Healthcare quality and efficiency support team: annual report 2013
Annual report in relation to improving the quality and efficiency of healthcare in Scotland.
QuEST Programmes
Efficiency and Productivity Portfolio Office

Linda Semple
0131 244 2297
linda.semple@scotland.gsi.gov.uk
The Efficiency and Productivity Portfolio Office (EPPO) is part of QuEST and supports the national programmes and NHS Boards to improve efficiency and productivity by:
- providing a national overview of efficiency and productivity across all NHS Boards and programmes
- developing an approach to 'doing' efficiency and productivity, including tools available on the Quality Improvement Hub website
- identifying areas with the greatest potential productive opportunity through benchmarking and data analysis
- coordinating networks across NHSScotland to encourage sharing of learning, resources and expertise
- signposting to support and information resources
- undertaking knowledge management activity such as horizon scanning, identifying and spreading best practice, capturing and sharing knowledge and learning, and feeding into strategic partnerships such as the Quality Improvement Hub, the Joint Improvement Team (JIT) and the Quality Unit
Achievements 2012-13
- During 2012-13 the EPPO refreshed the Efficiency and Productivity Portfolio of programmes. This included changes to the way in which support to programmes is delivered and changes to the governance and scrutiny of the Portfolio to ensure that key objectives are met.
- The EPPO has established an Efficiency and Productivity Leads Network. Every NHS Board has nominated a key individual(s) to act as the primary contact within their Board in relation to efficiency and productivity. The first Network event was held in January 2013 and focused on sharing good practice and innovative ideas and exploring some of the challenges around increasing efficiency and productivity while improving quality.
- The EPPO has established an approach for testing small changes to drive efficiency and productivity where these do not logically fit within one of the larger QuEST programmes, for example using health economics to quantify the benefits of improving diabetes care in Scottish hospitals or assessing the efficiency and productivity benefits of NHS Boards moving towards a paperless system.
- Health economics can inform and improve decision-making about the allocation of scarce healthcare resources. The EPPO in partnership with NHS Health Scotland has developed a Health Economics Network with the aim of facilitating collaboration between the health economics academic, policy and practice communities across the health system in Scotland to develop the use of health economics evidence by policy makers and practitioners.
- The QuEST web presence on the Quality Improvement Hub website has been refreshed as a key medium for communicating with our stakeholders, including providing access to quality and efficiency tools, techniques and information.
- The Danish Government is currently developing its own national plan for health. A highly successful visit to Copenhagen, as invited guests of the Danish Government, was undertaken to exchange knowledge and showcase the quality and efficiency work being done in Scotland.
- The Health Services Journal (HSJ) has acknowledged the excellent work undertaken by QuEST and NHS Boards to realise significant efficiency savings whilst also improving quality of healthcare. Following a submission by the EPPO, QuEST was shortlisted for an HSJ Efficiency Award.
Priorities 2013-14
- The EPPO will lead the refresh of the NHSScotland Efficiency and Productivity Framework for SR10 to ensure it continues to reflect the context within which NHSScotland operates, and provides practical tools and guidance to support NHS Boards to deliver high-quality and efficient healthcare.
- The EPPO will work with QuEST National Programme Leads to refresh the role and remit of QuEST to ensure that our work continues to be focused on supporting NHS Boards to deliver NHS priorities, whilst also horizon scanning to discover innovations internationally, nationally and locally, to identify and test good practice to spread across NHS Boards.
- The EPPO held a major event in August 2013 which focused on the use of data and information to drive quality, efficiency and productivity and brought together colleagues working in the fields of quality improvement, efficiency and productivity, health intelligence, health economics, finance, performance management and planning.
- The EPPO will lead the Soft Facilities Management Programme, to optimise synergies between this Programme and the Facilities Shared Services Programme which focuses on hard facilities management. The Soft Facilities Management Programme will involve a strategic review of catering, laundry, domestic, portering and retail provision across NHSScotland.
Outpatients, Primary and Community Care

Susan Bishop
0131 244 2019
susan.bishop2@scotland.gsi.gov.uk
Key Drivers
- The Outpatients, Primary and Community Care Programme supports NHS Boards and local partnerships to move care closer to home and enable more people to receive the right care, from the right person, at the right time, in the right place.
- The Programme supports teams and networks across outpatient services, primary and community care to work together to understand and diagnose system issues, design and innovate, and use continuous quality improvement to deliver excellent safe, effective and person-centred care.
- Each of the three streams of work includes a focus on reducing variation, waste and harm and making best use of resources including the time of patients, the public and staff.
Programme Aims
- The overall aim of the Programme is for more people to receive the right care, from the right person, at the right time, in the right place.
- This is reflected in the Transforming Outpatient Services driver diagram (figure 1).
Key objectives for work in Community Care are to:
- partner JIT in supporting planning and implementation of Reshaping Care for Older People Pathways, including the design and delivery of the Reshaping Care Improvement Network and evidencing impact of improvement
- commission and deliver support for sustaining and spreading the use of Releasing Time to Care
Key objectives for work in Primary Care are to:
support the delivery of a reduction in variation, waste and harm through better use of data, peer review and development and improvement of patient pathways
design and test new models of care and concepts of service delivery that make best use of resources and improve the flow of patient pathways through the health and social care system
Programme Workstreams
Transforming Outpatient Services
All NHS Territorial Boards working with some of the NHS Special Boards are engaged in:
- adopting, spreading and sustaining reliable high impact changes
- increasing the quality and use of data for peer review, benchmarking, and understanding and managing demand and capacity
- design and innovation in the way outpatient services are provided (clinicians, managers, patients and public representatives working together to imagine the future for those services that we currently recognise as outpatient services and generating new concepts, designing and testing prototypes)
Four commissioned NHS Boards will also lead projects to innovate through technology, improve utilisation of resources and rapidly test and spread reliable improvements.
Figure 1: Transforming Outpatient Services
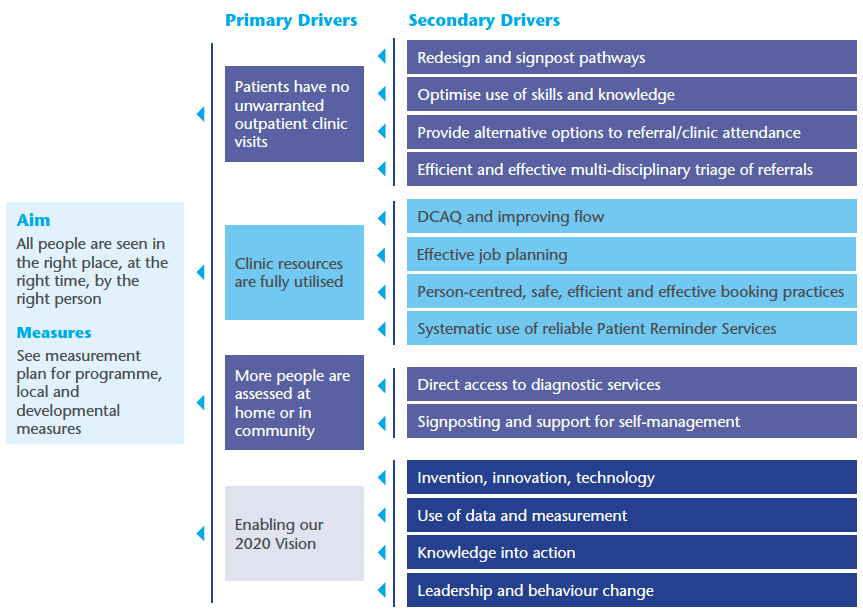
Primary and Community Care
The Primary and Community Care workstreams deliver projects and support to reduce unwarranted variation and waste, release time to reinvest in patient care and design and test new ways of working.
In Primary Care, working closely with the Scottish Government's Primary Care Division, this includes:
- supporting the design and delivery of the Quality and Outcomes Framework (QOF) Quality Product Indicators
- exploring the use of data and improvement tools
- supporting General Practices in the systematic use of Lean in the form of Productive General Practice
Achievements 2012-13
Key achievements to date include:
Transforming Outpatient Services
- publication of Towards Our 2020 Vision
- testing to identify five reliable and sustainable high impact changes to spread within and across all NHS Boards
- NHS Grampian (digital information and tailored postcards) and NHS Lanarkshire (self-care planning for skin conditions) designed potential technology solutions to enable people to access outpatient support to self-manage
- teams in NHS Highland increased availability and use of appointment slots, case notes and the clinic environment
- NHS Lothian introduced the use of advice only requests in a number of specialties and initiated review of consultant to consultant referrals
- innovation and learning sessions
Community Care
- commissioning of a cost consequence analysis of anticipatory care planning with polypharmacy and a planning tool to aid partnerships in development of anticipatory care planning
- commissioning Healthcare Improvement Scotland (HIS) and NHS Education for Scotland (NES) to implement Stocktake Report recommendations and support NHS Boards to spread and measure the impact of Releasing Time to Care
Primary Care
- over 200 General Practices using Productive General Practice tools as part of Local Enhanced Services
- over 400 General Practices registered to use Productive General Practice
- joint implementation support from QuEST and the Royal College of General Practitioners Scotland
- integration of the Primary Care Patient Safety Programme's SafeQuest tool into Productive General Practice
Priorities 2013-14
Transforming Outpatient Services
- adoption and spread of five high impact changes (use of advice only, clinical dialogue and referral feedback, centralised and eTriage, improved booking practices and use of reminder services, direct access to diagnostics and musculoskeletal redesign)
- continue to support four commissioned NHS Boards to generate new evidence base and rapidly share and spread learning
- increase the quality and use of data for peer review to understand and reduce unwarranted variation and to inform and test improvements
Community Care
- commissioning HIS and NES to produce resources to support sustainability of Releasing Time to Care and transition to use of Releasing Time to Care as business as usual for NHS Boards, and in partnership with JIT, test the use of the tools and approaches to support development of integrated health and social care teams
- supporting design and testing of new models of care, ways of working and technologies, and evidencing the impact of improvement
Primary Care
- supporting the design and delivery of the QOF Quality Product Indicators for anticipatory care planning/polypharmacy review and outpatient referrals
- delivering Managing Patient Flow, a project to test and extend the use of data and improvement tools to improve patient flow within primary care and across secondary care-primary care interfaces
- continuing to integrate Productive General Practice and other improvement programmes and initiatives
This report includes the following case studies from NHS Boards in relation to Outpatients, Primary and Community Care:
- NHS Highland: Why Did the Patient Cross the Road? Because their Rehab was on the Other Side!
- NHS Western Isles: Community Nursing Patient Held Record and Digital Pen Technology
- NHS National Services Scotland (Scottish National Blood Transfusion Service): Transforming the Donation Experience
- Scottish Ambulance Service: Scheduled Care Project
Acute Flow and Capacity Management

Jane Murkin
07748 335 549
jane.murkin@scotland.gsi.gov.uk
Key Drivers
The 18 Weeks Service Redesign and Transformation Programme supported NHSScotland to deliver the 18 Weeks Referral to Treatment (RTT) Standard in December 2011.
The 18 Weeks Service Redesign and Transformation Programme was primarily focused on elective care and there was an increasing desire to broaden the focus on whole hospital flow and capacity management. This was driven by a need to improve flow and to make best use of capacity to ensure acute services can meet the growing demands of the population whilst maintaining a high-quality and efficient service.
Building on the achievements of the 18 Weeks Service Redesign and Transformation Programme, the Acute Flow Capacity Management Programme was initiated. This Programme ensured a continued focus on improvement areas on which NHS Boards were working, to support delivery of access standards which were not yet consistently and uniformly applied across the service.
Programme Aims
The aims of the Acute Flow and Capacity Management Programme were to:
- increase use of day and short stay surgery models
- embed a sustainable approach to demand and capacity planning at sub speciality level
- optimise the management of inpatient capacity, including the use of beds and theatres
- accelerate the roll-out of Enhanced Recovery in surgical specialities
- optimise the management of queues and pathways in high volume specialities, such as orthopaedics
- sustain delivery of acute access standards
- horizon scan to discover innovations internationally, nationally and locally to identify good practice to spread across NHS Boards
Programme Workstreams
The Acute Flow and Capacity Management Programme comprised the following workstreams:
- Day and Short Stay Surgery
- Demand and Capacity Planning
- Enhanced Recovery
- Inpatient Capacity and Flow
- Orthopaedics
- Theatres
Achievements 2012-13
Some of the key achievements of The Acute Flow and Capacity Management Programme are as follows:
- The national team supported NHS Boards to set up local infrastructures to implement and spread Enhanced Recovery in Colorectal, Urology, Gynaecology, Breast and Orthopaedics. This included providing national support for spreading and sharing best practice across NHS Boards, for example through the Programme Managers Network. Most NHS Boards now have Enhanced Recovery programmes in place which are providing improved quality of care for patients. Local achievements include:
- establishment of local measurement databases
- development of standardised pre-operative education for patients and carers, including producing DVDs and YouTube videos to support effective communication
- multi-disciplinary team working
- development of standardised pathways
- establishing processes to collect and audit patient experience, which is used to support further improvement
- supporting a culture which empowers patients to be partners in their own care
- The national team developed Demand, Capacity, Activity and Queue (DCAQ) methodology to support NHS Boards with capacity planning and delivery of waiting times targets. The methodology is supported with a suite of modelling tools which help to produce DCAQ analysis at subspecialty level enabling NHS Boards to evidence pressure areas within their service and to support job planning processes. The national team also provided tailored support to a number of NHS Boards where the DCAQ tools and methodology were utilised to help improve performance against waiting times targets. In order to help embed robust capacity planning through DCAQ in NHS Boards and develop peer networks, training was provided for NHS Board analysts. The team also delivered a two day technical workshop which analysts from most NHS Boards attended.
- An annual Day Surgery Conference was held in October 2012 in partnership with the British Association of Day Surgery (BADS) to promote day and short stay surgery and allow the sharing of national data and best practice.
Priorities 2013-14
Designing care systems with effective patient flow is critical to the delivery of NHSScotland's Quality Ambitions of safe, effective and person-centred healthcare.
Poor flow can lead to failures, increased costs, poor quality and poor patient experience. Moreover, evidence links poor flow and sub-optimal scheduling in healthcare to an increase in mortality, adverse events, readmissions and poor financial performance.
It is observed that a high level of variation remains in the way demand is managed within healthcare systems. Although natural variation will always exist, artificial variation should be reduced, smoothed and eliminated. Significant progress has been made by NHS Boards in improving flow; however, there are still opportunities for improvement and spread of good practice.
Building on the work done through the Acute Flow Capacity Management Programme, a new programme of work has been initiated to respond to these challenges.
The Whole System Patient Flow Programme will move away from focusing on a specific area of flow (i.e. unscheduled or elective flows) in isolation and will adopt a whole system approach to patient flow designed to ensure patients receive the right care, at the right time, in the right place, by the right team.
The Whole System Patient Flow Programme will test, implement and spread an approach that will optimise and improve flow across the whole system through the application of operations management science. The national team will lead this work in partnership with NHS Boards and a technical partner. The aim of this work will be to successfully test, implement and spread an operations management approach that will optimise throughput and improve flow across the whole system as well as improve the experience of both patients and staff and improve patient safety by reducing variation. Successful implementation will be a crucial element of the programme and will require executive, middle management, and clinical leadership and engagement at local Board level to support successful testing, implementation and spread.
The Whole System Patient Flow Programme is currently being established, and key priorities for 2013-14 include:
- proof of concept work to test an innovative approach to improving whole system patient flow will be piloted in four NHS Boards (NHS Greater Glasgow and Clyde, NHS Tayside, NHS Forth Valley, and NHS Borders) with a plan to spread across NHSScotland
- an improvement programme and approach to ensure a focus on, and spread and sustainability of:
- Day surgery
- Day of surgical admission
- Enhanced Recovery
- Non-operative fracture pathway redesign
- testing a flow, cost, quality improvement programme in one health system similar to the Health Foundation's Flow, Cost, Quality Programme
Programme visuals are set out in figure 2.
Figure 2: Whole Systems Patient Flow Improvement Programme
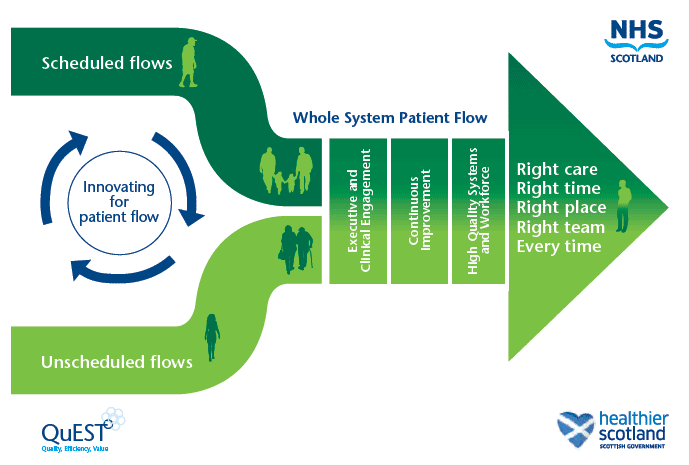
Case Study Example
NHS Greater Glasgow and Clyde developed a new, innovative model of care for patients with non-operative limb fractures. Traditionally patients with a non-operative fracture present at the Emergency Department and are referred to a Fracture Clinic within a few days of injury. However, many of these patients were discharged after the first visit to the Fracture Clinic with no change to their treatment. Unnecessary attendance at the Fracture Clinic results in increased demand and longer waiting times.
In order to address these issues the Fracture Service at Glasgow Royal Infirmary and Stobhill Minor Injuries Unit redesigned the patient pathway. Patients are now either discharged directly by the Emergency Department supported by standardised information of self-care using advice leaflets (around 38 per cent of patients) or are reviewed at a virtual clinic by an Orthopaedic Consultant via PACS (around 62 per cent of patients). Of these patients around 40 per cent are discharged by telephone and the remaining 60 per cent of patients are referred to see the appropriate specialist. This approach has a key benefit of freeing up staff time so that it can be used elsewhere in the department.
This transformational change has led to a safer, more patient-focused, efficient and clinically effective process. There has been interest in this model of care from both Scotland and England and other NHS Boards are implementing a similar model including NHS Tayside, NHS Dumfries and Galloway, NHS Fife, NHS Grampian and NHS Forth Valley.
This report includes the following case studies from NHS Boards in relation to Acute Flow and Capacity Management:
- NHS Ayrshire and Arran: Emergency Care Quality Improvement Programme
- NHS Fife: Fracture Pathway Redesign
- NHS Lanarkshire: Clinical Decisions Unit: Hairmyres Hospital
- NHS Lothian: Outpatient Antimicrobial Therapy
- NHS National Waiting Times Centre Board: Streamlining Job Plans across Surgical Specialties and Anaesthesia
Mental Health

Ruth Glassborow
0131 244 5142
ruth.glassborow@scotland.gsi.gov.uk
Programme Aims
- In 2012-13 the aims of the Mental Health Programme were to:
- Support NHS Boards to deliver a maximum waiting time of 18 weeks from referral to treatment for psychological therapies by December 2014 through:
- enabling the use of system improvement techniques in mental health including DCAQ theory
- ensuring clinical outcomes and service user experience data are routinely used to drive improvement.
- Lead the National Dementia Demonstrator Programme which is a partnership between three Health and Social Care Partnerships, QuEST, JIT, Alzheimer Scotland, the Scottish Government Mental Health Division, the Scottish Dementia Working Group and the Local Government Improvement Service. Its purpose is to show that it is possible to deliver better care for more people with the same or less resource by redesigning services and strengthening cross sector working across health and social care.
- Support NHS Boards to release efficiency and productivity savings in mental health services whilst maintaining or improving the quality of care.
Achievements 2012-13
Some of the key achievements of the Mental Health Programme are as follows:
- Working with NHS Lothian to complete the first full DCAQ analysis in a mental health service. This work has generated significant new learning on the application of these techniques to a mental health setting and has resulted in the development of a range of tools and guidance to support work across Scotland. QuEST's work in this area has also generated interest from mental health services in New Zealand where it has informed their national work around access to psychological therapies. A detailed report on this work can be found on the QuEST Mental Health web pages.
- The Programme continued to support the three National Dementia Demonstrator sites: Midlothian Community Health Partnership (CHP), North Lanarkshire CHP and Perth and Kinross CHP. Some of the highlights this year included the publication of the Midlothian Dementia Demonstrator Integrated Resource Framework 2008-09 data which has generated significant insights into the current resources used by people with dementia across health and social care; the Motherwell Dementia Friendly Community Initiative which has generated interest across the country and the piloting of Family Group Conferencing for people with Dementia in Midlothian. We were also delighted to see North Lanarkshire Dementia Demonstrator Site winning the COSLA Excellence Award 2013 One to Watch category, recognising the significant and innovative work that is taking place to redesign Dementia Services.
- Working jointly with four health and social care partnerships, JIT, NHS National Services Scotland Information Services Division (ISD), Alzheimer Scotland and the Mental Health Division to define the new Dementia Post Diagnostic Support HEAT Target. The project also involved working together to better understand the opportunities for delivering the target through the redesign of services across health and social care. Working in partnership with front-line health and social care teams to define the target has ensured that it is measured in a way that provides useful information that helps local services to drive forward improvements in care. Testing its application in advance helped us to understand some of the key challenges that services would face in meeting this target. It also enabled us to provide guidance and tools to support local partnerships to meet those challenges.
- Production of a range of tools/guidance to support NHS Boards to deliver HEAT Targets including efficiency and productivity savings. Examples include:
- Mental Health Pathway Efficiency and Productivity Report
- Effective and Efficient Community Mental Health Teams Toolkit
- a suite of tools to support DCAQ work - including the QuEST Mental Health DCAQ Tool
- Dementia Post Diagnostic Support Workforce Planning and Costing Tool
- examples of what data community mental health teams need to look at regularly to support improvement work and how it should be presented to maximise understanding
- A Mental Health National Learning Event was held in October 2012 which provided a forum to share practical experiences and ideas on how to deliver improvements which save money whilst also maintaining or improving the quality of mental health services. Feedback from attendees was extremely positive about the benefit of the day which also saw the launch of the new Effective and Efficient Community Mental Health Teams Toolkit. This new toolkit brings together a range of existing resources and tools, many of which have been developed by the QuEST Mental Health Team, into one accessible format. Responses have included 'tremendous piece of work' and 'thanks for all the work you've put into this, since it does make life a bit easier out here on the front-line'.
Priorities 2013-14
The priorities for the Mental Health Programme for 2013-14 are detailed below:
- Setting up the new National Dementia Care Improvement Programme in partnership with JIT will:
- support the delivery of the Post-Diagnostic HEAT target across all Health and Social Care Partnerships across Scotland
- support the test of Alzheimer Scotland '8 Pillars' model for in-community pilots
- support improvement in the care of individuals with dementia in acute hospitals
- work with colleagues in primary care to identify specific initiatives that can be taken forward to improve primary care services for individuals with dementia and their families
- test initiatives around community capacity and co-production
- managing the end of the National Dementia Demonstrator Programme including the production of an overall national evaluation report
- consolidating work around access to psychological therapies to enable delivery of the 18 weeks referral to treatment target
Case Study Example
Midlothian is one of three Dementia Demonstrator Sites in Scotland established following the launch of Scotland's National Dementia Strategy in 2010, to create better outcomes for people with a diagnosis of dementia with the same or less resource.
In Midlothian, the project seeks through a whole system approach (within existing resource constraints), to develop responsive services for people with dementia which support them throughout their journey from a diagnosis of dementia through to the end of life. To meet this aim the project has focused work across a number of different workstreams:
Mapping and Data Gathering
- The Firefly Research team within Queen Margaret University conducted an in-depth narrative study of the lived experience of individuals living with dementia and their carers in Midlothian. The findings were published in the International Psychogeriatrics journal and have been used to inform the redesign of services locally.
- Midlothian are using data generated through the Integrated Resource Project to better understand the local use of health and social care resources by individuals with dementia and from this to identify opportunities for redesign.
Post Diagnostic Support
To deliver the five pillars of post diagnostic support, the following services have been established:
- the new 'Link Worker' provides people with dementia and their carers with information and support for up to a year after they are diagnosed
- a new Local Area Co-ordinator for Dementia promotes access to activities in the community for people with dementia which suit their skills and interests
- a pilot of Family Group Conferencing is being conducted with people with dementia and their families to empower and support family based solutions to planning care and support
- to improve the support in the community and minimise unnecessary admissions to acute hospital, a self-management care plan is being piloted with clients referred through a local General Practice
Midlothian Single Dementia Service
- A joint multi-disciplinary dementia service is being developed in Midlothian to provide a single point of access for people with dementia and their carers with services and support from diagnosis to end of life.
- The development of the single service is supported by the newly established user and carer reference group. The group advises and influences the decisions being made around the new service in order to ensure that it is shaped around service users' and carers' needs and views.
Workforce Development
Workforce development will include:
- an audit of services including the private and voluntary sector, against the Standards of Care for Dementia in Scotland has been completed including a staff survey
- a training programme is being developed and delivered for professionals to improve their understanding of dementia and outcomes based approaches
This report includes the following case studies from NHS Boards in relation to Mental Health:
- NHS Borders: Analysis of Increasing Referrals into the CAMH Service
- NHS Borders: Incorporating Patient Choice in Appointment Allocation
- NHS Shetland: Mental Health (Administration Services and Clinical Governance)
- NHS Tayside: Child and Adolescent Mental Health Service
Cancer Performance Support

David Linden
0131 244 3288
david.linden@scotland.gsi.gov.uk
Key Drivers
Every year, about 30,000 people in Scotland are diagnosed with cancer and trends predict that the number is likely to rise to almost 35,000 in 2016-2020. The reason for this increase is that there are more elderly people in the population and life expectancy is increasing further.
Over the last 20 years, almost all cancers have shown improvements in survival five years after diagnosis and survival rates from cancer in Scotland are broadly similar to those in England and Wales.
The Cancer Programme focuses on three key areas:
- sustaining cancer waiting times standards performance
- Cancer Modernisation: further improvements in the effectiveness, efficiency and patient-centeredness of service delivery
- Detect Cancer Early: contributing to and improving five year survival from cancer for the population of Scotland, through earlier diagnosis and treatment
Programme Aims
Over the last few years, cancer services have developed and improved significantly with more doctors, nurses and other healthcare professionals and state-of-the-art equipment in all five cancer centres. The Scottish Cancer Taskforce Cancer Modernisation Programme aims to build upon the progress already made in effective and efficient cancer service delivery, further improving patient experience and patient outcomes, whilst managing the anticipated increase in cancer incidence.
The Detect Cancer Early Programme aims to increase the proportion of people diagnosed and treated in the first stage of breast, colorectal and lung cancer by 25 per cent by 2015.
Programme Workstreams
The Cancer Programme includes six main workstreams:
- Cancer waiting times performance support
- Detect Cancer Early Programme
- Acute oncology service delivery
- Surgical oncology, including enhanced recovery after surgical treatment
- Radiotherapy, including the capacity and capability for radiotherapy treatment
- Transforming Care After Treatment
Achievements 2012-13
The key achievements of the Programme to date include:
Cancer Waiting Times Standards Performance
NHSScotland achieved and sustained performance above 95 per cent in all quarters against the 31-day cancer access target and in most quarters against the 62-day target throughout 2012. During the final quarter, October - December 2012, 95.8 per cent of patients started treatment within 62 days of urgent referral with a suspicion of cancer. Within the same period, 98.1 per cent of patients started treatment within 31 days of decision to treat, irrespective of the route of referral.
Cancer Modernisation
- The development and piloting of the 24-hour cancer treatment helpline
- The Radiotherapy Programme Board (RTPB) was established in June 2012 to drive forward improvement work across Scotland. The RTPB reports to the Scottish Cancer Taskforce. A cohesive work-plan has been developed and implementation of the RTPB's objectives is supported by the wider Radiotherapy community. RTPB priority areas of work include:
- development of national pathways to ensure equity of access to new innovative techniques and technologies
- continued development of workforce capacity and capability
- development of evidence based consensus treatment protocols and pathways
- robust patient engagement to better understand and improve the experience of radiotherapy
- development of future models of working that meet the rising incidence of cancer and radiotherapy demand
- promotion of clinical trials and research, and the unique opportunities that exist within Scotland
- proactive commitment to exploring new technologies and techniques to ensure Scotland's radiotherapy programme is up-to-date and well-prepared
- collaboration with our NHS colleagues across all UK countries, and Europe, to better understand the cost benefits of radiotherapy
Transforming Care After Treatment Programme
The Transforming Care After Treatment (TCAT) Programme was launched in May 2013 and aims to ensure that people diagnosed with cancer are prepared for and supported to live with the consequences of the diagnosis and its treatment.
To achieve this aim, Macmillan Cancer Support is working in partnership with the Scottish Cancer Taskforce and providing up to £5 million in funding over the next five years, supporting clinical teams and other partners to review, redesign and test new approaches and models of cancer care after treatment.
The Programme will focus on the redesign of current models of cancer follow-up, managing the transition between acute care and home, and enablement and support for effective self-management.
It will seek to build upon what has already been achieved in Scotland and other parts of the UK and also contribute to the delivery of the Quality Strategy. The timing of this development coincides with a growing appetite for greater collaboration and mutuality across the public sector.
The Scottish Cancer Taskforce will monitor progress of the programme to ensure that there is delivery against focused, evidenced outcomes that will inform on-going commissioning of services.
Detect Cancer Early
Key achievements of the Detect Cancer Early Programme include:
- development and launch of priming, breast and bowel cancer social marketing campaigns
- development of systems and processes for data collection to support the detect cancer early HEAT target
- development and implementation of nGMS contract element to support primary care contribution to increasing bowel screening programme participation
- a programme of work is being taken forward to refresh the GP Referral Guidelines for Suspected Cancer and provide education sessions for primary care professionals
- funding to support diagnostic and treatment capacity building has been released to NHS Boards
Priorities 2013-14
Priorities for 2013-14 include:
- Sustain cancer waiting times standards performance
- Cancer Modernisation
- roll-out of cancer treatment helpline
- continue to support efficient and productive radiotherapy treatment delivery
- support Transforming Care After Treatment pilot projects
- Detect Cancer Early
- develop lung cancer and breast screening social marketing campaigns
- support NHS Boards to build capacity in diagnostics and work towards HEAT target achievement
- build upon impact of social marketing campaigns to date
- continue to support NHS Boards around diagnostic and treatment capacity building
Prescribing

Simon Hurding
0131 244 2397
simon.hurding@scotland.gsi.gov.uk
Key Drivers
NHSScotland spends around £1.3 billion a year on medicines. Of this expenditure, around £1 billion is spent on medicines dispensed in primary care and just over £300 million a year is spent on medicines in hospitals.
Despite much work over the last 10 years to improve prescribing practice in primary care, there is still significant variation in the quality of prescribing and cost-effectiveness.
The Prescribing Programme has been set up to ensure medicines are used appropriately and that cost-effective choices are made.
Programme Aims
Improve the quality and cost-effectiveness of prescribing by:
- identifying the major improvement opportunities in Scottish prescribing
- resolving issues that need to be addressed at a national level
- monitoring progress and sharing learning between NHS Boards
Programme Workstreams
The Prescribing Programme includes five workstreams:
- National Therapeutic Indicators
- Polypharmacy
- National Prescribing Policy
- Waste and Repeat Prescribing
- Development of Prescribing Advisor Networks (e.g. Scottish Prescribing Advisers Association)
Achievements 2012-13
The key achievements of the Programme to date include:
- National Therapeutic Indicators (NTIs) have been set up to provide benchmarks across primary care prescribing in Scotland. NTIs identify major areas where there is variation in prescribing quality and help GPs understand and apply the latest clinical evidence. Prescribing information is used to encourage General Practices to move towards the 'best' quartile of prescribers. In addition to savings in 2012-13 from patent expiries, there have been underlying efficiency savings of almost £8 million as a result of changes in prescribing behaviour.
This includes almost £3 million from using more evidence based cholesterol lowering drugs, plus reductions in inappropriate prescribing of high dose inhaled steroids, dipyridamole, quinine and anti-microbial wound products. - Providing a plan to tackle polypharmacy. Polypharmacy is the term for patients receiving lots of medicines. Almost half of Scots aged 65 and over are now prescribed five or more medicines. It is important to be sure the benefits of these medications do not outweigh the potential side effects and drug interactions.
It is important to review patients who are taking multiple medications to ensure those medicines are still needed and to check they are not causing problems. Guidance was issued in 2012 to NHS Boards in Scotland about the management of polypharmacy. This has been supported in the 2013-14 GP contract.
Priorities 2013-14
The key areas of focus for the coming year will be:
- NTIs will be refreshed for 2013-14 and work will be undertaken to continue to embed these in prescribing practice.
- Work will be undertaken to support the implementation of polypharmacy reviews and to measure the impact of the reviews on patient safety.
- Waste occurs from medicines that are dispensed to patients but not taken. Tools and guidance are being developed to help General Practices identify preventable waste in their repeat prescribing.
- Prescribing guidance is being developed for five specific clinical areas where opportunities exist to improve product choice, based on clinical evidence and cost-effectiveness. This includes respiratory, diabetes, oral nutritional supplements, wound management, and gluten free products.
Case Study Example
Audit Scotland published a report Prescribing in General Practice in Scotland in 2013 and recognised improvements in prescribing efficiency over recent years. We have worked with NHS Boards to build on this good practice and have provided the impetus and framework for NHS Boards to implement and sustain improvements.
NHS Fife has implemented the NTI guidance in relation to drugs to reduce cholesterol. This leads to more people receiving drugs with a strong evidence base, at lower cost. A saving of between £210 and £314 per patient per year has been identified, resulting in over £1 million being saved for NHS Fife.
This report includes the following case studies from NHS Boards in relation to Prescribing:
- NHS Ayrshire and Arran: Pharmacist Led Review of Patients Prescribed Last-Line Antimicrobials
- NHS Forth Valley: GP Prescribing Incentive Scheme
- NHS Greater Glasgow and Clyde: ScriptSwitch Software Implementation across Inverclyde CHCP and East Dunbartonshire CHP
Procurement
Key Drivers
Virtually all NHS Board activity involves the requirement to procure some form of product or service meaning spend with suppliers is approximately 20 per cent of NHSScotland's total budget.
NHSScotland spends £2.1 billion per annum on goods and services from around 10,000 suppliers. Currently about £1.5 billion of this spend is influenced nationally, regionally or locally by the procurement community.
As such, efficient and effective procurement is imperative.
Programme Aims
Our Procurement Programme aims to drive increased value from NHSScotland spending as well as supporting economic growth. This will be achieved through improving processes and tools, obtaining reductions in price, influencing demand, working closely with suppliers and creating new and improved structures.
Focus Areas
Focus areas for the Procurement Programme include:
- ensuring a higher percentage of total spend is covered by an appropriate procurement process and increasing the level of national contracting activity
- improving current contract conformance and compliance levels
- driving further savings from existing national and local contracts while improving quality through initiatives such as Intensive Improvement Activity (IIA)
- developing regional procurement consortia (the East of Scotland Procurement Consortium and West of Scotland Procurement Consortium) to drive economies of scale, share expertise, reduce costs and improve capability and capacity
- continued roll-out of eProcurement systems and a National Spend Dashboard to support management decision-making
Achievements 2012-13
Some of the key achievements of the Procurement Programme are as follows:
- The East of Scotland Procurement Consortium has delivered £4.7 million through implementing national contracts and £670,000 through regional contracting and joint working in 2012-13, with a further £4.5 million in savings targeted in 2013-14. Additional efficiency gains of £100,000 in resource savings per annum have also been achieved by sharing management and operational resources between NHS Lothian and NHS Tayside, with further resource saving opportunities identified for 2013-14 between NHS Highland and NHS Grampian.
- The West of Scotland Procurement Consortium has delivered over £4.6 million in savings during 2012-13 as a result of implementing national contracts and better buying decisions - better deals from existing suppliers or better value for money products from new suppliers. It is targeting a further £5 million saving during 2013-14.
- Development of a National Spend Dashboard, building on existing systems, to increase availability and use of management information to support decision-making.
- 14 Intensive Improvement Activity events have been undertaken to improve procurement capability and to identify savings opportunities. Three commercial review engagements have been undertaken and have identified £4.7 million of savings opportunities so far.
Priorities 2013-14
Some of the key priorities for the Procurement Programme in 2013-14 are outlined below:
- implementation of NHSScotland Procurement Framework which will give strategic direction and a performance framework for the function
- a review of Procurement structures across NHSScotland will be undertaken to identify the optimum structures that could drive increased savings and effectiveness
- regional consortia will continue to create consistent operational practice and systems, build procurement capability by sharing best practice, exploit economies of scale to deliver savings and share workload to improve capacity
- National Procurement will continue to deliver Intensive Improvement Activity (IIA) to support NHS Boards to identify additional savings opportunities, increase procurement capability, and improve performance
- during 2013-14, the National Spend Dashboard will be tested with four pilot NHS Boards (NHS Tayside, NHS Highland, NHS Forth Valley and NHS Greater Glasgow and Clyde) with an aim to roll-out the Dashboard to all NHS Boards by December 2013
Case Study Example
Prior to the West of Scotland Procurement Consortium Continence Product project, suppliers had regularly demanded unrealistic price increases, quoting supply and production costs.
Following a retender by National Procurement, the West of Scotland Procurement Consortium Project Team worked with National Procurement and the National Distribution Centre (NDC) to promote a single supplier fixed price award contract for all west of Scotland Boards.
Expert end users from each NHS Board were appointed to a Technical User Group decision-making group, and following the completion of a mini-competition, SCA Molnlycke were appointed to supply all continence products to west of Scotland acute hospitals via the NDC and direct to patients via their direct delivery service.
The combined efforts of this group approach released over £1.2 million back to patient care across the west of Scotland.
This report includes the following case study from NHS Boards in relation to Procurement:
- NHS National Services Scotland: Modernisation of Home Oxygen Service
HR Shared Services

Lynn Marsland
07500 033 738
lynn.marsland@nhs.net
Key Drivers
Best practice from industry and the wider public sector suggests there may be a better way of working; the majority of organisations across a number of sectors (including health) have already implemented or are exploring shared service operating models.
This is supported by a desire to improve quality and to increase the professionalisation of the HR service for NHSScotland.
It is recognised that within HR there is already collaboration around workforce planning in particular, along with other HR initiatives, at regional level. In 2012, the implementation of a national single instance HR system (eESS) commenced, enabling standardisation, sharing of information, links to other workforce related IT systems and consistency of HR transactional processes across all NHS Boards. This builds upon the successful implementation of Financial Shared Services for NHSScotland.
There is an on-going focus on maintaining and delivering front-line services within NHSScotland and as a result it is necessary to develop a sustainable and efficient HR service for the future.
The underpinning ethos of the Shared Services agenda is:
- Simplify: processes and procedures are as lean as possible minimising inappropriate waste
- Standardise: variation between NHS Board areas and individual users is minimised or removed
- Share: where there are benefits in doing so, processes are delivered from fewer locations or once for the whole of Scotland
Programme Aims
The Programme has been established with the high level objectives of ensuring that the appropriate development of HR Shared Services:
- improves the quality and efficiency of HR services delivered to customers
- improves the governance of HR and workforce related services and activities
- improves the resilience and sustainability of HR services
- delivers redesigned HR service processes which are effective, efficient and productive
- ensures the maximisation of business systems integration opportunities (e.g. eESS, ePayroll)
Programme Workstreams
Phase 1 of the HR Shared Services Programme has focused on the following areas:
- Recruitment
- Employee Services
- Medical Staffing and Trainees
These three areas cover approximately 50 per cent of HR activity in NHSScotland.
A further workstream focused on Payroll and Benefits Advice will progress following the roll-out of ePayroll across NHS Boards.
In addition, the programme may develop a workstream focused on Training, Development and Education which covers a further 14 per cent of HR activity undertaken in NHSScotland.
Achievements 2012-13
The key achievements of the Programme to date include:
- Visible ownership of the Programme by HR Directors, supported by a common understanding of shared service models and how they operate. HR Directors are providing strategic leadership and are focusing on the potential for overarching HR transformation.
- Significant engagement in the baselining and benchmarking exercise, which has provided, for the first time, a complete and robust picture of HR and HR related activity across the whole of NHSScotland. This data will be used to identify opportunities for improvement, including quick wins and longer term benefits which can be realised by developing a model of shared services.
- Increased senior staff understanding of the potential of shared services gained by examining other models, identifying and sharing best practice.
Priorities 2013-14
The key areas of focus for the coming year will be:
- building on the activity scoping work previously undertaken, to develop options for appraisal and a supporting business case
- engaging in a more detailed data verification and analysis exercise with NHS Boards based on that already captured through the baselining and benchmarking exercise earlier in 2013
- working with the eESS project team as it rolls out the single national HR system to ensure standardisation of processes and to ensure benefits of the new system are identified, tracked and realised
Case Study Example
The case studies below are examples of how the HR Shared Services Programme could develop, based on shared services principles and practices that have already been adopted at the local level.
NHS Grampian currently provides HR services to NHS Orkney through a service level agreement (SLA). Although some HR support is still available locally, the SLA with NHS Grampian enables NHS Orkney to access the full breadth of specialist HR services, demonstrating the benefits of exploiting economies of scale and adopting a 'centre of excellence' approach.
NHS National Services Scotland (NSS) have implemented an HR Service Centre Model supported by a call logging case management system. NSS is a national board covering a wide geographical area which makes it challenging to provide access to HR support at every location. NSS has restructured its HR Service so that all staff, regardless of location, have access to the same quality of HR service.
This report includes the following case studies from NHS Boards in relation to Shared Services:
- NHS Borders: Local Forensic Learning Disability Service
- NHS Orkney: Contracting Out Payroll Services
Facilities Shared Services

Douglas Seago
01463 705 801
douglas.seago@nhs.net
Key Drivers
The key drivers for change were identified by Directors and Heads of Facilities Services across NHSScotland, these include:
- skills shortages and a need to share scarce specialist resources
- a need to develop services, building on models of good practice already extant in NHSScotland
- a need to reduce variation and exploit the economies of scale offered by NHSScotland
- a need to share intelligence amongst NHS Boards regarding major contracts
- changes in legislation and government policy in relation to recycling and improved environmental standards
Programme Aims
There are a number of overarching objectives for the Facilities Shared Services Programme:
- improve the quality, efficiency and resilience of facilities services
- support change in healthcare delivery and where possible accelerate change
- ensure that facilities services are fit for purpose to support NHS Boards to deliver the 2020 Vision
- build on the opportunities offered by wider collaboration with public and private sectors
- ensure better use of specialist resources, ensuring specialist skills are shared across NHS Boards
- ensure compliance with the Waste (Scotland) Regulations 2012
These objectives are supported by a number of workstream specific objectives:
- ensure the capital programme is delivered
- ensure proper skills are available for delivering maintenance
- ensure better investment of capital in relation to sterile services
- improve procurement for transport
- Increase contract management capacity and capability
- ensure compliance with the Waste (Scotland) Regulations 2012
Programme Workstreams
The Facilities Shared Services Programme comprises five key workstreams:
- Capital and Hard FM
- Sterile Services
- Transport
- PPP
- Waste
Achievements 2012-13
The key achievements of the Programme to date include:
- Extensive data collection has been undertaken in relation to the Capital and Hard FM workstream, including reviewing the skill mix and age profile of the workforce to assess preparedness for delivery of a changing care environment (capital programme) to meet the requirements of the 2020 Vision and ensure sustainability for the future.
- Ensuring service engagement with the solutions that are identified through use of the technical advisory structure of Health Facilities Scotland (HFS). This, combined with full partnership engagement through Scottish Partnership Forum (SPF), has enabled the process to be well advised and fully transparent.
- In addition to fleet management, the Transport workstream has developed a logistics subgroup to examine the delivery of goods and services from the NDC and the 'final mile distribution' from local hubs to patient care facilities. This has involved working with National Procurement and other logistics services to ensure a joined up approach and reduction of duplication. A more efficient logistics service also has the added environmental benefit of a reduced carbon footprint.
- Working with Zero Waste Scotland we are preparing a national service for health to meet the new requirements of the Waste (Scotland) Regulations 2012 to effectively segregate recycleate into its constituent parts to reduce waste going to landfill and potentially generate income from waste.
Priorities 2013-14
The key areas of focus for the coming year will be:
- the Transport and Fleet Management Working Group will identify a common specification and procurement policy for all vehicles, with the aim of reducing variation across NHSScotland and maximising the procurement benefits
- NHSScotland will be compliant with the Waste (Scotland) Regulations 2012 as they apply from January 1, 2014
- there will be effective benchmarking of sterile services departments across NHSScotland and assessment of the capital investment necessary to continue to deliver services which are compliant with all current legislation and mandatory standards
- development of an effective communications plan to ensure that all staff affected, or potentially affected, by changes emanating from the Programme are fully informed and engaged in the process from the development of options to delivery of solutions
- alignment with the Soft Facilities Management Programme, to optimise synergies between the two Programmes of work
Case Study Example
By pulling together contract management expertise from NHS Lothian and working with the Scottish Futures Trust (SFT), effective negotiations with a PPP provider has resulted in savings of £495,000 for NHS Lothian in relation to the Edinburgh Royal Infirmary contract.
The experience gained will be spread across the service to ensure this good practice is consistently embedded nationally. This expertise will be used to negotiate with contractors as and when PPP contracts are reviewed.
This report includes the following case studies from NHS Boards in relation to Shared Services:
- NHS Borders: Local Forensic Learning Disability Service
- NHS Orkney: Contracting Out Payroll Services
This report includes the following case studies from NHS Boards in relation to Estates and Facilities:
- NHS Borders: Hawick Inpatient Facilities
- NHS 24: Facilities Management Contract
- Healthcare Improvement Scotland: Accommodation Rationalisation
Performance Support

Martin Hopkins
0131 244 5178
martin.hopkins@scotland.gsi.gov.uk
Key Drivers
The QuEST Performance Support team continues to support NHS Boards to deliver HEAT targets and standards which contribute towards delivery of the Scottish Government's Purpose and National Outcomes; and NHSScotland's Quality Ambitions.
The key drivers of the team are:
- the Performance Support team maintains a flexible response to NHS Boards encountering difficulty in delivery
- to bring together external expertise and facilitate a mechanism for collective support
- to provide a detailed analysis of local operational data, known as 'walking the patient pathway'
- supporting the exchange of ideas with staff providing the service
- identifying recommendations for NHS Boards to implement, and identify additional support as necessary
Programme Aims
The QuEST Performance Support Programme aims to help NHS Boards to achieve key Scottish Government objectives.
Further aims are:
- to provide a mechanism of finding collective support and opportunities for NHS Boards to focus jointly on areas of concern such as the HEAT targets
- to assist in drawing together resources to support NHS Boards by making connections between experts and staff
- to aid NHS Boards in the understanding and analysis of patient 'pathways', which may result in more rapid identification of inconsistencies and delays
- to collate data for the informed evaluation of improvement and performance measures
- to identify and offer further avenues of support for implementation such as timely assessment, appropriate interventions and use of specialist skills
- to stimulate the development of pathways to community support
Programme Workstreams
The responsive nature of the Performance Support Programme accommodates a range of skills. NHS Boards are able to access the skills and time of the Performance Support team when needed.
Support available via the Programme includes:
- Seeking out partners and expertise on behalf of NHS Boards to focus skills on the area of concern. In some areas the Programme has assisted in creating professional networks of support and creating local champions to sustain change.
- The collection and analysis of data via the Programme has assisted in the facilitation of informed discussions between NHS Boards and stakeholders and assists in raising issues beyond the local area if necessary. The collection of data assist in identifying patterns and trends in an unbiased manner that NHS Boards, clinicians and other stakeholders have found valuable.
The process of working with the Performance Support Programme is shown in figure 3.
Figure 3: Performance Support Process
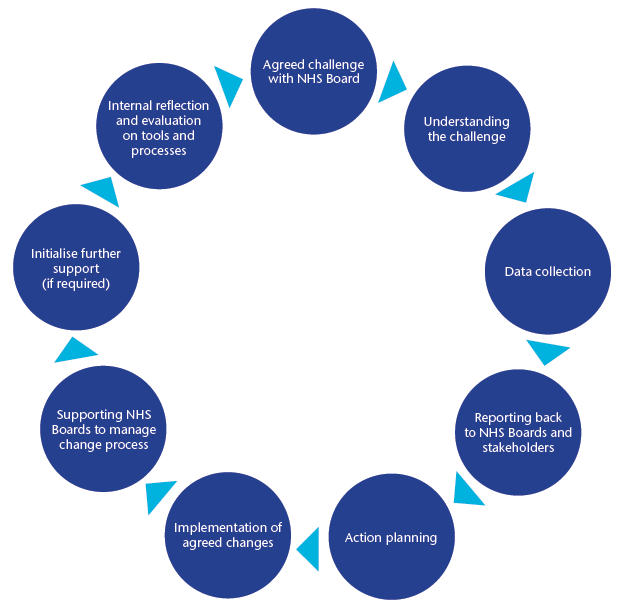
Achievements 2012-13
The achievements of the Performance Support Programme 2012-13 included sustained work in Scotland but also providing advice to health systems in England and Australia.
The Programme also spent time drawing together learning from their supportive work throughout the year and identified ways of moving towards deeper customised analysis of the data collected.
The Programme has become more accomplished in the analysis of large data sets and creating clean operational data that is more easily scrutinised by NHS Boards and other stakeholders.
The Programme has become more adept at exploring patterns and trends within data and sharing knowledge with NHS Boards and stakeholders to increase awareness and support informed change.
Priorities 2013-14
Throughout 2013-14 the Performance Support Programme will offer support to NHS Boards in a flexible way that offers guidance and balance to the requirements of improvement and performance.
Further priorities in 2013-14 for the Performance Support Programme are to:
- continue to provide responsive support that is informed and flexible for NHS Boards
- continue to improve the understanding of data to identify emerging priorities for NHS Boards and other stakeholders
- continue to work closely with the Scottish Government in improving the quality of care, including accomplishing HEAT targets
- support broader plans and wider ambitions for improvement and performance objectives
Case Study Example
During 2012-13 the Performance Support Programme undertook an exploration of 'boarding', reporting to the Scottish Medical and Scientific Advisory Committee (SMASAC) and informing guidance to NHS Boards for winter planning.
Demand for hospital services continually changes. Hospital patients are sometimes treated in areas not designed, staffed or equipped for their specific care needs. The need to understand the consequences of such patient boarding was a common issue raised during recent performance support visits as well as successive national winter reviews, with implications for future planning and improvement.
The team reviewed the limited evidence available, a new paper for which has been submitted for publication in November 2013. The Performance Support team also agreed with ISD and clinical experts to implement this operational definition of inpatient boarding:
"A boarder is a patient who occupies a borrowed bed.
This includes patients in beds who are:
1. managed by an individual consultant or consultant team outwith the main allocated inpatient area for that consultant, or patient speciality
2. transferred to any non-inpatient bedded area (for example day units)"
Inpatient boarding levels for each acute hospital are now reported to the Scottish Government within weekly monitoring returns. This, together with monitoring of compliance with the four hour Emergency Department Standard, 12 hour Emergency Department length of stay breaches and numbers of hospital discharges delayed in excess of four weeks, represents near real-time intelligence regarding flow across transitions of care, and thus planning and management of capacity within hospitals.
The detrimental effect of boarding on both boarded and non-boarded patient outcomes was investigated through analysis of large datasets. This is the first such multi-centre analysis of its kind and preliminary results have been presented to SMASAC and winter planning conferences.
Detailed results have been presented at the Royal College of Physicians of Edinburgh Consensus Conference in November 2013 and will be submitted for peer reviewed publication. These will include: what types of boarding for which patients were found to be most harmful or disruptive; and queue modelling to estimate what level of capacity with what degree of specialisation would be expected to minimise boarding and 'turnaway' rates for patients. Both elements have provided insight for planning and prioritising improvement.
Contact
Email: Dayna Askew