The best start: maternity and neonatal care plan executive summary
Executive summary of the five-year forward plan for the improvement of maternity and neonatal services in Scotland.
The Best Start: A Five-Year Forward Plan for Maternity and Neonatal Care in Scotland - Executive Summary
The Case For Change
Maternity and neonatal care and services matter to the health and wellbeing of Scotland's people. The health, development, social, and economic consequences of childbirth and the early weeks of life are profound, and the impact, both positive and negative, is felt by individual families and communities as well as across the whole of society.
Scotland's maternity and neonatal services are generally providing high quality care, with high levels of satisfaction amongst women and families who use those services. However, services have largely developed over time, rather than being designed around the needs of women and families, leading to different approaches and care across Scotland. The birth rate in Scotland has been relatively static in recent years, with around 54,000 births in 2015; the changing needs of the population, however, mean that services will no longer be fit for the future.
Increasing levels of long-term conditions such as diabetes and obesity, and of mental health problems, need a pro-active response from the health services. Social problems have an important influence on pregnancy and birth, and social and health inequalities bring particular challenges for women, children and families from more deprived communities.
Within the context of wider change within NHSScotland, this Review offers a unique opportunity to place the current and future needs of women, babies and families, and person-centred, relationship-based care, at the heart of redesigned maternity and neonatal services.
There are important changes within the health service itself, and for the staff who provide care. There is a need for consistent quality improvement, to ensure that all women, babies and families receive equitable, high quality, safe and compassionate care.
Staff providing care need to continue to deliver high quality services in light of the changing workforce demographics and new evidence, and it is important that education and training keep pace with the workforce skills requirements.
The needs and expectations of women and their families are changing and we need to ensure that the right care is available and accessible when needed.
The current model
The overall framework for maternity and neonatal services is established at a national level. However, there is no single prescribed model of service delivery, and individual NHS Boards design services locally for their own population.
Maternity services are provided in all 14 NHS Territorial Boards, offering a range of midwife-led and obstetric- led care in both hospital and community settings. Over 97% of births take place in hospital. There has been a steady rise in interventions in labour and birth, largely from a rise in caesarean sections to 31.1% of all births in 2015, with significant variation in the rate across NHS Boards.
Neonatal services are provided from 15 neonatal units across Scotland. Outcomes and survival rates for all preterm and sick newborns have improved significantly over the last 20 years with enormous advances in newborn care. The majority of additional care provided to newborn infants is classified as high dependency or special care with only a small proportion requiring intensive care. However, for that small proportion, the complexity of neonatal intensive care has increased.
For many women and families, having a baby is a straightforward and joyful experience. For some women however, having a baby is a very difficult and challenging period in their lives and they will require additional support and care from a wider range of professionals and multiple agencies. The options for care for women and access to additional support is currently not consistent or equitable across Scotland.
The views of women and families and third sector organisations
In general, the quality of maternity care in Scotland is rated very highly by service users. Women have reported very positive experiences of their care and treatment. However, there are key elements of overall maternity care which are viewed as less positive. In particular, women and families have expressed a wish to see improvements in:
- continuity of care and carer, building relationships with staff and seeing the same person or team throughout their care, breastfeeding support, the opportunity for more partner support for bonding with their babies, and minimising separation.
- more information and choice, and better communication and consistent advice including the use of digital technology.
- better emotional support for families with babies in neonatal care, and care for bereaved parents.
- more access to services locally, and support for parents of babies in neonatal units to stay with their babies.
The views of staff
Staff described positive views and experiences, but also challenges in providing care in the current system. There were concerns about sustainability of current ways of working, the need for interdisciplinary education, training and working, skills for remote and rural working, and improved career pathways and role development. In particular:
- maternity staff described finding it hard to provide continuity of carer; risk pathways being too restrictive; challenges in offering women real choice; and concerns about rising rates of interventions in labour and birth.
- neonatal staff valued recent positive developments in regard to safety, communication, and family- centred care. They however reported that improvements were needed in facilities for parents to be with their babies, in information and communication, and in working across the system, especially in regard to transport and support for early discharge home.
- suggested solutions included shared communication and monitoring through electronic records and a national dataset, and the use of telemedicine.
The Review
This Strategic Review of Maternity and Neonatal Services in Scotland was announced by the Minister for Public Health in early 2015. Sitting within the context of the Scottish Government's Transformational Change Plan, the Review was requested to make recommendations for a Scottish model of care that contributes to the Scottish Government's overall aim of delivering person-centred, safe and effective care.
The focus of the Review was to create a refreshed model of care and approach to maternity and neonatal services and to examine choice, quality and the safety of those services in light of current evidence and best practice, in consultation with service users, the workforce and NHS Boards.
The Review group consisted of representatives from the key professional groups involved in managing and delivering maternity and neonatal services, representatives of the Scottish Government, staff side organisations, third sector representatives and academics working in maternal and infant health research. Working across four sub groups, the work of the Review group included:
Engagement with service users, staff and service providers across Scotland.
A systematic process to assess current evidence through the conduct of eight efficient reviews and summaries of current data.
Drawing on the findings of the engagement, the evidence reviews, and the knowledge, experience and insight of the Review group and sub group members to agree the new model of care for maternity and neonatal services.
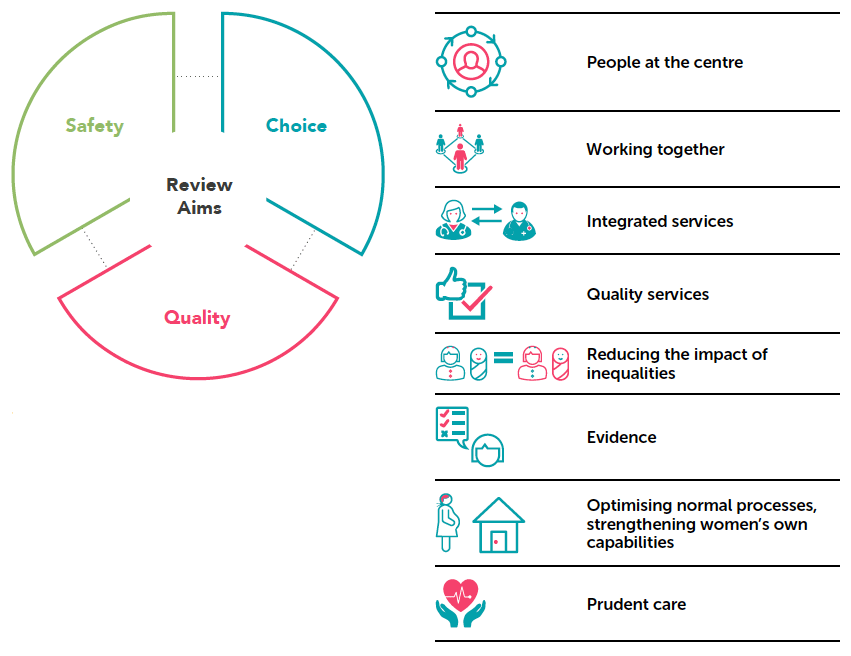
Underlying principles
The above underlying principles were agreed by the Review group to underpin all of their work and ensure a common approach:
Scope Of The Engagement Process
The overall engagement process included the following activities:

The New Model Of Care
The future vision of maternity and neonatal services across Scotland is one where:
- All mothers and babies are offered a truly family-centred, safe and compassionate approach to their care.
- Fathers, partners and other family members are actively encouraged and supported to become an integral part of all aspects of care.
- Women experience real continuity of care and carer across the whole maternity journey, with vulnerable families being offered any additional tailored support they may require.
- Services are redesigned using the best available evidence, to ensure optimal outcomes and sustainability, and maximise the opportunity to support normal birth processes and avoid unnecessary interventions.
- Staff are empathetic, skilled and well supported to deliver high quality, safe services, every time.
- Multi-professional team working is the norm within an open and honest team culture, with everyone's contribution being equally valued.
Key Recommendations
Continuity Of Carer
- All women will have continuity of midwifery carer from a primary midwife.
- Midwifery and obstetric teams will be aligned with a caseload of women and be co-located for the provision of community and hospital-based services.
- Specific details of the way in which continuity is managed will vary across settings (e.g. urban or rural) and population groups (e.g. women with particular social vulnerability). Different models of providing continuity should be audited and evaluated.
- The existing midwifery and obstetric workforce will be reconfigured to work in a way that supports continuity of carer for all women.
- Education and support for all staff will be needed to adapt to the new way of working.
- Early adopter NHS Boards should be identified to lead the change in practice.
Person-Centred Maternity And Neonatal Care
- Maternity and neonatal care should be co-designed with women and families from the outset, with information and evidence provided to allow her to make informed decisions in partnership with her family, her midwife and the wider care team as required.
- Services will regard mother and baby as one entity and truly put the mother, baby and family at the centre of service planning and delivery.
Accessible And Appropriate Local Services
- Integrated team care for women, babies and families will, over time, take place in local community 'hubs'.
- All women should have an appropriate level of choice in relation to place of birth and there are a number of choices that should be available to all women in Scotland including birth at home, birth in an alongside or freestanding midwifery unit, and hospital birth.
- Factors contributing to the rising caesarean section rate should be examined, from both the clinical and woman's perspective, and optimal levels of intervention that balance risk and potential harm should be identified and implemented.
- Babies with moderate additional care needs (for example late preterm) should, when possible, be cared for in postnatal wards.
- The provision of high quality postnatal care should be afforded a high priority.
- Achieving this new model of working will require considerable re-design of services, especially in the way that midwives work.
- Maternity and neonatal services should be organised so that units providing the most highly specialised care are co-located.
- Maternal and fetal medicine services for women with the most complex needs should be managed by a core group of experienced consultants at a regional or national level.
- All women, and in particular the most vulnerable, should be supported with compassion and support, and with advice and services to promote lifestyle changes during their pregnancy to improve their own health and the health of their baby.
- All NHS Boards should review their current access to perinatal mental health services to ensure early and equitable access is available to high quality services, with clear referral pathways.
- In every case where a family is bereaved, they should be offered access to appropriate bereavement support before they leave the unit, and each maternity and/or neonatal unit should have access to staff members trained in bereavement care.
Re-Designing Neonatal Care And Services
- Three to five neonatal intensive care units should be the immediate model for Scotland, progressing to three units within five years.
- A national Framework for Practice should be developed which outlines clear pathways for newborn care and also supports the development of consistent and equitable specialty paediatric and allied health professional outreach support for local neonatal units from larger units.
- A national level group should be established to develop National Frameworks for Practice for Scotland, which are evidence-based and describe minimum acceptable standards for newborn care.
- Workforce planning, role development, and high quality education, and training will be needed for all neonatal staff.
Supporting The Changes
- Transport services: The transport team must continue to be an integral part of the neonatal community, and effective communication and liaison between neonatal units and neonatal transfer teams should be routine.
- Remote and rural care: It is essential that all staff can access high quality education, training and support and rotation to larger units for skills maintenance.
- Telehealth and telemedicine: The enhanced use of telemedicine in maternity and neonatal care should be developed.
- Workforce planning: NHS Boards should undertake comprehensive workforce planning based on the new model.
- Education and training: Education and training capacity planning is needed to ensure staff are fully supported to deliver the new models of care.
- Quality improvement: National maternity and neonatal dashboards should be developed.
- Data and IT: A national data hub, integrated with Information Services Division, part of NHS National Services Scotland, should be developed to coordinate the collection and verification of all Scottish-related neonatal and maternity data.
- Electronic records: A Scottish electronic women's maternity record should be developed.
Wider Implications
- A single Maternity Network for Scotland should be developed, along with a single Neonatal Managed Clinical Network for Scotland.
- The implementation process should consider the phasing and prioritisation of the recommendations to ensure the implications of the considerable level of service change are managed appropriately.
- A systematic evaluation of the impact of the more significant recommendations should be undertaken.