Healthcare quality and efficiency support team: annual report 2013
Annual report in relation to improving the quality and efficiency of healthcare in Scotland.
Acute Flow and Capacity Management
NHS Ayrshire and Arran: Emergency Care Quality Improvement Programme
Background/Context
NHS Ayrshire and Arran initiated the Emergency Care and Quality Improvement Programme (ECQIP) to identify an improvement programme to address the increasing activity and challenges within the organisation. The programme is led by the Director of Integrated Care and Emergency Services and the clinical lead is the Associate Medical Director. This programme of work has been supported by a service improvement facilitator with the assistance of funding from QuEST in 2012-13.
Problem
Increasing demand on A&E services particularly with the demographic changes associated with the aging population, impact of increased demand on capacity and resulting inefficiencies caused by high occupancy levels, including boarding of patients outwith specialty.
Aim
ECQIP was set up to:
- improve the quality of care for patients needing emergency care
- retrieve the standard that 98 per cent of patients will wait less than four hours from arrival to admission, discharge or transfer within A&E
- test new ways of working in relation to the development of the combined assessment unit planned for University Hospitals Crosshouse and Ayr and planned for autumn 2015 and 2016, supported by Building for Better Care
Action Taken
Under ECQIP a number of projects were identified and using PDSA methodology, the service improvement facilitator has supported operational managers and clinicians to identify, plan and implement improvements, monitoring progress and evaluating outcomes.
The outcomes from these projects are reported on an on-going basis via the service improvement plan.
Results
An assessment area has been introduced in University Hospitals Ayr and Crosshouse allowing GP referred patients to go direct to the assessment area and be reviewed by a consultant physician who will carry out real-time assessment.
This process of assess and then admit has proved successful and reduced the time for first consult and increased the number of patients being discharged home.
Patients were waiting between two and 20 hours to see a consultant physician. The pilot was trialled using PDSA methodology and introduced as a new way of working in January 2013. With the introduction of continuous real-time assessment, patients were seeing a senior decision-maker in approximately five hours. This new process removed the 'batched' ward rounds and improved the quality of care for patients. This is a more satisfying way of working for staff and the rate of discharge from the assessment area was around 40 per cent therefore reducing the number of admissions and creating capacity within the organisation.
These new ways of working are closely supported by the clinical lead and service improvement facilitator, due to inability to recruit consultant physicians. This assessment area is currently working Monday - Friday 11am - 8pm when possible. It is anticipated to extend the hours and include weekends once consultant physicians are in post.
Efficiency Savings and Productive Gains
As ECQIP is still in progress, efficiency savings have not been realised as yet. However, it is anticipated that the improvements from this programme for the patient, staff and organisation will be hugely beneficial.
Sustainability
The sustainability of new ways of working will be supported by the service improvement facilitator and will be continually measured to ensure that the improvements are sustained.
Continuous engagement with medical, nursing and diagnostic staff is imperative to support this initiative and continues on a regular basis.
Lessons Learned
NHS Ayrshire and Arran has highlighted that the management of this programme through a clinical lead and service improvement facilitator has worked very well and enabled the delivery of a number of changes that have resulted in improvements.
NHS Fife: Fracture Pathway Redesign
Background/Context
Traditionally, patients with a limb fracture will first attend an NHS emergency department (ED) and most non-operative fractures will then be referred to a fracture clinic for review by a specialist orthopaedic team. Various audits from across the country have identified that current fracture pathways lead to patients having unnecessary visits to hospital, waiting in clinics only to be informed that their problem will resolve without intervention, or ending up on a delayed pathway.
Problem
Discussion with NHS Fife orthopaedic consultants suggested that there were referrals from ED which were not necessarily required to be seen in an orthopaedic fracture clinic. However there was no current objective data to support this perception.
To establish the size and nature of the problem 125 referrals from the ED department at the Victoria Hospital, Kirkcaldy to the NHS Fife orthopaedic fracture clinics were screened by three orthopaedic consultants during the month of July 2012. The referrals were reviewed to ascertain, based on the information available, the most appropriate pathway for that patient referral. Data collected included clinic date, consultant clinic, patient's name, date of birth, diagnosis, and prospective patient pathway/exit route based on information from the ED referral card and whether the patient was appropriate for orthopaedic fracture clinic.
The analysis identified that 35.6 per cent of patients could potentially have been managed under the care of their General Practitioner or discharged from ED with an advice leaflet. 41.6 per cent were identified as appropriate for further care from an orthopaedic consultant. The results suggested that it was worth undertaking a pathway redesign for patients with suspected fractures presenting at ED, provided the appropriate infrastructure was in place.
Aim
Fracture pathway redesign is a key priority area of the Scottish Orthopaedics Services Development Group.
The aim of the pathway redesign was to implement the principles of the Glasgow Royal Infirmary fracture clinic model based on the principles of the Institute of Healthcare Improvement: safe, effective, patient-centred, timely, efficient and equitable. A patient-focused approach to managing fractures in a safe and efficient way.
Action Taken
We agreed some core principles for the pathway redesign:
- standardisation of the treatment of common injuries with a clear and comprehensive range of management options
- the only reason for a patient to be seen in a fracture clinic is 'for something to be done' either for assessment and/or an action
- many patients can be seen, treated and discharged from the ED with suitable advice, and if appropriate, a removable Velcro splint rather than plaster
- the visit should add value to their management
- the patient should see the most appropriate health professional at the correct time
- there should be an 'open door' for any patient wishing to access the service at any time
- consultant (subspecialist) led agreement of patient protocols/pathways
- prevent unnecessary delays to intervention where required and more efficiently utilise fracture clinics
- eliminate duplication and use technology to streamline the process
- regular audit of the service using a real-time database, including patients' outcomes and satisfaction using telephone standardised questionnaires
Method
Our method was to learn from others in Scotland and then start testing and adapting these ideas to our local systems and processes.
Learning from Others
- conference call with NHS Greater Glasgow and Clyde colleagues
- team meeting with ED consultants/orthopaedic consultants/outpatient charge nurse/orthopaedic project lead to identify the stakeholders involved in the process
- link with national fracture pathway redesign facilitator
- site visit to Glasgow Royal Infirmary
Testing and Adapting to Our Local Systems and Processes
- revamping NHS Greater Glasgow and Clyde fracture leaflets, working with NHS Fife orthopaedic and ED consultants
- collaborative working with IT to develop clinical pages
- health records processes
- template changes
- data collection
- set up telephone hotline
- order 'tenner boots' and paediatric splints
- identify phasing and dates
We stratified the patients to test and implement the new pathway.
Testing of phase 1 of the redesign began in November 2012 covering patients with specific fractures such as avulsion fractures of 5th metatarsal head, 5th metacarpal neck fractures, undisplaced radial head fractures, and mallet deformity of the finger, being discharged from A&E with comprehensive advice leaflets, and where appropriate, a removable splint rather than a plaster so that the patient does not need to re-attend for plaster removal.
Testing of phase 2, implementation of virtual fracture vetting, was started in February 2013. From this date patients who have fractures who would normally be considered for attendance at a small fracture clinic are booked into a virtual fracture clinic. The consultant virtual fracture clinic occurs three times a week and consists of a review of the medical record and x-ray. The management plan for each patient is recorded and an experienced nurse then phones every patient to inform them of the plan and discuss it with them.
Results
The following results were achieved:
- good training experience for registrars
- team approach to redesign with collaboration across directorates
- good use of 'small test of change'
- developing nursing roles
- presented the 'Fife Experience of Fracture Redesign' at the National Supporting Group
Efficiency Savings and Productive Gains
The data for phase 1 of the redesign is currently being analysed but there is some indication that there has been a reduction in small fracture clinic attendance.
Sustainability
Further work on the pathway redesign includes:
- full evaluation of fracture redesign and impact
- development of nurse led foot and ankle dressing clinic
- development of a scaphoid pathway
- evaluation of clinic capacity
Lessons Learned
Lessons learned include:
- education is important to the concept of reducing variation and standardising treatment pathway
- communication and involvement with all stakeholders is crucial
- small group problem solving meetings with link person create ideas to test
- there is always a solution worth trying
- it takes time to get everyone on board
- baseline data and data collection processes are essential to understand size and scale of the problem
- need a link person to keep change on track and energy up
- you can plan but it is not until you start the process that some issues may surface
- importance of enthusiasm by staff on the 'shop floor' to make changes
NHS Lanarkshire: Clinical Decisions Unit: Hairmyres Hospital
Background/Context
Hairmyres Hospital has experienced challenges to deliver against the four hour emergency care standard. Waits for beds had led to congestion in the emergency department (ED) and difficulties with flow within the ED itself.
Providing rapid access to assessment for GP patients and ambulatory care alternatives to medical admissions were identified as interventions which would assist with streamlining the patient journey.
Data analysis identified that a joint assessment area for GP referrals, a clinical decisions unit (CDU), and a short stay facility would vastly improve the pathway for patients accessing acute medical review.
Problem
Data informed that there has been a 16 per cent rise in all emergency admissions in the past five years at Hairmyres Hospital, which equates to an additional six admissions per day since 2007. All GP referrals were admitted through the ED, causing congestion. Access block was an issue in the ED, with patients waiting prolonged periods for access to beds and delays for GP referred medical patients to be seen by a senior clinical decision-maker. Achieving performance against the four hour standard challenged the site to be innovative in development of a service developed in partnership between two specialties, both concentrated on delivering high-quality care, improved patient experience, and enhanced patient flow.
Aim
The overall aim of the project and the new unit was to:
- improve patient access to acute medical services at Hairmyres Hospital
- improve patient experience - all care will be patient-centred and no patient will be kept in hospital longer than is clinically necessary
- offer rapid streamlined specialist assessment
- initiate investigation, treatment and a management plan
- provide care for patients who need a period of observation, treatment or a diagnostic test that is likely to lead to a discharge within 12/24 hours
- increase the site performance with the unscheduled care target
- decrease clinical risk
- provide rapid senior clinical decision-making support
Action Taken
A multi-disciplinary project implementation team was developed to open a new unit in November 2012 with:
- A joint assessment bay (JAB) - six emergency care trolleys and waiting room for emergency medical and surgical referrals from primary care.
- A clinical decisions unit - two four-bedded shared rooms for patients who meet the criteria for the operational clinical protocols in the unit. The unit would commence with four clinical protocols in the first instance: non-traumatic chest pain, DVT, cellulitis and seizure. Pathway documentation would support focused management together with specialist in-reach where appropriate. The unit is jointly run by emergency medicine and medical consultants.
- Five general medical side rooms.
The project implementation team developed a range of workflows to ensure all aspects of opening a new unit were considered and completed as part of an overall project task matrix. These included:
- staff recruitment and training - nursing, and admin and clerical
- standard operating procedures (SOPs) developed
- development of clinical protocols for the clinical decisions unit
- development of a new cardiology in-reach service for this unit as well as the acute medical receiving unit (AMRU)
- information services - changes to the patient management system (Trakcare)
- support from laboratories and radiology
- support from pharmacy
- support from hospital cleaning and linen services
- medical staff rota
- equipment purchase
- hospital ward moves to facilitate the best location for the new unit
- communication plan - to ensure all relevant stakeholders are informed i.e. other ward areas, GPs
- support from the Scottish Ambulance Service
- support from the emergency referral centre (ERC) to direct flow from primary care to the joint assessment bay
Results
The new unit was opened in November 2012.
Daily data is being captured within the unit and a database is currently being established to provide effective audit of the impact and performance of the unit.
Initial CDU Data
Data are available for the first 33 operational days:
- during this time, 169 patients were managed in the CDU
- mean activity - five patients per day
- maximum activity - 11 patients per day
- staff experience - feedback has been very encouraging and this unit has seen a positive impact on the flow within the A&E department. This has been the experience of both medical and nursing staff within the A&E department
Cardiology
A cardiology in-reach service also formed part of this project and this has proved to be very successful:
- data has shown that over a 51-day period, 163 patients were referred for cardiology review (from both AMRU and the CDU)
- of this total number, only two of these were deemed inappropriate
- 52 per cent of the patients seen by cardiologists were discharged same day in contrast to before the intervention when patients would wait to be transferred to a cardiology ward before being seen
This has led to faster access for patients to a consultant cardiology review and clinical decision-making.
Sustainability
This unit was opened as a one year pilot and plans are currently in place to provide robust data and information pertaining to the performance of the unit as well as the patient experience.
For the clinical decisions unit, further clinical protocols have been developed and are continuing to be implemented to include a wider range of clinical conditions that can be admitted to the unit. Work continues to increase access to this unit.
Lessons Learned
- Robust project management was required to bring together the complex workflows. Engagement of supporting services was critical to success.
- Protection of the assessment area function is critical in times of increased demand for beds.
- Good communication and an understanding of accountability and responsibility were imperative to the delivery of this multi- functioning unit.
- Effective clinical partnership working was required to deliver a shared model of clinical responsibility.
- At the end of this pilot all aspects of the project will be assessed and evaluated and a detailed account of all aspects of the unit will be developed for continued improvement.
NHS Lothian: Outpatient Antimicrobial Therapy (OPAT)
Background/Context
For many patients, intravenous antimicrobial therapy needs to be prolonged and thus dictates the length of their hospital stay, e.g. bone and joint infections (BJI), endocarditis, vascular device infections and meningitis. In other patients, admission to hospital is for the sole purpose of administering IV antibiotics, and these individuals are otherwise mobile and self-caring (e.g. skin and soft tissue infections (SSTI), Lyme disease, some HIV-associated opportunistic infections).
It is recognised that a significant number of patients who were being treated as inpatients would be more appropriately cared for in an outpatient setting, with resulting benefits in improved patient experience, efficiency gain through 'bed days saved', and reduction in the risk of hospital associated infection (HAI).
Problem
Inpatient antimicrobial therapy had been the traditional way of delivering this treatment. It was agreed that an invest to save project, established for one year, would be the best way to test the viability of an outpatient service.
Aim
The critical element of this redesign is that wherever possible patients will be treated in an outpatient facility instead of an inpatient setting. There are two strands to the redesign:
- Strand 1 - increase in 'avoidance of admission' as part of the ambulatory care programme. Patients are referred directly to outpatient antimicrobial therapy (OPAT) at initial point of contact, and are not admitted to hospital unless absolutely necessary.
- Strand 2 - decreased length of stay through the transfer of treatment from inpatient to outpatient at the earliest opportunity.
Action Taken
The OPAT service was initiated in January 2011 using a non-recurring investment of £359,000 through NHS Lothian's invest to save programme. The service is consultant led and nurse managed.
The investment funds 5.6 WTE nursing staff, two sessions of pharmacy staff time, drugs and consumables, and some patient transport costs. The service is delivered in a modified area within the Regional Infectious Diseases Unit at the Western General Hospital.
Results
The development of an OPAT service for NHS Lothian has enabled safe and effective management of a myriad of infections, allowing patients to remain in their own home, reducing exposure to healthcare associated infections, improving the quality of the healthcare experience and increasing the number of people with complex healthcare needs receiving care at home.
A recently completed patient satisfaction survey provided the following response (sample of questions asked):
- the overall median satisfaction score was 95 per cent
- 95.6 per cent strongly agree or agree treatment outcome was good
- 95.6 per cent strongly agree or agree it was better to be at home rather than in hospital to receive treatment
- 100 per cent strongly agree or agree the care given during visits to the OPAT centre was satisfactory
Some direct comments left by patients:
- "The care I received was exceptional and so much better than being admitted."
- "Efficient and helpful. The feeling of expert help is very reassuring."
- "Thanks to the service I have recovered in a much shorter time than previously expected. Thanks again."
Efficiency Savings and Productive Gains
Performance monitoring is undertaken by analysing the number of patients treated by the OPAT service who would otherwise have been admitted to hospital and treated as an inpatient. The target trajectory applies an average length of stay based on the type of infection identified for each patient. This is measured against the actual number of patients treated and the duration of their treatment. This methodology gives a total number of bed days 'saved' which can be attributed to the most likely hospital site of admission and specialty. The saved bed days are identified on a virtual basis; since avoidance of admission and reduced length of stay does not directly correlate to a reduction in actual bed occupancy, which remains subject to the impact of wider demand factors. Chart 8 shows the projected number of bed days saved (3,276 days), and the actual achieved (4,719 days).
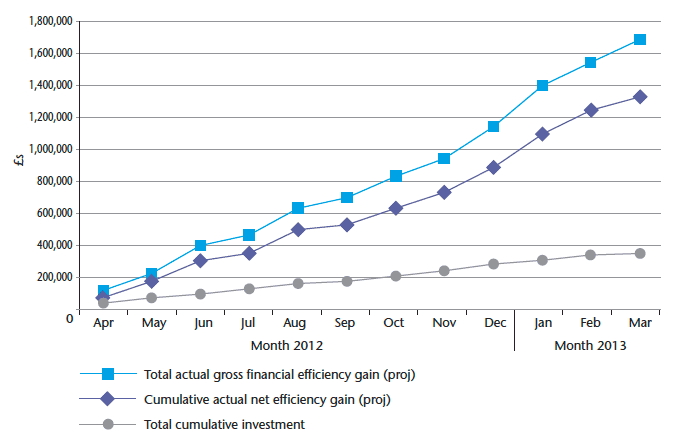
Chart 9 shows the financial evaluation of bed days released. This is the full cost per day for an acute medical admission based on the NHS Cost Book (£360). This figure has been used to calculate both the savings and the original target set against the project. The financial evaluation is used as a performance indicator to reflect the impact of changes to resource utilisation and demonstrate the efficiency gain.
The net productive gain based on bed days saved and the cost per day for a bed is £1.34 million. This is net of the annual cost of the OPAT service (£360,000).
The capacity which has been released is being used to meet demand for inpatient beds on the acute sites.
Sustainability
The funding has been agreed on a recurring basis to maintain and further develop the OPAT service. There are further areas, including acute oncology and treatment of bronchiectasis which will be developed during 2013-14.
Lessons Learned
Clinical leadership is critical to success. The development of an OPAT service in NHS Lothian had the benefit of a consultant who initiated and led the redesign.
The success of the redesign was dependent on a steady and increasing flow of patients who would otherwise have been admitted to hospital. Significant work was required to build clinical relationships, and raise both awareness and confidence amongst clinicians across the system.
Chart 8: OPAT Cumulative Activity April 2012 - March 2013
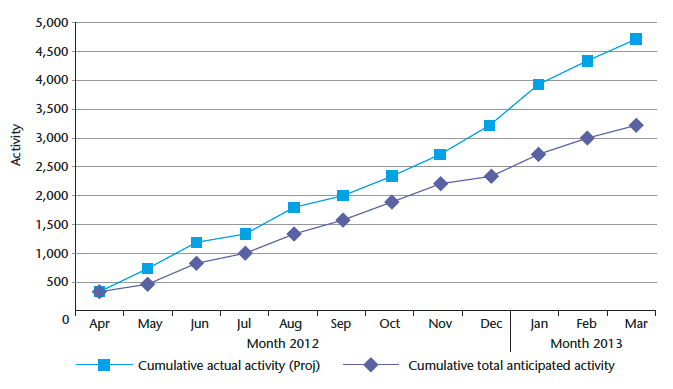
Chart 9: OPAT Investment and Efficiency Gain April 2012 - March 2013
NHS National Waiting Times Centre Board: Streamlining Job Plans across Surgical Specialties and Anaesthesia
Background/Context
This work commenced following a review of the current patient flows including bottlenecks and scheduling. We used the job planning review as an opportunity to smooth the activity flows across the week. We also reviewed the requirements for additional/ ad hoc theatre sessions and streamlined these into fixed and sustainable sessions. In addition this allowed an opportunity to ensure sufficient protected time for continued medical education requirements.
Problem
The key problem arose following a review of the existing patient flows and scheduling, where it became apparent:
- there were bottlenecks within the system due to consultant availability working between theatre and outpatient times
- there was also significant variation between surgical and anaesthetic job plans, which needed to be realigned to deliver a more efficient work plan for the weekly theatre slots
- an increasing number of additional theatre sessions being put in place at a premium cost
Aim
The aim was to produce a higher quality patient-centred journey by reducing bottlenecks within the patient pathway and reducing theatre cancellations.
There was also a plan to become more efficient with our current resources by reducing the requirement for extra theatre sessions at a premium cost and assess the need to convert these into permanent planned sessions and reduce the level of premium rates paid.
Action Taken
The revised job plans facilitated the following:
- consultants being in outpatient clinics in the same day as their patients were being pre-assessed for surgery
- better realignment of surgeons and anaesthetist job plans to match theatre schedules
- more flexible sessions were put in place reducing the need for extra theatre sessions at an additional cost
- transferring premium ad hoc theatre sessions into planned sessions
Results
The outcome of the actions aims to demonstrate a more efficient use of medical time, this is measured through:
- a reduction in theatre cancellations resulting in improved efficiency for the organisation
- any issues at pre-assessment stage can be addressed as quickly as possible which aims to reduce unnecessary hospital admissions
- an improved patient experience with fewer cancellations and a more streamlined approach to pre-assessment and outpatient consultations
Efficiency Savings and Productive Gains
There has been a reduction in costs as a result of implementing this project which equates to a total saving of £240,000 per annum. This is primarily delivered through a reduction in the premium rate theatre sessions and replacing these with planned sessions with substantive posts. In addition, there is a reduction in cancelled theatre sessions. The productivity savings for medical staff have not as yet been quantified but would be significant.
Sustainability
The revised job plans have been put in place and supported our workforce plans. The cancellations and theatre slots continue to be reviewed on a weekly basis through the routine performance management processes.
Lessons Learned
The project has demonstrated improved quality benefits and increased efficiency. In terms of lessons to other NHS Boards the key critical success benefits are: ensure full staff engagement, clearly demonstrate the patient quality benefits and commit time to understanding the current bottlenecks within the system.
Contact
Email: Dayna Askew