Family Nurse Partnership: 10 year analysis
To mark the first ten years of the Family Nurse Partnership in Scotland, we have undertaken a review of data from the programme over this time.
Section 1: Intake and Client Characteristics
Summary – Intake and Client Characteristics
- At a national level, there has been a substantial decline in the pregnancy and birth rate among younger mothers over the last 10 years.
- The number of first time births to mothers aged 19 and under in Scotland is now a third of what it was when FNP was first delivered in 2010. The geographical pattern of decline has changed the profile of younger mothers in Scotland with the majority (73%) now within the most deprived (SIMD 1 and 2) areas.
- Young women under 20 years old in the most deprived areas of Scotland are 13 times more likely to have a pregnancy that results in delivery compared to those in the least deprived areas.
- Evidence suggests that young mothers aged 20-25 years can face similar circumstances to young mothers aged under 20[24]. This evidence highlighted the importance of FNP accepting some clients aged 20-24 at enrolment,with some additional criteria. This is being trialled in some Health Boards in Scotland.
- From 2018/19 onwards, around 80% of all first time mothers aged 19 and under in Scotland voluntarily enrol onto FNP.
- Overall, just under a third (30%) of clients enrolling onto FNP were aged 17 or under at the time of enrolment. The majority (54%) were aged 18 to 19 and a sixth (16%) were aged 20 and older[iv].
- There has been a decrease in the proportion of clients aged 17 and under and an increase in those aged 18-24 years over the 10 years of delivery of FNP, in line with the decrease in births to younger mothers.
- The majority of FNP clients were of white origin (96%) and a small proportion (4%) of FNP clients were of a non-white ethnic group, similar to the proportions indicated in Scottish Maternity records.
- The Scottish statistics for attainment[25] show that the average qualification attainment for school leavers in Scotland is much higher than that seen among FNP clients.
- Analysis completed in 2018 has shown that almost all FNP clients (98%) had experienced some form of trauma or adverse experience in their lives before enrolling onto FNP. The most prevalent complexities for FNP clients at entry to FNP were; anxiety or other mental health issues (63%), experience of parental separation (63%), low income (60%), not being in work, education or training (57%). Over a fifth (22%) of FNP clients were care experienced or on the child protection register.


Pregnancy in Scotland
Pregnancy at an early age can be positive for some young people. It can be a planned choice and a new beginning. For others, it can increase the likelihood of poverty and reduce or compromise life chances, and this cycle can then repeat from one generation to the next[26]. Evidence shows that having a pregnancy at a young age can contribute to a cycle of poor health and poverty as a result of associated socio-economic circumstances before and after pregnancy (as opposed to the biological effects of young maternal age).
Pregnancy in young women is often a cause and a consequence of social exclusion and should not been seen narrowly as a health challenge[27]. The Institute of Fiscal Studies concluded that to significantly reduce levels of teenage pregnancy you cannot concentrate on high risk groups alone; a proportionate universalism approach is needed to ensure the needs of all young people are met. Universal services, across all agencies, have an important role to play in identifying and supporting the needs of young people[28].
Over the past ten years the rate of pregnancy (defined as all conceptions i.e. live births and terminations) in young people in Scotland have been reducing consistently. However, it is still high compared to other comparable western countries[29]. Between 2010 and 2019, Scotland experienced a reduction in the number of pregnancies in young people under 20 years of age, from 7,933 annual pregnancies to 3,814. However, as shown in Chart 1, young women from the most deprived areas are much more likely to experience a teenage pregnancy. The data shows that young people living in the most deprived areas are 4.5 times more likely to experience a pregnancy in Scotland, compared to those in the least deprived areas[30].
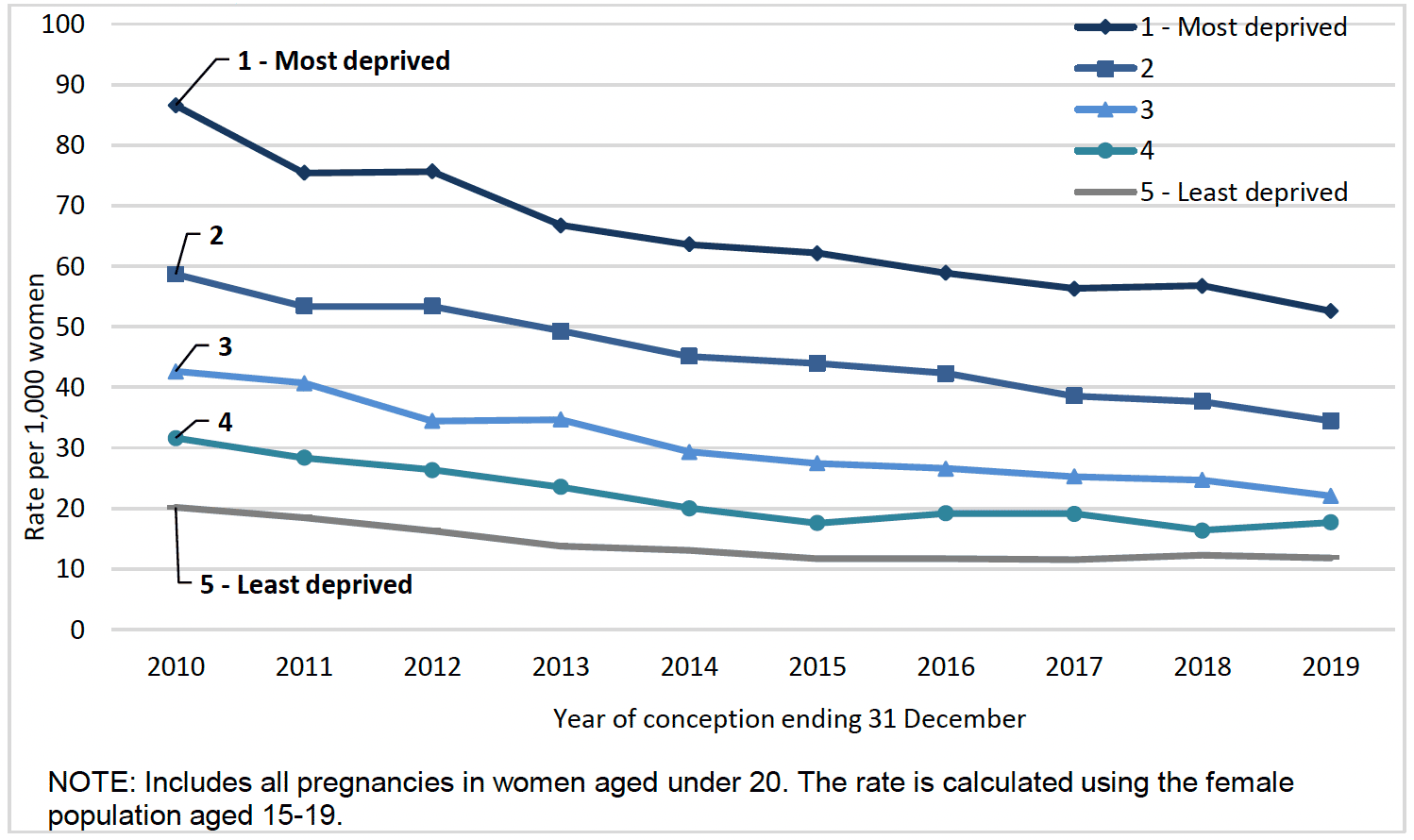
Births to Younger Mothers
The average age at which women have their first baby in Scotland has been gradually increasing[3]. The trend of increasing maternal age is seen both when looking at first births exclusively, and all births. In 2020-21 the proportion of women giving birth that were aged 35 years and over was the highest recorded at 23.4% of all births and the proportion aged under 20 was the lowest recorded at 2.6%[31]. The number of young people giving birth to their first child aged under 20 was 2752 in 2011-12. This had decreased by almost two-thirds to 1,017 first time births in 2020-21 as shown in Chart 2.
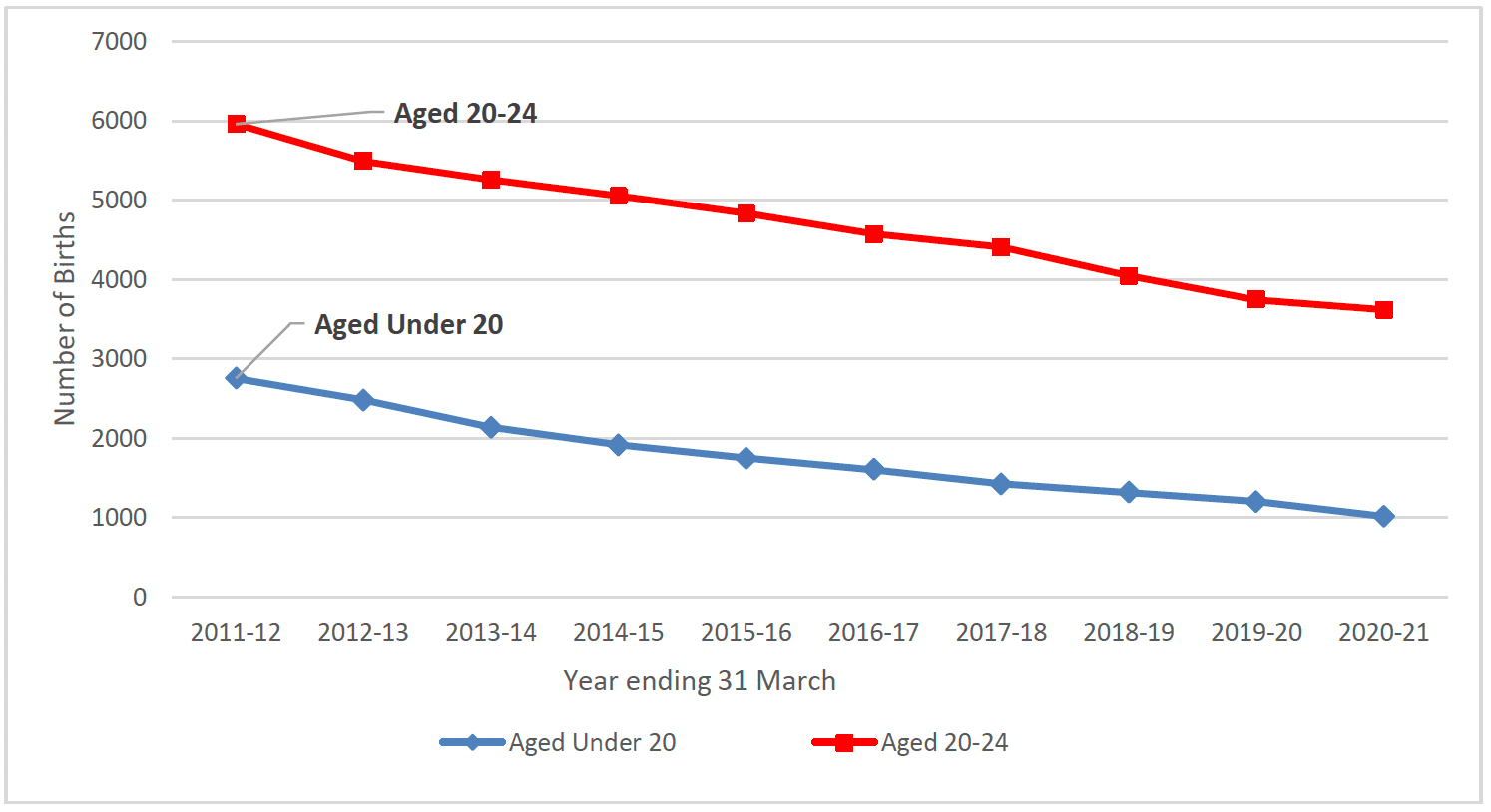
There is also a deprivation divide. The most common maternal age at first birth is substantially lower in the most deprived areas, at 21 years compared to 32 years in the least deprived[32]. Young women in the most deprived areas of Scotland are more likely to have a pregnancy and they are also more likely to continue on with pregnancy and give birth. The vast majority of births to younger mothers are concentrated amongst those that live in the areas with the highest levels of deprivation as measured by Scottish Index of Multiple Deprivation (SIMD)[v] as highlighted in Chart 3 below.
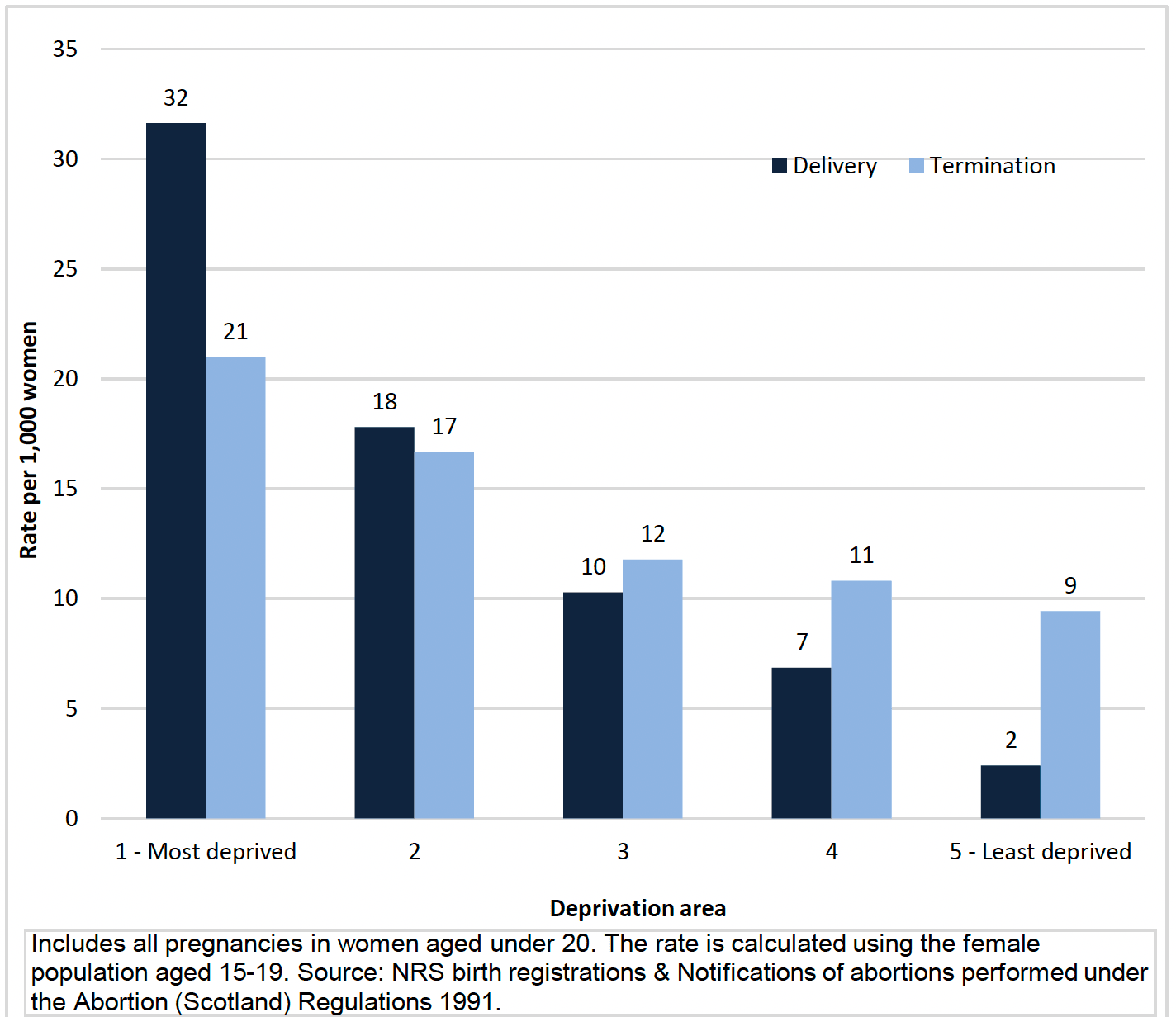
Young women in the most deprived areas are 13 times more likely overall to have a pregnancy that results in delivery than those in the least deprived areas[33]. This difference is even higher than when FNP began in Scotland, and makes it important to consider and understand FNP clients in terms of how client characteristics have changed over the 10 years of service provision.
Young mothers and babies in Scotland who live in the most deprived areas can face a range of health issues as well as socioeconomic disadvantages. The births in Scottish hospitals statistics show that in 2020-21, young mothers (aged under 25) living in the most deprived areas (SIMD 1) were more likely than those in the least deprived areas to be underweight, but also more likely to be overweight or obese. Almost a third (31%) of young mothers in deprived areas smoked at the time of their antenatal booking, which is more than double the rate for all mothers in Scotland (13%). More than one in ten (12%) babies born to young mothers living in deprived areas required extra neonatal care at birth, which is almost double the rate of babies born to young mothers living in the least deprived areas (7.8%). This highlights the complexity of the challenges faced by young mothers – both in terms of health behaviors and outcomes – particularly those from more deprived backgrounds.
Intake to FNP
FNP commenced in Scotland in 2010 with 6 family nurses, 1 supervisor, 1 data manager and a cohort of 148 clients. Following implementation, there has been a national programme of expansion to build towards FNP becoming a universally offered service in mainland Scotland. This was achieved in 2018. FNP is a voluntary programme, all young people aged 19 and under that become pregnant and plan to proceed with their pregnacy in NHS Boards that deliver FNP[vi] are offered a place on the programme. As at 31st March 2021 there were 2,909 active clients in Scotland.
The recruitment and training of FNP staff has run in parallel with the national roll out of the programme and as at 31st March 2021 there were:
- 182.45 whole time equivalent (WTE) Family Nurses
- 32.6 WTE Family Nurse Supervisors
- 25.41 WTE Data managers
- 19.93 WTE Admin staff
One of the measures within FNP is the percentage of eligible women that choose to enrol onto the programme. The international benchmark is 75%. In Scotland this has always been exceeded with approximately eight in ten (80%) of those offered the programme deciding to participate.
Currently, little is known about those that opt not to take up the offer of a place on the FNP programme. While details of all young mothers are held centrally in Scottish maternity and birth records, the Turas FNP system does not capture data on young mothers that are not FNP clients. While some local areas capture data locally this is not systematic.
Eligible young mothers who choose not to take up the offer of FNP will continue to receive usual care, through the universally offered maternity and health visiting services.
The majority of young women that enter the programme stay on until their child reaches age two, at which point they graduate from the programme and are transferred to the Health Visiting Service. If a client leaves the programme early, then they will automatically be transferred to the Health Visiting Service at that point, ensuring they can continue to access the care and support they may need.
Between 21 July 2011 and 31 March 2021[vii], 9177 FNP clients had enrolled onto the FNP programme. Of these clients, 5006 (55%) had graduated from the programme, 1262 (14%) had left before graduating (attrition), and 2909 (32%) were still active FNP clients as at 31st March 2021.
As shown in Chart 4 below, the number of clients joining FNP increased each year from 175 clients joining in 2011-12 to 1372 clients joining in 2018-19. This is due to the roll out of the programme across Scotland. Between 2018-19 and 2019-21, the number of FNP clients enrolling each year has become relatively stable at around 1300 annually, as it has become a continuous programme across NHS boards. The regions of Scotland[viii] rolled out the programme at different times and the scale up of the programme can be seen in the Chart 4 below.
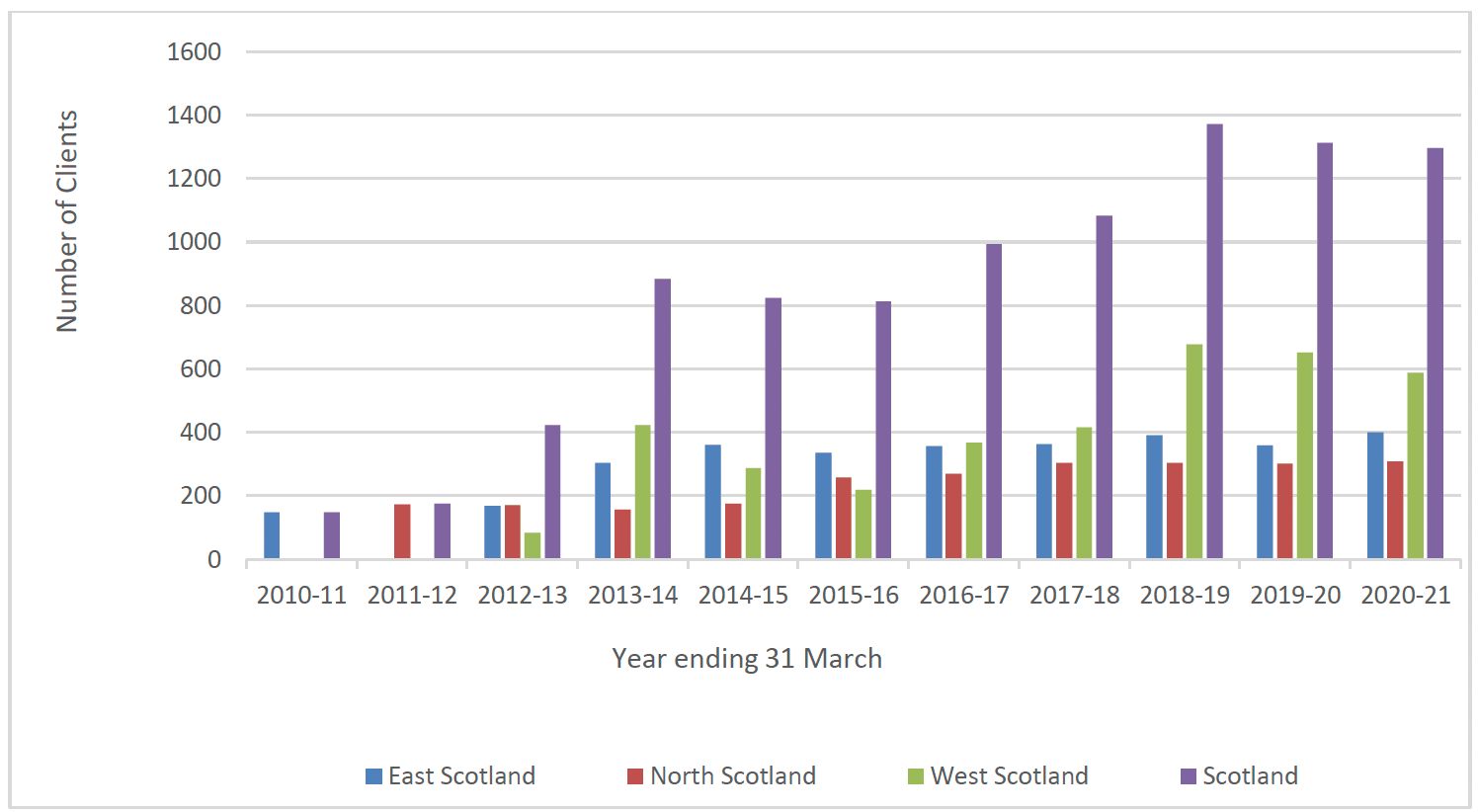
NOTE: Data from the Pilot site in NHS Lothian is included (2010/2011). Health Boards are grouped as follows (North Scotland – NHS Grampian, Highland, NHS Tayside), (East Scotland – NHS Borders, NHS Forth Valley, NHS Lothian, NHS Fife), (West Scotland – NHS Ayrshire and Arran, NHS Dumfries & Galloway, NHS Greater Glasgow and Clyde, NHS Lanarkshire)
Client Characteristics
In this section, the characteristics of clients are explored further, and compared with relevant comparator groups such as first time mothers under 20 years old.
Age
At the commencement of the FNP programme in Scotland, young people aged 19 or under having their first child were the eligible client group for FNP. However, in recognition of the similar poorer outcomes[34] for older mothers up to 25, the eligibility criteria was extended in 2016 to target some 20-24 year old first time mothers with additional needs. Alongside this deepening understanding of the client groups that would most benefit from FNP, the reduction in births to younger mothers (under 20 years) meant that some FNP teams had capacity to test the FNP programme with mothers aged 20-24 years.
This has not yet been consistently rolled out across Scotland, with areas testing slightly different approaches. The majority of 20-24 year old clients have been recruited in NHS Tayside and NHS Lothian. There have also been small numbers in NHS Ayrshire and Arran, NHS Grampian, NHS Borders and Highland.
There is a developing evidence base for expanding the FNP offer to other groups based not only on age, but also on other characteristics. Internationally, there are targeted client groups relevant to individual countries[ix], including in:
- Australia - the programme is adapted specifically for women pregnant with an Aboriginal and/or Torres Strait Islander baby; there is no age criteria.
- Bulgaria - the programme is predominately aimed at first time mothers from the Roma community under the age of 22 years.
- Norway - the programme is offered to first parents with complex challenges based on fulfilling two or more criteria from a ten point inclusion criteria; they have only a small number of younger mothers and no age criteria.
This provides further evidence that the FNP programme has been adapted to the local context, and that this can be achieved in Scotland if the groups that would benefit most from the programme are effectively targeted.
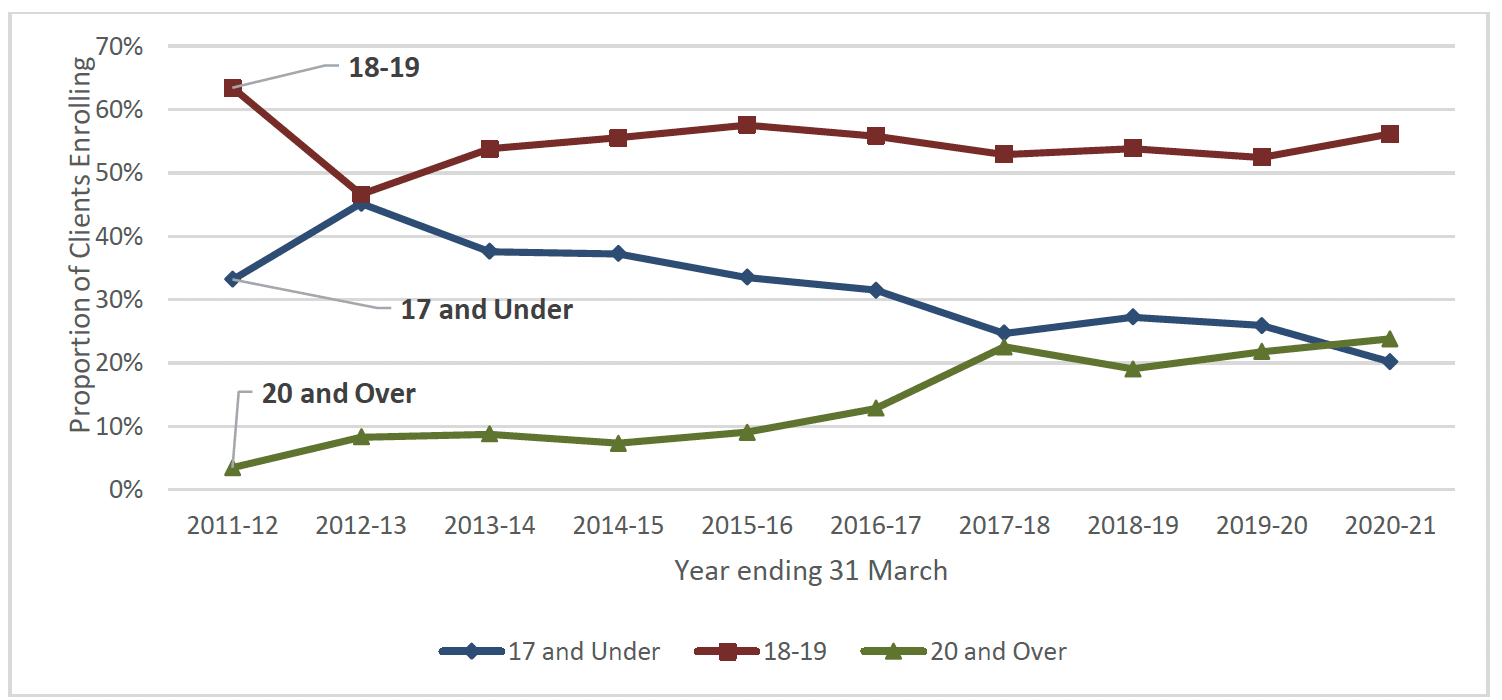
In Scotland, over the ten years of the programme just under a third (30%) of clients enrolling onto FNP were aged 17 or under at the time of enrolment. The majority (54%) were aged 18 to 19 and 16% were aged 20 and older[x]. As shown in Chart 5, the age composition of the FNP client group has changed somewhat over time. The most common ages at enrolment have typically been 18 or 19 years old, and there has been an increasing proportion of clients aged 20 and over. Over time, there has been a gradual reduction in the proportion of the FNP client group aged 17 and under, though there is still a sizeable proportion of clients aged 16 or 17 at enrolment. Although clients aged 15 and under make up a relatively small proportion of the overall FNP client group, around 25 to 50 clients in this age group enrol every year.
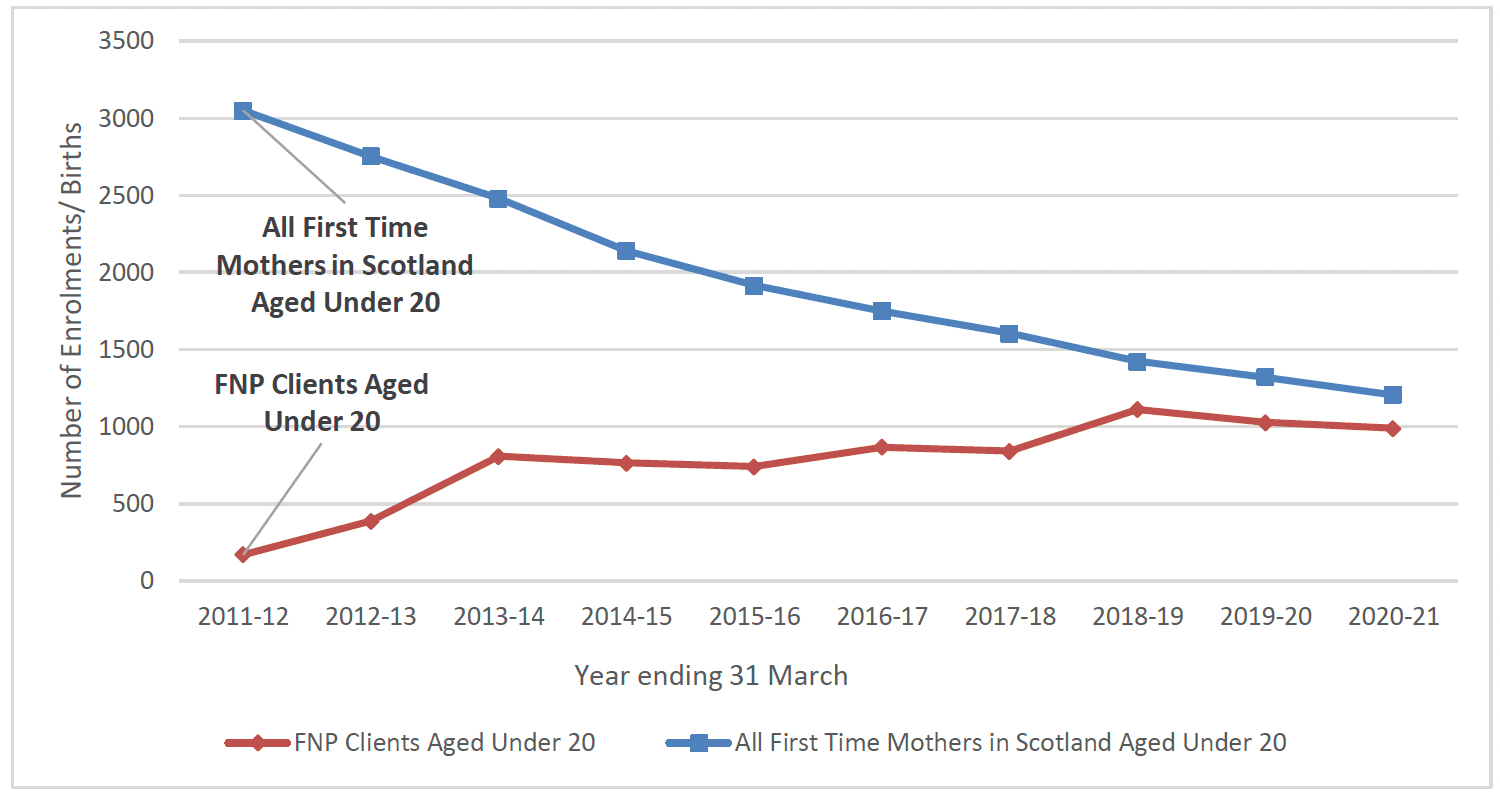
As shown in the Chart 6 below, the coverage of FNP has increased each year with coverage for the 19 and under age group increasing as the roll out of the programme progressed. By 2018/19, when FNP became available in all mainland NHS Boards, there were 1,423 births to mothers aged 19 and under and 1,111 enrolments onto FNP which indicates a 78% enrolment rate, in 2020/21 the enrolment rate has increased to 83%.
Deprivation
The majority of FNP clients (71%) are from the most deprived areas of Scotland (SIMD 1 and 2) upon entry to the programme. This reflects the evidence above, with those in more deprived areas more likely to continue with their pregnancy.
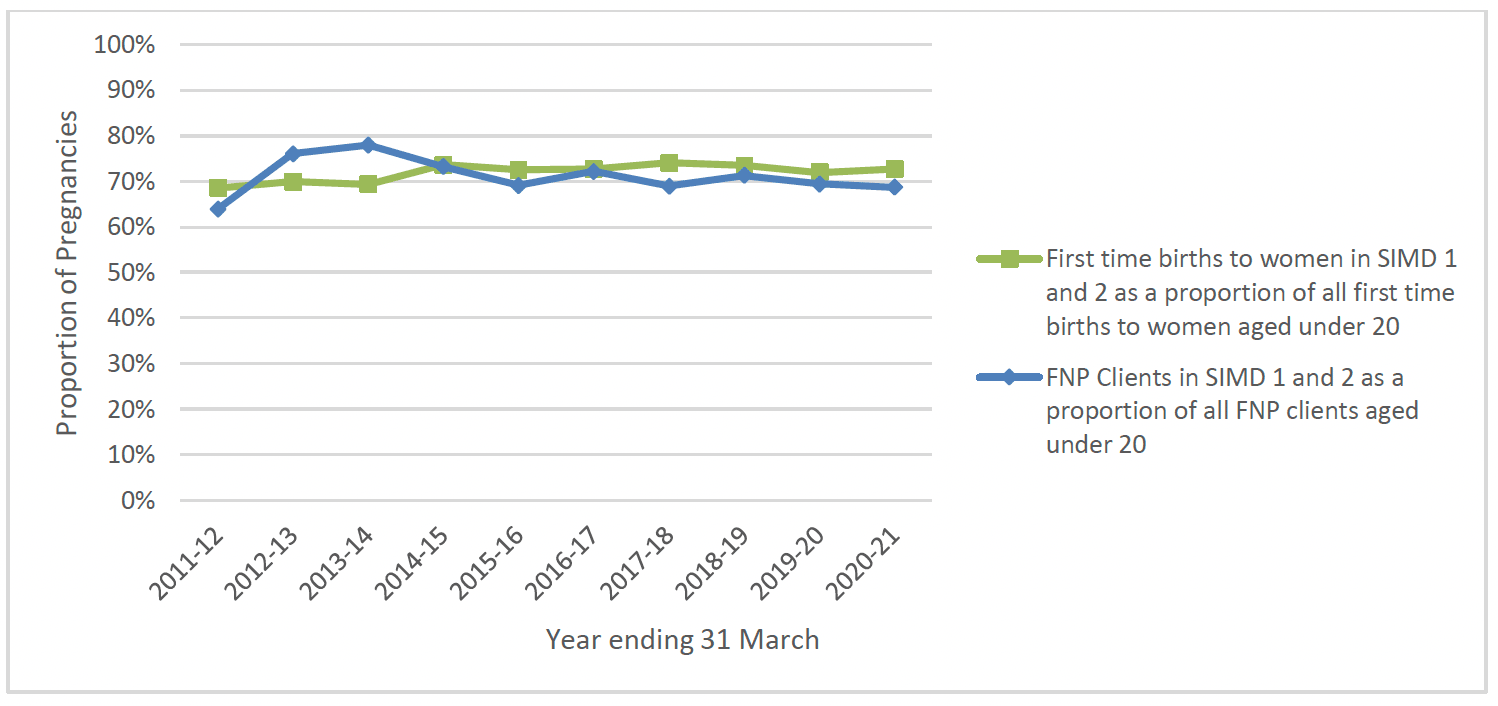
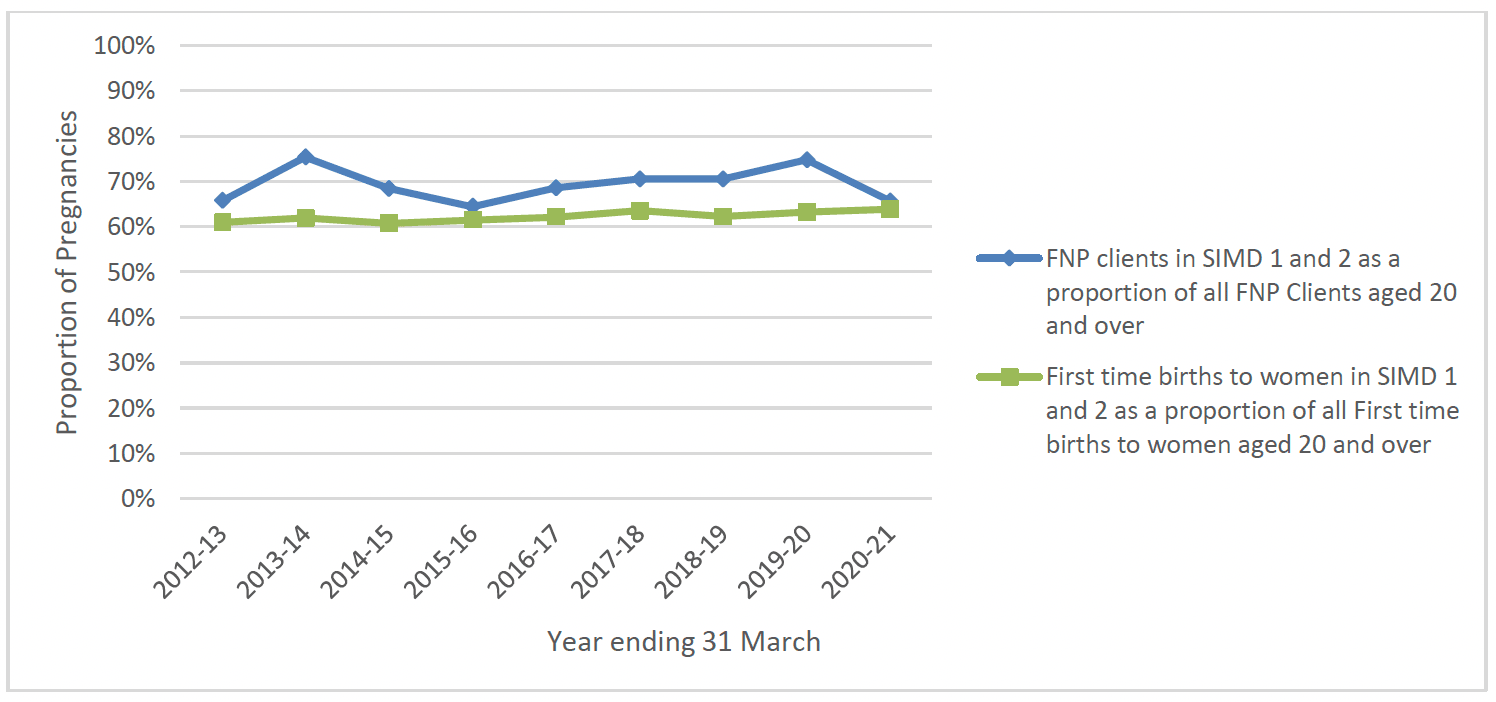
As shown in Chart 7 below, the proportion of FNP clients aged under 20 from more deprived areas is similar to the profile of first time younger mothers across Scotland, at around 70% of all first time births in Scotland and FNP enrolments annually. In the first 3 years of FNP there was a large increase in the proportion of clients from SIMD 1 and 2 areas enrolling, but this has decreased slightly since 2013. Chart 8 shows that the proportion of FNP clients aged 20-24 from more deprived areas is slightly higher than the profile of first time mothers aged 20-24 across Scotland, which would reflect with the targeting of women living in the most deprived areas within this age group as a proxy measure for need.
Ethnicity
The majority of FNP clients were of white origin (96%), with 91% identifying as "White Scottish" or "White other British". A very small proportion (4%) of FNP clients were from all other ethnic groups combined. This is similar to data shown in Scottish Maternity Records (SMR02). In 2020-21, 97% of young mothers (under 20 years) with a known ethnicity were white[35].
As shown in Chart 9, the majority of FNP clients were white, however there has been an increase over time in the proportion of clients from all other ethnic groups combined. As the roll-out of FNP progressed across Scotland, areas with higher levels of diversity have been more exposed to the programme which has changed the client profile over time.
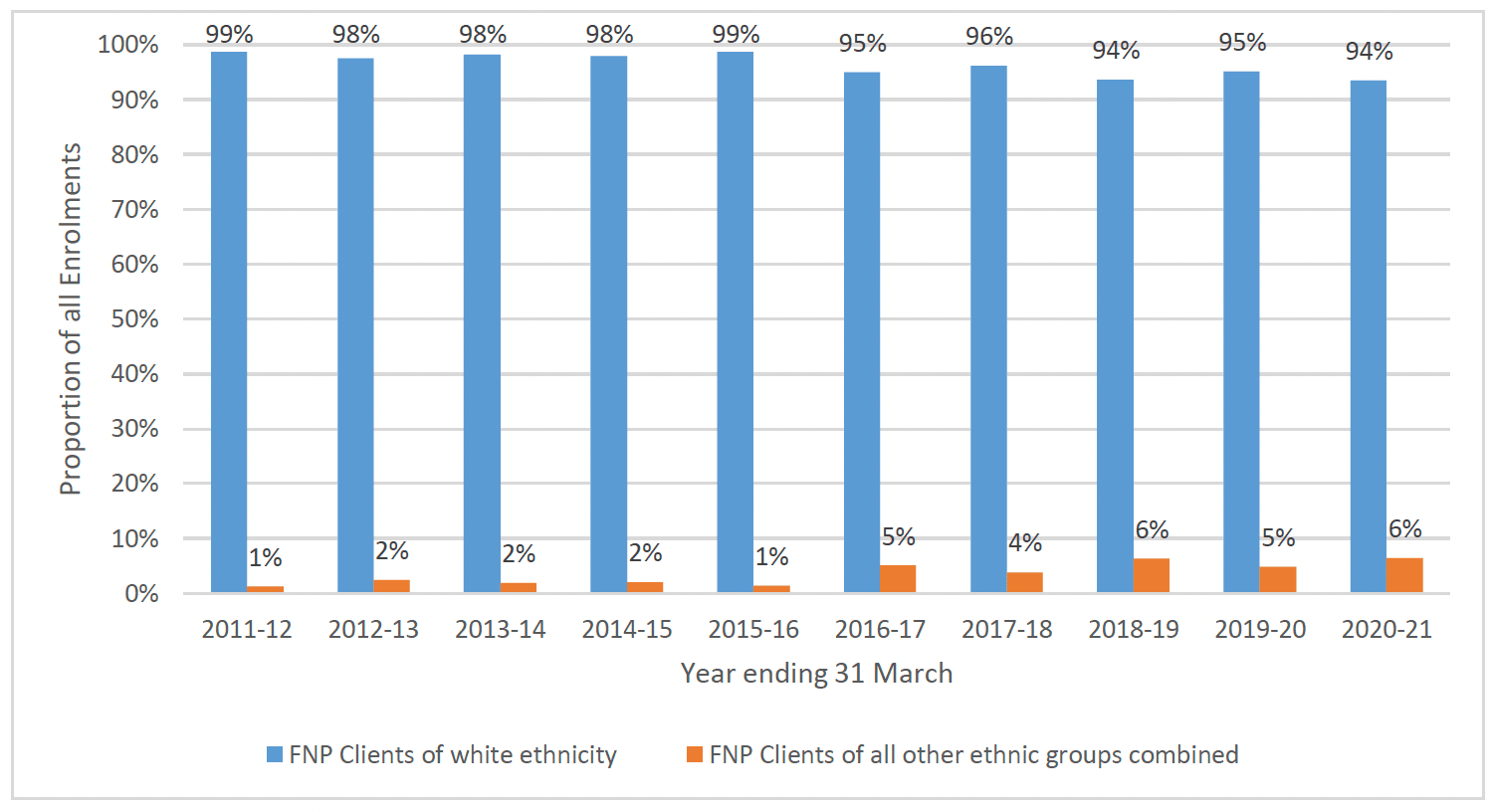
Table 2 shows that the majority of clients who were from all other ethnic groups combined at intake were primarily based in NHS Greater Glasgow & Clyde and NHS Lothian.
| Health Board | Number of all FNP clients of all other ethnic groups combined | Proportion of all FNP clients in Health Board |
|---|---|---|
| NHS Ayrshire and Arran | 7 | 1.2% |
| NHS Borders | * | * |
| NHS Dumfries and Galloway | * | * |
| NHS Fife | 17 | 2.1% |
| NHS Forth Valley | 11 | 3.1% |
| NHS Grampian | 15 | 3.3% |
| NHS Greater Glasgow and Clyde | 139 | 9.8% |
| Highland | 7 | 2.2% |
| NHS Lanarkshire | 30 | 2.7% |
| NHS Lothian | 93 | 4.9% |
| NHS Tayside | 38 | 2.5% |
| Scotland | 360 | 4.1% |
English as a Second Language
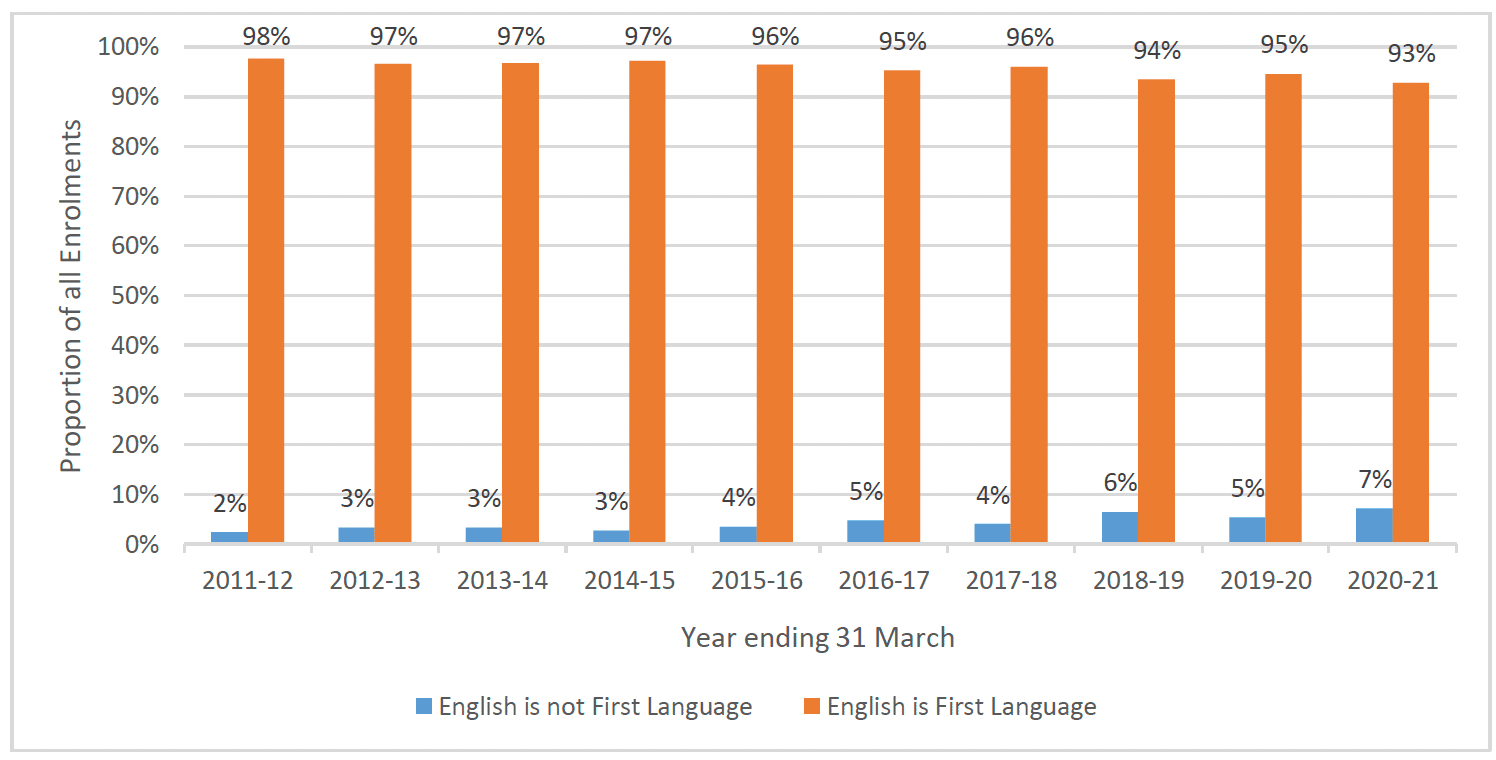
A smaller proportion of FNP clients (5%) did not speak English as their first language at intake, compared to the proportion of young people in Scotland who do not speak English as their first language (9% of all 3-24 year olds in Scotland[36]). There is no national dataset to compare those that do not speak English as a first language and the birth rates by age in Scotland. As shown in Chart 10 below, there has been an increase over time in the proportion of clients who did not speak English as a first language at enrolment.
There was also geographical variation in the proportion of clients who did not speak English as a first language. Table 3 shows that the majority of clients who did not speak English as a first language at intake were primarily based in NHS Greater Glasgow & Clyde and NHS Lothian. Therefore, similar to ethnicity above, as areas with higher levels of diversity began to fully roll-out FNP, the client group has become more diverse.
| Health Board | Number of all FNP clients who did not speak English as a First Language | Proportion of all FNP clients in Health Boards |
|---|---|---|
| NHS Ayrshire and Arran | * | * |
| NHS Borders | 6 | 3.5% |
| NHS Dumfries and Galloway | * | * |
| NHS Fife | 18 | 2.2% |
| NHS Forth Valley | 8 | 2.2% |
| NHS Grampian | 18 | 4.0% |
| NHS Greater Glasgow and Clyde | 150 | 10.6% |
| Highland | 14 | 4.5% |
| NHS Lanarkshire | 25 | 2.3% |
| NHS Lothian | 130 | 6.9% |
| NHS Tayside | 47 | 3.1% |
| Scotland | 418 | 4.8% |
* Indicates number is less than 5
Qualifications and Working Status at Enrolment
A pregnancy at a young age can have an impact on schooling and education. For those that go on to give birth at a young age, the FNP data shows a clear linear pattern of an increase in qualifications with higher maternal age. Of all clients enrolling onto FNP, the majority (77%) reported having a National 1 to 5 equivalent qualification at entry onto the programme. Just over one in eight (13%) reported having a Higher or Advanced Higher level qualification (including those who also had a National level qualification) and a similar proportion reported having no qualifications (14%) upon entry to the programme.
The Scottish statistics for attainment[37] show that the average qualification attainment for school leavers in Scotland is much higher than that seen in FNP clients. This reflects the deprivation profile of FNP clients, as pupils from SIMD 1 and 2 areas are much less likely to leave school with a Higher or Advanced Higher level qualification than their peers. However, FNP clients typically had a lower rate of attainment of these qualifications than pupils from SIMD 1 and 2 areas overall. Age is another important factor: younger mothers (those aged 16 years and under) (33%) in FNP were almost 4 times as likely to have no qualifications at enrolment compared to those enrolling aged 19 or over (9%).
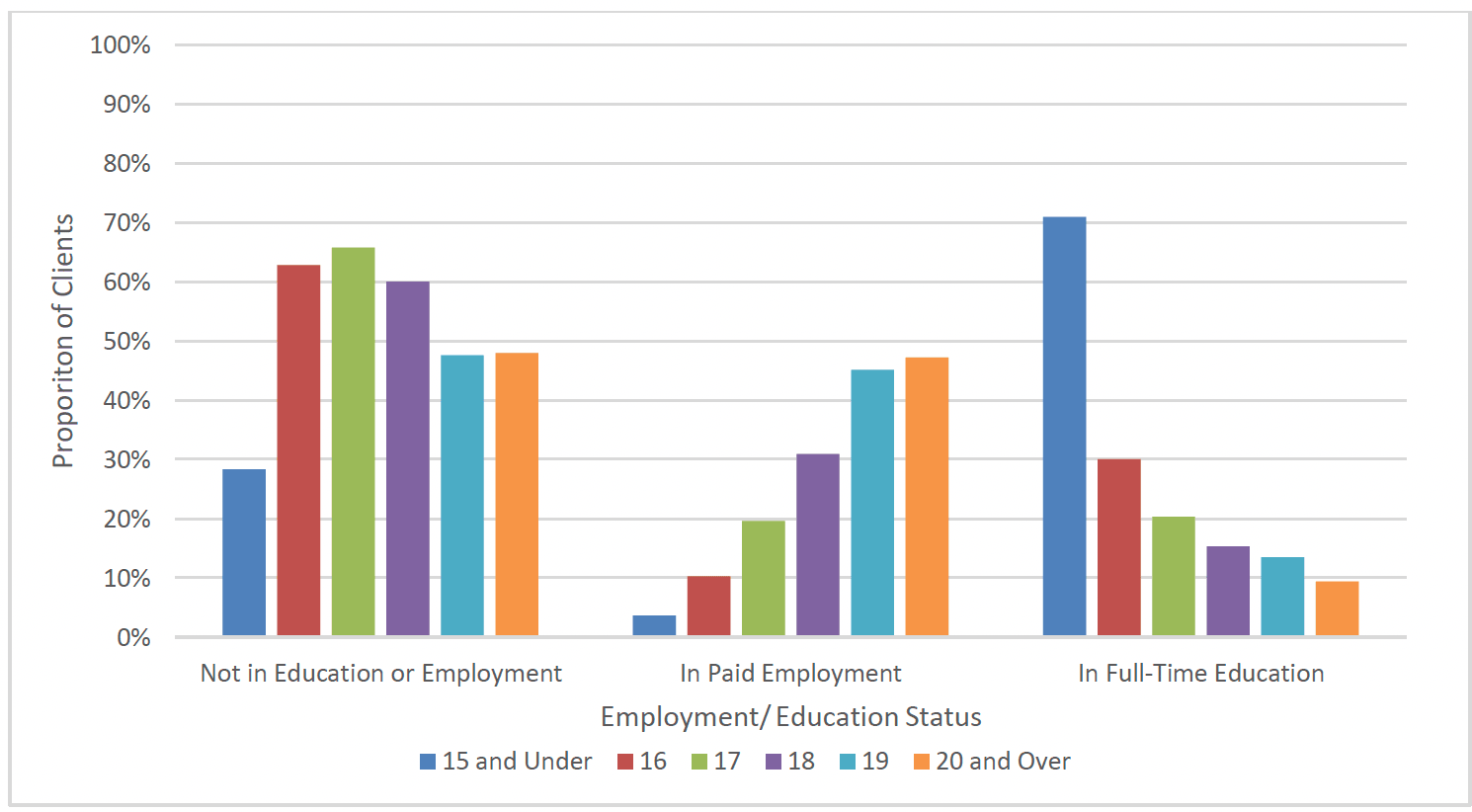
Overall, one in three clients (33%) were in paid employment at enrolment, one in five (18%) were in full-time education, and more than half were in neither paid employment or full-time education (55%)[xi]. There was notable variation between clients of different age groups in their employment status (Chart 11). Among clients who were above compulsory school age, those aged 19 and older were more likely to be in full-time education or employment (52%) than those aged 16-18 (38%) (Chart 11). Over time there was a slight reduction in the proportion of clients who were neither in education or employment at enrolment. This is possibly attributable to a larger number of clients who were aged 20 and over at enrolment in more recent years, as well as an increase in the proportion of clients aged 18-19 who were in paid employment at enrolment.
Relationships at Enrolment
Relationships are key in FNP. The therapeutic relationship between the Family Nurse and the client is at the centre of the way in which FNP seeks to influence change. However, how parents perceive the connections they have in relation to others and how they are influenced by those relationships also play a central role in the programme.
More than a third (37%) of FNP clients said they were not in a relationship at enrolment. Around half of younger clients aged 17 and under were single at enrolment (49%), compared to a third of clients aged 18-19 (34%) and a quarter of clients aged 20 and older (26%). Younger clients were also less likely to be living with a partner at enrolment, though it was only a minority of clients who lived with a partner in all age groups (15% of those aged under 17, compared to 26% of those aged 18-19 and 30% of those aged 20 and older).
This is echoed in the findings from Growing Up In Scotland (2014), which found that the composition of the household in which mothers aged under 20 live differ greatly from those of mothers aged 20 or older. With nine in ten (89%) mothers aged 25 or older living with the child's biological father compared with 30% of those aged under 20.[38]
Data on fathers' involvement and communication with FNP clients at enrolment was only captured on the data system in more recent years. Of the 2267 clients for whom this data was captured between 2019 and 2021, more than three in four young mothers (77%) reported being in daily contact with the father, an additional 8% reported being in contact with the father at least once a week, while 15% of clients reported being in contact with the father less frequently or never.
Housing at Enrolment
The majority of FNP clients (53%) lived in local authority or housing association housing at enrolment. 17% of clients lived in privately rented accommodation and 17% in privately owned accommodation. Under one in twenty (4%) clients lived in temporary accommodation, and a small number of clients (1%) lived in supported accomodation. Most of the remaining clients had a housing type recorded as "other" or did not have housing data collected.
A notable percentage of FNP clients (5%) were registered homeless, highlighting the complex lives of the client group. While the majority of mothers who were registered homeless were aged 18 and older, there were also mothers aged 17 and younger who were registered homeless. Further, information on homelessness was not consistently captured in the earliest years of the programme, so the true figure is likely to be higher.
Complex Lives
While some of the complexities of clients' lives are captured in the FNP data as shown above, the recent Revaluation report[39], a qualitiative evaluation of FNP in Scotland, sought to understand this more fully. In 2018, all Family Nurses delivering the FNP programme in Scotland completed a questionnaire about their clients to help provide a deeper understanding of FNP clients' lives. They used a list of 43 items (Annex 2) to identify events experienced by FNP clients prior to entry to the programme.
The results of this exercise were stark and highlight the complex environments in which Family Nurses and clients are working to achieve the outcomes of the FNP programme. The Revaluation report provides insight into the many issues that some clients face alongside their new role as a parent. The incidence of mental health issues, insecure housing and poverty are high within the FNP client group. The needs of the client group are wide ranging across many different professional areas such as health, social work, housing and benefits. An essential element of the delivery of FNP in Scotland is the need to cultivate connections and partnerships with other professionals and organisations in order to best serve the needs of all clients and their children.
The results of the analysis of clients experiences pre-enrolment to FNP in 2018 from the Family Nurse Partnership in Scotland: revaluation report are found in the box below.
Complex Lives
Detailed analysis of clients experiences prior to entry to FNP. Data from The Family Nurse Partnership in Scotland: Revaluation Report published in 2019[xii]
Findings
The majority of FNP clients (98%) had experienced some form of trauma or adverse experience in their lives. The most prevalent complexities for FNP clients at entry to FNP were: anxiety or other mental health issues (63%), experience of parental separation (63%), low income (60%) and not being in work, education or training (57%).
Socio-economic Circumstances
Almost all clients in FNP in 2018 (88%) were recorded to have at least one socio-economic disadvantage upon entry to FNP. This was shown across all age groups, including those over 20 years old.
Six in ten (60%) of all clients were living on a low income and one in ten (11%) were viewed as having low job stability such as zero hours or temporary contracts. The majority of clients (57%) were not in work, education or training at the time of enrolment. Those aged 16 or 17 years were the most likely of all groups to be not in education, work or training (67%), whereas just under half (45%) of 19 and 20 year olds were not in education work or training.
A third of all clients had irregular, limited or no school attendance (31%). This varied substantially by age with younger clients being more likely to have irregular, limited or no school attendance (51% of those 16 and under) compared to a quarter of those aged 18-24 years (22%).
Over a quarter of clients (28%) had experienced homelessness and 28% were viewed as living in poor or unsuitable housing at the start of the programme. Of those that were living in poor or unsuitable housing almost half (47%) were also recorded as having experienced homelessness.
A majority of clients were parenting on their own (58%), while two in five were recorded as having had a partner at the start of the programme (42%). Over a third of clients (36%) were viewed as having limited social networks or as being social isolated. This was spread across the age ranges. However, for those that were care experienced or had been on the child protection register this was 56% and 53% respectively.
Just over one in twenty (7%) had caring responsibilities for dependent others.
Health
Family Nurses rated three quarters of clients as having health issues upon entry to the programme (75%) with 63% experiencing anxiety or other mental health issues. Physical health issues were reported at a much lower rate among this group compared to mental health issues. A small proportion of FNP clients were recorded as having had a long-term health issue (7%) or were registered disabled (1%). 5% of clients were thought to have a learning disability. Within the FNP cohort, less than one in ten (8%) were rated as having substance misuse issues or alcohol misuse issues (7%) when they entered the programme in pregnancy. Clients rated as having a parent with substance or alcohol misuse problems were more likely to use substances or alcohol themselves (21%).
A significant proportion of clients were viewed by their nurses (based on subjective judgement rather than a BMI measurement) to have been at an unhealthy weight (either over-weight/ obese or underweight) (22%). Within FNP, 63% of clients were thought to have anxiety or other mental health issues upon entry to the programme. This is high compared to the Scottish Health Survey which indicated that 26% of 16-24 year olds had signs of a possible psychiatric disorder[40].
Two in ten FNP clients (22%) were thought to have self-harmed, 10% to have attempted suicide, and 20% had attended Child and Adolescent Mental Health Services (CAMHS). Almost one in ten (8%) of all clients have experienced a previous pregnancy.
Social Services
The proportion of FNP clients recorded as ever having been care experienced or on the child protection register was 22%. Similarly, a significant minority of FNP clients were rated as being from families with previous involvement with social services (36%) or from families that are known to social services (31%).
Criminal Justice
Overall, 6% of clients were rated as having been involved with the criminal justice system, this increased to 17% among those that were care experienced or had been on the child protection register. Family Nurses recorded that almost a quarter (22%) of clients who had experience of a family member being incarcerated had also had involvement with the criminal justice system themselves.
Adverse Childhood Experiences
Adverse Childhood experiences have been defined as intra–familial events or conditions causing chronic stress responses in the child's immediate environment. These include notions of maltreatment and deviation from societal norms. Evidence shows that adversity and trauma in childhood can impact on a wide range of education, health, justice and social outcomes. Of the top ten events that clients had experienced, as identified by Family Nurses, only two are regarded as adverse childhood experiences. These are parental separation (63%) and parental mental health problems (33%).
Overall, 7% of FNP clients had experience of incarceration of a family member and 10% were believed to have experienced the death of their mother, father or primary attachment figure. At least a fifth of clients are recorded as having experienced bullying, with clients aged 15 and 16 years old more likely to experience bullying (30%).
A quarter of FNP clients (25%) were recorded by Family Nurses as having experienced emotional abuse. Exposure to emotional abuse in childhood decreases in prevalence among FNP clients with age on entry. Those entering the programme at a younger age (13-17 years) appeared more likely (31%) than the older age groups (16%) to have experienced emotional abuse. This pattern was similar among clients who have experienced emotional neglect, with younger clients (23%) more likely to have experienced this than older clients (12%). Exposure to sexual abuse also decreased with age upon entry with clients who entered the programme at a younger age being more likely to have experienced some form of sexual abuse (20% of those aged 13-17 years) than their older counterparts (12%). Experience of physical abuse was recorded for 16% of clients.
Almost one fifth (18%) of clients were rated as having experienced intimate partner violence in their relationships. A similar figure was recorded (17%) for FNP clients experiencing their mother being treated violently. Those that had witnessed their mothers being treated violently were more likely to have experienced intimate partner violence themselves (33%).
Whilst we need to bear in mind that these recorded events are based on the views of Family Nurses, the findings highlight the complex lives and substantial burden of challenge that young women entering FNP face.
Contact
Email: Justine.Menzies@gov.scot