Transforming Roles paper 9: allied health professions advanced practice
Guidance for developing Allied Health Professions (AHP) advanced practice roles in Scotland. Outlines policy context, role definition, education pathways, governance, and impact metrics to support consistent, sustainable workforce transformation across health and social care.
Direction for AHP advanced practice roles in Scotland
Delivery of AHP advanced practice roles in a sustainable way requires: integrated workforce planning and transformation, appropriate regulation, robust clinical governance arrangements, defined education and training pathways which are supported by clinical supervision, and the ability to measure and demonstrate impact in a range of areas including patient outcomes.
Integrated workforce planning and transformation
Effective workforce planning ensures we have the right people in the right place at the right time to deliver high quality care that meets Scotland’s population needs. All health boards are required to develop workforce plans and use workforce tools to inform decisions on service redesign and skill mix. The NHS in Scotland report[24] identified three workforce transformation priorities:
1. Recruitment and retention: Addressing workforce availability challenges
2. Data-driven planning: Improving use of data for workforce and service planning
3. Transform roles and services: Adapting roles and services to meet evolving health and care needs
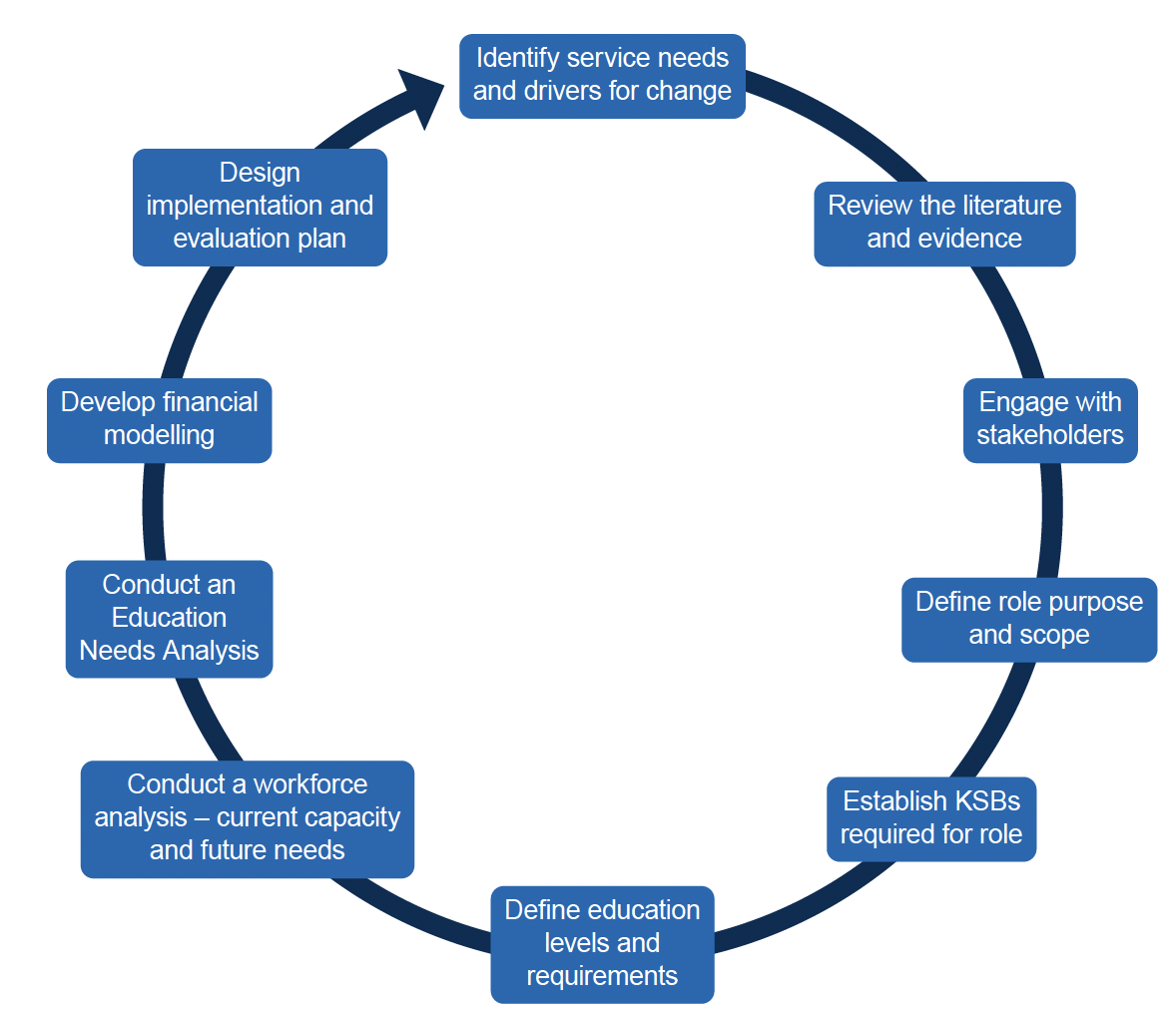
Advanced practice roles support recruitment and retention by providing clear, progressive career pathways and opportunities for professional development, which in turn increase job satisfaction[13]. The Transforming Roles methodology (Figure 2) is an example of a framework that can be used to develop and transform AHP roles, ensuring nationally consistent, sustainable and progressive roles, education and career pathways in Scotland.
- Develop financial modelling
- Conduct an Education Needs Analysis
- Conduct a workforce analysis – current capacity and future needs
- Design implementation and evaluation plan
- Identify service needs and drivers for change
- Define education levels and requirements
- Review the literature and evidence
- Establish KSBs required for role
- Define role purpose and scope
- Engage with stakeholders
Job planning
National job planning for individual AHP groups should be undertaken, with additional support provided to AHP leaders to enable this work to be undertaken[10]. In the context of AHP advanced practice, effective job planning supports transparency, accountability and governance by making explicit the roles and responsibilities undertaken. It also ensures practitioners have dedicated time to contribute meaningfully to the non-clinical pillars that are critical for service transformation. Workload measurement tools that allow workload and workforce calculations to be made should be developed alongside national job plans and agreed across relevant stakeholders. This should be supported by an appropriate digital system.
Regulation of AHP advanced practice
All AHPs are statutorily regulated by the HCPC. An independent review[25] commissioned by the HCPC to assess the need for additional regulatory measures for AHPs working at advanced practice level concluded that there was no clear evidence that additional regulation is currently needed or desired to protect the public. Based on this, HCPC agreed that the case for additional regulation of advanced practice for HCPC regulated professions had not been made. Advanced practice AHPs are required to meet the standards that are relevant to their scope of practice and to undertake CPD that reflects this[26]. The HCPC has developed resources to support advanced practice AHPs to optimise their scope of practice, effectively supervise and delegate work and meet regulatory standards[27].
Clinical governance arrangements
Robust clinical governance can be described as the process by which accountability for the quality of health and social care is monitored and assured[28]. It is essential to support the safe, effective employment and utilisation of AHPs in advanced practice roles. As shown in Figure 3, responsibility for clinical governance of AHP advanced practice roles is shared across three domains.

Clinical Governance Responsibilities
Employers
Ensure advanced practice AHPs meet the clinical standards to deliver safe and effective care in the workplace supported through training, development and supervision.
HCPC
Sets and monitors compliance with professional standards required for safe and effective practice.
Individuals
Advanced practice AHPs are professionally responsible and accountable for their practice, including recognising their scope of practice and evidencing their KSBs and demonstrating capabilities.
Employers have a duty to recognise the roles, responsibilities and capabilities of the advanced practice workforce and to establish governance arrangements that clearly define lines of professional and managerial accountability, extending up to the Director of AHPs or equivalent[22].
The Governance Maturity Matrix[29] provides a structured approach to help employers evaluate and strengthen their governance of advanced practice and should be used in conjunction with the seven standards of clinical governance[28](Annex 4). Additionally, the Minimum Standards of Governance[30] support the implementation of the matrix themes into practice.
Scope of practice
AHP advanced practice roles are diverse, and the scope of practice will vary depending on several factors. Scope (or capability) of practice describes the area in which a registered health and care professional has the knowledge, skills and experience to practise lawfully, safely and effectively, and within which they have freedom to make decisions and act[31].
As illustrated in Figure 4 (adapted from the Chartered Society of Physiotherapy[32]), scope of practice develops across a practitioner’s career, extending beyond the point of entry to the profession. This development is closely linked to education, training, reflection, supervision and professional frameworks.

It can be helpful to think about scope of practice as having two overlapping elements:
1. Professional scope
The knowledge, skills and activities that typically fall within the practice of a particular profession. This is informed by the contemporary evidence base and shaped by standards and guidance published by professional bodies, regulators and other recognised sources.
2. Individual scope
The knowledge, skills and activities that an individual AHP is competent to undertake.
While many aspects of advanced practice fall within the professional scope of an AHP, others may sit outside it but are within the individual’s scope, provided they have developed the necessary competencies. AHPs can extend their practice beyond the traditional boundaries of their profession to meet agreed service needs, provided they adhere to HCPC standards of proficiency and are aware of the limits of their capabilities. Additional guidance on scope of practice and professional indemnity for advanced practitioners is available[30], [33].
Education and training pathways
The CAHPO statement[22] notes that “Advanced practice education and training is undertaken by AHPs who have acquired post-registration experience. Some AHPs will enter the workforce through completing a pre-registration master’s level award. However, they will need to build their capability and experience whilst delivering professional care over time before undertaking further recognised post-registration education and training which addresses all four pillars at advanced level.” This highlights that a combination of post-registration experience and structured education and training is essential for preparing AHPs to manage complexity, uncertainty and risk effectively. NHS England’s Education and Training Standards[34] emphasise the need for high quality, sustainable academic and practice-based learning and assessment across all four pillars of practice to develop advanced practice capabilities.
Education and training pathways are built on KSB frameworks, which are tools that specify learning outcomes and/or competencies that define, classify and recognise educational, learner and sector expectations[35]. They align education with the needs of learners and the demands of the sector. Published frameworks also support education providers in mapping modules to KSBs, helping practitioners and managers identify relevant courses and opportunities aligned to specific roles or clinical areas.
Robust oversight is essential for the development of KSB frameworks to support AHP advanced practice roles[36]. The Transforming Roles Group has adopted a structured approach[37] to framework development. The approach is underpinned by the NES Nursing, Midwifery and Allied Health Professions (NMAHP) Development Framework[38], which provides the core content that can be supplemented with additional KSBs from profession and role-specific frameworks relevant to specific areas of practice. The approach outlines ten best practice steps for framework development[36] and includes a template to support consistent framework structure and terminology. This approach has been implemented to develop nursing frameworks, such as the Nursing in Cardiology Framework[39] and should now be applied in developing frameworks to support the consistent development of AHP advanced practice roles.
Education and training considerations:
Trainee roles
Trainee AHP advanced practice roles[40] are specific, time-limited positions that allow a registered AHP to develop the KSBs required to work at an advanced practice level. Postgraduate experience is a requirement for trainee roles, which typically combine workplace training with academic learning at master’s level, include multifaceted assessment and formal sign-off. Preceptorship should be used to provide structured support and supervision to guide trainees through this period of career transition. The NES AHP Preceptorship Hub[41] provides information and resources to support preceptorship programmes, aligned with the HCPC Principles for Preceptorship[42].
Professional portfolio
As part of the sign-off process and to provide on-going evidence of competence, advanced practice AHPs should maintain a professional portfolio to demonstrate how they meet the capabilities required for their role. Professional portfolios are tools for collecting, recording, and sharing evidence of academic learning, clinical training, and reflection, allowing both trainee and qualified advanced practice AHPs to demonstrate how they are delivering safe, effective and person-centred care. Use of the NES Professional Portfolio[43] is recommended and resources to support portfolio development and sign-off are included in Annex 3.
Demonstrating equivalence
Not all advanced practice AHPs will use the trainee route. The definition of AHP advanced practice in the CAHPO statement[22] uses “post-registration master’s level award or equivalent” to indicate that advanced practice education and training has developed over time. As a result, there will be AHPs in the existing workforce who have followed a variety of different education, training and development routes into advanced practice roles.
Educational equivalence refers to the process of ensuring that an individual’s knowledge, skills, and experience are comparable to those expected from formal academic qualifications at master’s level.
Individuals currently in role, but without a post-registration master’s level award, should focus on mapping their role to the definition contained within the CAHPO statement[22] , and an appropriate capability framework, using learning needs analysis. Local arrangements should be agreed to meet any learning and development needs, and a portfolio of evidence used to demonstrate attainment of capabilities. This approach is in line with the transitional approach under development by The Nursing and Midwifery Council to recognise and support those already working at advanced level, enabling them to demonstrate they meet the future standards of proficiency. It ensures recognition of prior learning and clinical experience, preventing disadvantage to those in existing roles. The use of the NES Professional Portfolio[43] is recommended to support this process. Boards should consider a robust sign-off process that involves portfolio review to ensure that advanced practice AHPs who meet the requirements of the role are recognised and recorded on the local electronic workforce system.
Supervision
Advanced practice AHPs require clinical and professional supervision throughout their careers to ensure professional and public safety. Scotland’s position statement on supervision for AHPs[44] outlines the core principles of supervision and its delivery, highlighting that effective supervision should be set up using established supervision models.
The initial focus of supervision for the advanced practice AHP is to establish the capabilities required for the role, utilising the key KSBs articulated in the NES NMAHP Development Framework[38] alongside additional profession and role-specific frameworks, to build an individual learning plan.
Supervision should include a clinical supervisor with sufficient experience of the role the trainee is preparing for, and an educational supervisor for the duration of any master’s level learning associated with an award of credit. Examples of good supervision are included in NHS England’s Standards for Workplace Supervision for Advanced Practice[45]. Protected time for supervision should continue to be scheduled regularly following qualification, with opportunity for the advanced practice AHP to update and discuss learning needs.
Continuing Professional Development
Protected learning time and resources for CPD are essential to promote the provision of evidence-based care and provide advanced practice AHPs with the opportunity to reflect on and develop their practice in line with HCPC requirements. A national circular[46] mandates protected learning time for all NHS staff and describes the conditions necessary to support this. Advanced practice AHPs have a duty to fulfil HCPC CPD requirements aligned with their advanced roles and scope of practice. CPD activities and reflections should be recorded within a professional portfolio, with learning needs identified and addressed through a robust appraisal process.
Measuring and demonstrating impact
Metrics are fundamental to the governance, development and sustainability of AHP advanced practice[3]. There are several underlying principles that should be applied when developing AHP advanced practice metrics:
Principle 1: Identify appropriate metrics when planning advanced practice roles, to articulate their impact on service delivery and ensure public value.
Principle 2: Use both qualitative and quantitative metrics, considering indicators of quality, safety, effectiveness and patient experience, and reflecting the four pillars of practice.
Principle 3: Align metrics with service and role priorities and utilise existing data sources where possible.
Principle 4: Timely analysis and feedback of metrics is required, with clear methods for displaying outcomes.
Annex 4 includes examples of metrics that could be used to demonstrate the role of advanced practice AHPs in delivering practical, scalable solutions to current service pressures and guide future workforce planning.
Additional considerations
Embedding environmental sustainability and equality, diversity and inclusion
In line with commitments to tackle the climate crisis[47], advanced practice AHPs have a pivotal role to play in delivering high quality, low carbon care. Their leadership roles enable them to redesign and transform services to ensure sustainable models of practice that address healthcare needs both now and in the future. Embedding sustainability principles into governance, education and workforce development is essential and advanced practice AHPs should role-model and advocate sustainable healthcare.
Equally, AHP advanced practice roles should be underpinned by a strong commitment to equality, diversity and inclusion. They have an individual and collective responsibility to challenge discrimination and ensure services are person-centred and inclusive[2].
Additionally, development opportunities for AHP advanced practice roles should provide equitable opportunities across professions, specialities and care settings[48].
Patient Public Involvement in the development of care pathways
Actively involving service users in the development of care pathways ensures services meet real needs and aligns with the principles of Realistic Medicine[6] . Embedding co-production, using a structured approach, will support the development of AHP advanced practice roles that are person-centred and effective.
Contact
Email: cno@scot.gov