Quality prescribing for chronic pain: guide for improvement 2026-2029
Chronic pain, defined as persistent pain lasting beyond three months, can significantly impact quality of life, affecting physical and mental wellbeing. This guide supports clinicians and people living with chronic pain, using a person-centred approach to pain management.
8. Non-pharmacological approaches to manage chronic pain
8.1 Introduction
Self-management is fundamental to improving an individual’s chronic pain experience. People’s preferences and choices should be explored, and clinicians should offer non-pharmacological resources and services to develop a personalised plan. Non-pharmacological approaches to pain management involve a wide range of lifestyle factors including activity, mental health, stress, sleep, social connection and nutrition. These methods can be used alone or to complement pharmacological management.
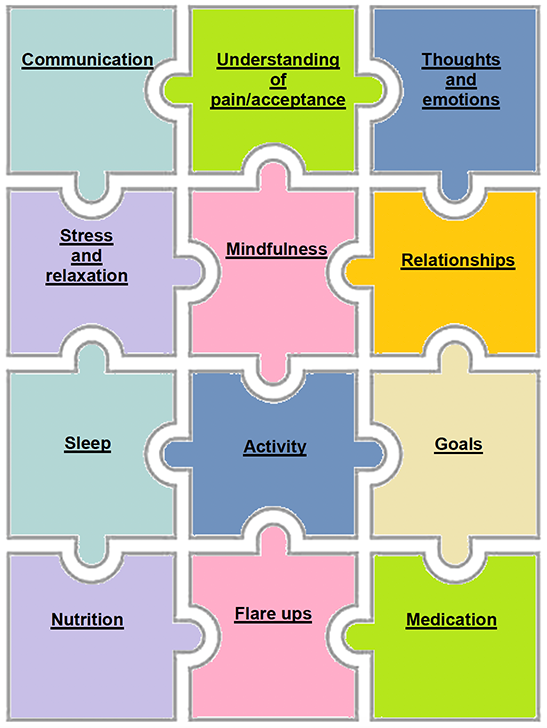
Chronic pain can affect every aspect of daily life. The pain management jigsaw (Figure 3) illustrates different approaches proven to be helpful in improving pain management.
8.2 Communication
Communication within a chronic pain consultation can be challenging.
Relationship between pain and communication
- Chronic pain can make communication difficult as an individual may find it challenging to express what they are feeling and the impact it has, e.g. less able to complete usual activities.
- Individuals can withdraw from communication, especially if they do not feel listened to.
- Communication can be challenging due to:
- limited time for appointments
- limitations of practitioner training in management of chronic pain
- varied consistency of advice (limitations of understanding of chronic pain due to evolving evidence)
- the experience of the individual that the impact of their pain has not been recognised
Potential strategies:
- See Chapter 7: Consultation conversations
- Use active listening to encourage behaviour change, demonstrate empathy and validate a person’s individual experience of pain.
- Schedule a longer appointment or make a specific appointment to address issues related to pain. Assessment and management are part of an ongoing relationship, and discussion may need to extend over several appointments.
- Use resources which help the individual to understand and express their situation so that they have the information and resources to be well-prepared for each appointment, such as use of PROMs.
Resources
- Helping others to understand chronic pain
- How to support a loved one with chronic pain
- What is chronic pain? course on TURAS
8.3 Understanding of pain - acceptance and empowerment
Acceptance enables the individual to acknowledge that pain exists in their life and that they can adapt and redefine what is now ‘normal’.
- Research indicates that greater acceptance of chronic pain is associated with better physical function, mental well-being, social function and overall quality of life[27]
- Pain acceptance involves the willingness to experience pain associated discomfort /distress and actively pursuing meaningful life activities despite the pain, thus enhancing quality of life and reducing suffering[28]
- Supporting individuals to understand their pain and the factors influencing it, can support pain willingness and activity engagement and help individuals manage their pain more effectively
Relationship between pain and understanding of pain and acceptance
- Acceptance of chronic pain can be difficult as individuals often require contemplation of a lifestyle/life plan different to one before a diagnosis of chronic pain.
- In the management of chronic disease in general, World Health Organisation (WHO) recognise four components of empowerment:
- Patient participation: involving people in their own care
- Patient knowledge: enhancing patients' understanding of their health and treatment options
- Patient skills: developing patients' ability to manage their health and make informed decisions
- Creating a facilitating environment: providing support and resources to enable people to take control of their health
Potential strategies:
- Support someone around acceptance of their pain condition to allow them to move forward and recover aspects of their life that matter to them.
- Support people to self-manage their condition and be empowered and supported. See HIS resource on Gathering views on chronic pain.
Resources:
8.4 Thoughts and Emotions
Living with chronic pain can be a challenging experience and very different to the experience of living with acute pain. Many people report feeling more pain when they are feeling down or more anxious or worried.
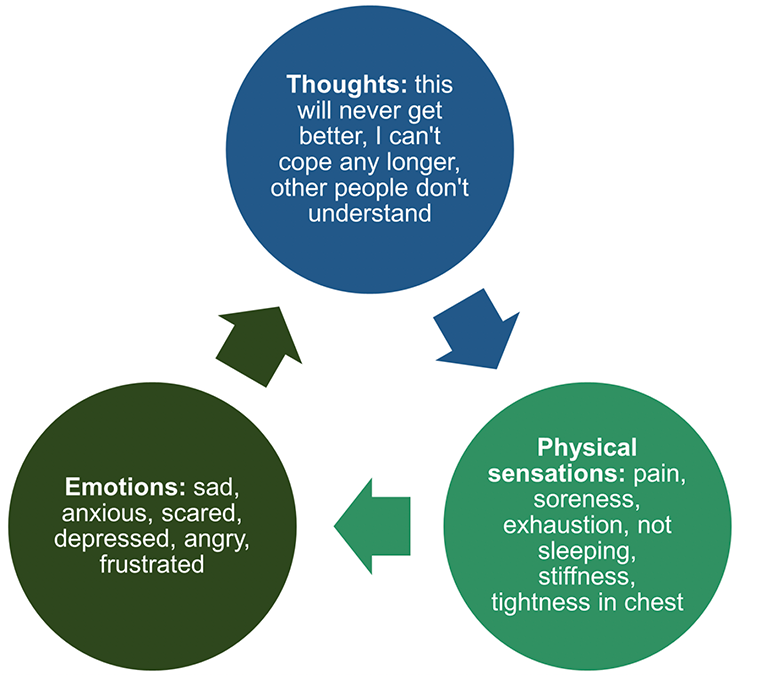
Relationship between pain, thoughts and emotions
- Pain and emotion are closely linked. It is almost impossible to have pain without there being an emotional impact.
- Recognising the emotional impact of chronic pain can be a first step towards being able to manage both pain and emotions better.
- Emotions people experience when they feel pain include: sadness, anxiety, frustration, anger, guilt, disappointment, shame, stress, a sense of loss.
- These emotions can affect how someone thinks and feels.
Potential strategies:
- Acknowledge that the experience of living with chronic pain is different from acute pain
- Acute pain:
- Medication relieves pain
- Short-term disruption to usual routine and activities
- May bring short-term frustration and stress
- Expectation of return to normal in weeks or months
- Family and friends often provide support
- Chronic pain:
- Limited benefit from medication
- Lasting changes to activities, routines and roles
- May feel low, exhausted, overwhelmed
- Likely to feel uncertain about the future, hopeless
- Family and friends may not understand and may become frustrated
- Acute pain:
- It is vital to spend time and actively listen to the whole person’s experience, with genuine warmth and empathy. This validates the individual’s experience
- Emotional reactions to pain (and other everyday life events) are normal and don’t necessarily mean that people are developing or have a mental health condition. Although normal, these reactions should be acknowledged and considered when we look to help those with chronic pain
- If able, it may be helpful for individuals to discuss their emotions with an appropriate clinician
- Consider other aspects of the pain management jigsaw which can support negative thoughts/emotions, e.g. activity, communication, social connection/relationships, mindfulness/relaxation
Resources:
- Chronic pain learning toolkit (practice level 2) on Turas
- Managing emotions with chronic pain
- Ten footsteps to living well with pain
- Discussing emotions can be challenging for both the individual and the clinician, and resources to support this include e-learning modules for clinicians:
- Emotion Matters e-learning module on Turas Learn which supports healthcare professionals to consider how to evaluate and assist with the emotional impact of a person's long-term condition, such as chronic pain.
- Building a shared understanding e-learning module on Turas Learn which helps develop cognitive behaviourally informed principles to help those with pain manage it effectively.
- Mental health improvement, and prevention of self-harm and suicide learning resources on Turas Learn can improve confidence and ability to support and signpost for the appropriate assistance.
Psychological therapies
Psychological therapies (cognitive behavioural therapy (CBT) and acceptance and commitment therapy (ACT) should be considered for adults experiencing chronic pain, depending on individual preference.[29] These should be delivered by appropriately trained professionals.[30]
All GP practices in Scotland can refer patients to Silvercloud CBT for chronic pain.
8.5 Stress and relaxation
Living with chronic pain can in itself be stressful. Stress and anxiety trigger our ‘fight or flight’ system. Pain is linked to this threat system.
Relationship between pain and stress
Activation of the fight or flight system releases hormones such as adrenaline and cortisol. These hormones increase the sensitivity of the nervous system and can amplify the perception of pain. Prolonged stress increases muscle tension which can further increases pain.
Relaxation techniques are a way of reversing the ‘fight or flight’ system and activating the body’s own relaxation, or ‘self-soothing’ system. Relaxation techniques are intended to help people to be more in control over their body’s response to stressful situations, thoughts or feelings and can be helpful in managing chronic pain.
Potential strategies:
- Consider relaxation techniques to support management of the interconnection between stress and pain
- Highlight to individuals that techniques, such as relaxation, may not change pain levels but can change the body’s response to pain and improve feelings of wellbeing
- Tailor interventions to individual needs and preferences
- Consistent practice is a critical factor in influencing effectiveness
- Consider other aspects of the pain management jigsaw which can support negative thoughts/emotions, e.g. activity, communication, social connection/relationships, mindfulness/relaxation
Examples of relaxation techniques include:
- Soothing Rhythm Breathing - is a breathing exercise which has been shown to promote calmness by activating the parasympathetic nervous system and increase the ability to self soothe
- Progressive Relaxation - when each muscle group is tensed, then relaxed progressively throughout the body
- Guided Imagery - guided imagery involves visualizing positive, peaceful setting like a beach or a meadow
Resources:
- Turas contains a module about how relaxation benefits people experiencing chronic pain: Chronic pain skilled (level 2): Non-pharmacological management
8.6 Mindfulness
Mindfulness in pain
- Mindfulness involves paying attention to our thoughts, feelings and bodily sensations so that we can become more aware of them, less enmeshed in them, and better able to manage them. Mindfulness skills allow people with pain to explore what they are actually experiencing and noticing physically in the present moment. It allows people to recognise feelings associated with their pain, with open, non-judgemental, kind and compassionate acceptance.
- Mindfulness can assist people’s understanding of self-management of pain, providing options beyond medication and additional wellbeing benefits, including stress, anxiety, insomnia and pain.[31]
- Mindfulness techniques are taught as a way of managing chronic pain, not eradicating pain.
- Consider offering Mindfulness based approaches to manage pain for individuals who express a preference for this.[32]
Resources:
- Self-directed courses are available, for example, Mindfulness for Health by Vidyamala Burch and Danny Penman
- A free app and resources are available to guide individuals with mindfulness Insight Timer — #1 Free Meditation App
Mindfulness and connection
A 54-year-old woman was referred for a chronic pain review by the community pharmacist. She expressed her frustration at the lack of pain control despite high doses of multiple pain medicines. She was diagnosed with fibromyalgia 11 years ago and has had depressive episodes. She was unemployed, rarely left her house, did minimal physical activity and lived with her teenager, with whom she had a difficult relationship.
The practice pharmacist reviewed her medication and suggested an initial plan for de-prescribing her opioids in a stepwise fashion. They recommended a ‘Mindfulness for pain’ small group course which was run online by a local pharmacist using NHS Near Me.
The mindfulness course was well received, with the individual able to acknowledge the contribution of emotional issues such as loneliness and relationship difficulties to her experience of chronic pain. She reported that she felt more in control of her pain after practicing mindful meditation regularly. Referral to the community link worker at the practice helped her identify volunteering opportunities which she subsequently took up, including a local food bank and a youth group.
Connection with others through mindfulness and volunteering has assisted with her ongoing management of chronic pain and successful de-prescribing of the majority of her opioids. The relationship with her teenager has improved and she is feeling much better and more hopeful. The community pharmacist still sees her regularly and noted that she now looks like a different person.
8.7 Relationships
People living with pain often report loss of social roles, family disruption and conflict at home and work.
Pain and relationships
- Living with chronic pain can be an isolating and lonely experience. People living with chronic pain consider improved social outcomes as a high priority
- Social support is associated with better pain outcomes and less emotional distress[33]
- To understand more about values based goals, access the Finding a way through resource on Turas
Potential strategies:
- Consider utilising local social prescribing and community resources to develop social networks and connections
- Signposting to online resources e.g. NHS Inform
- Discuss values-based goals using a “what matters to me” or Realistic Medicine approach
8.8 Sleep
Sleep is essential for maintenance of good health. Chronic poor sleep is associated with increased all-cause mortality, cardiovascular disease, diabetes, obesity, long term pain, depression and anxiety and is associated with reduced cognition.
Relationship between pain and sleep
- Sleep and pain are bi-directional, poor sleep affects pain and pain can disrupt sleep. Poor sleep is a greater predictor of pain than pain is of poor sleep[34]
- Between 67% and 88% of individuals with chronic pain experience sleep disruption and insomnia, and at least 50% of people with insomnia report chronic pain
- There is a dose dependent association between poor sleep and pain[35]
Potential strategies:
- Ask the individual about their sleep quality and sleep routine
- Consider CBT for insomnia as an effective management strategy:[36]
- Consider providing sleep hygiene advice and reassure individuals that changing sleep habits can take time so they should persist with the strategies:
CBT Insomnia (CBT-i): The Sleepio App is an app based on CBT-i. It is available free of charge to individuals in Scotland. Quick Guide for Accessing Sleepio - National Wellbeing Hub
8.9 Activity
Chronic pain can have a significant impact on activity levels as individuals may consider ongoing pain to be an indication of further injury or damage.
Relationship between pain and activity management
- Chronic pain can make some people fearful of “exercise” as they associate this with pain. The terms “movement” and “physical activity” are more supportive
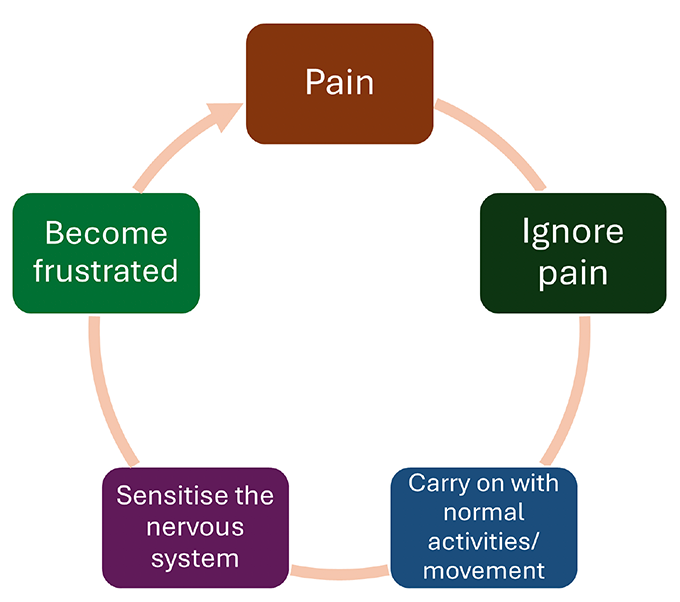
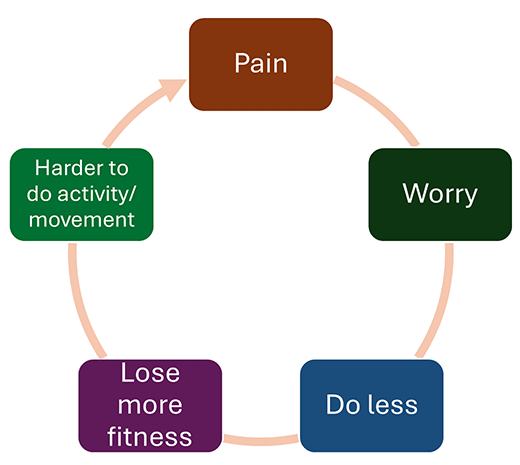
- Recognising unhelpful activity patterns such as ‘Boom and Bust’ (over and under activity) is a useful step in enabling individuals to adopt a more consistent approach to activity
Potential strategies:
- Tailor management approaches to the individual’s activity patterns, e.g. behavioural activation if underactive, pacing if overactive
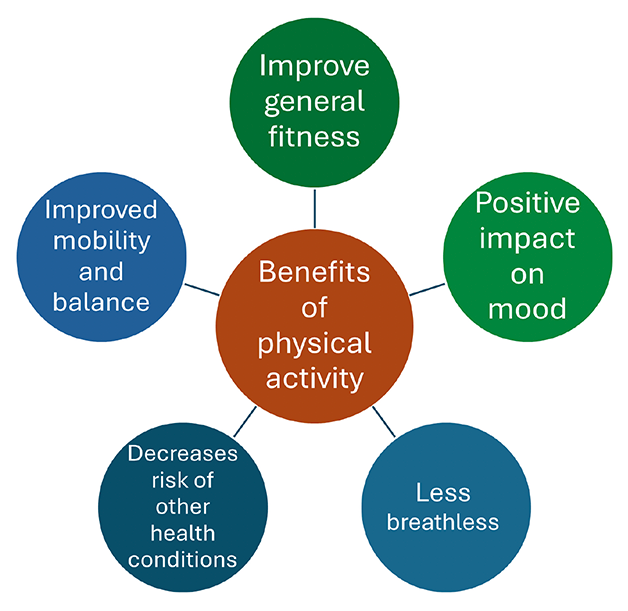
- Physical activity is a recommended treatment for people living with chronic pain. [37] The benefits of exercise are summarized in Figure 7 below
- Based on the individual’s needs, preferences and capabilities discuss possible activity interventions and choices regarding suitable activities[38]
- Activity management interventions delivered by psychologically-informed clinicians and underpinned by a values-based approach and pain science education may encourage greater activity engagement, improving person-centred outcomes
- The following approaches should be used to improve adherence to activity and exercise interventions:17
- supervised exercise sessions
- individualised exercises in group sessions
- addition of supplementary material
- provision of a combined group and home exercise programme
- Reassure the individual that pain can be thought of as a protective system rather than an indicator of damage
- Establishing barriers to activity or movement is important and addressing these will lead to improved outcomes
- Acknowledge it can take practice to regulate activity and find a balance between over and under activity
- Prioritise activity - prioritise what activities matter most
- Plan activity - plan what do and when. Consider the activity and what is required. Break up activity into manageable steps
- Proceed with activity - carry out the plan and be prepared to adapt it
- Acknowledge you might not be able to complete it as initially planned and have different options to fall back on
- Pacing can gradually help someone manage daily activities in a way that’s right for them, while reducing the risk of flare ups. Pacing can help because it allows someone to do things within their limits. This can help re-train the nervous system to be less protective
Resources:
- A video from Dr. Tim Williams on Pacing Skills: Developing patients' pacing skills - Live Well with Pain
- The Pain Toolkit includes lots of information about Chronic Pain. Within the ‘tools’ section there are further videos on pacing and rest
- A step by step guide to pacing and goal setting
- Arthritis UK has various information leaflets and links to exercise for people with arthritis
- Additional resource: Pacing from a lived experience perspective
8.10 Goals
Goals can help people living with chronic pain to regain the confidence to move towards doing more of their valued activities.
Relationship between pain and goals
- Goals provide milestones on the journey which can help with motivation and achievement
- Some people may struggle to set goals as they can initially be difficult to identify
Potential strategies:
- Person-centred: Goals need to be person-centred to be more effective and should be generated by the person working towards the goal
- Values based: Choose goals or targets related to what is important to the person
- SMART (IES): Specific, Measurable, Achievable, Realistic and Timed (Independent, Enjoyable/or Satisfying)
- Action: Goals should target an action rather than a result e.g. being fitter is a result, walking to the shop and back is an action
- Create an action plan: A series of goals put together to reach a longer term/ bigger goal
- Break down: Break down goals into achievable steps
- Easy start : Start with the easiest step
- Reward: Identify meaningful rewards that can be used
- Reassess : Regular reassessment of goals to modify when required to make more achievable or more of a challenge
Resources:
- Pain management and goal setting
- Setting goals and getting active - Live Well with Pain
- Pacing and Goal Setting - Pain Management - painHEALTH (uwa.edu.au)
- Healthtalk
- 12 Quick Tips for Setting Goals with Chronic Pain – Northern Pain Centre
Re-engaging with meaningful activity
Martin, a 50-year-old male, presented with widespread pain. He was prescribed liquid morphine, co-codamol and amitriptyline with limited benefit. A recent MRI scan of the whole spine and pelvis was normal for age. On assessment, he presented with significant health anxiety on a background of previous trauma. He was experiencing significant social stress including past bereavement, terminal illness within the family and job insecurity. Pain had a significant impact on quality of life, sleep and relationships with family and friends.
Discussion and guided reflection (through pain education) helped develop an understanding of the connection between current life experiences, stress, distress and heightened sensitivity of the pain system. This reduced the belief that pain meant injury to the body thus reducing health related anxiety.
Support focussed on activities that mattered to him, including time with his children and re-engaging in hobbies, in combination with pacing, self-care, sleep hygiene and relaxation.
To address the significant psychological distress and anxiety, an interdisciplinary team approach was implemented. A review of his case with the Psychological Therapies team, resulted in mental health support being tailored to his individual needs. Face-to-face sessions were arranged as he did not feel comfortable with group or telephone consultations. Third sector social support was also offered.
The outcome was that he re-engaged with valued activities and had greater understanding of the multifactorial nature of his pain. He was no longer seeking a medical diagnosis, and felt a significant reduction in health anxiety. Over time, he stopped his pain medication and engaged with mental health services.
Practitioner reflection:
In individuals experiencing nociplastic pain, who have high psychological distress or previous trauma and low support/resilience, then caution is advised when prescribing opioids and other dependence forming medications, due to the risk of tolerance, dependency and addiction.
8.11 Nutrition
A healthy diet, focusing on the quality and variety of foods eaten, ensures the body gets the essential nutrients it needs to function at its best.
Relationship between pain and nutrition:
- For people living with pain, nutrient-rich foods can support overall health and may also play a role in managing pain levels [39]
- Limited/reduced mobility and functional strength can affect a person’s ability to shop, cook and prepare meals
- Comfort eating and/or lack of meaning around mealtimes can lead to low quality diet
- Lack of sleep can result in irregular eating habits
Potential strategies:
- Consider providing advice for healthy eating
- Incorporate fruit and vegetables into the daily food intake to support overall health. These can be fresh, dried, tinned, or frozen as all offer nutritional benefits
- Include good quality fats in die such as omega-3 fats from oily fish, e.g. salmon or mackerel, to meals, or plant-based sources like walnuts, chia seeds, flax seeds or edamame. Extra virgin olive oil can be used for cooking and salad dressings
- Reduce ultra-processed foods which are typically high in salt, sugar and saturated fat. Try to cut back on highly processed foods like chips, sugary snacks, fast food and ready meals
- Include plenty of fibre in diet - fibre keeps the digestive system healthy and supports gut health. Fibre helps to prevent constipation which is a common side effect of medicines commonly prescribed for pain, including opioids. Increase fibre intake by consuming more vegetables, wholegrain options and legumes such as lentils, beans and pulses
- Stay hydrated - dehydration can cause constipation, and affect wound healing. Aim for six to eight glasses of water a day, and try to drink regularly, not just when feeling thirsty
- There is insufficient evidence of benefit from dietary supplements in chronic pain, such as vitamin D, glucosamine or chondroitin17,[40]
Resources:
- Nutrition and Chronic Pain - International Association for the Study of Pain (IASP)
- Nutrition and pain - Live Well with Pain
8.12 Flare-ups
A flare up is a temporary increase in pain intensity. They can last a few days, weeks or sometimes longer.
Relationship between pain and flare-ups
- Flare-ups can occur without warning, often with no set pattern and can feel worrying, overwhelming and difficult to cope with
- They are temporary, and it may not always be possible to identify the cause
- They are a common experience in persistent pain and are multifactorial, often due to changes in sensitivity of the nervous system and not necessarily an indication that things are getting worse
Potential strategies:
- Each of the non-pharmacological management strategies may be utilised to reduce the impact of a flare up and promote recovery.
- Personalise advice / strategies to determine the most appropriate approach for the individual.
- Provide flare up top tips:
- Actively listen and validate the individual’s experience.
- Provide reassurance that flare-ups are common, manageable and will settle.
- Encourage the individual to be prepared. Creating a flare-up plan when pain levels are manageable can help build confidence at times when pain is more severe.
- Encourage movement, activity and rest.
- Increases in pain may increase fear and avoidance of movement so reduce levels of activity. However, maintain gentle movement during a flare up and gradually return to usual activities as pain subsides.
- Support self-care and self-kindness.
- Make space and time for things that they find relaxing, provide enjoyment and happiness.
- Consider use of relaxation or mindfulness.
Encourage as much independence as possible (e.g. dressing, getting food shopping), but encourage the individual to seek support or help if needed.
Consider thoughts and emotions: Flare ups often generate negative or unhelpful thoughts. Feeling low, anxious, frustrated and overwhelmed are common. Helpful strategies in managing thoughts and emotions can be found in the links below and in our section on Thoughts and Emotions.
Resources:
- NHS Inform: Coping with a flare up of chronic pain
- Livewell with pain
- https://livewellwithpain.co.uk/practitioner-resources/10-footsteps/managing-setbacks/Recovering from a persistent pain 'flare' - Living Well with Pain
- Pain Toolkit
8.13 Medication
Please see Chapter 9: Benefits and limitations of treatment with medication
8.14 Group consultations for chronic pain
Group consultations are a way to bring together individuals for support with long-term conditions, helping them to better manage their own health and share their experiences and learning.
Peer support interventions should be considered as part of the holistic and individualised management for people with chronic pain. [41]
While a traditional medical consultation is approximately 10 minutes, group consultations can run for around 90 minutes and allow up to 12 participants to spend more time with their healthcare team – and each other. The sessions are generally led by a facilitator, who could be any member of the practice team, with medical or therapeutic input from the appropriate clinicians or allied health professionals.
They foster a sense of community between the individual and their care team, allowing everyone to learn from each other in a safe and secure setting.
Why would group consultations be suitable for chronic pain?
- Short consultations often lead to short term solutions such as firefighting, ineffective medications and inappropriate polypharmacy.
- Group consultations allow more time with individuals which can create the space to:
- Validate their experience
- Give people time to feel heard
- Participants share their experiences and feel less alone
- Deliver pain neuroscience education
- Group consultations consider the whole person including non-pharmacological options.
- Allocate time to share techniques that can improve their experience of pain including breathing techniques, mindfulness and safe movement.
| Our recommendations | Strength of recommendation |
|---|---|
| Explore people’s preferences and choices for self-management, due to the importance of this in managing chronic pain | Good Practice Point |
| Clinicians should offer non-pharmacological resources and services to develop a personalised plan, which may include pharmacological management | Good Practice Point |
| Physical activity should be advised as a recommended treatment for people living with chronic pain | Strong |
|
The following approaches should be used to improve adherence to activity and exercise interventions:
|
Strong |
| Consider CBT for insomnia as an effective management strategy36 | Good Practice Point |
| Consider providing sleep hygiene advice and reminding individuals that changes in sleep habits can take time to develop | Good Practice Point |
| Support person-centred goals in management of chronic pain which are specific, measurable, achievable, realistic and timed (SMART) | Good Practice Point |
| Consider providing advice for healthy eating and hydration39 | Good Practice Point |
| Psychological therapies (cognitive behavioural therapy (CBT) and acceptance and commitment therapy (ACT) should be considered for adults experiencing chronic pain, depending on individual preference.29 These should be delivered by appropriately trained professionals30 | Strong |
| Consider offering Mindfulness based approaches to manage pain for individuals who express a preference for this32 | Strong |
| Peer support interventions should be considered as part of the holistic and individualised management for people with chronic pain41 | Strong |
| Consider utilising local social prescribing and community resources to develop social networks and connections | Good Practice Point |
Contact
Email: EPandT@gov.scot