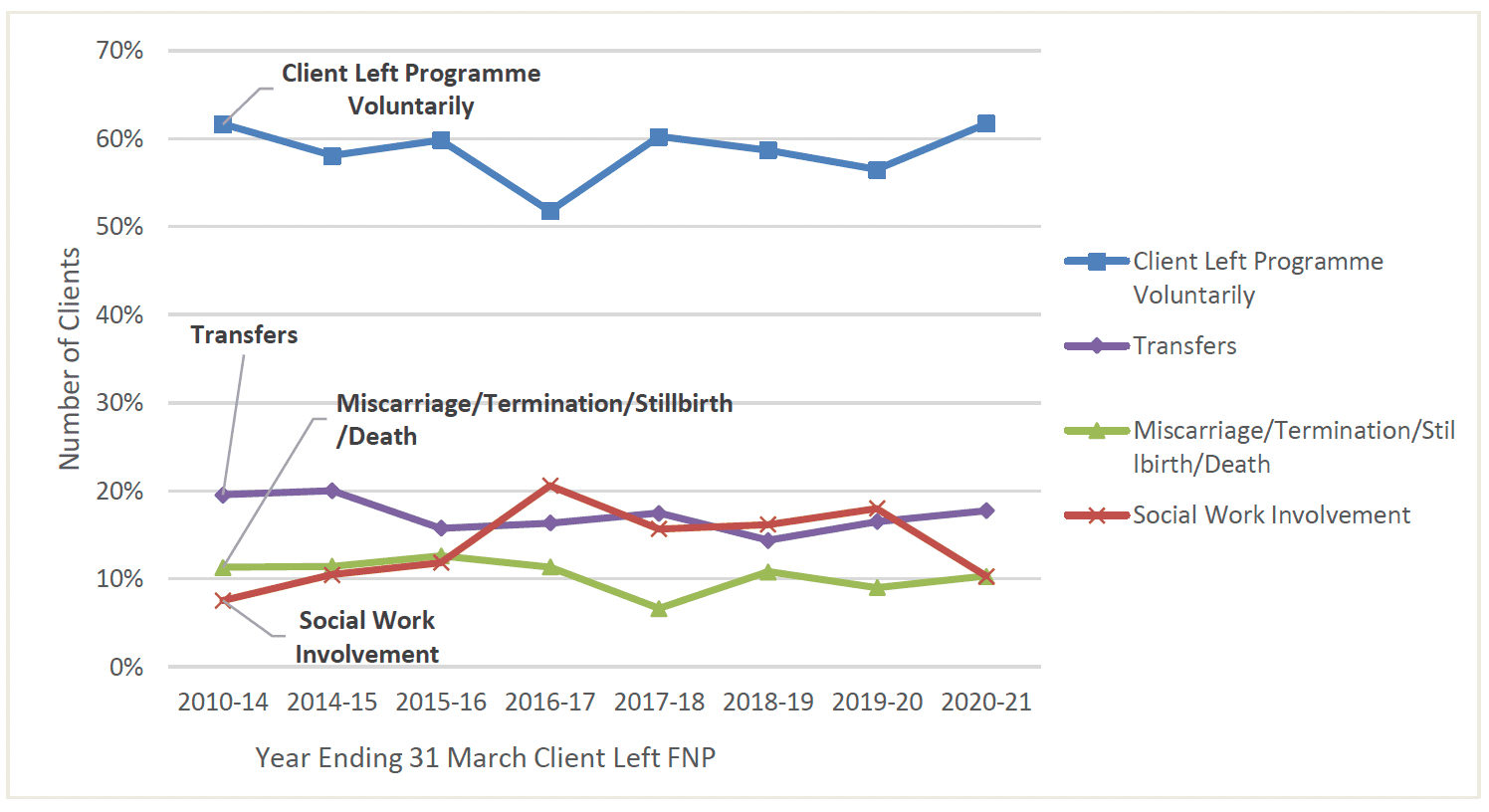
When looking at the different reasons for attrition, (Chart 15), many of the reasons for leaving the programme are due to extenuating circumstances. The proportion leaving that move to an area that does not provide FNP accounts for 17% of all leavers. While miscarriage/termination/stillbirth/death accounts for 11% of all leavers and removal of the child or parental rights accounts for 14%.
After accounting for the reasons mentioned above, overall 41% of attrition is due to these extenuating circumstances, while 59% opt to voluntarily leave the programme.
Voluntarily Leaving FNP
When comparing the group of clients who left the programme voluntarily with those who either left for other reasons or completed the programme, there was a slightly higher proportion of clients who left the programme voluntarily from the least deprived areas (SIMD 5) (18%) than those who did not leave voluntarily(13%). There was also a slightly higher proportion of clients who left voluntarily who were aged 20 and over (17%) than does who did not leave voluntarily (13%). There was a slightly lower proportion of clients who left voluntarily who had enrolled onto FNP by 16 weeks gestation (45%) than those who did not leave voluntarily (50%).
A slightly lower proportion of clients who left voluntarily lived with a partner upon leaving the programme (23%) compared to those who did not leave voluntarily (27%). A slightly higher proportion of clients who left voluntarily were either in full-time education or employment (43%), compared to 39% of those who did not leave voluntarily. A lower proportion of those who left voluntarily were in local authority or housing association housing (52%) compared to those who did not leave voluntarily (65%), with a higher proporiton of those who left voluntarily in privately owned accomodation (16% vs 8%).
Attrition due to Child Entering Long Term Care
Of the 160 clients leaving the programme due to the child entering long term care, 44% (71 clients) left during infancy and 56% (89 clients) left during toddlerhood. Almost one in five clients in the North region who left by attrition left for this reason (18%, 61 clients), compared with one in ten in the East (11%, 53 clients) and West (10%, 46 clients).
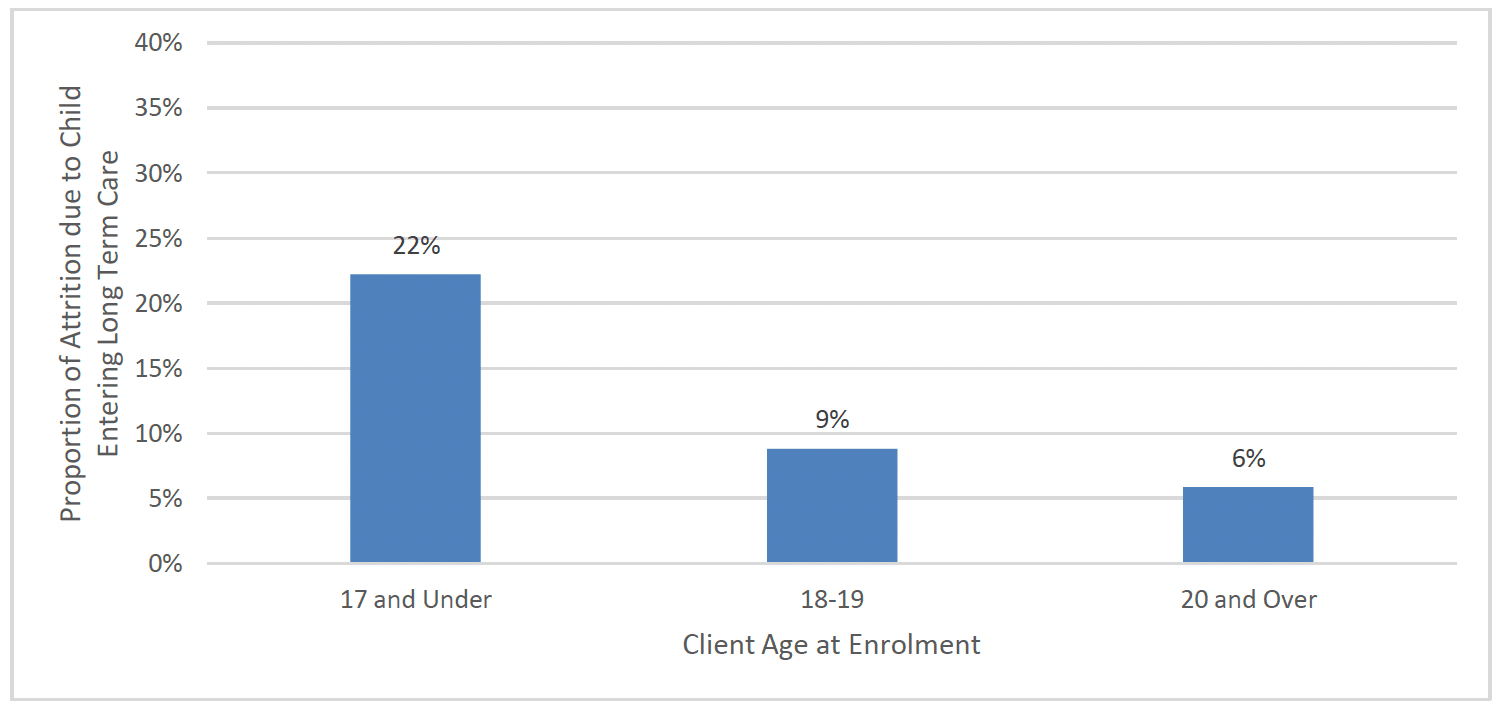
As shown in Chart 16 below, clients aged 17 and under at enrolment were more likely than older clients to leave due to their child entering long term care. Of those that left, over one in five (22%, 90 clients) aged 17 and under left due to their child going into long term care. There was no clear correlation between attrition due to the child going into long term care over time or SIMD quintile.
Miscarriages (8%), still births (7%), and termination of pregnancies (4%) accounted for some of the clients who left the programme during the pregnancy phase.
Visits and Attrition
There was some evidence of a correlation between the number of visits a client received in a given phase and likelihood of graduating. For example, clients who left FNP in the infancy phase received, on average, 8 visits in preceding phase (pregnancy), compared to an average of 10 visits among those who went on to graduate. Clients who left FNP in the toddlerhood phase received, on average, 9 visits in pregnancy and 18 visits in infancy, whereas those who went on to graduate received 10 visits in pregnancy and 19 visits in infancy.
The difference in the number of completed visits between clients who went on to graduate and those who did not appears to be due to a higher rate of completion of scheduled visits in this group, as opposed to a higher number of scheduled visits overall. Clients who went on to graduate completed 77% of scheduled visits, with 12% cancelled by the client, 9% attempted and 1% cancelled by the nurse. Clients who left by attrition completed 72% of scheduled visits, with 14% cancelled by the client, 13% attempted and 1% cancelled by the nurse.
Clients enrolling after 28 weeks and 6 days gestation also had slightly lower graduation rates than clients who enrolled prior to 16 weeks and 6 days gestation (77% compared with 81%), with more than double the rate of clients in the former group leaving during infancy (13% vs 6%), though it should be noted that the total number enrolling after 28 weeks was low, with only 53 clients in this group.
The same pattern was not found for average visit duration – with the average visit duration for graduates similar to or slightly less than clients who left the programme by attrition. For example, graduates received visits averaging 68 minutes in pregnancy, whereas clients who left the programme in toddlerhood had visits averaging 70 minutes long in pregnancy.
Contact
Email: Justine.Menzies@gov.scot