Undergraduate medical education: recommendations
A series of recommendations to increase undergraduate medical education in Scotland by enabling more general practice based teaching in primary care.
Chapter Two: Challenges and Facilitators to Increasing Undergraduate Education in Primary Care
There is a range of UK and international evidence on factors that affect career choice among undergraduate medical students. Understanding these drivers, both negative and positive, is essential in developing approaches which actively encourage students to consider general practice as a career choice. Equally, there are a range of organisational and structural issues that can impact on teaching capacity at both medical school and practice / community level. These issues are explored in more detail below and help inform both the approaches to innovative practice highlighted in section 4 and the recommendations that follow.
Influences on career choice
The ambition to increase the primary care workforce and deliver increased education and training in community settings has to be considered in the current context of a range of challenges including addressing widely held negative perceptions of careers in general practice. In a response to a crisis of GP numbers more than twenty years ago, Sullivan and Morrison (Sullivan and Morrison, 1997) suggested that medical schools needed to 'broaden the range of entrants, make general practice attachments mandatory and at least six weeks long'. We have come a long way since 1997, but the journey is not yet over.
Student perceptions
The Royal College of General Practitioners and Medical Schools Council's (RCGP/MSC, 2017) Destination GP report found a range of issues relating to promoting general practice as an excellent career choice.
Peers and role models
Peers at medical school are one of the most influential groups on students' views of future career choices. However, over 9 in 10 (91%) medical students believe their peers hold negative views about general practice. The RCGP/MSC analysis reported that students are most likely to associate the profession with being "boring", "lower status than other medical professions" and "less intellectually challenging". It is concerning that students' peers' attitudes towards general practice are much more likely to have a negative impact on students' likelihood of pursuing a career in general practice (33%) than a positive one (13%). There is therefore a pressing need to challenge these perceptions.
The RCGP/MSC survey also found that GP tutors in medical schools have a particularly positive impact, with 71% of students saying this group made them want to work in general practice more (only 12% saying the opposite). GP Society events also appear to have a positive impact, with 41% of students saying attending had a positive influence on their interest in general. This is reinforced by positive feedback from a successful recent Scottish Universities GP society event in Aberdeen. (see boxed text on p 42).
Clinical placements:
Previous studies (Alberti et al., 2017; Wiener-Ogilvie et al., 2015) found the presence or quantity of undergraduate placements in general practice to be associated with increased entry to general practice training and careers. The RCGP (RCGP/MSC, 2017) found that GPs interacting with students on placements are the most influential group on students' perceptions of general practice, with four fifths (81%) of students reporting that this group had most influenced their perceptions. Similarly, Wiener-Ogilvie et (2015) survey of foundation trainee doctors across Scotland found "undergraduate GP placement was reported as the strongest influence in favour of a career in General Practice followed by discussion with family and friends and discussion with specialty trainees". This influence was particularly marked in graduates from Aberdeen and Dundee medical schools. In addition, the RCGP survey reports that those who say they are most influenced by GPs on placements are more likely than other students to associate general practice with the positive phrases such as "continuity of care" and "varied", and less likely to use terms like "boring" and "lower status". One Foundation Year doctor interviewed to inform this report noted:
In clinical years, so that is the final three years, I think I had a total of six weeks in general practice, out of three years. It actually wasn't that much and I would definitely have liked to have done more. I could have benefitted from more experience of general practice.
The quality of placements is also important. A focus group study of students from nine UK medical schools reported that they were more likely to pursue a career in general practice if their placements were of good quality, provided authentic practice experience and showed the impact which GPs can make. This is consistent with a Scottish study that found that Foundation Year doctors were more likely to consider a career in GP if they had had good quality experience of undergraduate general practice placement.
As well as quality of exposure itself, longitudinal placements (>6 months) are associated with increased likelihood of pursuing GP as a career compared to traditional block placements (Amin et al, 2018) and this may reflect their capability to deliver the experience students identify as influential to career choice. Longitudinal programmes are found to promote a number of characteristics including clinical responsibility, developing a broad skill set, patient-centred practice and holistic practice (Walters et al, 2012) which can all complement primary care practice. Research also suggests that longitudinal programmes can also lead to reduced exposure to potentially negative effects of institutional hidden curricula (Hirsh et al. 2012). Furthermore, longitudinal programmes claim to offer a nurturing environment by placing greater focus on strategies to deal with the challenges of primary care.
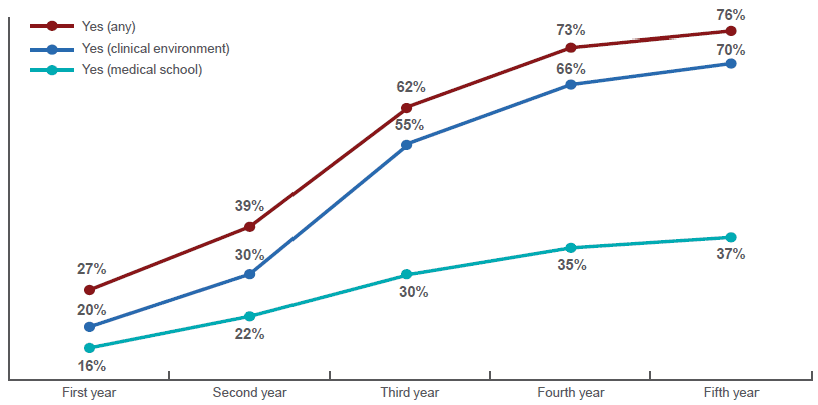
However, clinical placements are also known to expose students to negative views about general practice and this builds over their time in medical schools (RCGP/MSC, 2017). By their fifth year, three quarters (76%) of students have encountered negativity towards general practice from academics, clinicians or educational trainers. Seven in ten (70%) have encountered this in a clinical setting. The study showed that no less than 79% of students believe doctors and other staff on placements have negative associations with general practice. When the students' experiences of negativity towards general practice were examined, they most commonly cited issues concerned referrals (37%), which often involved secondary care clinicians criticising referrals they had received from GPs.
Figure 2: Whether students have encountered any negativity towards general practice from academics, clinicians and/or educational trainers over time (RCGP/MSC, 2017)
Attitudes within medical schools
Despite GPs comprising around 27% of the medical workforce, the UK's academic GPs account for only about 6% of all clinical academics. Academic leadership and role modelling is important to ensure that students recognise the breadth and complexity of general practice care, and that they become aware of and are stimulated by the complex intellectual challenges. GP academics will also play an important role in supporting undergraduate tutors to deliver high quality education (HEE/MSC, 2016).
Concerns about isolation
The RCGP report found that a concern around isolated working was the second most common reason given for not wishing to pursue a career in general practice, and that this concern built up over the students' time in medical school.
General Practice Perspective
As part of the work of the Group, a survey of current and anticipated future capacity in general practices to support undergraduate education in general practice in Scotland was conducted over the summer of 2018. The survey, which had an overall response rate of 44%, built on a previous survey undertaken in NHS Highland earlier that year. The key aim of the survey was to identify current and future teaching capacity, including perceived barriers and facilitators to increase teaching in primary care.
The majority (69%) of practices who responded to this survey are currently involved in undergraduate or postgraduate teaching at some level. About half of those who are not currently involved said they would like to be in the future, with a similar proportion saying they would not like to be involved (see Figure 3). Note that the question about future involvement was not asked of practices in NHS Highland.
Figure 3: Practice involvement in teaching
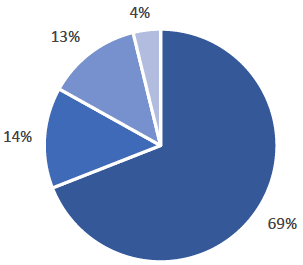
- Practice currently involved in teaching
- Practice not currently involved in teaching but would like to be in the future
- Practice not currently involved in teaching and would not like to be in the future
- Other
Likelihood of involvement in teaching varied according to the list size of practices. Practices with a list size of less than 4,000 patients were less likely to be currently involved in teaching than larger practices. Those practices which said that they currently had at least one GP vacancy were also less likely to be involved in teaching.
Critically, respondents described a tension between teaching and clinical service. This tension was manifested as competition for the resources of time and space which has been exacerbated by rising clinical workload and inadequate staffing levels in many practices. Respondents described staffing gaps or inability to secure locums as barriers to becoming involved in teaching. For some practices the pressures of providing clinical service alone or lack of time resource to adequately support teaching efforts was enough.
"I work full time in general practice and would very much like to teach. We had representatives from [Scottish University] attend and would like to offer us this. However, such is patient demand we would need to take on more staff and the costs would not be recuperated."
Four sets of factors were identified as potential barriers to teaching: organisation interface, practice, patient and personal.
Organisation interface
A range of perceived barriers to involvement in undergraduate teaching were reported, although many of these described perceptions of undergraduate teaching requirements which were factually misinformed (e.g. needing to have MRCGP, teaching always involves school holidays). This suggests a need to better inform the GP workforce on the range of teaching opportunities available as well ensuring ready access to accurate information on the different accreditation processes and qualifications required.
Other reported barriers included:
- Perceived onerous application and ongoing accreditation processes;
- Feeling disconnected from the teaching organisation;
- Structure of teaching.
Practice level
Many of the respondents described lack of space hindering development of teaching in their practice.
"Room space within the practice. We would like to be more involved and have the teaching capacity to do this but are constrained by our building and have not had any support from [NHS Health Board] to help accommodate more students/trainees."
Specific issues for more peripheral (including rural) practices included:
- Transport for learners;
- Learner preferences to be more central leading to fewer allocations;
- Multiple sites made teaching logistically more challenging for practices with branch surgeries;
- Accommodation costs needing to be met by some practices and the need to arrange accommodation were barriers.
These issues of limited space, GP shortage and accommodation costs are highlighted in the vignette from Biggar Medical Practice (page 28)
Some respondents felt that changes to clinical service delivery due to new developments could be detrimental to teaching. This included the move to a doctor first telephone triage system; recent practice mergers or practice collapses; practices becoming established as 2C practices having been taken over by the health board, thus creating uncertainty over future sustainability.
Patient factors
Increased patient demands, including more complex cases and increased frailty, were also noted to have increased pressure on practices. GPs were also mindful of not overburdening patients with teaching involvement (noting potential 'patient fatigue' with repeated requests for involvement with teaching).
Personal factors
Personal barriers mentioned included a lack of confidence, access to tutor training, enthusiasm and lack of experience. It was recognised that teaching can potentially be stressful and tiring. Working patterns were highlighted as an issue including several GPs identifying part-time or locum working as a barrier. A number of GPs mentioned career stage (early and late) as a potential barrier to taking on teaching commitments.
Respondents to the GP Capacity Survey were asked what would allow their practice to take on a role in medical education or increase current capacity to do so. The proposal which respondents felt would make the most difference to capacity was the backfill of GP time with locum provision, with 82% of respondents agreeing that this would be "highly likely" or "likely" to help. This was closely followed by 79% of respondents citing increased financial compensation for time lost to teaching.
Figure 4: Proposals to increase current capacity
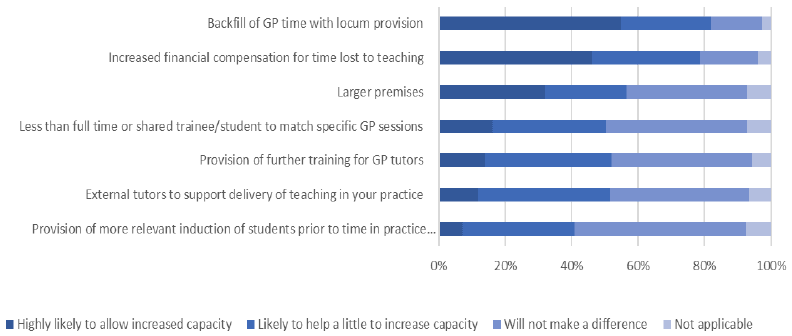
The proposal which was felt would have least impact was the provision of more relevant induction of students prior to time in practice. Only 41% of respondents felt that this would make a difference to capacity.
These views were common across all types of practice, although small practices (list size of less than 2,000 patients) were generally more likely to say that the proposals would make no difference to their capacity. Practices which had declared a GP vacancy were less positive about the suggestion of increased financial compensation than those which were at full complement and they had a stronger preference for the proposal to backfill GP time with locum provision.
A recent review (Barber et al 2019) of undergraduate educators from four medical schools in England found very similar barriers to general practice UG teaching. In addition, they cite lack of support from the medical school, patient fatigue and the development of different models of employment of GP (salaried/ sessional/ locum) as barriers.
Contact
Email: rachael.fairbairn@gov.scot