Quality prescribing for chronic pain: guide for improvement 2026-2029
Chronic pain, defined as persistent pain lasting beyond three months, can significantly impact quality of life, affecting physical and mental wellbeing. This guide supports clinicians and people living with chronic pain, using a person-centred approach to pain management.
21. Appendix H: Data to drive change in chronic pain
This section aims to introduce the relevant data sources and tools used in prescribing for polypharmacy and how these can be used to drive improvements in individual care.
Healthcare delivery produces a large amount of data which can be used to identify areas of unwarranted variation and drive improvements in healthcare at an individual and organisational level.
Understanding this data and how these systems and tools interact can be challenging, especially where care of the individual is the key. However, tools for aggregate data visualisation, benchmarking and patient identification are available from a number of different sources. Figure 9 below outlines how data can be gathered from a range of sources and used to improve individual care.
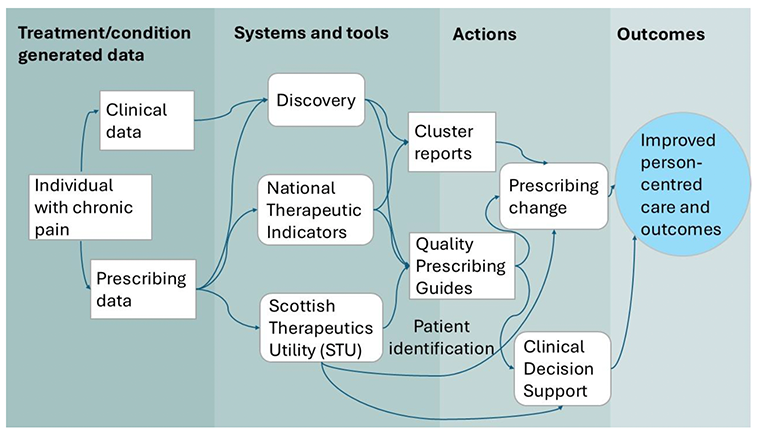
The tables below outline the systems and resources available to monitor and utilise data, and how to use them.
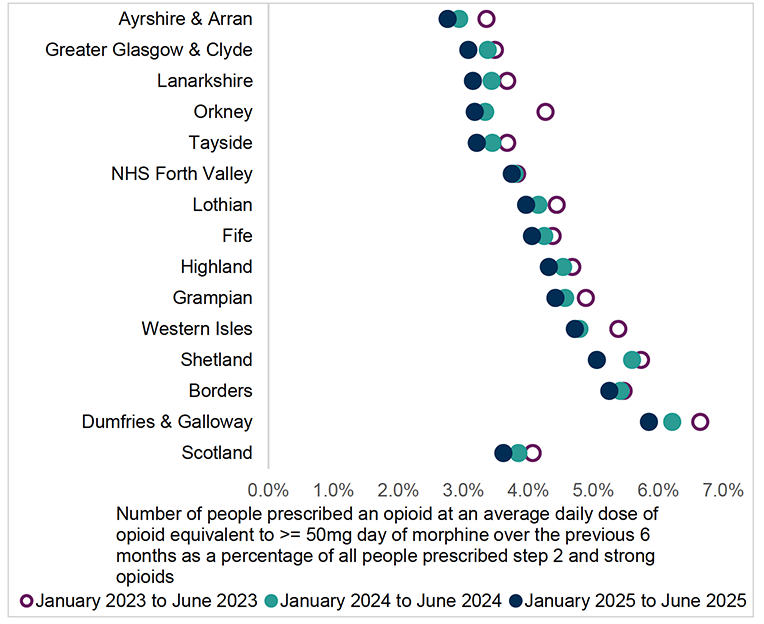
| System/resource | National Therapeutic Indicators (NTIs) |
|---|---|
| What is it? |
An indicator of clinical practice. National Therapeutic Indicators (NTIs), use prescription data to provide a measure of prescribing activity in specified therapeutic areas for comparison across NHS Boards, Health and Social Care Partnerships (HSCPs), GP clusters and GP practices. |
| Who can access/ use? | National Therapeutic Indicators are online with open access to anyone. |
| Why? What for? |
NTIs benchmark prescribing across set parameters (usually defined by expert working groups to identify areas for improvement within a particular area). Data is presented in a variety of ways. Examining variation over time can indicate where improvements in prescribing can be made. Indicator detail provides further detail and suggested actions. A new dashboard view is also available, providing additional context such as demographics and prevalence. |
| System/resource | Scottish Therapeutics Utility (STU) |
|---|---|
| What is it? |
A system to identify individuals in general practice, according to a set of pre-defined parameters, such as prescribing and clinical data (including read coding). STU focuses on identifying people to improve prescribing practice and improve medication safety. |
| Who can access/use? |
GP practice staff only. |
| Why? What for? |
STU was developed to improve safety, optimise efficiency and reduce avoidable waste (processes and costs), particularly in relation to repeat prescribing. The utility allows users to interrogate their prescribing data in real time and provides graphs to identify trends in repeat prescribing. STU includes reports which identify areas of high-risk prescribing. This supports clinicians in reviewing individuals at risk to determine if prescribing is necessary and how the risk can be reduced. |
Example
The polypharmacy indicators (developed from the NTIs and prescribing guide) highlight the number of people in each indicator. From each indicator title, the names of individuals are shown and their precribing record summarised below. STU has the facility to open the patient record to allow changes directly in EMIS or Vision.
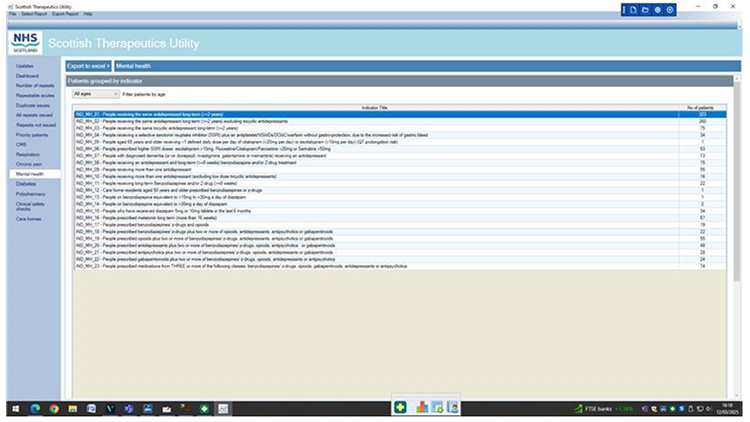
| System/resource | Discovery |
|---|---|
| What is it? | Discovery is an information system that provides approved users from the Scottish Government, health boards, local authorities and Health & Social Care Partnerships with access to a range of comparative healthcare information to support performance and quality improvement across Health & Social Care in Scotland. There is a prescribing dashboard, including measures including: Polypharmacy, Primary and Secondary Care Expenditure and Secondary Care Use of Medicines (HMUD). |
| Who can access/use? | NHS Staff (including Board staff, GPs), Public Health Scotland (PHS) and Scottish Government. There are different security levels. Level 1 allows access to Board level data. Level 2 allows access to general practice level data. |
| Why? What for? | Discovery provides comparative and benchmarking information to underpin service planning and delivery. |
Example
The example below is from the Polypharmacy dashboard:
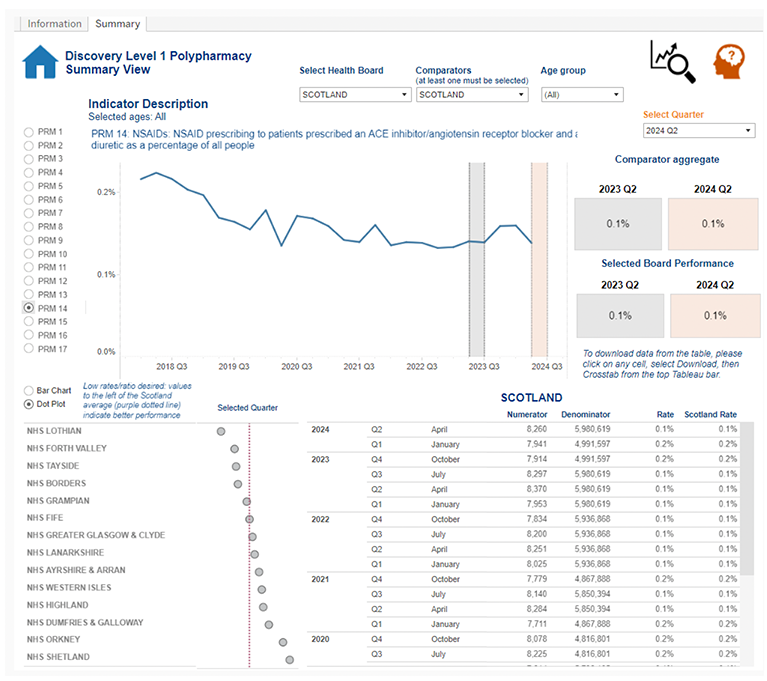
Contact
Email: EPandT@gov.scot