Undergraduate medical education: recommendations
A series of recommendations to increase undergraduate medical education in Scotland by enabling more general practice based teaching in primary care.
Chapter One: Context
Introduction
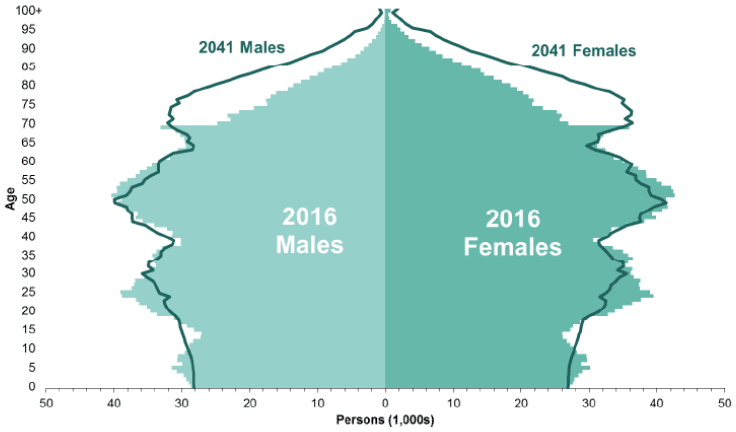
Across the UK and internationally, demand on our primary care services is steadily increasing due to a combination of an ageing population, rising levels of multi-morbidity and increasing patient expectations. According to National Records of Scotland (NRS, 2017) the number of people aged 65 and over is estimated to increase by around 45% from 1.00 million to 1.44 million by 2041, leading to substantial rises in those with long-term conditions and a rising demand on services. To be fit for purpose, the healthcare system must innovate and modernise, focus on developing preventative models of care to improve long-term outcomes. It must be financially sustainable and structured in such a way as to reduce pressure on the workforce while meeting the needs of the population of Scotland.
Figure 1: Estimated and projected age structure of Scotland's population, mid-2016 and mid-2041
To deliver this modernised health care system NHS Scotland has committed to the Chief Medical Officer's vision of "Realistic Medicine" (Scottish Government, 2016a); putting the person receiving health and care at the centre of decision-making and encouraging a personalised approach to their care. Its aims of reducing harm and waste, tackling unwarranted variation in care, managing clinical risk, and innovating to improve, are essential to a well-functioning and sustainable NHS. The CMO has stated that by 2025 all health care professionals will deliver care aligned to these principles. In order to realise this ambition, it is imperative that we examine how and where we educate our future health professionals.
The Health and Social Care Delivery Plan (Scottish Government, 2016b) sets out the ambition of shifting the balance of where care and support is delivered from hospital to community care settings, and to individual homes when appropriate. To help deliver this, The National Health and Social Care Workforce Plan: Part 3 - Improving workforce planning for primary care in Scotland focusses on developing, building and expanding Multidisciplinary Teams (MDTs), made up of professionals each contributing their unique skills to managing care and improving outcomes. This vision closely reflects the 21 underpinning principles on the future of primary care set out by Scotland's health professional groups in 2016 (QNIS,RCGP 2016).
The Plan sets out a series of ambitious commitments to significantly expand and strengthen the primary care workforce, backed by a historic increase in investment of £500m in primary care by 2021 (including £250 million in direct support of general practice). This includes an intention to deliver an additional 2,600 nurse and midwife training places by 2021-22, an investment in general practice and community nursing, increasing the number of health visitors by 500, and a commitment to recruit at least 800 (headcount) additional GPs over the next 10 years to address predicted increases in demand and ameliorate current vacancy and workload issues.
To help to increase the medical workforce (including the General Practice workforce) substantial investment in excess of £23 million has been made by Scottish Government. By 2021 undergraduate medical places will have been increased by 190 (22%) over 2016 levels. Additional places have been commissioned with a focus on encouraging graduates into shortage specialties and locations. Sixty new places commencing in 2019/20 will have a strong focus on general practice based education. In addition, 100 additional General Practice Specialty Training (GPST) posts were introduced in Scotland from 2016 to develop future capacity in the GP workforce.
The increase in the primary care workforce is being supported by refocused roles for clinical and non-clinical staff. Integrated community nursing teams will play a key role in planning, providing, managing, monitoring and reviewing care, building on current roles and best practice to meet the requirements of people with more complex health and care needs in a range of community settings. The new GMS Contract (Scottish Government/BMA, 2017) articulates a refocused role for GPs as Expert Medical Generalists (EMGs). This recognises the GP as the senior clinical decision maker in the community, who will focus on:
- undifferentiated presentations;
- complex care in the community;
- whole system quality improvement and clinical leadership.
Expert Medical Generalists will ensure strong connections to, and coordination with, the enhanced primary care team, health and social care community based services and with acute services where required. Better coordination of patient care, enabling access to the right professional at the right time, will deliver improved patient outcomes and a more proportionate use of resources.
Current context
Delivery of primary care
Under the current model of undergraduate medical education, approximately 90% of medical education is delivered in secondary care while an estimated 90% of patient contacts are delivered in primary care (Hobbs et al, 2016). Annually in Scotland we see over 4 million attendances in hospital outpatients and admit approximately 1.2 million people to hospitals (NHS NSS, 2018a). However, with an estimated 25 million appointments in general practice in Scotland annually (Scottish Government, 2016c) there is both necessity and opportunity to shift the balance of where future doctors learn and importantly what they learn. GPs in Scotland constitute 27% of the medical workforce.
Clinical decisions made in primary care impact, directly and indirectly, on activity and costs elsewhere in the healthcare system. This can include the number of unplanned admissions, rates of referral for new outpatient appointments, A&E attendances and prescribing costs. Primary care is therefore able to influence the level of demand for other care settings, acting as a 'navigator' to secondary care, developing anticipatory care plans, coordinating care, screening and health promotion. Primary care is particularly well placed to support self-management and shared decision-making by helping patients to fully understand and manage their problems, promoting a focus on prevention, rehabilitation and independence.
The dramatic demographic change in our population and shortening hospital stays are also both drivers for increasing undergraduate education in primary care. In addition, continuity of care is now recognised as making a significant contribution to reducing mortality (Pereira Gray et al., 2018). Continuity is important for high quality clinical care and also enables students to learn about the course of illness in patients. It may be easier to achieve through increased provision of general practice based primary care.
The work of the late Barbara Starfield over a period of more than twenty years showed that increasing the supply of primary care physicians (GPs) results in lower mortality from cancer, heart disease, and stroke as well as all-cause mortality; better self-reported health; reduced hospital admissions and decreased infant mortality. There is also an impact on health inequalities and a reduction in cost (see, for example, Caley, 2013).
Recently published evidence from the United States (Basu, et al., 2019) supports Starfield's findings. An increase in the supply of primary care physicians is associated with a decrease in population mortality, and conversely a decrease in GP supply is associated with an increase in mortality. Any reduction in GP numbers in Scotland relative to population is therefore a matter of serious concern. Don Berwick (Berwick, 2012), President of the Institute for Healthcare Improvement, and an important advocate for person-centred care, suggested this in his ten top tips for the NHS:
'Reinvest in general practice and primary care. These, not hospital care, are the soul of a proper, community-oriented, health-preserving care system. General practice, not the hospital, is the jewel in the crown of the NHS. It always has been. Save it. Build it.'
GP Workforce
The evidence tells us that high quality exposure to GP and primary care during the undergraduate years makes it more likely that students will choose a future career in general practice (see, for example, Health Education England/ Medical Schools Council 2016). There are also likely to be benefits for all medical students from increased exposure to general practice in gaining an understanding of whole system working, and the importance for patients of being able to move seamlessly from primary to secondary care and vice versa.
There is new evidence from the Scottish Medical Education Research Consortium (SMERC) that medical students from less traditional backgrounds are more likely to work in underserved areas and in primary care on qualification (NES, 2018). In a large recently published study using the UKMED database (Kumwenda et al, 2018) of 6,065 doctors entering specialty training after Foundation Year 2 posts, they found that the trainees coming from a family background where no parent was educated to a degree level and those entering medicine as mature students were significantly more likely to choose general practice or mental health. This has clear implications for UK medical school admissions policy.
Bringing together the considerable weight of the educational and the health services evidence, it is therefore vital that we collaboratively find ways of increasing the amount of high quality undergraduate teaching that takes places in primary care and by GPs during the undergraduate years. The Scottish Funding Council (SFC) has set out an aspiration in its outcomes agreement with Scottish universities, to work to increase the percentage of teaching that takes place in general practice to 25% of the clinical curriculum. All of this provides a useful impetus for all involved to work together to increase undergraduate education in primary care.
The desire to increase education in primary care needs to be seen in the context of a primary care system that is already under considerable pressure, with nearly a quarter (24%) of GP practices responding to the 2017 Primary Care Workforce Survey reporting GP vacancies, compared with 9% in 2013 (NHS NSS, 2018b). In addition, 6% of responding GP practices reported vacancies for registered nurses. Workload challenges are well documented. 37% of Scottish GPs feel overwhelmed on a weekly basis (RCGP Scotland 2019). Despite these pressures, patients remain highly positive of their experience of the health service, with 83% of people rating the overall care provided by their GP practice as good or excellent in 2017-18.
The current workload stresses are exerting considerable pressures on the ability of primary care to deliver undergraduate and postgraduate teaching. Scottish medical schools typically report increasing difficulty in recruiting practices and in delivering placements in primary care. For instance,
- Glasgow and Dundee medical schools seeing the number of practices involved in teaching fall by over a third in the last 6-7 years. There have also been falls in Aberdeen and St Andrews.
- Glasgow reports increased difficulty in recruiting GP tutors to teach vocational studies in years 1 and 2; with rate of ACT reimbursement being quoted as the most significant factor.
- Dundee sought to introduce 2 half-day sessions in general practice per student in each of years 1-3 but couldn't recruit sufficient placements, having to limit them to 1 session for each student in years 2 and 3.
These recruitment problems currently put further pressure on GP educators and staff to try to maintain currently levels of undergraduate teaching. Increasing clinical teaching in primary care, and by GPs in medical schools, therefore brings with it both significant opportunities but also a number of complex challenges for NES, medical schools, service planners and the NHS. If the ambitions set out in the primary care workforce plan and in the SFC outcomes agreement are to be met, a systematic approach to increasing undergraduate education in primary care needs to be prioritised and developed. Individual initiatives on their own will not be sufficient
Short Life Working Group
Under the joint auspices of the Scottish Government and the Board for Academic Medicine, an Increasing Undergraduate Education in Primary Care Working Group was established in 2018 to consider ways of increasing undergraduate education in primary care settings. The Group was chaired by Professor John Gillies with representation from all Scottish medical schools, the Royal College of General Practitioners Scotland (RCGP Scotland), Scottish General Practitioners' Committee (SGPC), National Education for Scotland (NES), the Scottish Deans' Medical Education Group (SDMEG), Scottish Funding Council, student representation and the Scottish Government (full remit and membership is provided in Annex A).
The aims of the Group were to:
- Determine the current level of undergraduate teaching in primary care in Scottish Medical Schools;
- Establish the number of GPs who currently teach, their capacity to increase teaching time and mechanisms to support them do so;
- Identify GPs who don't teach who would like to do so and mechanisms to support them do so;
- Understand the infrastructure, physical and digital, needed to support an increase in undergraduate teaching;
- Investigate factors that have a positive influence, including innovative practice within Scotland and elsewhere, and barriers to change;
- With support from NHS Education for Scotland, consider the role of funding in increasing clinical placements in primary care.
The group met approximately every 2 months between March 2018 and May 2019 to discuss and share key learning on the barriers and facilitators to increasing undergraduate teaching and discuss innovative teaching approaches being used across Scottish medical schools. Professor Gillies conducted a series of meetings with key stakeholders during the duration of the group including with the Scottish Deans' Medical Educators Group and the Scottish Academics GP Heads of Teaching Group. An intern supported the work of the group as part of the Scottish Graduate School of Social Science-Scottish Government for a three-month period from October 2018.
In addition, NHS Education has established the Educational Capacity Group, chaired by Professor Moya Kelly, to review current training capacity in primary care, identifying the training needs of learners from all disciplines delivering primary care. This group, with multi-disciplinary membership including representatives from Medicine, Pharmacy, Nursing, Allied Health Professionals and undergraduate medical schools, has postgraduate education as its initial focus. There are clear synergies across the groups with joint representation to ensure a joined up approach across undergraduate and postgraduate training with the awareness of need to develop capacity for both.
As set out in Chapter 3, a concurrent review of Additional Cost of Teaching (ACT) funding, provided by the Scottish Government to cover the cost of teaching medical undergraduate students, has been undertaken by NHS Education for Scotland (NES).
Contact
Email: rachael.fairbairn@gov.scot