Healthcare quality and efficiency support team: annual report 2013
Annual report in relation to improving the quality and efficiency of healthcare in Scotland.
Outpatients, Primary and Community Care
NHS Highland: Why Did the Patient Cross the Road? Because their Rehab was on the Other Side!
Background/Context
Fort William in the Highlands of Scotland has a rural general hospital with wards located 0.5 km apart. Belford is the main building and delivers more acute services. On the other side of the main road, is the Belhaven Ward - a rehabilitation unit.
Problem
This layout meant duplication of some services and resources split (medical staff only based in the main Belford building). This imposed a barrier to good patient flow and resulted in significant cost implications.
Aim
To reorganise services to be more person-centred, safe and efficient by relocating staff and community services to better but fewer facilities.
Action Taken
The following actions were undertaken:
- Lean improvement techniques and PDSA (Plan, Do Study, Act) cycles
- staff consultation and patient feedback
- monitoring of emergency admissions, length of stay and occupied bed days
Results
Inpatient Facilities (Belford Hospital)
Improvement work in Belford Hospital has delivered significant reductions in occupied bed days freeing up bed capacity:
- five beds transferred from Belhaven Unit to Ward 1 in Belford (November 2011)
- originally the unit had 17 beds but occupancy steadily declined
- reduction in 'hand-offs' and movement of staff and patients between wards
- daily presence of social work and community nursing staff in the Belford
Community Services
- transfer of staff (physiotherapists and occupational therapists) from Belhaven Unit to Fort William Health Centre completed (March 2013)
- rehabilitation services delivered from better facilities (individual clinic rooms, air conditioned gym and fully equipped tele-rehabilitation)
- development of physiotherapy classes in Fort William Leisure Centre
Patients and Staff
- patient feedback very positive on better atmosphere and nicer surroundings
- better transport links and car parking
- lone working and security issues for staff resolved
- staff morale improved by providing better permanent facilities
Efficiency Savings and Productive Gains
Significant savings from reduced running costs and cost avoidance (£1 million):
- total cost avoidance from essential upgrade works (£634,900)
- recurring savings from the overall redesign (£250,000)
- running costs saved from closing the Belhaven (£90,000)
- value of Belhaven, now surplus to NHS requirements (£68,300)
Lessons Learned
"The whole thing has been a big success. It is a much better physical working environment and we've been made very welcome. Staff have responded really positively and have taken on real ownership of the move. The benefits of co-location with the other professions are becoming more and more apparent."
Kenny Mackintosh (Superintendent Physiotherapist), April 2013
NHS Western Isles: Community Nursing Patient Held Record and Digital Pen technology
Background/Context
November 2009 - Leading Better Care programme invited senior charge nurses to lead on improvement initiatives.
January 2010 - Documentation Group established to develop, standardise and improve on current documentation practice and to manage the patient held record at point of care.
March 2010 - Invitation to stakeholders to join group initiated a synergy and joint working with the IT department that would impact on the design and implementation of core objectives.
Problem
Patient held documentation evidenced only a narrative of care given by nurses; it did not evidence patient involvement, nursing assessment or plan of care. Additionally, inefficient use of community nursing time spent duplicating patient documentation in the patient's home and then electronically back at base. This raised the question of the quality of data being recorded electronically several hours after interaction as opposed to recording at point of contact.
A scoping exercise evidenced that 41 per cent of community nurses' time was spent on administration tasks at base, 28 per cent of time was spent on direct patient contact.
Aim
To achieve improvements in efficiency and productivity and patient safety by:
- producing a universal patient held record that would be patient-centred involving patients and carers in developing and agreeing their plan of care involving aspects of self-care where appropriate, thereby enhancing the quality of patient care, experience and safety
- reducing the amount of time community nurses spend on administration and data entry and increase patient facing and patient enhancing activity time
- reducing the lapsed time and duplication of data entry
The project aims to evidence an increase in patient facing time and a decrease in administration time by community nurses; this should be clearly evidenced one year on from commencement of the project.
Action Taken
The following actions were taken:
- an inclusive approach was used involving key stakeholders
- the group worked jointly with the IT department to explore solutions to improve efficiency - a scoping exercise was commissioned to identify issues and propose solutions
- digital pen technology commissioned
- patient held documentation piloted across the Western Isles and improved and finalised using PDSA cycles of change
- digital pen technology pilot launched alongside revised patient held documentation in July 2012 in one community nursing team in the Western Isles
- a local workload tool was utilised to evidence outcomes
- patient and staff satisfaction surveys were conducted and will be repeated one year on from implementation
Results
The project has delivered on developing a universal patient held record which has improved on the quality of data recorded. Documentation is instant at the point of patient contact and records can be shared with other professionals electronically evidencing safer practice.
The initial phase of the project met with significant technological challenges which were overcome over time; these problems compromised the planned phased roll-out to other teams resulting in a much longer than anticipated pilot phase. Phased roll-out to other teams began in March 2013.
The finalised product has now been implemented in four out of five community nursing teams within the Western Isles with significant support being provided during each team's initiation phase. Feedback from staff is extremely positive. Improvement in efficiency and productivity can be evidenced. The pilot team (East Team) has by far the largest caseload, practice population 13,000, and is less geographically spread. The East Team can evidence an increase in patient facing time from 29 per cent to 44 per cent pre and post digital pen. Travel and administration time have reduced by small margins (see charts 1 and 2).
Similarly the Uist Team, a remote geographically dispersed team with a practice population of 4,000, can evidence similar results since commencing the patient held record in March 2013. Patient facing time has increased, travel time has decreased, administration time has however increased; this can be attributed to the transition phase when all patients on the case load required to be transferred onto the new system (see charts 3 and 4).
Additionally, the East Team can evidence an increasing proportion of complex contacts over the period since implementation of the project. This may reflect work arising from the more comprehensive assessment now in the new patient held records as well as an increasing number of patients discharged home with complex needs (see chart 5).
Efficiency Savings and Productive Gains
The pilot community nursing team has been absolutely integral to the implementation of the digital pen project, initially through simply trialling the technology but, more latterly, by playing a proactive role in its development and effective application in practice. This is reflected in the significant increase in time spent on service development as the digital pen and PHR were being introduced (see chart 6). This investment in nurses' time has been essential in the roll-out of this project and demonstrates that nurses have helped to develop a system that suits their and their patients' needs rather than adapting their work practice to fit in with an existing system. This increased productivity, used to improve working practice and service development, is an essential investment initially to deliver a system that will improve efficiency and productivity.
Sustainability
This plan has been sustainable by ensuring good partnership working with IT colleagues and service providers and solving all potential problems within pilot phase prior to disseminating to other areas.
We have kept key stakeholders informed and included at all times throughout the initial pilot phase and have not spread to other areas until problems encountered within the pilot phase have been rectified and the infrastructure is in place to ensure a seamless progression. Staff feedback is extremely positive and encouraging despite initial technological problems.
The initiative has attracted national attention and prompted a number of other NHS Boards to undertake feasibility studies into the adoption of digital pen technology. Our providers inform us that to date four other NHS Boards have bought the technology; NHS Ayrshire and Arran, NHS Dumfries and Galloway, NHS Highland and NHS Orkney.
The technology is to be further deployed to other areas of NHS Western Isles where similar productivity gains are required.
Plans are in place to increase the scope of practice for clinicians e.g. development of apps toolkits (such as patient nutrition assessment tools and staff workload tools) and explore the potential for integrated working with social care utilising digital pen and patient held record.
This is now embedded in practice: it is the way we work now.
Lessons Learned
The following lessons were learned:
- investment in time to iron out technology problems before 'going live'
- IT staff should shadow clinical staff in clinical areas in order to experience problems first hand, such as connectivity problems, and resolve any issues found quickly to maintain engagement with clinical staff
- recognise variation in staff technology skills
- utilise clinical staff alongside IT staff when rolling out to other areas
Provider Comments
- create more process/workflow material that is specific to the new processes and easy to digest for clinical staff
- introducing two new processes to clinical staff (patient held records AND new technology) was brave but worked
- engaging patients through using the media created an atmosphere of 'collaborative excitement' when the nurses were seen using the technology in the patient's home
- engaging clinical staff at all stages of procurement and seeking 'buy-in' pays dividends when teething issues occur
Chart 1: Breakdown of time May 2012 - East team pre digital pen
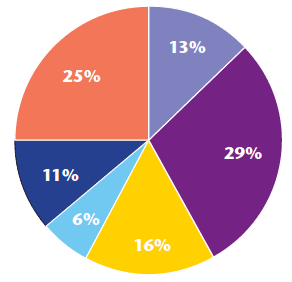
Chart 2: Breakdown of time July 2013 - East team post digital pen
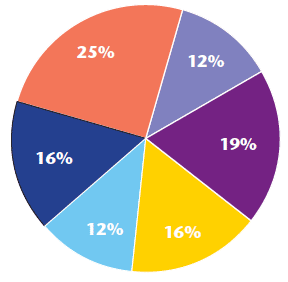
Chart 3: Breakdown of time May 2012 - Uist team pre digital pen
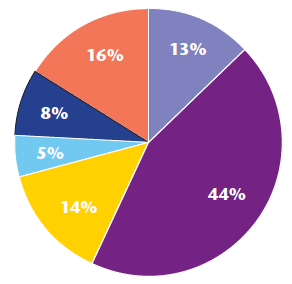
Chart 4: Breakdown of time July 2013 - Uist team post digital pen
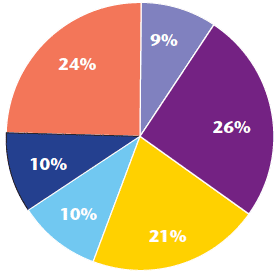
Key
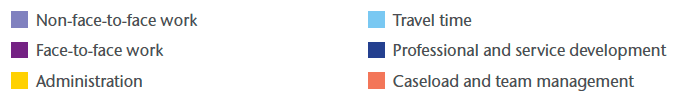
Chart 5: Complex and highly complex contacts
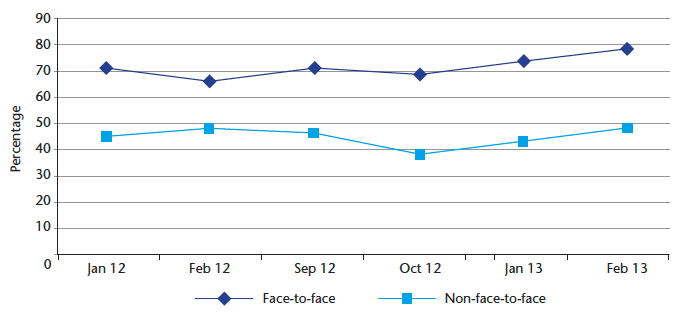
Chart 6: Time spent on service development
NHS National Services Scotland (Scottish National Blood Transfusion Service): Transforming the Donation Experience
Background/Context
The Scottish National Blood Transfusion Service (SNBTS) Strategy identified the need to transform the donation experience by improving the quality of care and communication, and to improve the efficiency and effectiveness of our service to volunteer, non-remunerated blood donors. Alongside this we aimed to streamline the process and improve efficiency and productivity, transforming the service in three phases. This case study relates the first phase which aimed to redesign and streamline the collection process, improve the donor experience while improving efficiency by balancing workloads across the session, and remove internal inefficiencies.
Problem
SNBTS had undertaken diagnostic work to analyse the underlying cause of process issues on blood collection sessions that could result in bottlenecks, extended wait times for donors and extended work hours for staff. This analysis indicated the following contributing factors:
- unbalanced workload at stages of the process
- suboptimal skill mix
- lack of control of flow of donors into the sessions
- lack of internal controls to trigger corrective action in process
- inability to control loss rates resulting from donor deferrals
Aim
Enable service excellence through delivery of high-quality, efficient and modern donor services that will ensure safe and sufficient blood is available to support the transfusion needs of Scotland and that demonstrates an effective and value for money service.
Action Taken
Introducing the Home DSR
Completion of the Donor Session Record and Health Check Questionnaire (DSR) is a requirement for all donors to assess their eligibility to donate. Although the time to complete this at session is not extensive it does require an element of privacy for the donor and can result in the donor being deferred from donation. This can impact negatively on both the donor (who has wasted their time in attending a session) and the productivity rates (as part of the donation time is reviewing the DSR with the patient to ascertain if they are eligible to donate). Prior to home DSR, 14.5 per cent of donors were deferred. By issuing the DSR to donors at home we are able to:
- save the donor from having to attend a session if they are deferred (telephone support is available if they wish to speak to a medical advisor)
- improve donor satisfaction through reduced waiting times at donor sessions (the health check can become a bottleneck and reducing the number of donors who attend and are then deferred will ultimately reduce the number of donors in the queue)
- increase productivity (a higher percentage of donors attending will be eligible to donate and it was anticipated that productivity rates will increase by 5 per cent)
- increase efficiency of mail shots (longer term the cost of home DSR is anticipated to be neutral as other stationary/postage costs will be reduced due to process changes)
- support change in process for both staff and donors as we move towards online DSR
Rebalancing Workload across the Process
Diagnostic work demonstrated the need to redistribute workload across the stages in the collection process and improve the session layout to facilitate effective use of all available resources. To support this work we:
- redesigned the session layout, co-locating welcome and donor registration alongside post-donation care and refreshments with staff flexing between the two stations to match the workload
- introduced a 'priming role' on session to increase the health-screening capacity at the start of the session to 'push' more donors through this stage as quickly as possible
- introduced a controlled queue for beds at pack issue to act as a trigger for staff to flex between beds and health screening and follow the workload
- introduced automated blood mixers to reduce loss and streamline the bedside process
Ensuring Session Appropriately Resourced
SNBTS Donor Services have used a well-defined collection staffing model to allocate resources for collection activities since 2003. In 2012 this was extensively overhauled to develop a workload planning and resourcing tool with the ability to scenario plan and cope with variations in donor types (new, regular, lapsed, age, etc.), venue layouts and restrictions. This can also be used to optimise skill mix and has the option for the session resource manager to apply professional judgement in deciding the resource level and skill mix. The revised model is also used to monitor individual collection session performance and this can provide feedback to the session manager.
Results
Phase 1 of Transforming the Donation Experience (TDE) was implemented across SNBTS Donor Services between April and July 2012. To deliver this, around 330 collection staff were trained and assessed as competent in the new process. The revised process has now been used in more than 1,000 community blood collection sessions. In addition the home DSR has also been used in 750 Donor Centre sessions.
Reduction in Loss Rates
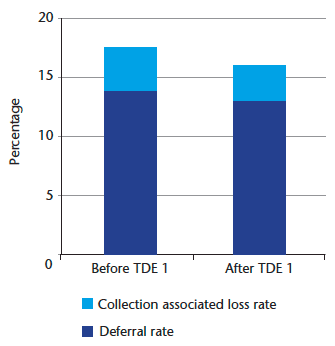
The number of donors attending sessions who are rejected on medical selection grounds has reduced from 14.6 per cent to 13.8 per cent at the end of 2012-13 (1,746 additional red cells banked from the donors attending). In addition, collection associated losses resulting from out of specification volumes reduced marginally from 3.6 per cent to 3.2 per cent (657 additional red cells banked).
Together these released an additional 2,400 red cells into the supply chain with an associated full cost value of approximately £280,000 (chart 7).
The home DSR also reduced the number of donors attending unnecessarily following travel to a malarial area by 1,000 and reduced the need to test these donors by 700 tests resulting in an additional saving.
Donor Satisfaction
Donor satisfaction is routinely measured twice each year using the industry standard measure of Top Box which aims to get as many donors as possible scoring the service they received as 10/10 across a number of indicators. The results of two surveys carried out after TDE implementation demonstrated significant improvement across a number of indicators, (see table 1).
Chart 7: Loss reduction following TDE 1
Efficiency Savings and Productive Gains
The TDE 1 programme exceeded the savings target of £364,000 during 2012-13 and these will be recurring.
SNBTS use two measures to assess collection productivity:
- useable donations per staff hour open (excludes travel to the session and non-donor contact time)
- useable donations per WTE (includes travel and non-donor contact time)
TDE resulted in the productivity gains outlined in table 2.
In addition we reduced the number of enhanced rate hours by 25 per cent and overtime by 19 per cent.
Table 1
| TOP BOX Question | Average Pre TDE 1 | Average Post TDE 1 | Per cent Change |
|---|---|---|---|
| The overall experience | 8.98 | 9.03 | 0.41 |
| Welcome on arrival | 8.95 | 9.05 | 0.90 |
| Waiting time | 8.05 | 8.40 | 3.52 |
| Fingerprick test | 9.07 | 9.16 | 0.82 |
| Sensitivity of health and lifestyle questioning | 9.16 | 9.17 | 0.15 |
| Insertion of needle | 8.78 | 8.83 | 0.52 |
| Cleanliness of the venue | 9.08 | 9.33 | 2.31 |
| Friendliness of our staff | 9.42 | 9.52 | 0.85 |
| Professionalism of our staff | 9.44 | 9.49 | 0.39 |
| Did we make you feel valued and appreciated? | 9.12 | 9.24 | 1.11 |
| Did we treat you with consideration and sensitivity? | 9.25 | 9.31 | 0.51 |
| Did we provide sufficient explanation at each stageof the process? | 9.09 | 9.23 | 1.29 |
| Average for all Top Box questions | 9.04 | 9.16 | 1.10 |
Table 2
| Productivity Indicator | Average Pre TDE 1 | Average Post TDE 1 | Per cent Change |
|---|---|---|---|
| Useable donations per staff hour open | 1.10 | 1.17 | 6.1 |
| Useable donations per WTE | 1,452 | 1,634 | 12.5 |
Sustainability
The following will ensure sustainability:
- the work to review our collection footprint and reduce non-donor contact time will further improve these gains and consolidate the improvements
- the workload on sessions has been further reviewed to reduce the workload in medical assessment of donors over 65
- plans are progressing to extend the use of appointments to control donor flow and smooth the workload
- feedback and communication to staff to demonstrate the benefits
- improvements in skill mix by introducing donor carer venepuncturists to reduce waiting times and collection losses
- improved information on website and all donor communications to promote accurate self-deferral if ineligible to donate
Lessons Learned
The following lessons were learned:
- effective planning is essential
- training, assessment and familiarisation are highly beneficial
- involve staff in finding solutions to issues raised
- effective partnership working is highly beneficial
- provide a mechanism for rapid improvements and trouble shooting
- effective anticipation and management of risks is essential
- use staff feedback and donor feedback and complaints as an opportunity to improve further and prioritise the next stage in service and process improvement
- phased implementation allowed us to support each team effectively and to continue to problem solve at each stage
Scottish Ambulance Service: Scheduled Care Project
Background/Context
The scheduled care project is a major piece of redesign and improvement work relating to the delivery of our patient transport service (PTS).
Problem
Analysis of the PTS in 2010 identified significant variation and inefficiency in the delivery of this service. This manifested itself in poor patient, staff and other stakeholder experience.
Aim
To improve the patient and staff experience of PTS by upgrading its IT infrastructure and redesigning its systems and processes. Additionally, whole system understanding of the role of PTS would underpin the redesign and improvement agenda to achieve a paradigm shift in culture, efficiency and quality.
Action Taken
The following actions have been taken:
- redeploy and streamline circa 30 hospital based Area Service Offices (ASOs) to three regional Ambulance Control Centres (PTS ACCs)
- refocus the clinical role of PTS from the perspective of the patient, staff and health colleagues
- invest in the IT infrastructure of the PTS
- initiate a review and redesign of all PTS systems and processes
- introduce direct patient access to the service
- introduce an industry standard call taking model for direct patient access
- reduce PTS request routes from 11 to two (phone and web)
- undertake major communication and engagement exercise with patients, NHS Boards and SAS staff
- initiate the creation of a capacity model for PTS
Results
The following results have been achieved:
- improving patient experience (on-going)
- improving staff experience (on-going)
- patients have direct access to PTS to discuss their individual health needs and hence ensure the right ambulance transport is provided to meet that need
- industry standard call taking performance
- better management of demand and appropriate use
- increase in use of PTS by patients with medical/mobility need
- improving PTS productivity (on-going)
- improving understanding of PTS capacity and demand (on-going)
- increasing efficient use of PTS resources (on-going)
- improving partnership with NHS Boards and other transport providers
Efficiency Savings and Productive Gains
Approximately £2.5 million savings released from improvement work to date.
Sustainability
This initiative is being delivered within the existing budget.
Lessons Learned
The following lessons have been learned as a result of this project:
- delivery of PTS is complex
- an efficient PTS creates similar benefits across the system e.g. alternative transport costs, delayed discharges, 18-week referral to treatment compliance
- an efficient PTS is dependent on an efficient outpatient, discharge and inter-hospital transfer system
- an effective PTS is central to a positive patient experience
Contact
Email: Dayna Askew