Healthcare quality and efficiency support team: annual report 2013
Annual report in relation to improving the quality and efficiency of healthcare in Scotland.
Prevention and Early Intervention
NHS Lanarkshire: Inpatient Falls Project
Background/Context
NHS Lanarkshire's Quality Hub has identified inpatient falls as one of the top five priorities. The Quality Hub has supported the funding of a small team of subject matters experts to examine this area of work in patients aged over 65 years, using SPSP improvement methodology over a six month period in the first instance. This commenced in October 2012 and has been extended to March 2014. The improvement team consists of physician, senior nurse (full time secondment) and clinical quality manager along with front-line nurses, AHP, physicians and overseen by a quality improvement advisor.
Problem
NHS Lanarkshire reports 5,000 inpatient falls per year and this has been constant for the last three years:
- 2010-11 - 4,572
- 2011-12 - 5,026
- 2012-13 - 4,732
Falls can cause serious injury, both physical and psychological. Falls also increase healthcare costs and increase hospital stay.
Aim
The project aim is to improve assessment and introduce preventative measures to reduce the number of inpatient falls using the evidence based FallSafe bundle, previously piloted in England and Wales:
- to have 95 per cent compliance against the falls bundle measure by April 2014
- to decrease the rate of total falls (measured by all falls in a month over total occupied bed days) by 50 per cent in April 2014 (October 2012 base line)
- to demonstrate a trend of an increase of the days between a fall with moderate or major harm by October 2013
Action Taken
Using patient safety methodology the bundle was first tested in a medicine for the elderly rehabilitation ward in Hairmyres, whose cohort of patients are at high risk of falls.
Background data was collected by the project team, shared and displayed. Stakeholder interviews were undertaken with staff, patients and carers.
A quality improvement approach was taken:
- identify where changes could be made
- establish the measures
- select the change
- test the change through PDSA cycles
- implement/spread changes
Weekly feedback was provided to staff, and there was visibility of the team in the clinical area.
Monthly meetings, including all members of the project team, were held.
The concept of falls champion in each ward was already established through the existing inpatient falls group, but there was a lack of structured education and support.
Monthly educational and supportive meetings with falls champion, chaired by senior nurse and medical consultant leads commenced April 2012.
Education in quality improvement methodology is also included to front- line staff.
An additional element was added to the existing bundle - the nurse confirms via a sticker on the medicine cardex that the full medicine cardex review has been carried out in relation to risk of medication that contributes to falls.
Results
The compliance with all elements of the FallSafe bundle in November 2012 was 0 per cent and moved to 95 per cent by April 2013 for the pilot ward. Spread to the second ward results mirrored the pilot ward.
We are at phase 2 spreading to six additional wards. The falls champion along with the senior nurse collected background data, rather than the senior nurse completing this section alone. Phase 3 commenced in June 2013 and Hairmyres implementation was completed by August 2013.
The spread to the second and third acute site is planned, enabling the completion of spread by end March 2014.
The data in charts 18-20 is for the pilot ward.
Efficiency Savings and Productive Gains
Efficiency is improving the patient experience and over time demonstrating, through the monitoring and support and education of the multi-disciplinary team, that inpatient falls, causing moderate and serious harm will reduce.
In time, reducing length of stay will improve efficiency and quality.
Sustainability
The commitment of senior management, on-going support for clinical staff to have the time for education, and on-going development in this subject is included within our older people strategy.
A designated person is available on each hospital site to support and provide on-going development and education to the falls champion to spread good practice in their team.
Clinical quality staff will continue to be visible and accessible to clinical staff.
Chart 18: Received all core bundle elements
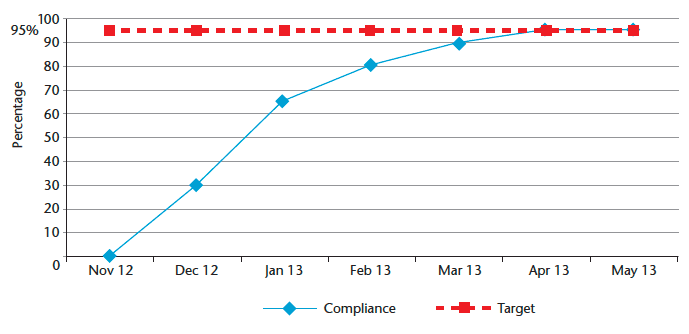
Chart 19: Falls rate per 1,000 bed days (injury only)
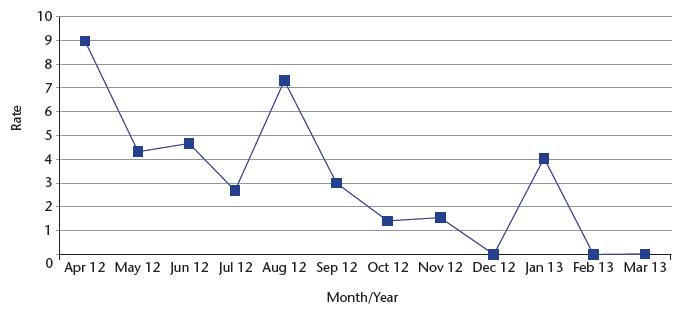
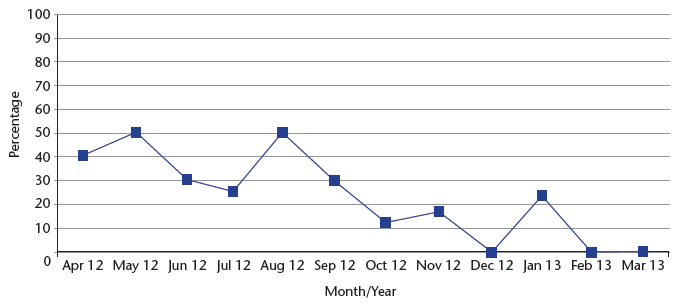
Chart 20: Percentage of falls resulting in injury
Lessons Learned
For the senior nurse on secondment, this has been a great opportunity to consolidate previous education on Lean/PDSA methodology and enable concentrated work, focused on a specific topic.
This model of having clinical quality as part of the project team rather than from afar providing data has been exceptional. The multi-disciplinary team having equal involvement from the beginning has been pivotal to the progression, and in the timeframe suggested.
Clinical staff feel supported and confident to discuss test of change with peers.
Contact
Email: Dayna Askew