The Scottish Health Survey 2011: Volume 1 - Adults
Annual report of the Scottish Health Survey for 2011. Volume focussing on adult health
CHAPTER 4 SMOKING
Shanna Dowling
SUMMARY
- In 2011, 23% of all adults aged 16 and over were current smokers. The smoking rates for men and women were similar (24% and 22% respectively).
- Smoking prevalence was highest among those aged 25-34 (30%) and lowest among over 75s (8%).
- Rates of smoking among men and women aged 16-64 declined between 1995 and 2011, from 35% to 26%.
- There was also a significant decline in smoking rates among all adults aged 16 and over since 2003 from 28% to 23% in 2011. The two percentage point drop in the prevalence between 2010 and 2011 was statistically significant.
- In 2011, the mean number of cigarettes smoked per day by smokers aged 16 and over was 13.8. Female smokers smoked fewer cigarettes per day on average than male smokers (13.3 and 14.3 cigarettes respectively).
- There has been a decline over time in the mean number of cigarettes smoked per day. In 2011, 16-64 year olds smoked on average 3 fewer cigarettes per day than they did in 1995 (from 16.7 cigarettes per day to 13.7). The figures for all adults aged 16 and over also show a decline from 2003 (from 15.3 cigarettes per day to 13.8 cigarettes).
- There was a clear association between smoking prevalence and socio-economic classification. People living in semi-routine and routine households were more than twice as likely as those living in managerial and professional households to report that they smoked (36% compared with 15%). Smokers in semi-routine and routine households also had the highest mean number of cigarettes smoked per day (15.1 cigarettes).
- For both men and women, smoking rates steadily increased as household income decreased. People in the lowest household income quintile were almost three times as likely as those in the highest income group to report that they smoked cigarettes (40% compared with 14%). However, there was no significant variation in the number of cigarettes smoked per day.
- Four in ten adults living in the 20% most deprived areas in Scotland reported smoking cigarettes compared with just one in ten of those living in the 20% least deprived areas. The mean number of cigarettes smoked per day by smokers also increased in line with deprivation from 12.3 cigarettes in the least deprived quintile to 15.2 cigarettes in the most deprived group.
- An estimate of the percentage of people who mis-report themselves as non-smokers can be made by comparing self-reported smoking estimates with cotinine levels. In 2008-2011, the under-estimation of current smoking was 3 percentage points. Mis-reporting was greatest among men aged 16-24 and 65 and over (6 percentage point difference).
- The sharp decrease in non-smokers' exposure to second-hand smoke in public places seen in the decade between 1998 and 2008 was maintained in 2011 when 8% of non-smokers (aged 16 and over) reported being exposed to smoke in public places. Non-smokers' (aged 16-74) exposure to second-hand smoke in either their own or someone else's home fell from 31% in 1998 to 16% in 2011 for men and from 35% to 14% for women.
- Exposure to other people's smoke was also measured objectively using geometric mean cotinine levels. Since 2003 there has been a significant decline in geometric mean cotinine levels of non-smokers (from 0.40ng/ml to 0.11ng/ml) in 2010/2011. There was no change in levels between 2008/2009 and 2010/11.
- The geometric mean cotinine levels of male and female non-smokers were similar and levels did not vary significantly by age.
- Deprivation was strongly associated with non-smokers' cotinine levels. The geometric mean cotinine level for non-smokers living in the 20% most deprived areas in Scotland was three times that of those living in the least deprived group (0.20ng/ml compared with 0.07ng/ml).
4.1 INTRODUCTION
The Scottish Government's revised National Performance Framework (NPF), published in December 2011,1 includes a new national indicator to reduce premature mortality (deaths from all causes in those aged under 75).2 The fact that smoking, and its strong link to deprivation, is cited as one of the risk factors that needs to be addressed to reduce premature mortality underlines its status as one of Scotland's most significant public health concerns. It has been estimated that around 13,000 deaths a year are attributable to smoking - around a quarter of all deaths in Scotland.3 Smoking prevalence is itself the subject of a national indicator - reduce the percentage of adults who smoke4 - which is measured by the Scottish Household Survey.
The introductions to the smoking chapters in the 2008, 2009 and 2010 Scottish Health Survey (SHeS) Reports5,6,7 provided a comprehensive overview of the recent policy context and outlined a number of actions being taken by the Government and NHS to help support smokers to quit, and to discourage people from starting to smoke. These included:
- The introduction of a ban on smoking in public places in 2006.
- The raising of the legal age for buying tobacco from 16 to 18 in 2007.
- The strategic framework set out in the 2004 publication A Breath of Fresh Air for Scotland and the 2008 action plan Scotland's Future is Smoke-Free.
- The Tobacco and Primary Medical Services (Scotland) Act 2010, which introduced new measures specifically designed to reduce the attractiveness and availability of tobacco to those aged under 18.
- Plans to ban the display of tobacco products in shops. The implementation was originally planned to start in large stores in April 2012, and in April 2015 for smaller stores.8 Ongoing legal disputes have delayed its initial implementation, however the Scottish Government remains committed to the 2015 target.9
- The development of a new tobacco control strategy for Scotland, due to be published in 2012.
In April 2012, the Department for Health in England launched a 12-week UK-wide consultation outlining proposals to introduce plain packaging for cigarette products.10,11 The consultation document was developed with the support of the Scottish Government and the other devolved administrations in Wales and Northern Ireland. A systematic review of plain packaging conducted in response to the publication of the Department for Health in England's Tobacco Control Plan for England concluded "that plain packaging would reduce the attractiveness and appeal of tobacco products, it would increase the noticeability and effectiveness of health warnings and messages, and it would reduce the use of design techniques that may mislead consumers about the harmfulness of tobacco products".12
The above policy actions to reduce the attractiveness of smoking are complimented by a programme of support to assist existing smokers who want to quit. For example, one of Scotland's HEAT targets13 for the NHS focuses specifically on smoking cessation, and includes a deprived-focused element:14
NHS Scotland to deliver universal smoking cessation services to achieve at least 80,000 successful quits (at one month post quit) including 48,000 in the 40% most-deprived within-Board SIMD areas over the three years ending March 2014.
According to the most recent figures, between April and December 2011, 14,637 successful quit attempts were recorded in the SIMD target areas described above.14 This target replaced a similar target for boards to deliver 83,975 successful quit attempts in the 2008/9-2010/11 period; 89,075 were recorded.15
This chapter presents figures for prevalence of smoking among adults aged 16 and over and for non-smokers' exposure to second-hand smoke. Two sources of data are used: self-reported information and direct assessment of smoking status and second-hand smoke exposure via saliva samples. Trends from 1995 onwards will be presented. Self-reported smoking prevalence is presented by age, sex, National Statistics Socio-economic classification, household income and Scottish Index of Multiple Deprivation (SIMD). Saliva-recorded second-hand smoke exposure is also presented by SIMD.
4.2 METHODS
4.2.1 Smoking questions in the 2011 Scottish Health Survey
The survey has included questions on smoking since 1995. Some small changes were introduced to the questionnaire in 2008, as outlined in the 20085 Report. This information is not repeated here. Instead, the main measures and definitions used in this chapter are outlined.
Information about cigarette smoking was collected from adults aged 16 and 17 by means of a self-completion questionnaire which offered them the privacy to answer without disclosing their smoking behaviour in front of other household members. For adults aged 20 and over it was collected as part of the main interview. Those aged 18 and 19, at the interviewers' discretion, could answer the questions either in the self-completion booklet or the main interview.
For young adults, the smoking questions in the self-completion questionnaire focus upon:
- current smoking status
- frequency and pattern of current smoking
- the number of cigarettes smoked by current smokers
- ex-smokers' previous smoking history
- exposure to second-hand smoke.
The self-completion and main interview questions are mostly similar. However the main interview also asked about past smoking behaviour, desire to give-up smoking and medical advice to stop smoking. The question about non-smokers' exposure to second-hand smoke covers a range of domestic and public places, including some locations covered by the 2006 smoking ban (such as pubs). In previous reports, people who were not exposed to smoke in any of the places asked about were described as never being exposed to second-hand smoke. This is not wholly accurate as they might have been exposed to smoke in a location that was not asked about. The tables and text below have been amended to reflect this.
Since its inception, SHeS has been collecting saliva samples to assess people's cotinine levels. Cotinine, a derivative of nicotine, is an objective measure of smoking. Levels above a certain threshold indicate that someone has smoked recently while levels below the threshold are a measure of exposure to second-hand smoke. All those aged 16 years and over who were visited by the nurse were asked to provide a saliva sample in order to measure cotinine levels. The 2009 smoking chapter6 described why the cotinine threshold used to identify smokers changed from 15ng/ml (used in the 1995-2003 reports) to 12ng/ml (used from 2008 onwards).16 To ensure comparability, all trend data presented in this chapter use the 12ng/ml level.
The measurement of cotinine levels in the SHeS series provides an objective cross-check on self-reported smoking behaviour, which is known to under-estimate prevalence. Inaccuracies in reporting arise in part from difficulties participants may experience in providing quantitative summaries of variable behaviour patterns, but in some cases arise from a desire to conceal the truth from other people, such as other household members who may be present during the interview. This study is the only data source in Scotland which can provide a validated measure of self-reported smoking in this way.
This chapter updates the survey's measures of cotinine last presented in 2009.6 To increase the sample size available for analysis the data from the 2010 and 2011 surveys have been combined, and in some tables combined data for all four years (2008-2011) are presented.
4.2.3 Definitions
The tables reported in this chapter use the following classifications of smoking status:
- Current smoking status: current smokers, ex-regular smokers, ex-occasional smokers and never smoked at all.
- Mean number of cigarettes smoked by current smokers: this is measured as per smoker per day.
4.3 TRENDS IN SMOKING PREVALENCE SINCE 1995
Self-reported smoking status rates for adults aged 16-64 from 1995 to 2011 are presented in Table 4.1 along with rates for all adults aged 16 and over since 2003. Between 1995 and 2008 smoking prevalence among adults aged 16-64 declined from 35% to 29%. The rates did not change much in 2009 and 2010 (28%) but significantly decreased in 2011 (26%) This pattern of an overall decline among 16-64 year olds with a levelling out in more recent years was evident among both men and women and across all age groups. The decline in smoking rates since 1995 coincided with a gradual increase in the proportion of 16-64 year olds reporting that they had never smoked or had never smoked regularly (49% in 1995 and 57% in 2011). There was little change in the proportion of people describing themselves as ex-regular smokers between 1995 and 2011 (17%-19%).
There was also a decline in the mean number of cigarettes smoked per day by smokers (from 16.7 cigarettes per day to 13.7) between 1995 and 2011. This reduction was more apparent among men (18.1 cigarettes per day in 1995 to 14.2 in 2011) than women (15.4 and 13.2 respectively).
The trend in smoking prevalence for all adults (aged 16 and over) since 2003 was similar to that discussed above for those aged 16-64. The proportion of all adults aged 16 and over who smoked was 28% in 2003, ranged from 25%-26% between 2008 and 2010 and was 23% in 2011. The decline between 2010 and 2011 was statistically significant. Over this same period the proportion of adults who had never smoked or had never smoked regularly increased from 50% to 55%. Among smokers, there was a significant decline in the mean number of cigarettes smoked per day between 2003 and 2011 (from 15.3 cigarettes to 13.8). Table 4.1
4.4 SMOKING PREVALENCE IN 2011
4.4.1 Smoking prevalence, by age and sex
23% of all adults aged 16 and over reported smoking cigarettes in 2011 (24% of men and 22% of women). A similar proportion (22%) reported that they used to smoke regularly while over half (55%) had either never smoked at all or used to smoke but not regularly. This suggests that significant progress is being made on the National indicator to reduce the percentage of adults who smoke.1,17 Progress towards the indicator is being monitored via the Scottish Household Survey which had a smoking estimate of 23.3% in 2011. While there was no significant difference between the smoking rate for men and women, women were more likely to report having never smoked or never smoked regularly (57% compared with 52%).
As noted in previous SHeS reports,5,7 and shown in Table 4.1 there were some notable variations in cigarette smoking status by age. Smoking prevalence was highest among those aged 25-34 (30%) and lowest among those aged 65-74 (15%) and 75 and over (8%). Rates for the remaining age groups were very similar (ranging from 25% to 26%). The overall pattern of declining prevalence in the older age groups was true for both men and women but with slightly different patterning. The pattern for men was similar to that seen for all adults - a peak in smoking rates among those aged 25-34 (34%), followed by a steady decline to 8% among those aged 75 and over. In contrast, the rates among women under the age of 65 were very similar (ranging between 25%-27%) with the drop occurring in the oldest two age groups (15% aged 65-74 and 8% aged 75 and over).
The proportion of people describing themselves as an ex-regular smoker increased with age (from 4% for 16-24 year olds to 39% for those aged 65-74 and over). This increase was coupled with a decline by age in the proportions reporting that they had never smoked or had never smoked regularly (from 70% for 16-24 year olds to 46% for those aged 65-74 before rising slightly to 53% for those aged 75 and over). Both these patterns were more pronounced for men than for women.
In 2011 the mean number of cigarettes smoked per day was significantly higher for men than for women (14.3 compared with 13.3).
The number of cigarettes smoked per day was lowest among 16-24 year olds (10.6 cigarettes) and increased gradually to a peak of 16.7 cigarettes for those aged 45-64 before declining in the oldest age groups (12.6-15.3 cigarettes). The consumption patterns for male and female smokers were very similar with men aged 55-64 (18.7) and women aged 45-54 (16.3) smoking the most cigarettes per day. Table 4.1
4.4.2 Smoking prevalence, 2011, (age-standardised), by socio-demographic group
Tables 4.2 to 4.4 present self-reported smoking behaviour by socio-economic classification (NS-SEC of the household reference person), equivalised household income and the Scottish Index of Multiple Deprivation (SIMD) for 2011 (descriptions of each of these measures are available in the Glossary at the end of this volume). To ensure that the comparisons presented in this section are not confounded by the different age profiles of the sub-groups, the data have been age-standardised (for a description of age-standardisation please refer to the Glossary). On the whole, the differences between observed and age-standardised percentages are small. Therefore, the percentages and means presented are the standardised ones only.
Socio-economic Classification (NS-SEC)
As was the case when these data were last analysed in 2008,5 in 2011 there was a significant association between NS-SEC and smoking levels for both men and women.
The smoking rate of those in semi-routine and routine households was more than double that of those in managerial and professional households (36% compared with 15%). Rates for the intervening groups varied from 17%-27%. This pattern by socio-economic group was similar for men and women. People living in lower-supervisory and technical and semi-routine and routine households were less likely than others to report that they had either never smoked or had never smoked regularly (49% and 42% respectively compared with 58%-64% for the other groups). The proportion of people describing themselves as an ex-regular cigarette smoker did vary a little by NS-SEC but with no obvious pattern.
Among smokers, the mean number of cigarettes smoked per day also varied by NS-SEC and followed a similar pattern to that of smoking prevalence. Those in semi-routine and routine households smoked more cigarettes per day than those in managerial and professional and intermediate households (15.1 cigarettes compared with 12.4 cigarettes). Male smokers from small employers and own account worker households and female smokers from semi-routine and routine households had the highest daily consumption of cigarettes (16.0 and 14.6 cigarettes respectively). Figure 4A, Table 4.2
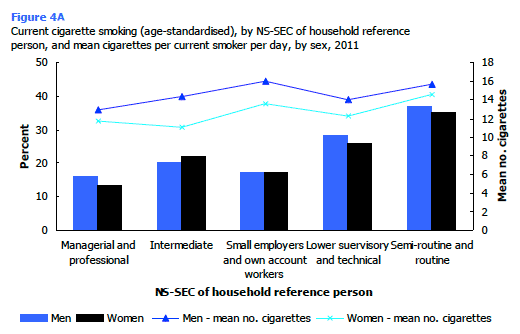
Equivalised household income
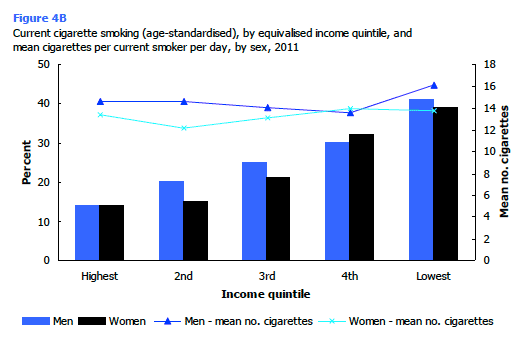
The significant association between self-reported smoking behaviour and equivalised household income is shown in Table 4.3 and Figure 4B.
For both men and women the smoking rate steadily increased in line with decreasing household income. People in the lowest household income quintile were almost three times as likely as those in the highest quintile to report that they currently smoked cigarettes (40% compared with 14%). The increase in prevalence by income coincided with a decrease in the proportions reporting that they had either never smoked or had never smoked regularly (65% in the highest income quintile compared with 41% in the lowest income group). The proportion of ex-regular smokers varied a little across income groups but with no obvious pattern. While smoking rates varied according to household income, for male and female smokers there was no significant variation in the mean number of cigarettes smoked per day across income groups. Figure 4B, Table 4.3
Scottish Index of Multiple Deprivation (SIMD)
Two measures of SIMD are being used throughout this report. The first, which uses quintiles, enables comparisons to be drawn between the most and least deprived 20% of areas and the intermediate quintiles. The second contrasts the most deprived 15% of areas with the rest of Scotland (described in the tables as the "85% least deprived areas").
As noted in the 20085 SHeS report and shown in Table 4.4 and Figure 4C, current smoking levels varied significantly according to area level deprivation. Four in ten adults (40%) living in the most deprived quintile were current smokers compared with just one in ten (11%) in the least deprived quintile. The pattern was slightly more pronounced for men with those living in the most deprived quintile four times as likely as those living the least deprived quintile to smoke (43% and 11% respectively). The equivalent figures for women were 38% and 11%.
Perhaps unsurprisingly, the increase in smoking prevalence as deprivation increased corresponded with a decrease in the proportion of men and women reporting that they had never smoked or had never smoked regularly. Two-thirds (67%) of those living in the least deprived quintile reported this compared with 39% of those in the most deprived quintile. Overall, there was little variation by deprivation in the proportion of adults who were ex-regular cigarette smokers although men in the most deprived quintile were less likely to report this than men in other areas (19% compared with 24%-25%).
The mean number of cigarettes smoked per smoker per day also increased in line with deprivation (12.3 cigarettes in the least deprived quintile compared with 15.2 for those in the most deprived). This was true for both male and female smokers but with slightly different patterning for both. For women, consumption was highest among those in the most deprived quintile but was fairly constant across the other groups (14.9 compared with 12.0-13.1). For men however, the largest difference occurred between the least deprived quintile and those living elsewhere (12.5 compared with 14.0-15.4).
In line with the findings across the quintiles, smoking prevalence among those living in the 15% most deprived areas was more than double that for the rest of Scotland (42% compared with 20%). This difference was particularly pronounced for men (45% compared with 21%). While there was no difference in proportion of people describing themselves as ex-regular smokers, those living in the 15% most deprived areas of Scotland were much less likely than those living elsewhere to report that they had never smoked or had never smoked regularly (38% compared with 58%).
Among smokers, those living in the 15% most deprived areas smoked the most cigarettes per day. This was particularly apparent for female smokers who smoked on average 3 cigarettes more per day than those living in the remaining 85% of areas in Scotland (15.5 cigarettes compared with 12.5 cigarettes). Figure 4C, Table 4.4
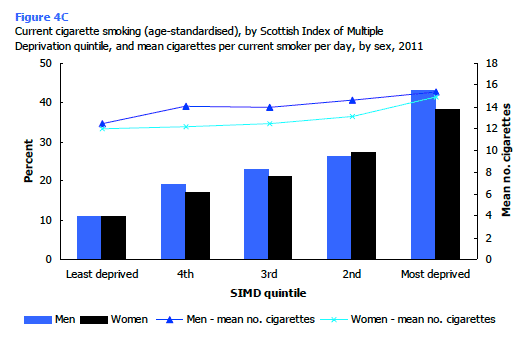
4.4.3 Cotinine-adjusted cigarette smoking status, by age and sex
The prevalence of smoking among adults before and after adjustment for saliva cotinine level is shown in Table 4.5. Note that the figures presented in this table are based on the sub-sample of participants who were eligible for a nurse visit and who provided a valid saliva sample. As the sample size is smaller than for the main survey interview, the figures presented here are based on combined data from the 2008 to 2011 surveys, so the self-reported estimates differ slightly to those in Table 4.1.
As discussed in Section 4.2.2, self-reported non-smokers with a cotinine level of 12ng/ml or above are very likely to be recent and/or regular smokers who have not disclosed their true smoking status in the main interview. The adjusted prevalence was calculated by classifying people as smokers if their cotinine level was 12ng/ml or above. However, the overall smoking prevalence for all adults eligible for the nurse visit, and for those who provided a valid cotinine sample differed as people who reported that they smoked were less likely than non-smokers to have participated in the nurse visit and/or provide a saliva sample. To analyse the adjusted smoking prevalence, the sub-sample of those with a valid saliva cotinine measurement was weighted back to the smoking profile of all adults who were eligible to take part in the nurse visit by age and sex, to correct for this bias in response.
In the 2008-2011 period, 24% of adults (24% of men and 23% of women) aged 16 and over reported being a current cigarette smoker. The adjusted rates, validated by participant cotinine levels, were 27% for all adults, 28% for men and 26% for women. This gap of three percentage points between self-reported smoking status and the adjusted smoking prevalence is consistent with findings from the 2003 and 2009 reports.6, 18 As shown in Table 4.5, the gap between the self-reported and validated estimates were greatest for men aged 16-24 and 65 and over (6 percentage point difference) and women aged 35-44 (4 percentage point difference). Table 4.5
4.5 EXPOSURE TO SECOND-HAND SMOKE
4.5.1 Trends in exposure to second-hand smoke since 1998 by age and sex
Since 1998, non-smokers have been asked whether they were regularly exposed to second-hand smoke in a variety of public and private settings. Previous SHeS reports5,6,7 have noted that exposure had fallen markedly since the introduction, in 2006, of the ban on smoking in public places. Non-smokers' self-reported exposure to smoke in a variety of contexts since 1998 is presented in Table 4.6. As the 1998 survey did not include adults aged 75 and over the below discussion of trends is based on adults aged 16-74. Figures for all adults aged 16 and over since 2003 are also presented in the table.
The proportion of non-smokers aged 16-74 who reported being exposed to second-hand smoke in any public place declined substantially from 50% in 1998 to 7% in 2008 and has remained fairly constant since then (7%-8% in the period 2009 to 2011). Over this same period there was also a significant drop in non-smokers exposure to smoke in the home (either own home or someone else's home) from 33% in 1998 to 20% in 2008. The 2009 and 2010 figures (19% and 18% respectively) were similar to the 2008 figure while there was a further small drop to 15% in 2011. The decline observed among those aged 16-74 between 2008 and 2011 was statistically significant.
These decreases in self-reported exposure to smoke were coupled with a corresponding increase in the proportion of non-smokers aged 16-74 reporting that they were not exposed to other people's smoke. In 1998 and 2003 the proportions reporting that they were not exposed to second-hand smoke in any of the places asked about were 36% and 40% respectively. This increased to 74% in 2008, 75% in 2009 and 2010 and 77% in 2011. These trends were similar for men and women.
Looking at figures for all adults aged 16 and over since 2003, the biggest drops in exposure to smoke both within and outwith the home also occurred between 2003 and 2008. There was an additional significant decline in the proportion of non-smokers reporting that they were exposed to second-hand smoke in their own or someone else's home between 2010 and 2011 (from 17% to 14%).
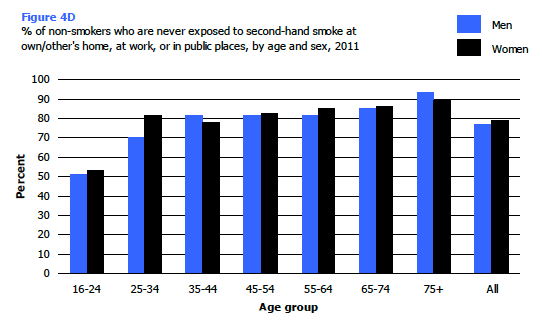
While the decline in exposure to second-hand smoke (in both public and private contexts) occurred across non-smokers of all ages, there were still some notable age differences in reported exposure levels. In 2011 for example, the youngest non-smokers (those aged16-24) were twice as likely as 25-74 years olds and around three times as likely as those aged 75 and over to report that they were exposed to smoke in their own or someone else's home (30%, 12-15% and 8% respectively). The same was true for exposure in any public place with 26% of those aged 16-24 reporting this compared with 2-8% for the remaining age groups. Figure 4D, Table 4.6
4.5.2 Trends in exposure to second-hand smoke: non-smokers' cotinine levels since 2003
The geometric mean19 cotinine levels of non-smokers in 2003, 2008/2009 and 2010/2011 are presented in Table 4.7. To be included in this analysis, self-reported non-smokers had to have a cotinine level below 12ng/ml (higher levels would suggest that these were smokers who misreported their behaviour in the interview). As the distribution of the data for non-smokers was very skewed, geometric means have been used rather than arithmetic means as these take into account extreme values (the Glossary at the end of this volume contains more details of these terms).
Non-smokers' geometric mean cotinine levels reduced significantly from 0.40ng/ml in 2003 to 0.11ng/ml in 2008/09 and remained at this level in 2010/2011. As Table 4.7 demonstrates, levels for male and female non-smokers were the same in 2010/2011 with both experiencing a decline since 2003. In 2003 the youngest age group (16-44 year olds) had significantly higher cotinine levels than older non-smokers (0.48ng/ml compared with 0.33-0.35ng/ml). The 2009 report6 noted that by 2008/2009 this difference across age groups had largely disappeared and by 2010/2011 there was no longer a significant difference in the mean cotinine levels by age (0.11ng/ml for all age groups). While there were some small differences by age, when the levels for male and female non-smokers when examined separately, these were not significant. Table 4.7
4.5.3 Non-smokers' cotinine levels by Scottish Index of Multiple Deprivation (SIMD)
The geometric mean cotinine levels of non-smokers by SIMD for the 2008 to 2011 period combined is shown in Table 4.8. Area level deprivation was strongly associated with the saliva cotinine levels of non-smokers. The geometric mean cotinine level for non-smokers living in the most deprived quintile was around three times higher than it was for those living in the least deprived quintile (0.20ng/ml compared with 0.07ng/ml). Levels for those in the intervening quintile groups ranged from 0.10ng/ml to 0.13ng/ml. This pattern was true for both male and female non-smokers but was slightly more pronounced for males (0.22ng/ml in the most deprived quintile compared with 0.07ng/ml in the least deprived quintile).
These differences were also apparent when the geometric mean cotinine level of non-smokers in the most deprived 15% of areas was compared with that for the rest of Scotland. The geometric mean cotinine levels for both male and female non-smokers living in the 15% most deprived of areas in Scotland were significantly higher than for those living elsewhere (0.25ng/ml and 0.20ng/ml for male and female non-smokers in the most deprived 15% of areas compared with 0.10ng/ml for those living in the rest of Scotland). Table 4.8
Contact
Email: Julie Ramsay