A Right to Speak Supporting Individuals who use Alternative and Augmentative Communication
Guidance to be used by people who use Alternative and Augmentative Communication (AAC), their familes, strategic and operational heads within health boards, local authority social work and education departments and the voluntary sector
How should AAC services be delivered?
Recommendation 4
To ensure that people who are required to use AAC have access to appropriate levels of high quality specialist assessment and support delivered as locally as possible, Health Boards and local authorities should work in Partnership with each other and with National AAC services.
Action
1. National services to design a planned programme of activity to develop capacity and competencies of regional and local services.
2. Local partnerships to establish multi-agency regional networks or centres providing support to local services and supported by National services.
3. National services to implement a programme to develop capacity and competencies of regional and local services.
Provision of AAC addresses five key areas of need within the International Classification of Function.38 These areas fall within the remit of provisions made by different statutory agencies. Provision of AAC supports access to the curriculum, education and employment, maintenance of safety, health and well-being, and the achievement of independent living.
Therefore, for all clients, AAC provision falls under the remit of more than one agency because the need of any client will undoubtedly be across more than one category. This supports the principle of joint provision of AAC.
Addressing the needs of people who use AAC contributes to several National Outcomes.39 By supporting individuals to communicate we are improving life chances for children, young people and families for those at risk, providing equity of opportunity through children having the best start, supporting young people as successful learners, promoting the population have healthier lives and tackling inequalities.
The evidence provided by people who currently use AAC and by some of the service providers suggests that we need to make some improvements around AAC provision of equipment and services. By implementing measures to improve how AAC is provided, we can ensure that public services are high quality, efficient and responsive to the needs of local people.
Provision of AAC services falls within the remit of several public agencies, with staff from education, health and social services involved in the assessment, training and support of people who use AAC. As illustrated below, each agency has a defined quality framework to support delivery of their respective services. The frameworks have a high degree of consistency and are summarised below:
| QUALITY | ||
|---|---|---|
| Health‡ | Social Care§ | Education** |
| Person-centred | Dignity, privacy, choice | Personal achievement Respect & positive ethos |
| Effective | Realising potential | Outcome focused |
| Safe | Safety | Integrated |
‡ Better Health, Better Care
§ National Care Standards
** Curriculum for Excellence
It is proposed here that a coordinated, multi-agency approach to the provision of AAC equipment and services will increase capacity within those services and contribute to improvements in quality.
Delivering for Health40 is concerned with delivering local, accessible and timely healthcare services with a shift in the balance of care from hospital to community care and partnership working. A further key aspect of this policy is the shift of emphasis onto preventative care and on tackling inequalities. Within education, The Early Years Framework 200841 is focused on developing the strengths of universal services to deliver prevention and early intervention, simplifying and streamlining delivery of services and building more effective collaborations. Similarly, within social work, Changing Lives42 places an emphasis on delivering 'joined up…. accessible, responsive services of the highest quality and promoting wellbeing'.
The consensus across all agencies is for high quality local provision that is resourced by appropriately skilled staff working collaboratively to deliver the best outcomes for individuals, families and communities. However, it is also acknowledged that regional, and in some instances national, planning is required to support the delivery of care in local settings10 particularly with regard to provision for children with complex needs.
At present, the level of AAC service provision varies across Scotland. In some regions a person with communication difficulties can expect to have input from AAC specialists at both regional and national level while in other areas there is no specialist provision. Access to national services is restricted in some areas. For the purposes of this document a national service comprises a multi-disciplinary team and provides input across several geographical boundaries across local authorities and health boards. A regional service is similarly multi-disciplinary in nature but provides services within a restricted geographical boundary, usually a single health board. In Scotland there are two regional services that fit this criteria: FAACT (Fife Assessment Centre for Communication Technology) and KEYCOMM (Lothian Communication Technology Service). There are currently two national AAC services in Scotland: the SCTCI (Scottish Centre of Technology for the Communication Impaired) and CALL (Call: Scotland). SCTCI provides services to the whole population, adults and children, within ten health board regions while CALL provides a national service for children in Scotland.
In other areas specialist services provide limited specialist AAC services. For example, in Ayrshire and Arran, one speech and language therapist provides specialist AAC services for the entire population, while in Grampian (TASSCC: Technological Assessment and Support Services for Children and the Curriculum), a multi-disciplinary service supports children with AAC needs principally within Aberdeen City and Aberdeenshire Community Health Partnership areas with limited services across the wider region. A description of these services is summarised in Appendix 5.
Several areas in Scotland have no designated specialist AAC service, although they have many staff with an interest and specialist skills within the field of AAC across different agencies and staff groups.
Effective implementation of AAC into an individual's communicative repertoire requires specialist assessment, appropriate provision, skilled support and universal recognition in the wider community. It is crucial that all AAC systems are reliable and that all systems, whether high-tech or low-tech, have up-to-date, age appropriate and relevant vocabulary. For a person who uses AAC, intervention is usually episodic but sustained throughout their life. These episodes may be related to initial introduction of a system, maintenance of a system, and education of family, carers and staff groups on how to support the individual to optimise their communicative effectiveness through use of the system. Episodes of care may be triggered by developing educational needs or by transitions, such as from school to college, hospital admission, relocation, or change of carers.
In education settings, generic AAC systems may be used to support learning and acquisition of literacy. It is here that a variety of resources can be utilised to augment an individual's personal AAC system. This requires skilled staff with dedicated time to amend, adapt and programme equipment to keep generic resources in step with the evolving curriculum. Joint funding and integration provide opportunities to develop capacity at a local level.
The Kaiser-Permanente Pyramid of Care43 has been adopted, in Scotland, as a model for care of people with long-term conditions44 and for the provision of specialist wheelchair services.45 This model appears to provide a structured approach for delivery of services that fits with the aim of delivering accessible, inter-agency AAC services. The model, applied to delivery of AAC services, is presented below.
This model encourages the development of regional, multi-agency and multi disciplinary AAC networks or centres that have equal access to national AAC services. These specialist AAC regional services may take the form of a specialist AAC centre or become virtual centres with a network of identified MDT teams of AAC specialists within a geographical boundary. These regional centres or networks support local services within their region. It would be anticipated that boundaries would include several local authorities and one health board region and that local authorities could elect to be part of one or more networks where their boundaries cross health board areas. Small Health Board areas may elect to become part of an AAC network with an adjoining Health Board.
Barriers to effective service provision identified by those working in the field include a lack of full access to the relevant range of specialists, particularly staff with a technical background. Networks or centres should be comprised of core staff across agencies, including AAC specialist speech and language therapists, AAC specialist teachers and medical technologists/bio-engineers. A medical technologist/bio-engineer is typically skilled in the use, maintenance and development of electronic assistive technologies.
Within this model it is anticipated that the AAC advisors will develop the competencies and practice of the specialist and generalist AAC workforce. The national centres would lead and support the development of regional centres or networks. They would be required to operate at a strategic level with Education, Health and Social Work partners and operationally in the delivery of education and training to regional networks and the wider community as appropriate. It is anticipated that they would be key to the development of inclusive communication and accessible information at a strategic level and would, for example, devise implementation plans taking a population approach to these areas. Some aspects of this model are already in place. For example, the Scottish Centre of Technology for the Communication Impaired runs a Link Therapy network of speech and language therapists across Scotland who receive regular updates on equipment and other developments within the field of AAC.
This model supports the development of an increase in capacity, hence providing an opportunity to improve quality for AAC services and should be achievable by providing local access to specialist support, universal access to National services and a reduction in waiting times to access all services.
Kaiser-Permanate Model
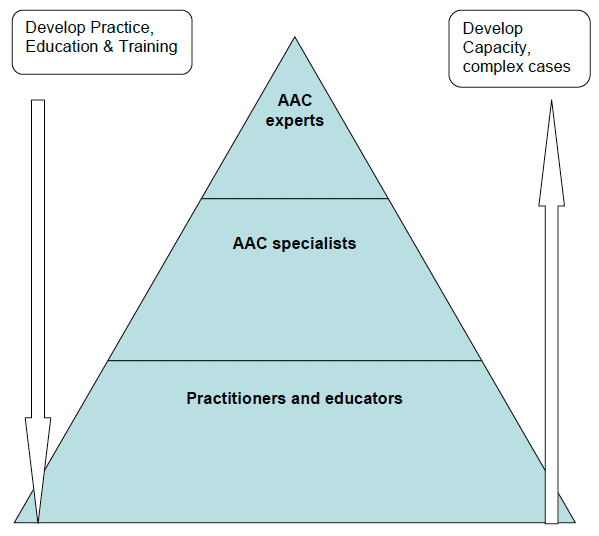
The model recognises that local solutions to providing AAC services may include a designated regional centre of specialist AAC staff or an identified network of multi-agency AAC specialist staff who are appropriately trained and have access to AAC assessment resources.
Model of Service Delivery for AAC
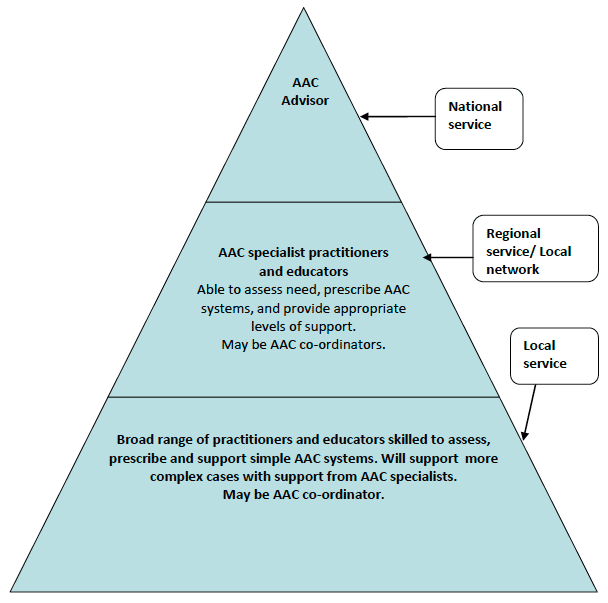
AAC advisor: role of national centres to develop capacity and practice in tiers below. Responsible for setting and monitoring of standards, planning education and training and an advisory role with complex cases.
AAC specialist: A practitioner or educator who is a specialist in ACC. The specialist works as part of a multi-disciplinary team and supports local staff when required. The specialist refers to the AAC advisor as required.
AAC co-ordinator: this role involves co-ordinating input from the multi-disciplinary team; ensuring that equipment is provided within local timescales; planning a programme of enhanced support; co-ordinating ongoing review of client needs and, where applicable, maintenance of equipment. Within children's services this may be the designated lead professional while within the adult services this may be the local SLT.
It is therefore recommended that AAC services are delivered by local partnerships that are aligned with Regional and National services within each Scottish region. These partnerships may take the form of regional centres or networks.
A set of principles to support the work of AAC services at national, regional and local levels has been agreed through consensus from service providers. These principles are consistent with the vision and strategic aims for AAC provision and are presented in Appendix 6.
Recommendation 5
The Scottish Government to explore the feasibility of NHS- based National AAC services transferring to NHS National Services to support the monitoring of quality and effectiveness of AAC provision as well as to protect this valuable resource.
Action
The Scottish Government will conduct an impact analysis on the transfer of NHS-based National AAC services to the National Services Division.
Throughout this document National AAC service providers are recognised as including both Call: Scotland (CALL) and the Scottish Centre of Technology for the Communication Impaired (SCTCI). While both are recognised as national services for AAC they have different funding mechanisms and provide slightly different services.
The SCTCI is funded by ten of the fourteen health boards across Scotland to provide AAC assessments, training and support for adults and children. CALL is funded centrally through education and provides services for children only across all of Scotland. The remit of CALL includes providing assessment and support for the communication, learning and literacy needs of children in education through the use of technology (including AAC) within the curriculum, and developing national resources for the classroom assessment. Recent work by CALL has included development of 'Books for All' and 'The Scottish Voice' (www.callscotland.org.uk).
Due to the nature of the services and funding mechanisms for CALL, recommendation 5 applies only to the SCTCI. National Commissioning is reserved for highly specialist services and provides support to services, ensuring equity and sustainability. SCTCI is currently hosted by a single health board. However, it is recommended that the mechanisms in place to support the SCTCI in the delivery of its services should be reviewed.
Contact
Email: Peter Kelly