Scotland and the sustainable development goals: a national review to drive action
This review provides a statement of our pre-COVID-19 ambition on driving progress towards the United Nations Sustainable Development Goals in Scotland. It brings together evidence, actions and stories of how we are making progress to meet the Goals.
3 Good Health and Well-Being
- Health
- Education
- Children
Scotland’s ambition is to be a ‘healthy and active nation’, as outlined in the NPF. To be a more successful country we need to close the gap between the health of our wealthiest communities and that of our poorest, and we need to see an overall improvement in our population health. While the solutions to improving our health are not wholly reliant on the NHS itself, we remain absolutely focused on our NHS meeting our needs now and being fit for the future. Scotland is taking a long term strategic approach to fulfilment of Goal 3, focusing on excellent health care services, as well as preventative population health approaches such as introducing minimum unit pricing for alcohol.
Closer Look - Equally Well Govanhill (EWG)
The EWG test site was a localised partnership approach involving the public and third sectors aiming to improve life quality and environmental conditions in this area of Glasgow. Established service structures have limitations when approaching complex issues such as health inequalities. The EWG test site has shown the importance of participation and empowerment, including participatory budgeting and ‘community anchors’ (community-based organisations involved in public health interventions). This in itself is not enough to improve local outcomes and eradicate poverty, although it may help reduce regional discrepancies as well as further Scotland’s progress in meeting Goal 3.
Our NHS is committed to Realistic Medicine, which puts the person receiving health and care at the centre of decision making and encourages a personalised approach to their care. Its aims of reducing harm and waste, tackling unwarranted variation in care, managing clinical risk, and innovating to improve, are essential to a well-functioning and sustainable NHS.
Maternal, infant and young children care (targets 3.1 and 3.2)
Scotland has extremely low maternal and child mortality. Maternal mortality in the UK continues to decline, and between 2013 and 2017 was less than 10 deaths per 100,000 live births. Neonatal and infant mortality in Scotland also continue to decline, with a neonatal mortality rate of less than 2.5 deaths per 1000 live births since 2013 and infant mortality rate of less than 3.6 per 1000 live births since 2013. Following the most recent peak in 2007, pregnancies in young people aged under 20 in Scotland are now at their lowest level since reporting began in 1994. Since 2007, rates per 1,000 in the under 20 age group have decreased by 45.1%, rates for under 18s have decreased by 55% and rates for under 16s have decreased by 60.6% (target 3.7).
Maternal care
The Scottish Government is committed to providing the best start for all children and that begins in pregnancy. In 2019 the Scottish Government announced a £12 million package to transform maternity and neonatal services across Scotland. The vision for maternity and neonatal care set out in The Best Start is one where all mothers and babies are offered a truly family-centred, safe and compassionate approach to their care, recognising their own unique circumstances and preferences.
This includes a new model for neonatal care, which is currently being tested in two areas covering four health boards, as well as a range of initiatives to give mothers and other family members the support they need. We are also introducing continuity of carer within maternity services which will completely transform the delivery of care. As well as improved relationships between the women and midwife, evidence tells us that we can expect to see other improvements in outcomes for both the mother and baby, for example a reduction in pre term and still births, a reduction in interventions during labour, an increase in spontaneous vaginal deliveries and an increase in successfully feeding their babies.
Postnatal support
The Scottish Government is supporting the delivery of a new universal health visiting underpinned by the Universal Health Visiting Pathway in Scotland, published in October 2015, which sets out 11 core home visits for all families from late pregnancy until school entry, and provide an opportunity for health visitors to build relationships with families and children, in which the health visitor can act as a gateway to other services.
Young people’s wellbeing
Children living in Scotland experience some of the poorest health in Europe, and there are marked inequalities in the health they experience. The RCPCH State of Child Health Report presented worrying statistics about the health of Scottish children. in 2015/16 roughly 23% of children entering school in Scotland were overweight or obese, children from more deprived background were more likely to enter school as obese or overweight. A higher proportion of young people coming from more deprived backgrounds were also likely to smoke. Both smoking and experience of overweight and obesity have been linked to a range of negative health outcomes later in life.
Similarly, outcomes for child and adolescent mental health are extremely troubling. A 2018 Audit Scotland report showed a 22% increase in referrals to specialist services since 2013/14. The report also showed that 26% of children and young people are waiting more than 18 weeks to see a specialist, an increase of 11% since 2013/14. Recent research by SAMH has also shone a light on the high rejected referrals rate from Child and Adolescent Mental Health Services (CAMHS).
The Scottish Government has established and Children and Young People’s Mental Health Taskforce to provide recommendations for improvement in the provision for children and young people’s mental health in Scotland. In response to the Taskforce’s initial recommendations the Scottish Government has invested an additional £4 million in CAMHS to provide 80 new staff. In the coming year COSLA and the Scottish Government will take forward the Taskforce’s concluding recommendations. Community wellbeing services will be established across Scotland, initially focused on children and young people from the ages of 5-24 who, importantly, will be able to self-refer to the service. In addition, a range of other actions will be progressed, including: the provision of additional counsellors across Scotland’s secondary schools, and supporting testing of the Distress Brief Intervention programme in Aberdeen, Inverness, Borders and Lanarkshire.
It is recognised by the Scottish Government that children’s and young people’s wellbeing is a key driver to positive life course trajectories. The Getting it Right for Every Child (GIRFEC) approach supports children and young people so that they can grow up feeling loved, safe and respected and can realise their full potential. The Children and Young People (Scotland) Act 2015 defines Child Wellbeing in terms of 8 indicators of wellbeing: Safe, Healthy, Active, Nurtured, achieving, Respected, Responsible, and Included. These wellbeing indicators hep make it easier for children and families and the people working with them to discuss how a child or young person is doing at a point in time and if there is a need for support.
In order to provide the best start for children born to first-time teenage parents, the Scottish Government introduced Family Nurse Partnerships. Negative experiences and poor parenting during pregnancy and early childhood can damage a child’s brain development, behaviour, learning, and long term health. The Family Nurse Partnerships supports young mothers to make positive decisions for themselves and their children. A specially trained nurse visits the homes of first-time teenage mothers from early pregnancy until their child is two years old.
Childhood Adversity can create harmful levels of stress which impact healthy brain development. This can result in long term effects on learning, behaviour, and health. Adverse Childhood Experiences (ACEs) have been found to be associated with a range of poorer health and social outcomes in adulthood and that these risks increase as the number of ACEs increase. The Programme For Government 2018-2019 sets out commitments to prevent ACEs and reduce the negative impacts of ACEs where they occur and supporting the resilience of children, families, and adults in overcoming adversity. The four key areas the Scottish Government is taking forward action are:
1. Providing inter-generational support for parents, families, and children to prevent ACEs
2. Reducing the negative impact of ACEs for children and young people
3. Developing adversity and trauma-informed workforce and services
4. Increasing societal awareness and supporting action across communities
The Scottish Government, In collaboration with NHS Education for Scotland, have announced funding to deliver a national trauma training program to help the current a future workforce develop skills and services that respond appropriately to people’s adverse childhood experiences and other traumatic experiences.
Life expectancy
Long term increases in life expectancy in Scotland have stalled and health inequalities have worsened. NHS Health Scotland report that the pattern is similar in England and Wales, the USA, Iceland and Northern Ireland and that policies of austerity are having an adverse impact. The issues are complex and relate to enduring inequalities, deprivation and poverty, and changes in the pattern of disease.
In December 2018, Glasgow Centre for Population Health published a report into trends in earnings and income inequalities in Scotland and the UK, 1997‑2016. It notes that income inequalities in Scotland have widened considerably since the late 1970s. The author said there was “absolutely no evidence of progress” over the last 20 years in tacking the gulf between rich and poor, and claimed attempts to tackle health inequalities are doomed to failure while income inequality remains unaddressed.
Recent work by NRS and NHS Health Scotland showed that the three areas that were impacting on life expectancy the most were: reduced gains from improvements in heart disease mortality, drug-related deaths and dementia.
Mental health (target 3.4)
There has been a steady and significant increase in the proportion of adults who have two or more symptoms of depression (8% in 2010/11 to 11% in 2016/17). Since 2002, the rate of suicide has generally been on a downward trend, to 14 deaths per 100,000 population in 2018. In 2018, the probable suicide rate for males was three times that for females. There is a known link between deprivation and suicide. Between 2014 and 2018 the probable suicide rate was three times higher in the most deprived areas compared to the least deprived areas.
As awareness of the far-reaching impact and danger of poor mental health is better understood, the Scottish Government has committed to further action to tackle it. In March 2017, they published the Mental Health Strategy 2017-2027. The strategy’s vision is a Scotland where people can get the right help at the right time, expect recovery, and fully enjoy their rights, free from discrimination and stigma.
In line with the Strategy, the Scottish Government announced a package of measures to increase support for good mental health for children, young people and adults. Over the next five years, the Scottish Government will invest an additional £250 million to support the delivery of this package, through all levels of government, public services, third sector and communities. This includes specific support for new mothers, including counselling (for 11,000 mothers, delivered through the third sector); and specialist help and services (for 7,750 mothers).
To make sure that children and young people have the support they need at the earliest possible stage, the Scottish Government is investing £60 million in additional school counselling services. This will create around 350 counsellors in school education ensuring that every secondary school has counselling services. There will be an additional 250 school nurses in place by 2022, to provide a response to mild and moderate emotional and mental health difficulties experienced by young people.
The Data Picture: Mental wellbeing
In 2018, the mean Warwick-Edinburgh Mental Wellbeing Scale (WEMWBS) for adults in Scotland was 49.4, not significantly different to 2017 but the lowest since the series began in 2008 where it was 50.0.
WEMWBS scores decrease (indicating poorer wellbeing) as area deprivation increases. The mean WEMWBS score in the most deprived 20% of areas (47.0) was significantly lower than in the least deprived 20% of areas (51.6).
Column chart showing the average score on the Warwick-Edinburgh Mental Wellbeing Scale in 2018 by Scottish Index of Mutliple Deprivation quintiles. There was a gradual decrease of scores, from 51.6 in the 20% least deprived quintile, down to 47 in the 20% most deprive quintile.
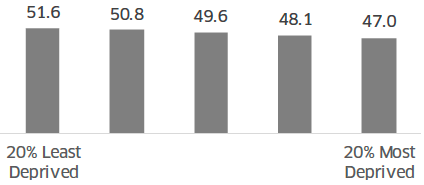
Source: Scottish Health Survey
In August 2018 the Scottish Government published its new Suicide Prevention Action Plan Every Life Matters. This sets out ten measures to continue the strong decline in the country’s rate of deaths by suicide. It has a target to reduce the rate by 20% by 2022 (from a 2017 baseline).
Health and housing
The relationship between making a homelessness application and more interactions with health services shows that the integration of housing advice in health settings is essential. The right advice, at the right time, can help ensure the housing safety net is in place for anyone who falls into housing crisis, ensuring everyone gets the support they need. Shelter Scotland provides outreach advice services in many health locations, including in GP surgeries and specialist housing advice in A&E in Victoria Hospital, in Fife, as part of a two-year partnership project with Fife Health and Social Care Partnership.
We know that, in general, people who have experienced homelessness have higher health needs than those who have not been through the homelessness system – particularly in relation to mental health and addictions. We also know, from the higher rate of missed appointments for people who have experienced homelessness, that people can find it harder to engage with traditional services during the crisis of homelessness. Again, this shows the need for an integrated response to ensure that the health needs of this group are adequately met, and for health and housing services to work together to tackle health inequalities and both prevent and alleviate homelessness.
Shelter Scotland has commissioned research this year to establish what practical changes are needed to improve service provision for people experiencing homelessness with mental health difficulties so that they can access and receive the right support for them.
Non communicable diseases (target 3.4)
Mortality rates from Scotland’s leading causes of death - including cancer, coronary heart disease (CHD), respiratory conditions and stroke - are declining long term following lifestyle improvements and improved health care (target 3.4). Scotland is on track to meet the SDG ambition of a one-third reduction by 2030. The overall mortality rate has dropped by 27%, from 1,560 per 100,000 in 1994 to 1,136 per 100,000 in 2016. This reflects a cumulative decline in cancer (18%, to 311 per 100,000), respiratory conditions (25%, to 149 per 100,000) and cerebrovascular (including stroke) mortality (60%, to 85 per 100,000) between 1994 and 2016.
Scotland has a high prevalence of the risk factors associated with heart disease, such as smoking, poor diet and physical inactivity. The mortality rate for heart disease fell by 35.5% between 2008 and 2017. However, the rate of decline has slowed in the last five years with increases in 2015 for both sexes and in the males rate only for 2017. Overall, it is estimated that around 6.4% of men and 4.0% of women are living with CHD (Scottish Health Survey 2017). Treating and preventing heart disease is a national clinical priority for Scotland, as outlined in the Heart Disease Improvement Plan.
Diet and healthy weight
It has remained challenging for Scotland to meet its dietary goals, and equally challenging to tackle the associated health inequalities. Nearly two thirds of people (65%) who live in Scotland continue to be overweight or obese; 26% of children are still at risk of becoming overweight or obese; and 33% of adults who live in the most deprived areas are obese compared with just 20% in the least deprived areas (Scottish Health Survey 2017).
A number of policies and initiatives aim to tackle obesity and diet as public health issues, for example, the Scottish Government published A Healthier Future: Scotland’s Diet and Healthy Weight Delivery Plan in July 2018. The plan sets out a vision “to create a Scotland where everyone eats well, and we all have a healthy weight”, and includes ambitions to halve childhood obesity by 2030 and to reduce health inequalities significantly. The actions in the plan are framed around five key themes: children and young people; transforming the food environment; weight management services; leadership; and health inequalities.
The Scottish Government has consulted on restricting the promotion and marketing of food and drink high in fat, sugar or salt where they are sold to the public and will bring forward a Bill on Restricting Foods Promotions for introduction in the 2020/21 Legislative Programme.
While legislation is not the only way to make progress, we recognise that there is a clear place for legislation to underpin the considerable work that is already being done to realise our Good Food Nation ambitions. The role of third-party stakeholders in both food provision and efforts to increase food education is significant, and noted as an avenue for expansion in the Scottish Government’s Independent Working Group on Food Poverty in 2016. The Scottish Government has committed to an enhanced £2 million fund to respond to food insecurity during the school holidays working with COSLA, local authorities, the third sector and other stakeholders. Further detail on food is included in Goal 2.
Closer Look – Children in Scotland
Children in Scotland co-ordinate the Children’s Sector Strategic and Policy Forum. The Forum is made of leaders from across the children’s sector to tackle issues of strategic importance. The Forum focuses on three main areas of work: Reducing Child Poverty; promoting Health and Wellbeing; and embedding the Meaningful Participation and Engagement of Children and Young People. The Forum has a role in scrutinising the implementation of the Tackling Child Poverty Delivery Plan and will advise the Scottish Government on cross-government co-ordination in delivering the plan.
Reproductive health (target 3.7)
It is widely recognised that short inter-pregnancy intervals of less than 12 months are associated with an increased risk of obstetric and neonatal complications including preterm birth, stillbirth and neonatal death. The provision of post-partum contraception (PPC) has therefore been a policy priority for the Scottish Government for some time. It is set out in the Refreshed Maternity Framework (2011), the Sexual Health and Blood Borne Virus Framework Update (2015) and the Pregnancy and Parenthood in Young People Strategy (2016).
The provision of long acting reversible contraception (LARC) methods as part of PPC is particularly key, as these provide a high level of efficacy and are independent of adherence for their effectiveness . However, it is essential that women are always offered LARC as a choice within a range of methods (if any is desired) so that they remain in control of their own reproductive health.
The APPLES (Accessing Post-Partum LARC in Edinburgh South East) project looked at improving access to contraception for postpartum women, with particular emphasis on LARC methods. This is now being rolled out across NHS Lothian. The Scottish Government has provided funding for pilot projects in NHS Greater Glasgow and Clyde and NHS Ayrshire and Arran to test rolling out provision of post-partum contraception in those areas.
Sexual health and blood borne viruses (targets 3.3 and 3.7)
In July 2017, Scotland became the first of the UK nations to provide PrEP (Pre-exposure Prophylaxis) through the NHS to prevent HIV and in the first year of its availability over 1,800 people started on PrEP. In 2018, Scotland achieved the UNAIDS 90-90-90 targets on HIV, with an estimated 91% of people living with HIV knowing their diagnosis, 98% on antiviral therapy, and 97% of those on treatment being virally suppressed.
There is no room for complacency, and the Scottish Government is providing funding of over £2 million between 2018 and 2021 to organisations tackling poor sexual health and blood borne viruses, and is working with third sector organisations to ensure progress is maintained. Current work includes ongoing consultations with the community and wider sector on the challenges of HIV in Scotland through the Scottish Parliament’s Cross-party Group on Sexual Health and Blood Borne Viruses. There is a wide range of organisations, including Waverley Care, HIV Scotland and Hepatitis Scotland who are working to reduce stigma and improve outcomes for those with communicable diseases.
Tobacco, alcohol and substance use (target 3.5)
Reducing the use of and harm from alcohol, tobacco and other drugs is a priority in Scotland.
Smoking
Smoking remains the greatest threat to health in Scotland contributing to over 9,000 deaths per year and over 100,000 hospital admissions per year. The percentage of adults who had never smoked regularly or at all increased from 50% in 2003 to 56% in 2017; the figure for ex-regular smoking increased from 22% to 26%
An action plan on Raising Scotland’s tobacco-free generation was published by the Scottish Government in June 2018. This sets out a five year action plan to continue with our ambition to create a tobacco free generation by reducing smoking rates to 5% or less by 2034. Smoking is an inequalities issue: Health inequalities and socio-economic inequalities tend individuals towards smoking; smoking is a principal driver for health inequality and a contributor to socio-economic inequalities. By setting targets each year for our stop-smoking services to achieve successful quits in our most deprived communities, Scotland is reducing health inequalities in respect of smoking. In 2018 Cancer Research UK measured the success of this approach and recommended the rest of the UK to follow Scotland’s lead. By reducing its levels of smoking, Scotland is likely to be reducing levels of health inequality - when comparing health outcomes between smokers and non-smokers there is a significant inequality relationship. Turning smokers into non-smokers will further help balance the health inequalities between those groups.
The 2018 action plan includes significant shorter-term initiatives such as removing all tobacco from prisons and making it an offence to smoke near hospital buildings. The action plan also includes proposals for the longer term such as more effective pricing interventions and actions that could be taken to reduce smoking in homes and reduce the clustering of tobacco outlets in less well-off communities.
The Data Picture: Smoking
Target 3a aims to strengthen the implementation of the World Health Organization Framework Convention on Tobacco Control in all countries, as appropriate.
In 2018, 19% of adults smoked, not significantly different to 2017 but a significant fall since 2003 (28%).
Graphic showing the number of men and women smoking, as well as the average cigarettes smoked. 17% of women reported that they were smoking in 2018, down from 28% in 2003. Women on average smoked 10.8 cigarettes per day in 2018, down from 14.7 in 2003. 21% of men reported that they were smoking in 2018, down from 29% in 2003. Men smoked on average 12.7 cigarettes per day in 2018, down from 15.9 in 2003.

Source: Scottish Health Survey
Substance use
Drug-related deaths in Scotland are rising and Scottish ministers have described the situation as a public health emergency. They are convening a taskforce to examine the main causes of drug deaths and advise on what changes could help save lives.
The Data Picture: Drug-related deaths
Target 3.5 Strengthen the prevention and treatment of substance abuse, including narcotic drug abuse and harmful use of alcohol.
In 2018 there were 1,187 drug-related deaths in Scotland, the highest since records began in 1996. This is more than double the 574 deaths recorded a decade earlier, in 2008.
Line graph showing the number of drug-related deaths in Scotland rising and falling but with a generally upward trend between 2007 and 2013, but then increasing consistently from 2013 to 2018.
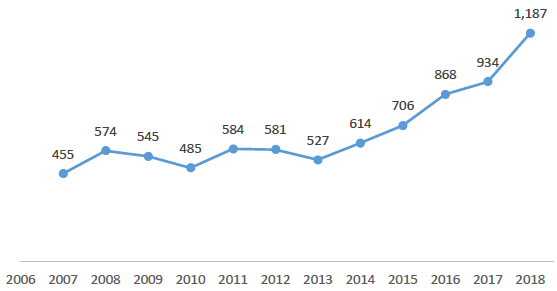
Source: National Records for Scotland, Drug-Related Deaths in Scotland, 2018
The Scottish Government’s approach to drugs policy is underpinned by a public health approach, guided by a principle of ensuring the best health outcomes for people who are, or have been, drug users (target 3.5).
The Scottish Government currently provide £53.8 million each year to Alcohol and Drug Partnerships, supplemented by £20 million annually following its 2017-18 Programme for Government for the combined Alcohol and Drugs Treatment Strategy, Rights, Respect, Recovery published in November 2018. The strategy focuses on prevention and early intervention, developing recovery oriented systems of care, getting it right for children, young people and families, and taking a public health approach to justice. This approach represents a strengthened approach to tackling the issue of drug use through a public health lens, seeking to divert people who use drugs away from the criminal justice system. In addition the Scottish Government committed in its 2019-20 Programme for Government to make an additional £20 million of funding available over two years to address the public health emergency of drug deaths in Scotland. This will allow the new Drug Deaths Taskforce to support innovative projects and test new approaches to improve the quality of services, to establish joint working protocols between alcohol and drug services and mental health services, and allow the development of a national pathway for opiate substation therapy.
Glasgow City Health and Social Care partnership are pursuing proposals to pilot a medically supervised overdose prevention facility – designed for an estimated 400-500 people who inject publicly and experience high levels of harm. The facility is expected to reduce the risk of further outbreaks of blood-borne viruses, though Scotland does not currently have all of the powers necessary to realise the facility.
Higher-risk alcohol use
The Scottish Government continues to take a whole population approach which aims to reduce alcohol consumption and the risk of alcohol-related harms across a population, because Scotland’s consumption remains too high.
In 2017, Scots bought enough alcohol (10.2 litres of pure alcohol) for everyone aged over 16 to drink 19.6 units of alcohol every week. This is 40% more than the UK CMOs’ low risk drinking guidelines of 14 units a week and 17% higher than in England & Wales. In 2017/18, there were 35,499 alcohol-related hospital admissions in general acute hospitals which represents a 2.5% decrease on the previous year but more than four times the level seen in the early 1980s.
The Alcohol Framework 2018: Preventing Harm, published in November 2018, sets out priorities for preventing alcohol-related harm, and builds on the progress made with the previous Alcohol Framework. A key focus is the reduction of health inequalities as there are more alcohol-related hospital admissions and deaths in the most deprived areas compared with the least. Minimum unit pricing targets harmful drinkers with a particular focus on harmful drinkers living in poverty.
The Data Picture: Alcohol specific deaths in Scotland
Target 3.5 (Indicator 3.5.2) aims to reduce the harmful use of alcohol, defined according to the national context as alcohol per capita consumption (aged 15 years and older) within a calendar year in litres of pure alcohol. Alcohol related deaths have decreased since 2011 but are still nearly three times more than in the early 1980s.
The number of males suffering from alcohol related deaths is approximately double that of females.
Line graph showing the number of alcohol-specific deaths overall, and for male and females. All three lines show a fairly flat trend between 1981 and 1993, before rising to a peak in 2006. Between 2007 and 2012 there is a gradual decrease. From 2013 to 2018 there is a gradual increase.
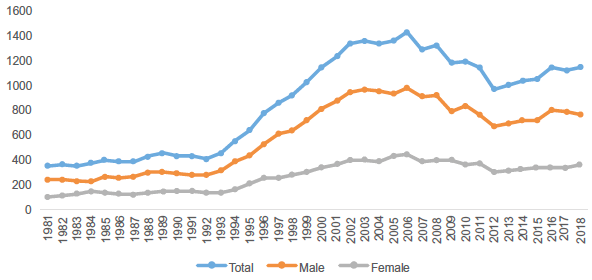
Source: National Records of Scotland, Alcohol-specific deaths, 2017
Road accidents and injuries (target 3.6)
There were 9,428 road accident casualties reported in 2017, 14% fewer than in 2016. The number of reported accidents has been falling over the past ten years, and in 2017 was 43% lower than in 2007; the lowest figure since current records began in 1970. There has been a long term downward trend in road traffic fatalities. In 2017 there were 146 people killed in road accidents in Scotland, a decrease of 24% on 2016, and the lowest level since annual records began in 1950.
This is mostly due to the governance structure of our road safety policy (where a collaborative approach to take Scotland towards an ultimate vision of zero fatalities and to meet five challenging casualty reduction targets is implemented) and the size of Scotland that allows agile planning and delivery between various partners.
Scotland’s road safety vision is that there will be “A steady reduction in the number of those killed and those seriously injured with the ultimate vision of a future where no-one is killed on Scotland’s road, and the injury rate is much reduced.” In 2009 our Road Safety Framework to 2020 was published setting out Scotland road safety targets to 2020.
The Data Picture: Road deaths
Target 3.6 (Indicator 3.6.1) aims to halve the number of global deaths and injuries from road traffic accidents.
In 2018, 160 people were killed, declining over the longer term from 281 deaths in 2007. There were more male fatalities (109) than female fatalities (51). 1,581 people were seriously injured in 2018.
Line graph showing the number of road casualty deaths between 2007 and 2018. The chart shows a gradual decrease between 2007 and 2013. Between 2014 and 2018 the chart rises and falls, but with a generally downward trend.
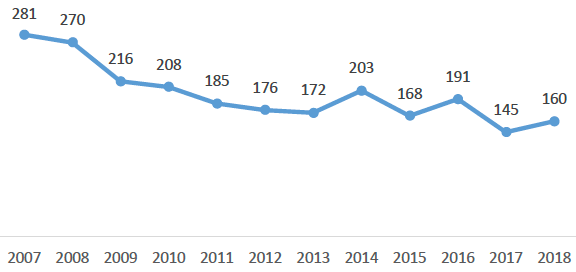
Source: Transport Scotland, Reported Road Casualties, 2018
Challenges and next steps
There are a number of broad areas where outcomes for young people show substantial room for improvement. Many of these are interrelated. Scotland continues to have some of the highest levels of diet‑related poor health in the world.
Among children, diet falls short of recommended good practice, with just over one in ten children eating the recommended five portions of fruit and vegetables and only two thirds eating breakfast every day. A substantial minority of children also do not meet the recommended guidelines of an average of 60 minutes of moderate-to-vigorous physical activity per day across the week. Maternal obesity during pregnancy has also increased since it was first recorded in 2011 and again displays a strong deprivation gap (Child and adolescent health and wellbeing: evidence review, 2018).
The poor performance on diet and physical activity is also likely to contribute to falling levels of mental wellbeing, another source for concern. Some mental wellbeing measures have shown a worsening position in recent years. The Scottish Government are working with partners in the public and third sector to develop a 10-year Child and Adolescent Health and Wellbeing Action Plan which will focus on improving health and wellbeing outcomes for children and young people across a range of domains.
The rising number of drug-related deaths is a public health emergency in Scotland. The Scottish Government and other partners will take action to tackle the issues and harms associated with the use of illicit drugs.
To meet the increasing demands on our Health and Social Care system, the Scottish Government are also developing a new smarter booking system for use in the NHS. The new system is being developed as part of CivTech, the Scottish Government’s innovative technology acceleration programme, and will allow patients to make, change and cancel outpatient appointments online, as well as providing text message reminders. The smarter booking system will also help ensure patients are seen by the right person, in the right place, and at the right time, reducing unnecessary appointments. The Scottish Government will also implement the Digital Health and Care strategy, launched in 2018, to ensure that digital enhances the delivery of health and care services.
The recent increase in government funding and action to tackle poor Mental Health will require good evaluation to understand better what interventions have the biggest impact. One commitment in the Mental Health Strategy is to develop a mental health strategy data framework, recognising that good mental health is not the sole preserve of health services, or even public services. The mental health strategy data framework comprises two elements: a mental health quality indicator profile to illustrate the quality of services; and a mental health population framework to provide an accessible overview for those seeking to understand Scotland’s mental health and wellbeing at the population level. A full progress review of the Mental Health Strategy will be held in 2022 to ensure that lessons are learnt from actions to that point.
Commitments in the Scottish Government’s 2019-20 Programme for Government that relate to this Goal
- An investment of an additional £20 million over two years to test new approaches and improve services to tackle the number of lives lost to drugs in Scotland. The Scottish Government will also consult on drug law reform, setting out the changes we would want to make to the 1971 Misuse of Drugs Act in the event the UK Government agrees to devolve the powers in the Act
- Increase the number of people treated each year for Hepatitis C and work to eliminate it in Scotland by 2024 by getting the message out that anyone how has been at risk should take action
- Expand the current vitamins scheme in Scotland to include all children under 3, in addition to the current scheme which provides free vitamin D for breastfeeding mothers and children under a year old
- Establish Precision Medicine Alliance Scotland, focusing on conditions of major importance in Scotland, including those that disproportionally impact those affected by socio-economic disadvantage
- Create a new national body to strengthen infection prevention and control, which will have oversight for the design, construction and maintenance of major NHS infrastructure developments
- New legislation for drug-driving limits covering 17 different drug types, coming in to force in October 2019
- Introduce a no-smoking perimeter around hospital buildings and seek views on further restrictions on advertising of nicotine vapour products, to discourage non-smokers, children and young people from taking up vaping
- Bring forward a Bill on Restricting Foods Promotions for the promotion and marketing of food and drink high in fat, sugar or salt in next year’s legislative programme
Contact
Email: nationalperformance@gov.scot