The Scottish Health Survey 2011: Volume 1 - Adults
Annual report of the Scottish Health Survey for 2011. Volume focussing on adult health
CHAPTER 8 CARDIOVASCULAR DISEASE, DIABETES AND HYPERTENSION
Catherine Bromley and Jennifer Mindell
SUMMARY
- In 2011, 15.6% of men and 13.8% of women had cardiovascular disease (CVD).
- CVD or diabetes prevalence was also higher for men than for women (19.2% and 17.0%, respectively) in 2011 and increased markedly with age for both sexes from 6.3% of men and 7.0% of women under 25 to 57.0% of men and 43.4% of women aged 75 and over.
- Rates of ischaemic heart disease (IHD) for men and women were 7.5% and 4.9% respectively, while 9.4% of men and 6.7% of women had IHD or stroke. Prevalence of these conditions also increased with age for both men and women.
- Between 1995 and 2011 there was a significant increase in the proportion of men aged 16-64 with CVD or diabetes (from 9.4% to 12.7%). This was largely accounted for by an increase in the prevalence of diabetes. There was no clear trend in the figures for women over this same period.
- In 2011, 6.1% of men and 4.9% of women aged 16 and over had doctor diagnosed diabetes.
- 2.4% of adults (2.6% of men and 2.1% of women) had a glycated haemoglobin level consistent with undiagnosed diabetes (HbA1C>=6.5%) in the 2008-2011 period-an increase from 1.1% in 2003.
- In 2010/2011, a third of men (33%) and women (32%) aged 16 and over had hypertension.
- Hypertension rates increased significantly by age for men and women.
- In 2010/2011, almost one in five (18.5%) men and one in six (15.7%) women had untreated hypertension.
- Between 1995 and 2008-2011 mean total cholesterol in men aged 16-64 declined from 5.6 to 5.2 mmol/l. The equivalent figures for women were 5.6mmol/l and 5.3 mmol/l. Most of this decline occurred between 1995 and 1998. As these figures include people taking lipid lowering drugs such as statins it is likely that the decline is almost entirely due to the increased use of such drugs.
- There was no change in mean HDL cholesterol of adults between 2003 and 2008-2011. Levels were lower in men than in women (mean of 1.3 mmol/l compared with 1.6mmol/l).
- There was an increase in mean fibrinogen levels for 16-74 year olds between 1998 and 2008-2011 (from 2.6g/l to 2.9g/l in men, and from 2.8g/l to 3.1g/l in women). The figure for all adults from 2003 onwards has been more stable.
- There was no significant difference in the fibrinogen levels of men and women in 2008-2011, but levels did increase by age for both sexes.
- Women had higher mean C-reactive protein (CRP) levels than men (3.4 mg/l compared with 2.9mg/l) in 2008-2011 and levels for both sexes generally increased with age.
- The mean CRP for men aged 16-74 has not varied significantly since 1998, but there was an increase in the proportion of men in the bottom two CRP quintiles between 1998 and 2008-2011 (from 20.7% to 27.0%). For women the mean declined (from 3.8mg/l in 2003 to 3.3mg/l in 2008-2011) but there were no notable changes in the proportions in each quintile group over this period.
8.1 INTRODUCTION
This chapter covers three related topics: cardiovascular disease (CVD), diabetes and hypertension. In addition, it presents results for a number of blood analytes measured in the Scottish Health Survey (SHeS) that can be used to assess diabetes status and CVD risk. As in the three most recent SHeS reports, the combined prevalence of CVD and diabetes is also reported, reflecting the status of these two conditions as major health burdens for individuals and the NHS.1,2,3 Additionally, people with diabetes are at particularly high risk for CVD, hence the inclusion of estimates of the burden of probable undiagnosed diabetes in the population.
CVD is one of the leading contributors to the global disease burden. Its main components are ischaemic heart disease (IHD) and stroke. In this chapter, the term IHD is used interchangeably with CHD (coronary heart disease). IHD is the second most common cause of death in Scotland after cancer; in 2011, 14% of deaths were attributed to it and a further 9% were caused by stroke.4 Prevalence of CVD is higher in lower social classes and in deprived areas.5 A number of the Scottish Government's National Performance Framework (NPF) national indicators6 are linked to key CVD risk factors (such as the smoking,7 physical activity8 and obesity9 indicators described in chapters 4, 6 and 7 respectively). In addition, the revised NPF, published in December 2011,10 now includes a target to reduce premature mortality (deaths from all causes in those aged under 75).11 CVD is described as one of the key 'big killer' diseases around which action must be taken if the target is to be met.
NHS Scotland's HEAT12 performance management system is based around a series of targets against which the performance of its individual Health Boards are measured. In 2007, the Scottish Government published Better Health, Better Care,13 outlining its action plan for improving health and health care in Scotland. This set out how NHS Scotland's HEAT9 system would feed into the Government's overarching objectives. As reported in last year's SHeS report,3 a HEAT target to achieve 23,579 inequalities-targeted cardiovascular Health Checks during 2010/11 was far exceeded via the delivery of 41,107 checks.14 The target for 2011/12 was for 26,682 checks to be carried out. This too was exceeded with 47,776 checks carried out in the year ending March 2012.
There are also HEAT targets addressing primary care of people with acute and chronic conditions. For example, the quality of acute care in the immediate aftermath of a stroke is an important factor in people's recovery rate and subsequent quality of life. A HEAT target exists to improve performance in this area: by March 2013, 90% of patients admitted with a stroke should be admitted to a specialist stroke unit within one day of admission.15 In 2011, 78% of stroke patients were admitted to a specialist stroke unit within one day of their admission, up from 67% in 2010 and 61% in 2009.
The introductions to the equivalent chapters in the 2008, 2009 and 2010 SHeS reports1,2,3 outlined the recent policy context for this topic in more detail, covering a number of strategies and initiatives that have been introduced by the Scottish Government and NHS Scotland to help reduce the prevalence of these conditions and improve their management in primary care. These included:
- The Scottish Government's Better Heart Disease and Stroke Care Action Plan,16 launched in June 2009, which built on the Coronary Heart Disease and Stroke Strategy for Scotland published in 2002, and updated in 2004.17
- The Quality and Outcomes Framework18 and initiatives such as the Keep Well programme.19
- The SIGN Guidelines on cardiovascular health20 published in 2007, which include a risk assessment tool (ASSIGN) to calculate a person's future risk of cardiovascular disease.
- The revised SIGN guidelines on diabetes21 published in March 2010.
- The revised Diabetes Action Plan, published in August 2010.22
- The roll-out of the "Life begins at 40" programme which invites all those turning 40 to participate in a health assessment delivered by NHS 24 via telephone or online.23
This chapter takes advantage of the nurse data collected throughout the 2008-2011 period and reports on the direct measures of blood pressure and a number of blood analytes that act as useful biomarkers of diabetes status and CVD risk. As only a sub-sample of participants were invited to have a nurse interview between 2008 and 2011, results based on the nurse data use either two or four years of nurse data combined.
This is the first time since the 2003 SHeS report that many of these blood analytes have been reported in detail.26 From 2012 the survey is no longer including a nurse visit and instead a sub-sample of adults will be asked to complete a new biomeasures module, conducted by specially trained interviewers. The use of dried blood spot samples, collected via finger-pricks, is currently under investigation (as opposed to the venous blood samples collected until the end of 2011). As yet, no decision has been taken about their use, and it is also conceivable that venous samples could be collected again in future, should funding become available. In contrast, interviewers began taking blood pressure readings in 2012, using the same equipment and measurement protocols that the nurses used. A validation study has been conducted to assess the impact on the time series data of the change in personnel for measuring blood pressure.24 Future SHeS reports will discuss the implications in full.
8.2 METHODS AND DEFINITIONS
8.2.1 Methods
CVD conditions
Participants were asked whether they suffered from any of the following conditions: angina, heart attack, stroke, heart murmur, irregular heart rhythm, 'other heart trouble', and (if they responded affirmatively) whether they had ever been told they had the condition by a doctor. For the purpose of this report, participants were classified as having a particular condition only if they reported that the diagnosis was confirmed by a doctor. Those participants who reported having a particular condition were also asked if they had had it in the last 12 months.
Diabetes
Participants were asked whether they suffered from diabetes and, if so, whether they had ever been told they had the condition by a doctor. Only those who reported that the diagnosis was confirmed by a doctor were classified as having diabetes. Women whose diabetes occurred only during pregnancy were excluded from the classification. No distinction was made between type 1 and type 2 diabetes in the interview. In some previous SHeS reports, rates for each type were estimated by examining the age of onset of the condition and whether a participant was on insulin therapy at the time of interview.25 However, with increasing rates of type 2 diabetes in younger age groups, and increasing use of insulin to treat it, this classification method is no longer considered appropriate.
Hypertension
There have been significant changes to both the definition and measurement of blood pressure since the survey began in 1995. These were discussed in detail in the 2003 survey report and are not repeated here.26
The 2008 to 2011 surveys used the same measurement equipment (the Omron HEM 907) as in 2003. The protocol for the measurement of blood pressure in adults remained the same as in all previous years; blood pressure was measured in participants aged 16 and over who took part in the nurse interview. Three blood pressure readings were taken at one minute intervals, on the right arm where possible, with the participant in a seated position, after a five minute rest. Blood pressure of pregnant women was not measured. The detailed protocol for blood pressure measurement is contained in Volume 3 of this report.
The blood pressure levels reported in this chapter are derived from the means of the second and third measurements obtained and are restricted to those participants who had not eaten, drunk alcohol, smoked or exercised in the 30 minutes before the measurement and for whom three readings were successfully obtained.
Blood samples
The table below shows the numbers of men and women from whom a non-fasting blood sample was obtained in each of the 2008 to 2011 surveys. Pregnant women, anyone with a history of fitting or convulsions, and those taking anti-coagulant medicines (such as warfarin) were excluded from giving a blood sample. Further exclusions (due to problems in the laboratory or the use of prescription medication that interferes with the analyte) further reduce the sample sizes available for analysis.
Blood samples obtained, 2008-2011
| 2008 | 2009 | 2010 | 2011 | |
|---|---|---|---|---|
| Men | 415 | 387 | 372 | 333 |
| Women | 488 | 498 | 471 | 392 |
| All aged 16+ | 903 | 885 | 843 | 725 |
Full details of the response to the blood samples in 2008 and 2009 were published in the 2009 technical report,27 and in the respective technical reports for the 201028 and 2011 surveys (Volume 3 of this report).
Although blood samples have been collected since the survey began in 1995, changes over the years to the laboratory, the analysis methods used, or the analytes tested for, mean that trends do not necessarily start in 1995.
8.2.2 Summary measures of cardiovascular disease and diabetes
Any CVD condition / Any CVD condition or diabetes
Participants were classified as having any CVD condition if they reported ever having any of the following conditions confirmed by a doctor: angina, heart attack, stroke, heart murmur, abnormal heart rhythm, or 'other heart trouble'.29 A second category that includes diabetes as well as the above CVD conditions is also presented in the tables as 'any CVD condition or diabetes' so that the total combined prevalence of these conditions can be seen. The trend table reports the prevalence of any CVD, and any CVD or diabetes from 1995 onwards.
Ischaemic heart disease
Participants were classified as having IHD if they reported ever having angina or a heart attack, confirmed by a doctor.
Ischaemic heart disease or stoke
Participants were classified as having IHD or stroke if they reported ever having angina, or a heart attack, or a stroke, confirmed by a doctor.
8.2.3 Classification of blood pressure levels
Blood pressure has a normal distribution within a population and thresholds to indicate the point at which someone has a level that is definitely clinically significant do not exist. The most recent NICE guidelines (developed jointly with the British Hypertension Society) cite evidence suggesting that with each 2mmHg increase in systolic blood pressure, risk of mortality from IHD increases by 7% and by 10% for stroke.30 Those guidelines recommend that antihypertensive therapy should be initiated in people with sustained clinic levels of systolic blood pressure (SBP) >160 mmHg or diastolic blood pressure (DBP) >100 mmHg. They also recommend that treatment should be initiated for people aged below 80 (who have CVD, diabetes, other target organ damage (e.g. kidney), or an estimated CVD risk ≥ 20% over 10 years) and who have sustained clinic levels of SBP between 140 and 159 mmHg and/or DBP between 90 and 99 mmHg. The guidance also advocates the use of ambulatory blood pressure monitoring, or home blood pressure monitoring before making the diagnosis. The most recent guidance from SIGN concurs with the guidance for treating those with existing or high risk of CVD,31 while separate SIGN guidance recommends the use of antihypertensive medication for people with a previous stroke or transient ischaemic attack (TIA, like a stroke but lasting less than 24 hours) regardless of BP level.32
These guidelines are not universally accepted.33 For example, the United States uses guidelines that are more restrictive so that 140/90 mmHg (irrespective of risk factor) is considered the threshold for treatment and target to achieve.34 In 2003 the European Society of Hypertension and the European Society of Cardiology jointly recommended a threshold of 140/90 mmHg for those without diabetes and 130/80 mmHg for those with diabetes.35
This report continues to use the blood pressure definition that was introduced in the 1998 SHeS (140/90 mmHg), in accordance with the 1999 British Hypertension Society guidelines.36
Based on their systolic (SBP) and diastolic (DBP) blood pressure and current use of anti-hypertensive medications, adult participants were classified into one of four groups as follows:
Normotensive |
SBP<140 mmHg and DBP<90 mmHg, not currently taking any drug specifically prescribed to treat high blood pressure |
Hypertensive controlled |
SBP<140 mmHg and DBP<90 mmHg, currently taking a drug specifically prescribed to treat high blood pressure |
Hypertensive uncontrolled |
SBP≥140 mmHg or DBP≥90 mmHg, currently taking a drug specifically prescribed to treat high blood pressure |
Hypertensive untreated |
SBP≥140 mmHg or DBP≥90 mmHg, not currently taking a drug specifically prescribed to treat high blood pressure |
For the purpose of this report, the term 'hypertensive' is applied to those in the last three categories.
Glycated haemoglobin
Glycated haemoglobin (HbA1C) reflects the level of glucose in the blood over the preceding two to three months, and is therefore a better indicator of diabetic control than a random glucose sample, which is affected by recent food or drink intake. Elevated glycated haemoglobin in people without diabetes is associated with increased mortality following acute myocardial infarction.37 Elevated levels are seen in people with undiagnosed diabetes. In June 2009, an international expert committee recommended using levels of 6.5% or more to diagnose diabetes.38 Levels of 5.7% or more have been proposed as a screening test for diabetes.39 The UK National Screening Committee is due to review its policy on diabetes screening in 2012/13.
The latest SIGN guidelines for diabetes set <7% as the HbA1C target for good glycaemic control in people with diabetes,21 consistent with indicator DM 23 within the Quality and Outcomes Framework (QOF) for 2009/2010. DM 23, which replaces DM 20, gives GPs the target of 40-50% of their diabetic patients having HbA1C <7%, a reduction from <7.5% within DM 20.40,41 The Task Force on Diabetes and Cardiovascular Diseases of the European Society of Cardiology (ESC) and of the European Association for the Study of Diabetes (EASD) recommends that HbA1C be kept <6.5% to reduce cardiovascular risk.42 For the purpose of this survey, a glycated haemoglobin value of 6.5% or above in people with no existing diabetes diagnosis was taken to indicate possible undiagnosed diabetes. The sample size for people with a diabetes diagnosis was too small to assess whether their condition is being adequately controlled so the chapter only looks at people with no such diagnosis.
HbA1C figures for participants with no self-reported diagnosis of diabetes are presented for 2003 and 2008-2011 combined.
Total cholesterol
Prospective studies have identified an increased risk of coronary disease associated with raised cholesterol concentration. A meta-analysis of all randomised trials of more than two years duration showed that lowering serum cholesterol confers clinical benefit as expressed in lower CHD mortality and total mortality risk, with the magnitude of benefit directly related to the degree of cholesterol reduction.43 Lipid-lowering drugs (statins) are effective in primary prevention44 as well as in people with established disease, and also reduce the risk of stroke.45
For the purpose of this survey, cholesterol was considered to be raised at a level of 5.0 mmol/l or over. In 2000, the National Service Framework for Coronary Heart Disease suggested a total cholesterol target below 5.0 mmol/l for all patients with arterial heart disease or significant cardiovascular risk.46 The QOF target for GPs relates to the percentage of patients with coronary heart disease whose total cholesterol is 5.0 mmol/l or below.47 In 2005, the recommendations for defining and treating hypercholesterolaemia were superseded by the second guidance from the Joint British Societies, JBS2.48 European guidance is based on assessing cardiovascular risk, using the SCORE tool,49 while in Scotland the ASSIGN risk assessment tool has been developed to take better account of the risks associated with social deprivation and family history of CVD.31 SIGN guidance advises the use of statins in people with pre-existing cardiovascular disease, diabetes, or estimated 10-year CVD risk of 20% or above, regardless of cholesterol level, or in those with total cholesterol of 8.0mmol/l or above.20,31,32 The Scottish Government's 2009 Better Heart Disease and Stroke Care Action Plan also covers Familial Hypercholesterolaemia, a genetic condition in which affected people have very high cholesterol levels and high risk of premature cardiovascular disease.16
Total cholesterol figures, which include participants who were taking lipid-lowering drugs, are presented for 1995, 1998, 2003, and 2008-2011 combined.50
High-density lipoprotein cholesterol
Studies have shown that high-density lipoprotein cholesterol (HDL-cholesterol) is inversely and independently associated with the risk of developing CHD.51,52 Furthermore, low levels of HDL-cholesterol are associated with a worse prognosis after myocardial infarction.53 Protection against CVD by HDL-cholesterol is conferred in at least two ways. The first is that it transports cholesterol back from organs such as arteries to the liver for elimination, thus protecting the arteries from further atheromatous plaque formation. The second is by acting as an antioxidant. Increasing physical activity, drinking alcohol,54 quitting cigarette smoking and losing weight can elevate HDL-cholesterol. Attention is generally recommended for HDL-cholesterol concentrations <1 mmol/l. HDL-cholesterol levels are generally higher in women than men.
Total: HDL cholesterol ratio
Total cholesterol has been criticised as a measure because it can be raised when the (beneficial) HDL fraction is high. LDL- (low density lipoprotein) cholesterol, the component that is directly associated with increased atherosclerosis (hardening of the arteries), is harder to measure and is generally considered to require fasting blood samples. Although LDL-cholesterol levels can be estimated by calculating 'non-HDL-cholesterol', and numerous other lipid-related measures have been suggested, the measure found to be most highly associated with CVD outcomes is the ratio of total to HDL-cholesterol,55 which is better than either total or HDL-cholesterol alone for predicting IHD.56
Canadian guidelines recommend treatment with statins for low risk individuals with a total: HDL cholesterol ratio above 6.0, and for individuals at moderate CVD risk (10 year CVD risk of 10-19%) with a ratio above 5.0.57 An American study found that secondary prevention targets in high risk individuals can be monitored using this ratio, aiming at levels below 3.0.58 However, no country within the UK routinely uses total: HDL-cholesterol ratio in its lipid-lowering guidance.
HDL-cholesterol and total: HDL cholesterol ratio figures and are presented for 2003 and for 2008-2011 combined. The figures presented include participants who were taking lipid-lowering drugs.
C-reactive protein
C-reactive protein (CRP) is an acute-phase reactant which is synthesised in the liver in response to the pro-inflammatory protein interleukin 6 (IL-6). It is therefore a sensitive marker of inflammation. Levels of these acute phase proteins have been related to risk of coronary heart disease (CHD). Elevated levels of CRP are associated with increased risk of myocardial infarction (MI) or sudden death among those with stable and unstable angina pectoris,59 as well as with coronary heart disease in the elderly and coronary mortality among high-risk patients. The follow-up of the Multiple Risk Factor Intervention Trial (MRFIT) has documented a strong relationship between levels of CRP and subsequent risk of CHD deaths among cigarette smokers.60
However, it is more likely that these associations are due to confounding, with CRP unlikely to be causally related to CHD.61,62 Although an American study raised the possibility that assessment of CRP may also provide a method of determining risk of future MI among apparently low-risk individuals, including non-smokers,63 a review in 31 studies found that CRP was generally no more effective than the classical Framingham score in predicting CHD.64 In the US, the first set of guidelines endorsing use of high-specificity CRP (hsCRP) in risk factor screening for CVD were produced in 2003,65 but CRP is not currently included in screening in the UK,48 nor is there a recommended CRP threshold in the UK.
CRP figures are presented for 1998, 2003 and 2008-2011 combined.
Fibrinogen
Fibrinogen is a major blood glycoprotein that plays an essential role in haemostasis (coagulation) and the maintenance of blood viscosity. High fibrinogen is a cardiovascular risk factor, being important in the cascade leading to thrombotic events. Epidemiological observations indicate that high plasma fibrinogen levels are strongly correlated with the incidence of two major thrombotic complications of atherosclerosis: stroke and myocardial infarction. The Scottish Heart Health Study confirmed that plasma fibrinogen is not only a risk factor for coronary heart disease and stroke, but is also raised with family history of premature heart disease and with personal history of hypertension, diabetes, and presence of intermittent claudication.66 Fibrinogen levels are higher in more deprived groups (even among non-smokers)67 and in smokers,68 and levels fall after quitting smoking.68 This may explain part of the excess CVD risk among smokers and those in lower socio-economic groups. However, fibrinogen is not used clinically for individual patients in determining cardiovascular risk.
Fibrinogen figures are presented for 1998, 2003 and 2008-2011 combined. As per the convention in all previous SHeS reports, and in contrast to the cholesterol measures, the fibrinogen figures exclude participants who were taking prescription medications that would affect fibrinogen levels (lipid lowering drugs and beta blockers).
8.3 PREVALENCE OF CARDIOVASCULAR CONDITIONS AND DIABETES
This section examines trends in the prevalence of: any CVD, any CVD or diabetes, IHD, stroke, and IHD or stroke from 1995 onwards. Changes to the sample composition over the first three years of the survey mean that discussion of the trend between 1995 and 2011 is based on those aged 16-64, while the trend for all adults aged 16 and over from 2003 onwards is also included.
8.3.1 Any CVD, and CVD or diabetes, IHD, stroke and IHD and stroke by age and sex, 2011
Figures for the prevalence of any CVD, any CVD or diabetes, IHD, stroke, IHD and stroke in 2011 are presented in Table 8.1 and summarised below. Rates were higher for men than women with particularly pronounced differences for IHD and IHD or stroke rates. The proportion of adults with these conditions increased markedly with age. For example, fewer than one in ten men or women under 45 had any CVD conditions or diabetes, whereas 57.0% of men and 43.4% of women aged 75 and over had at least one of these conditions. Table 8.1
| Stroke | IHD | IHD or stroke | Any CVD | Any CVD or diabetes | |
|---|---|---|---|---|---|
| Men (%) | 2.9 | 7.5 | 9.4 | 15.6 | 19.2 |
| Women (%) | 2.7 | 4.9 | 6.7 | 13.8 | 17.0 |
8.3.2 Trends in any CVD, and CVD or diabetes since 1995
The prevalence of any CVD in men aged 16-64 was 8.4% in 1995, 8.1% in 1998 and then increased significantly to 9.7% in 2003. The figure in 2011, 9.8%, was similar to that reported in the three previous survey years (9.5% to 10.5%) which suggests that prevalence has been fairly static since 2003. Prevalence of any CVD in women aged 16-64 has shown small fluctuations over time but with no obvious pattern; the 2011 figure (8.4%) was very similar to that in 1998 (8.5%).
Until 2010, the prevalence of CVD or diabetes among men aged 16-64 increased by a small amount each year (from 9.4% in 1995 to 13.6% in 2010). The 2011 and 2009 figures were identical (12.7%). As noted in previous reports, the overall upward trend in any CVD or diabetes is largely accounted for by increasing levels of diabetes over time (rather than increased rates of CVD conditions). However, it is not possible to establish whether this trend represents an overall increase in the incidence of CVD and/or diabetes among men and/or improved diagnostic or survival rates for these conditions.
In contrast, the level of any CVD or diabetes among women has not followed such a consistent pattern. The rate fluctuated between 9.6% and 10.2% in the three earliest surveys, peaked in 2008 (12.8%), and has sat at around 11% since then (11.2%-10.8%). Table 8.1
8.3.3 Trends in IHD, stroke, and IHD or stroke since 1995
The proportion of men aged 16-64 with IHD has been similar across the survey years (ranging between 3.2% and 4.1%) with no significant trend. However, there has been a decrease in IHD prevalence among particular age groups of men: there was a seven percentage point drop in IHD among those aged 55-64 between 1995 and 2011, and a four point decline for those aged 65-74 between 1998 and 2011. This may well contribute to declining rates of IHD in the future (assuming that IHD onset has been avoided rather than just delayed for these cohorts of men).
The prevalence of stroke among men has also been fairly static: it ranged from 0.7% and 1.2% between 1995 and 2009, was somewhat higher in 2010 (1.8%), but was lower again in 2011 at 1.3%. The combined prevalence of IHD or stroke in men has remained relatively unchanged across the survey years (4.2%-5.0%).
For women aged 16-64, there was a slight decrease in IHD prevalence between 1995 (2.9%) and 2008 (2.2%), with little change since then (1.9% in 2009, 2.2% in 2010 and 1.8% in 2011). As was for the case for men, those aged 55-64 and 65-74 saw larger decreases in IHD prevalence than any other age group. The most recent figures for stroke prevalence for women (0.9%-1.2%) have all been a little higher than in the 1995-2003 period (0.5%-0.7%). With the exception of the 2009 and 2011 figures (2.4% and 2.6%, respectively), the rates of IHD or stroke in women have remained fairly constant over time at 3.0%-3.2%. Table 8.1
8.4 DOCTOR-DIAGNOSED AND UNDIAGNOSED DIABETES
8.4.1 Trends in doctor-diagnosed diabetes since 1995
There has been an increase over time in doctor-diagnosed diabetes among adults aged 16-64 (Table 8.2). Prevalence doubled between 1995 and 2008, from 1.5% to 3.1%, and was a little higher in the three most recent survey years (3.6%-3.8%). The increase between 1995 and 2008 was slightly steeper for men (from 1.5% to 3.3%) than for women (from 1.5% to 2.8%), and while prevalence increased further in men from 2009 onwards (4.0%-4.7%), for women it remained fairly stable (2.8%-3.2%).
The figures for all those aged 16 and over are available from 2003 onwards and the trend shows a similar pattern to that for adults aged 16-64, with prevalence between 2003 and the three most recent survey years increasing from 3.8% to 6.1-6.3% for men, and from 3.7% to 4.4%-4.9% for women. Table 8.2
8.4.2 Trends in undiagnosed diabetes since 2003
As described in Section 8.2.4, levels of glycated haemoglobin (measured in the blood samples collected in the nurse interview) can be used to estimate the prevalence of undiagnosed diabetes in the population. Levels of glycated haemoglobin are reported in three groups in Table 8.3: 6.5% or above (a level consistent with undiagnosed diabetes), 6.0-<6.5% (a level that could indicate a high risk of developing diabetes), and <6.0% (low risk). Participants who reported that they had doctor-diagnosed diabetes have been excluded from the table. As only a sub-sample of participants was eligible for the nurse interview each year in the 2008-2011 period, the data for these years have been combined to provide more robust estimates.
Between 2003 and 2008-2011, the proportion of adults with undiagnosed diabetes increased from 1.1% to 2.4% (1.2% to 2.6% for men, 1.0% to 2.1% for women). Table 8.3
In the table below the self-reported doctor-diagnosed diabetes figures collected in the survey are combined with the glycated haemoglobin results (presented in Table 8.3), to estimate prevalence of the total 'true' level of diabetes (both diagnosed and undiagnosed) in the population. Note that the diagnosed diabetes figures here are based on the 2008-2011 combined data, so differ slightly to those presented in Table 8.2. The table below also provides an estimate of the proportion of all diabetes that is undiagnosed. Based on these figures, just under a third (32%) of all cases of diabetes in adults are undiagnosed.
Prevalence of diagnosed and undiagnosed diabetes, 2008-2011 combined
| Men | Women | All adults | |
|---|---|---|---|
| % | % | % | |
| Doctor-diagnosed diabetesa | 6.0 | 4.5 | 5.2 |
| Glycated haemoglobin ≥6.5% but no diagnosed diabetes (i.e. undiagnosed diabetes)b | 2.6 | 2.1 | 2.4 |
| All diabetes | 8.6 | 6.6 | 7.6 |
| Undiagnosed diabetes as a percentage of all diabetes | 30% | 32% | 32% |
a Among those interviewed
b Among those providing a blood sample in the nurse interview
There has been a much more notable increase in the prevalence of glycated haemoglobin levels of 6.0-<6.5% in adults without diagnosed diabetes, from 2.7% to 11.8% between 2003 and 2008-2011. The scale of the increase was similar for men and women. The Health Survey for England has also been measuring glycated haemoglobin over time, using the same blood collection technique and analysis laboratory as SHeS. In 2003, 3.4% of adults in England without diabetes had a glycated haemoglobin level of 6.0-<6.5%, by 2009 (the most recent comparable year for which data are available) it had increased to 10.9% (data not shown). Like Scotland, England also experienced a small increase in the prevalence of glycated haemoglobin levels of 6.5% or above, from 1.4% in 2003 to 2.5% in 2009 (data not shown).69
It is important to note that, as is always the nature with risk estimates, only some people in the group classified as being at high risk of developing diabetes will actually progress to the point of meeting the diagnostic threshold for the condition, while some people with levels currently below 6.0% will develop it, so these figures are simply an estimate of the possible future burden of diabetes. Studies have shown a very small increase in diabetic retinopathy with increasing glycated haemoglobin until a threshold at 6.5%, after which it climbs steeply; this has therefore been taken as the best threshold for diagnosing diabetes.70 Although there is no specific level at which risk of developing diabetes clearly begins, the International Expert Committee report on the use of glycated haemoglobin to diagnose diabetes suggested that those with glycated haemoglobin levels of 6.0% to <6.5% are at higher risk and should receive effective lifestyle interventions. For example, they recommend that those at risk of developing diabetes should be advised as a minimum to control their weight and be more physically active; and suggest such individuals may also benefit from formal assessment of other cardiovascular risk factors, such as blood pressure.70 Table 8.3
8.5 HYPERTENSION
8.5.1 Trends in blood pressure levels since 1998
The four levels used to classify hypertension (presented in Table 8.4) draw a distinction between people with normal blood pressure who are not receiving any treatment for hypertension, and those with normal levels who are taking anti-hypertensive medication. They also distinguish between people with raised blood pressure who are receiving treatment, and those who are not. These latter two categories are important target groups in the population. The first (those with raised blood pressure who are receiving treatment) includes people with poorly managed hypertension, while the second provides an estimate of the prevalence of potentially undiagnosed cases of this condition. It should be noted, when considering this last category, that not everyone with a one-off raised blood pressure measurement actually has hypertension on repeated measurement; the definition of hypertension is 'sustained raised BP'. Nor does everyone with a blood pressure of 140-159/90-99mmHg warrant treatment, which is indicated for people aged under 80 with existing CVD, diabetes, damage from raised blood pressure (e.g. kidney disease) or at high risk of developing CVD.
Blood pressure levels from 1998 onwards are presented in Table 8.4. The blood pressure categories use information about prescribed medications. As questions about medications were first included in SHeS in 1998, the trends in blood pressure levels exclude 1995. Since adults aged 75 and over were not included in the 1998 survey, the discussion on the trend since 1998 is based on those aged 16-74. The figures for all adults aged 16 and over from 2003 onwards are also included in the table.
Prevalence of hypertension has changed over time, though it is worth noting, as previous reports have, that the change in the measurement equipment used between 1998 and 2003 might have contributed to some of this change.26 Between 1998 and 2003 the proportion of men aged 16-74 with hypertension increased from 22.3% to 29.5%; the 2008/2009 and 2010/2011 figures were similarly high (31.9% and 29.9%, respectively). The increase occurred across each of the three separate hypertensive categories. Table 8.4
A similar, but less pronounced, increase was observed among women; a significant increase between 1998 and 2003 with prevalence in more recent years remaining at this higher level. In 1998, 21.2% of women aged 16-74 had hypertension compared with 26.7% in 2003, 26.5% in 2008/2009 and 26.6% in 2010/2011. As seen with men, prevalence increased in each of the hypertensive categories.
The pattern for adults aged 16 and over, from 2003 onwards, was very similar to that described for the 16-74 year old population. In 2010/2011, the total proportions of men and women aged 16 and over with hypertension (33.0% and 32.0%, respectively) were similar to the 2008/2009 and 2003 figures.
8.5.2 Blood pressure levels by age and sex, 2010/2011 combined
In 2010/2011 the prevalence of hypertension (blood pressure of ≥140/90 mmHg and/or taking anti-hypertensive medication) was not significantly different in men (33.0%) and women (32.0%) and the proportions of men and women in each of the three hypertensive categories were very similar. As Figure 8A shows, increasing age is a major risk factor for hypertension, though patterns differ between men and women. In 2010/2011, prevalence of hypertension among men doubled between the ages of 16-24 and 45-54 (from 13.6% to 29.1%), and again between the ages of 45-54 and 65-74 (to 61.0%), and was highest (69.4%) among those aged 75 and over. Women had lower hypertension rates than men up until the age of 55-64, after which point rates were higher than for men. Rates fluctuated among younger women before showing a steady increase. Prevalence rose from 13.2% of those aged 35-44, to 26.3% and 50.8% in the next two age groups, and reached a peak of 77.2% among women aged 75 and over. Figure 8A, Table 8.4
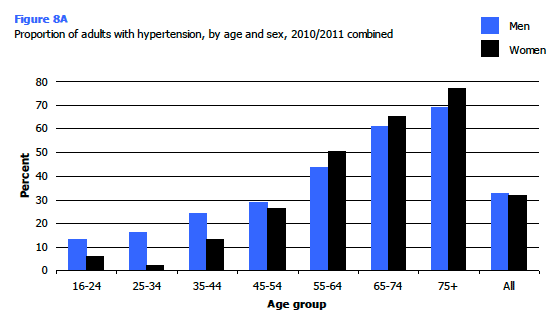
Almost one in five men and one in six women had untreated hypertension in 2010/2011: for both sexes this was the most common category of hypertension among those aged 16-74 (controlled hypertension was more common for men aged 75 and over, while uncontrolled hypertension was more common for women of this age). As the inset table below shows, untreated hypertension accounted for around half (52%) of all hypertension detected in the survey. Its contribution to total hypertension prevalence decreased with age, as prevalence of both uncontrolled and controlled hypertension increased. Table 8.4
Prevalence of treated and untreated hypertension, 2010/2011 combined
| Men | Women | All adults | |
|---|---|---|---|
| % | % | % | |
| Untreated hypertensiona | 18.5 | 15.7 | 17.0 |
| Treated hypertension (controlled and uncontrolled)b | 14.5 | 16.4 | 15.5 |
| All hypertension | 33.0 | 32.0 | 32.5 |
| Untreated hypertension as a percentage of all hypertension | 56% | 49% | 52% |
a Not taking drugs prescribed to treat high blood pressure and with SBP of ≥140 mmHg or DBP ≥90 mmHg.
b Taking drugs prescribed to treat high blood pressure with any BP level.
8.6 BLOOD ANALYTES
8.6.1 Total cholesterol
Between 1995 and 2008-2011 the mean level of total cholesterol in men aged 16-64 declined from 5.6 to 5.2 mmol/l. This was accompanied by a notable decline in the proportion of men with a total cholesterol level of 5.0 mmol/l or above (from 69.8% to 57.8%). The greatest decrease occurred between 1995 and 1998. The proportion of men with a total cholesterol level of 5.0 mmol/l or above was lower in every age group in 2008-2011 compared with 1995.
Among women aged 16-64, the overall trend between 1995 and 2008-2011 was also one of decline both for mean cholesterol (from 5.6 mmol/l to 5.3 mmol/l) and for the proportion with levels of 5.0 mmol/l or above (from 67.8% to 59.9%). As with men, most of the decline occurred between 1995 and 1998 with little change in the figures since then.
The more recent trend, for all adults aged 16 and over from 2003 onwards, also showed a decline on both measures, largely driven by a particularly pronounced drop among men aged 75 and over (for example, the proportion of men aged 75 and over with levels of 5.0 mmol/l or above halved between 2003 and 2008-2011). Women aged 65 and over also saw large declines (of 14-17 percentage points) in the proportions with levels of 5.0 mmol/l or above. These figures include people taking lipid lowering drugs (LLD) such as statins, so the decline in total cholesterol will almost entirely be due to the increased use of such drugs. As the inset table below indicates, between 2003 and 2008-2011, there was a significant increase in LLD use among men and women particularly among those aged those aged 65 and over, to the extent that in 2008-2011, 44% of men, and 38% of women aged 65 and over took such drugs (compared with 25% and 20%, respectively, in 2003).
Prevalence of lipid lowering drug use, 2003 and 2008-2011 combined
| Aged 16-44 | Aged 45-64 | Aged 65 and over | All aged 16 and over | |
|---|---|---|---|---|
| % (95% CI)a | % (95% CI) | % (95% CI) | % (95% CI) | |
| Men 2003 | 1 (0.3-1.7) | 12 (10-14) | 25 (21-28) | 9 (8-10) |
| Men 2008-2011 | 1 (0.4-1.8) | 20 (17-23) | 44 (40-49) | 15 (14-17) |
| Women 2003 | 1 (0.3-1.3) | 7 (5-9) | 20 (17-24) | 7 (6-8) |
| Women 2008-2011 | 0 (0.1-1.0) | 12 (10-15) | 38 (34-42) | 13 (11-14) |
a 95% confidence intervals are shown to help interpret the trend (sample sizes= 5,444 in 2003 and 4,273 in 2008-2011)
Table 8.5 and Figure 8B show that, in 2008-2011, prevalence of a total cholesterol level of 5.0 mmol/l or above increased notably with age among men, from 21.9% of those aged 16-24 to 69.6%-73.3% of those aged 35-64, before declining to 59.9% at age 65-74, and further to 28.4% of those aged 75 and over. For women, the peak occurred at age 55-64 (84.0%) and the decline thereafter was much less pronounced so that a majority of women aged 75 and over (64.3%) had a total cholesterol level of 5.0 mmol/l or above. SIGN's recommendations for statin treatment are based on CVD risk and cholesterol levels, but they advise statins for anyone with a total cholesterol level of 8.0 mmol/l or above; in the 2008-2011 period just 1.4% of adults fell into this group (data not shown). Figure 8B, Table 8.5
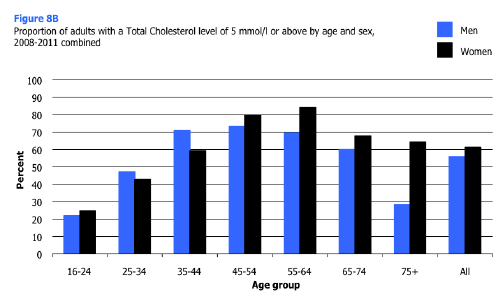
8.6.2 HDL cholesterol and total: HDL cholesterol ratio
Mean HDL cholesterol levels were the same in 2003 and 2008-2011 for both men (1.3 mmol/l) and women (1.6 mmol/l)50 and varied little by age. Men were more likely than women to have low levels of HDL cholesterol. While the proportion of men with HDL levels below 1.0 mmol/l increased between 2003 and 2008-2011 (from 7.7% to 10.8%), the figures for women were very similar (2.0% and 3.1%, respectively). The proportion of men with HDL cholesterol levels below 1.0 mmol/l varied with age in both 2003 and 2008-2011, but with no consistent pattern. In contrast, in 2003 the proportion of women with levels below 1 mmol/l was lowest among those aged 35-74, whereas in 2008-2011 it was broadly similar across all age groups.
As discussed in Section 8.2.4, the ratio of total cholesterol to HDL cholesterol is a stronger indicator of cardiovascular risk than either measure alone. The mean ratios were very similar in 2003 and 2008-2011 (4.2 and 4.1 respectively for men, 3.6 in both years for women). Ratios in 2008-2011 showed a similar inverted U-shaped distribution with age to that shown in Figure 8B for men's total cholesterol. For both men and women, ratios increased with age from 3.5 and 3.1, respectively, at age 16-24 to peaks of 4.7 in men aged 45-54, and 4.0 in women aged 55-64, before dropping to 3.5 for both men and women aged 75 and over. Table 8.6
8.6.3 Fibrinogen
Between 1998 and 2008-2011, mean fibrinogen levels in adults aged 16-74 increased from 2.6 g/l to 2.9 g/l in men, and from 2.8 g/l to 3.1 g/l in women. In contrast, the figures for adults aged 16 and over from 2003 onwards were more stable, for both sexes. Fibrinogen levels did not differ significantly by sex and increased with age among both men and women. For example, for men in 2008-2011 they increased from 2.7g/l at age 16-24 to 3.3g/l at age 75 and over. The equivalent figures for women were 2.9 g/l and 3.3 g/l in respectively. Table 8.7
8.6.4 C-reactive protein (CRP)
Mean CRP levels (measured as mg/l) from 1998 onwards are presented in Table 8.8. As CRP is not normally distributed (most people had very low levels of CRP so it was very skewed to the right), mean values are not a good measure of levels in the population. Instead, quintile distributions have been presented and are discussed to help illustrate the pattern over time, and between men, women and different age groups.
The 1998 CRP thresholds have been applied to the 2003 and 2008-2011 data to enable comparisons in quintile distributions over time to be made. Any analyses based on a single point in time would, of course, need to apply the quintile thresholds applicable to those data.
Although the mean CRP for men aged 16-74 changed little over time, there was some change in the proportions in the bottom two quintiles. Between 1998 and 2008-2011, the proportion in the bottom CRP quintile increased from 20.7% to 27.0%. This was coupled with a decrease (from 22.1% to 17.7%) in the proportion in the second quintile. The increase over time in the proportion of men in the lowest CRP quintile was greatest for men aged 55-64 (a doubling from 7.8% to 15.3%). However, in absolute terms, it was men aged 25-34 who experienced the largest percentage point increase (from 25.9% to 40.0%).
The pattern among women was a little different: the mean CRP level for those aged 16-74 was significantly lower in 2008-2011 (3.3 mg/l) than in 2003 (3.8mg/l) and lower, but not significantly, than in 1998 (3.6mg/l). The only notable changes in the proportions in each of the quintile groups between 1998 and 2008-2011 were a small decrease in the proportion in the highest quintile (from 20.0% to 17.3%), and a small increase in the overall proportions in the second to fourth quintiles (from 80.1% in 1998 to 82.7% in 2008-2011).
In every survey year, CRP levels were higher for women than for men, and levels for both sexes generally increased with age. For example, in 2008-2011, the proportion of men with a CRP level in the highest quintile increased from 9.4%-10.5% for those aged 16-34 to 19.9%-24.5% for those aged 55-74. The pattern for women fluctuated more, with those aged 55-74 also the most likely to have a CRP level in the highest quintile. Table 8.8
Contact
Email: Julie Ramsay