Rejected referrals to child and adolescent mental health services: audit
A qualitative and quantitative audit of rejected referrals to Child and Adolescent Mental Health Services (CAMHS).
Findings: Being Rejected
Reflections from the qualitative research
- The most common reason cited by young people for their referral being rejected is that their case was not serious enough. This leads to a belief that unless the child or young person is suicidal or at immediate risk of harm, they will not be seen
- One in ten survey respondents sought help privately following a rejected referral. This suggests that other NHS or third sector services to which they may be signposted are either not appropriate or not available
- More than half of young people whose referrals were rejected took no further action, suggesting that the opportunity to help them has now been missed
- There could be a problem with multiple referrals for the same person, with 20% of participants mentioning that they sought another referral after being rejected. Sometimes these are consistently rejected, sometimes they are eventually accepted. We do not know what level of ‘churn’ is created by these multiple referrals but it suggests an opportunity exists to operate more efficiently by routing these referrals appropriately at the first time of asking
- Young people and their families report that while signposting does take place, it is generally not felt to be helpful. Few people spoke of being directly referred to or helped to access another service, suggesting that people are largely being left to select and try to access a service or information resource by themselves
- Some young people report being rejected because, by the time they were due for assessment, they were almost too old for CAMHS. This may suggest there can be a greater focus on structural issues than on the needs of the child or young person
There is a widespread belief that the reasons given for rejection are either inadequate or unjustified. Children, young people and their families reported that they often did not understand or did not agree with the reasons given for rejection, where any were provided. Many participants spoke of poor communication, a dismissive attitude and a lack of explanation for rejection. In some instances, the referrer does not pass the information on to the child, young person or family, leaving the family and or young person waiting.
The impact of being rejected can include worsening health, a financial impact of finding help privately and the effect of stress on family relationships. Signposting does take place but this was generally not felt to be useful, either pointing to websites or signposting to services that the family have already exhausted or that are unavailable or unsuitable. After rejection, some report paying for private help, some asked for another referral to be submitted and some did nothing.
More than half of the 87 young people who engaged with the online survey reported doing nothing after rejection. Multiple referrals are an issue, with 20% of participants in the online survey mentioning that they sought another referral after being rejected.
There are also issues with young people ‘falling between the cracks’, either because they have left school but are not yet 18 or because they are not attending school due to their emotional, behavioural or mental health issues.
Some young people waited so long that they were rejected because, by the time of their assessment, they were about to become eligible for adult services.
Why are children, young people and their families rejected from CAMHS, and what happens then?
Current national data collection only records a count of the referrals that have been rejected by NHS Board CAMH services. The qualitative audit found a noted variation in the proportion of referrals which are rejected across NHS Boards. This may be due to the differing referrals processes.
Reason for rejecting a referral
The reasons for rejections were similar across both the qualitative and quantitative elements of the audit. Figure 15 shows various categories for the reasons for rejecting a CAMHS referral, drawn from the seven Audit Boards. Three out of five referrals (62%) were rejected as they were deemed unsuitable. This means that either the referral did not meet NHS Board criteria, the child or young person was at the early stage of mental illness or disorder, the child or young person had a mild mental illness or disorder, there was no mental health issue or the child or young person was outwith the NHS Board catchment area.
Figure 15: Reasons for rejected referral collected from seven Audit Boards
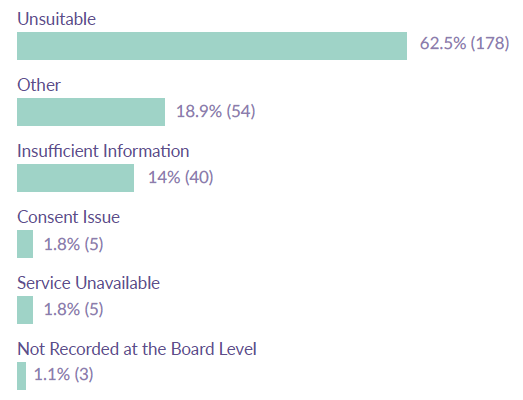
Source: ISD CAMHS Rejected Referrals Audit
Another common reason for rejecting the CAMHS referral was reported in the quantitative element as insufficient information referring to incomplete information in the referral documentation. This meant that the referral could not be reviewed or triaged for appointment or assessment.
The ‘other’ category in the reasons for rejecting CAMHS referral reported varied reasons, such as referral was a duplicate referral, inappropriate referral reason, referral did not have any indication of mental health issues or the child or young person referred was not physically seen by the referrer prior to referral.
It was also noted that there were five records (1.75%) where there was a ‘consent issue’. On further investigation, this meant that consent had not been obtained from the child or young person (as the referrer had not physically seen them) or had not been obtained from the parent or guardian. It is important to note that no referrals were rejected due to the refusal of service by the child or young person. In other words, no child or young person refused to engage with CAMHS or were non-responsive to the CAMHS appointment letters.
Table 2 shows that just under half (49.4%) of the referrals considered ‘unsuitable’ were for children between the ages of five and 11 years. ‘Unsuitable’ was generally recorded where the referrals was deemed inappropriate for the CAMH service.
Table 2: Age range of unsuitable referrals
| Age | Number | Percentage (%) |
|---|---|---|
| Under 5 | 10 | 5.6 |
| 5-11 years | 88 | 49.4 |
| 12-15 years | 53 | 29.8 |
| 16-17 years | 16 | 9.0 |
| 18 years | 9 | 5.1 |
| Age not available | 2 | 1.1 |
| Total | 178 | 100.0 |
Source: ISD CAMHS Rejected Referrals Audit
The main reason identified by the Audit Boards for referrals being rejected is that of ‘unsuitable’ (n=178 62%). Figure 16 shows a breakdown of these records as to why the referral was deemed unsuitable. Over half (52.8%) of these unsuitable referrals were because they did not meet the NHS Board criteria for accessing a CAMHS and almost a quarter (23%) were due to no mental health/illness identified. In these records, where no mental health/illness was identified, there were two common reasons for referral which were ‘behaviour problems’ and referral for an ‘Autism Spectrum Disorder ( ASD) assessment’. This may merit further investigation, given that behavioural problems are included in the definition of CAMHS. [10]
Data was also captured on the main reason that referrals were rejected by CAMHS and additional detail on why they were rejected. For example, of the 178 referrals that were deemed ‘unsuitable’, 94 did not meet the referral criteria of CAMHS and 41 referrals did not have a mental health disorder when reviewed by CAMHS. For those referrals that were rejected because of ‘other’ and insufficient information, no further information was available.
Figure 16: Reason for rejected referral in unsuitable category, collected from seven Audit Boards

Source: ISD CAMHS Rejected Referrals Audit
The qualitative research found a widespread belief that the reasons given for rejection are either inadequate or unjustified. People often did not understand the reasons given, as shown in Figure 17.
Figure 17: Understanding of the reason given for rejection, collected from the 253 participants of the online survey
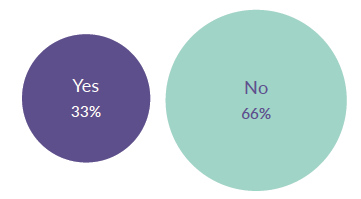
Source: SAMH CAMHS Rejected Referrals Audit
Common reasons for rejection include:
- The referring issue is not serious enough or meets the threshold for a tier 3 or 4 service. This is the most common reason cited by young people themselves, and leads to a belief that unless the child or young person is suicidal or at immediate risk of harm, they will not be seen by CAMHS.
“We were told….we recognise that you have anxiety issues, this was to my daughter, but they’re not severe and you’re self-harming, but it’s not severe enough for us to be able to offer you support. If things get worse, you’re welcome to go back to your GP for a further referral.” (Parent, group)
“She was not, is it Tier three level, Tier three and that they would not be able to support her in any capacity, but perhaps to go back to her GP to see whether or not something could be done elsewhere through the NHS as part of the hospital setting.” (Parent, depth)
“They said that he doesn’t have an eating disorder, he hasn’t committed suicide or tried to commit suicide.” (Parent, depth)
- The referring issue is not a mental health issue but rather a behavioural issue, related to an ASD diagnosis, a problem relating to lack of sleep or other non-mental health issue
“I remember a bit from the letter that says that my daughter didn’t have a mental health problem.” (Parent, group)
“His anxiety is a result of his autism and not understanding the world around him and it’s not something that they can help with.” (Parent, depth)
- The person does not meet the criteria – with little or no further explanation
“They said on the letter that they had discussed it at one of their meetings and she didn’t meet the criteria. They gave me a leaflet on sensory processing for autistic children, all of which I was already doing…so it wasn’t really any help.” (Parent, depth)
“They literally said, ‘She doesn’t meet the criteria’” (Parent, group)
- The referral is inappropriate: this was mentioned in cases where children or young people had been sexually abused or assaulted, and cases where other services such as the police or social work were involved or cases where CAMHS felt another agency should be contacted.
“I got a letter through the door basically saying it was an inappropriate referral and that I was to be referred to Sleep Scotland. I think the CAMHS sent the GP letter to me rather than the parent’s version because of the language that was used, it was almost like they were talking to the GP saying, “This is inappropriate, it needs to be referred to Sleep Scotland.” (Parent, depth)
“ CAMHS say, ‘No, it’s not an appropriate referral for us so go and see social work’, and then social work are getting inundated with things and, to be honest, it’s not their area of expertise either.” (Parent, depth)”
“I eventually spoke to the girl. She was very nice and said, “I’m really sorry, she’s been rejected. They don’t feel it’s appropriate and it explains it in the letter.”” (Parent, depth)
- In many cases no further explanation is given
“It didn’t have any information about why they were rejecting it, it didn’t have any advice, it didn’t have a contact number, nothing, it just said “We’re rejecting the referral, go back and speak to your GP.” (Parent, depth)
How are rejected referrals communicated to children, young people and their families?
In some instances, parents and or young people are told at the end of their assessment that no treatment will be given by CAMHS.
“He [my child] spoke with her for about 15 minutes, then I was called in to the room and told he wasn’t severe enough and no further appointments would be offered.” (Parent, survey)
“We got the referral that was straightforward, but when we got there they turned round and said it was us that was the problem, we were the bad parents.” (Parent, depth)
In other cases, there is a further wait for a decision about whether children and young people will be accepted for treatment.
“I think we had one appointment and they never seen him again and we never heard nothing and I think I was told it was maybe lost on the system or some kind of system changeover, and they never got back in touch and nothing ever come of it.” (Parent, depth)
Some people receive a direct letter to the parent or young person, with nothing sent back to the referrer. Some receive a copy of the letter sent to the referrer: this is often written in clinical language.
“I got a letter through the door, as I say very quickly, and the letter basically said along the lines of we’ve had a referral from your GP, we’ve discussed it and we won’t see him. And attached are a list of various different things that you can use, look into, progress with in order to provide additional support. There was no attachment, so that information wasn’t in the letter, and that was it.” (Parent, depth)
Others hear direct from CAMHS in person or by phone.
“She [ CAMHS nurse] basically said to me that because I’d left school, all my other options would have been adult mental health services, but they wouldn’t do anything for me because I wasn’t…. basically like my case wasn’t serious enough for them to be able to treat me.” (Young person, depth)
“I phoned CAMHS and they said, ‘Oh, oh no, she never met the criteria, did the GP not tell you?’” (Parent, depth)
Some hear of the rejection via the initial referral route. Some people were invited to an appointment with their GP or a meeting with school, some were told by phone, either by the GP or a receptionist.
“Then I got a phone call, I don’t know, maybe about 10 weeks later, ish, from the GP receptionist saying that CAMHS refused to take the referral any further because the GP had not seen [my son] and the discussion had not taken place with my son, at the consultation.” (Parent, depth)
Some did not hear back at all.
“It wasn’t technically rejected, we just didn’t hear anything back.” (Parent, group)
Figure 18: Who communicated the rejected referral from CAMHS, collected from participants of the online survey
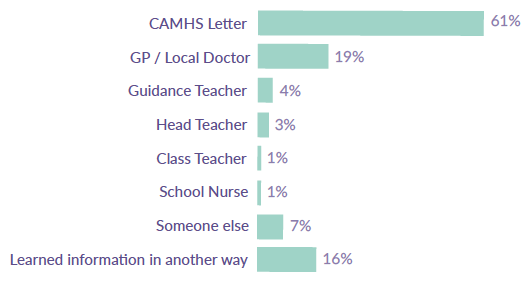
Source: SAMH CAMHS Rejected Referral Audit
The language used in communicating the rejection can also be problematic – either from the perspective of seeming uncaring or dismissive; not being easy to comprehend; or blaming the parents.
“It doesn’t have to be like that, it’s just a little bit of dignity and a more respectful means of either offering some alternative or explaining why a decision has been made, rather than, “You’re clearly not mentally ill, go away”. It’s shocking.” (Parent, depth)
“Was told that my suicide attempt was me attention seeking and that there was nothing wrong with me.” (Young person, survey)
“It doesn’t tell you why. It just tells you it’s been rejected and didn’t actually give any reasons for the rejection really. We were both pretty baffled by it in terms of the way it was written, and the language in it…for us it wasn’t very helpful in terms of understanding the reasons behind it and also what the next stage in the process was.” (Parent, depth)
“When I received the follow up letter which basically accused us of being the problem I slumped into depression myself. Crucially, the letter mentioned absolutely nothing about my son’s previous history, his self-harming or the fact that he mentioned in the meeting that he would attempt suicide again!” (Parent, survey)
In some instances, the referrer does not pass the information on, leaving the family and or young person waiting longer than they should; still assuming they are in the system.
“I gave them the benefit of the doubt and waited three months. I phoned CAMHS, and I was told, “Oh did they not tell you you were rejected?” I said, “So when was this?” And they said, “A couple of weeks after the referral was made.” I said, “Well I’ve been waiting for three months, and I’ve not had an answer.” So, I phoned the doctors and they confirmed that it had been rejected.” (Parent, depth)
“Well when I got rejected I was waiting… I waited all summer for an appointment because I already knew that they sent your appointment in the post so I was waiting all the time, all the time and then it got about one month, because I’m not very patient, so I phoned up the GP and was like, ‘I’ve still not heard anything back’, and it was then the GP said, ‘ CAMHS rejected your referral’, and then I was heartbroken, so heartbroken because I was like I’m never going to get help.” (Young person, group)
Actions taken following rejection
Figure 19 shows the categories for the actions taken by CAMHS following the rejection of the referral. Nearly half (46%) of rejected referrals to CAMHS were returned to original referrer with signposting, although researchers did not examine the type of signposting provided or the availability of the services to which people are signposted. This would infer either the referral was considered unsuitable for the referred service, insufficient information was provided or the service was not provided in the particular NHS Board area.
Figure 19: Actions taken by CAMHS following the rejection of the referral
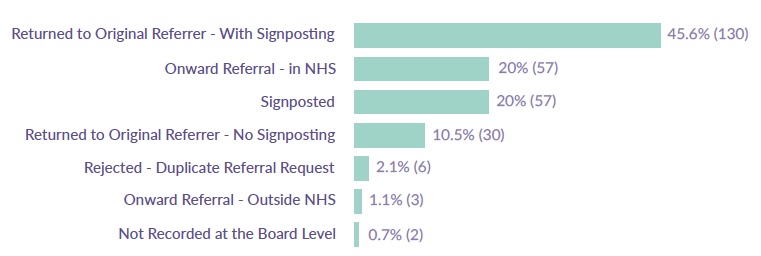
Source: ISD CAMHS Rejected Referrals Audit
Other main categories reported for the actions taken following the rejection of the CAMHS were that the referral were signposted (20%), the referral was referred onward within NHS (20%), or returned to original referrer without signposting (11%). Figure 19 indicates that overall 66% of rejected referrals do include signposting. However, approximately one in ten referrals that are rejected do not have any follow up/signposting identified.
One in five (20%) of the rejected referrals were signposted directly and not returned to the original referrer. This means that the child or young person was either directed to online support via a self-help website or to other support services such as the third sector.
This research did not examine the type of signposting provided or the availability of the services to which people are signposted.
During the month of February, the seven participating Audit Boards report that 66% of the 285 rejected referrals include signposting. Yet there is a disparity between this and the extent to which children, young people and their families themselves recognised being signposted. Of the 253 people who participated in an online survey of their experiences, just 42% feel they have been signposted.
During the audit, demographic data was collected including the child or young person’s Community Health Index number ( CHI), postcode and gender. This data will enable ISD to interrogate other health datasets to find out if the child or young person used other statutory services such as Accident and Emergency. This will help with further establishing what happens to children and young people if they are rejected from CAMHS. An update on this will be provided once data is available, it is hoped this will be by spring 2019 – though caution should be noted as there are small numbers involved.
What support are children, young people and their families offered when their referral is rejected?
Children, young people and their parents often did not feel well supported at the point of rejection. Those who had a more positive experience tended to report that their referrer was both supportive and persistent in seeking to get them support. This seems to be down to the attitude and persistence of the individual referrer. Although signposting did happen in around two-fifths of cases (as shown in Figure 20), in general it was not felt to be of high quality.
Figure 20: Were people signposted to another service or resource? collected from participants of the online survey
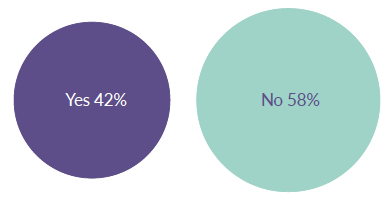
Source: SAMH CAMHS Rejected Referral Audit
“She [ CAMHS nurse] gave me the website Moodjuice….and basically for any other thing like helplines she said I would have to go back to my doctor and speak to them, because she didn’t know.” (Young person, depth)
In many instances, young people and their families have already exhausted these avenues prior to seeking a referral to CAMHS. For some, the signposting feels generic and not particularly useful.
“The only thing they suggested, and to put it really bluntly and to look back, it was a load of bollocks, it was just links to websites…. I did visit the websites, and they were like generic, top 10 tips to deal with anxiety.” (Young person, depth)
In other cases, the options suggested are unavailable or unsuitable.
“We had nowhere to turn. The support they suggested wasn’t actually available to us. I had to find out for myself what was available it was taking too long so we went private and got a counsellor because she was in crisis. In [our area] there were no NHS or third sector options for her?” (Parent, survey)
Parenting courses are often suggested.
“ CAMHS refused to see us again saying that I needed to go on a parenting course.” (Parent, depth)
Following a rejected referral, just under a quarter of those responding to our survey contacted another service: we do not know how many received help from this service or found it useful. A similar proportion used online or other resources. More than one in 10 paid for private help. A fifth asked for another referral to be submitted. More than half of the 87 young people who engaged with the online survey reported doing nothing after rejection.
Figure 21: What people did after being rejected from CAMHS, collected from participants of online survey
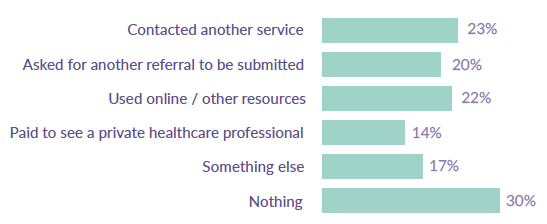
Source: SAMH CAMHS Rejected Referral Audit
What impact do rejected referrals have on children, young people and their families?
The effect of having a referral to CAMHS rejected can include:
- Issues escalate / worsen
“When I kept on getting rejected I was just in a really, really bad place and I feel like say if I got the help that I needed then when I got rejected, I probably wouldn’t have had as many suicide attempts or had to go up to accident and emergency so many times.” (Young person, group)
“The [assessment] experience affected my daughter and she opted not to be referred back there and just to continue seeing the school nurse who she has a really good relationship with. Unfortunately she has since self-harmed, making lots of quite superficial cuts on her wrist. She did this during the night when we were all sleeping. She needs help which was denied her from CAMHS so we are taking her to see somebody privately, shouldn’t have to do this but my daughter has been let down and we just can’t sit back and wait for something serious to happen.” (Parent, survey)
- Financial impact of finding alternative, private, help
“We saw a child psychotherapist in Glasgow for maybe September to the Christmas time. But I got to the point where I thought I need to get back to the doctor and re-refer and try and get him support through the NHS because I can’t sustain… £280 a month. But at the same time you’re feeling extremely guilty because I’m thinking that’s the only support that my son has. And he didn’t want it at first, but then eventually he really felt the benefit, and he was really upset when I said that we need to stop this, I can’t keep this up. He was really angry with me, and that was really difficult because then you’re thinking I’m putting financial implications before my own son. But at the same time I thought we can’t sustain this, we need to try and look for other ways to help you.” (Parent, group)
- Impact on family relationships
“Because the thing is, when you feel that you’ve got nowhere to go, me and my husband have talked about splitting up and my husband keeping X and me moving out with the other three children, because it’s really disruptive for the other three children as well.” (Parent, depth)
There can also be an emotional impact from a rejected referral.
- Feeling let down, with nowhere to turn
“You kind of feel like the one place that maybe could have told you what to do, have just kind of shut the doors on you and you just feel helpless, you just don’t know what to do with yourself or where to go.” (Young person, depth)
“It just affected everything, every aspect of your life it just affected, because you were walking on eggshells and you just never, there was just nowhere to turn, absolutely no help at all out there.” (Parent, depth)
“It’s just massively stressful. It’s just another added stress on an already stressful situation. We just feel very much if they’re not offering any kind of input then who is, because we’ve exhausted all avenues. We feel there’s nowhere else we can turn for help with my son especially. It’s massively stressful. I mean you’re still dealing with the issues that you’re dealing with, so you’re still dealing with the behaviour of whatever’s gone on, on top of the kind of stress of thinking, ‘So what do we do now?’ It’s just really, really stressful.” (Parent, depth)
“We were very upset, felt very let down and not taken seriously. I think when you’re in the midst of trying to support a young person who’s having serious mental health issues and you get told that it’s not serious enough, it’s a pretty horrible experience.” (Parent, depth)
- Feeling alone and in despair
“For a while I thought that there would have been no help available to me, and that basically I would have to lump it for the rest of my life and find different ways to cope with how I’m feeling. It really upset me, because I genuinely thought that there was nothing that anybody could do for me. Like I said, I would just have to like live with it for the rest of my life. Like feeling as low as I did at the time, and it was a really horrible thought. Because every day was quite difficult, and it was like a new challenge in itself. I would never want to go back to how I felt at that point, once the CAMHS nurse said there was nothing that I could do. Even like just thinking back, like now, I never want to feel like that again, I felt so alone.” (Young person, depth)
“I felt really isolated by it because I wasn’t sure why I wasn’t getting the help and I felt completely misunderstood.” (Young person, depth)
“When I was then told I was rejected I was like well, it made me feel rejected because it made me feel am I not worthy of help, am I not deserving, am I not ill enough? These are the questions that go through my head, was I not ill enough? Was I not severe enough? Was I not mentally ill enough? And it was just thoughts like them and I feel no person should feel like that.” (Young person, group)
- Feelings of guilt or failure among parents
“For me I feel like I’ve let her down to get things to this point. So going to the doctor in the first place was a huge step. And then letting her down again by not actually getting any help from it. At least she was too young to know.” (Parent, group)
- Feeling angry
“Disgusted. Angry. Let down. Confused. Unheard. Ignored. Irrelevant. Unworthy. To name the first few off the top of my head I honestly don’t understand their logic and how they can completely dismiss my son and in turn our family! My eldest son really needed their help and support and we got nowhere! CAMHS should be absolutely ashamed of themselves for the way they have treated my family, and I’m under no illusion that we aren’t the first they have done this to!” (Parent, survey)
Multiple referrals
Multiple referrals are an issue, with 20% of those responding to our survey mentioning that they sought another referral after being rejected. It was common for young people and their parents to speak of being referred and rejected several times. Some reported being accepted after two or three rejected referrals.
In some cases several referrals are submitted, sometimes by different referrers, for the same case.
“The issues were like self-harm, stuff like that which had kinda got a lot more dramatic in the space of a few months, so that was my first referral to them; we’ve had several attempts. So then the second one was I attempted suicide and that went to my GP and that got rejected again, and then on the third one, that was another suicide one, and it got a bit further into the process but got rejected just at the end of the process and then the fourth one was just needed to get a referral somehow, so we put another referral in and it got rejected because I was too close to being 18, even though it was like a year and a half away; and then they put a referral in at the start of this year and I got into the adult one straightaway.” (Young person, depth)
“So, the first time I was referred I was accepted and my social worker put a referral in and that was fine, I had six sessions with her and then the person was nice and then I was discharged. But then things went downhill rapidly and then I was referred from my GP and then they rejected me and then my social worker then said, ’Well, my referral was rejected, so I put another referral in and it was rejected from her. And then my GP put another referral in and it was rejected.” (Young person, group)
Falling between the gaps
Another issue raised was that of young people who have left school but are not yet 18 years old.
“I think more needs to be done for young people that are at that awkward position, where they’re not 18 yet, but they have left school. Because there’s quite a few services for young people that are still at school, and there’s quite a lot of services for adults.” (Young person, depth)
“My doctor still put the referral through and he knew that I’d left school because of the anxiety… it was really upsetting, because it was the actual CAMHS nurse that told me that there was nothing that she could do for me.” (Young person, depth)
“The second referral was actually accepted, but when I got to ... I actually turned up to the place for like my first meeting with the new CAMHS nurse, and she basically told me that there was nothing that she could do for me, because at that point I’d left school because my anxiety was so bad.” (Young person, depth)
A further issue relates to the transition between child and adult services – in a few cases the waiting time from referral to being seen meant that a young person became ineligible during the process.
“She was in fifth year at school when the process started of referral to CAMHS…It got to the point where it was three and a half months short of her 18th birthday and that’s a really significant timeframe because actually what happened was they wouldn’t accept a referral because it was too close to the 12 week window in which they refer young people. They basically refuse to take a young person if they’re within 12 weeks of their 18th birthday.” (Parent, depth)
Suggested improvements: being rejected
In relation to being rejected, parents and young people wanted:
- Detailed reasons why a referral is being rejected. These should be provided to the young person and their parent as well as the referrer and should be written in Plain English, with empathy, acknowledging that the child or young person and family are in severe distress
“Surely there’s more helpful ways to respond to people, more compassionate ways to respond to people, because it felt just like we were dismissed.” (Parent, depth)
“They [ CAMHS] should have to justify to families and to the other professionals involved why a referral has been turned been down and not to say, ‘We can’t see them at this time’. They should be accountable to families and to the people who have referred families to them, the other professionals involved, as to why the referral hasn’t been accepted and where else families can go so that people in crisis are not just abandoned.” (Parent, depth)
- It should be mandatory for rejections to include relevant signposting to other services
- If no other services are available there needs to be careful consideration before leaving children and young people with nothing
“You can’t leave people in limbo, if you’re rejecting them, you still can’t leave them in limbo.” (Parent, depth)
- A mechanism for checking in with families after six months to make sure they’re getting help
“There’s no system in place to track it, to monitor it, to follow-up on it.” (Parent, group)
“I also feel if their advice and recommendations don’t work that you should be able to get back in touch.” (Parent, survey)
- Clarity about what to do next, whether a second opinion can be sought, and how best to do this
“There’s no appealing the decision process that I could see and I think there should be.” (Parent, depth)
- Someone to talk to
“Being able to talk to somebody. Somebody that understands what you’ve gone through and maybe somebody can say, “Well, try this till you get help”” (Parent, depth)
“I think there should be a counsellor in school trained in mental health training if CAMHS are not willing to provide help.” (Young person, survey)
Participants’ suggestions for change: overall
Participants also made suggestions for changing the overall CAMHS process.
- Greater recognition of importance of providing support to children and young people before crisis point
“Prioritising mental health care as a way to reduce cost of long term physical/social effects e.g. alcoholism, drug use, self-harm, obesity, inability to work.” (Parent, survey)
“If you catch them early, most of these conditions are treatable, they have a much higher success rate of treating them if they’re got early rather than when they’re in deep crisis.” (Parent, group)
- Availability of more options for non-Tier 3 & 4 help and support
“There really needs to be something else that schools, GPs, social workers, can offer quickly.” (Parent, depth)
“I think there’s a massive gap in the service that maybe CAMHS can’t address, and that’s fair enough, but there needs to be something else.” (Parent, group)
“Either you get the top notch CAMHS, highly paid psychotherapist for two years or something similar or nothing, there’s nothing else, there’s no tiered approaches it feels like, so clearly there needs to be a variety of different types of interventions at different levels.” (Parent, depth)
“I think reconfiguring the system to allow for different levels of intervention at different levels of need and at different times, so you can drop in and out, rather than it being all or nothing when you’re deemed to be ill enough.” (Parent, depth)
“If the resources were re-looked at and there was more generic help for parents, you go to a support group but if you had the same amount of people, once a month somebody coming in and just talking about things, that would give an awful lot of information to people.” (Parent, group)
“The service is stretched and therefore only those with severe symptoms are being seem. Even after they are seen you are directed to a charity for on-going support post diagnosis (in the case of ASD) we are as a country missing out on those with great potential with relatively mild symptoms who get no NHS support. These children with the right support could go on to lead completely normal lives and required no adult help. Without support they will struggle to get an education and will not reach their potential.” (Parent, survey)
Increased resources
- Funding, so more children and young people can be seen, more quickly, and for as long as they need help
“Probably more money into the system, because I suspect they’re greatly over-stretched, but a rethink entirely, a complete branch rethink about how they organise themselves, about the staff they employ, and the abilities of the staff they employ.” (Parent, depth)
“The funding needs to be increased so that children and young people can be seen for as long as they need to be seen, not for as long as the cost says they can be.” (Parent, depth)
“I believe that the system is desperately underfunded and that that is the only reason that my daughter was rejected and not given the help she needed.” (Parent, survey)
“Give more funding to provide more resources to allow all children some real help before they reach a point of no return.” (Parent, survey)
- Increased staffing
“We need more clinical psychologists.” (Parent, group)
“They need more therapists.” (Parent, group)
- Alternatives to CAMHS/more support available in schools
“They should also go into the schools more, there should be a CAMHS counsellor or a CAMHS support worker in schools.” (Parent, group)
“If they had somebody coming in to the school, even once a month, to have some kind of discussion. But, you know, there are a number of play based, art based, music based, therapist, yoga, mindfulness, all of those things that we know make a difference.” (Parent, depth)
“If there was a counselling service in the school, you know, that the children could drop in, it could be as simple as there’s a wee girl upset, she’s, her dog’s died, she could go in there and speak to somebody to somebody who’s been bereaved to somebody who’s taking drugs, whatever. To me a service like that should be at the school, even (one) that parents could drop into.” (Parent, depth)
“I feel like I’m so glad that I’m not 16, 14 anymore because I’ve now got a lot more support than I could ever dream of and I’m incredibly grateful for that. I just feel like if I could get the help and support from CAMHS, I wouldn’t be in the state that I was in, I wouldn’t have had to have so many hospitalisations, I only had four psychiatric ones but I had countless ones through self-harm and doing things to cause harm to myself. But if CAMHS helped me I would have thought that I wouldn’t have had so many and I wouldn’t have self-harmed as much as I have done.” (Young person, group)
Figure 22: Words most used in the qualitative interviews that describe people’s feeling about CAMHS process
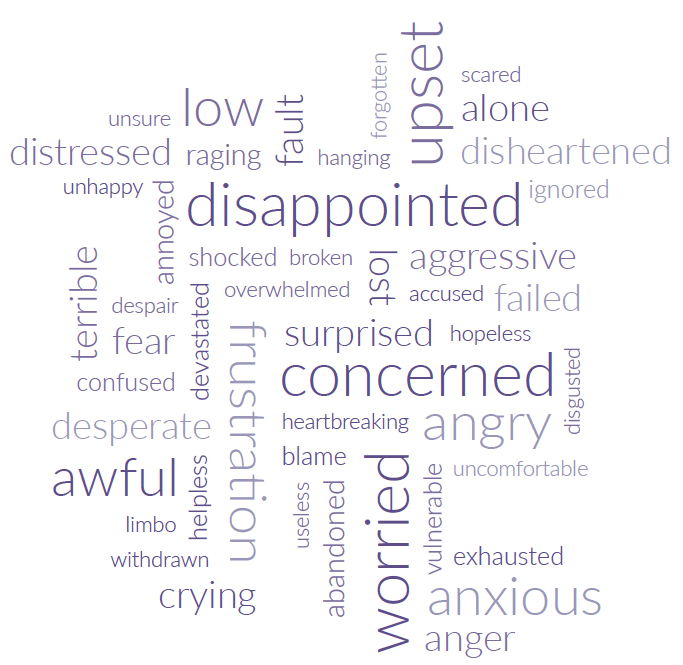
Source: SAMH CAMHS Rejected Referral Audit
Contact
An easy-read version is available on request from MentalHealthStrategyandCoordinationUnit@gov.scot.