Healthcare quality and efficiency support team: annual report 2013
Annual report in relation to improving the quality and efficiency of healthcare in Scotland.
Mental Health
NHS Borders: Analysis of Increasing Referrals into the CAMH Service
Background/Context
Anecdotal evidence within the NHS Borders Child and Adolescent Mental Health (CAMH) Service reported a consistent increase in the number of referrals over the past few months. Changes had been made to the acceptance criteria, and the change in the number of referrals was being attributed to this. Previously, patients at age 16 were referred to adult services. In January 2012 and January 2013, patients were accepted at 16 years and 17 years of age respectively.
Problem
Historical data was created and displayed objectively in a run chart to determine the actual pattern of referral activity. Chart 10 displays the proportion of referrals associated with each school age group.
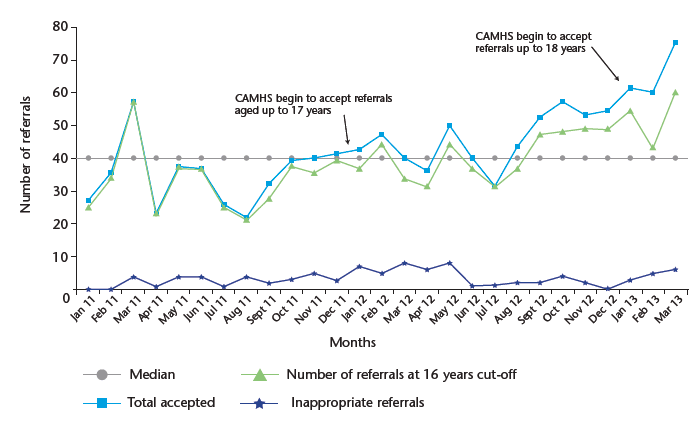
Although we have only looked at two data points (February and March 2013) for an indication of the changes in referral numbers per age group, it is apparent to date that the 16 and 17 years olds have contributed little to the rising referral rates. Chart 11 reveals how the referrals would have increased without the increase in age cut-off.
The data points only cross the median four times in chart 11 indicating a non-random pattern or signal of change. This significant change is occurring regardless of the additional referrals associated with the 16 and 17 year age groups.
The increase in referrals was instead attributed to three possible causes:
- change in referrer behaviour due to uncertainty of appropriate referrals
- change in staff behaviour as patients are accepted for one-off assessment appointments
- genuine increase in appropriate referral
Aim
To understand the reasons for this change in referral numbers so as to inform the team response to this increase.
Action Taken
Different responses are required whether the change in the number of referrals was due to the change in behaviour or a genuine increased need for the service. A value stream mapping event was held that invited CAMHS staff and referrers to meet informally and discuss the differing interpretations and understanding of the referrals process and what the service has to offer.
Chart 10: Total referrals into CAMHS 2011 - 2013 (includes inappropriate)
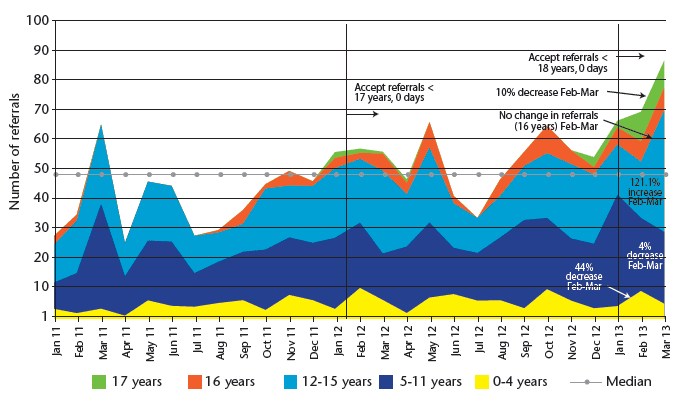
Chart 11: Total referrals into CAMHS according to new and old criteria
One key theme was extracted from this event - clarity of communication through:
- one-click access to well-defined referral criteria on the website
- clear and speedy feedback of referral status to the referrers
- early actions to allocate patients to the correct staff member
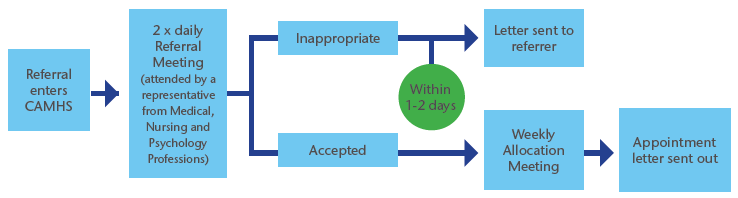
The referral process was redesigned from the weekly team meetings to daily monitoring of incoming referrals as shown in figure 4a and 4b. A representative from each profession would meet daily to discuss incoming referrals and mark as inappropriate or accepted. As referrals will be checked on the day, the inappropriate referrals and the justifications will be identified immediately with the referrer. A multi-professional discussion about incoming referrals will reduce the chances of patients being seen as a one-off session with one professional before being forwarded on to a more suitable intervention.
Staff are now being actively encouraged to attend the weekly meetings where all referrals are allocated to the appropriate staff member and discussions are held regarding new referrals and the longest waiting patients. Working through this process as a team has generated a sense of team responsibility for the waiting times target, rather than focus on the individual clinician allocated to the patient.
Results
Chart 12 shows a break in the steady increasing of referrals after April 2013. However, we must be cautious in comparing two data points. The referral trend must be monitored over the next few months to determine a lasting result of the small changes made to the referral process.
If this PDSA caused a significant reduction in the number of referrals in the future months, the increase that began in July 2012 could be considered a product of referrer and service behaviour rather than a genuine increase in service demand.
Benefits
Improved communication has benefited the understanding of the referrers but also the understanding of team members within CAMHS. Discussions between professionals allow for faster access to the correct clinician. Patients will experience a more consistent service as they engage with the same professional. All of these factors benefit the organisation as time is saved via less unnecessary contacts.
Sustainability
A standard operating procedure has been designed so that a continuous production (chart 12) can be produced to monitor any early changes in the system. Assessing early changes are important to allow for early intervention.
Figure 4a: Old referral process
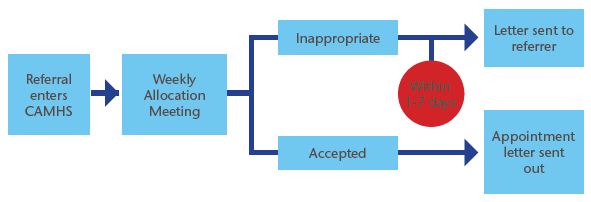
Figure 4b: New referral process
Lessons Learned
This case study has revealed the importance of consistent data reporting to understand variations in the process. Data reporting is also an important tool for visualising the targets for staff to create responsibility as a team for achieving the results. It is not just important to create these charts for management, but to share them with the team.
Constant vigilance on procedures is required as time progresses to meet changing demands. In this case, clarity in the referral criteria could clear access for only those individuals requiring engagement with the service. Communication with referrers is key to educate in what the service provides and prevent one-off appointments that lead to signposting elsewhere.
The use of a focus group involving all individuals who have a role to play in the journey of a patient is beneficial to reveal the diversity of opinions and to isolate the frequently occurring concerns.
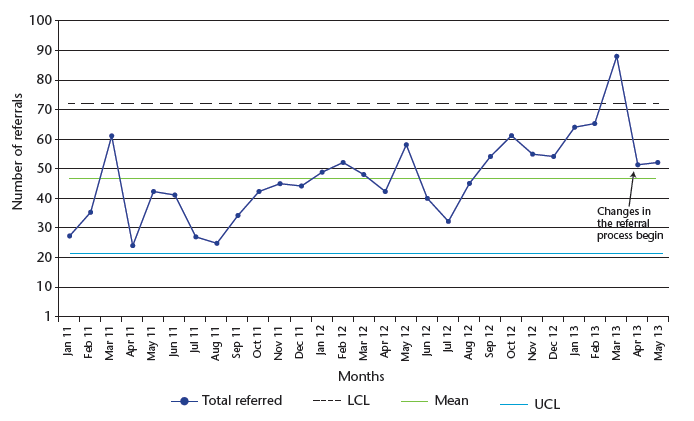
We have recently been able to replicate the above results in Statistical Process Control charts (SPC). Chart 13 displays eight or more plots above the average indicating a shift in the process average and so special cause variation.
This chart will be used for the monitoring of referrals in the future. Attention needs to be drawn to the months that may breach the upper control limits of 72 referrals suggesting a special cause variation.
Following these small adopted changes, an SPC chart will be produced to assess whether the small changes have contributed to a change in the average number of referrals and upper/lower control limits.
Chart 12: Total referrals into the CAMHS
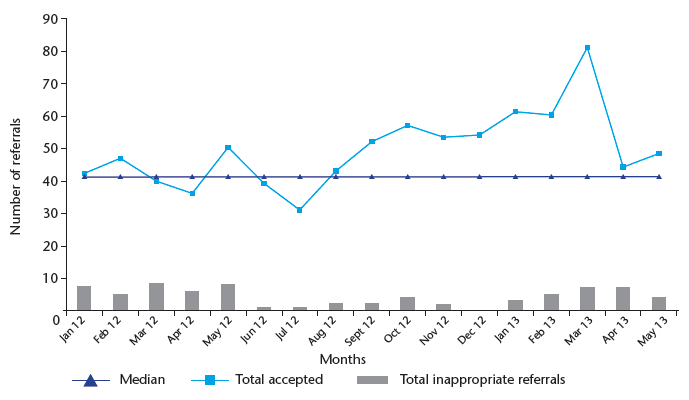
Chart 13: Accepted referrals into the CAMHS
NHS Borders: Incorporating Patient Choice in Appointment Allocation
Background/Context
In one community mental health team, the number of hours lost per week to appointments cancelled by patients was much higher than the other teams. If these appointments were not cancelled with an adequate amount of notice, they could not be allocated to other patients and so valuable face-to-face contact time with patients was lost.
Problem
The biggest loss of hours was for follow-up appointments. As these were patients that had already engaged with the system, it was important to focus on this. An analysis of the method of appointment allocation raised some concerns. Clinicians were sending letters out once back at the office and after meeting with the patient to assign the date and time of the next session. No patient choice was involved.
Aim
To decrease the hours lost to follow-up appointments within this community mental health team.
Action Taken
The main focus was to change the clinician's approach to a patient. The manager discussed the use of appointment cards, which could be given to a patient at the end of a session when the next appointment was mutually agreed upon. Appointment cards were printed and handed out to all staff.
Scottish Recovery Network ran a training day for the team, which placed emphasis on patient-centred care. This training was used as a tool to encourage clinicians to understand patient choice in their treatment process.
Results
Although it was not possible to incorporate this technique with every patient on every occasion, the number of appointment letters sent out weekly decreased from approximately 50 to 20 letters (60 per cent decrease). A reduction in letters has benefited the admin staff by freeing up time for other tasks. The clinicians have greater responsibility and flexibility over their job plans. Most importantly, the change has given patients greater control over their treatment process with a system that does not interfere with their personal commitments.
The organisation is benefiting from this improvement as the reduction in admin time is making the process more financially viable. This change in approach is also helping us to meet the values put in place for NHS Borders of caring and compassionate staff.
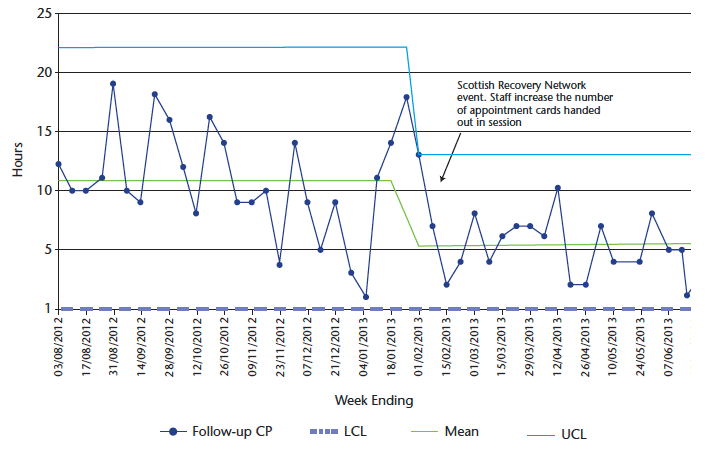
The Statistical Process Control chart (chart 14) demonstrates a clear picture of change. An average of 11 hours a week was lost to follow-up appointments cancelled by patients compared to five hours a week on the introduction of appointment cards.
Sustainability
Agreeing upon appointment dates and times within a previous appointment has been a long standing practice for other teams in mental health. Although this is not always a good indicator of how effective a system will be in a different team, the data is promising to date.
An SPC chart will be continuously produced to monitor any significant variation in the data. This means that managers can be proactive rather than reactive if any changes occur.
Chart 14: Hours lost to follow-up contacts cancelled by patients for West CMHT (excluding psychologist activity)
Lessons Learned
Staff can be very reluctant to change a system that has previously seemed to work so well. Having visual data to indicate how much time is actually lost has provided some concrete support and encouraged action for change.
This study has demonstrated the effectiveness of a PDSA exercise. The introduction of appointment cards has had little effect on the did not attend (DNA) rate; those that DNA may have some other barrier in their way. This must be addressed differently in an alternative PDSA exercise.
NHS Shetland: Mental Health (Administration Services and Clinical Governance)
Background/Context
A long term plan to support mental health was introduced in 2011; this project followed on from the first stage and was completed in 2012. However, like most improvement initiatives, the improvements are on-going and continue to this day. An admin team of four staff had been developed over a number of years. Ad-hoc additions of staff had evolved rather than being planned. This resulted in historical working patterns and the funding provided allowed the service to take time to analyse what was in place and what the future could look like.
Problem
- admin staff were continually working over their contracted hours
- nine separate filing systems for all mental health disciplines resulting in wasted time filing and finding notes - duplication of notes is common
- each member of the admin team was a specialist in only one area of mental health administration - no cross working and resilience
- admin staff were not clear about the admin processes for some areas outwith their own area of expertise
- DATIX incidents identified problems with clinical communication as a consistent factor in errors and complaints
- the patient's paper record had to be sent to Aberdeen if the patient was admitted to Royal Cornhill Hospital. This posed risks to the security of patient identifiable information and risks in treatment because of delays in returning the paper records to Shetland
- psychiatric case notes not available out of hours to Gilbert Bain Hospital A&E or Royal Cornhill Hospital 'on-call' duty psychiatrist
Aim
To identify and minimise waste within the mental health admin team and provide a better and safer service to patients.
Action Taken
The following actions were undertaken:
- implemented a single IT filing system and removed all the physical filing cabinets (FACE (Electronic Patient Record) planned 'go-live' in August 2013)
- issued all clinical staff with iPads to allow remote access/completion of notes and reduce need for daily return to base
- introduced a server based digital dictation system that allows a letter to be typed as soon as it is dictated
- removed six printers and reduced paper/ink costs by introducing a centralised printing service
- all filing cabinets archived to a storage area thereby increasing office space and improving the quality of clinic rooms
- developed written standardised operating procedures (SOPs) to support admin staff flexibility
Results
It is anticipated that there will be a reduction in the number of 'clinical communication' incidents once FACE is implemented. This will be monitored and audited once the electronic record system is in place. The digital dictation system has already increased the response/flexibility of the admin staff. Both clinical staff and patients have commented favourably on the improvements in the office/clinical environment due to the removal of filing cabinets.
Efficiency Savings and Productive Gains
The following achievements have been made:
- reduction in the amount of administrator time required to process clinical files/records
- electronic notes mean that clinicians can work more flexibly from home or remotely/out of hours more easily
- clinical letters processed more efficiently and flexibly
- improves clinical communication/safety in and out of hours because of a single shared electronic record
- reduction in the amount of management/clinician time involved in dealing with the consequences of errors and complaints
- savings equivalent to £28,000 have been achieved as a result of freeing up staff time and the need for fewer admin staff (enabling NHS Shetland to reinvest this time in other areas of work and to release a vacant post as a result of the improvement work)
Sustainability
This is a fundamental change in clinical administration processes. It is supported by the eHealth Strategy.
Work is also in progress to establish written standardised operating procedures (SOPs) for admin to support and maintain role flexibility for admin staff.
Lessons Learned
The work highlighted the importance of understanding and planning small scale PDSA changes in the context of a 'whole system' approach to service redesign. Implementation of larger changes took longer than anticipated due to the interwoven nature of systems and services. Stakeholder involvement was/is a critical success factor.
NHS Tayside: Child and Adolescent Mental Health Service
Background/Context
Tayside Centre for Organisational Effectiveness (TCOE) was asked to help with this challenge, providing a range of tools and support to get the job done. Our consultants supported the Child and Adolescent Mental Health Service (CAMHS) team in analysing and measuring data to see where changes had to be made to the service, particularly to address staff capacity and patient flow.
A service improvement advisor facilitated the improvement work associated with the introduction of a Choice and Partnership Approach (CAPA) and also conducted pathway development work to map current processes and develop service redesign initiatives. These pathways were then revised in line with the CAPA model.
Meanwhile, an organisational development consultant was commissioned to undertake a systemic 'diagnostic', looking at the culture and dynamics within the service, and to formulate recommended interventions for action. TCOE later backed up this initial work with change management support to help team members embrace the necessary changes to the CAMHS service.
Problem
Faced with excessive waiting times, the CAMHS team recognised that change was needed. The previously existing model of service delivery no longer met the needs of a much larger service with significantly increased demands placed upon it.
Complaints were common, and a high rate of DNAs exacerbated an already bad situation.
A staff survey at the outset of the improvement work highlighted further difficulties:
- pressurised, stressed staff, with low morale
- inter-professional and team difficulties
- poor communication
- leadership, accountability and management issues
- lack of clarity, and poor understanding of roles, competencies and capacity
- mistrust and avoidance of addressing issues
Aim
The CAMHS team committed to a service redesign and to reducing Tayside CAMHS waiting times in line with national targets by March 2013. To achieve this, the service moved to three locality teams and adopted CAPA, a clinical system implemented in many CAMHS teams across the UK.
Hurdles to overcome in reaching this target included:
- a 51 per cent increase in referrals to CAMHS generally from 2006-10
- inequity of service provision and access across the three localities comprising NHS Tayside
- a backlog of more than 100 patients who had been waiting > 26 weeks; 38 of this number had already waited > 52 weeks
- high DNA rate of around 32 per week
- unclear and often ineffectual leadership and communication structures
Action Taken
NHS Tayside set about redesigning its service around CAPA - a CAMHS system flow management tool designed to reduce waiting lists and enable quicker response times for patients.
In order to address the waiting times issues, a number of initiatives were taken forward by the CAMHS Teams.
These comprised:
- Revision of the referral criteria and distribution to all referrers.
- Mapping of key stakeholders to inform them of the service's adoption of CAPA.
- The weekly referral screening meeting which involved four to five staff was replaced by daily referral screening by one to two staff. This resulted in referrals being allocated more quickly and effectively.
- An opt in letter was sent to patients/families on the waiting list to ask if they still required CAMHS services. A waiting list 'blitz' was planned to clear the backlog before instituting the service transformation.
'Choice champions' were selected to roll-out the new approach centring on choice appointments. In this approach, an appointment scheduled for around six weeks following receipt of referral aims to establish with the patient and family what they view as the problems they face. The appointment is structured towards a 'choice point' where the patient, family and clinician agree the way forward. Options here include support from CAMHS, from services within the community or a combination of both. Self-supporting strategies are also encouraged, and the patient and family may be directed to a range of media materials for further information.
Results
After consulting with the CAMHS team, the service structure was revised. Certain meetings were rationalised and/or discontinued, and three locality teams formed to provide better and more targeted service coverage. The staff resource was tailored to meet patient requirements in each locality, while retaining the capacity to flex this resource when required to meet demand.
Throughout this service transformation, a small CAMHS improvement team comprising senior management and TCOE consultants provided invaluable support and direction. The team enabled clear lines of communication to be established and ensured that any concerns were addressed swiftly and effectively. Organisational development and leadership development were other key areas of focus, and TCOE's interventions zeroed in on team dynamics and team building.
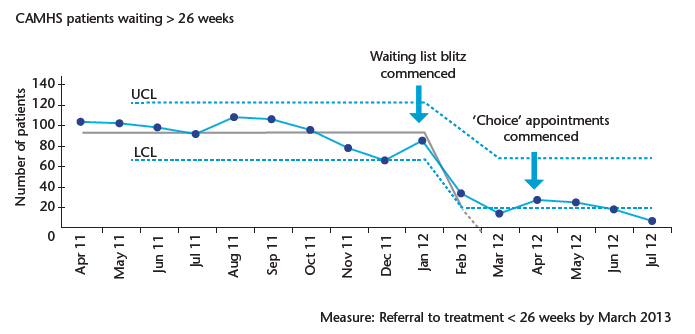
Chart 15: Waiting times
Feedback for the Team
"The consultants inspired hope of change and improvement for a system which was struggling considerably in the light of differing expectations and delivery targets. Through comprehensive observations of, and communication with, all parties involved, the resources required for change were mobilised. It was noted that significant investment of time was involved in the early stages of this project - this helped give the consultants legitimacy and respect from the whole staff group in CAMHS - genuine understanding of the systems was achieved. There was also a degree of responsiveness to problems that was refreshing - problems were clearly highlighted as soon as they arose with no opportunity for avoidance. There was also tenacity in terms of problem solving options that helped situations move on much more quickly than would be CAMHS' past experience. Finally, as well as problem solving, the consultants were exceptionally sensitive too and rewarding of progress made - this was always genuine and a refreshing change for all concerned - something to be emulated!"
Efficiency Savings and Productive Gains
Early results show a demonstrable improvement in waiting times (chart 15) and the service also reports improved patient and carer experience as a result. The introduction of DCAQ through CAPA will continue to support clinical and process efficiency by reducing flows, reducing DNAs and optimising clinical time in patient facing activities.
Sustainability
Over time, and with backup from TCOE, the CAMHS team developed the knowledge and skills required to deliver improved patient access, care and outcomes.
A year on, in November 2012, the three biggest improvements remarked on by staff were: improved waiting times; improved care, choice and consistency for children and their families; and improved team working.
The majority of CAMHS staff now rated the service's performance as seven out of 10, where previously they had given it just 4.87 on the same scale.
The formation of locality teams - and support for the locality team leader model - appeared to be a major factor in the culture change.
Dr Sheenagh MacDonald feels positive that NHS Tayside CAMHS will continue to develop and build upon what has been achieved.
Says Dr MacDonald: "There will be challenges ahead, but the service is well on the way to fully achieving its redesign goals and it is now much better equipped to deliver the future improvements to which it aspires."
Lessons Learned
The cultural and change management required cannot be underestimated and needs to underpin data collection and analysis. PDSA testing has supported the organisation to gain the knowledge, experience and clinical champions to allow us to spread the approach within the CAMHS service. The approach gave assurance in the robustness of information supporting future service planning and provides transparency for all concerned in identifying the recurring and non-recurring activity necessary to achieve and sustain waiting time guarantees. The clinicians were engaged throughout the process, and they have supported the findings for the development of solutions and are assured that capacity can be tailored to meet demand.
Contact
Email: Dayna Askew