Rejected referrals to child and adolescent mental health services: audit
A qualitative and quantitative audit of rejected referrals to Child and Adolescent Mental Health Services (CAMHS).
Findings: Being Referred
Both elements of the audit found that rejections are generally processed quickly. There was no evidence of any correlation between the source of a referral and its likelihood of being rejected. There is some commonality across the referral criteria used by NHS Boards and only one lists reasons that a referral may be deemed as inappropriate. There is substantial variation between the reasons for referral noted by NHS Boards and the reasons given by children, young people and their families. The qualitative element found parents and young people do not have a good understanding of the referral process.
When a referral is submitted, the widespread expectation is that the next stage is treatment. Many children, young people and their families receive a rejection letter within a very short timescale and feel angry, aggrieved, cheated and let down due to a feeling that no proper assessment process has been undertaken. Children, young people, their families and referrers often spoke of a lack of alternatives to CAMHS for children and young people with emotional, behavioural and mental health problems across all levels of severity.
Others who do get invited for assessment often believe this is the start of treatment, and are then left feeling in limbo when they are either rejected or then placed on a waiting list to access treatment.
“I didn’t understand anything, I’ve never been in this situation where anybody in my family has got autism. So, it was all new and all daunting to me. I didn’t get any information back from them to tell me this is the stuff we’re looking for and things like that. I just didn’t get any feedback from them at all.” (Parent, depth)
Experiences prior to referral
The qualitative research found a lack of clarity for children, young people and their parents about the referral process. They do not understand what is meant to happen, particularly relating to assessment.
It was clear that CAMHS is rarely the first port of call. In most cases, before a referral to CAMHS is considered there has been an escalation of issues to a debilitating degree, such as:
- School refusal / exclusion
“He was highly, highly stressed at school…the school weren’t really aware, and that resulted in him refusing to go to school.” (Parent, depth)
“It got that bad where I couldn’t get her out the house, some days I couldn’t even get her out of bed.” (Parent, depth)
- Behaviour becoming too difficult to manage
“His behaviour became more and more difficult to handle, and a lot more meltdowns, a lot more kind of emotional distress…. I felt that we were at a point where I had exhausted the strategies that I could try basically myself.” (Parent, group)
- Concern over potential harm (to children or young person or other family members)
“Self-harm, stuff like that which had kinda got a lot more dramatic in the space of a few months.” (Parent, depth)
“She was self-harming, scratching herself and drawing blood with fingernails. She’s got scars all over her body from doing this. She was displaying OCD behaviours, light switches on, off, on, off all the time.” (Parent, group)
- Anxiety, panic attacks, unable to control emotions
“Flying up with rage, not able to control his own emotions.” (Parent, depth)
“I was struggling with anxiety, I was having panic attacks every single day and self-harming, and then that’s when I got referred to CAMHS the first time.” (Young person, group)
“I started to develop this really bad anxiety. I wasn’t, like I was always kind of, you know, distant from other kids and stuff, so there was a little bit of social anxiety, but what it really boiled down to was this, like irrational fear of wasps and flying insects. Like I wouldn’t leave the house during summer.” (Young person, depth)
Referral process
Generally, once CAMHS receives a referral, the service will triage or review the content of the referral letter. If the referral has enough information and the service provides that care, then the child or young person will be added to the waiting list and an appropriate appointment given to begin treatment. In some cases an assessment appointment may be given but the waiting times clock does not stop until the child or young person is seen at their first treament appointment. If the details in the referral letter are not clear or there is not enough information, the service may contact the referrer for more information. Rejected referrals occur when the service does not provide that care and the referral is sent back to the original referrer. Figure 10 demonstrates this process.
Figure 10: Referrals process to CAMHS
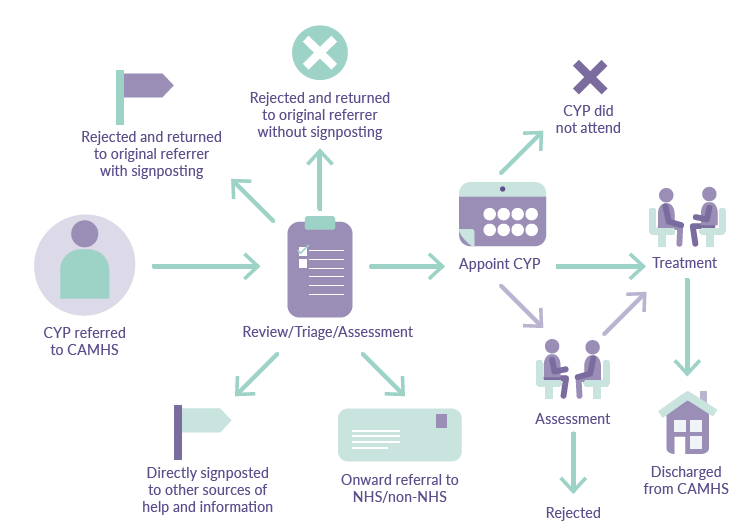
Referral criteria
The participating Audit Boards were asked to provide information on their referral and triage/vetting processes as well as their criteria for accepting a child or young person into the CAMH service. Four of the seven Audit Boards provided all the requested information with the remaining three providing their referral criteria document.
Reviewing the criteria documents showed that there is some consistency in the written criteria amongst the Audit Boards however; some do provide more detail than others.
Common referral acceptance criteria include:
- Age: The child or young person should be between 0 to16 years old or up to 18 years if still in full time education
- Consent:
- This must be obtained from the parents/carer/guardian or young person before the referral is submitted to CAMHS
- The referrer must have physically seen the child or young person before referring them, with one Audit Board adding ‘must be seen within five days of the referral’
- Severity of Condition:
- The child or young person must be experiencing moderate to severe difficulties, with two Audit Boards adding that these must be impacting their daily functioning
- These difficulties must have been present for ‘some time’. Only one Audit Board stated a time period of more than 6 months
In addition to the referral criteria that were common to all Audit Boards, there were local variations that provided referrers with more detailed guidance. Some of the Audit Boards add more detail to their referral criteria document than others, such as:
- Geographical Criteria: One Audit Board states that the child or young person must live within the catchment area of the team they are referred to. They also list essential information that should be included in the referral letter. This Audit Board was the only one that added this criteria and gave further information on what should be included in the referral
- Referral Pathways:
- One Audit Board has a flowchart to assist with referrals
- Three Audit Boards have a list of difficulties which also include a referral pathway and advice for each of the difficulty listed
- CAMHS Waiting Times Definition: Three of the Audit Boards reference the ISD CAMHS waiting times definition document and state the two level thresholds that are used (condition 1 - basic threshold and condition 2 - complexity and severity threshold)
Only one of the Audit Boards listed reasons for which a referral to CAMHS would be considered inappropriate. These include: response to normal life event, difficulties that only occur at school, child or young person whose parents are in dispute with legal proceedings or whose primary difficulty is substance misuse with additional difficulties described as offending behaviour.
Sources of referrals
There are many ways a child or young person can be referred to CAMHS. Both the quantitative and qualitative elements of the research found that the majority of referrals came from a GP. The qualitative research found that in a small number of cases, both the school and the GP were involved in the same referral.
The quantitative audit findings show that of the 285 rejected referrals submitted, 226 (79%) of these were from a GP. Other referrers were school nurse, teacher, and paediatric outpatient services. There is no significant difference between the referral sources for rejected referrals and those for other CAMHS referrals across the seven Audit Boards. This suggests that there is no correlation between the source of a referral and its likelihood of being rejected.
Table 1: Sources of rejected referrals
| Source | Number | Percentage (%) |
|---|---|---|
| General Practitioner ( GP) | 226 | 79.3 |
| Paediatrics Out-Patient Service | 11 | 3.9 |
| School Nurse | 11 | 3.9 |
| Teacher | 9 | 3.2 |
| Paediatrics In-Patient Service | 5 | 1.8 |
| Social Work Dept | 5 | 1.8 |
| Other | 5 | 1.8 |
| A&E (Adult) | 3 | 1.1 |
| Psychiatrist - other hospital | 3 | 1.1 |
| Voluntary Agency | 3 | 1.1 |
| Speech and Language Therapist | 2 | 0.7 |
| Dietician | 1 | 0.4 |
| Educational Psychologist | 1 | 0.4 |
| Total | 285 | 100 |
Source: ISD CAMHS Rejected Referrals Audit
Reason for referral
There are many reasons a child or young person may be referred to CAMHS. Both the qualitative and quantitative elements of the audit collected data on the most common reasons for referral amongst those that were rejected.
Anxiety, low mood and depression, self-harm and suicidal ideation were more frequently mentioned by participants in the qualitative audit than in the data submitted by the Audit Boards. The Audit Boards were more likely to list behavioural problems, other reasons and anger issues as reasons for referral.
Figure 11 shows the various categories for reasons of CAMHS referral according to the data gathered from the Audit Boards. The ‘other’ category included a variety of reasons such as:
- referral was considered premature i.e. not all investigations were complete before referral to CAMHS
- the child or young person was referred for reasons such as ‘stress’ or ‘needs counselling’
Figure 11: Reasons for referral from quantitative element of audit
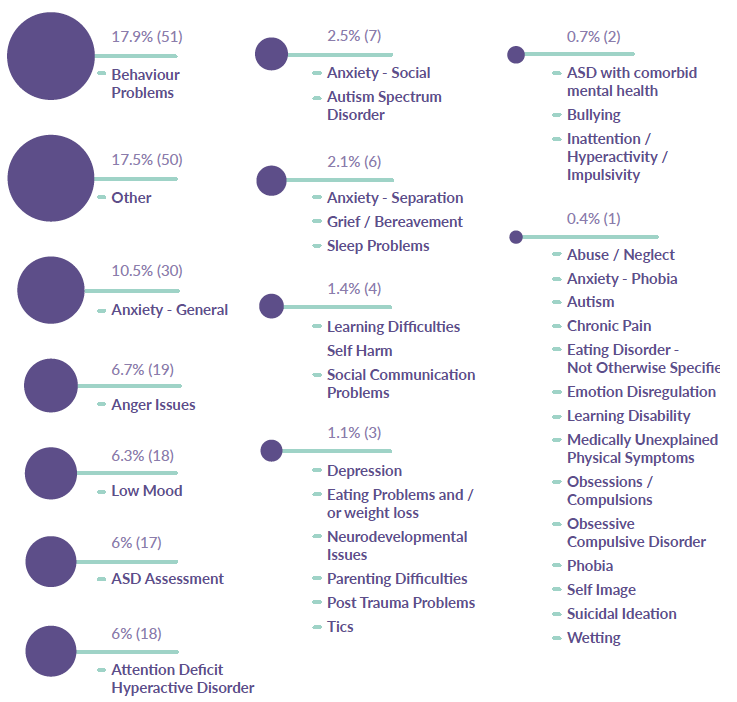
Source: ISD CAMHS Rejected Referrals Audit
In the screening questionairre which formed part of the qualitative research, children, young people and their families were invited to record the main reason they had for seeking referral to CAMHS. The results show anxiety was the most common reason for the young people to seek a referral to CAMHS.
Figure 12: Reason for referral, collected during qualitative element of the audit
| Reasons for referral | |
|---|---|
| Anxiety | 146 |
| Low mood/ depression | 87 |
| Self-harm | 67 |
| Suicidal ideation | 54 |
| Other | 52 |
| Behaviour problems | 47 |
| Anger issues | 41 |
| ASD assessment | 31 |
| ASD / Autism / Aspergers | 25 |
| Eating disorder / eating problems | 17 |
| Sleep problems | 15 |
| ADHD | 15 |
| N/A | 11 |
Note: it was possible to mention more than one reason
Source: SAMH CAMHS Rejected Referral Audit
There are other reasons for a CAMHS referral, beyond the possible existence of a medical problem. These include:
- A requirement to go through CAMHS for certain issues
Some children, young people and families reported having to go to CAMHS to be assessed for Autistic Spectrum Disorder ( ASD), Attention Deficit Hyperactivity Disorder ( ADHD) or Autism, or in order to be prescribed psychiatric medication.
- Previous experience of CAMHS
Some families had previously been through CAMHS with another child or family member, and felt they now needed its input again.
“My oldest boy had been diagnosed with Asperger’s, so he’s on the autism spectrum and my youngest one was showing similar traits.” (Parent, depth)
- Lack of alternatives
Children, young people, their families and referrers often spoke of a lack of alternatives to CAMHS for children and young people with emotional, behavioural and mental health problems across all levels of severity.
“To be honest the GP was, I mean he was lovely, but he was a wee bit lost at where to refer him to. He says, “I don’t think there is anywhere else that I can refer him to other than CAMHS.” But he didn’t think it was a CAMHS problem as it were.” (Parent, depth)
- Feeling as though they have exhausted all other avenues
For many people, CAMHS was their last hope.
“We tried all the usual routes, paediatrician, going to the GP, but they all said this is CAMHS, we do need a bit of psychological intervention here.” (Parent, depth)
“I’d actually gone for all the classes in Teen Triple P and Incredible Years and all of those classes.” (Parent, group)
“I went to the school and they had said that they would get the school nurse involved. The school nurse then came back and said that it was something that they couldn’t help with, and they were going to get Home Link involved. The Home Link worker said that she would meet with H a few times and look to doing Seasons for Growth…however, at that time she was also pregnant and she was off sick a lot. Which didn’t help because then H never really got that support.” (Parent, depth)
“I was put on Incredible Years. [Then] I think there was a few visits to the doctors. The school was doing wee bits and pieces to try and help, to get an educational psychologist on board but, again, we were given a few different books to read and things. I had done some research online because there wasn’t really a great deal of information available.” (Parent, depth)
Others reported previous CAMHS involvement for the child or young person being referred, and were seeking a follow-up or a transfer to a different geographic area. Reasons for this included:
- Previous ASD assessment
- Previous treatment given but discharged
- Moved health board
“We were under CAMHS in (one health board)….and when they tried to refer her to the CAMHS in (another health board), they told her she didn’t meet their criteria, that she was Tier 2 and not Tier 3.” (Parent, depth)
Referral screening time
The qualitative research found that when a referral is being made through a GP, it is submitted quickly. However, it was apparent that there was often a lengthy period pre-referral, where families are trying to manage without support, or looking for advice and support from third sector organisations, online resources or consulting with teachers. By the time parents and young people get to the referral stage, they are looking for immediate help.
“We’ve struggled for years and years and years and are still continuing to struggle with no help, no answers and J is in crisis.” (Parent, depth)
Both the quantitative and qualitative elements found that most rejections were received quickly following a referral. Whilst this is not necessarily a bad thing, the qualitative element found that this can come as a shock to the child or young person and their family, who, having been referred, are expecting a face to face assessment, and then to receive help. Improvements in communication and better understanding of process would help.
During the quantitative audit, data was collected on the date the referral was received by the service and the ‘date the referral was screened’ i.e. triaged or assessed by the service. The data showed that (Figure 13):
- 44% of referrals were triaged/assessed on the same day as they were received
- 44% are seen between one and five days, and
- 10% in less than 20 days (between six and 20)
The referrals that were screened between six and 20 days were across five Audit Boards, thus eliminating any pattern for referral screening processes. It was found that only two referrals (0.7%) were classed as ‘pending’ as they were awaiting a decision on the referral during the audit period. These two records were found to be triaged in the first week of March with a screening time of 21 and 30 days respectively.
Figure 13: Screening time upon referral to CAMHS
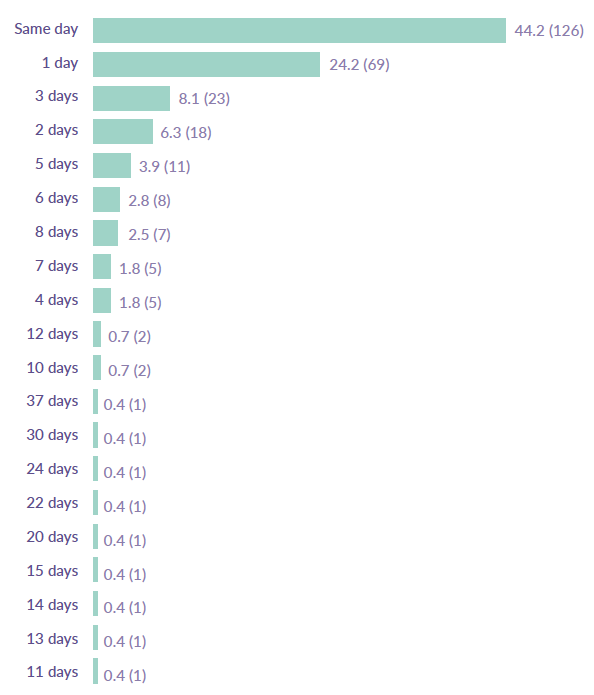
Source: ISD CAMHS Rejected Referrals Audit
It should be noted that referral screening time has been calculated based on seven days and these findings therefore do not account for weekends where screening may not take place.
It was also noted that one NHS Board uses a different practice to screen or assess referrals. Most children and young people at this NHS Board are offered an initial assessment appointment. From there they are seen by the service or directly signposted to other areas of help. The child or young person may be discharged after this assessment appointment which effectively means they are rejected, as this appointment serves as triage or review for the referral. The quantitative audit found that the main reason these children and young people were rejected during February 2018 was that CAMHS was unsuitable for them.
Children, young people and their families’ expectations pre-referral
The main expectation at referral stage is that the child or young person will get help from CAMHS.
“I was hoping I could see a counsellor just to sort of talk through what I was worried about.” (Young person, depth)
“We thought people were going to intervene, people were going to actually help us.” (Parent, group)
“I didn’t actually know that much about CAMHS, I hadn’t ever heard of it before, so I really went in with no expectation…. I was just hoping that they’d help me.” (Young person, depth)
“We’re in limbo at the moment, I’m not sure whether this referral…. is going to be accepted. Obviously we’re keeping our fingers crossed but we’ve had two in the last six months which have been knocked back and it’s just devastating, absolutely devastating because I know that Z needs some kind of intervention.” (Parent, depth)
People generally expect that it may take a little time (weeks) to hear back.
“I’ve read many articles, I’ve done lots of reading online and stuff and I knew how under pressure the service was, so I was aware that it was going to be a long wait.” (Parent, depth)
This has the important consequence that almost no-one is prepared to hear within days that their referral has been rejected.
- For some, expectations are solely based on what the referrer tells them
“But the GP, she did the referral, she had said “Please be aware that this will just get completely rejected.” (Parent, depth)
“We are failing our young people when it takes several months to hear back from a CAMHS referral, for it to be refused on the grounds that the young person does not have ‘complex’ needs based on minimal information written in a referral letter, without a one-to-one professional assessment. Alternatives to CAMHS also need to be put in place for young people who do not have multiple social, emotional or behavioural issues. e.g. emotional literacy education in schools or a GP accessible counselling service. Psychologists should be available and accessible to all young people who experience any form of mental health issue.” (Parent, survey)
Information given at point of referral
29% of respondents to the online survey were given an idea of timescales at the point of referral.
The type of information given at the referral stage varies hugely based on the individual referrer:
- Some give resources for use by parent and or young person whilst waiting for assessment
“I was like given a bit about what I could do in the meantime before obviously, if I got accepted…. I got given like resources and things like that to read through, I got told a bit about what they might be able to do for me but then that was kind of it.” (Young person, depth)
“When I was referred the second time from my GP he gave the number for Breathing Space and for Child Line.” (Young person, group)
- Some give an estimate of timescales
“He said that there would be quite a long waiting list.” (Young person, depth)
“They would send a referral letter and to expect a long waiting list time for an appointment.” (Parent, survey)
- Some express a lack of confidence that the referral will be accepted
“They’d probably reject him as taking on few children unless self-harming or expressing suicidal thoughts.” (Parent, survey)
“We were told that our referral would probably be rejected due to our daughters young age.” (Parent, survey)
- Some give no information at all
“Not a lot, to be honest, the GP didn’t really say anything.” (Parent, depth)
Being Referred: Participants’ suggestions for Improvement
In relation to being referred, parents and young people wanted:
- More clarity on the requirements for being accepted to CAMHS
“ CAMHS should have a set deadline for when they acknowledge getting receipt of something and explain how they make the decisions.” (Parent, depth)
“I think if we knew what the criteria really was, it would be easier for us.” (Parent, depth)
- More information to be submitted prior to the referral:
Greater input from parents and young people themselves
A full picture to be presented, with information from the school, GP and other professionals involved with the child or young person
- More thought about the transition process between CAMHS and adult services
Because of long waiting times, young people can end up being ineligible by the time they are assessed and accepted
- A potential “fast track” referral process for children and young people who are looked after, adopted or at risk
- Suggestions of how to help and signposting to websites, third sector organisations and other resources at the point of referral
“If we at least had some things that we could take away from CAMHS and put into practice at home I would know that I was doing all I could do to try and bring the situation down, but I don’t know exactly what it is I should be doing.” (Parent, depth)
Contact
An easy-read version is available on request from MentalHealthStrategyandCoordinationUnit@gov.scot.