Rejected referrals to child and adolescent mental health services: audit
A qualitative and quantitative audit of rejected referrals to Child and Adolescent Mental Health Services (CAMHS).
Findings: Being Assessed
Of the 253 people who took part in the online survey, 31% of people report getting a face to face assessment. Most rejections are made on the basis of the written referral. Where assessments are held, processes are inconsistent in terms of the time taken between referral and assessment, who attends the assessment and what information is given about what will happen next. In some cases the parent and child are both seen, in others only one or the other is seen. Practice also varies in terms of whether parents and children are seen together or separately, and this can cause difficulties for parents seeking to explain the situation. Young people find the assessment difficult and many leave feeling that they have not been properly listened to. Where the child or young person has a diagnosis of Autistic Spectrum Disorder ( ASD), some people report being told that CAMHS could not help with an apparent mental health issue because of the ASD diagnosis.
One third of those referrals that are rejected get to the point of a face to face assessment: it was reported by the 253 people who took part in the online survey that no assessment meeting was held in more than two-thirds of cases.
Figure 14: Invited to assessment meeting with CAMHS
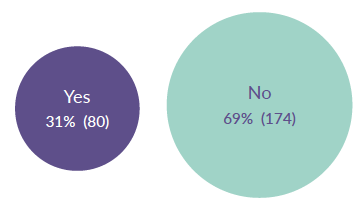
Source: SAMH CAMHS Rejected Referral Audit
How long do children and young people wait for an assessment?
The preceding section shows that, in this sample of rejected referrals, most people did not receive a face to face assessment. However, the qualitative element of this research did explore experiences of children and young people who are waiting for a face to face assessment where one takes place.
Perceptions of the time taken between referral and assessment vary. Many of those in the sample had been through multiple referrals and/or many steps in the process of getting help. That meant that their assessments of how long they waited could be vague.
Some waited months after their referral, while others were invited for an assessment relatively quickly.
“It was about, I’d say six, seven months maybe.” (Young person, depth)
“First time it was two weeks, I think. Second time, rejected. Third time, rejected. Fourth time, it was a week but that was an emergency referral because I tried to commit suicide in school so that was an immediate referral. And then the fourth time it was through A and E so that was a week as well, so yeah. I’ve not had bad waiting times it was just when I kept on getting rejected I was just in a really, really bad place and I feel like say if I got the help that I needed then when I got rejected, I probably wouldn’t have had as many suicide attempts or had to go up to A and E so many times.” (Young person, group)
For those who have to wait longer, the effect is usually negative.
“You kind of just forget that it’s done because you don’t hear from them for so long, at first you’re like it’s a bit better because you know you’ve done something to try and get help but because it takes so long, that initial period is a bit more relief knowing that you’ve done something that’s going to maybe get you help, it kind of just goes away and you just go back to feeling as rubbish before, you kind of just feel forgotten.” (Young person, depth)
“I think not knowing if you’re going to get accepted, rejected, it can make your family quite stressed, especially if things aren’t getting better so it noticeably impacts everyone pretty much, especially my parents were quite like concerned.” (Young person, depth)
What support are children, young people and their families offered when awaiting assessment?
Most received no or little support while waiting for assessment.
“They never spoke to me after the referral, not even a phone conversation, nothing.” (Parent, depth)
“No, nothing, we were just left to deal with it.” (Parent, depth)
“No other support. GP, obviously was very understanding but their hands are tied.” (Parent, group)
Where support was offered, it tended to be via schools.
“The school were quite supportive at that point.” (Parent, depth)
“I was still in contact with the school so they were also looking at other avenues because they were aware that there could be a long waiting list for any assessments from CAMHS.” (Parent, depth)
What is the process for assessing a child or young person for CAMHS?
The qualitative research suggests an inconsistent approach regarding whether both the young person and the parent were at the assessment, or they were seen separately.
“We met with two psychologists then I was separated from my child (then 5) while they spoke to her.” (Parent, survey)
“My son was observed in a different room while I had the opportunity to speak to the clinical psychologist.” (Parent, survey)
“They spoke to both myself and my daughter. However, we were in the same room which made it very difficult to speak openly in front of my daughter and so I requested a time to meet them separately but it was declined.” (Parent, survey)
Some people found this approach difficult. Parents reported feeling uncomfortable when asked to provide background details and answer questions in front of their child.
“I was mainly disappointed…because we would have spoke a lot stronger if he wasn’t there. My son is very, very sensitive, and it was things you would not necessarily say in front of him.” (Parent, depth)
Children and young people sometimes wanted the parent to be present and at other times not.
“I had my mum with me, and they were asking me loads of these questions and I started getting a little bit uncomfortable, just because I wasn’t sure how to answer them, I wasn’t very comfortable talking about it. Yeah, and they asked my mum if she wanted to leave the room, if that would help, and, that made me feel even worse, because it felt like I was hiding stuff from my mum. Yeah, obviously that’s just like, they’re just asking, to see it’ll be, to make me more comfortable, but it just, it made me feel worse and I ended up speaking less.” (Young person, depth)
There is a general sense that parents and young people don’t feel they are being properly listened to during the assessment.
“I just felt that they didn’t want to listen to what I had to say.” (Parent, depth)
“He asked me and my parents questions about how I was feeling, questions about my past, he asked if I had ever experienced panic attacks but I didn’t know what that was so answered ‘no’ when I had in fact had panic attacks and quite often. I told him I had tried to kill myself and he asked if my parents knew, and said he would not tell them, then he decided that exercise was the best thing for me and that they could offer me no more help.” (Young person, survey)
For young people in particular the assessment process can be very difficult and quite traumatic.
“I basically had to spill all my deepest thoughts and feelings to a referral person who did nothing except take note of all of this for my file. I had self-harmed the night before the visit, as well as had been trying to kill myself at this point but could not bring myself to it. I told this to the person, as well as the fact I had a day in my head to try again. At the end of the session, they told me they could not help me for the THIRD time.” (Young person, survey)
“I told them all about my life and what’s gone wrong in it, I didn’t get to explain everything and it was a really difficult experience, having to retell everything wrong about my life.” (Young person, survey)
The research found some particular issues where the child or young person had been referred for possible Autistic Spectrum Disorder ( ASD). Some reported difficulties in getting an appointment in the first place, while others were unhappy with the assessment process.
“So, within 40 minutes to 45 minutes I had been in, seen and spoke to people, went to the shop, come back, and was told that X was not on the spectrum.” (Parent, depth)
Once a diagnosis has been given, there is often no further support provided. Where the child or young person already has a diagnosis of ASD, we found some parents being told that CAMHS could not help with an apparent behavioural, emotional or mental health issue because of the ASD diagnosis. This left families feeling there was nowhere else for them to turn.
“I was devastated, honestly, and I was very, very upset for her and I was angry that she had been discriminated against because she had a name, a title against her, autism spectrum disorder and that that was somehow stopping her from getting a service that other children with high levels of stress and anxiety were getting.” (Parent, depth)
There seems to be little consistency in what information is provided at the end of the assessment, so young people and their parents leave without a clear understanding of what will happen next.
“I kind of thought once we have the assessment then it will only be another couple of weeks waiting and then I’ll actually get help.” (Young person, group)
“It was never really clear what they would do, it’s not like you’d get a letter and you’ll be informed about it and stuff like that, they never really said what would happen next.” (Young person, depth)
“I think it becomes more confusing because you don’t really know what’s going to happen next after that, like they don’t really give you the options of what might happen or an indication of what might happen in your case, there’s just like a general assumption that you kind of know what’s going to happen next.” (Young person, depth)
In addition, the language used is not always clear, especially to young people, meaning they do not always understand what is being recommended by CAMHS.
“I still remember to this day, [ CAMHS said] ‘Your problems are relational in origin’, which when you’re 17, you’re like, ‘What does that mean?’. And even today no-one can tell me what that means.” (Young person, group)
“It was confusing as well. Just the language was confusing….It wasn’t a very clear and helpful letter to be honest.” (Parent, depth)
Participants’ suggestions for improvement: being assessed
In relation to being assessed, parents and young people wanted:
- Clarity around the assessment process, with a clearer triage process and how decisions are taken whether to conduct a face to face assessment.
“Say okay, if you score 10 points then you go to CAMHS, but if you score 5 or under then it’s community based and here’s the list.” (Parent, group)
- An expectation that CAMHS will meet children and young people for assessment, in an environment in which they feel comfortable (particularly for those with an ASD diagnosis)
“That every child at least gets an initial appointment to see what the need is. If unable to progress with CAMHS, then appropriate guidance or information given.” (Parent, survey)
“I don’t see how they can reject anybody without seeing them.” (Parent, group)
- The opportunity for parents and young people to meet CAMHS staff separately, where they feel it would be helpful
“There’s not enough support, that if you’ve got to take the child with you to the appointment, make time so the adult or one of the parents can talk to the person without the child sitting there so that the parent can talk freely.” (Parent, depth)
“Your initial discussion, you should be able to have it without the child being present. So, if you have concerns about their ability to cope there has to be a way that you can talk about your child’s problems without the child being there…. I can’t imagine somebody talking about me in those terms and me sitting there and having no voice and feeling no good about myself.” (Parent, depth)
“If I had a parent with me, at any of the appointments that I did have with them, they would listen to them rather than what I was saying, and then give me like advice based on what my parents were saying.” (Young person, depth)
- The involvement of a wider group of family and professionals who are working with the young person, to gain a more holistic picture
“The autism assessment was very good, he [YP] was spoken to for an hour and a half, there were three professionals there, a language specialist, a psychologist and the autism assessor herself and then afterwards they met with us, spoke with us, myself and my husband for an hour or so and they had received information from the school as well, they’d asked for information from the school.” (Parent, depth)
- Make better use of multi-disciplinary child planning meetings where all those who are supporting the child or young person can gain a holistic picture
- A more person-centred approach by staff who would listen more, create a welcoming atmosphere, speak in plain English and not be dismissive or patronising
“If they made more of an effort to make, look for example, me or another patient feel more, more engaged, less like an object, less like something to be examined.” (Young Person, depth)
Contact
An easy-read version is available on request from MentalHealthStrategyandCoordinationUnit@gov.scot.