Practising Realistic Medicine: Chief Medical Officer for Scotland annual report
The Chief Medical Officer's third annual report on applying the personalised, patient-centred realistic medicine approach across Scotland.
Chapter 2 - Changing Our Style To Shared Decision Making
Making Shared Decision making the Norm –
Where are we now?
For shared decision making to take place, there needs to be a trusting partnership between professionals and patients, where both feel able to share their understanding and expertise and together, aim to reach an agreed goal. Shared decision making achieves its potential only if healthcare professionals make collaborative decisions with patients and their families. In order to achieve this, we must encourage openness and ensure that patients and families understand this will not diminish the quality of the care they receive. Crucially, this means routinely talking about people’s preferences, values and needs.
Many clinicians are keen to practise Realistic Medicine but are unsure how to go about sharing decisions. Often clinicians feel that they are doing this very well already and many do so, to a high standard. But we also know we have some way to go before shared decision making is a part of everyday practice. Achieving this is integral to what has become a shared vision for Realistic Medicine.
The Vision: By 2025, everyone who provides healthcare in Scotland will demonstrate their professionalism through the approaches, behaviours and attitudes of Realistic Medicine.
Consultation time
The Citizens Panel results show that the public greatly values a doctor who listens. However, there is evidence that the balance of a clinical conversation involves the clinician talking far more than the patient. A study demonstrated that patients were observed to speak for only 24% of the time; they asked an average of just 5.6 questions which took up 0.07% of the total consultation time. Yet physicians spoke for 44% of the consultation time, only 5% of which was spent answering patient questions. [6]
Care Opinion
Care Opinion is the UK’s leading independent feedback platform for health and social care services. Like Care Opinion, we want people to be able to share their experiences of health and care in ways which are safe, simple, and lead to learning and change.
Care Opinion is about honest and meaningful conversations between people and health and social care services. It now has more than 11,000 stories about care experiences in Scotland.
The following is a snapshot of Care Opinion’s interactive “tag-bubble” visualisation which is available at https://www.careopinion.org.uk/vis/naz7x:
Figure 2. Care Opinion “Tag Bubble”

By accessing the link and clicking on the various bubbles it will tell you how many positive and negative stories have been received from the public about that theme, and the actual stories will appear. During the period September 2017 to March 2018, a total of 1698 stories were posted on Care Opinion. 68% of these stories were positive and 32% were negative. However, drilling down more deeply, 272 of these stories were tagged with “communication”; “information” or “involved”. Of these 272 stories, 61% of these stories were negative and 39% positive. The opposite of the overall picture. Specifically, there were 88 positive stories about communication and 142 negative stories.
Communication is consistently the most negative theme on Care Opinion and within the stories about communication, “information” is the most frequent negative theme.
It may be that as clinicians we think we are engaging in shared decision making more than we truly are and there are lessons for us all on how to do better.
The Imbalance of Information
The gradient of power and knowledge imbalance between patients and clinicians needs to be recognised and its implications understood. Often the choices are not straightforward. When people are making decisions about treatment options with a serious condition, they may be frightened and vulnerable; at the time they may seek to be guided by the doctor. It is afterwards that they may question the merits of the treatment decision or experience regret, if their expectations are not met.
Tessa Richards has written in a recent article published by the BMJ about her experience of being treated for cancer:
‘The options here are seldom easy, of course, and no one forces patients to embark on chemotherapy, aggressive or otherwise. Indeed, oncologists argue that patient pressure is what makes them prescribe – an apology I don’t find wholly convincing. Patients may be desperate for “magic bullets”, but they still take doctors’ advice seriously. It’s a professional responsibility to present people with uncomfortable truths, to be transparent about the limitations of the evidence and how “effectiveness” of cancer treatments is judged, and to be objective about information on risks, harms and benefits.’ [7]
How can we give people the best chance of participating in shared decision making?
Many clinicians will have been faced with “oh you choose, doctor” and sometimes patients may feel they must please their doctor, because they worry their care may suffer. It’s vital that professionals do not underestimate the value and skill of working with patients to understand what fits for them and empowering them to make their own choices based on what is most important to them.
Good Communication
Good communication is at the heart of effective health care, yet it is complex and is based on deeply rooted patterns of behaviour. Effective communication skills lead to improved patient safety, symptom resolution and improvements in functional and psychological status. [8,9] We know that patients express more satisfaction during consultations where they have been able to express their perspective and objectives – what matters most to them. In doing so they are able to achieve a greater degree of shared decision making. [10,11,12] Not only are people more likely to have greater confidence in reaching decisions through this person centred approach, but there is evidence that adherence to treatment is improved as well as patients experiencing less regret about treatment choices.
A key part of shared decision making is honesty and realism about possible outcomes; recognising the benefits but also the risks and limitations of treatment in the context of the patients’ life and what matters most to them.
We know that people want to be more involved in decisions about their care, yet they may not know what to ask, or feel that they don’t have “permission” to participate in the decision making process. Building and maintaining trust is paramount. Without trust, people may not disclose all relevant information or follow clinical advice. We must move away from the “Doctor knows best” culture and generate supportive environments where people truly feel comfortable asking questions about their care, and can expect to get clear answers.
Health Literacy
Health Literacy is an issue in Scotland as it is across the world and can be a sometimes overlooked barrier to having meaningful conversations. We want Scotland to be a health literate society which enables all of us to have sufficient confidence, knowledge, understanding and skills to live well, on our own terms, with any health condition we may have. Professor Richard Osborne, the Director of the WHO Collaborative Centre for Health Literacy, gave this definition of health literacy.
A person’s health literacy is their current combination of health knowledge (including general concepts and specific knowledge), beliefs and skills that have developed through life experiences including education, illnesses, interacting with health services and interacting with their families and communities.
Professor Osborne has noted Scotland’s mission to make healthcare easier to access as an exemplar for other countries. He has said that while very few countries have a specific health literacy policy, those that do generally seek to raise the health literacy of the population so that they are able to engage in prevention and self-care more effectively. Scotland has this focus too, but avoids a deficit approach, and seeks to make the system fairer, adjusting the complexity and barriers such that all people living in Scotland can have a fair go. He describes this approach as critical, noting the deficit approach to health literacy will continue to promote and deepen health inequalities.
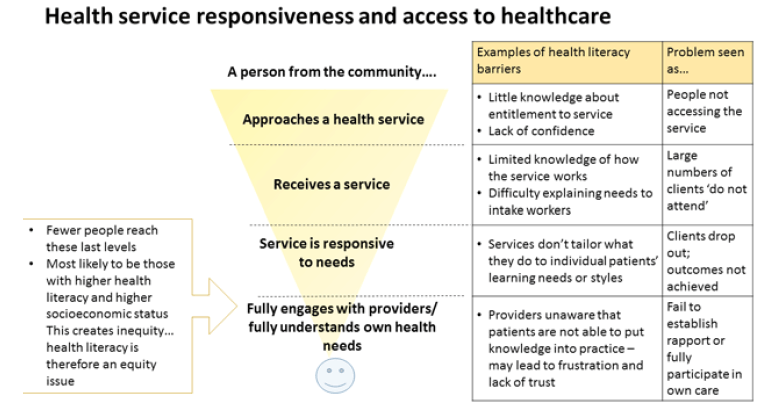
Professor Osborne kindly provided this image ( Fig.3) which helps to demonstrate the importance of adapting services to ensure people are able to engage effectively.
Realising Realistic Medicine identified the work on health literacy in Scotland, through the Making it Easy action plan, as a key element in creating the conditions for the delivery of Realistic Medicine. It set out our ambition for Scotland to be a health literate society that enables people to have the confidence, knowledge, understanding and skills to maintain good health.
Figure 3. Health literacy: applying current concepts to improve health services and reduce health inequalities. [13]
Making it Easier
A new action plan Making it Easier, a health literacy action plan for Scotland for 2017-2025, was published in November 2017. It focusses on sharing the learning which has occurred so far and embedding this in policy and practice. It also aims to develop more health literacy responsive organisations and communities and design supports and services which are better able to meet people’s health literacy needs.

A key element of Health Literacy is the co-production of services between clinicians and patients. Throughout Scotland, forward thinking clinicians and patient groups have already been adopting some of these philosophies and engaging in quality improvement projects which are co-produced by clinicians, patients and carers. One such example is the Helping Us Grow Group ( HUGG) in the Neonatal Unit, of the Royal Hospital for Children, Glasgow.
We are also keen to learn from successful approaches which have been developed elsewhere. The Ophelia ( OPtimise HEalth LIteracy and Access) process was developed in Australia. This was trialled by the Health Foundation in the UK among recent immigrants and people with COPD and is being applied in several other countries. The project resulted in a wide range of positive and innovative impacts: citizens were empowered, and at times even thrilled to contribute, and frontline practitioners also felt genuinely respected and efficiently shared their local wisdom.
The new Health and Social Care Standards feature in Making it Easier, the Health Literacy Action Plan. The standards promote involvement and shared decision making for everyone who experiences health and social cares services. Health and Care Professionals need to reflect on how we can make this a reality.
On the Health Literacy Place website, you can find some excellent examples of work, tools and techniques which can be helpful in improving health literacy. We encourage you to consider whether there are projects in the Health Literacy Place that might inspire you to start up your own health literacy project.
Asking the Right Questions Matters
Question prompt sheets are effective and inexpensive interventions used in cancer care, enabling patients to become more involved in medical consultations. [14] Increases in question asking have been associated with significant increases in patient satisfaction. [15]
In Realising Realistic Medicine, we highlighted that some NHS Boards are encouraging people to ask their clinicians 5 questions, to help them make informed choices about their care.
Asking the Right Questions Matters
To help ensure you have all the information you need to make the right decisions about your care, please ask your doctor or nurse:
- Is this test, treatment or procedure really needed?
- What are the potential benefits and risks?
- What are the possible side effects?
- Are there simpler, safer or alternative treatment options?
- What would happen if I did nothing?

NHS Borders, Lanarkshire, Forth Valley, Borders and Dumfries and Galloway are all piloting the 5 questions and we encourage the remaining Boards to follow suit.
Evaluation of the 5 questions approach is under way so that we can understand their impact on patient care and determine how useful they are.
“The questions were great, really explained everything to me the staff were super helpful, they are fine examples of the caring professions.“
Patient, NHS Forth Valley
Helping Us Grow Group ( HUGG), Royal Hospital For Children, Glasgow.
The Helping Us Grow Group ( HUGG) is a unique inclusive collaboration of families and staff in the neonatal unit. Our aim is to support parents to be primary caregivers for their baby, no matter how sick, in partnership with clinical staff. This is our model of Family Integrated Care ( FIC). Two key elements of our work are education for families and encouraging peer-to-peer support.
Inspired by other leading FIC centres, and motivated by feedback from families in our unit, we organised a programme of innovative daily Family Awareness Sessions ( Figure 4). These are held most days from 2-3pm for all families in the neonatal unit and aim to give parents skills and knowledge to care for their baby, as well as an important to meet and support each other. Topics are requested by parents and sessions are led by staff of all backgrounds including staff nurses, nursery nurses, neonatal doctors, pharmacists, dieticians and psychologists. “Veteran” parents, both mothers and fathers, also return to lead sessions and share their experiences
Figure 4. HUGG Family Awareness Session

Family feedback is extremely positive. Parents tell us they feel more confident, have improved understanding of their baby’s condition and care, and are forming strong and long-lasting friendships.
These sessions are organised by a fantastic group of staff nurses, working above and beyond their normal clinical duties. HUGG has empowered them to lead change and improve care for our patients.
In order to foster collaboration we also developed a simple but effective innovation; shared whiteboards at each cot-space. Families are able to leave messages for staff, including when they can be present to care, which care they want to be involved in and their baby’s likes and dislikes. Staff, especially those on nightshift, write updates and messages of support, including translations for non-english speaking families. Parents are delighted to know that staff are listening. These simple white-boards have created a new relationship with staff, as one parent wrote “thank you for being a voice for my baby”.
Another innovation was inspired by a father in the neonatal unit. He told us that he used video messaging for his clients, and asked if we could send him a video of his baby. Working with an industry partner, IT and governance teams we developed and piloted a secure video-messaging system in the neonatal unit in March 2017. Staff create short, friendly video updates for parents when they cannot be with their baby ( Figure 5).
Figure 5. HUGG Video Messaging

The positive impact of this innovation has far exceeded all of our expectations. Parents tell us they feel reassured, less anxious and sleep better. They feel a deeper trust and connection to staff who took the time to make and send the video message of their baby. With the support of grateful families we are now spreading our system to over 60 neonatal units throughout the UK, and to other clinical areas in our organisation.
www.vcreate.tv/secure-video-messagingRealistic Medicine flash card
In order to help clinicians and patients have more meaningful conversations about their care options, we’ve produced Realistic Medicine flash cards. We hope that they will help professionals to further spread awareness of Realistic Medicine and the importance of shared decision making. The 5 Questions will be printed on the flash cards and we very much hope they will support meaningful discussions on ward rounds, in consultations and clinics and as part of clinical supervision. We also hope that you will encourage patients to promote the use of the 5 questions among their families, friends and care providers, as well as aiding you during your clinical encounters.
We plan to distribute the flash cards through our Realistic Medicine Clinical Leads and at events across Scotland.
Decision Aids
For clinicians, working in pressurised and busy clinical settings, it may be difficult to know how much people want to know about their treatment options, compounded by limited access to decision aids that are up to date and relevant. While professionals will be used to engaging in discussions about informed consent, going a step further by asking about the person’s perspective, health beliefs and preferences is a highly skilled interaction. Talking about risk in the context of treatments is complex and requires careful explanation to avoid misinterpretation.
Figure 6. Three Talk Model of shared decision making
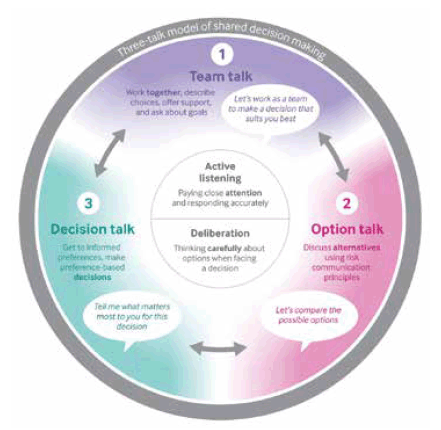
Although shared decision tools are available, these are not often used in routine clinical practice. Decision tools are best used within the consultation as a way of enabling the discussion about choices and options. There are a growing range of up to date decision aids for different conditions, available from the National Institute for Health and Care Excellence ( NICE) website, or Right Care ( https://www.england.nhs.uk/rightcare/shared-decision making/). There is not a tool for every condition and tools are not a substitute for a meaningful discussion.
Consultation Skills Training And Models
Experiential training over just one day is enough to help professionals develop consultation skills that are more patient centred. [16,17] As was demonstrated in the MAGIC programme supported by the Health Foundation, “Skills trump tools and attitudes trump skills.”
To help embed shared decision making in clinical practice, clinicians can be aided by a model that plans the conversation in stages 1) treatment choices 2) “trade-offs” and 3) decisions, taking into account the persons individual goals and preferences. Glyn Elwyn and others [18] have recently published the “three talk model” which can be used to facilitate shared decision making. The flexibility of this model recognises the different levels of participation and support that people may want to have in the decision making process.
More ways of supporting Shared Decision making
We must encourage people to take a pro-active approach to making decisions about their care. This could involve providing them with access to shared decision making aids,facilitating audio recordings of their consultations, and encouraging them to view online videos about treatment choices. All of these methods can and do help people make realistic decisions about their care that are right for them and help them recognise the limitations, but also benefits of the options available to them.
Shared Decision Making And Incapacity
In some instances a person’s ability to make decisions about aspects of their care may be impaired. It is essential that all clinicians understand how to assess capacity and use opportunities to maximise a person’s ability to make decisions wherever possible. Information on how to assess capacity is available on the GMC website.
Sometimes a person will lack the capacity to make a particular decision and clinicians should be aware how to use the legislation which exists to protect the person’s rights and provide safeguards. ( Adults with Incapacity (Scotland) Act 2000 and via the Mental Welfare Commission).
Shared decision making remains relevant in this group of people and may require enquiry into what a person’s views were in the past, discussion with relatives or carers and anyone advocating on their behalf.
Conclusion
Shared decision making must become embedded in routine clinical practice. The evidence we have discussed in this chapter suggests that while many professionals practice shared decision making, we can do better. It is the key to strengthening relationships between professionals and individuals, and to reducing unnecessary harm and regret caused by inappropriate or unwanted treatments.
Professionals working in the NHS today are working in challenging environments and making changes to the way we work can be difficult. Nevertheless, we must adapt the way we deliver care to ensure that we are empowering and enabling patients to be in control of their own health and health care. Let’s not underestimate the importance of being human; sometimes offering a supportive hand and displaying empathy will give people the courage they need to decide what is best for them.
We hope that some of the methods, tools and case studies highlighted in this chapter will support and encourage your work in partnership with patients to deliver care that people really value.