Practising Realistic Medicine: Chief Medical Officer for Scotland annual report
The Chief Medical Officer's third annual report on applying the personalised, patient-centred realistic medicine approach across Scotland.
Chapter 7 - A Realistic Approach To Population Health
Figure 11. Social determinants of health

Can we use Realistic Medicine principles
to influence the wider determinants
of health?
Health is more than just an absence of illness: it’s a resource that enables us to live lives we have reason to value. [51] That will mean something unique to each of us, whether an older person keeping active and mobile so they can continue to visit friends and family, a new mother supported to return to work after post-natal depression, or a child growing up in an environment that allows them to flourish and reach their full potential.
To realise this for the Scottish population, we need to think broadly about the factors which shape our health. These range from the individual, to the local, to the national, to the international, and are sometimes referred to as the wider, or social determinants of health. [52]
Everyday obstacles to a healthy diet
“I want to feed my family a healthy diet, but rising food costs prevent me from doing so. I can buy 20 sausage rolls for the price of one melon; or five packets of biscuits for the price of a loaf of bread.
The unseen costs of cooking meals are also a barrier I face. I have a prepayment meter. It costs me £4.00 to cook a chicken in the oven, so instead I opt for unhealthy ready meal chicken dinners, which only cost 12p to cook in a microwave.”
Extract from ‘Poverty in Scotland’ (2015), Poverty Truth Commission and Scottish Government [53]
To truly improve health and reduce inequalities, we therefore need not only to provide high quality healthcare but to address the societal, economic, cultural, commercial, and environmental context in which we live.
The potential rewards of doing so are enormous:
- The recent Scottish Burden of Disease study found that if everyone in Scotland enjoyed the same level of health as the most affluent group, we would be one of the healthiest countries in Europe. [54]
- What’s good for health and wellbeing often has many other societal benefits. For instance, increasing active travel through better infrastructure and investment can not only increase rates of physical activity but reduce congestion, noise, and environmental pollution. [55]
- In the context of growing demands and costs, acting on these wider determinants is essential to the sustainability of our healthcare system in the decades to come. A recent review found that on average, every £1 invested in public health interventions provides £14 of return. [56]
Just like good healthcare, good population health therefore requires a whole system approach. As health and care professionals, we have a crucial role to play in each part of that system – and in Scotland we have unrivalled opportunities to do so.
We can build on a strong tradition of pioneering public health initiatives to seize new opportunities created by health and social care integration and by legislation on community empowerment. We have a dedicated workforce of frontline health and care staff, many of whom have expertise in quality improvement, and world class health data which is increasingly being integrated with data from other areas of society. Finally, we’re a perfect size for innovation. [57]
Following a review of public health in 2015, the Scottish Government has committed to specific actions to improve the health of the nation: to improve local public health partnerships, including reforming how the NHS and local government collaborate on improving health; establishing a national public health body to strengthen the leadership and voice for public health in Scotland; and setting out clear priorities for action across the whole system, recognising the roles that multiple partners must play. The core theme running through the whole reform is that we must work collaboratively to achieve change. The major levers for health improvement in Scotland lie outside the health service, and they are best tackled in partnership with others. This section therefore asks how, as health professionals, we can apply the principles of Realistic Medicine to ensure everyone in Scotland has an equal chance of a long and healthy life and how we might work in partnership with others to best reduce the burden of avoidable ill health that we see daily in our services.
How can we reduce harm and waste by embedding prevention in our clinical culture in a way that is responsive to the social determinants of health?
Too often, clinical staff feel they are seeing the same problems again and again at a late stage, when a greater impact could have been made by earlier management or prevention. Many complex healthcare interventions represent wasted opportunities for prevention – at an enormous human and financial cost.
Better and more timely prevention not only improves the lives of individuals but also relieves pressure on the system and makes the work of our clinical staff more rewarding.
Although there are inspiring examples of preventative work happening across NHSScotland, these initiatives too need to be scaled up to the stage where they become embedded in practice, as was proposed in our chapter on innovation and knowledge.
Prevention also needs to address the wider determinants that influence individual behaviour. Focusing on individual behaviours can only go so far towards improving population health, and can even widen health inequalities – because those who already have the most resources are those most able to take up offers of support. [58]
These wider determinants are often much higher priorities for people than achieving better diabetic control or giving up smoking. As we increasingly ask people “what matters to you?”, we need to consider how to respond when they name poor-quality housing, loneliness, or financial worries. Realising our aspiration to person-centred care – and to effective prevention – therefore requires action to understand and address these wider determinants.
One way of doing this is through holistic support in healthcare settings, in the form of advice workers or referral to local sources of community support (sometimes called social prescribing). This doesn’t mean that NHS staff need to be experts in these issues. On the contrary, such initiatives can free up healthcare professionals to focus on what they do best – providing high-quality clinical care – whilst at the same time addressing patients’ priorities and the wider influences on their health. Here, we can learn much from our colleagues in social care who are very familiar with these approaches.
By making sure that patients are able to address their basic needs and social circumstances, we can maximise the chances that our clinical interventions succeed. For example, stable housing has been shown to improve medication concordance among people with several long-term conditions (including schizophrenia and HIV). [59,60]
Embedding holistic support into healthcare settings
A number of pioneering schemes across Scotland have recently shown the potential of providing holistic support services in healthcare settings to help people address wider life circumstances affecting their health. These schemes, developed in partnership between the NHS, local authorities, and the third sector, aim to tackle health inequalities and reduce pressure on general practice.
For instance, welfare rights advisors embedded in clinical settings can provide advice and support on benefits, debt, housing, pension and employment issues. A recent pilot project in two GP practices in Parkhead, Glasgow, delivered £850,000 worth of unclaimed benefit entitlement to 165 people and helped identify and manage £156,000 worth of debt.
Given the evidence showing that our income and financial situation is one of the strongest determinants of health, projects like this have enormous potential to benefit patients. They have also been welcomed by GPs, allowing them to focus on providing clinical care.
GP - “It is contributing to reduced time spent by GPs on paperwork relating to benefits, (it) lets us get on with the job we are trained to do.”
Patient – “Before – I was not really managing – I was upset/not doing really well… Now – I can put money towards things.” [61]
Only by realigning our efforts so that we give equal priority to causes as to conditions can we realise the vision of a National Health Service, rather than a National Illness Service. This is a profound shift, but a necessary one if our health system is to truly meet the needs of the public and the demands of the future.
How can we tackle unwarranted variation by using our roles as leaders and patient advocates to support action on health inequalities in Scotland?
On average, a boy born in one of the 10% most deprived areas of Scotland can expect to enjoy only 44 years of good health – a full 26 years less than his peer born in one of the 10% most affluent areas of Scotland. [62]
Such profound injustice in life chances based only on the circumstances into which one is born, is perhaps the most powerful example of unwarranted variation in Scotland today.
Inequalities across socioeconomic groups in healthy life expectancy, overall life expectancy, and a range of other health outcomes have been static or increasing in recent years. Especially stark inequalities in health are also seen among groups of people with specific vulnerabilities, such as learning difficulties, long-term mental health conditions, refugee or asylum seeker status, or experience of homelessness.
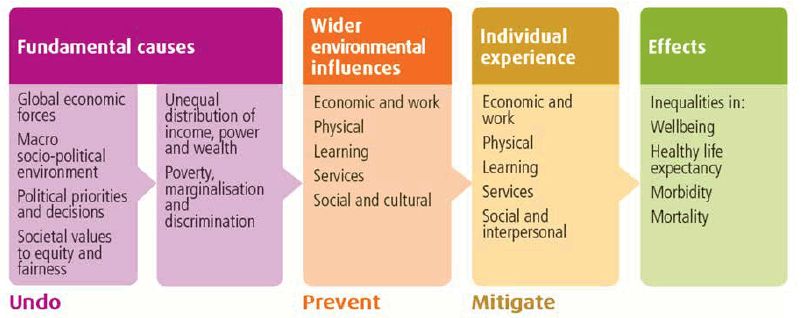
There is now good evidence to show that the “fundamental causes” of health inequalities are the unequal distribution of income, wealth, and power across the population, which in turn affect people’s individual experience of social determinants of health ( Figure 12).
The most effective interventions for improving health and reducing inequalities are therefore those which address the fundamental causes and the societal context in which we live – like the introduction of a living wage, pricing of unhealthy commodities and speed limits in residential areas. [63] Minimum unit pricing for alcohol, due to be introduced in Scotland on 1st May 2018, is one such intervention.
As health and care professionals, we can tell stories which bear witness to the consequences of health inequalities in everyday practice, and we can amplify the voices of those with lived experience. When we use our expertise, values, and influence to raise awareness of the social determinants of health and health inequalities, and support evidence-based interventions to address them, we maximise our impact on the health of the people we serve.
Figure 12. What causes inequalities in health? NHS Health Scotland’s Model [64]
Changing the culture by changing the context
Scotland has some of the highest rates of alcohol-related harm in Europe, and problem drinking is estimated to cost Scotland £3.6 billion per year. Although alcohol is seen by many as an integral, and unchangeable, part of Scottish culture, our consumption habits are in fact greatly dependent on societal and commercial factors like availability and price. Since 1980, alcohol affordability has increased by approximately 60% - as has the rate of alcohol-related deaths. People living in more deprived communities are more likely to experience adverse health and social impacts of alcohol than their more affluent peers.
The most effective interventions for reducing alcohol-related harm to individuals and communities are therefore those which aim to change the context in which drinking takes place. Minimum unit pricing (MUP) for alcohol, recently deemed legal by the UK Supreme Court after a five-year legal battle, is one example. The introduction of MUP exemplifies what can be achieved through the combination of clinical and third sector advocacy, rigorous public health research, and policy leadership.
The impact of MUP on health and health inequalities will be closely monitored over the coming years through a portfolio of studies covering compliance, availability, consumption, health outcomes, public attitudes, and economic impacts. [65]
How can we improve and innovate for health by collaborating across the NHS, social care and wider society?
Just as addressing multi-morbidity requires new ways of working across clinical specialties, improving population health and reducing inequalities requires new ways of working across society. The case study below on adverse childhood experiences is just one example, demonstrating how complex problems need holistic, multi-agency responses.
Addressing childhood adversity to improve lifelong health
There is increasing awareness that stressful events occurring in childhood, such as neglect, abuse, or having parents affected by domestic violence or alcohol and drug problems, are associated with lifelong impacts on health and wellbeing.
For instance, a Welsh study found that suffering four or more such ‘adverse childhood experiences’ ( ACEs) increases the chances of high-risk drinking in adulthood by four times, being a smoker by six times and being involved in violence by around 14 times. ACEs are also associated with poorer educational and employment outcomes.
ACEs occur across the population but are more common among children living in areas of higher deprivation. Indeed, poverty itself should be considered a form of childhood adversity given its close association with poorer long-term health, wellbeing, and life opportunities.
To prevent ACE, we must improve the societal context in which families live through measures to reduce poverty, inequality, and social isolation; parenting support programmes; and multiagency working that meets the needs of families in a flexible and holistic way. To mitigate the effect of ACEs, we must build resilience among children, families, and wider communities through fulfilling, supportive relationships, and provide public services in a ‘psychologically informed’ way that recognises and responds to previous trauma.
Addressing childhood adversity therefore requires collaborative action across the whole of society: uniting health, social care, education, policing and justice, housing, and many other areas. A cross-sectoral ACEs Hub has been established to lead this work in Scotland. [66, 67]
One approach which offers a systematic approach to this kind of collaborative working is “Health in All Policies” (“Partnership working for healthy public policy”).
Partnership working to inform healthy public policy
Policymaking in areas outwith healthcare – such as planning, housing, transport, education, and economic policy – has an enormous influence on our health. The most realistic approach to improving health, reducing inequalities, and reducing future demand for care is therefore to ensure that decisions in all policy areas are designed to support good health: an approach known as ‘Health in All Policies’.
The Scottish Health and Inequalities Impact Assessment Network ( SHIIAN) recently brought together public health, local authority housing departments, policymakers, and the third sector to assess the potential health impacts of the Scottish Government’s commitment to building 50,000 new affordable homes.
The project identified various potential health benefits including improved mental and physical health due to better housing conditions; increased independence and reduction in falls due to increase in specialist housing provision; and the potential for positive effects on people’s financial situation. Features of the places where new houses are built are also important for health – for example greenspace, community amenities and good walking and cycling access. SHIIAN is now working with partners in national policy, community planning, and place-making to ensure that the implementation of the policy maximise these benefits and minimise potential risks. [68]
Community initiatives have the potential to reach and engage people in ways that the health service cannot, helping individuals and communities to flourish and realise their potential. One example is Sistema Scotland’s Big Noise community orchestra projects.
Figure 13. Big Noise Community Orchestra

Improving health, wellbeing, and life chances by making a ‘Big Noise’
The Big Noise project, run by Sistema Scotland, aims to transform the lives of children living in disadvantaged communities of Scotland through free musical learning and performance, from six months old to school-leaving age. The programme is being delivered to over 2,000 children and young people within four areas in Scotland: Raploch (Stirling); Govanhill (Glasgow); Torry (Aberdeen); and Douglas (Dundee). Significant attention is paid to ensuring that all eligible children are able to participate, whatever their circumstances, needs or abilities.
An evaluation by the Glasgow Centre for Population Health has shown that Big Noise has positive impacts on children’s wellbeing, learning and education, social and life skills, and health-related behaviours.
In particular, Big Noise provides a degree of security, routine and structure to children’s time, over and above that offered by school and home life. This is particularly beneficial for vulnerable children with less wellstructured home lives.
The next part of the evaluation will focus on children’s educational attainment – an important area given its influence on longterm health outcomes. [69]
Any collaborative endeavour for health must ensure that the voice of the public is at the very centre of decision making. By prioritising the voices of the public and empowering those seldom heard, we can create a health service - and a public health service - that is humane, genuinely responsive, and much more likely to succeed. Greater control by individuals and communities over their own lives is itself also likely to benefit health. [70]
Conclusion
To ensure that everyone in Scotland has an equal chance of a life they have reason to value, we must think broadly about the factors that determine our health. As health professionals, we have a role to play at every stage of the causal chain that links “upstream” societal, economic, cultural, commercial, and environmental determinants with their “downstream” impacts on health. We can build on our strong foundation of a high-quality, universal healthcare system to:
- Embed prevention in our clinical culture;
- Ensure our practice is responsive to the social determinants of health;
- Advocate for effective population-level action on health and health inequalities;
- Create collaborations across health care, social care, and wider society; and,
- Empower people and communities to take their rightful place at the centre of decision making.